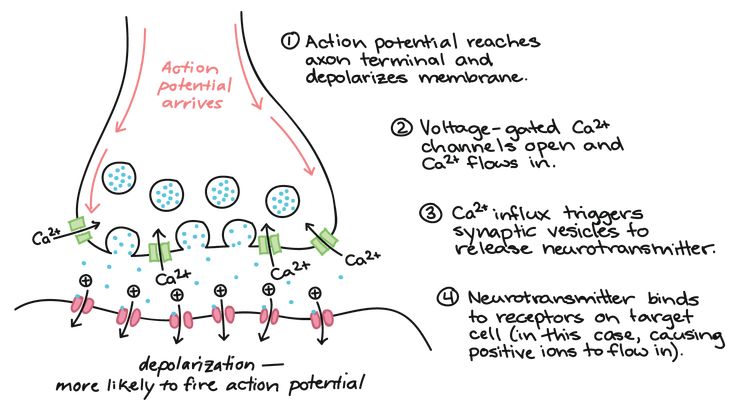
What does gaba neurotransmitter do
GABA Receptor - StatPearls - NCBI Bookshelf
Mary J. Allen; Sarah Sabir; Sandeep Sharma.
Author Information and Affiliations
Last Update: February 17, 2022.
Introduction
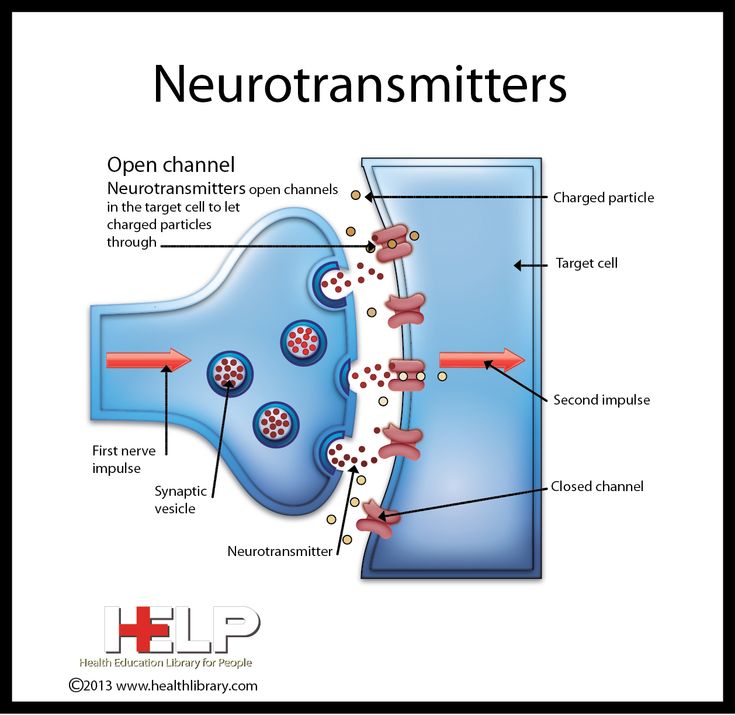
Gamma-aminobutyric acid (GABA) is an amino acid that functions as the primary inhibitory neurotransmitter for the central nervous system (CNS). It functions to reduce neuronal excitability by inhibiting nerve transmission. GABAergic neurons are located when the hippocampus, thalamus, basal ganglia, hypothalamus, and brainstem. The balance between inhibitory neuronal transmission via GABA and excitatory neuronal transmission via glutamate is essential for proper cell membrane stability and neurologic function.
Function
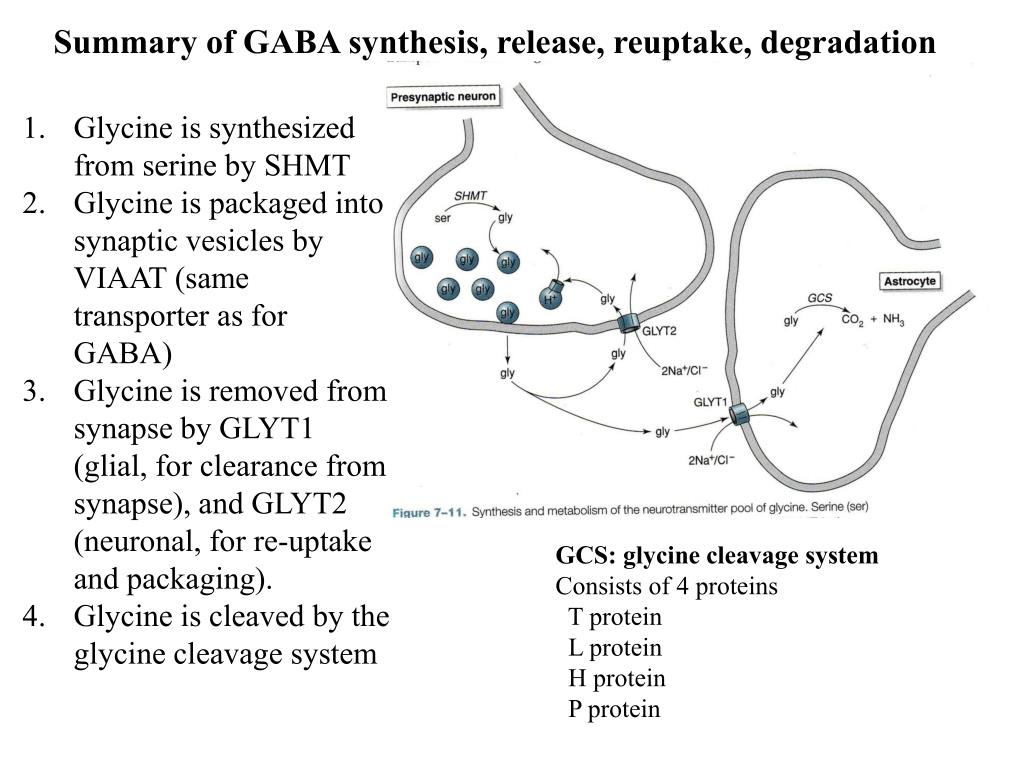
Synthesis
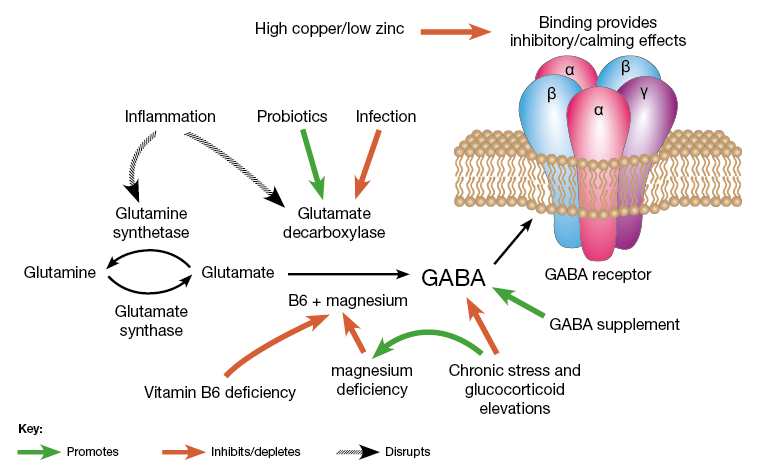
GABA is formed from glutamate via the addition of glutamate decarboxylase and vitamin B6. GABA can then be used to form succinate, which is involved in the citric acid cycle. Once GABA is formed, is it released into the post-synaptic terminals of neurons.
Although glutamate is a precursor for GABA, their roles are opposite in the nervous system. Glutamate is considered an excitatory neurotransmitter, while GABA is an inhibitory neurotransmitter. The imbalance of glutamate and GABA can play a role in various pathologies, as discussed in Clinical Significance.[1]
Receptors
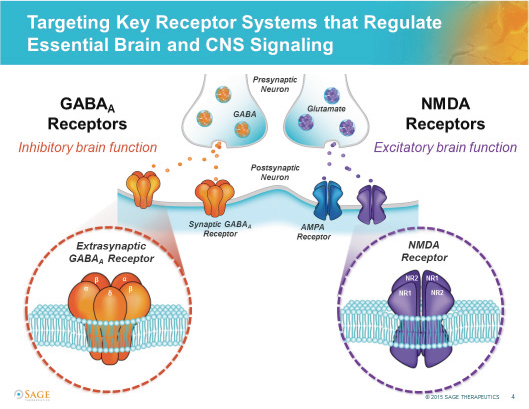
GABA receptors are receptors that respond when GABA is released into the post-synaptic nerve terminal. They are considered the chief inhibitory receptors for the central nervous system. GABA receptors are subdivided into GABAa and GABAb. [2]
GABAa is classified as a ligand-gated ion channel/inotropic receptor. GABAa is considered in fast synaptic inhibition. Upon the receptor binding to GABA, an ion pore opens to allow chloride to move across the cell membrane. Chloride is a negatively charged ion and will follow into the area of positive charge. Typically, chloride will flow into the intracellular space.
 The addition of negative charge will decrease the resting potential of the cell, thus causing an inhibitory effect. GABAa receptors are located throughout the central nervous system. However, they have high concentrations in the limbic system and the retina. [2]
The addition of negative charge will decrease the resting potential of the cell, thus causing an inhibitory effect. GABAa receptors are located throughout the central nervous system. However, they have high concentrations in the limbic system and the retina. [2]GABAb receptor is a G-couple protein receptor. GABAb receptors are considered slow synaptic inhibitors. After GABA has bound to the receptor, potassium conductance is increased. Adenylyl cyclase is activated, which prevents calcium entry thus inhibits presynaptic release of other neurotransmitters. GABAb locations include the thalamic pathways and cerebral cortex.[3]
Brain Development
Within the adult central nervous system, GABA is the primary inhibitory neurotransmitter. However, during embryonic development, GABA acts as an excitatory neurotransmitter. GABA is thought to be the first neurotransmitter active within the developing brain and plays a role in the proliferation of neuronal progenitor cells.
 High levels of GABA in ventricular areas increased proliferation and neural progenitor cell size; however, in the subventricular zone, GABA decreased proliferation. [4],[5]
High levels of GABA in ventricular areas increased proliferation and neural progenitor cell size; however, in the subventricular zone, GABA decreased proliferation. [4],[5]
Clinical Significance
Various diseases have been associated with low levels of GABA. Many psychiatric illnesses have been linked to low concentrations of GABA. Generalized anxiety is one example. As GABA is an inhibitory neurotransmitter, decreased concentration of it would produce a feeling of anxiousness. It has also been associated with schizophrenia, autism spectrum disorder, and major depressive disorder. It is important to note that although GABA concentrations may be altered in these psychiatric diseases, treatment using GABAa receptor agonists are not first-line therapy, due to high addiction potential and potentially fatal adverse effect. Valproic acid, a GABA analog, can be used for mood instability due to the enhancement of GABA concentrations. [1],[6]
Seizures and epilepsy are associated with low levels of GABA. With decreased levels of inhibition in the cerebral cortex, cells become depolarized, leading to seizure activity. GABA agonists, such as Valproic acid, are used for the treatment of seizures. Abrupt withdrawal from medications such as benzodiazepines, a GABAa positive allosteric modulator, can provoke seizures. Also, GABA antagonists are pro-convulsant. [7]
With decreased levels of inhibition in the cerebral cortex, cells become depolarized, leading to seizure activity. GABA agonists, such as Valproic acid, are used for the treatment of seizures. Abrupt withdrawal from medications such as benzodiazepines, a GABAa positive allosteric modulator, can provoke seizures. Also, GABA antagonists are pro-convulsant. [7]
Inherited disorders of GABA metabolism are rare and therefore require an increase in clinical suspension. The most common diseases are GABA-transaminase deficiency, succinic semialdehyde dehydrogenase deficiency (SSADH), and homocarnosinosis. SSADH is the most common of neurotransmitter deficiencies. It presents with vague phenotype, varying neurological manifestations, and psychiatric illness. GABA is unable to be converted to succinic acid, and gamma-hydroxybutyrate (GHB) accumulates. Elevated concentrations of GABA and GHB are found within serum and urine. Diagnosis can be made with urinary excretion of GABA and increased signaling in the globus pallidus on MRI.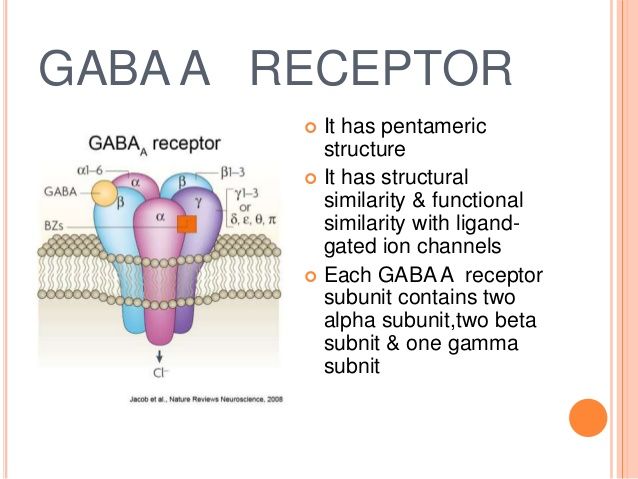 Characteristics include expressive language impairment, hypotonia, and seizures. The most common neuropsychiatric problem is sleep disturbance; other issues include inattention, hyperactivity, and obsessive-compulsive disorder (OCD). There is currently no standard treatment for SSADH deficiency. [8]
Characteristics include expressive language impairment, hypotonia, and seizures. The most common neuropsychiatric problem is sleep disturbance; other issues include inattention, hyperactivity, and obsessive-compulsive disorder (OCD). There is currently no standard treatment for SSADH deficiency. [8]
GABA-transaminase deficiency and homocarnosinosis are much rarer. GABA-transaminase deficiency is an autosomal recessive disorder. Patients may have seizures presenting in the neonatal period; other manifestations include hypotonia, hyperreflexia, severely delayed psychomotor development, and a high-pitched cry. High concentrations of GABA are found in serum and cerebrospinal fluid (CSF). Cerebrospinal fluid is needed for diagnosis. Homocarnosinosis has only been reported in one family. Characteristics include progressive spastic diplegia, intellectual disability, and retinitis pigmentosa. [8]
Other Issues
Pharmacology
GABA Agonist
Drugs that increase the amount of GABA are commonly used as anticonvulsants, sedatives, and anxiolytics. Due to the increase in GABA, CNS depression is a common adverse effect. Some GABA agonist has addiction potential, and use should be monitored closely. [9]
Due to the increase in GABA, CNS depression is a common adverse effect. Some GABA agonist has addiction potential, and use should be monitored closely. [9]
GABAa receptor agonists: Alcohol (ethanol), barbiturates, and benzodiazepine. Barbiturates include phenobarbital and sodium thiopental. Barbiturates are less frequently used due to the high addiction potential and lack of an antidote. Benzodiazepines have mainly replaced them. Benzodiazepines can treat anxiety, agitation, seizures, and muscle spasms. Only short-term use of benzodiazepine is encouraged. An overdose of benzodiazepines can be fatal due to respiratory depression, especially if concomitant use with alcohol and opioids. Flumazenil is the reversal agent for benzodiazepines. [9]
GABAb receptor agonists: Baclofen, sodium oxybate (GHB), propofol. GABAb agonists increase CNS depression. Baclofen is typically used as a muscle relaxant to treat spasticity. GHB is approved for the treatment of narcolepsy.
 Severe CNS depression is common is GHB. Significant respiratory depression and obtundation are commonly seen. Propofol is used for induction and maintenance of general anesthesia. Adverse effects include hypotension, apnea, and involuntary body movements. [9][10][11]
Severe CNS depression is common is GHB. Significant respiratory depression and obtundation are commonly seen. Propofol is used for induction and maintenance of general anesthesia. Adverse effects include hypotension, apnea, and involuntary body movements. [9][10][11]GABA analogs: Valproic acid, pregabalin, gabapentin. GABA analogs are used as anticonvulsants, sedatives, and anxiolytics. As with other medications that increase GABA, CNS depression is common in this class of drugs. Valproate is prescribed for the treatment of seizures and mood instability. Pregabalin is used for fibromyalgia, diabetic neuropathy, and postherpetic neuralgia. Gabapentin’s approved uses include postherpetic neuralgia and seizures. Off-label uses include diabetic neuropathy and fibromyalgia. [9]
GABA Antagonist
Drugs that bind to but do not increase the amount of GABA are considered antagonists. Examples include picrotoxin or bicuculline methiodide.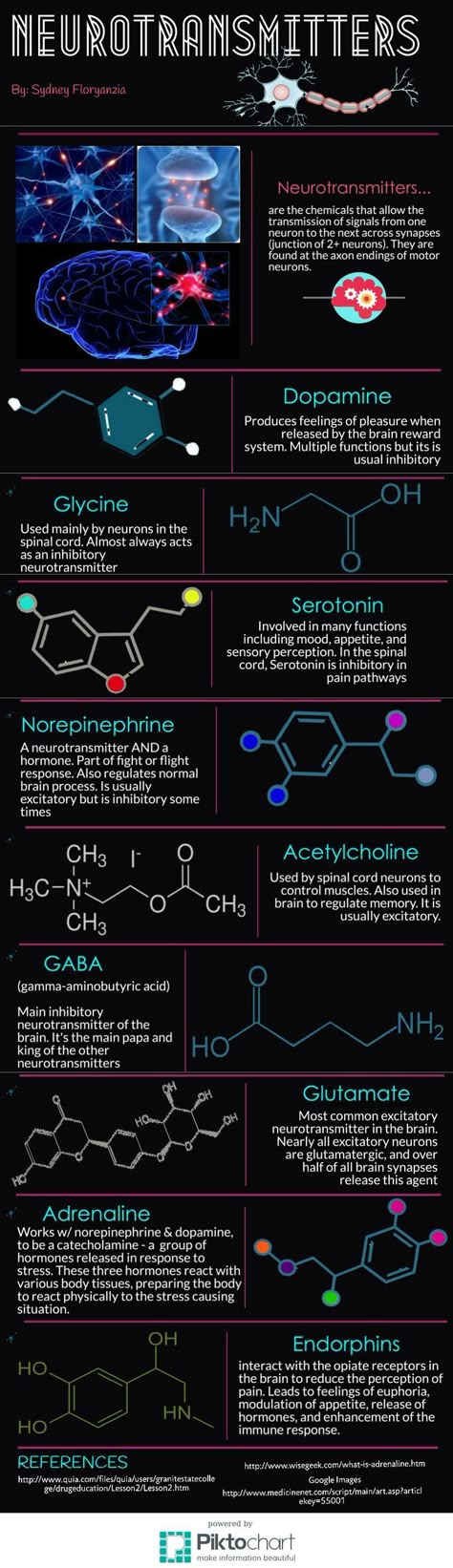 Both are mainly used for research. GABA antagonists are pro-convulsant and stimulants. [7],[12]
Both are mainly used for research. GABA antagonists are pro-convulsant and stimulants. [7],[12]
Enhancing Healthcare Team Outcomes
The healthcare team, including physicians, physician assistants, nurse practitioners, nurses, and pharmacists must work together to monitor the usage of GABA receptor agonists. The time should recall that low levels of GABA are associated with seizures and precautions should be taken.
Review Questions
Access free multiple choice questions on this topic.
Comment on this article.
References
- 1.
Wong CG, Bottiglieri T, Snead OC. GABA, gamma-hydroxybutyric acid, and neurological disease. Ann Neurol. 2003;54 Suppl 6:S3-12. [PubMed: 12891648]
- 2.
Sigel E, Steinmann ME. Structure, function, and modulation of GABA(A) receptors. J Biol Chem. 2012 Nov 23;287(48):40224-31. [PMC free article: PMC3504738] [PubMed: 23038269]
- 3.
Padgett CL, Slesinger PA.
 GABAB receptor coupling to G-proteins and ion channels. Adv Pharmacol. 2010;58:123-47. [PubMed: 20655481]
GABAB receptor coupling to G-proteins and ion channels. Adv Pharmacol. 2010;58:123-47. [PubMed: 20655481]- 4.
Wang DD, Kriegstein AR. Defining the role of GABA in cortical development. J Physiol. 2009 May 01;587(Pt 9):1873-9. [PMC free article: PMC2689328] [PubMed: 19153158]
- 5.
Wu C, Sun D. GABA receptors in brain development, function, and injury. Metab Brain Dis. 2015 Apr;30(2):367-79. [PMC free article: PMC4231020] [PubMed: 24820774]
- 6.
Schür RR, Draisma LW, Wijnen JP, Boks MP, Koevoets MG, Joëls M, Klomp DW, Kahn RS, Vinkers CH. Brain GABA levels across psychiatric disorders: A systematic literature review and meta-analysis of (1) H-MRS studies. Hum Brain Mapp. 2016 Sep;37(9):3337-52. [PMC free article: PMC6867515] [PubMed: 27145016]
- 7.
Treiman DM. GABAergic mechanisms in epilepsy. Epilepsia. 2001;42 Suppl 3:8-12. [PubMed: 11520315]
- 8.
Pearl PL, Hartka TR, Cabalza JL, Taylor J, Gibson MK.
 Inherited disorders of GABA metabolism. Future Neurol. 2006 Sep;1(5):631-636. [PMC free article: PMC3675887] [PubMed: 23842532]
Inherited disorders of GABA metabolism. Future Neurol. 2006 Sep;1(5):631-636. [PMC free article: PMC3675887] [PubMed: 23842532]- 9.
Chen X, de Haas S, de Kam M, van Gerven J. An Overview of the CNS-Pharmacodynamic Profiles of Nonselective and Selective GABA Agonists. Adv Pharmacol Sci. 2012;2012:134523. [PMC free article: PMC3273701] [PubMed: 22363345]
- 10.
Cash CD. Gamma-hydroxybutyrate: an overview of the pros and cons for it being a neurotransmitter and/or a useful therapeutic agent. Neurosci Biobehav Rev. 1994 Summer;18(2):291-304. [PubMed: 7914688]
- 11.
Brohan J, Goudra BG. The Role of GABA Receptor Agonists in Anesthesia and Sedation. CNS Drugs. 2017 Oct;31(10):845-856. [PubMed: 29039138]
- 12.
Johnston GA. Advantages of an antagonist: bicuculline and other GABA antagonists. Br J Pharmacol. 2013 May;169(2):328-36. [PMC free article: PMC3651659] [PubMed: 23425285]
Dystonia
Overview
Dystonia can happen for many reasons and can take many forms, depending on what causes it and the body parts affected.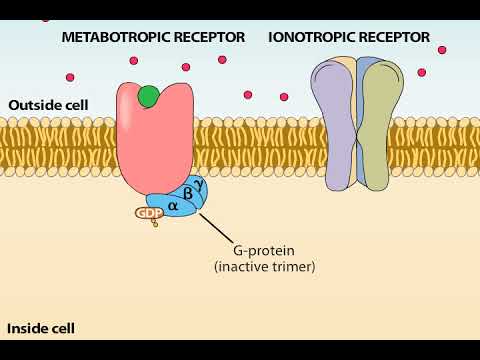
What is dystonia?
Dystonia is a nervous system disorder that causes uncontrollable muscle contractions, meaning a person’s muscles tense up without trying to make the muscles do so. Though it affects muscles, it’s actually an issue with your brain or another part of your nervous system.
The name “dystonia” is a combination of the Latin prefix “dys-,” and the Greek word “-tonos,” which refers to muscle tension. The combination of the two words describes a problem where your muscles tense up in a way that’s faulty or incorrect.
What is the difference between dystonia and dyskinesia?
Dyskinesia and dystonia are closely related but aren’t the same.
- Dyskinesia: This word comes from Greek. “Kinesia” comes from the word “kinesis,” which means “movement.” The combined word refers to movements that are faulty or happen in a way they shouldn't. Dyskinesias are involuntary muscle movements, meaning you don't control that they’re happening.
- Dystonia. This is a specific type of dyskinesia. With dystonia, muscles tense up for longer periods. Depending on what part of your body they happen in, they can often cause you to move or pose in certain ways.
Who does dystonia affect?
Depending on why it happens, anyone can develop dystonia. Some causes are age-specific, affecting people at birth or in childhood, while others are more likely to develop late in life.
How common is this condition?
The available research indicates that dystonia affects about 300,000 people in the United States. However, it’s difficult to know how common dystonia is because experts believe it’s underdiagnosed. That’s because dystonia can take so many different forms.
How does dystonia affect my body?
Dystonia is a brain condition that affects how your brain controls muscles throughout your body. This can affect muscles or groups of muscles in different ways. Exactly how and why this happens is still a mystery, though.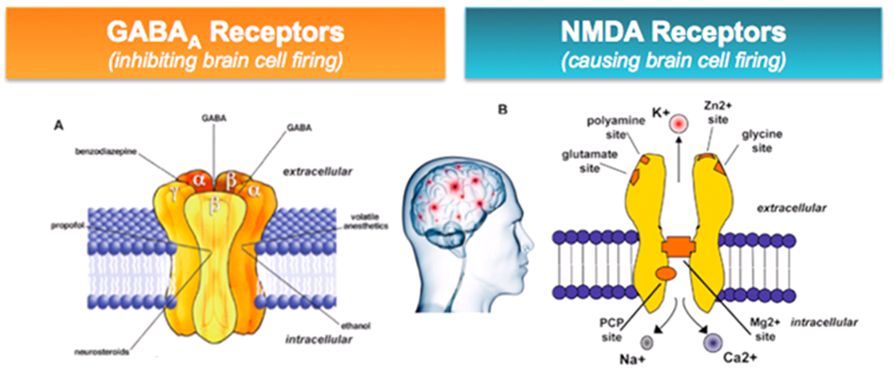 The effects of dystonia can also worsen when you feel tired or stressed, or if you drink caffeine or alcohol.
The effects of dystonia can also worsen when you feel tired or stressed, or if you drink caffeine or alcohol.
Some types of dystonia happen because of genetic mutations or conditions that disrupt the way parts of your brain work. This can cause the affected cells to work incorrectly, leading to faulty signals reaching your muscles and causing dystonia’s effects.
Dystonia can also happen because of injuries or conditions that disrupt your brain function, and some of these conditions are visible on imaging scans or detectable with certain tests. But it can also happen for other reasons.
Symptoms and Causes
What are the symptoms of dystonia?
In general, the key symptom of dystonia is uncontrollable muscle movements. These movements are often:
- Uncomfortable or even painful, sometimes feeling like electric shocks.
- Repetitive (especially with tremors).
- Variable in how long they last; some last seconds or minutes while others can continue for months.
- Twisting or stretching in nature, causing a person to look like they’re holding an unusual pose.
- Worse when using the affected muscles.
There are also some slight differences in the symptoms depending on where dystonia happens in your body. There are five main ways that symptoms happen (with more about each below):
- Focal dystonia.
- Segmental dystonia.
- Multifocal dystonia.
- Hemidystonia.
- Generalized dystonia.
Focal dystonia
Focal dystonia only affects one part of your body, and experts estimate these cases are about 10 times more common than generalized dystonia cases. Depending on the body part affected, this can take different forms:
- Eyelids: Eyelid spasms (blepharospasm).
- Jaw: Teeth-grinding (bruxism).
- Hand or wrist: Cramps or muscle spasms, often known as “writer’s cramp” or “musician’s cramp.” Golfers and baseball players often call these “the yips.
 ”
”
Segmental dystonia
This affects two or more adjacent body parts, such as different parts of your face, your head and neck, or your hand and arm. The most common example of segmental dystonia is cervical dystonia, which affects muscles in your head and neck. Another example is Meige syndrome, which affects multiple parts of your face.
Multifocal dystonia
This affects two or more body parts that aren’t directly connected. An example of this is dystonia that affects both hands. Tardive dyskinesia is an example of multifocal dystonia when it affects more than one non-connected part of your body.
Hemidystonia
Hemidystonia gets its name partly from the Greek word “hemi,” which means “half.” In this context, it affects just half — one side — of your body. An example of this is uncontrollable muscle movements in the right side of your face and your right hand. Strokes are a key cause of hemidystonia.
Generalized dystonia
This can involve your body’s leg and trunk (the main part of your body to which your arms, legs and head connect) or even your entire body. This can happen when dystonia is progressive, meaning it worsens over time. When focal dystonia turns into generalized dystonia, the symptoms spread from your limbs to the trunk of your body.
This can happen when dystonia is progressive, meaning it worsens over time. When focal dystonia turns into generalized dystonia, the symptoms spread from your limbs to the trunk of your body.
What causes dystonia?
Dystonia happens because of disruptions in how your brain should function. It usually involves your basal ganglia, a group of brain structures that link many different brain areas and coordinate how those areas work together.
Experts organize the causes of dystonia into three categories: Primary, secondary and “dystonia plus” conditions.
- Primary dystonia: This is when dystonia is the main condition. It’s usually “idiopathic,” which means it happens for an unknown reason. Experts also suspect genetics are a factor, meaning it runs in families.
- Secondary dystonia: This is when dystonia is a symptom of another condition or issue.
- Dystonia plus: These are neurological conditions where dystonia is a main symptom, but there are other symptoms, too.
Secondary dystonia causes
Secondary dystonia can happen because of, or in connection with, a wide range of reasons:
- Brain tumors.
- Other brain conditions (such as epilepsy, Parkinsonism, Parkinson’s disease, etc.).
- Cerebral hypoxia (especially for newborns who experienced a lack of oxygen during their birth).
- Drugs (prescription or recreational).
- Genetic conditions (such as Wilson’s disease or Huntington’s disease).
- Infections (such as encephalitis).
- Metabolic conditions.
- Stroke.
- Toxins and poisons (carbon monoxide poisoning, manganese poisoning, etc.).
- Traumatic brain injuries.
Is dystonia contagious?
Dystonia isn’t contagious, and you can’t spread it or catch it from others.
Diagnosis and Tests
How is dystonia diagnosed?
A healthcare provider, often a neurologist, can diagnose dystonia based on your symptoms, a neurological exam and various medical tests. Diagnosing dystonia is often tricky because its symptoms can happen with so many other conditions. That means it’s important to rule out those other conditions, some of which are life-threatening medical emergencies.
Diagnosing dystonia is often tricky because its symptoms can happen with so many other conditions. That means it’s important to rule out those other conditions, some of which are life-threatening medical emergencies.
What tests will be done to diagnose dystonia?
A wide range of lab, diagnostic and imaging tests are possible with dystonia. The most likely tests depend on your symptoms and what conditions healthcare providers suspect. Possible tests include, but aren’t limited to, the following:
- Blood tests (these can detect many problems, ranging from immune system issues to toxins and poisons, especially metals like copper or manganese).
- Computerized tomography (CT) scan.
- Electroencephalogram (EEG).
- Electromyogram (nerve conduction test).
- Genetic testing.
- Magnetic resonance imaging (MRI).
- Positron emission tomography (PET) scan.
- Spinal tap (lumbar puncture).
Other tests are possible, so your healthcare provider is the best person to ask about the tests they recommend for your specific case. The information they provide will be the most accurate for your circumstances.
The information they provide will be the most accurate for your circumstances.
Management and Treatment
How is dystonia treated, and is there a cure?
There’s no way to cure dystonia, but it might be treatable. Many possible treatments depend on the underlying cause or condition, or the symptoms you have. Your healthcare provider is the best person to tell you the treatment options they recommend in your specific situation.
Is there anything I can’t eat or drink with dystonia?
Your healthcare provider may recommend that you avoid caffeine and alcohol. For some people, drinking beverages that contain either can make dystonia symptoms worse.
What medications or treatments are used?
The possible medications or treatments for dystonia depend on why it’s happening and the specific symptoms you have. In general, the following treatment types are possible:
- Deep brain stimulation. This treatment involves surgery to implant electrodes into your brain.
 These electrodes deliver a mild electrical current to part of your brain, which can help the symptoms of dystonia. This is the most common and most useful surgical treatment for dystonia.
These electrodes deliver a mild electrical current to part of your brain, which can help the symptoms of dystonia. This is the most common and most useful surgical treatment for dystonia. - Medications. Depending on why dystonia happens, it’s often possible to treat it with medication. The medication (or combination of them) depends on the symptoms and the underlying cause — if there is one — of the dystonia.
- Botulinum toxin injections. Botulinum toxin — commonly known under the trademarked name Botox® — can block all nerve signals for weeks or even months when injected in the right place. That keeps the signals that cause dystonia from getting to your muscles, making botulinum toxin a treatment option for focal or some segmental dystonia symptoms.
- Physical, occupational and speech therapy. These forms of treatment can often help a person adapt or recover from dystonia, especially when dystonia happens because of a temporary health condition or circumstance.
Complications/side effects of treatment
The complications and side effects possible with dystonia depend on several factors, starting with the treatments themselves. Your healthcare provider is the best person to explain what’s possible or likely for you because they can give you information that considers your circumstances.
How do I take care of myself or manage symptoms?
Dystonia is a neurological problem, which means it isn’t something you can self-diagnose and self-treat. It’s also important to talk to your healthcare provider sooner than later because dystonia can happen with severe or life-threatening conditions.
How soon after treatment will I feel better, and how long does it take to recover?
The timeline for you to feel better and recover depends on why your dystonia happened, how severe it is, the treatments you received, any other health conditions you might have and more. Your healthcare provider is the best person to tell you about the likely timeline for you to feel better and recover.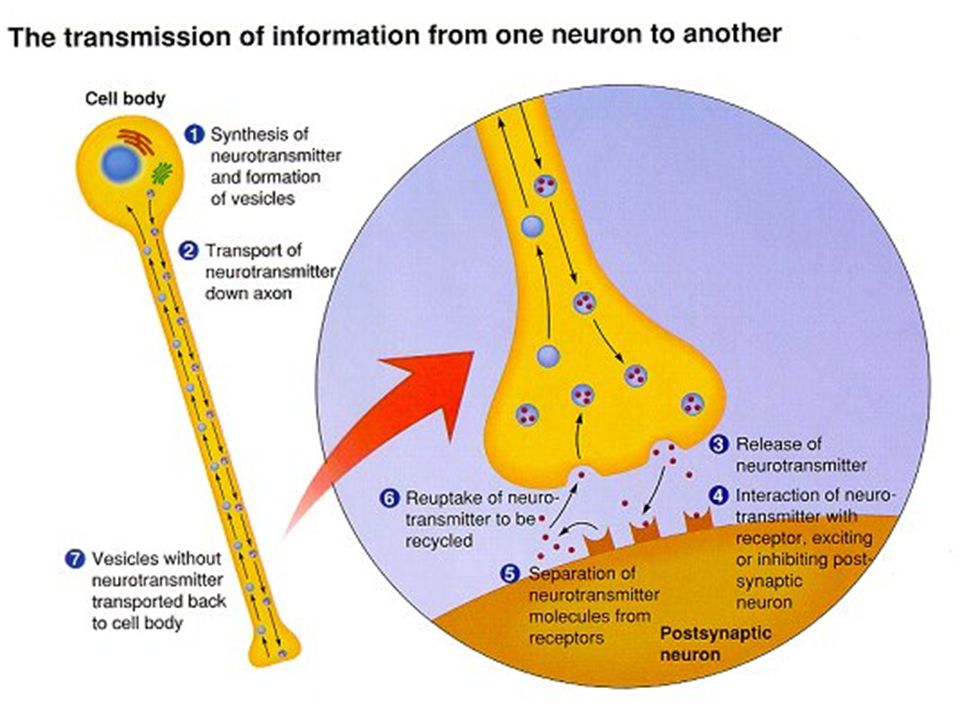
Prevention
How can I reduce my risk or prevent dystonia altogether?
Dystonia happens unpredictably, so you can’t prevent it. You also can’t reduce the risk of developing primary dystonia. That’s because you either inherit it or develop it for unknown reasons.
However, some causes of secondary dystonia are preventable, or you can reduce your risk of developing them. The things you can do include:
- Eat a balanced diet and maintain a healthy weight. Many conditions related to your circulatory and heart health, especially stroke, can damage areas of your brain, causing dystonia. Preventing, delaying or reducing the severity of these conditions can have a big effect on whether or not you develop dystonia.
- Don’t ignore infections. Eye and ear infections need fast treatment. When these infections spread to your brain, they become a serious threat. Infections can cause brain inflammation (encephalitis) that can lead to dystonia.
- Wear safety equipment. Traumatic brain injuries can damage your brain and cause dystonia. That makes safety equipment essential in reducing your risk of developing this condition.
- Manage your health conditions. Chronic conditions cause or contribute to other conditions that lead to dystonia. That includes conditions like Type 2 diabetes, high blood pressure, epilepsy and others.
Outlook / Prognosis
What is the outlook for dystonia, and what can I expect if I have it?
The outlook for dystonia depends on what caused it, when you develop it, where in your body it causes symptoms, your health history, the treatments you receive and more. Your healthcare provider is the best person to tell you more about the outlook for your case.
Primary dystonia outlook
In general, primary dystonia tends to have a less-favorable outlook when it happens early in life. That’s because primary dystonia can progress from focal to generalized.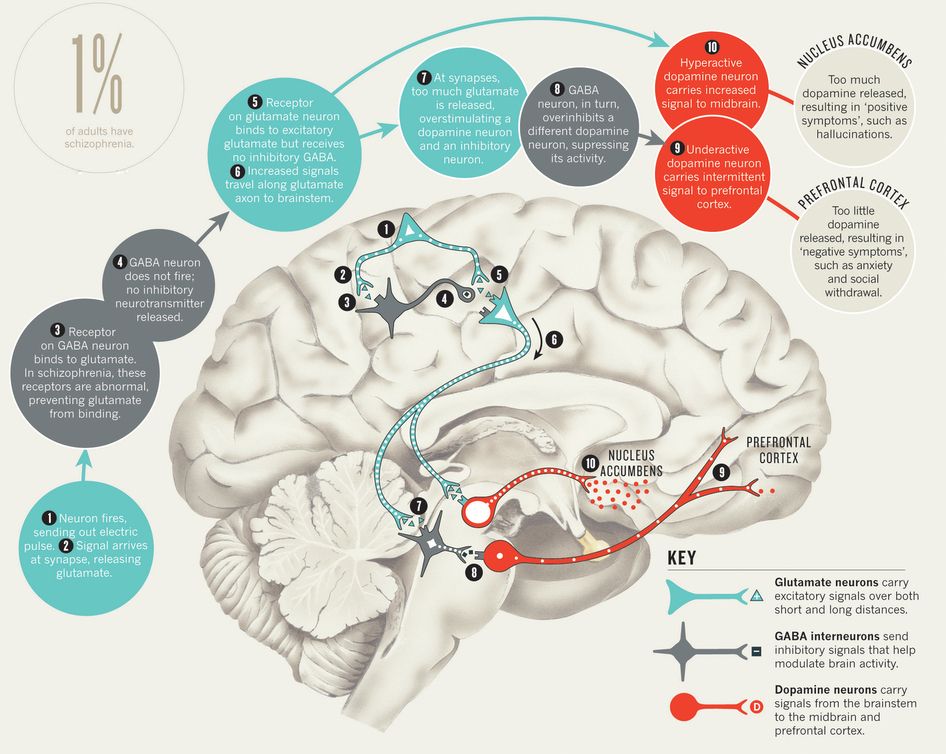 The earlier in life you develop this condition, the further the condition can progress.
The earlier in life you develop this condition, the further the condition can progress.
Focal dystonia tends to have a better outlook because it’s limited in how it affects your body. When dystonia affects multiple areas of your body, especially areas that aren’t directly connected, it’s usually because of more severe disruptions in your brain.
Secondary dystonia outlook
The outlook for secondary dystonia depends strongly on the condition causing it. When the underlying cause is a curable or reversible condition, there’s a much better likelihood of a good outcome. When it happens because of a chronic (long-term) condition, the odds of a good outcome go down. However, there are some chronic conditions where a good outcome and recovery from dystonia are still possible.
How long does dystonia last?
Primary dystonia is a lifelong condition once it develops. It’s treatable, but it isn’t curable and doesn’t go away on its own.
Secondary dystonia can be a short-term condition, depending on the underlying cause.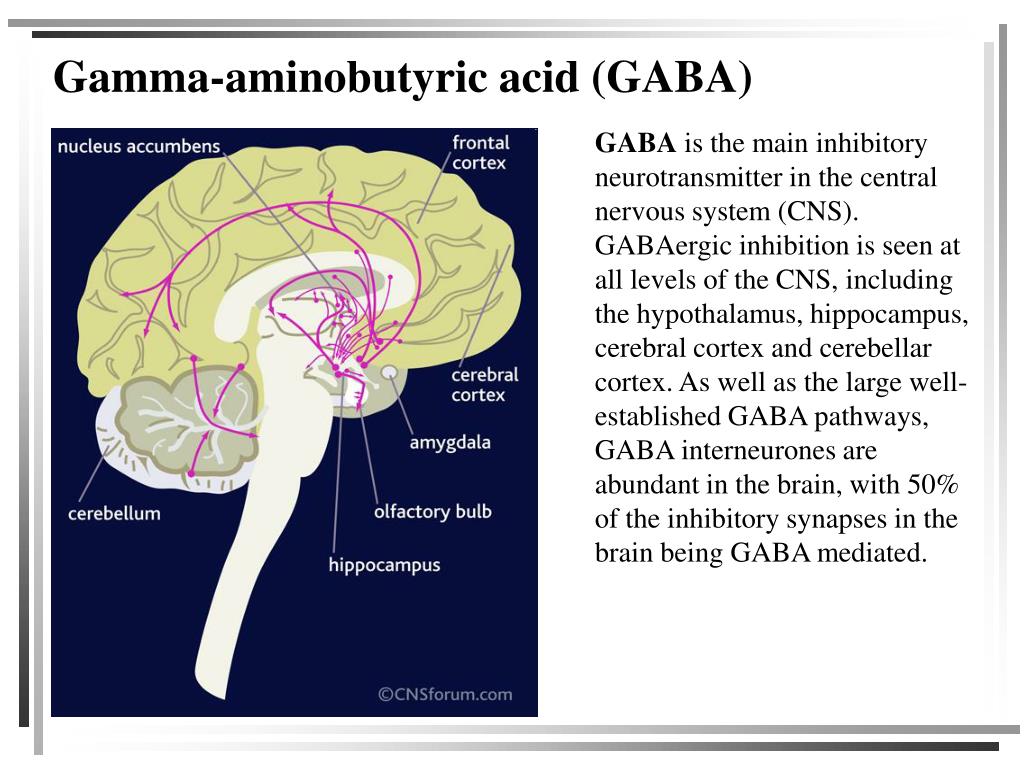 This is more likely with conditions like infections, traumatic injuries and certain drugs. However, other factors can influence this, so your healthcare provider is the best person to tell you what you should expect in your case.
This is more likely with conditions like infections, traumatic injuries and certain drugs. However, other factors can influence this, so your healthcare provider is the best person to tell you what you should expect in your case.
Living With
How do I take care of myself?
If you have dystonia, there may be some things you can do to take care of yourself, including:
- Avoid caffeine and alcohol if your healthcare provider recommends this. These can make dystonia symptoms worse.
- Manage your stress. Anxiety and stress can cause dystonia to worsen. You can reduce this risk by managing your stress and anxiety with techniques like meditation, relaxation training, exercise and more.
- Avoid activities that make symptoms worse. Some forms of dystonia are more likely to happen under certain circumstances. Avoiding those circumstances, when possible, can reduce the chances of dystonia symptoms flaring up.

- Learn how to manage your condition. Different forms of dystonia are often manageable with “sensory tricks.” A key term for this is “geste antagoniste,” which is French for “antagonistic gesture.” An antagonistic gesture can cause dystonia symptoms to get better temporarily, though experts don’t know exactly why this happens. An example of an antagonistic gesture is touching your chin or the side of your face to help relieve the symptoms of cervical dystonia (which affects muscles in your head and neck). Your healthcare provider can help find if you respond to these gestures and teach you how to use them.
- Take your medication. If you take medication for dystonia, take your medication as prescribed. Suddenly stopping your medication can worsen dystonia symptoms or cause other side effects.
When should I see my healthcare provider, and when should I seek care?
If you have dystonia, you should see your healthcare provider for follow-up visits as recommended. You should also see them if your symptoms change or worsen, especially if the changes disrupt your life and routine. Also see them if medications or other treatments lose effectiveness or cause side effects that are difficult to deal with or disruptive.
You should also see them if your symptoms change or worsen, especially if the changes disrupt your life and routine. Also see them if medications or other treatments lose effectiveness or cause side effects that are difficult to deal with or disruptive.
When should I go to ER?
You should go to the ER if you have any symptoms that could also happen with a stroke. To know when you need to call 911 (or your local emergency services number) because of stroke symptoms, remember to think FAST.
- F is for face. Does one or both sides of the person's face droop when they try to smile?
- A is for arm. Does one arm sag downward when the person tries to raise their arms upward?
- S is for speech. Can the person speak clearly and understand others talking to them?
- T is for time. Call 911 or your local emergency services number IMMEDIATELY if a person has the above symptoms. Stroke is a time-critical condition, and fast treatment is the best way to increase the chances of having a good outcome and recovery.
Frequently Asked Questions
What does dystonia feel like?
What dystonia feels like depends on what’s causing it, where it happens in your body, how severe it is and more. Dystonia can vary greatly from person to person, and what one person experiences with the same type of dystonia could be wildly different from what another person experiences.
For some people, dystonia causes minor symptoms, and the muscle movements feel like light fluttering or twitching. For others, the muscle movements are sharper, faster and may be uncomfortable or painful. Some types of dystonia cause muscle movements that feel like electric shocks.
What is the life expectancy of someone with dystonia?
The life expectancy with dystonia depends strongly on why it happens, if it happens in connection with any other conditions, your health history, the treatments you receive and more. Your healthcare provider is the best person to tell you more about whether or not dystonia affects your life expectancy and, if yes, how it will do so.
A note from Cleveland Clinic
Dystonia is a brain condition that causes faulty signals to your muscles, which makes those muscles move uncontrollably. This condition can happen for many reasons, ranging from lifelong inherited conditions to short-term illnesses. The severity of the symptoms and how widespread the effects are in your body can make this condition a minor inconvenience, or they can be severely disruptive and keep you from doing certain things.
While it isn’t curable, dystonia is often treatable, especially with certain causes. In some cases, dystonia may go away entirely when it happens with short-term or curable conditions.
GABA (GABA) what it is, how it works and what are the benefits
Contents:
➦ What is gamma-aminobutyric acid (GABA)
➦ How does GABA work?
➦ What are the benefits of GABA?
➦ GABA for athletes
➦ Gamma aminobutyric acid deficiency symptoms
➦ How to increase the level of Gamma?
➦ What is gamma-aminobutyric acid?
➦ The most popular GABA supplements in Phytomarket
➦ GABA in food products
➦ Gaba tea as a source of acid
➦ How to take a GABA supplement
➦ Side effects of GABA
➦ Frequently asked questions answered
Gamma-aminobutyric acid preparations are becoming increasingly popular among natural remedies with anti-stress properties. They are able to eliminate anxiety and improve sleep, they are also in demand in sports practice to enhance the growth of muscle mass. Learn about the benefits of this substance for the body and how it can be used in everyday life.
They are able to eliminate anxiety and improve sleep, they are also in demand in sports practice to enhance the growth of muscle mass. Learn about the benefits of this substance for the body and how it can be used in everyday life.
What is gamma-aminobutyric acid (GABA)
Gamma-aminobutyric acid (chemical formula C4H9NO2) or GABA is an organic substance that is synthesized by the body and is present in all areas of the brain. It is the main inhibitory neurotransmitter in the central nervous system, that is, it slows down the transmission of nerve impulses, and competes with glutamate, the main excitatory neurotransmitter, affecting approximately 30-40% of synaptic connections. In nature, this substance is present in some plants, such as valerian or green tea.
Neurotransmitters influence our thoughts, feelings, sensations. An imbalance between the main neurotransmitters (serotonin, dopamine, GABA and acetylcholine) can manifest itself in various psychological disorders.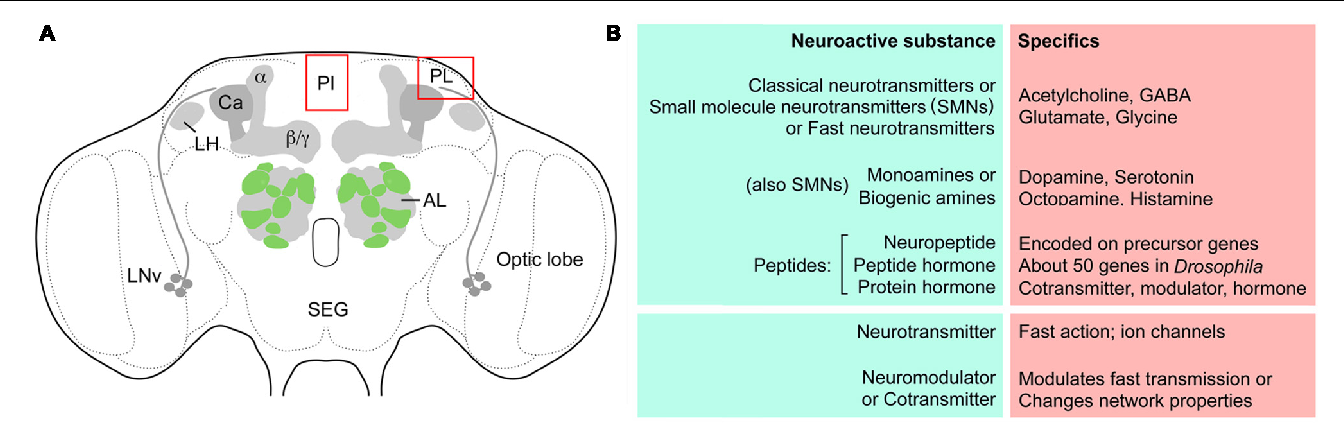
The main task of GABA is to block unnecessary information flows to create parity between the processes of excitation and inhibition in our brain, providing functions such as attention, motor and emotional control.
Gamma-aminobutyric acid receptors are found in high concentration in the cerebellum, thalamus and spinal cord. Moreover, recent studies have shown that GABA molecules are also present in the walls of the uterus, spermatozoa, retina, lungs and respiratory tract, as well as in the insulin-producing beta cells of the pancreas.
A bit of history
The presence of GABA in the brain became known in 1950, when the American scientist Eugene Roberts, while studying free amino acids, came across a compound whose migration on paper chromatograms did not correspond to any compound containing known amino acids. He drew attention to the presence of this substance in various tissues of the central nervous system: the brain, cerebellum and spinal cord of vertebrates and suggested a direct or indirect connection with the conduction of nerve signals.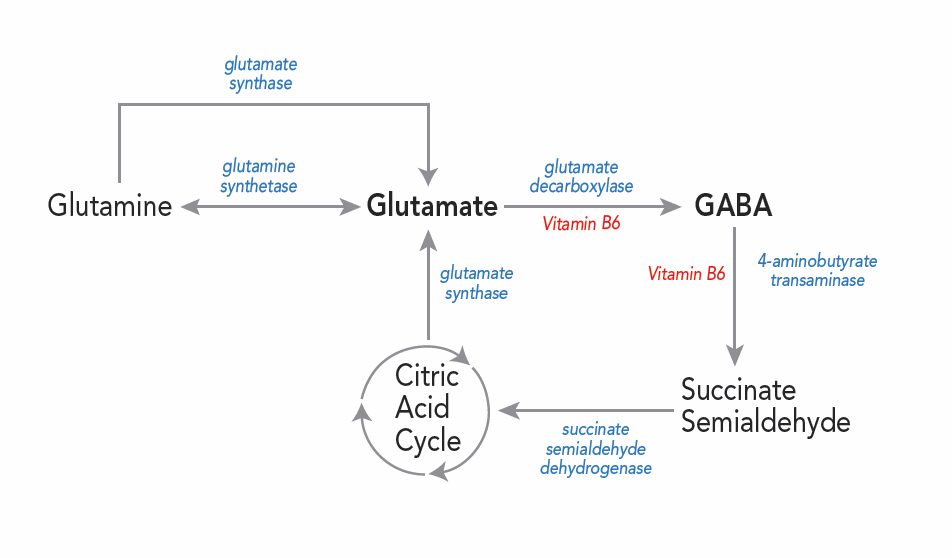 7 years later, researchers in Canada reported that the unknown compound with neuronal inhibitory activity was GABA. A number of subsequent discoveries have determined its role in our brain.
7 years later, researchers in Canada reported that the unknown compound with neuronal inhibitory activity was GABA. A number of subsequent discoveries have determined its role in our brain.
How does GABA work?
GABA is an amino acid that occurs as a result of processes occurring in different cells and, above all, in nerve cells. The "chemistry" of the brain is such that the main brake for the mediator - gamma-aminobutyric acid is a product of the main excitatory neurotransmitter - glutamate, which produces it under the action of the enzyme glutamate decarboxylase (GAD), and vitamin B6 acts as a cofactor. It all happens in a part of the brain called the hippocampus. Maintaining a balance between these two neurotransmitters is a key condition for physical and mental health, as well as good mood. A low level of GABA leads to the development of anxiety, depression, impairs concentration, attention, and some cognitive functions.
To understand the role of GABA, it is important to know how it interacts with its receptor.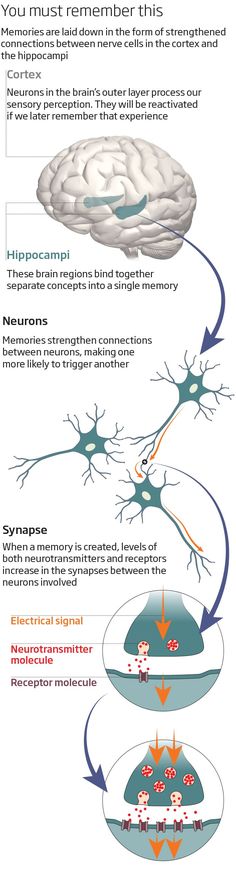 When GABA binds to the GABA receptor, the latter changes shape slightly, allowing ions to pass through its central channel. This leads to a decrease in the excitability of the neuron, which is why GABA is called an inhibitory neurotransmitter.
When GABA binds to the GABA receptor, the latter changes shape slightly, allowing ions to pass through its central channel. This leads to a decrease in the excitability of the neuron, which is why GABA is called an inhibitory neurotransmitter.
Getting into the brain from food, supplements or drugs, GABA becomes not just an additional inhibitory neurotransmitter, but also food for neurons, as it is captured by mitochondria. In neurons, it performs two tasks: about 1% of the substance works as a neurotransmitter, and 99% provides energy exchange in mitochondria during ATP synthesis and glucose breakdown. This substance stimulates metabolism, saturates the brain with oxygen and improves blood circulation throughout the body.
What are the benefits of GABA?
The main function of gamma-aminobutyric acid is to reduce the neural activity of the neurons to which it attaches. It prevents long-term activation of neurons and also plays a neurotrophic role by promoting the growth of certain neurons.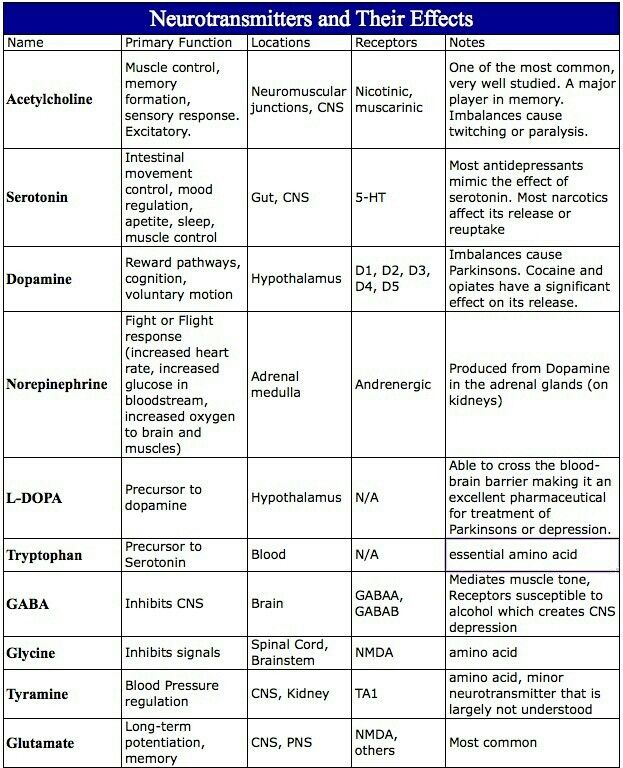
The main functions of the GABA:
- Regulation by motor activity
- Providing memory processes and thinking
- Anti -icing effect
- Activation of energy processes
- acceleration exchange.
The inhibitory effects of GABA serve to counteract the excitatory (activator) effects of glutamate. Indeed, when the brain is overexcited, it can contribute to feelings of restlessness, irritability, and even insomnia. Taking GABA helps to correct the imbalance associated with anxiety, has a relaxing and sedative effect. It is also associated with better sleep quality, allowing you to switch off, helping you fall asleep faster.
GABA plays a stabilizing role on a mental and physical level, helping to restore balance and maintain normal mood. This substance is involved in certain stages of memory and can be used to relax, control fear or anxiety, which manifests itself in overexcitation.
GABA has been scientifically proven to significantly stimulate growth hormone (HGH = Human Growth Hormone) secretion during the early stages of deep sleep.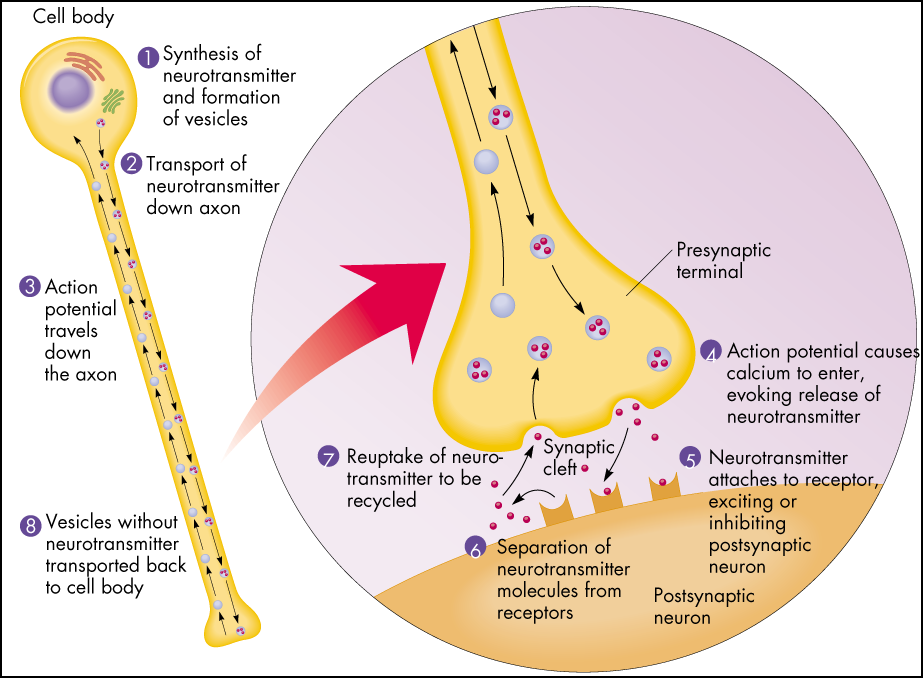 Growth hormone is one of the muscle growth hormones in the human body. It helps to reduce body fat and stimulates muscle growth. GABA acts on certain chains of neurons that stimulate the hypothalamus so that more growth hormones are released. This ability is highly valued by athletes.
Growth hormone is one of the muscle growth hormones in the human body. It helps to reduce body fat and stimulates muscle growth. GABA acts on certain chains of neurons that stimulate the hypothalamus so that more growth hormones are released. This ability is highly valued by athletes.
Based on GABA, nootropics are produced - drugs that improve the higher functions of the human brain. They are widely used in the treatment of strokes, brain injuries, age-related changes, when the performance of the brain is significantly reduced. The advantages of nootropics over other drugs that affect synaptic activity are that they do not cause addiction and dependence, unlike psychomotor stimulants and antipsychotics. And because GABA is an inhibitory neurotransmitter, it is widely used in the treatment of epilepsy.
Thus, tableted gamma-aminobutyric acid contributes to the overall strengthening of the nervous system, in particular, such brain functions as thinking, perception and attention.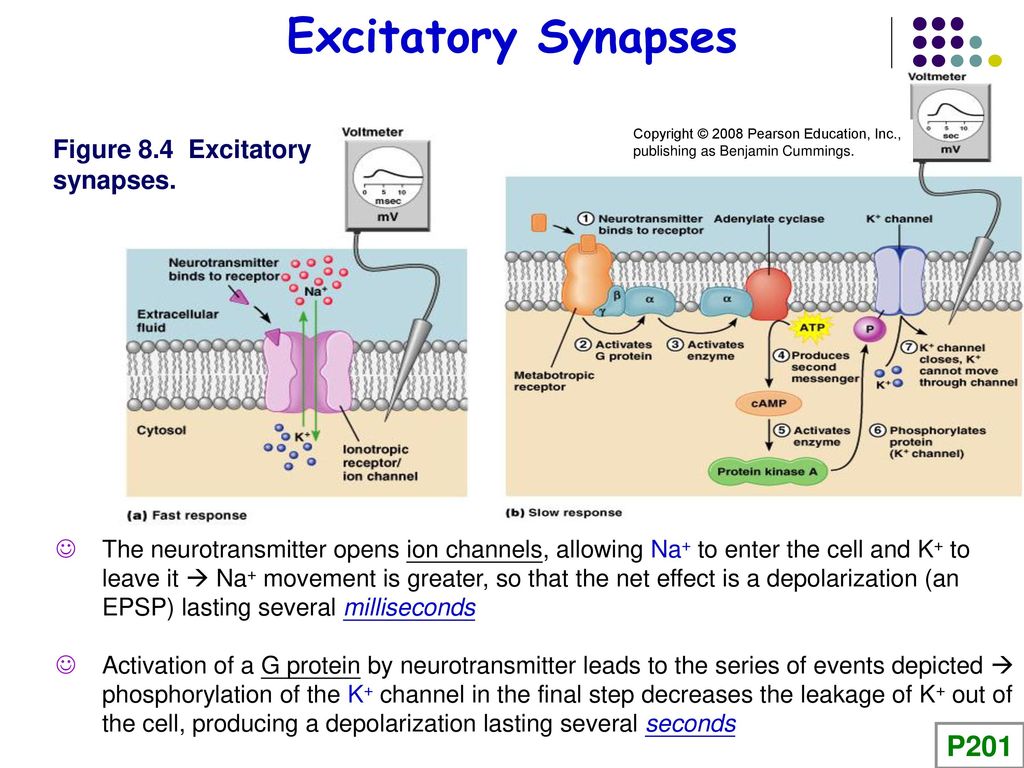
GABA receptors are located, among other things, in the hypothalamus, which controls circadian rhythms and is directly related to sleep. Many insomnia medications, as well as their herbal counterparts, raise GABA levels, thereby improving the quality of sleep.
What are the benefits of GABA?
Thanks to numerous studies, today GABA is officially recognized as an effective cytoprotective antihypoxant and antioxidant for various organs and systems. She is credited with antitumor and anti-inflammatory properties, as well as the ability to positively influence the functioning of the immune system.
The effect of GABA on sleep is especially noticeable. Under its influence, mental excitation decreases, the energy processes of the brain are activated, the respiratory activity of tissues and glucose utilization improve, which leads to high-quality deep sleep.
Gaba action on the body:
- Helps to calm and relax
- controls “panic” states associated with anxiety
- reduces muscle tone
- reduces
- .

- normalizes blood pressure
- helps control anxiety
- promotes quality sleep
- reduces blood sugar levels
- improves overall immunity
- accelerates the recovery process after injuries
- improves sexual activity
GABA preparations are used to treat mental retardation, cerebral palsy, post-stroke conditions, and also restore brain function after injuries. Taking GABA supplements is appropriate for high mental, physical and psychological stress. They help to normalize the work of the brain, cope with stress.
GABA for athletes
Many professional athletes today recognize the benefits of GABA for athletic performance. The advantage of sports nutrition based on it is high efficiency in the absence of a hormonal component. Acting on the anterior pituitary gland of the brain, GABA stimulates the production of growth hormone, which increases the growth of muscle tissue and reduces the percentage of body fat. This is especially important for bodybuilders and athletes.
This is especially important for bodybuilders and athletes.
The advantages of a margin for athletes:
➦ Increases the growth of the growth hormone by 4-6 times, being a safe alternative to steroids
➦ stimulates the production of somatotropin even after training
➦ participates in the process of fat burning, contributing to a faster
➦ helps to quickly achieve a beautiful relief body
➦ normalizes the functioning of the nervous system
➦ eliminates insomnia, improves sleep
➦ accelerates recovery after injuries: dislocations and sprains.
GABA supplements are consistently in high demand among professional athletes and amateurs, which is the best confirmation of their high effectiveness. Single negative reviews are associated with the incorrect use of drugs with GAB or a violation of the training process.
It is important to remember that all dietary and sports supplements are taken in a certain dosage, courses, after consultation with a doctor.
Gamma aminobutyric acid (GABA) deficiency symptoms
GABA is synthesized naturally by the body. When its level in the body is sufficient, we experience peace and well-being. With a deficiency of GABA, there is an imbalance between the processes of excitation and inhibition, which leads to disturbances in the functioning of the nervous system: from increased anxiety and irritability to insomnia. Low levels of this neurotransmitter cause difficulty falling asleep despite being tired, as well as restlessness, recurring muscle or neuropathic pain, and a tendency to be irritable. In children, this manifests itself in the form of hyperactivity, attention deficit disorder, problems with perseverance and attention.
Here are some of the symptoms indicating a marriage deficiency:
✔ Nervousness and inability to concentrate
✔ periodically occurring tremor
✔ Frequent difficulties with breathing
✔ Strong sweating
✔ Fatigue even after a good night dream
✔ mood swings
✔ mental confusion
The most severe case, which is associated with a lack of γ-aminobutyric acid, is epilepsy. This neurological disease is caused by the fact that as a result of malformations or brain tumors, a huge wave of excitation periodically occurs in some of its areas (most often in the local area), which leads to an epileptic seizure. Using preparations containing GABA, it is possible to enhance the work of the GABA system by suppressing the activity of the excitatory neurotransmitter.
This neurological disease is caused by the fact that as a result of malformations or brain tumors, a huge wave of excitation periodically occurs in some of its areas (most often in the local area), which leads to an epileptic seizure. Using preparations containing GABA, it is possible to enhance the work of the GABA system by suppressing the activity of the excitatory neurotransmitter.
Deficiency cases for which GABA is recommended:
✔ Trouble falling asleep due to nervousness and anxiety
✔ Inability to relax
✔ Constant feeling of physical tension
✔ Mood and behavior disorder
How to increase the level of Gamk?
In a healthy body with a balanced diet and a proper lifestyle, the production of gamma-aminobutyric acid is regulated independently, but bad habits, stress and certain diseases can provoke its deficiency. GABA is naturally present in plants, but it is primarily synthesized endogenously by our bodies from glutamic acid.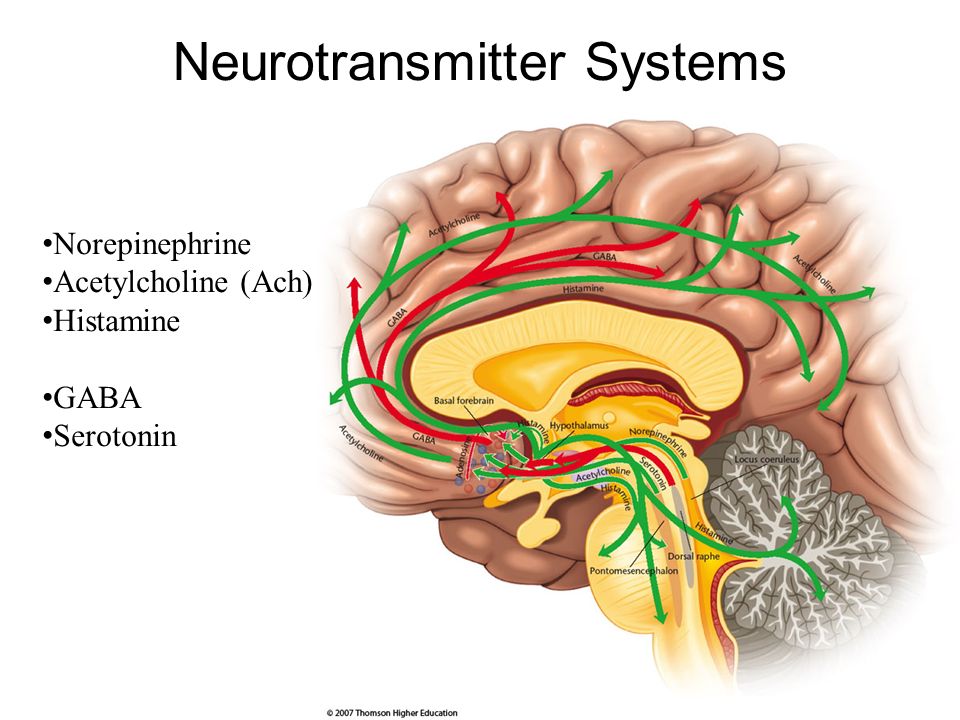
Restore the GABA balance in the body will help the consumption of food or special supplements containing gamma-aminobutyric acid, as well as glutamine, since GABA is its derivative. This substance is found in animal proteins: eggs, white meat, legumes such as lentils or chickpeas, leafy vegetables such as spinach and parsley. And to turn it into GABA, it is important to take supplements with vitamin B6 and magnesium.
Some plant extracts may also interfere with GABA production. For example, lemon balm is a transaminase inhibitor, and consuming it increases GABA levels in the brain, as it will be less degraded. GABA stimulants include: inositol, glutamic acid, melatonin (at night), thiamine (vitamin B1), niacinamide (vitamin B3), pyridoxine, valerian, passionflower 200–1000 mg.
| Connection name | What does it contain |
| Inositol, a sugar normally synthesized by the body | fruits, vegetables, legumes, seeds, oilseeds |
| Branched-chain amino acids (leucine) | turkey meat, spirulina, beans, pistachios, whey |
| Isoleucine | nuts of all kinds, seeds, lentils, rye, eggs, chicken |
| Valine | peanuts, mushrooms, soybeans, lupins, parmesan, all kinds of seeds |
| Arginine | pumpkin seeds and peanuts |
| Coenzyme Q10 | spinach, broccoli and cauliflower |
| Ribose | mushrooms |
| vitamin C | Brussels sprouts, bell peppers and citrus fruits |
| All B vitamins, including B6. | nuts (especially walnuts), tomatoes, potatoes, cabbage, cereals, citrus fruits, berries |
The following measures will help to stimulate the production of GABA:
+ good rest
+ breathing techniques to reduce stress
+ meditation practices
+ physical activity
What is GABA?
GABA is found naturally in foods such as chestnuts, potatoes, rice, astragalus, fresh leaves of selected teas from which natural GABA extracts are obtained.
It is also found in medications and supplements for anxiety, anxiety, blood pressure and sleep, and sports nutrition for athletes and bodybuilders.
Studies have shown that with long-term use of products and preparations with gamma-aminobutyric acid, it is possible to raise its level in the body to the optimum.
The most popular GABA supplements in Phytomarket
More items in Vitamins for the nervous system!
GABA in food
Foods rich in gamma-aminobutyric acid include:
| Food | Quantitative content of GABA per 100 g |
| Gaba tea | 150-400 mg |
| Tomatoes (depending on variety), sauerkraut, fermented soybeans | to 63 mg |
| Germinated rice, especially anoxic fermented in nitrogen | 25. |
| Eggplant | 20 mg |
| Potato | 16 to 35 mg |
| Grapefruits | 23 mg |
| Peaches | 13 mg |
| Kiwi | 11 mg |
| Oranges | 11.5 mg |
| Carrot | 10 mg |
| Shiitake mushrooms | 8 mg |
| Green soybeans | 6 mg |
| Beets | 4 to 8 mg |
Based on this table, we can conclude that the most complete natural source of GABA is Gaba tea.
Gaba tea as a source of acid
Gaba Tea is a unique product produced in the north of Taiwan. Now he is at the peak of popularity. Due to its richness in GABA molecules, it has a large list of benefits for human health. Among them: support for memory, relaxation, fighting stress and depression, building muscle mass and delaying aging. Studies have shown that regular consumption of Gaba tea helps reduce blood pressure, boost immunity, and improve sexual function.
Now he is at the peak of popularity. Due to its richness in GABA molecules, it has a large list of benefits for human health. Among them: support for memory, relaxation, fighting stress and depression, building muscle mass and delaying aging. Studies have shown that regular consumption of Gaba tea helps reduce blood pressure, boost immunity, and improve sexual function.
Gaba is not a type of tea, but a special oxygen-free fermentation technology that releases gamma-aminobutyric acid. The origins of this unusual drink are the Japanese. In the late 1980s, a team at the National Tea Experiment Station, led by Dr. Tsushima Tojiro, experimentally determined that fresh tea leaves release large amounts of GABA during fermentation in the absence of oxygen.
It is believed that unlike synthetic GABA, which hardly crosses the protective blood-brain barrier to access the brain, the gamma-aminobutyric acid contained in the natural tea leaf is absorbed much better.
Today, Taiwan is the world's largest producer and supplier of Gaba tea. The delicious taste, as well as the extraordinary health benefits, have earned Taiwanese Gaba tea a prominent place in catalogs of exceptional teas.
The delicious taste, as well as the extraordinary health benefits, have earned Taiwanese Gaba tea a prominent place in catalogs of exceptional teas.
How much Gamma in tea?
The largest plant source of GABA is the Taiwanese version of Oolong tea. 100 g of the product contains 150-400 mg of gamma-aminobutyric acid.
How is Gaba tea made?
High quality fresh leaves are used in the production, which are placed under vacuum in sealed bags and kept at a temperature of at least 40 ˚C for about 8 hours. Then they are taken out into the air and shaken thoroughly for several minutes. This cycle is repeated 5 times with slight variations in air exposure time between vacuum steps. This anaerobic reaction develops the natural potential of gamma-aminobutyric acid in the leaves, and also provides a rich fruity taste of tea: baked apple with hints of cinnamon and nutmeg.
How to brew Gaba tea?
To make Gaba tea not only healthy, but also tasty, you need to brew it properly.
Proceed as follows :
- Boil water
- Preheat the kettle with hot water
- Put 7 grams of tea (approximately 1.5-2 tablespoons), fill with hot water and immediately drain (rinsing tea) 906 6 again and wait about 10 seconds
- Repeat the previous step several times, increasing the steeping time by 10-20 seconds.
How to take for sleep?
As a remedy for insomnia, Gaba tea is best consumed at least 2-3 hours before bedtime.
How to take GABA supplement
The positive effect of GABA intake is observed when taking at least 2g / day after about a week. It is recommended to start with 0.5 g - 1 g per day, gradually increasing the dose to 4 g. Small doses of the supplement do not work, since only a small part of the substance penetrates the brain.
It is best to take a GABA supplement before bed or after a workout on an empty stomach with water or juice, but not in the morning, as this may affect performance. The course is at least 1 month. A break while taking GABA is not regulated.
The course is at least 1 month. A break while taking GABA is not regulated.
It is desirable to combine the use of GABA with the intake of vitamin B6. In case of its shortage, sleep disturbance, nervousness and other unpleasant symptoms may occur. In addition to B6, GABA can be taken along with 5-HTP, as well as magnesium and zinc, which are responsible for activating GABA receptors.
Side effects of GABA
GABA has very few side effects. In very rare cases, tingling on the skin may be felt, even less often: nausea, vomiting, insomnia, fluctuations in blood pressure (during the first days of treatment), dyspepsia, hyperthermia, a feeling of heat. Such side effects may be associated with individual intolerance.
On the other hand, the simultaneous use of GABA and anxiolytics may be associated with an increased risk of sedation, so it is important to consult a doctor in advance.
Overdose of drugs that inhibit GABA reuptake can cause an excess of GABA, which is manifested by neurological and psychiatric symptoms: memory loss, convulsions, hallucinations and cognitive impairment.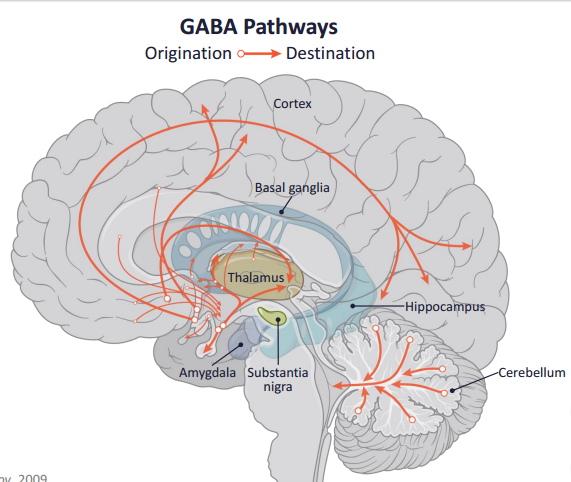
Contraindications to the use of GABA drugs are hypersensitivity, children under 1 year of age, acute renal failure, pregnancy and lactation.
Answers to popular questions:
When is the best time to drink GABA?
Best GABA supplement to take before bed or after workout
How much GABA to take?
It is recommended to start with 0.5 g - 1 g per day, gradually increasing the dose to 4 g. For a noticeable effect, take the supplement for at least 1 month. Break while taking GABA is not regulated
Where are GABA receptors located?
Neurons carrying receptors for GABA molecules can be found in almost any area of the brain.
How long will it take to see a noticeable result?
Noticeable improvement can be seen as early as a week after taking a GABA supplement.
Brewer's yeast: real benefit or harm? Isotonic for athletes and not only. Everything you need to know about drink
Everything you need to know about drink
As calm as GABA
Gamma-aminobutyric acid (GABA) is the main inhibitory mediator in the human nervous system. But only those of us who have already developed it. And in order to provide us with truly Olympian calm, a motley company of very famous substances sometimes helps her. We will take a closer look at GABA and learn that this molecule is not as simple as it seems at first glance.
Resting neurotransmitter
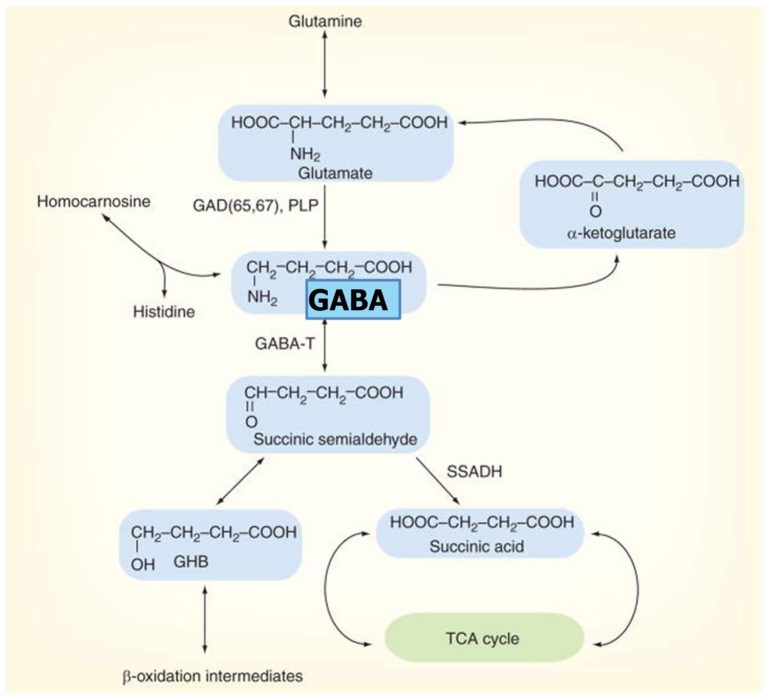
Gamma-aminobutyric acid (GABA; γ-aminobutyric acid, GABA) is synthesized in the brain from glutamic acid, another neurotransmitter, by its decarboxylation (removal of the carboxyl group from the main chain) (Fig. 1). According to the chemical classification, GABA is an amino acid, but not a habitual one, that is, an α-amino acid used for the synthesis of protein molecules, where the amino group is attached to the first carbon atom in the chain. In GABA, the amino group is linked to the third atom from the carboxyl group (in glutamate, it was the first one before decarboxylation).
Figure 1. Synthesis of GABA. Using the enzyme glutamate decarboxylase (GAD) , another neurotransmitter, GABA, is obtained from the neurotransmitter glutamate.
Behavioral and Structural Anatomy Web Atlas Caenorhabditis elegans
GABA is synthesized directly in the brain and binds to two types of receptors on the surface of neurons, GABA receptor types A and B. are found mainly in the retina of the eye), but were subsequently combined due to the commonality of action. This type of receptor is ionotropic : when GABA binds to them, an ion channel opens in the nerve cell membrane, and chloride ions rush into the cell, reducing its reactivity. The nerve cell membrane has a resting potential of [1]. There are fewer charged ions inside the cell than outside, and this creates a charge difference. Outside, superiority is created by chlorine, calcium and sodium, and inside potassium ions and a number of negatively charged organic molecules predominate. In a theoretical sense, the membrane potential has two paths: an increase (called depolarization ) and decrease ( hyperpolarization ) (Fig. 2). At rest, the membrane potential is approximately -70...-90 mV (millivolts), and during the work of the nervous system, a "tug of war" begins between two forces that excite the cell (depolarize the membrane) and inhibit it (hyperpolarizing).
In a theoretical sense, the membrane potential has two paths: an increase (called depolarization ) and decrease ( hyperpolarization ) (Fig. 2). At rest, the membrane potential is approximately -70...-90 mV (millivolts), and during the work of the nervous system, a "tug of war" begins between two forces that excite the cell (depolarize the membrane) and inhibit it (hyperpolarizing).
Figure 2. Scheme of the occurrence of an action potential on the cell membrane. It is necessary to change the content of ions inside and outside the cell of such strength that the value of the charge on the membrane changes and reaches a certain threshold. If this happens, then the membrane continues to depolarize further, the neuron is excited and transmits a signal to other cells. Overshoot (inversion) - the period when the membrane potential is positive. Then the repolarization phase follows, and the membrane charge returns to its previous values.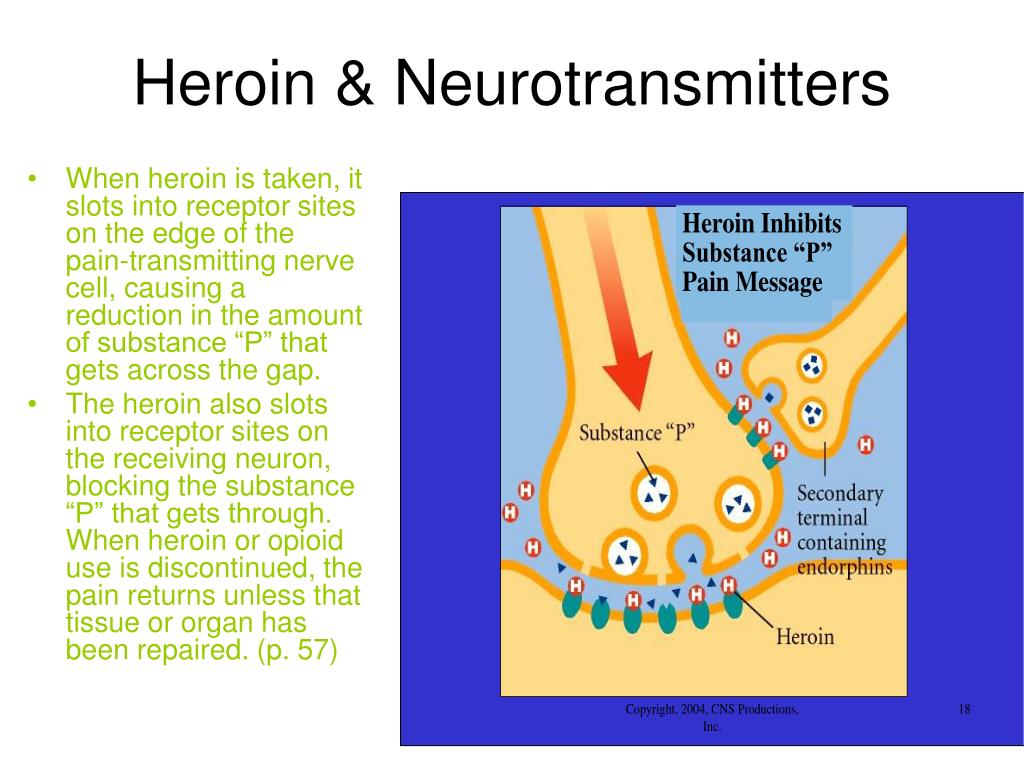
Wikipedia
To understand how this works, two points must be taken into account. The first is that several oppositely directed forces can act on one neuron at the same time: for example, five excitatory and three inhibitory neurons converge on one cell in this part of the nervous system. At the same time, they can affect the dendrite of this neuron and the axon in the presynaptic part. The second point is that a nerve cell experiencing these effects will work according to the “all or nothing” principle. It cannot send a signal and not send it at the same time. All the effects of the signals that came to the cell are summed up, and if the resulting changes in the membrane potential exceed a certain value (called excitation threshold ), then the signal will be transmitted to another cell through the synapse. If the threshold value is not reached, then sorry - try again guys. All this is reminiscent of Krylov's fable about the swan, cancer and pike: each pulls in its own direction, but it is not very clear what will come of it.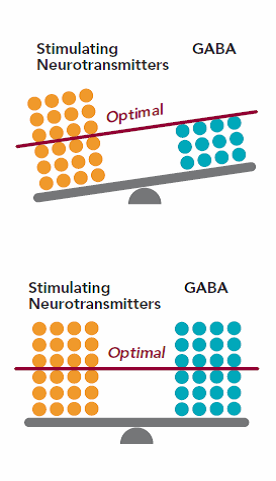
So, the GABA molecule has bound to the ion channel receptor. The ion channel, which has a rather complex structure (Fig. 3), opens and begins to let negatively charged chloride ions into the cell. Under the influence of these ions, the membrane hyperpolarizes, and the cell becomes less susceptible to excitatory signals from other neurons. This is the first and, perhaps, the main function of GABA - inhibition of the activity of nerve cells in the nervous system .
Figure 3. Ionotropic GABA receptor. GABA receptor A - heteropentamer: consists of 5 protein subunits, which, depending on the homology of amino acid sequences, can belong to eight different families (more often - to α, β, γ; members of the ρ-family are homooligomerized - GABA receptors are obtained A -ρ, "former" GABA C ). This determines the diversity of GABA A receptors. a - Scheme of the structure of the receptor.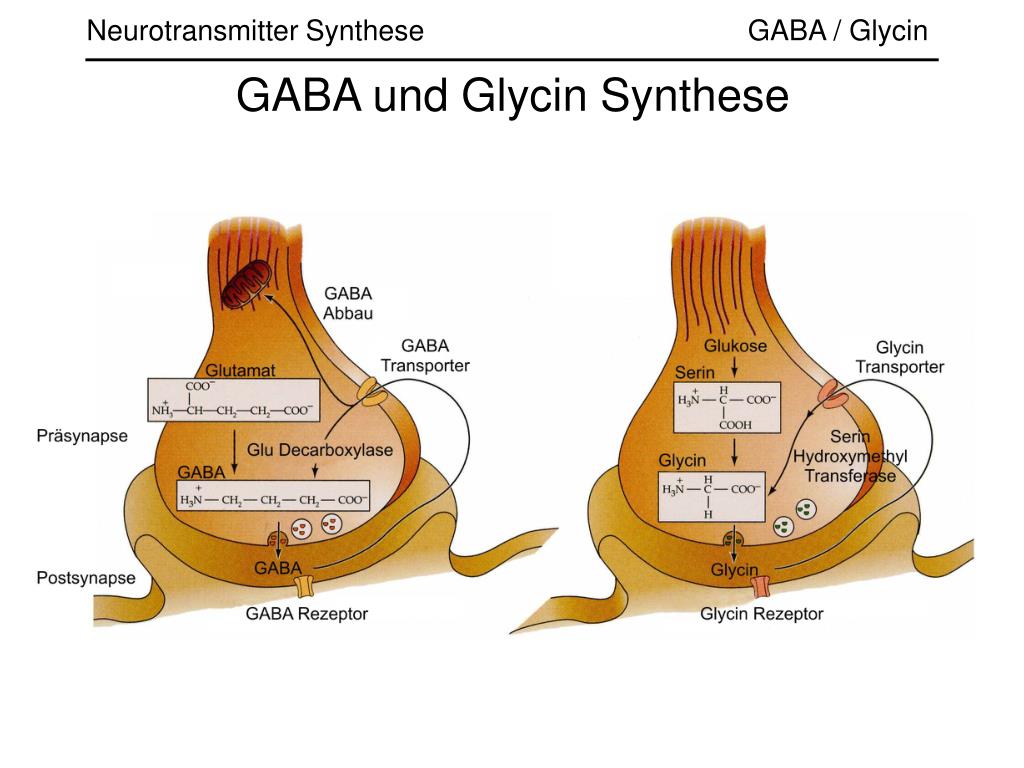 Left: Each of the subunits at the long globular N-terminus exposed to the surface of the neuron has a characteristic "cysteine loop" structure and binding sites for GABA and other ligands. This is followed by 4 α-helical transmembrane domains (between the last of them there is a large cytoplasmic loop responsible for binding to the cytoskeleton and "internal" modulators) and a short C-terminus. Right: Five subunits form an ion channel guided by the second transmembrane domain ( orange cylinder ) to each other. This is the quaternary structure of the receptor. When binding to two GABA molecules, the receptor changes its conformation, opening a pore for anion transport. b - Photomicrograph of the GABA receptor in the porcine brain.
Left: Each of the subunits at the long globular N-terminus exposed to the surface of the neuron has a characteristic "cysteine loop" structure and binding sites for GABA and other ligands. This is followed by 4 α-helical transmembrane domains (between the last of them there is a large cytoplasmic loop responsible for binding to the cytoskeleton and "internal" modulators) and a short C-terminus. Right: Five subunits form an ion channel guided by the second transmembrane domain ( orange cylinder ) to each other. This is the quaternary structure of the receptor. When binding to two GABA molecules, the receptor changes its conformation, opening a pore for anion transport. b - Photomicrograph of the GABA receptor in the porcine brain.
a - from Wikipedia, b - from the article [4]
Type B receptors are metabotropic , that is, they affect the metabolism in the cell.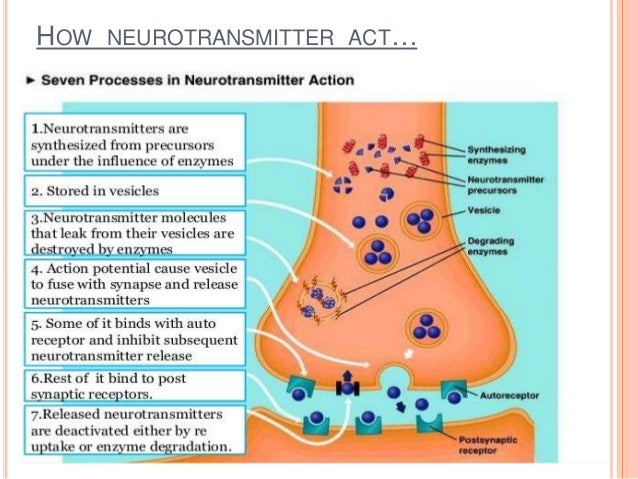 They also reduce the level of excitation in the cell, but they do it in slower ways, through the G-protein system. Receptors of this type help the cell to reduce sensitivity to excitatory influences through the effect on calcium and potassium channels.
They also reduce the level of excitation in the cell, but they do it in slower ways, through the G-protein system. Receptors of this type help the cell to reduce sensitivity to excitatory influences through the effect on calcium and potassium channels.
Seizures and anxiety
The structure of the GABAergic system of the brain resembles all the others (Fig. 4). There are a number of structures deep in the brain from where GABA-releasing nerve fibers travel to other parts of the nervous system. Therefore, GABA is an inhibitory neurotransmitter that regulates many processes, from muscle tone to emotional reactions.
Figure 4. GABAergic pathways in the human brain. Accumulations of nerve cells in the depths of the brain send out their processes to different parts of the nervous system in order to reduce excessive levels of excitation.
website www.cnsforum.com
However, GABA becomes an inhibitory neurotransmitter only in the mature brain. In the developing nervous system, GABAergic neurons can produce an excitatory effect on cells, also changing the membrane permeability to chloride ions [2]. In immature nerve cells, the concentration of chloride ions is higher than in the environment, and stimulation of GABA receptors leads to the release of these anions from the cell and subsequent depolarization of the membrane. Over time, the main excitatory system of the brain matures - glutamate , - and GABA acquires the role of an inhibitory (hyperpolarizing membrane) neurotransmitter.
In the developing nervous system, GABAergic neurons can produce an excitatory effect on cells, also changing the membrane permeability to chloride ions [2]. In immature nerve cells, the concentration of chloride ions is higher than in the environment, and stimulation of GABA receptors leads to the release of these anions from the cell and subsequent depolarization of the membrane. Over time, the main excitatory system of the brain matures - glutamate , - and GABA acquires the role of an inhibitory (hyperpolarizing membrane) neurotransmitter.
Brain maturation itself is a complex process that is regulated by many genes at different stages of ontogeny (Fig. 5). Violation of the processes of maturation and migration of neurons leads to various neurological diseases, for example, epilepsy [3]. Epilepsy is one of the most common neurological diseases. With it, brain neurons do not generate nerve impulses as they should - too often and too strongly, which leads to the appearance of a pathological focus of excitation in the brain.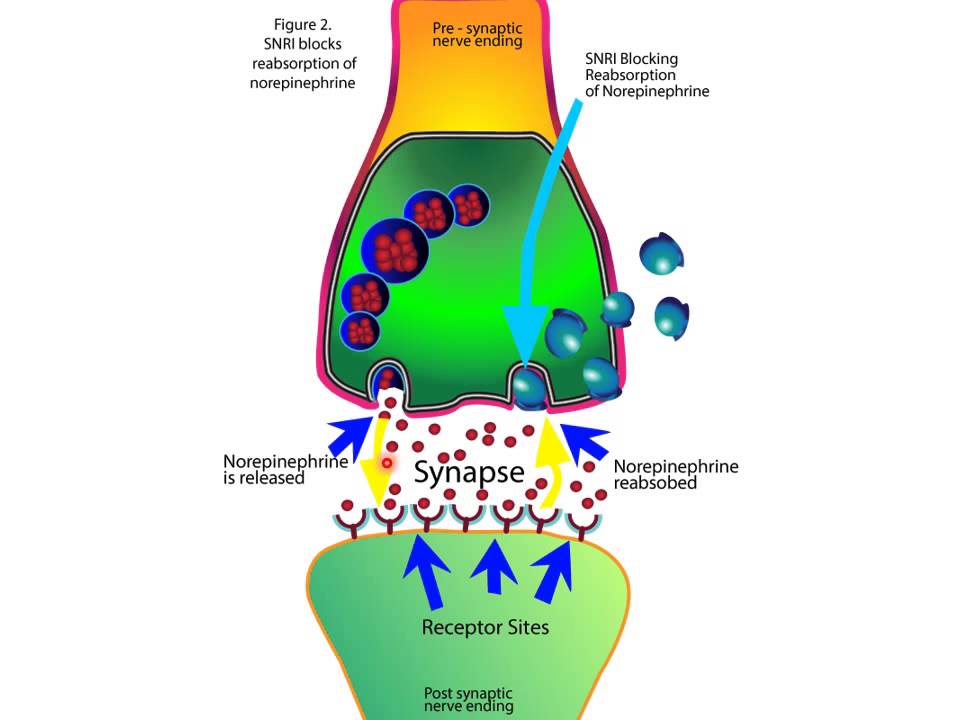 It is the existence of such a focus that leads to seizures - the most important and dangerous symptom of epilepsy. Such a "discharge" allows you to temporarily reduce excitation in the nervous system. Mutations in a number of genes lead to the fact that GABAergic interneurons are out of place and cannot fully perform their inhibitory functions. In mouse models and in the study of the human genotype, a relationship has been established between mutations, impaired migration and maturation of GABAergic neurons, and the development of epilepsy.
It is the existence of such a focus that leads to seizures - the most important and dangerous symptom of epilepsy. Such a "discharge" allows you to temporarily reduce excitation in the nervous system. Mutations in a number of genes lead to the fact that GABAergic interneurons are out of place and cannot fully perform their inhibitory functions. In mouse models and in the study of the human genotype, a relationship has been established between mutations, impaired migration and maturation of GABAergic neurons, and the development of epilepsy.
Figure 5. Genes responsible for brain maturation are activated at different stages of ontogeny. The embryonic and postnatal periods are separated by a point P0 (birth). The DLX, ARX, DCX, RELN genes are responsible for the growth, maturation and function of inhibitory cells. The DLX (distal-less homeobox) gene family encodes homeodomain-containing transcription factors. Most are expressed during the formation of sensory organs and migration of ridge cells and interneurons; regulate gene expression ARX. ARX (aristaless-related homeobox) encodes a homeodomain-containing transcription factor that controls cell differentiation in various organs. In the developing brain, it is necessary for the migration of interneurons. DCX (doublecortin) encodes doublecortin (lissencephalin-X), a microtubule-associated protein synthesized in immature neurons during their division (a marker of neurogenesis, including in adults). It is necessary for the correct migration and differentiation of neuroblasts, since it affects the dynamics of cytoskeletal microtubules (stabilizes and groups them). RELN (reelin) - secreted signal glycoprotein gene reelin . With the development of the nervous system, the fibers of the radial glia are oriented in the direction of a higher concentration of reelin, building "paths" for the migration of neurons. This protein is also necessary for the correct construction of the layers of the cortex.
ARX (aristaless-related homeobox) encodes a homeodomain-containing transcription factor that controls cell differentiation in various organs. In the developing brain, it is necessary for the migration of interneurons. DCX (doublecortin) encodes doublecortin (lissencephalin-X), a microtubule-associated protein synthesized in immature neurons during their division (a marker of neurogenesis, including in adults). It is necessary for the correct migration and differentiation of neuroblasts, since it affects the dynamics of cytoskeletal microtubules (stabilizes and groups them). RELN (reelin) - secreted signal glycoprotein gene reelin . With the development of the nervous system, the fibers of the radial glia are oriented in the direction of a higher concentration of reelin, building "paths" for the migration of neurons. This protein is also necessary for the correct construction of the layers of the cortex.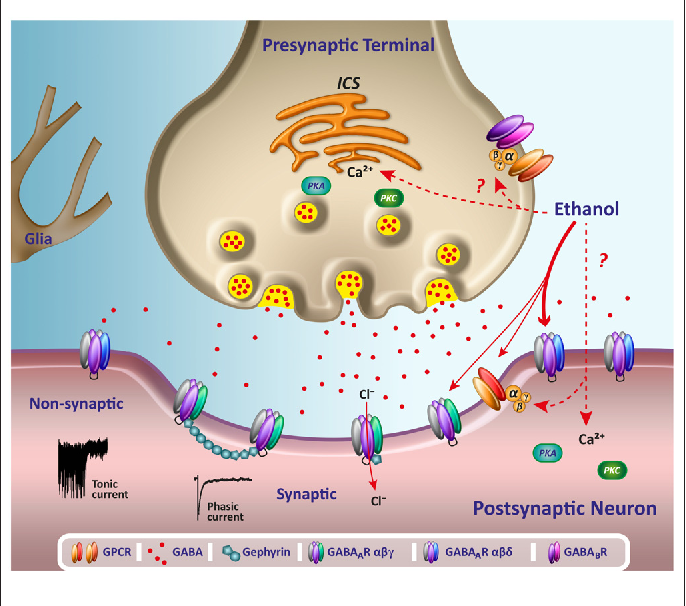 RELN is also active in other tissues, even in adults. In the developed brain, reelin is secreted by GABAergic interneurons in the hippocampus and cortex. It probably stimulates the elongation of neuronal processes, affects synaptic plasticity and memory [7].
RELN is also active in other tissues, even in adults. In the developed brain, reelin is secreted by GABAergic interneurons in the hippocampus and cortex. It probably stimulates the elongation of neuronal processes, affects synaptic plasticity and memory [7].
Another aspect of the inhibitory effect of GABA is its effect on emotional processes, in particular on anxiety. Anxiety is a very broad concept. It contains both perfectly healthy human reactions to stressful influences (an exam, a dark gateway, a declaration of love), and pathological conditions (anxiety disorders in the medical sense of the word). Based on the provisions of modern psychiatric science, we can say that there are normal anxiety and anxiety as a disease . Anxiety becomes a disease when it interferes with your daily or professional life, blocking you from making any decisions - even the most necessary ones.
The part of the brain that is responsible for emotional reactions is the amygdala - the accumulation of nerve cells in the depths of our head. It is one of the most ancient and important parts of the nervous system in animals. The specialty of the amygdala is negative emotions—we get angry, angry, fearful, and anxious through the amygdala. GABA allows the brain to reduce the intensity of these experiences.
It is one of the most ancient and important parts of the nervous system in animals. The specialty of the amygdala is negative emotions—we get angry, angry, fearful, and anxious through the amygdala. GABA allows the brain to reduce the intensity of these experiences.
Nerve pill
Drugs that are effective in combating anxiety and seizures must bind to the GABA receptor. They are not direct receptor stimulants, i.e. do not bind to the same part of the molecule as GABA. Their role is that they increase the sensitivity of the ion channel to GABA, slightly changing its spatial organization. Such chemicals are called allosteric modulators . Allosteric modulators of GABA receptors include ethanol, benzodiazepines, and barbiturates.
Figure 6. Barbituric acid molecule.
Wikipedia
Alcohol is known for its relaxing and anti-anxiety effects. Solutions of ethyl alcohol in various concentrations have long been widely used by the population of the Earth to calm the nerves. Ethanol gives people relaxation by binding to the GABA receptor and facilitating its further interaction with the mediator. It happens that people overestimate their ability to drink alcohol, and this leads to a gradual loss of control over their actions and an increase in lethargy. Alcoholic hyperrelaxation sets in, which, with continued use, can reach an alcoholic coma - the inhibitory effect of alcohol on the central nervous system is so strong. Potentially, alcohol could be used during surgical operations as an anesthetic (previously, in critical situations - for example, at the front - this was done - Rev. ), but the range of concentrations where it turns off pain sensitivity and still does not “turn off” a person completely is too small.
Ethanol gives people relaxation by binding to the GABA receptor and facilitating its further interaction with the mediator. It happens that people overestimate their ability to drink alcohol, and this leads to a gradual loss of control over their actions and an increase in lethargy. Alcoholic hyperrelaxation sets in, which, with continued use, can reach an alcoholic coma - the inhibitory effect of alcohol on the central nervous system is so strong. Potentially, alcohol could be used during surgical operations as an anesthetic (previously, in critical situations - for example, at the front - this was done - Rev. ), but the range of concentrations where it turns off pain sensitivity and still does not “turn off” a person completely is too small.
Figure 7. Veronal box by Bayer (upper left corner).
photo by the author, taken at the Museum of Pharmacy (Riga, Latvia)
Another class of substances - barbiturates - is now used in neurology to treat epileptic seizures. All drugs of this class are allosteric modulators, derivatives of barbituric acid - barbital (Fig. 6). Barbital itself was sold by a well-known firm Bayer under the trade name "Veronal" (Fig. 7). Subsequently, other derivatives of barbituric acid were synthesized: phenobarbital ("Luminal") and benzobarbital. These drugs, which appeared at the beginning of the 20th century, became the first effective and relatively safe medicine to combat epilepsy. Barbituric acid derivatives have also been used to combat sleep disorders, but in smaller doses.
All drugs of this class are allosteric modulators, derivatives of barbituric acid - barbital (Fig. 6). Barbital itself was sold by a well-known firm Bayer under the trade name "Veronal" (Fig. 7). Subsequently, other derivatives of barbituric acid were synthesized: phenobarbital ("Luminal") and benzobarbital. These drugs, which appeared at the beginning of the 20th century, became the first effective and relatively safe medicine to combat epilepsy. Barbituric acid derivatives have also been used to combat sleep disorders, but in smaller doses.
Another group of drugs that enhance the effect of GABA on cells are benzodiazepines . Like the previous substances, benzodiazepines bind to the GABA type A receptor (Fig. 8). On one of the subunits of the ion channel there is a special place where the benzodiazepine is attached. All drugs in this class have sedative (sedative), anti-anxiety and anticonvulsant effects. Now psychiatrists and neurologists consider it bad form to treat anxiety and insomnia in patients with long courses of benzodiazepines, and even more so to prescribe them on a permanent basis.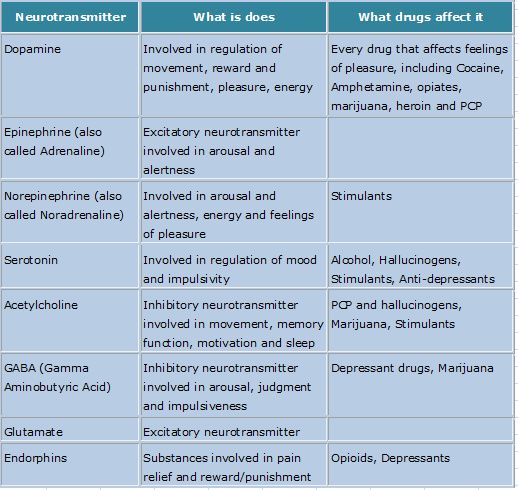 Dependence is quickly developed to these drugs, and withdrawal leads to persistent sleep disturbances and the resumption of anxiety. For these reasons, it is recommended to prescribe benzodiazepines in short courses - for several days. To treat anxiety, doctors currently use antidepressants and other drugs, such as etifoxine [4].
Dependence is quickly developed to these drugs, and withdrawal leads to persistent sleep disturbances and the resumption of anxiety. For these reasons, it is recommended to prescribe benzodiazepines in short courses - for several days. To treat anxiety, doctors currently use antidepressants and other drugs, such as etifoxine [4].
This and other groups of drugs used in the complex treatment of not anxiety, but depression are described in the “juicy” review “ A Brief History of Antidepressants ”: with all the ins and outs of this condition, with theories / hypotheses and doubts about them [5 ]. — Ed.
Figure 8. GABA receptor A and drug binding sites. The most common combination of subunits in the CNS (about 40% GABA A receptors) - two α1, two β2 and one γ2s located around the chloride pore ( top view ). GABA site (on the surface, junction of α and β) - the place where GABA attaches to the receptor; BDZ site (on the surface, α and γ junction) - benzodiazepine binding site, ETF site (on β) - etifoxine, NS site (in the channel) - neurosteroids.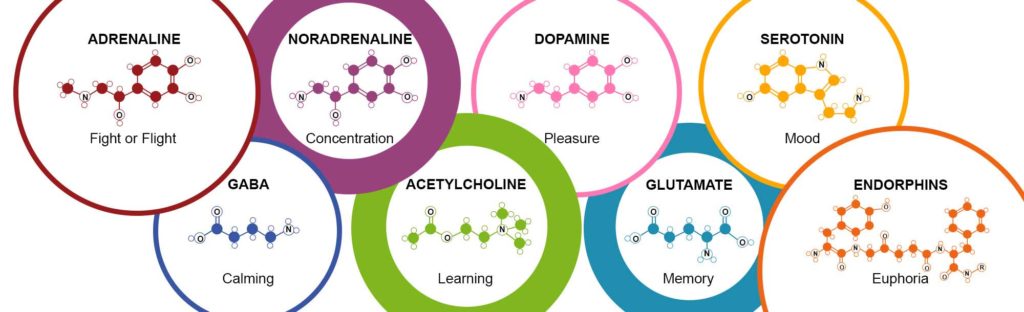 The binding sites for barbiturates and ethanol are presumably located in the depth of the channel (on the transmembrane domains). In the first case, the β-subunit probably plays the main role, while different subunits, including ρ and δ, interact with ethanol, but their sensitivity differs.
The binding sites for barbiturates and ethanol are presumably located in the depth of the channel (on the transmembrane domains). In the first case, the β-subunit probably plays the main role, while different subunits, including ρ and δ, interact with ethanol, but their sensitivity differs.
The reason for the dislike of benzodiazepines lies in their side effects, which are quite a lot, and not all of them are taken into account by official structures [6]. First, benzodiazepines, like all GABAergic drugs, are highly addictive. Secondly, benzodiazepines impair a person's memory. The use of this group of drugs enhances the inhibitory effect of GABA on the cells of the hippocampus - the memory center. This can lead to difficulties in remembering new information, which is observed against the background of taking benzodiazepines, especially in older people.
GABA, despite its narrow "specialty", is an amazing neurotransmitter. In the developing brain, γ-aminobutyric acid excites nerve cells, while in the developed one, on the contrary, it reduces their activity.

 9 mg
9 mg