Lithium for ocd
Management of obsessive-compulsive disorder comorbid with bipolar disorder
1. Chen YW, Dilsaver SC. Comorbidity for obsessive-compulsive disorder in bipolar and unipolar disorders. Psychiatry Res. 1995;59:57–64. [PubMed] [Google Scholar]
2. Merikangas KR, Akiskal HS, Angst J, Greenberg PE, Hirschfeld RM, Petukhova M, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64:543–52. [PMC free article] [PubMed] [Google Scholar]
3. Amerio A, Odone A, Liapis CC, Ghaemi SN. Diagnostic validity of comorbid bipolar disorder and obsessive-compulsive disorder: A systematic review. Acta Psychiatr Scand. 2014;129:343–58. [PubMed] [Google Scholar]
4. Amerio A, Odone A, Marchesi C, Ghaemi SN. Treatment of comorbid bipolar disorder and obsessive-compulsive disorder: A systematic review. J Affect Disord. 2014;166:258–63. [PubMed] [Google Scholar]
5. Math SB, Janardhan Reddy YC. Issues in the pharmacological treatment of obsessive-compulsive disorder. Int J Clin Pract. 2007;61:1188–97. [PubMed] [Google Scholar]
6. Pacchiarotti I, Bond DJ, Baldessarini RJ, Nolen WA, Grunze H, Licht RW, et al. The international society for bipolar disorders (ISBD) task force report on antidepressant use in bipolar disorders. Am J Psychiatry. 2013;170:1249–62. [PMC free article] [PubMed] [Google Scholar]
7. Schaffer A, McIntosh D, Goldstein BI, Rector NA, McIntyre RS, Beaulieu S, et al. The CANMAT task force recommendations for the management of patients with mood disorders and comorbid anxiety disorders. Ann Clin Psychiatry. 2012;24:6–22. [PubMed] [Google Scholar]
8. Provencher MD, Hawke LD, Thienot E. Psychotherapies for comorbid anxiety in bipolar spectrum disorders. J Affect Disord. 2011;133:371–80. [PubMed] [Google Scholar]
9. Vázquez GH, Baldessarini RJ, Tondo L. Co-occurrence of anxiety and bipolar disorders: Clinical and therapeutic overview. Depress Anxiety. 2014;31:196–206. [PubMed] [Google Scholar]
10. Faravelli C, Abrardi L, Bartolozzi D, Cecchi C, Cosci F, D’Adamo D, et al. The sesto fiorentino study: Background, methods and preliminary results. Lifetime prevalence of psychiatric disorders in an Italian community sample using clinical interviewers. Psychother Psychosom. 2004;73:216–25. [PubMed] [Google Scholar]
The sesto fiorentino study: Background, methods and preliminary results. Lifetime prevalence of psychiatric disorders in an Italian community sample using clinical interviewers. Psychother Psychosom. 2004;73:216–25. [PubMed] [Google Scholar]
11. Henry C, Van den Bulke D, Bellivier F, Etain B, Rouillon F, Leboyer M. Anxiety disorders in 318 bipolar patients: Prevalence and impact on illness severity and response to mood stabilizer. J Clin Psychiatry. 2003;64:331–5. [PubMed] [Google Scholar]
12. Koyuncu A, Tükel R, Ozyildirim I, Meteris H, Yazici O. Impact of obsessive-compulsive disorder comorbidity on the sociodemographic and clinical features of patients with bipolar disorder. Compr Psychiatry. 2010;51:293–7. [PubMed] [Google Scholar]
13. Shashidhara M, Sushma BR, Viswanath B, Math SB, Janardhan Reddy YC. Comorbid obsessive compulsive disorder in patients with bipolar-I disorder. J Affect Disord. 2015;174:367–71. [PubMed] [Google Scholar]
14. Krüger S, Bräunig P, Cooke RG. Comorbidity of obsessive-compulsive disorder in recovered inpatients with bipolar disorder. Bipolar Disord. 2000;2:71–4. [PubMed] [Google Scholar]
Comorbidity of obsessive-compulsive disorder in recovered inpatients with bipolar disorder. Bipolar Disord. 2000;2:71–4. [PubMed] [Google Scholar]
15. Tamam L, Ozpoyraz N. Comorbidity of anxiety disorder among patients with bipolar I disorder in remission. Psychopathology. 2002;35:203–9. [PubMed] [Google Scholar]
16. Zutshi A, Reddy YC, Thennarasu K, Chandrashekhar CR. Comorbidity of anxiety disorders in patients with remitted bipolar disorder. Eur Arch Psychiatry Clin Neurosci. 2006;256:428–36. [PubMed] [Google Scholar]
17. Magalhães PV, Kapczinski NS, Kapczinski F. Correlates and impact of obsessive-compulsive comorbidity in bipolar disorder. Compr Psychiatry. 2010;51:353–6. [PubMed] [Google Scholar]
18. Angst J, Gamma A, Endrass J, Hantouche E, Goodwin R, Ajdacic V, et al. Obsessive-compulsive syndromes and disorders: Significance of comorbidity with bipolar and anxiety syndromes. Eur Arch Psychiatry Clin Neurosci. 2005;255:65–71. [PubMed] [Google Scholar]
19. Strakowski SM, Sax KW, McElroy SL, Keck PE, Jr, Hawkins JM, West SA. Course of psychiatric and substance abuse syndromes co-occurring with bipolar disorder after a first psychiatric hospitalization. J Clin Psychiatry. 1998;59:465–71. [PubMed] [Google Scholar]
Strakowski SM, Sax KW, McElroy SL, Keck PE, Jr, Hawkins JM, West SA. Course of psychiatric and substance abuse syndromes co-occurring with bipolar disorder after a first psychiatric hospitalization. J Clin Psychiatry. 1998;59:465–71. [PubMed] [Google Scholar]
20. Simon NM, Otto MW, Wisniewski SR, Fossey M, Sagduyu K, Frank E, et al. Anxiety disorder comorbidity in bipolar disorder patients: Data from the first 500 participants in the systematic treatment enhancement program for bipolar disorder (STEP-BD) Am J Psychiatry. 2004;161:2222–9. [PubMed] [Google Scholar]
21. Zutshi A, Kamath P, Reddy YC. Bipolar and nonbipolar obsessive-compulsive disorder: A clinical exploration. Compr Psychiatry. 2007;48:245–51. [PubMed] [Google Scholar]
22. Timpano KR, Rubenstein LM, Murphy DL. Phenomenological features and clinical impact of affective disorders in OCD: A focus on the bipolar disorder and OCD connection. Depress Anxiety. 2012;29:226–33. [PMC free article] [PubMed] [Google Scholar]
23. Dell’Osso B, Buoli M, Bortolussi S, Camuri G, Vecchi V, Altamura AC. Patterns of Axis I comorbidity in relation to age in patients with bipolar disorder: A cross-sectional analysis. J Affect Disord. 2011;130:318–22. [PubMed] [Google Scholar]
Dell’Osso B, Buoli M, Bortolussi S, Camuri G, Vecchi V, Altamura AC. Patterns of Axis I comorbidity in relation to age in patients with bipolar disorder: A cross-sectional analysis. J Affect Disord. 2011;130:318–22. [PubMed] [Google Scholar]
24. Perugi G, Toni C, Frare F, Travierso MC, Hantouche E, Akiskal HS. Obsessive-compulsive-bipolar comorbidity: A systematic exploration of clinical features and treatment outcome. J Clin Psychiatry. 2002;63:1129–34. [PubMed] [Google Scholar]
25. Masi G, Millepiedi S, Perugi G, Pfanner C, Berloffa S, Pari C, et al. Pharmacotherapy in paediatric obsessive-compulsive disorder: A naturalistic, retrospective study. CNS Drugs. 2009;23:241–52. [PubMed] [Google Scholar]
26. Johnson SL, McKenzie G, McMurrich S. Ruminative responses to negative and positive affect among students diagnosed with bipolar disorder and major depressive disorder. Cognit Ther Res. 2008;32:702–3. [PMC free article] [PubMed] [Google Scholar]
27. Cannon DM, Ichise M, Fromm SJ, Nugent AC, Rollis D, Gandhi SK, et al. Serotonin transporter binding in bipolar disorder assessed using [11C] DASB and positron emission tomography. Biol Psychiatry. 2006;60:207–17. [PubMed] [Google Scholar]
Serotonin transporter binding in bipolar disorder assessed using [11C] DASB and positron emission tomography. Biol Psychiatry. 2006;60:207–17. [PubMed] [Google Scholar]
28. Matsumoto R, Ichise M, Ito H, Ando T, Takahashi H, Ikoma Y, et al. Reduced serotonin transporter binding in the insular cortex in patients with obsessive-compulsive disorder: A [11C] DASB PET study. Neuroimage. 2010;49:121–6. [PubMed] [Google Scholar]
29. Spies M, Knudsen GM, Lanzenberger R, Kasper S. The serotonin transporter in psychiatric disorders: Insights from PET imaging. Lancet Psychiatry. 2015;2:743–55. [PubMed] [Google Scholar]
30. Cannon DM, Ichise M, Rollis D, Klaver JM, Gandhi SK, Charney DS, et al. Elevated serotonin transporter binding in major depressive disorder assessed using positron emission tomography and [11C] DASB; comparison with bipolar disorder. Biol Psychiatry. 2007;62:870–7. [PubMed] [Google Scholar]
31. Praschak-Rieder N, Kennedy J, Wilson AA, Hussey D, Boovariwala A, Willeit M, et al. Novel 5-HTTLPR allele associates with higher serotonin transporter binding in putamen: A [(11) C] DASB positron emission tomography study. Biol Psychiatry. 2007;62:327–31. [PubMed] [Google Scholar]
Novel 5-HTTLPR allele associates with higher serotonin transporter binding in putamen: A [(11) C] DASB positron emission tomography study. Biol Psychiatry. 2007;62:327–31. [PubMed] [Google Scholar]
32. Kalbitzer J, Erritzoe D, Holst KK, Nielsen FA, Marner L, Lehel S, et al. Seasonal changes in brain serotonin transporter binding in short serotonin transporter linked polymorphic region-allele carriers but not in long-allele homozygotes. Biol Psychiatry. 2010;67:1033–9. [PubMed] [Google Scholar]
33. Rousseva A, Henry C, van den Bulke D, Fournier G, Laplanche JL, Leboyer M, et al. Antidepressant-induced mania, rapid cycling and the serotonin transporter gene polymorphism. Pharmacogenomics J. 2003;3:101–4. [PubMed] [Google Scholar]
34. Sanacora G, Zarate CA, Krystal JH, Manji HK. Targeting the glutamatergic system to develop novel, improved therapeutics for mood disorders. Nat Rev Drug Discov. 2008;7:426–37. [PMC free article] [PubMed] [Google Scholar]
35. Krystal JH. N-methyl-d-aspartate glutamate receptor antagonists and the promise of rapid-acting antidepressants. Arch Gen Psychiatry. 2010;67:1110–1. [PubMed] [Google Scholar]
N-methyl-d-aspartate glutamate receptor antagonists and the promise of rapid-acting antidepressants. Arch Gen Psychiatry. 2010;67:1110–1. [PubMed] [Google Scholar]
36. Michael N, Erfurth A, Pfleiderer B. Elevated metabolites within dorsolateral prefrontal cortex in rapid cycling bipolar disorder. Psychiatry Res. 2009;172:78–81. [PubMed] [Google Scholar]
37. Dager SR, Friedman SD, Parow A, Demopulos C, Stoll AL, Lyoo IK, et al. Brain metabolic alterations in medication-free patients with bipolar disorder. Arch Gen Psychiatry. 2004;61:450–8. [PubMed] [Google Scholar]
38. Pittenger C, Bloch MH, Williams K. Glutamate abnormalities in obsessive compulsive disorder: Neurobiology, pathophysiology, and treatment. Pharmacol Ther. 2011;132:314–32. [PMC free article] [PubMed] [Google Scholar]
39. Moore GJ, MacMaster FP, Stewart C, Rosenberg DR. Case study: Caudate glutamatergic changes with paroxetine therapy for pediatric obsessive-compulsive disorder. J Am Acad Child Adolesc Psychiatry. 1998;37:663–7. [PubMed] [Google Scholar]
1998;37:663–7. [PubMed] [Google Scholar]
40. Rosenberg DR, MacMaster FP, Keshavan MS, Fitzgerald KD, Stewart CM, Moore GJ. Decrease in caudate glutamatergic concentrations in pediatric obsessive-compulsive disorder patients taking paroxetine. J Am Acad Child Adolesc Psychiatry. 2000;39:1096–103. [PubMed] [Google Scholar]
41. Whiteside SP, Port JD, Deacon BJ, Abramowitz JS. A magnetic resonance spectroscopy investigation of obsessive-compulsive disorder and anxiety. Psychiatry Res. 2006;146:137–47. [PubMed] [Google Scholar]
42. Bolton J, Moore GJ, MacMillan S, Stewart CM, Rosenberg DR. Case study: Caudate glutamatergic changes with paroxetine persist after medication discontinuation in pediatric OCD. J Am Acad Child Adolesc Psychiatry. 2001;40:903–6. [PubMed] [Google Scholar]
43. Starck G, Ljungberg M, Nilsson M, Jönsson L, Lundberg S, Ivarsson T, et al. A 1H magnetic resonance spectroscopy study in adults with obsessive compulsive disorder: Relationship between metabolite concentrations and symptom severity. J Neural Transm (Vienna) 2008;115:1051–62. [PubMed] [Google Scholar]
J Neural Transm (Vienna) 2008;115:1051–62. [PubMed] [Google Scholar]
44. Frye MA, Watzl J, Banakar S, O’Neill J, Mintz J, Davanzo P, et al. Increased anterior cingulate/medial prefrontal cortical glutamate and creatine in bipolar depression. Neuropsychopharmacology. 2007;32:2490–9. [PubMed] [Google Scholar]
45. Geddes JR, Calabrese JR, Goodwin GM. Lamotrigine for treatment of bipolar depression: Independent meta-analysis and meta-regression of individual patient data from five randomised trials. Br J Psychiatry. 2009;194:4–9. [PubMed] [Google Scholar]
46. Calabrese JR, Bowden CL, Sachs GS, Ascher JA, Monaghan E, Rudd GD. A double-blind placebo-controlled study of lamotrigine monotherapy in outpatients with bipolar I depression. Lamictal 602 study group. J Clin Psychiatry. 1999;60:79–88. [PubMed] [Google Scholar]
47. Bruno A, Micò U, Pandolfo G, Mallamace D, Abenavoli E, Di Nardo F, et al. Lamotrigine augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: A double-blind, placebo-controlled study.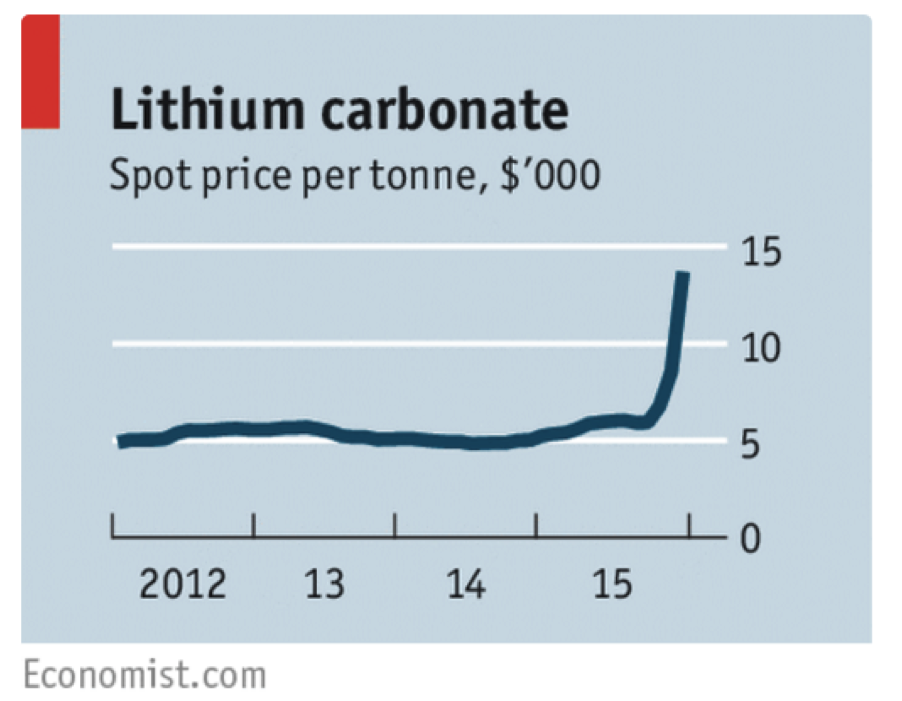 J Psychopharmacol. 2012;26:1456–62. [PubMed] [Google Scholar]
J Psychopharmacol. 2012;26:1456–62. [PubMed] [Google Scholar]
48. Poyurovsky M, Glick I, Koran LM. Lamotrigine augmentation in schizophrenia and schizoaffective patients with obsessive-compulsive symptoms. J Psychopharmacol. 2010;24:861–6. [PubMed] [Google Scholar]
49. Uzun O. Lamotrigine as an augmentation agent in treatment-resistant obsessive-compulsive disorder: A case report. J Psychopharmacol. 2010;24:425–7. [PubMed] [Google Scholar]
50. Du J, Suzuki K, Wei Y, Wang Y, Blumenthal R, Chen Z, et al. The anticonvulsants lamotrigine, riluzole, and valproate differentially regulate AMPA receptor membrane localization: Relationship to clinical effects in mood disorders. Neuropsychopharmacology. 2007;32:793–802. [PubMed] [Google Scholar]
51. Pittenger C, Krystal JH, Coric V. Glutamate-modulating drugs as novel pharmacotherapeutic agents in the treatment of obsessive-compulsive disorder. NeuroRx. 2006;3:69–81. [PMC free article] [PubMed] [Google Scholar]
52. Pittenger C, Coric V, Banasr M, Bloch M, Krystal JH, Sanacora G. Riluzole in the treatment of mood and anxiety disorders. CNS Drugs. 2008;22:761–86. [PubMed] [Google Scholar]
Riluzole in the treatment of mood and anxiety disorders. CNS Drugs. 2008;22:761–86. [PubMed] [Google Scholar]
53. Anand A, Gunn AD, Barkay G, Karne HS, Nurnberger JI, Mathew SJ, et al. Early antidepressant effect of memantine during augmentation of lamotrigine inadequate response in bipolar depression: A double-blind, randomized, placebo-controlled trial. Bipolar Disord. 2012;14:64–70. [PubMed] [Google Scholar]
54. Koukopoulos A, Serra G, Koukopoulos AE, Reginaldi D, Serra G. The sustained mood-stabilizing effect of memantine in the management of treatment resistant bipolar disorders: Findings from a 12-month naturalistic trial. J Affect Disord. 2012;136:163–6. [PubMed] [Google Scholar]
55. Ghaleiha A, Entezari N, Modabbernia A, Najand B, Askari N, Tabrizi M, et al. Memantine add-on in moderate to severe obsessive-compulsive disorder: Randomized double-blind placebo-controlled study. J Psychiatr Res. 2013;47:175–80. [PubMed] [Google Scholar]
56. Moran MM, McFarland K, Melendez RI, Kalivas PW, Seamans JK. Cystine/glutamate exchange regulates metabotropic glutamate receptor presynaptic inhibition of excitatory transmission and vulnerability to cocaine seeking. J Neurosci. 2005;25:6389–93. [PMC free article] [PubMed] [Google Scholar]
Cystine/glutamate exchange regulates metabotropic glutamate receptor presynaptic inhibition of excitatory transmission and vulnerability to cocaine seeking. J Neurosci. 2005;25:6389–93. [PMC free article] [PubMed] [Google Scholar]
57. Deepmala, Slattery J, Kumar N, Delhey L, Berk M, Dean O, et al. Clinical trials of N-acetylcysteine in psychiatry and neurology: A systematic review. Neurosci Biobehav Rev. 2015;55:294–321. [PubMed] [Google Scholar]
58. Lafleur DL, Pittenger C, Kelmendi B, Gardner T, Wasylink S, Malison RT, et al. N-acetylcysteine augmentation in serotonin reuptake inhibitor refractory obsessive-compulsive disorder. Psychopharmacology (Berl) 2006;184:254–6. [PubMed] [Google Scholar]
59. Berlin HA, Koran LM, Jenike MA, Shapira NA, Chaplin W, Pallanti S, et al. Double-blind, placebo-controlled trial of topiramate augmentation in treatment-resistant obsessive-compulsive disorder. J Clin Psychiatry. 2011;72:716–21. [PubMed] [Google Scholar]
60. Fineberg NA, Reghunandanan S, Brown A, Pampaloni I. Pharmacotherapy of obsessive-compulsive disorder: Evidence-based treatment and beyond. Aust N Z J Psychiatry. 2013;47:121–41. [PubMed] [Google Scholar]
Pharmacotherapy of obsessive-compulsive disorder: Evidence-based treatment and beyond. Aust N Z J Psychiatry. 2013;47:121–41. [PubMed] [Google Scholar]
61. Sahraian A, Bigdeli M, Ghanizadeh A, Akhondzadeh S. Topiramate as an adjuvant treatment for obsessive compulsive symptoms in patients with bipolar disorder: A randomized double blind placebo controlled clinical trial. J Affect Disord. 2014;166:201–5. [PubMed] [Google Scholar]
62. van Enkhuizen J, Janowsky DS, Olivier B, Minassian A, Perry W, Young JW, et al. The catecholaminergic-cholinergic balance hypothesis of bipolar disorder revisited. Eur J Pharmacol. 2015;753:114–26. [PMC free article] [PubMed] [Google Scholar]
63. Yatham LN, Goldstein JM, Vieta E, Bowden CL, Grunze H, Post RM, et al. Atypical antipsychotics in bipolar depression: Potential mechanisms of action. J Clin Psychiatry. 2005;66(Suppl 5):40–8. [PubMed] [Google Scholar]
64. Cousins DA, Butts K, Young AH. The role of dopamine in bipolar disorder. Bipolar Disord. 2009;11:787–806. [PubMed] [Google Scholar]
Bipolar Disord. 2009;11:787–806. [PubMed] [Google Scholar]
65. Koo MS, Kim EJ, Roh D, Kim CH. Role of dopamine in the pathophysiology and treatment of obsessive-compulsive disorder. Expert Rev Neurother. 2010;10:275–90. [PubMed] [Google Scholar]
66. Keuneman RJ, Pokos V, Weerasundera R, Castle DJ. Antipsychotic treatment in obsessive-compulsive disorder: A literature review. Aust N Z J Psychiatry. 2005;39:336–43. [PubMed] [Google Scholar]
67. Yatham LN, Kennedy SH, Schaffer A, Parikh SV, Beaulieu S, O’Donovan C, et al. Canadian network for mood and anxiety treatments (CANMAT) and international society for bipolar disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: Update 2009. Bipolar Disord. 2009;11:225–55. [PubMed] [Google Scholar]
68. Amerio A, Stubbs B, Odone A, Tonna M, Marchesi C, Ghaemi SN. The prevalence and predictors of comorbid bipolar disorder and obsessive-compulsive disorder: A systematic review and meta-analysis. J Affect Disord. 2015;186:99–109. [PubMed] [Google Scholar]
J Affect Disord. 2015;186:99–109. [PubMed] [Google Scholar]
69. Pigott TA, Pato MT, L’Heureux F, Hill JL, Grover GN, Bernstein SE, et al. A controlled comparison of adjuvant lithium carbonate or thyroid hormone in clomipramine-treated patients with obsessive-compulsive disorder. J Clin Psychopharmacol. 1991;11:242–8. [PubMed] [Google Scholar]
70. Swartz CM, Shen WW. Is episodic obsessive compulsive disorder bipolar? A report of four cases. J Affect Disord. 1999;56:61–6. [PubMed] [Google Scholar]
71. Bisol LW, Lara DR. Improvement of obsessive-compulsive disorder with divalproex and lamotrigine in two patients with bipolar II disorder. Pharmacopsychiatry. 2009;42:37–9. [PubMed] [Google Scholar]
72. Corá-Locatelli G, Greenberg BD, Martin JD, Murphy DL. Valproate monotherapy in an SRI-intolerant OCD patient. J Clin Psychiatry. 1998;59:82. [PubMed] [Google Scholar]
73. Zink M, Englisch S, Knopf U, Kuwilsky A, Dressing H. Augmentation of clozapine with valproic acid for clozapine-induced obsessive-compulsive symptoms. Pharmacopsychiatry. 2007;40:202–3. [PubMed] [Google Scholar]
Pharmacopsychiatry. 2007;40:202–3. [PubMed] [Google Scholar]
74. Hollander E, Soorya L, Wasserman S, Esposito K, Chaplin W, Anagnostou E. Divalproex sodium vs. placebo in the treatment of repetitive behaviours in autism spectrum disorder. Int J Neuropsychopharmacol. 2006;9:209–13. [PubMed] [Google Scholar]
75. Veale D, Miles S, Smallcombe N, Ghezai H, Goldacre B, Hodsoll J, et al. Atypical antipsychotic augmentation in SSRI treatment refractory obsessive-compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry. 2014;14:317. [PMC free article] [PubMed] [Google Scholar]
76. Rakofsky JJ, Dunlop BW. Treating nonspecific anxiety and anxiety disorders in patients with bipolar disorder: A review. J Clin Psychiatry. 2011;72:81–90. [PubMed] [Google Scholar]
77. Joshi G, Mick E, Wozniak J, Geller D, Park J, Strauss S, et al. Impact of obsessive-compulsive disorder on the antimanic response to olanzapine therapy in youth with bipolar disorder. Bipolar Disord. 2010;12:196–204. [PubMed] [Google Scholar]
2010;12:196–204. [PubMed] [Google Scholar]
78. Jonkers F, De Haan L. Olanzapine-induced obsessive-compulsive symptoms in a patient with bipolar II disorder. Psychopharmacology (Berl) 2002;162:87–8. [PubMed] [Google Scholar]
79. Lykouras L, Alevizos B, Michalopoulou P, Rabavilas A. Obsessive-compulsive symptoms induced by atypical antipsychotics. A review of the reported cases. Prog Neuropsychopharmacol Biol Psychiatry. 2003;27:333–46. [PubMed] [Google Scholar]
80. Muscatello MR, Bruno A, Pandolfo G, Micò U, Scimeca G, Romeo VM, et al. Effect of aripiprazole augmentation of serotonin reuptake inhibitors or clomipramine in treatment-resistant obsessive-compulsive disorder: A double-blind, placebo-controlled study. J Clin Psychopharmacol. 2011;31:174–9. [PubMed] [Google Scholar]
81. Sayyah M, Sayyah M, Boostani H, Ghaffari SM, Hoseini A. Effects of aripiprazole augmentation in treatment-resistant obsessive-compulsive disorder (a double blind clinical trial) Depress Anxiety. 2012;29:850–4. [PubMed] [Google Scholar]
2012;29:850–4. [PubMed] [Google Scholar]
82. Bruno A, Pandolfo G, Cedro C, Gallo G, De Felice M, Zoccali RA, et al. Effect of ziprasidone augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: A 12-week, open-label uncontrolled preliminary study. Clin Neuropharmacol. 2016;39:6–9. [PubMed] [Google Scholar]
83. Krause DL, Matz J, Schennach R, Müller N, Dehning S. Ziprasidone for obsessive compulsive disorder in schizophrenia. Ther Adv Psychopharmacol. 2013;3:115–6. [PMC free article] [PubMed] [Google Scholar]
84. Stratta P, de Cataldo S, Mancini G, Gianfelice D, Rinaldi O, Rossi A. Quetiapine as adjunctive treatment of a case of rapid-cycling bipolar disorder with comorbidity. Hum Psychopharmacol. 2003;18:559–60. [PubMed] [Google Scholar]
85. Raja M, Azzoni A. Clinical management of obsessive-compulsive-bipolar comorbidity: A case series. Bipolar Disord. 2004;6:264–70. [PubMed] [Google Scholar]
86. Petrikis P, Andreou C, Bozikas VP, Karavatos A. Effective use of olanzapine for obsessive-compulsive symptoms in a patient with bipolar disorder. Can J Psychiatry. 2004;49:572–3. [PubMed] [Google Scholar]
Effective use of olanzapine for obsessive-compulsive symptoms in a patient with bipolar disorder. Can J Psychiatry. 2004;49:572–3. [PubMed] [Google Scholar]
87. Uguz F. Successful treatment of comorbid obsessive-compulsive disorder with aripiprazole in three patients with bipolar disorder. Gen Hosp Psychiatry. 2010;32:556–8. [PubMed] [Google Scholar]
88. Chang JS, Ha K. Management of bipolar depression. Indian J Psychol Med. 2011;33:11–7. [PMC free article] [PubMed] [Google Scholar]
89. El-Mallakh RS, Hollifield M. Comorbid anxiety in bipolar disorder alters treatment and prognosis. Psychiatr Q. 2008;79:139–50. [PubMed] [Google Scholar]
90. Leverich GS, Altshuler LL, Frye MA, Suppes T, McElroy SL, Keck PE, Jr, et al. Risk of switch in mood polarity to hypomania or mania in patients with bipolar depression during acute and continuation trials of venlafaxine, sertraline, and bupropion as adjuncts to mood stabilizers. Am J Psychiatry. 2006;163:232–9. [PubMed] [Google Scholar]
91. Gijsman HJ, Geddes JR, Rendell JM, Nolen WA, Goodwin GM. Antidepressants for bipolar depression: A systematic review of randomized, controlled trials. Am J Psychiatry. 2004;161:1537–47. [PubMed] [Google Scholar]
Gijsman HJ, Geddes JR, Rendell JM, Nolen WA, Goodwin GM. Antidepressants for bipolar depression: A systematic review of randomized, controlled trials. Am J Psychiatry. 2004;161:1537–47. [PubMed] [Google Scholar]
92. Sachs GS, Nierenberg AA, Calabrese JR, Marangell LB, Wisniewski SR, Gyulai L, et al. Effectiveness of adjunctive antidepressant treatment for bipolar depression. N Engl J Med. 2007;356:1711–22. [PubMed] [Google Scholar]
93. Schaffer A, Cairney J, Veldhuizen S, Cheung A, Levitt A. Comparison of antidepressant use between subjects with bipolar disorder and major depressive disorder with or without comorbid anxiety. J Clin Psychiatry. 2007;68:1785–92. [PubMed] [Google Scholar]
94. Simon NM, Otto MW, Weiss RD, Bauer MS, Miyahara S, Wisniewski SR, et al. Pharmacotherapy for bipolar disorder and comorbid conditions: Baseline data from STEP-BD. J Clin Psychopharmacol. 2004;24:512–20. [PubMed] [Google Scholar]
95. Tondo L, Vázquez G, Baldessarini RJ. Mania associated with antidepressant treatment: Comprehensive meta-analytic review.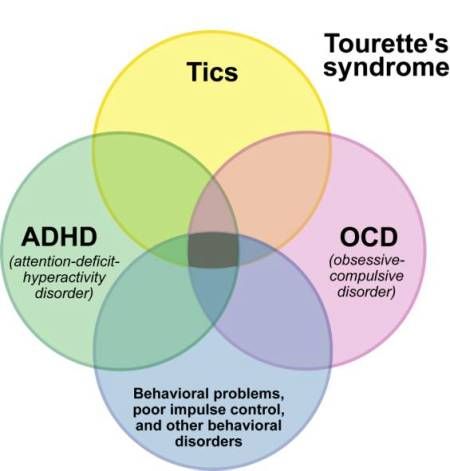 Acta Psychiatr Scand. 2010;121:404–14. [PubMed] [Google Scholar]
Acta Psychiatr Scand. 2010;121:404–14. [PubMed] [Google Scholar]
96. Philip J, Janaki R. Antidepressant-induced mania in obsessive compulsive disorder. Indian J Psychiatry. 2012;54:194–5. [PMC free article] [PubMed] [Google Scholar]
97. Marazziti D, Pfanner C, Dell'Osso B, Ciapparelli A, Presta S, Corretti G, et al. Augmentation strategy with olanzapine in resistant obsessive compulsive disorder: An Italian long-term open-label study. J Psychopharmacol. 2005;19:392–4. [PubMed] [Google Scholar]
98. Kalra H, Tandon R, Saluja B, Mohan I. Obsessive compulsive disorder: Co-morbidity in manic phase of bipolar affective disorder. Indian J Psychiatry. 2002;44:377–9. [PMC free article] [PubMed] [Google Scholar]
99. Baer L, Minichiello WE, Jenike MA. Behavioral treatment in two cases of obsessive-compulsive disorder with concomitant bipolar affective disorder. Am J Psychiatry. 1985;142:358–60. [PubMed] [Google Scholar]
100. Herstowska M, Cubala WJ. Escitalopram efficacy in obsessive-compulsive disorder comorbid with bipolar disorder. Dusunen Adam. 2013;26:115–6. [Google Scholar]
Dusunen Adam. 2013;26:115–6. [Google Scholar]
101. Dittrich WH, Johansen T, Padhi AK, Smith IE, Chamberlain SR, Fineberg NA. Clinical and neurocognitive changes with modafinil in obsessive-compulsive disorder: A case report. Psychopharmacology (Berl) 2010;212:449–51. [PubMed] [Google Scholar]
102. Tan O, Coban A, Tarhan N, Baripoglu S, Guducu F, Izgi HB, et al. Exacerbation of obsessions with modafinil in 2 patients with medication-responsive obsessive-compulsive disorder. Prim Care Companion J Clin Psychiatry. 2008;10:164–5. [PMC free article] [PubMed] [Google Scholar]
103. Mowla A, Kardeh E. Topiramate augmentation in patients with resistant major depressive disorder: A double-blind placebo-controlled clinical trial. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35:970–3. [PubMed] [Google Scholar]
104. Hollander E, Dell’Osso B. Topiramate plus paroxetine in treatment-resistant obsessive-compulsive disorder. Int Clin Psychopharmacol. 2006;21:189–91. [PubMed] [Google Scholar]
105. Crockett BA, Churchill E, Davidson JR. A double-blind combination study of clonazepam with sertraline in obsessive-compulsive disorder. Ann Clin Psychiatry. 2004;16:127–32. [PubMed] [Google Scholar]
Crockett BA, Churchill E, Davidson JR. A double-blind combination study of clonazepam with sertraline in obsessive-compulsive disorder. Ann Clin Psychiatry. 2004;16:127–32. [PubMed] [Google Scholar]
106. Hollander E, Kaplan A, Stahl SM. A double-blind, placebo-controlled trial of clonazepam in obsessive-compulsive disorder. World J Biol Psychiatry. 2003;4:30–4. [PubMed] [Google Scholar]
107. Koukopoulos A, Reginaldi D, Serra G, Koukopoulos A, Sani G, Serra G. Antimanic and mood-stabilizing effect of memantine as an augmenting agent in treatment-resistant bipolar disorder. Bipolar Disord. 2010;12:348–9. [PubMed] [Google Scholar]
108. Keck PE, Jr, Hsu HA, Papadakis K, Russo J., Jr Memantine efficacy and safety in patients with acute mania associated with bipolar I disorder: A pilot evaluation. Clin Neuropharmacol. 2009;32:199–204. [PubMed] [Google Scholar]
109. Serra G, De Chiara L, Manfredi G, Koukopoulos AE, Sani G, Girardi P, et al. Memantine in the management of affective recurrences of bipolar disorders after the discontinuation of long-term lithium treatment: Three case histories. Ther Adv Psychopharmacol. 2014;4:53–5. [PMC free article] [PubMed] [Google Scholar]
Ther Adv Psychopharmacol. 2014;4:53–5. [PMC free article] [PubMed] [Google Scholar]
110. Stewart SE, Jenike EA, Hezel DM, Stack DE, Dodman NH, Shuster L, et al. A single-blinded case-control study of memantine in severe obsessive-compulsive disorder. J Clin Psychopharmacol. 2010;30:34–9. [PubMed] [Google Scholar]
111. Aboujaoude E, Barry JJ, Gamel N. Memantine augmentation in treatment-resistant obsessive-compulsive disorder: An open-label trial. J Clin Psychopharmacol. 2009;29:51–5. [PubMed] [Google Scholar]
112. Pasquini M, Biondi M. Memantine augmentation for refractory obsessive-compulsive disorder. Prog Neuropsychopharmacol Biol Psychiatry. 2006;30:1173–5. [PubMed] [Google Scholar]
113. Hezel DM, Beattie K, Stewart SE. Memantine as an augmenting agent for severe pediatric OCD. Am J Psychiatry. 2009;166:237. [PubMed] [Google Scholar]
114. Sani G, Serra G, Kotzalidis GD, Romano S, Tamorri SM, Manfredi G, et al. The role of memantine in the treatment of psychiatric disorders other than the dementias: A review of current preclinical and clinical evidence. CNS Drugs. 2012;26:663–90. [PubMed] [Google Scholar]
CNS Drugs. 2012;26:663–90. [PubMed] [Google Scholar]
115. Coric V, Taskiran S, Pittenger C, Wasylink S, Mathalon DH, Valentine G, et al. Riluzole augmentation in treatment-resistant obsessive-compulsive disorder: An open-label trial. Biol Psychiatry. 2005;58:424–8. [PubMed] [Google Scholar]
116. Grant P, Lougee L, Hirschtritt M, Swedo SE. An open-label trial of riluzole, a glutamate antagonist, in children with treatment-resistant obsessive-compulsive disorder. J Child Adolesc Psychopharmacol. 2007;17:761–7. [PubMed] [Google Scholar]
117. Pittenger C, Kelmendi B, Wasylink S, Bloch MH, Coric V. Riluzole augmentation in treatment-refractory obsessive-compulsive disorder: A series of 13 cases, with long-term follow-up. J Clin Psychopharmacol. 2008;28:363–7. [PubMed] [Google Scholar]
118. El-Mallakh RS, Elmaadawi AZ, Gao Y, Lohano K, Roberts RJ. Current and emerging therapies for the management of bipolar disorders. J Cent Nerv Syst Dis. 2011;3:189–97. [PMC free article] [PubMed] [Google Scholar]
119. Zarate CA, Jr, Quiroz JA, Singh JB, Denicoff KD, De Jesus G, Luckenbaugh DA, et al. An open-label trial of the glutamate-modulating agent riluzole in combination with lithium for the treatment of bipolar depression. Biol Psychiatry. 2005;57:430–2. [PubMed] [Google Scholar]
Zarate CA, Jr, Quiroz JA, Singh JB, Denicoff KD, De Jesus G, Luckenbaugh DA, et al. An open-label trial of the glutamate-modulating agent riluzole in combination with lithium for the treatment of bipolar depression. Biol Psychiatry. 2005;57:430–2. [PubMed] [Google Scholar]
120. Yazici KU, Percinel I. N-acetylcysteine augmentation in children and adolescents diagnosed with treatment-resistant obsessive-compulsive disorder: Case series. J Clin Psychopharmacol. 2015;35:486–9. [PubMed] [Google Scholar]
121. Magalhães PV, Dean OM, Bush AI, Copolov DL, Malhi GS, Kohlmann K, et al. N-acetyl cysteine add-on treatment for bipolar II disorder: A subgroup analysis of a randomized placebo-controlled trial. J Affect Disord. 2011;129:317–20. [PubMed] [Google Scholar]
122. Magalhães PV, Dean OM, Bush AI, Copolov DL, Malhi GS, Kohlmann K, et al. A preliminary investigation on the efficacy of N-acetyl cysteine for mania or hypomania. Aust N Z J Psychiatry. 2013;47:564–8. [PubMed] [Google Scholar]
123. Berk M, Dean O, Cotton SM, Gama CS, Kapczinski F, Fernandes BS, et al. The efficacy of N-acetylcysteine as an adjunctive treatment in bipolar depression: An open label trial. J Affect Disord. 2011;135:389–94. [PubMed] [Google Scholar]
Berk M, Dean O, Cotton SM, Gama CS, Kapczinski F, Fernandes BS, et al. The efficacy of N-acetylcysteine as an adjunctive treatment in bipolar depression: An open label trial. J Affect Disord. 2011;135:389–94. [PubMed] [Google Scholar]
124. Kellner CH, Ahle GM, Geduldig ET. Electroconvulsive therapy for bipolar disorder: Evidence supporting what clinicians have long known. J Clin Psychiatry. 2015;76:e1151–2. [PubMed] [Google Scholar]
125. Lapidus KA, Stern ER, Berlin HA, Goodman WK. Neuromodulation for obsessive-compulsive disorder. Neurotherapeutics. 2014;11:485–95. [PMC free article] [PubMed] [Google Scholar]
126. Bülbül F, Copoglu US, Alpak G, Unal A, Tastan MF, Savas HA. Maintenance therapy with electroconvulsive therapy in a patient with a codiagnosis of bipolar disorder and obsessive-compulsive disorder. J ECT. 2013;29:e21–2. [PubMed] [Google Scholar]
127. Hanisch F, Friedemann J, Piro J, Gutmann P. Maintenance electroconvulsive therapy for comorbid pharmacotherapy-refractory obsessive-compulsive and schizoaffective disorder. Eur J Med Res. 2009;14:367–8. [PMC free article] [PubMed] [Google Scholar]
Eur J Med Res. 2009;14:367–8. [PMC free article] [PubMed] [Google Scholar]
128. Seibell PJ, Hollander E. Management of obsessive-compulsive disorder. F1000Prime Rep. 2014;6:68. [PMC free article] [PubMed] [Google Scholar]
129. Bersani FS, Minichino A, Enticott PG, Mazzarini L, Khan N, Antonacci G, et al. Deep transcranial magnetic stimulation as a treatment for psychiatric disorders: A comprehensive review. Eur Psychiatry. 2013;28:30–9. [PubMed] [Google Scholar]
130. Mantione M, Nieman DH, Figee M, Denys D. Cognitive-behavioural therapy augments the effects of deep brain stimulation in obsessive-compulsive disorder. Psychol Med. 2014;44:3515–22. [PubMed] [Google Scholar]
131. Chang CH, Chen SY, Hsiao YL, Chen SJ, Tsai ST, Chang CH, et al. Hypomania-like syndrome induced by deep brain stimulation of bilateral anterior limbs of the internal capsules. Prog Neuropsychopharmacol Biol Psychiatry. 2009;33:906–7. [PubMed] [Google Scholar]
132. Eddy KT, Dutra L, Bradley R, Westen D. A multidimensional meta-analysis of psychotherapy and pharmacotherapy for obsessive-compulsive disorder. Clin Psychol Rev. 2004;24:1011–30. [PubMed] [Google Scholar]
A multidimensional meta-analysis of psychotherapy and pharmacotherapy for obsessive-compulsive disorder. Clin Psychol Rev. 2004;24:1011–30. [PubMed] [Google Scholar]
133. Rosa-Alcázar AI, Sánchez-Meca J, Gómez-Conesa A, Marín-Martínez F. Psychological treatment of obsessive-compulsive disorder: A meta-analysis. Clin Psychol Rev. 2008;28:1310–25. [PubMed] [Google Scholar]
134. Albert U, Rosso G, Maina G, Bogetto F. Impact of anxiety disorder comorbidity on quality of life in euthymic bipolar disorder patients: Differences between bipolar I and II subtypes. J Affect Disord. 2008;105:297–303. [PubMed] [Google Scholar]
135. Knopp J, Knowles S, Bee P, Lovell K, Bower P. A systematic review of predictors and moderators of response to psychological therapies in OCD: Do we have enough empirical evidence to target treatment? Clin Psychol Rev. 2013;33:1067–81. [PubMed] [Google Scholar]
136. Mahasuar R, Janardhan Reddy YC, Math SB. Obsessive-compulsive disorder with and without bipolar disorder.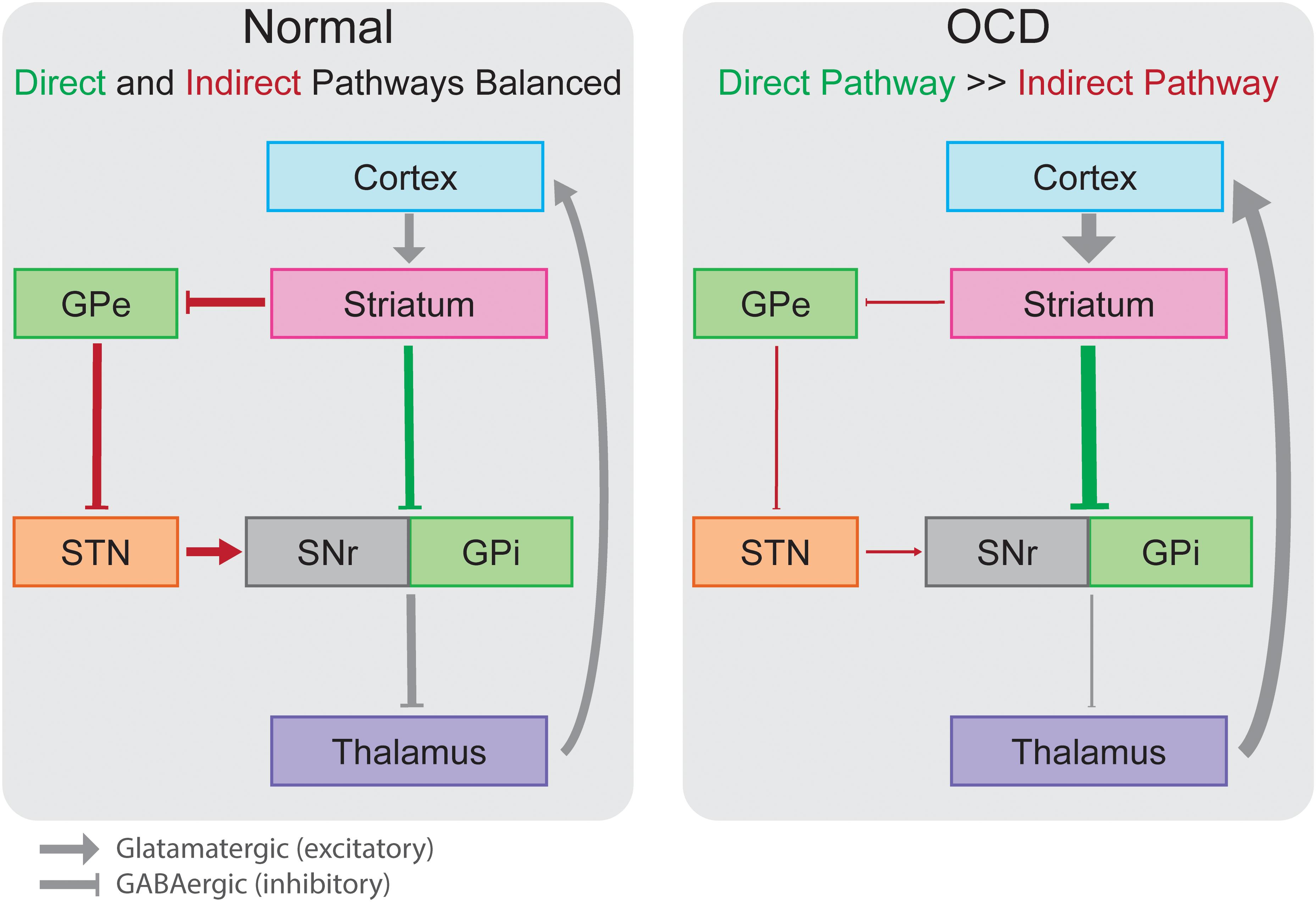 Psychiatry Clin Neurosci. 2011;65:423–33. [PubMed] [Google Scholar]
Psychiatry Clin Neurosci. 2011;65:423–33. [PubMed] [Google Scholar]
137. Marazziti D, Dell’Osso L, Di Nasso E, Pfanner C, Presta S, Mungai F, et al. Insight in obsessive-compulsive disorder: A study of an Italian sample. Eur Psychiatry. 2002;17:407–10. [PubMed] [Google Scholar]
The Incredible, The Amazing, Lithium!
It’s an amazing metal. Not only does it treat acute mania, prevent recurrences, and treat refractory depression, but when consumed as LiCl, it tastes pretty good on vegetables. Or at least it did before the 1950s, when it was dropped from the list of acceptable salt-substitutes for hypertensives because of a nasty tendency to cause toxicity.
The history of lithium is colorful, and is covered elsewhere in this month’s issue. In this article, TCR covers lithium from a clinical perspective, in the hopes of reminding you that it’s easy to prescribe and to monitor, it’s effective, and it’s very cheap.
Lithium’s benefits
In treating acute manic episodes, lithium’s response rate is in the range of 70-80%. That’s the good news. The bad news is that it takes up to two weeks to kick in, and thus is about a week slower than its main competitors, Depakote and the atypical antipsychotics. This is not a huge problem, however, because we will often use adjunctive neuroleptics or benzodiazepines for acute mania anyway.
That’s the good news. The bad news is that it takes up to two weeks to kick in, and thus is about a week slower than its main competitors, Depakote and the atypical antipsychotics. This is not a huge problem, however, because we will often use adjunctive neuroleptics or benzodiazepines for acute mania anyway.
Not only does lithium treat mania, but it is the only medication in the world that has been shown to be more effective than placebo in preventing recurrences of both mania and depression in bipolar disorder (1). Other medications may be effective for preventing specific problems in bipolar disorder. Thus, Lamictal (lamotrigine) prevents bipolar depression, and a recently reported but not yet peer-reviewed abstract reports that Zyprexa (olanzapine) was better than lithium at preventing relapse to mania in one trial (2). But lithium has been shown effective in bipolar disorder prophylaxis in study after study over the last 30 years.
Lithium is a good antidepressant, and is currently one of two drugs recommended in APA Guidelines for the treatment of bipolar depression (3). Lithium is the only psychiatric medication (other than clozapine) proven to prevent suicide. Meta-analytic studies have reported a 93% reduction in suicide acts in patients on lithium. Interestingly, lithium’s antisuicide effect was most robust in recurrent major depression, although it was still a boon in both bipolar I and bipolar II disorders. Does this suicide data imply that we should be putting all our severely depressed patients on lithium, whether they have bipolar disorder or not? It’s an arguable point!
Lithium is the only psychiatric medication (other than clozapine) proven to prevent suicide. Meta-analytic studies have reported a 93% reduction in suicide acts in patients on lithium. Interestingly, lithium’s antisuicide effect was most robust in recurrent major depression, although it was still a boon in both bipolar I and bipolar II disorders. Does this suicide data imply that we should be putting all our severely depressed patients on lithium, whether they have bipolar disorder or not? It’s an arguable point!
There are a variety of allegations floating around related to certain supposed advantages of Depakote over lithium, especially in any manic presentation other than classic euphoric mania. Read the Depakote article in this issue for TCR‘s version of clarity on this topic.
How to Use Lithium
Now that you’re chomping at the bit to start prescribing lithium, how should you do it? Start by getting baseline TSH, T4, and BUN/Cr levels drawn before the first dose, and then start with regular old Lithium Carbonate, 300 or 600 mg QHS. LiCO3 may cause a bit more initial GI distress than Eskalith CR or Lithobid but it’s about half the price. Lithium’s half life is 24 hours, so don’t even think of dosing more than once a day, unless it becomes clear over time that your patient has fewer side effects with split dosing. Dosing it at night also has the beneficial effect of causing less polyuria.
LiCO3 may cause a bit more initial GI distress than Eskalith CR or Lithobid but it’s about half the price. Lithium’s half life is 24 hours, so don’t even think of dosing more than once a day, unless it becomes clear over time that your patient has fewer side effects with split dosing. Dosing it at night also has the beneficial effect of causing less polyuria.
Try to get the lithium level up to 0.8 meq/L or so. Comparative studies have shown that higher serum levels are more effective at preventing relapse, but on the down side, they lead to lower tolerability and more treatment drop-out. So shoot for 0.8, but if you have to drop down to 0.6 or 0.7 to maintain a happy camper, by all means do so. You’ll probably end up at a dose between 900 mg – 1500 mg QHS for most patients.
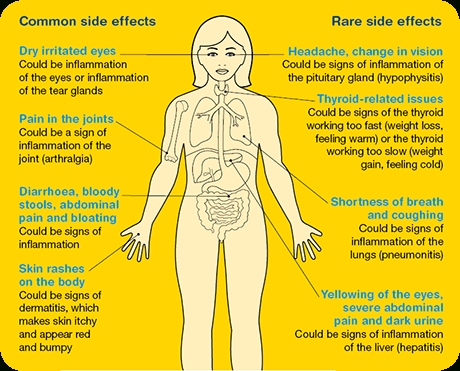
Check lithium levels, TSH/T4, and BUN/Cr after one week, at one to two months, then every 6 to 12 months thereafter. The most common side effects are GI discomfort (remedies: split dosing, take with meals, switch to long-acting formulation, or switch to Li Citrate syrup), tremor (use Inderal LA 60 mg QAM or regular Inderal 20 mg BIDTID prn), polyuria/excessive thirst (dose it all at night, use low dose hydrochlorthiazide but watch lithium levels, which will often increase on this regimen), memory problems (no proven remedy, some try stimulants or acetylcholinesterase inhibitors), weight gain (diet and exercise and prayer).
Two side effect issues are confusing and controversial. First, can lithium actually damage the kidneys, beyond causing reversible polyuria? The answer is: probably, but it’s quite rare. A ten-year prospective followup study of lithium’s effects on the kidney found that declining kidney function was more related to age of the patient than duration of lithium use. One risk factor appears to be a history of frank lithium toxicity. Bottom-line is that kidney damage is unlikely, but caution dictates yearly BUN/Cr levels.
The second issue is lithium’s effects on the heart. A Medline search reveals many case reports of lithium-induced sinus node dysfunction. Recall that the sinus node is our main cardiac pacemaker, and keeps our hearts beating in the 60-100 range. The usual symptoms of sinus node dysfunction are the results of bradycardia–fatigue, dizziness, and fainting. Studies that have bothered to measure sinus node functioning in large groups of patients on lithium have been pretty reassuring: severe, symptomatic sinus node dysfunction is quite rare (5). Based on this, a common sense approach would be to: 1) Get a pre-lithium EKG in patients with documented cardiac disease, especially in patients over 50, who have a higher rate of bradycardia due to age alone; and 2) Order an EKG in any lithium treated patient who has new onset dizziness or fainting.
Based on this, a common sense approach would be to: 1) Get a pre-lithium EKG in patients with documented cardiac disease, especially in patients over 50, who have a higher rate of bradycardia due to age alone; and 2) Order an EKG in any lithium treated patient who has new onset dizziness or fainting.
TCR VERDICT: Dont Neglect the Magic of Lithium!
23 roles of lithium in the human body. Scientific data.
Lithium is an alkali metal found naturally in trace amounts in minerals, water, soil, and fruits, vegetables, and other plants grown in lithium-enriched soils (https://www.ncbi.nlm.nih.gov/pubmed /11601880).
Lithium is essential for the proper functioning of a number of enzymes, hormones, vitamins, growth factors and the immune and nervous systems (https://www.igsli.org/general-information-on-lithium/biochemical-effects-of-lithium.html).
In addition to lithium's role in treating psychiatric patients, this mineral has many health benefits, and the list continues to grow.
1. Lithium has a neuroprotective effect (protection of brain cells)
Long-term lithium treatment reduces glutamate-induced toxicity mediated by N-methyl-D-aspartate (NMDA) receptors. This effect was at least partially explained by the ability of lithium to suppress calcium influx, which affects the activity of the NMDA receptor. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39)
Thus, lithium has the potential to be beneficial for conditions such as mood disorders, Alzheimer's, diabetes, cancer, and inflammatory and autoimmune diseases (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/# R39).
2. Lithium inhibits apoptosis
Lithium increases levels of heat shock proteins (HSPs), which promote proper 3D folding of proteins, refolding of damaged proteins, and utilization of atypical proteins (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
Among heat shock proteins, HSP70 has a wide range of neuroprotective effects against apoptosis. These effects are caused by GSK-3 inhibition (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39). Lithium is also known to inhibit GSK-3 (https://www.ncbi.nlm.nih.gov/pubmed/8994831).
These effects are caused by GSK-3 inhibition (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39). Lithium is also known to inhibit GSK-3 (https://www.ncbi.nlm.nih.gov/pubmed/8994831).
Long-term lithium treatment has been noted to induce the production of Bcl-2, a protein in the frontal lobe of the brain that protects cells from apoptosis (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
3. Lithium increases levels of neurotrophic factors BDNF, NGF and GDNF
Prolonged exposure of neurons to lithium in culture induces BDNF activity. (reference 2)
BDNF is one of the main neurotrophic agents indispensable for cognitive development, synaptic plasticity and neuronal survival, which also has antidepressant and calming effects. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39)
This probably occurs as a result of GSK-3 inhibition. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39)
Lithium also increases nerve growth factor (NGF) and glial neurotrophic factor (GDNF) levels in the hippocampus, frontal cortex, occipital region, and striatum (https://www. ncbi.nlm.nih.gov/pubmed/12974988). NGF and GDNF help increase neuronal survival and plasticity (the ability to regenerate and form new connections) among dopaminergic, cholinergic, and serotonergic neurons in the central nervous system.
ncbi.nlm.nih.gov/pubmed/12974988). NGF and GDNF help increase neuronal survival and plasticity (the ability to regenerate and form new connections) among dopaminergic, cholinergic, and serotonergic neurons in the central nervous system.
4. Lithium promotes the regeneration of cerebral and cardiac vessels (VEGF)
Lithium leads to an increase in the production of vascular endothelial growth factor, VEGF, which promotes cell growth and regeneration of blood vessels after a stroke (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
By increasing VEGF levels, lithium may promote faster recovery after a stroke or heart attack (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
The likely mechanism is lithium inhibition of GSK-3 (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
5. Lithium induces autophagy
Autophagy or "cell self-destruction" is when cells break down and recycle cellular components to reuse raw materials (https://www. ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39). Autophagy is thought to slow down aging, prevent cancer, and is important for neuronal function and survival (http://genesdev.cshlp.org/content/21/22/2861.full, https://www.ncbi.nlm.nih .gov/pmc/articles/PMC2020444/).
ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39). Autophagy is thought to slow down aging, prevent cancer, and is important for neuronal function and survival (http://genesdev.cshlp.org/content/21/22/2861.full, https://www.ncbi.nlm.nih .gov/pmc/articles/PMC2020444/).
Lithium can induce autophagy by depleting inositol stores independently of mTOR inhibition (which by itself usually induces autophagy) (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
Since lithium induces autophagy, the drug may be especially useful for patients with neurodegenerative diseases - Alzheimer's disease, Parkinson's disease, amyotrophic lateral sclerosis and Huntington's disease, since such disorders are characterized in part by the accumulation of misfolded proteins (https://www.ncbi.nlm .nih.gov/pmc/articles/PMC3172812/#R39).
6. Lithium increases neurogenesis and improves cognitive function
Lithium has been found to stimulate progenitor and stem cells in a culture of brain hippocampal neurons (neurons from the memory center). In addition, lithium prevents loss of proliferation caused by glutamate or cortisol (glucocorticoids). Also, long-term lithium treatment promotes the conversion of these precursor cells into neurons (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
In addition, lithium prevents loss of proliferation caused by glutamate or cortisol (glucocorticoids). Also, long-term lithium treatment promotes the conversion of these precursor cells into neurons (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39).
In addition, long-term lithium treatment not only improves neurogenesis in the hippocampus (memory center) in healthy mice, but also restores neurogenesis in the brain of an animal model of Down syndrome (https://www.ncbi.nlm.nih.gov/pmc/articles /PMC3172812/#R39).
The drug also enhances neurogenesis (the formation of new neurons) in the subventricular zone, the only area besides the hippocampus (memory center) where such an effect was observed, which caused a persistent increase in gray matter volume in patients (https://www.ncbi.nlm.nih. gov/pmc/articles/PMC3172812/#R39).
Lithium increases N-acetyl aspartate (NAA) levels (http://www.biologicalpsychiatryjournal.com/article/S0006-3223(00)00252-3/abstract), which can be seen as an indicator of creativity and correlates with IQ scores (https http://www. ncbi.nlm.nih.gov/pubmed/21983183). One possible consequence of this may be more efficient communication between the two hemispheres of the brain, resulting in improved brain activity. (https://www.ncbi.nlm.nih.gov/pubmed/21983183)
ncbi.nlm.nih.gov/pubmed/21983183). One possible consequence of this may be more efficient communication between the two hemispheres of the brain, resulting in improved brain activity. (https://www.ncbi.nlm.nih.gov/pubmed/21983183)
Long-term lithium treatment increases long-term potentiation (LTP) in hippocampal neurons, which makes nerve cells more efficient and thus aids in learning and memory (http://europepmc.org/abstract/MED/17996377).
7. Lithium can calm and stabilize mood
In animals, lithium staunchly reduces search activity and aggression. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2150568/)
In humans, lithium is also known to have a calming and mood-stabilizing effect, and is also used to treat depression, bipolar disorder, and schizophrenia (https://en.wikipedia.org/wiki/Lithium_(medication).
Lithium carbonate is the standard of care for bipolar affective disorder (BAD), reducing the frequency of manic episodes (https://www. ncbi.nlm.nih.gov/pmc/articles/PMC2560740/pdf/10885180.pdf, https://www. ncbi.nlm.nih.gov/pmc/articles/PMC3181868/, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3876031/).
ncbi.nlm.nih.gov/pmc/articles/PMC2560740/pdf/10885180.pdf, https://www. ncbi.nlm.nih.gov/pmc/articles/PMC3181868/, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3876031/).
Lithium has also been shown to be effective in reducing aggressive behavior in people with attention deficit hyperactivity disorder (ADHD) (https://www.ncbi.nlm.nih.gov/pubmed/12154153).
Increased levels of naturally occurring lithium in drinking water may reduce suicide rates (https://en.wikipedia.org/wiki/Lithium_(medication)). This may be partly due to the fact that lithium increases the synthesis and release of serotonin (it also reduces the level of norepinephrine) (https://en.wikipedia.org/wiki/Lithium_(medication)).
Lithium increases CCK levels in the brain and this is part of the mechanism by which lithium prevents mania in bipolar disorder.
8. Lithium fights depression
Lithium administration is one of the most studied approaches in the treatment of depression refractory to standard therapy (https://www. ncbi.nlm.nih.gov/pubmed/22796912).
ncbi.nlm.nih.gov/pubmed/22796912).
Lithium increases postsynaptic sensitivity to serotonin via the 5-HT1A receptor, which partly explains its antidepressant activity. (http://onlinelibrary.wiley.com/doi/10.1002/syn.8
Lithium also increases BDNF levels, which helps with depression.
Lithium partially alleviates depression in animals by increasing the number of neural stem cells.
9. Lithium has potential use in the treatment of Huntington's disease
Lithium prevents nerve cell death in animal models of Huntington's disease (https://www.ncbi.nlm.nih.gov/pubmed/11591460, https://www.ncbi.nlm.nih.gov/pubmed/14702090).
Lithium reduces excess NMDA receptor function, and thus may potentially counteract the increased NMDA receptor activation that occurs in the brains of patients with Huntington's disease (https://www.ncbi.nlm.nih.gov/pubmed/21492946).
Research into patients with Huntington's disease is ongoing.![]()
10. Lithium reduces insulin resistance
Lithium improves insulin-stimulated glucose transport and glycogen synthesis in insulin-resistant rat muscle rat muscle (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC26339thirty/). These effects depend on p38 MAPK (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2633930/).
Lithium reduces insulin release (https://www.ncbi.nlm.nih.gov/pubmed/369819).
The use of lithium significantly increased glucose transport into muscle cells by 2.5 times in response to insulin administration and also increased insulin sensitivity (https://www.ncbi.nlm.nih.gov/pubmed/8013755).
11. Lithium has a positive effect on autoimmune diseases and reduces inflammation
Lithium has shown strong immune system activation effects (https://www.ncbi.nlm.nih.gov/pubmed/15236914/, https://www.ncbi.nlm.nih.gov/pubmed/12208183).
Lithium, by inhibiting GSK-3, has been noted to have a beneficial effect in animal models of autoimmune disease. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3532311/)
(https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3532311/)
Lithium inhibits the activity of Th2 cells and interferon-gamma (but not Th27 cells). (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3532311/)
Lithium has anti-inflammatory effects by decreasing the production of IL-1β and TNF-α, and increasing the production of IL-2, TGF, IL-1RA and IL-10 (http://www.if-pan.krakow.pl/pjp/pdf/ 2003/3_353.pdf, https://www.ncbi.nlm.nih.gov/pubmed/10367558).
However, studies have also shown that, under certain experimental conditions, lithium also has pro-inflammatory effects by increasing the production of IL-4, IL-6 and TNF-α (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4063502 /).
Lithium increases IgG and IgM antibody levels (https://www.sciencedirect.com/science/article/pii/009825).
Lithium reduces the production and activity of prostaglandins, thus preventing their negative effect on the immune system (https://www.sciencedirect.com/science/article/pii/0006295274

Lithium reduces the frequency and duration of recurrent infections of labial and genital herpes, and also reduces the frequency of colds (https://www.ncbi.nlm.nih.gov/pubmed/2155671, https://jhu.pure.elsevier.com/ en/publications/suppression-of-recurrent-genital-herpes-infections-wit...).
12. Lithium has a positive effect on bone tissue
A comparative study was conducted to assess the bone density of the hip and lumbar spine in 75 volunteers who received lithium and 75 healthy volunteers who did not receive lithium; groups were normalized for age, sex, and body mass index. The study found lower rates of bone remodeling in volunteers who received lithium. Mean bone mineral density in lithium-treated volunteers was 4.5% higher at the spine, 5.3% higher at the femoral neck, and 7.5% higher at the trochanter of the femur (https://www.ncbi .nlm.nih.gov/pubmed/18992857).
Lithium use is associated with a reduced risk of bone fractures and increased osteogenesis , https://www. ncbi.nlm.nih.gov/pmc/articles/PMC1297659/).
ncbi.nlm.nih.gov/pmc/articles/PMC1297659/).
13. Lithium can be helpful in restoring our circadian rhythm
As you know, lithium is the standard of care for the treatment of patients suffering from bipolar disorder, which is characterized by the presence of episodes of mania and depression.
One mechanism by which lithium may help with bipolar disorder is by lengthening the circadian rhythm. People with bipolar disorder tend to have a shorter circadian rhythm compared to 24 hours.
Lithium promotes a faster recovery of our circadian rhythm in response to light and darkness (http://geum.ru/next/art-91286.php).
14. Lithium improves mitochondrial function
Lithium increased the lifespan of roundworms (nematodes) and improved overall health outcomes, including mitochondrial energy production (https://www.ncbi.nlm.nih.gov/pubmed/24398558).
Lithium may improve mitochondrial function by increasing the rate of replacement of broken mitochondria (https://www. ncbi.nlm.nih.gov/pubmed/24398558).
ncbi.nlm.nih.gov/pubmed/24398558).
Lithium also inhibits mir-34a, which in turn inhibits NAMPT, an enzyme involved in the formation of NAD+ (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3172812/#R39, https://en .wikipedia.org/wiki/Nicotinamide_phosphoribosyltransferase). Therefore, lithium likely increases free NAD+ levels.
15. Low doses of lithium increase life expectancy
The researchers found a positive correlation between life expectancy and lithium levels in drinking water. There has been a decrease in the risk of death from all diseases in areas of Japan with higher lithium levels.
Similar was noted in the situation with roundworms (nematodes). Long-term low-dose lithium exposure can delay aging and clearly reduce mortality in evolutionarily distinct species (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3151375/). The improvement in health status was accompanied by improved mitochondrial function. (https://www. ncbi.nlm.nih.gov/pubmed/24398558)
ncbi.nlm.nih.gov/pubmed/24398558)
16. Lithium may improve symptoms of Tourette's syndrome
Tourette's syndrome is a neurological disorder characterized by involuntary muscle movements and uncontrolled vocal sounds (https://www.nhs.uk/conditions/tourettes-syndrome/).
In a small study of 3 patients, lithium resulted in a better outcome than haloperidol, a common drug prescribed for Tourette's syndrome. In patients who took lithium, there was a significant decrease in the number of tics and involuntary speech sounds. Patients had no side effects and were symptom-free for several months (https://www.ncbi.nlm.nih.gov/pubmed/27089four).
17. Lithium may be useful in cases of tardive dyskinesia
Tardive dyskinesia is a neurological disorder characterized by sudden, involuntary, jerky movements of the face and/or body that occur with long-term use of psychotropic drugs (https://www. ninds.nih.gov/Disorders/All-Disorders/Tardive-Dyskinesia- Information-Page).
ninds.nih.gov/Disorders/All-Disorders/Tardive-Dyskinesia- Information-Page).
Studies have shown that lithium significantly reduced the severity of tardive dyskinesia (https://www.sciencedirect.com/science/article/pii/S0924977X07001496, https://www.ncbi.nlm.nih.gov/pubmed/788002, https://www.ncbi.nlm.nih.gov/pubmed/804260).
Lithium reduced arousal and aggression, and reduced involuntary movements (https://www.ncbi.nlm.nih.gov/pubmed/788002, https://www.ncbi.nlm.nih.gov/pubmed/804260).
However, two large studies found no consistent effects of lithium on tardive dyskinesia (https://www.ncbi.nlm.nih.gov/pubmed/7
, https://www.karger.com/Article/Abstract/117629).
18. Lithium helps to cope with obsessive-compulsive behavior
Obsessive-compulsive disorder (OCD), or obsessive-compulsive disorder, is a mental disorder characterized by obsessive thoughts and behavior (https://www.nimh.nih.gov/health/topics/obsessive-compulsive-disorder-ocd/index. shtml).
shtml).
The addition of lithium to the diet results in a reduction in OCD symptoms resistant to standard therapy (https://www.ncbi.nlm.nih.gov/pubmed/6435460).
Compulsive and pathological gamblers have also shown a good response to dietary lithium supplementation, which may regulate dopamine imbalance in the brain (https://www.ncbi.nlm.nih.gov/pubmed/20588072).
19. Lithium can relieve headaches
Lithium can reduce the severity of both chronic and episodic cluster headache (http://scielo.isciii.es/scielo.php?pid=S0213-616320000006&script=sci_arttext).
Lithium carbonate taken before bed helped eliminate "hypnic headache" (headache that older people suffer from waking up at the same time at night) (https://www.ncbi.nlm.nih.gov/pmc/ articles/PMC1891726/, http://pn.bmj.com/content/practneurol/5/3/144.full.pdf).
20. Lithium may be effective in treating anorexia nervosa
Patients suffering from anorexia nervosa for many years have been successfully treated with lithium carbonate (https://www. ncbi.nlm.nih.gov/pubmed/842388, https://www.ncbi.nlm.nih.gov/pubmed /6801096).
ncbi.nlm.nih.gov/pubmed/842388, https://www.ncbi.nlm.nih.gov/pubmed /6801096).
One patient gained 12 kg and the other 9 kg within 6 weeks, and the weight gain on lithium therapy was maintained for a year (https://www.ncbi.nlm.nih.gov/pubmed/842388).
However, further studies of lithium are required to evaluate its utility in the treatment of anorexia nervosa.
21. Lithium may be effective in treating alcoholism
Lithium orotate is used to treat alcoholism.
The drug has been shown to be safe, with minimal side effects such as muscle weakness, loss of appetite, or mild lethargy (https://www.ncbi.nlm.nih.gov/pubmed/3718672).
Lithium carbonate promotes alcohol abstinence, reduces subjective withdrawal symptoms, and delays time to first alcohol consumption (https://jamanetwork.com/journals/jamapsychiatry/article-abstract/494005, https://www.ncbi.nlm.nih.gov /pubmed/181193).
Patients treated with lithium were less likely to be rehospitalized for alcohol rehabilitation during 18 months of follow-up (https://www. ncbi.nlm.nih.gov/pubmed/2494686).
ncbi.nlm.nih.gov/pubmed/2494686).
22. Lithium may reduce seizure frequency
Data on the effect of lithium on seizure frequency is still controversial (https://www.ncbi.nlm.nih.gov/pubmed/3379144).
Some patients with epilepsy show a statistically significant reduction in seizure frequency as well as behavioral improvement with lithium treatment (https://jamanetwork.com/journals/jamapsychiatry/article-abstract/490891).
Lithium can be used to control treatment-resistant temporal lobe epilepsy.
However, some patients with epilepsy have experienced an increase in the number of seizures during lithium treatment (https://www.healio.com/psychiatry/journals/psycann/2013-6-43-6/%7B0346b54f-2ca1-4215-8d9e-10708601ad..., http://www.academia.edu/6195616/Non-convulsive_status_epilepticus_during_lithium_treatment_at_therap..., https://neuro.psychiatryonline.org/doi/full/10.1176/jnp.11.3.414).
23. Lithium may relieve symptoms of Meniere's disease
Lithium may relieve symptoms of Meniere's disease
Meniere's disease is an ear disease that causes severe dizziness, tinnitus, hearing loss, and a feeling of fullness in the ear (https://www.mayoclinic.org/diseases-conditions/menieres-disease/symptoms-causes/syc-203749ten).
In 70% of patients with Ménière's disease, a decrease in the frequency and severity of seizures was observed during lithium treatment (http://www.tandfonline.com/doi/abs/10.3109/00016487409126326?journalCode=ioto20&).
However, in a study involving patients who received lithium and placebo for 6 months, there was no difference between the two groups (https://www.ncbi.nlm.nih.gov/pubmed/790893).
Additional information
• Lithium reduces brain levels of inositol (https://www.nature.com/articles/newbio233267a0).
• Lithium increases vasopressin, which stimulates ACTH and cortisol (http://journals.plos.org/plosone/article?id=10. 1371/journal.pone.0027613).
1371/journal.pone.0027613).
Genetic factors that influence lithium sensitivity
Serotonin transporter 5-HTTLPR (SLC6A4)
Patients with 2 copies of the short form of this gene respond less well to lithium treatment than patients with the long form of the gene (https://www.nature.com/articles/6500006).
Corresponding allele: The presence of rs25531 may indicate the long form of the gene.
GSK3beta -50T/C
These mutations are responsible for the variability in responses to lithium in patients with bipolar disorder, although the results are not uniform (https://www.ncbi.nlm.nih.gov/pubmed/14729229, https://www.ncbi.nlm. nih.gov/pubmed/15694273, https://www.ncbi.nlm.nih.gov/pubmed/16861141)
The C allele is associated with a more improved response to lithium supplemented antidepressants (https://www.ncbi.nlm.nih.gov/pubmed/17628506).
Journal of the RAS
Artificial Societies
artsoc. jes.su
jes.su
The electronic scientific and educational journal "Artificial Societies", acting as an analogue of the English-language journal Journal of Artificial Societies and Social Simulation (JASSS), is the most convenient platform for publishing works not only on the topic of artificial societies , but also scientific articles of a wider profile.
Show more
Asia and Africa Today
asaf-today.ru
Publishes scientific articles about political, economic and social processes taking place in Asian and African states, about their culture, art and literature.
Show more
Chelovek
chelovek-journal.ru
The journal “Chelovek” is a scientific publication that publishes the results of the study of man in the social, humanitarian and natural sciences in close connection with the understanding of man in philosophy, which initially seeks to answer the question “What is a man?” . The journal is open to various intellectual traditions and theoretical platforms. Works that develop complex studies of man at the intersection of sciences are especially welcome. The articles of the journal are addressed to the interdisciplinary readership. Along with research articles, the journal publishes analytical reviews of discussions and scientific conferences, polemical essays, and book reviews.
Works that develop complex studies of man at the intersection of sciences are especially welcome. The articles of the journal are addressed to the interdisciplinary readership. Along with research articles, the journal publishes analytical reviews of discussions and scientific conferences, polemical essays, and book reviews.
Show more
Digital Orientalia
do.jes.su
"Digital Orientalia" (Digital Oriental Studies) is an international scientific periodical that reflects a wide range of problems in the development of modern oriental studies and the humanities.
Show more
Eastern Analyticscs
analitika.jes.su
Eastern Analytics has been published since 2010. The journal is aimed at analyzing economic, social and political processes in the modern East.
Show more
Ekonomika i matematicheskie metody
emm.jes.su
The journal Economics and Mathematical Methods positions itself as an open platform for international communication and exchange of scientific information, results of fundamental and applied research of academic and expert-analytical specialists. The journal strives to maintain a high scientific level of discussion about the problems, methods of studying and developing the economy, involving the most qualified experts in this process - researchers and practitioners.
The journal strives to maintain a high scientific level of discussion about the problems, methods of studying and developing the economy, involving the most qualified experts in this process - researchers and practitioners.
Show more
Energy law forum
mlcjournal.ru
The purpose of the journal is to improve the quality of coverage of the main results of dissertations and create the basic conditions for fulfilling the requirements of the Higher Attestation Commission of the Ministry of Education and Science of Russia for scientific publications of applicants for scientific degrees of candidates and doctors of legal sciences (5.1 .2, 5.1.3, 5.1.5)
Show more
Epistema
epistema.jes.su/
Epistema magazine is a unique communication platform for scientific discussions, where young scientists and well-known researchers in the field of philosophy, social sciences and human sciences meet. At the center of these discussions lies the understanding of knowledge as a phenomenon of culture in its various aspects and research contexts.
At the center of these discussions lies the understanding of knowledge as a phenomenon of culture in its various aspects and research contexts.
Show more
Etnograficheskoe obozrenie
"Ethnographic Review" is one of the oldest Russian academic journals devoted to research in the sciences of peoples. Founded in 1889The journal specializes primarily in the publication of articles on ethnography, ethnology and social/cultural anthropology, as well as reviews and reviews of scientific literature in these areas.
Show more
Eurasia. Expert
journal.eurasia.expert
Electronic scientific journal “Eurasia. Expert” is an online periodical dedicated to the scientific analysis of political, economic and humanitarian processes in the Eurasian region.
Show more
Gosudarstvo i pravo
gospravo-journal.ru
The journal covers: theoretical issues of state and law; problems of the formation of the rule of law; human and civil rights and freedoms; analysis of new legislation; chronicle of scientific life.
Show more
Indo-European linguistics and classical philology
iling.jes.su
Yearbook "Indo-European Linguistics and Classical Philology" is a periodical published by the Institute of Linguistic Studies of the Russian Academy of Sciences since 1998 The publication is a registered media. Certificate number: PI No. FS 77–60970.
Show more
ISTORIYA
history.jes.su
The electronic scientific and educational journal "History" (ENOSH "History") is a unique online periodical publication that contains scientific and educational articles by leading domestic and foreign historians, reflecting the results of modern research .
Show more
Izvestiia Rossiiskoi academii nauk. Seriia literatury i iazyka
izv-oifn.ru
The journal covers the problems of linguistics and literary criticism, folklore, art history, theory of literature and the history of Russian and foreign literature.
Show more
Journal of Foreign Legislation and Comparative Law
jzsp.jes.su
The Journal of Foreign Legislation and Comparative Law is aimed at scholars and practitioners involved in the problems of legal regulation.
Show more
Journal of Russian Law
jrp.jes.su
The general concept of the Journal reflects the nature, level and diversity of domestic doctrinal research, the main trends in the development of certain branches of legislation, Russian experience, which served as the starting point for synthesizing new ideas and discoveries in the field of legal science .
Show more
Journal of the Institute of Oriental Studies RAS
vestnik-ivran.jes.su
The journal publishes original scientific articles in all areas of Oriental studies: history, archeology, culture, economics, politics, linguistics and linguistics of the countries of the East from antiquity to the present day. The main goal of publishing the journal is to inform the scientific community about new results and achievements made by the staff of the Institute of Oriental Studies of the Russian Academy of Sciences.
The main goal of publishing the journal is to inform the scientific community about new results and achievements made by the staff of the Institute of Oriental Studies of the Russian Academy of Sciences.
Show more
Latin America
latamerica-journal.ru
Journal "Latinskaya Amerika" is a full-fledged multidisciplinary professional publication in Russian, unique for Russia and the CIS, analyzing topical theoretical, scientific and practical problems of Ibero-America; - gives readers a broad panorama of the Ibero-American world, prints exclusive interviews of heads of state, ministers, politicians, diplomats, parliamentarians and public figures, prominent representatives of science, business, culture and art, works of world famous writers from Latin America, Spain and Portugal.
Show more
Law & Digital Technologies
ldt-journal.com
Law & Digital Technologies (LDT) is a peer-reviewed and interdisciplinary journal dedicated to advancing the dialogue between legal scholars and computer scientists. This journal publishes innovative theoretical and methodological research dedicated to digital technologies such as Blockchain, Artificial Intelligence, BigData, etc. LDT is looking for papers within the subject area that display good quality legal analysis or new lines of legal thought that go beyond mere description of Law, however accurate that may be. It also welcomes research in the field of theoretical computer science, applied mathematics and informatics, aimed at the development of scientific and methodological foundations of convergent cognitive-information technologies. The journal especially fosters interdisciplinary approaches.
This journal publishes innovative theoretical and methodological research dedicated to digital technologies such as Blockchain, Artificial Intelligence, BigData, etc. LDT is looking for papers within the subject area that display good quality legal analysis or new lines of legal thought that go beyond mere description of Law, however accurate that may be. It also welcomes research in the field of theoretical computer science, applied mathematics and informatics, aimed at the development of scientific and methodological foundations of convergent cognitive-information technologies. The journal especially fosters interdisciplinary approaches.
Show more
Linguistica Fundamentalis
linguistica-fundamentalis.jes.su
The journal "Fundamental Linguistics" / "Linguistica Fundamentalis" is designed to draw special attention of researchers in the field of linguistics and related fields of knowledge to the theoretical understanding of the identified and described features of the languages of the world.
Show more
Man and Education
man and education.rf
The Man and Education periodical has been published since 2005.
Founder: Institute of Education Management of the Russian Academy of Education
Editorial staff: St. Petersburg Branch of the Institute of Education Management of the Russian Academy of Education
Show more
Metamorphoses of History
history-metamorph.ru
The electronic scientific journal "Metamorphoses of History" is an online periodical that publishes scientific articles by leading domestic and foreign historians. The materials of the journal are intended not only for specialists, but also for all those interested in issues of world and national history.
Show more
Mirovaia ekonomika i mezhdunarodnye otnosheniia
The monthly journal “Mirovaya ekonomika i mezhdunarodnye otnosheniia” was founded in 1956 and published since January 1957. It is the leading multidisciplinary publication in Russia and the CIS on topical theoretical, scientific and practical problems of international politics, world economic relations, development of individual countries and regions.
It is the leading multidisciplinary publication in Russia and the CIS on topical theoretical, scientific and practical problems of international politics, world economic relations, development of individual countries and regions.
Show more
Nauka.me
nauka.me
Nauka.me, an electronic scientific and educational journal, is an online periodical that brings together young researchers in the field of social sciences and the humanities. The main goal of the journal is to create an accessible platform for the publication of scientific works of young scientists, bachelors and masters of both Russian and foreign scientific and educational organizations.
Show more
Novaia i noveishaia istoria
nni.jes.su
The journal publishes articles by leading Russian and foreign historians on the political, economic and social processes taking place in the countries of Western and Eastern Europe, the USA, Canada and Latin American countries. Much attention is paid to the history, foreign policy of the leading countries of Asia and Africa.
Much attention is paid to the history, foreign policy of the leading countries of Asia and Africa.
Show more
Obshchestvennye nauki i sovremennost
ons-journal.ru
The journal discusses the following issues: the economy, society, politics, culture of Russia; construction of a general scientific picture of the world; features and prospects of transformation processes; synergetics and methodology of social science; perspectives of man and world civilization; regional studies and modernization processes; international relations.
Show more
Obshchestvo i ekonomika
oie.jes.su
Society and Economics is an international scientific and socio-political journal dedicated to the economic, political and social processes taking place in post-socialist countries.
Show more
Oiental Epigraphy
epigraphy.jes.su
The journal “Epigraphics of the East” publishes original scientific articles on Eastern source studies, epigraphy, numismatics, original historical philological and linguistic studies of already published epigraphic materials, reviews and reviews of new publications containing archeographic and epigraphic expeditions, as well as those devoted to the description and study of material and epigraphic monuments of the East.
Show more
Oriental courier
oriental-courier.ru
Oriental courier is conceived as a platform for discussing problems of a wide range of politics, economics, practical oriental studies, field research, "scientific travels", questions of cultural studies, art history, philology, history of the East and history oriental studies.
Show more
Orientalistica
orientalistica.com
Orientalistica ("Orientalistica") is a scientific peer-reviewed publication covering a wide range of areas of oriental studies.
Show more
Polylogos
polylogos-journal.ru
Polylog/Polylogos is a scientific and theoretical publication published four times a year and aimed at a professional audience. The objective of the journal is to publish the results of research in the field of political science, philosophy of politics and philosophy of history.
Show more
Problemy Dalnego Vostoka
pdv. jes.su
jes.su
The journal provides its readers with an opportunity to get acquainted with the history, culture, politics and economy of the Asia-Pacific countries, to follow the development of international cooperation in this dynamic and strategically world economy - China and Japan - as well as the rapidly growing India, Vietnam and other ASEAN countries, include Siberia and the Russian Far East with their enormous potential.
Show more
Psikhologicheskii zhurnal
psy.jes.su
The journal publishes articles on the fundamental problems of psychology, its methodological, theoretical and experimental foundations, as well as the results of research related to applied issues of social and scientific life. Discussions on the pages of the journal contribute to the identification of general trends in the development of psychology and its convergence with practice.
Show more
Pskov Journal of Regional Studies
prj. pskgu.ru
pskgu.ru
The journal presents the results of scientific research aimed at analyzing the political, economic, social, demographic, ethno-cultural and environmental problems of the development of various regions of Russia and foreign countries. In addition, the tasks of the journal include consideration of the theory and methodology of complex and "sectoral" regional studies, as well as the identification of regional specifics by studying the features of the historical and geographical development of territories.
Show more
Publishing House of the Institute of Oriental Studies of the RAS
izd.ivran.ru
The Publishing Center of the Institute of Oriental Studies of the Russian Academy of Sciences publishes original scientific articles in all areas of Oriental studies: history, archeology, culture, economics, politics, linguistics and linguistics of the countries of the East from antiquity to the present day.
Show more
Rossiiskaia arkheologiia
The journal has more than 50 years of existence. The journal is aimed at professional scientists - archaeologists, historians of material culture, art and architecture. As a fundamental scientific publication, the journal accepts for publication only original author's works (articles, short notes, book reviews , a chronicle of ongoing scientific forums
The journal is aimed at professional scientists - archaeologists, historians of material culture, art and architecture. As a fundamental scientific publication, the journal accepts for publication only original author's works (articles, short notes, book reviews , a chronicle of ongoing scientific forums
Show more
Rossiiskaia istoriia
russian-history.ru
Scientific journal publishing materials on history, historiography and methods of historical research. The journal covers all areas of study of the Russian historical process from antiquity to the present, and encourages interdisciplinary and comparative approaches. The priority of the journal is the publication of original materials based on the introduction of new sources into scientific circulation and written taking into account the latest domestic and foreign historiography. The journal also pays great attention to the professional discussion of new scientific publications (monographs, collections of articles and academic publications of sources), which is carried out both in the format of reviews (the department of criticism and bibliography is the largest of all similar departments of Russian historical periodicals), and in the heading "Dialogue about the book. "
"
Show more
Russia and America in the 21st century
rusus.jes.su
The Russia and America in the 21st century journal is an online periodical that collects scientific and educational articles by leading domestic and foreign historians, reflecting the results of modern research.
Show more
Russian Journal of Bilingualism Studies
bilingualism.ru
Russian Journal of Bilingualism Studies is an international interdisciplinary journal for the study of bilingualism in various fields and scientific schools of linguistics, psycho- and sociolinguistics, literary criticism, cultural studies, pedagogy, psychology and sociology.
Show more
Russkaia literatura
On the pages of the magazine the reader gets acquainted with the works devoted to folk art, the literature of Old Russian and the 18th century, the classical heritage, the literature of the newest period (20th century). Theoretical, historical and literary research coexists in it with biographical and textological research, thematic headings related to the anniversaries of classical writers, critical reviews, polemics, attributions, extensive information about current scientific life based on the materials of numerous international conferences.
Theoretical, historical and literary research coexists in it with biographical and textological research, thematic headings related to the anniversaries of classical writers, critical reviews, polemics, attributions, extensive information about current scientific life based on the materials of numerous international conferences.
Show more
Russkaya Rech’
Popular science academic journal about the Russian language (about its history and current state), about Russian culture and literature
Show more
Scientific and Analytical Herald of IE RAS
The journal publishes the results of research in the field of economic, social, political and spiritual life of European society; bibliographic reviews and reviews, as well as information about scientific conferences.
Show more
Slavianovedenie
slav.jes.su
Thematic articles, materials of discussions, round tables, documents, critical reviews, bibliography, chronicle of scientific life, information about books published by the Institute of Slavic Studies, etc. are published.
are published.
Show more
Sotsiologicheskie issledovaniya
The journal publishes articles on the entire spectrum of sociological science: theory, methodology and history of sociology, methods and results of sociological research in the field of economic, social, political and spiritual life of society both in Russia and abroad. Among the leading rubrics are ethnosociology, sociology of culture, family, education, science, religion, government, law, youth, demography and migration. New headings - "Historical Sociology", "Sociology of Health and Medicine", "Sociology of International Relations", "Sociology of Professions".
Show more
Sovremennaya Evropa
Modern Europe is an academic scientific publication published by the Institute of Europe of the Russian Academy of Sciences (http://www.instituteofeurope.ru) since 2000 and is a social and political research journal recognized in Russia and in the world. Frequency: six times a year. The journal "Modern Europe" publishes materials on economics, sociology, political science, international relations, history. is included in the List of Russian peer-reviewed scientific journals of the Higher Attestation Commission of the Russian Federation, in which the main scientific results of dissertations for the scientific degrees of doctor and candidate of sciences should be published.
Frequency: six times a year. The journal "Modern Europe" publishes materials on economics, sociology, political science, international relations, history. is included in the List of Russian peer-reviewed scientific journals of the Higher Attestation Commission of the Russian Federation, in which the main scientific results of dissertations for the scientific degrees of doctor and candidate of sciences should be published.
Show more
Studies in Transcendental Philosophy
transcendental.su
The thematic orientation of the journal is connected, first of all, with transcendental philosophy (in the narrow sense), which includes the transcendental philosophy of I. Kant, neo-Kantianism, [transcendental] phenomenology, modern Kant studies.
Show more
Ural-Altaic Studies
ural-altai.ru
The journal "Ural-Altai Studies" is oriented, first of all, to the interests of linguists - specialists in the languages of the Ural and Altai communities. We expect that we will be able to attract as authors those historians, ethnographers, literary critics (as well as representatives of other sciences) who are interested in exchanging information with linguists.
We expect that we will be able to attract as authors those historians, ethnographers, literary critics (as well as representatives of other sciences) who are interested in exchanging information with linguists.
Show more
USA & Canada: ekonomika, politika, culture
usacanada.jes.su
USA & Canada: Economics, Politics, Culture was founded in 1970 as USA: Economics, Politics, Ideology (with Canada added since 1998). Its main goal was and remains to inform readers about all aspects of the domestic and foreign policy of the United States and Canada, as well as topical theoretical and practical problems of international politics, world economic relations, and development in different countries of the world. The journal publishes materials presenting the results of research by Russian specialists and foreign analysts on Russian-American and Russian-Canadian relations.
Show more
Vestnik CEMI
cemi. jes.su
jes.su
Scientific electronic quarterly journal Vestnik CEMI is a unique online periodical that publishes works of a high scientific level on reviewing and preparing materials, which is provided by the staff of the Central Economics and Mathematics Institute of the Russian Academy of Sciences.
Show more
Vestnik drevnei istorii
The journal publishes original scientific articles on all areas of ancient history, classical and ancient Eastern philology and archeology of ancient and ancient Eastern civilizations, in Russian, English, French and German.
Show more
Voprosy istorii estestvoznaniia i tekhniki
vietmag.org
The main block of journal materials consists of original articles in which qualified specialists in the history and philosophy of science and technology publish the results of their research. The journal is published under the direction of the Presidium of the Russian Academy of Sciences.