Elisabeth kubler ross 5 stages of grieving
5 stages of grief: What they are and how to get through them
CNN —
When someone you love dies, the world as you’ve known it is totally upended.
One way people cope, added psychologist Sherry Cormier, is by trying to find some sort of certainty. This need for structure is probably one factor behind the popularity that latched onto the “five stages of grief” over 50 years ago and hasn’t yet let up, said David Kessler, who founded grief.com, a resource aiming to help people deal with uncharted territory related to grief. Kessler coauthored “On Grief and Grieving” with the late Dr.
Elisabeth Kübler-Ross.
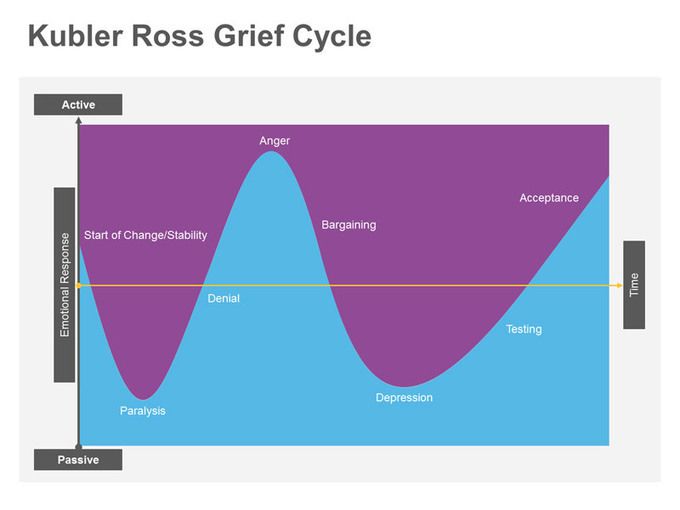
A Swiss American psychiatrist and pioneer of studies on dying people, Kübler-Ross wrote “On Death and Dying,” the 1969 book in which she proposed the patient-focused, death-adjustment pattern, the “Five Stages of Grief.” Those stages are denial, anger, bargaining, depression and acceptance.
“In the actual book, she talked about more than five stages,” Kessler said. “Think about the context of 1969 – doctors and hospital personnel were not talking about the end-of-life process. … Elisabeth really hoped ‘On Death and Dying’ would start the conversation.”
Since then, there has been extensive media coverage of the five stages; use in television shows including “Grey’s Anatomy” and “House”; clinician support; and criticism. Those five stages are what people clung to, Kessler said.
Those five stages are what people clung to, Kessler said.
Grief and psychology experts and academics have criticized the framework for not being thoroughly supported by research, suggesting that the bereaved move through grief sequentially or implying one correct way to grieve. But these suggestions weren’t Kübler-Ross’ intentions, and she stated these caveats on the first page of the book, Kessler said.
While there’s debate among experts about the stages of grief, “people who are in the pain of grief are just saying, ‘Help me,’” Kessler said. Here’s what the five stages of grief are, and how you can consider and process them in whichever order you experience them.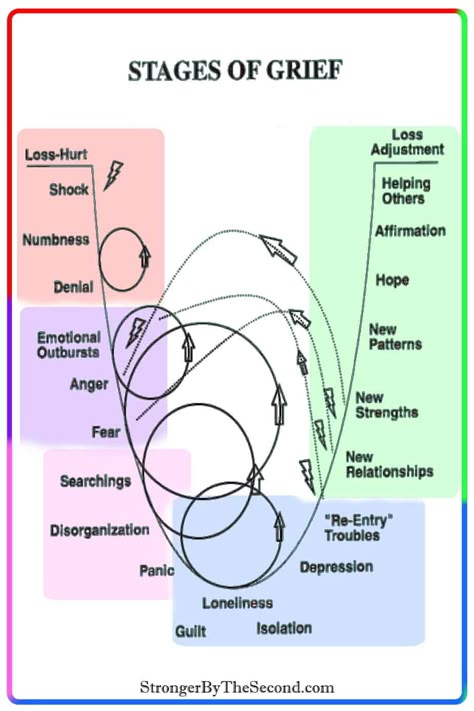
In denial there is grace, in that we can’t fully register the total pain, shock and disbelief over our loss in one moment or day, so the pain is spread over time, Kessler said.
Grief isn't linear, as you might experience each stage within one moment, out of order or cyclically.
Getty ImagesWhile denial in a literal and dysfunctional sense would be trying to convince yourself your loved one isn’t dead, an inability to comprehend the loss for a while is healthy – not something you need to quickly snap out of, he added.
If you’re struggling with overwhelming denial, you can try to stop fighting the reality you’ve been presented with, said Cormier, who is also a bereavement trauma specialist and consultant.
Anger is another natural reaction to loss, whether it’s anger at the cause of death, the deceased, the god of your religion, yourself or the randomness of the universe, Kessler said.
“Anger is pain’s bodyguard. It’s how we express pain,” he said. “That stage gives people permission to be angry in healthy ways, and to know it’s not bad.”
Courtesy of Museo Reina Sofia, Madrid
The art of processing our collective grief
Anger “can be an anchor, giving temporary structure to the nothingness of loss. At first grief feels like being lost at sea: no connection to anything,” according to Kessler’s website. “Then you get angry at someone, maybe a person who didn’t attend the funeral, maybe a person who isn’t around, maybe a person who is different now that your loved one has died. Suddenly you have a structure – your anger toward them.”
At first grief feels like being lost at sea: no connection to anything,” according to Kessler’s website. “Then you get angry at someone, maybe a person who didn’t attend the funeral, maybe a person who isn’t around, maybe a person who is different now that your loved one has died. Suddenly you have a structure – your anger toward them.”
Beneath anger can be feelings of hopelessness or powerlessness, Cormier said, sometimes prompting guilt and blame that some people use to maintain an illusion of control or express frustration.
“Our minds would always rather feel guilty than helpless,” Kessler said.
Depending on how your loved one died, one way to overcome guilt- and blame-related anger is by realizing that as horrific as your loss is, it wasn’t personally done to you, Kessler said.
“The reality is the death rate in families is 100%,” he said. “Everyone is going to die eventually, but our minds just can’t fathom that.”
Allow yourself to express anger in healthy ways, Kessler advised, whether it’s “grief yoga,” screaming in your car, using a punching bag, running or other forms of exercise.
Often also stemming from guilt, bargaining after a loss typically involves “if only” statements, focused on regrets about what you did or didn’t do before the person died, Kessler said.
Shutterstock
Grief-induced anxiety: Calming the fears that follow loss
“We may even bargain with the pain. We will do anything not to feel the pain of this loss,” Kessler’s site says. “People often think of the stages as lasting weeks or months. They forget that the stages are responses to feelings that can last for minutes or hours as we flip in and out of one and then another. ”
”
Remember that we live in a world where sometimes bad things happen despite our best efforts, Kessler said.
Depression, or an acute sadness, is when the great loss begins more deeply affecting your life. Maybe the sadness feels as if it will last forever, or you’ve withdrawn from life or are wondering if life is worth living alone.
Sadness hits people at different times, Cormier said. She has known people who aren’t distraught in the first year after loss, but by year three are consumed with sadness.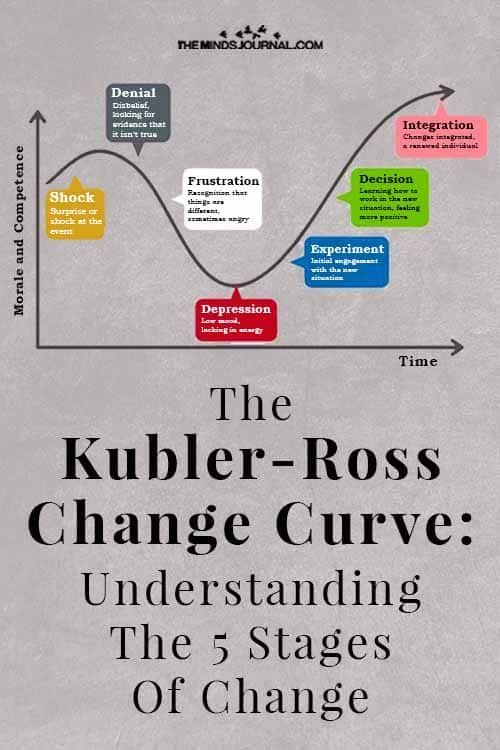 Why? Because for a time, some can maintain the illusion that their loved one is away on vacation and may be returning, she said.
Why? Because for a time, some can maintain the illusion that their loved one is away on vacation and may be returning, she said.
Overcoming Depression: Facts and Resources
Often, the eventual, deep sadness “is really an expression of, ‘my loved one is gone and not coming back,’” Cormier said.
But those feelings shouldn’t always be labeled as clinical depression, Kessler said. If you think you’re depressed around a death, see a psychiatrist for an evaluation, he advised.
If you think you’re depressed around a death, see a psychiatrist for an evaluation, he advised.
To cope with sadness, you can also seek support from friends, family or grief support groups, and regularly practice self-care, Cormier suggested.
Acceptance doesn’t mean you’re OK with your loved one being gone. “It just means that I now accept the new reality of my life. I’m a widow, I live alone. I don’t have siblings to call up anymore. I don’t have parents to call up anymore,” said Cormier, who wrote “Sweet Sorrow: Finding Enduring Wholeness After Grief and Loss” after losing her husband and immediate family.
Acceptance isn’t grief’s end, either. You might have many little moments of acceptance over time, Kessler said, such as when you plan and attend the funeral.
“One of the questions I get asked most is, ‘When will this grief be over?’” Kessler added. “Very gently, I’ll ask, ‘How long is the person going to be dead? Because if the person is going to be dead for a long time, you’re going to grieve for a long time. It doesn’t mean you will always grieve with pain. To me, the goal of grief work is to eventually remember the person with more love than pain.”
Courtesy Ruedi Habegger
My friend chose an assisted death in Switzerland.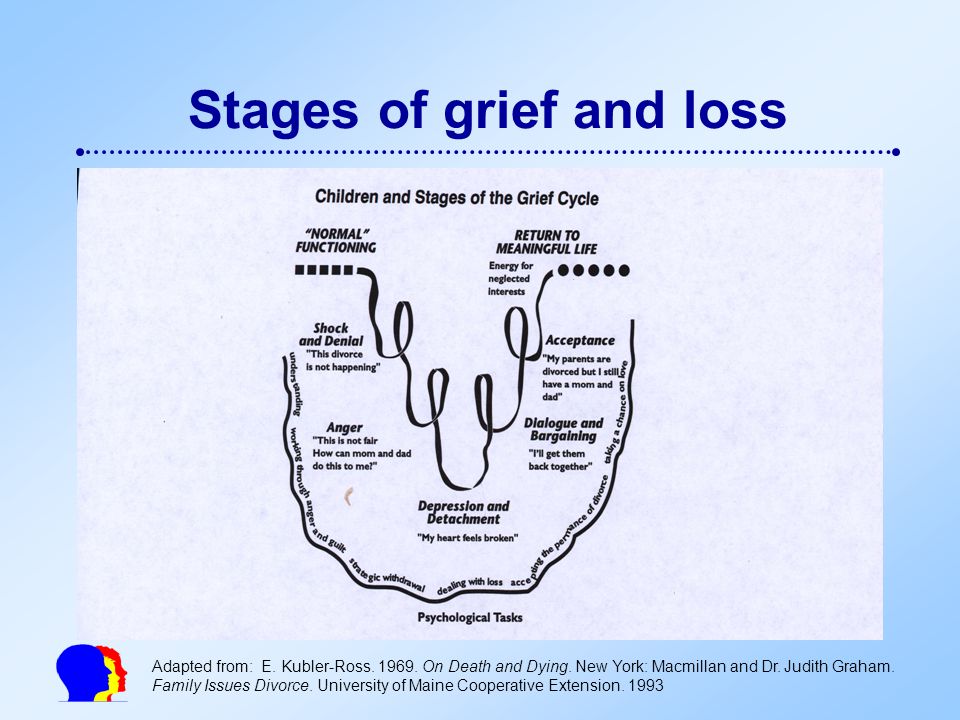 Her dying wish was to tell you why
Her dying wish was to tell you why
Arriving at acceptance means you’re healing, Cormier said. But if you can’t get there, you need to seek professional help. Intense and persistent grief that causes problems and interferes with everyday functioning, in a way that typical grief doesn’t after some time has passed, is known as prolonged grief disorder, according to the American Psychiatric Association. The disorder is the newest disorder to be added to the revised Diagnostic and Statistical Manual of Mental Disorders released in March.
To be diagnosed with prolonged grief disorder, a loved one’s death had to have occurred at least a year prior for adults, and at least six months ago for children and adolescents, according to the association, which publishes the DSM. One symptom is difficulty with reintegration, such as pursuing interests or interacting with friends.
One symptom is difficulty with reintegration, such as pursuing interests or interacting with friends.
Cormier doesn’t think we ever “get over” grief. Our task is different than moving on – it’s learning to integrate the loss into our lives so that we can move forward with a new reality, she added. “It’s sort of offensive to grievers to say, ‘Oh, you’ve really moved on.’ No, I don’t think grievers move on. We move forward.”
After Kessler’s son died at age 21 nearly five years ago, Kessler wanted something beyond acceptance. He had studied late neurologist, psychiatrist and philosopher Dr. Viktor Frankl’s work on meaning, and wondered how meaning related to grief – which inspired his book “Finding Meaning: The Sixth Stage of Grief. ”
”
Meaning didn’t eliminate Kessler’s pain, but it did cushion it, he said.
Meaning is in what we later do or realize as the bereaved people, Kessler explained. Maybe you recognize the fragility of life, try to change a law or donate money to research so no one dies the way your loved one did, or make a change in your life.
Sign up for CNN’s Stress, But Less newsletter. Our six-part mindfulness guide will inform and inspire you to reduce stress while learning how to harness it.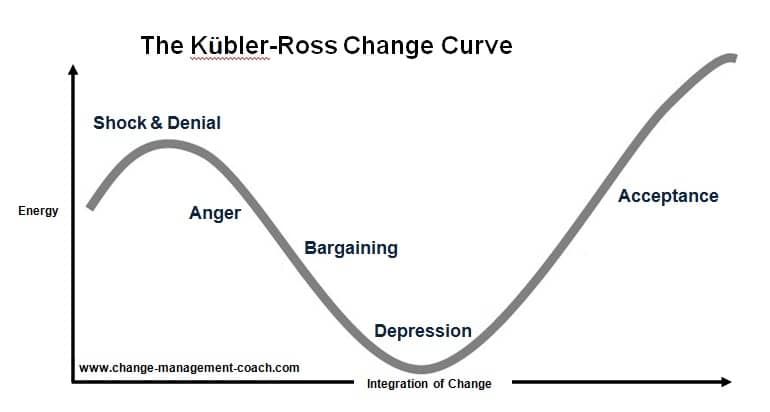
Five Stages of Grief by Elisabeth Kubler Ross & David Kessler
A Message from David Kessler
I was privileged to co-author two books with the legendary, Elisabeth Kübler-Ross, as well as adapt her well-respected stages of dying for those in grief. As expected, the stages would present themselves differently in grief. In our book, On Grief and Grieving we present the adapted stages in the much needed area of grief. The stages have evolved since their introduction and have been very misunderstood over the past four decades. They were never meant to help tuck messy emotions into neat packages. They are responses to loss that many people have, but there is not a typical response to loss as there is no typical loss.
The five stages, denial, anger, bargaining, depression and acceptance are a part of the framework that makes up our learning to live with the one we lost. They are tools to help us frame and identify what we may be feeling.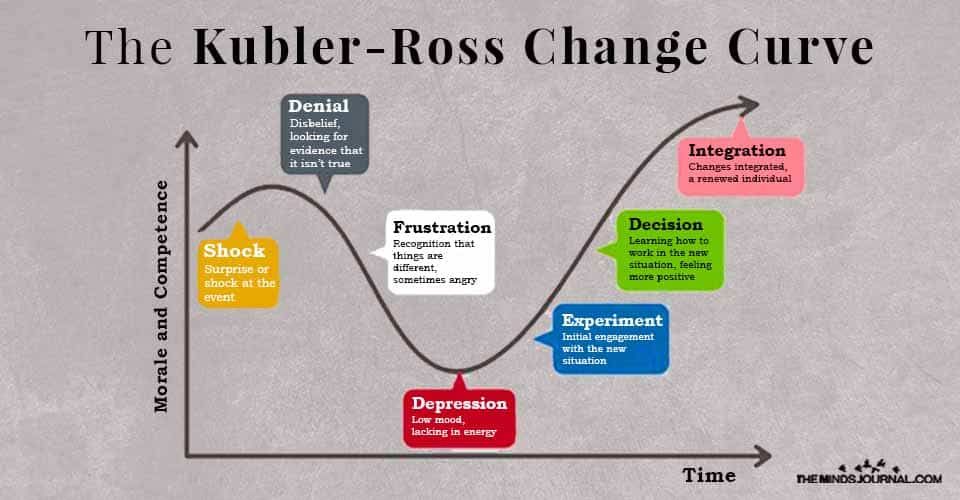 But they are not stops on some linear timeline in grief. Not everyone goes through all of them or in a prescribed order. Our hope is that with these stages comes the knowledge of grief ‘s terrain, making us better equipped to cope with life and loss. At times, people in grief will often report more stages. Just remember your grief is an unique as you are.
But they are not stops on some linear timeline in grief. Not everyone goes through all of them or in a prescribed order. Our hope is that with these stages comes the knowledge of grief ‘s terrain, making us better equipped to cope with life and loss. At times, people in grief will often report more stages. Just remember your grief is an unique as you are.
NEW BOOK
Finding Meaning: The Sixth Stage of Grief
In this groundbreaking new work, David Kessler—an expert on grief and the coauthor with Elisabeth Kübler-Ross of the iconic On Grief and Grieving—journeys beyond the classic five stages to discover a sixth stage: meaning.
In this book, Kessler gives readers a roadmap to remembering those who have died with more love than pain; he shows us how to move forward in a way that honors our loved ones. Kessler’s insight is both professional and intensely personal. His journey with grief began when, as a child, he witnessed a mass shooting at the same time his mother was dying.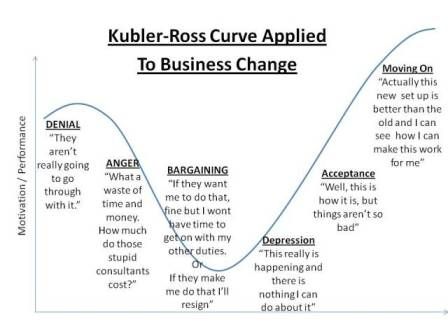 For most of his life, Kessler taught physicians, nurses, counselors, police, and first responders about end of life, trauma, and grief, as well as leading talks and retreats for those experiencing grief. Despite his knowledge, his life was upended by the sudden death of his twenty-one-year-old son.
For most of his life, Kessler taught physicians, nurses, counselors, police, and first responders about end of life, trauma, and grief, as well as leading talks and retreats for those experiencing grief. Despite his knowledge, his life was upended by the sudden death of his twenty-one-year-old son.
How does the grief expert handle such a tragic loss? He knew he had to find a way through this unexpected, devastating loss, a way that would honor his son. That, ultimately, was the sixth state of grief—meaning. In Finding Meaning, Kessler shares the insights, collective wisdom, and powerful tools that will help those experiencing loss. Read More
DENIAL Denial is the first of the five stages of grief™️. It helps us to survive the loss. In this stage, the world becomes meaningless and overwhelming. Life makes no sense. We are in a state of shock and denial. We go numb. We wonder how we can go on, if we can go on, why we should go on. We try to find a way to simply get through each day. Denial and shock help us to cope and make survival possible. Denial helps us to pace our feelings of grief. There is a grace in denial. It is nature’s way of letting in only as much as we can handle. As you accept the reality of the loss and start to ask yourself questions, you are unknowingly beginning the healing process. You are becoming stronger, and the denial is beginning to fade. But as you proceed, all the feelings you were denying begin to surface.
Denial and shock help us to cope and make survival possible. Denial helps us to pace our feelings of grief. There is a grace in denial. It is nature’s way of letting in only as much as we can handle. As you accept the reality of the loss and start to ask yourself questions, you are unknowingly beginning the healing process. You are becoming stronger, and the denial is beginning to fade. But as you proceed, all the feelings you were denying begin to surface.
ANGERAnger is a necessary stage of the healing process. Be willing to feel your anger, even though it may seem endless. The more you truly feel it, the more it will begin to dissipate and the more you will heal. There are many other emotions under the anger and you will get to them in time, but anger is the emotion we are most used to managing. The truth is that anger has no limits. It can extend not only to your friends, the doctors, your family, yourself and your loved one who died, but also to God. You may ask, “Where is God in this? Underneath anger is pain, your pain. It is natural to feel deserted and abandoned, but we live in a society that fears anger. Anger is strength and it can be an anchor, giving temporary structure to the nothingness of loss. At first grief feels like being lost at sea: no connection to anything. Then you get angry at someone, maybe a person who didn’t attend the funeral, maybe a person who isn’t around, maybe a person who is different now that your loved one has died. Suddenly you have a structure – – your anger toward them. The anger becomes a bridge over the open sea, a connection from you to them. It is something to hold onto; and a connection made from the strength of anger feels better than nothing.We usually know more about suppressing anger than feeling it. The anger is just another indication of the intensity of your love.
It is natural to feel deserted and abandoned, but we live in a society that fears anger. Anger is strength and it can be an anchor, giving temporary structure to the nothingness of loss. At first grief feels like being lost at sea: no connection to anything. Then you get angry at someone, maybe a person who didn’t attend the funeral, maybe a person who isn’t around, maybe a person who is different now that your loved one has died. Suddenly you have a structure – – your anger toward them. The anger becomes a bridge over the open sea, a connection from you to them. It is something to hold onto; and a connection made from the strength of anger feels better than nothing.We usually know more about suppressing anger than feeling it. The anger is just another indication of the intensity of your love.
BARGAININGBefore a loss, it seems like you will do anything if only your loved one would be spared. “Please God, ” you bargain, “I will never be angry at my wife again if you’ll just let her live. ” After a loss, bargaining may take the form of a temporary truce. “What if I devote the rest of my life to helping others. Then can I wake up and realize this has all been a bad dream?” We become lost in a maze of “If only…” or “What if…” statements. We want life returned to what is was; we want our loved one restored. We want to go back in time: find the tumor sooner, recognize the illness more quickly, stop the accident from happening…if only, if only, if only. Guilt is often bargaining’s companion. The “if onlys” cause us to find fault in ourselves and what we “think” we could have done differently. We may even bargain with the pain. We will do anything not to feel the pain of this loss. We remain in the past, trying to negotiate our way out of the hurt. People often think of the stages as lasting weeks or months. They forget that the stages are responses to feelings that can last for minutes or hours as we flip in and out of one and then another. We do not enter and leave each individual stage in a linear fashion.
” After a loss, bargaining may take the form of a temporary truce. “What if I devote the rest of my life to helping others. Then can I wake up and realize this has all been a bad dream?” We become lost in a maze of “If only…” or “What if…” statements. We want life returned to what is was; we want our loved one restored. We want to go back in time: find the tumor sooner, recognize the illness more quickly, stop the accident from happening…if only, if only, if only. Guilt is often bargaining’s companion. The “if onlys” cause us to find fault in ourselves and what we “think” we could have done differently. We may even bargain with the pain. We will do anything not to feel the pain of this loss. We remain in the past, trying to negotiate our way out of the hurt. People often think of the stages as lasting weeks or months. They forget that the stages are responses to feelings that can last for minutes or hours as we flip in and out of one and then another. We do not enter and leave each individual stage in a linear fashion. We may feel one, then another and back again to the first one.
We may feel one, then another and back again to the first one.
DEPRESSIONAfter bargaining, our attention moves squarely into the present. Empty feelings present themselves, and grief enters our lives on a deeper level, deeper than we ever imagined. This depressive stage feels as though it will last forever. It’s important to understand that this depression is not a sign of mental illness. It is the appropriate response to a great loss. We withdraw from life, left in a fog of intense sadness, wondering, perhaps, if there is any point in going on alone? Why go on at all? Depression after a loss is too often seen as unnatural: a state to be fixed, something to snap out of. The first question to ask yourself is whether or not the situation you’re in is actually depressing. The loss of a loved one is a very depressing situation, and depression is a normal and appropriate response. To not experience depression after a loved one dies would be unusual. When a loss fully settles in your soul, the realization that your loved one didn’t get better this time and is not coming back is understandably depressing.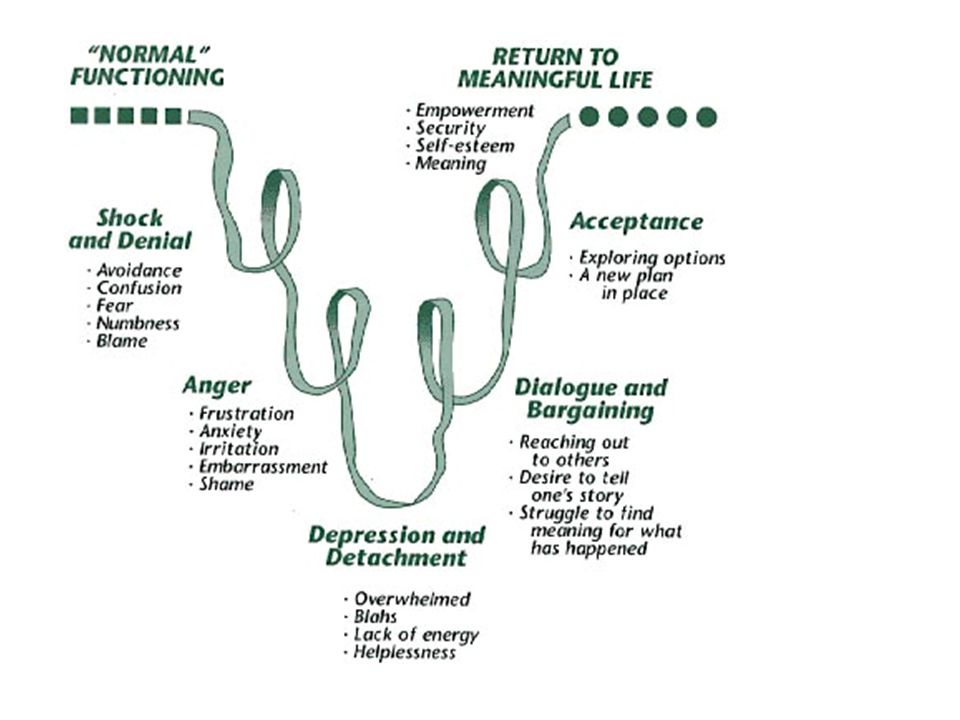 If grief is a process of healing, then depression is one of the many necessary steps along the way.
If grief is a process of healing, then depression is one of the many necessary steps along the way.
ACCEPTANCEAcceptance is often confused with the notion of being “all right” or “OK” with what has happened. This is not the case. Most people don’t ever feel OK or all right about the loss of a loved one. This stage is about accepting the reality that our loved one is physically gone and recognizing that this new reality is the permanent reality. We will never like this reality or make it OK, but eventually we accept it. We learn to live with it. It is the new norm with which we must learn to live. We must try to live now in a world where our loved one is missing. In resisting this new norm, at first many people want to maintain life as it was before a loved one died. In time, through bits and pieces of acceptance, however, we see that we cannot maintain the past intact. It has been forever changed and we must readjust. We must learn to reorganize roles, re-assign them to others or take them on ourselves. Finding acceptance may be just having more good days than bad ones. As we begin to live again and enjoy our life, we often feel that in doing so, we are betraying our loved one. We can never replace what has been lost, but we can make new connections, new meaningful relationships, new inter-dependencies. Instead of denying our feelings, we listen to our needs; we move, we change, we grow, we evolve. We may start to reach out to others and become involved in their lives. We invest in our friendships and in our relationship with ourselves. We begin to live again, but we cannot do so until we have given grief its time.
Finding acceptance may be just having more good days than bad ones. As we begin to live again and enjoy our life, we often feel that in doing so, we are betraying our loved one. We can never replace what has been lost, but we can make new connections, new meaningful relationships, new inter-dependencies. Instead of denying our feelings, we listen to our needs; we move, we change, we grow, we evolve. We may start to reach out to others and become involved in their lives. We invest in our friendships and in our relationship with ourselves. We begin to live again, but we cannot do so until we have given grief its time.
Learn More About The Five Areas of Grief
Watch The FREE Video Now Click Here
Books About the Five Stages by Elisabeth Kübler-Ross and David Kessler
Download Chapter One Click Here
Download Chapter One Click Here
Stages of acceptance of the disease - Pro Palliative
Content
Individual reaction of the patient
First stage: shock, denial
Second stage: anger and aggression
I worked as a psychologist in the service of cancer patients and their relatives for eight years, four of which I worked for eight years - on the hotline. I talked a lot with patients and their relatives, and I know firsthand what they have to deal with. It often happens that a person calls the hotline and says that his relative has changed a lot after he fell ill, and he does not understand how to communicate with him and what approach to choose. And the opposite situation, when the sick person calls and says that his family is turning away from him: “In a situation of illness, I feel completely alone, despite the fact that there are close people around me” . That is, the disease seems to create a barrier between people.
I talked a lot with patients and their relatives, and I know firsthand what they have to deal with. It often happens that a person calls the hotline and says that his relative has changed a lot after he fell ill, and he does not understand how to communicate with him and what approach to choose. And the opposite situation, when the sick person calls and says that his family is turning away from him: “In a situation of illness, I feel completely alone, despite the fact that there are close people around me” . That is, the disease seems to create a barrier between people.
There are a lot of classifications of reasons and difficulties in communication, but if we talk about the main reasons, there are actually two of them, and they are quite simple. On the one hand, this is a lack of understanding of the emotional state in which the sick person is: "I do not understand you, therefore we do not have mutual understanding." Moreover, there is an opposite situation, when it is difficult for a person to understand himself: “I don't understand what is happening to me.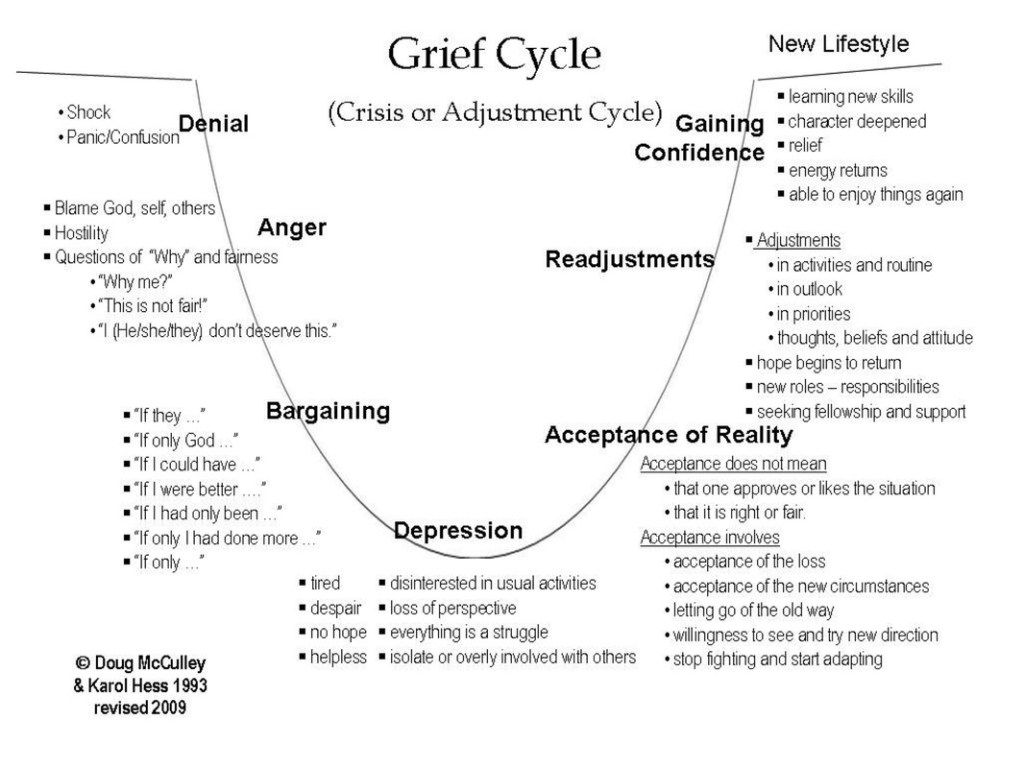 I don't understand why I react this way. I don’t understand what psychological processes are going on in me right now.”
I don't understand why I react this way. I don’t understand what psychological processes are going on in me right now.”
Individual patient response
Faced with a diagnosis, a person can experience five stages of response to illness - shock, anger, bargaining, depression, and acceptance. These stages were proposed by the physician and psychologist Elisabeth Kübler-Ross in her book On Death and Dying.
It is important to say that each person goes through all the stages differently, and there is no single way of responding for everyone. There is a general scheme according to which people, as a rule, give out certain psychological reactions. And when we try to completely transfer the scheme to a specific person, to our loved one, we can make mistakes if we do everything literally. Therefore, I urge you to always treat the person in front of you with understanding, and not literally shift this scheme.
It happens that a person has gone through a series of stages, and instead of moving to the next one, he returns to the previous one.
It happens that a person begins to move in a spiral. It happens that a person after the stage of depression again returns to the stage of anger and moves in a circle.
This, as a rule, indicates that he did not live something, did not receive something in this process. Of course, all stages of experience are necessary for a person. This is a normal reaction of the psyche to a crisis, to an abnormal situation, to a situation of illness.
First stage: shock, denial
This is the state that a person enters immediately after being told of the diagnosis. It can last from a few seconds or minutes to several hours.
Webinar: "Five stages of experiencing the disease" Psychologist Natalya Gorozhanina about what happens to a person when he learns about the diagnosis, how his psychological state changes at different stages of experiencing the disease and how to build communication at each of these stages.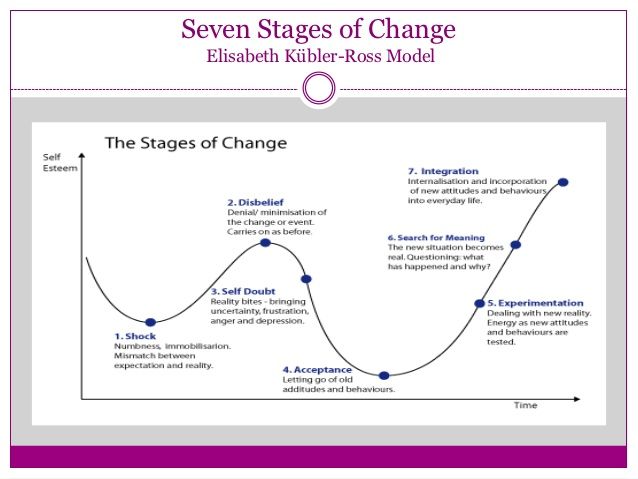
There are such folk expressions - “like a blow on the head with a butt” or “like snow on the head”. At this moment, a person has difficulty in contact with reality, that is, information is perceived "like a butt on the head." A person is characterized by a state of stupor of the psyche, a slight stupefaction.
When a person learns about a terrible diagnosis for him, the psyche naturally defends itself. In this condition, there is a risk of accidental injury. There were cases when a doctor reported a diagnosis to a person when there was no one near him, and the person went out into the street and crossed the road at a red light. Not because he wanted to commit suicide, but because he saw nothing, did not hear anything around him. And therefore it is not recommended, if possible, to leave a person alone in this state. But if you still leave it, then it is important to make sure that he is safe, that nothing bad can happen to him at the moment. It is also not recommended during this period to explain complex information to a person, speak in complex sentences and plan treatment regimens. And if it is very necessary to convey some information, then it is better to strive to do it as accessible as possible, in simple phrases and sentences.
And if it is very necessary to convey some information, then it is better to strive to do it as accessible as possible, in simple phrases and sentences.
Very often people at the stage of denial can say: “it can't be”, “it couldn't happen to me”, “it couldn't happen to my loved one”, “it's just impossible”. It is difficult for a person to believe what he has just learned.
The main risk at this stage is distrust of doctors and refusal of treatment. It happens that a person does not want to be treated, and we, his relatives, begin to argue, shout, try to convince and convey information almost by force. But doing this is highly discouraged, because a person may experience a backlash. If he is under pressure, he starts to defend himself : "No, I'm not going to the doctor for anything. And in general, leave me alone” . When you put in the first place the preservation of trust in a relationship, and not the task of convincing a person at all costs, then it will be easier for a person to decide on treatment.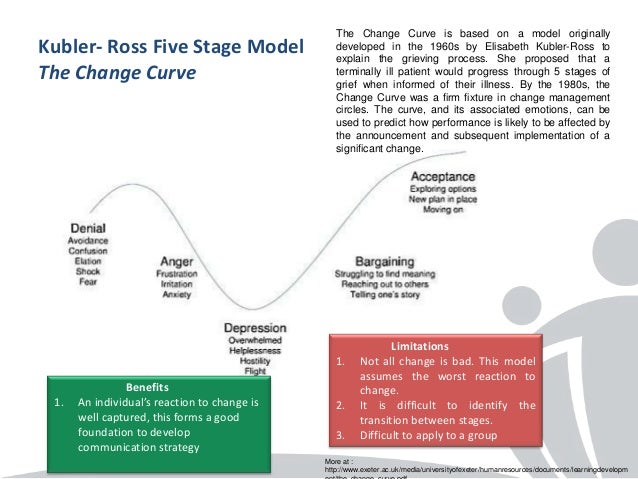
“It’s easier to tuck in the blanket than to talk to a person” What you need to know about the experiences of a seriously ill person and his relatives, and how to support each other
You need to emotionally support a person and give him at least a little time to perceive this information. It is very important to show warmth and care during this period. say "I'm here, next to you, we'll get through this together, I won't leave you, I love you very much and I really hope that everything will be fine." You can talk about your feelings: "I'm scared that you refuse to be treated, because I'm very afraid of the consequences of such a decision."
Second stage: anger and aggression
When a person begins to realize that he is ill, the second stage begins. This is the stage of the collapse of hopes and life plans. Very often people experience at this moment a feeling of acute injustice, very strong anger.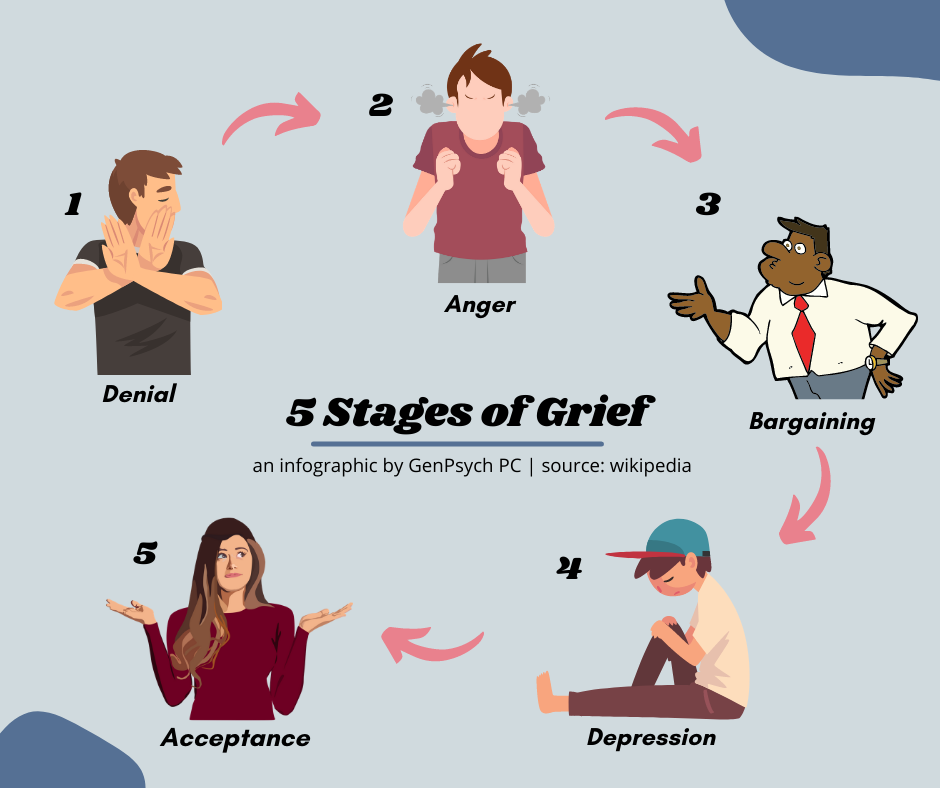 And this anger can be directed both outside - at loved ones, at doctors, at society as a whole, at God, at fate, at the world - and at oneself.
And this anger can be directed both outside - at loved ones, at doctors, at society as a whole, at God, at fate, at the world - and at oneself.
In fact, when the reaction goes outward, it is considered a normal reaction, despite the fact that it can lead to serious conflicts and relationship problems. A much more abnormal reaction is when a person directs aggression at himself.
Feelings of guilt can lead to this when a person says: “It's my own fault that I got sick. I did something wrong, I somehow lived the wrong way, I did something wrong, I did some things not in fairness” . Or says: "I didn't take care of my health enough" . And the risk of this self-accusation is that a person begins to destroy his inner resource, which could be used to fight the disease.
Therefore, if you see that your loved one blames himself for his illness, it is very important at this moment to support him as much as possible and help remove this feeling of guilt. Say that "it's not your fault that you got sick" . It could happen to absolutely anyone. Not a single person on earth - not a child, not an elderly person, not a person leading a healthy lifestyle, or, conversely, not a very healthy lifestyle - no one is immune from such a disease as oncology.
Say that "it's not your fault that you got sick" . It could happen to absolutely anyone. Not a single person on earth - not a child, not an elderly person, not a person leading a healthy lifestyle, or, conversely, not a very healthy lifestyle - no one is immune from such a disease as oncology.
Anger is a very large resource that can be used to treat and fight illness. Anger can be a support at this stage. It is a very big mistake to respond with anger to the anger of a person with a disease. Behind every aggression is pain. You need to support him, make it clear that you are there, that you are not against him, and help him redirect this anger from himself, from society, from doctors, to the disease itself. Sometimes it’s worth leaving a person alone for a while, letting him be alone with himself. But at the same time, always be available and explain that you can fight the disease together.
Read about the third, fourth and fifth stages in the continuation of the material: follow the link.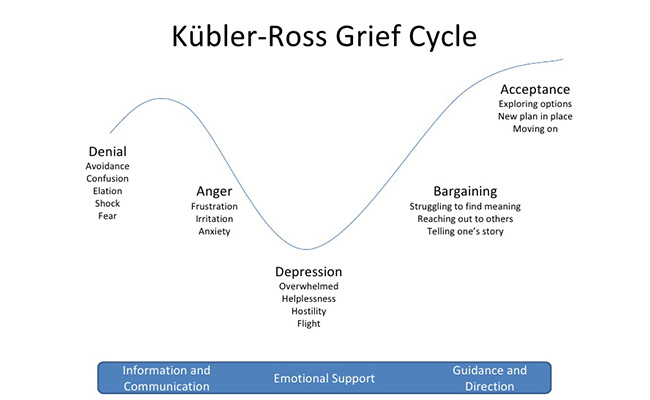
Five stages of grief. The Rise and Fall of Kübler-Ross
- Lucy Burns
- BBC
Image copyright Getty Images
Denial. Anger. Finding a compromise. Despair. Adoption. Many people know the theory according to which grief, when receiving unbearable information for a person, goes through these steps. The scope of its application is wide: from hospices to boards of directors of companies.
A recent interview with a psychologist in English on the Internet proves that the perception of the current quarantine is subject to the same rules. But do we all experience the same?
When Swiss psychiatrist Elisabeth Kübler-Ross began working in American hospitals in 1958, she was struck by the lack of methods of psychological care for dying patients.
- A method that can predict your death
"Everything was impersonal, attention was paid exclusively to the technical side of things," she told the BBC at 1983 year.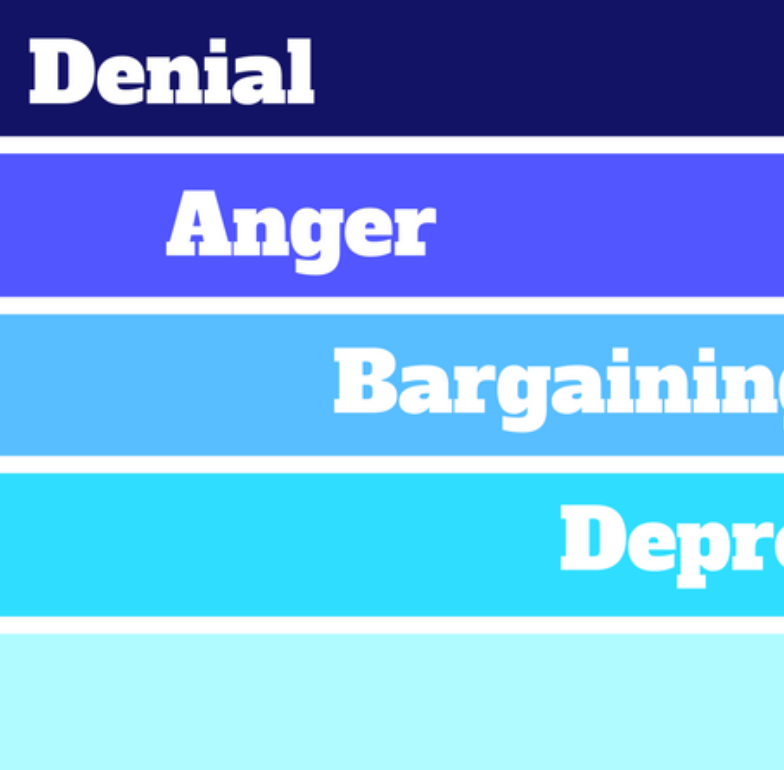 “Terminally ill patients were left to their own devices, no one talked to them.”
“Terminally ill patients were left to their own devices, no one talked to them.”
She started a seminar with Colorado State University medical students based on her conversations with cancer patients about what they thought and felt.
Author photo, LIFE/Getty Images
Photo caption,Elisabeth Kübler-Ross talks to a woman with leukemia in Chicago, 1969. Seminar participants observe through a special mirror glass
Despite the misunderstanding and resistance of a number of colleagues, soon there was nowhere for an apple to fall at the Kübler-Ross seminars.
In 1969 she published a book, On Death and Dying, in which she quoted typical statements from her patients, and then moved on to discuss how to help doomed people pass from life as free of fear and pain as possible.
Kübler-Ross described in detail the five emotional states that a person goes through after being diagnosed with a terminal diagnosis:
- Denial: "No, that can't be true"
- Anger: "Why me? Why? It's not fair!!!"
- Bargaining: "There must be a way to save myself, or at least improve my situation! I'll think of something, I'll behave properly and do whatever is necessary!"
- Depression: "There is no way out, everything is indifferent"
- Acceptance: "Well, we must somehow live with this and prepare for the last journey"
difficult situation.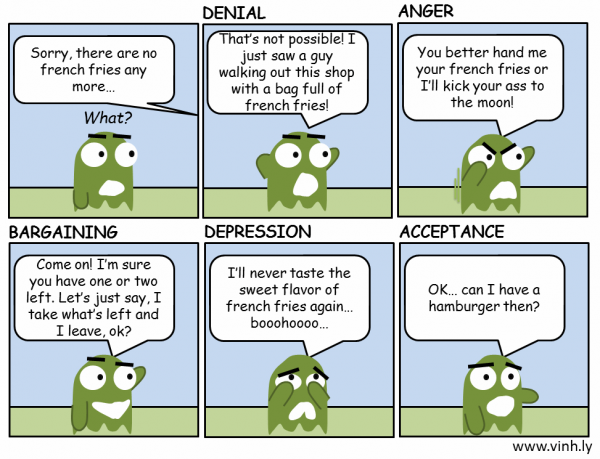
A separate chapter of the book is devoted to each of the stages. In addition to the five main ones, the author identified intermediate states - the first shock, preliminary grief, hope - from 10 to 13 types in total.
Image copyright Getty Images
Elisabeth Kübler-Ross died in 2004. Her son, Ken Ross, says she never insisted that every person must go through these five stages in sequence.
"It was a flexible framework, not a panacea for dealing with grief. If people wanted to use other theories and models, the mother did not object. She wanted to start a discussion of the topic first," he says.
- Last will: how did the photo of a dying American touch the world?
- "You hear everything, Fernando." How was the evening in honor of the terminally ill football player
The book "On Death and Dying" became a bestseller, and Elisabeth Kübler-Ross was soon inundated with letters from patients and doctors from all over the world.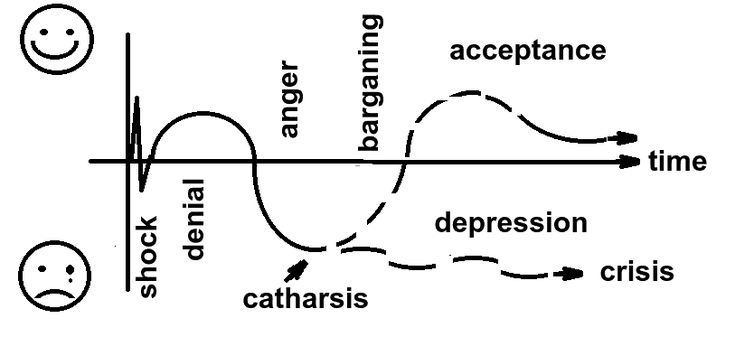
"The phone kept ringing, and the postman started visiting us twice a day," recalls Ken Ross.
The notorious five steps took on a life of their own. Following the doctors, patients and their relatives learned about them. They were mentioned by the characters of the series "Star Trek" and "Sesame Street". They were parodied in cartoons, they gave food for creativity to the mass of musicians and artists and gave rise to many successful memes.
Literally thousands of scientific papers have been written that have applied the theory of the five steps to a wide variety of people and situations, from athletes suffering career-incompatible injuries to Apple fans' worries about the release of the 5th iPhone.
Image copyright, Getty Images
Skip the Podcast and continue reading.
Podcast
What was that?
We quickly, simply and clearly explain what happened, why it is important and what will happen next.
episodes
The End of History Podcast
Kübler-Ross's legacy has found its way into corporate governance: big companies from Boeing to IBM (including the BBC) have used her "change curve" to help employees at times of great business change.
And during the coronavirus pandemic, it applies, says psychologist David Kessler.
Kessler worked with Elisabeth Kübler-Ross and co-authored her latest book, Grief and How We Grieve. His interview with the Harvard Business Review at the start of the pandemic garnered a lot of attention online as people everywhere searched for solutions to their emotional problems.
"And here, first comes denial: the virus is not terrible, nothing will happen to me. Then anger: who dares to deprive me of my usual life and force me to stay at home?! Then an attempt to find a compromise: okay, if after two weeks of social distancing it gets better, then why not? Followed by sadness: no one knows when it will end.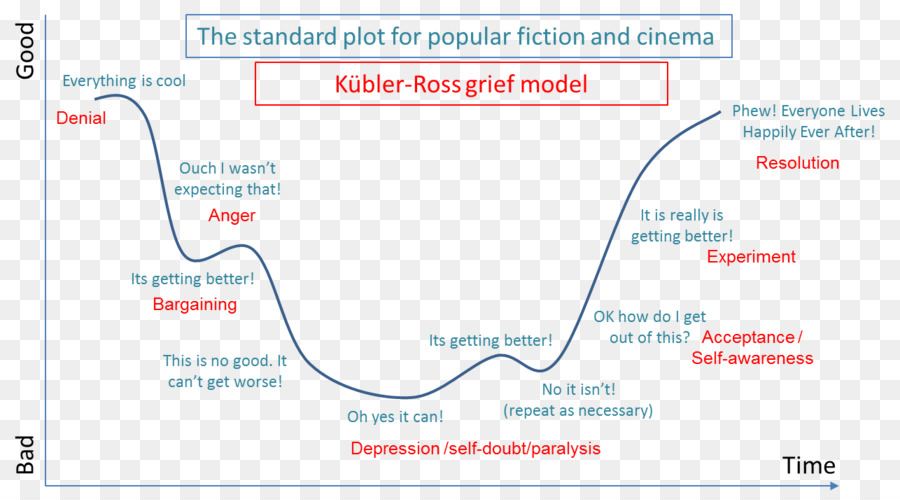 And, finally, acceptance: the world is now like this, you have to somehow live with it, "describes David Kessler.
And, finally, acceptance: the world is now like this, you have to somehow live with it, "describes David Kessler.
"As you can see, strength comes with acceptance. It gives you control: I can wash my hands, I can keep a safe distance, I can work from home," he says.
"It's a roadmap," says George Bonanno, professor of clinical psychology and head of the Loss, Trauma, and Emotion Laboratory at Columbia University. "When people are in pain, they want to know: How long will it last? What will happen to me? What do they need for something to grab on to. And the five-step model gives them that opportunity."
"This scheme is seductive," remarks Charles Corr, social psychologist and author of Death and Dying, Life and Being, "It offers an easy solution: sort everyone, and it takes no more than the fingers of one hand to label each one." .
George Bonanno sees this as a possible harm.
"People who don't fit exactly into these stages - and they are, in my observation, the majority - may decide that they are, so to speak, grieving wrong," he explains.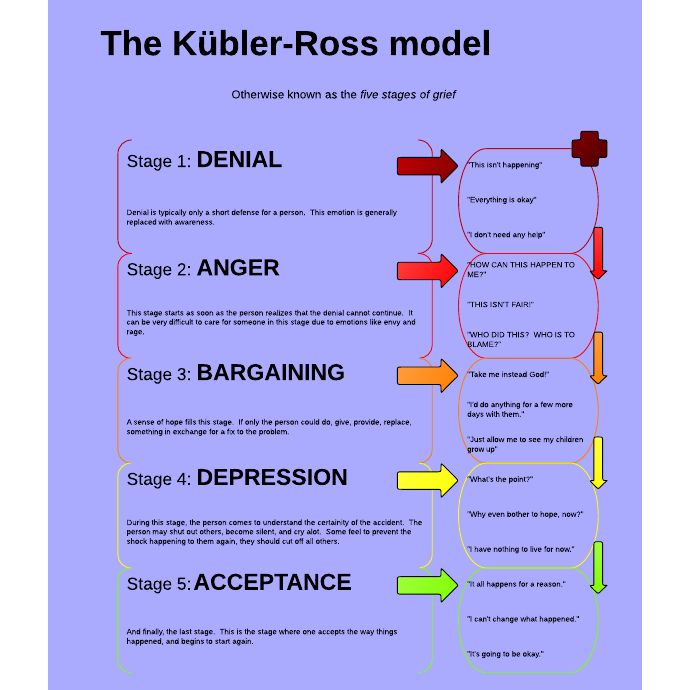
According to him, over the years he has seen many cases when people themselves inspired that they must certainly experience this and that, or they were convinced of this by friends and relatives, but they did not feel it and decided, that they need a doctor.
Experimental evidence of the existence of the five stages of grief is not enough. The longest and most extensive bereavement interview was conducted in 2007.
According to him, the most common state at any time is acceptance, only a few go through the stage of denial, and the second most common emotion is longing.
However, according to David Kessler, while scientists debate the nuances and terms, people who experience grief continue to find meaning in the Kübler-Ross scheme.
"I meet people who tell me, 'I don't know what's wrong with me. Now I'm angry, and a minute later I'm sad. I must be crazy.” And I say, “It has names. These are called the stages of grief.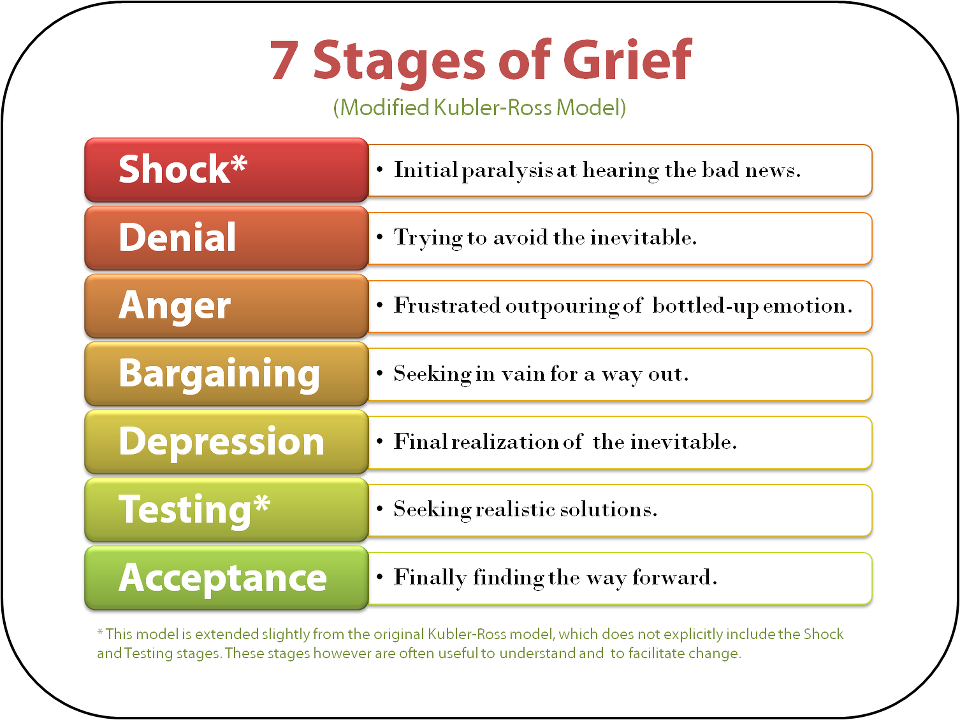 ” The person says, “Oh, so there is a special stage called 'anger'? It's about me!" And feels more normal."
” The person says, “Oh, so there is a special stage called 'anger'? It's about me!" And feels more normal."
Image copyright, Getty Images
"People need catchy language. If Kübler-Ross hadn't called it stages and stated that there are exactly five of them, then she would probably be closer to the truth. But then she would not attract to attention," says Charles Corr.
He believes that talking about the five stages distracts from the main scientific legacy of Elisabeth Kübler-Ross.
"She wanted to take up the topic of death and dying in the broadest sense: how to help terminally ill people come to terms with their diagnosis, how to help those who care for them, support these patients and cope with their own emotions, how to help everyone live a full life, realizing that we are not eternal,” says Charles Corr.
"The terminally ill can teach us everything: not only how to die, but also how to live," said Elisabeth Kübler-Ross at 1983 year.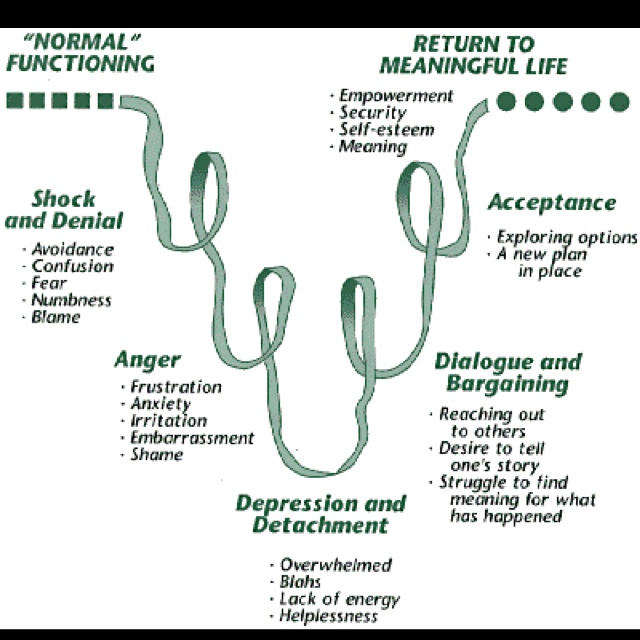
During the 1970s and 1980s, she traveled the world, lecturing and giving workshops to thousands of people. She was a passionate supporter of the hospice idea pioneered by British nurse Cecily Saunders.
Kübler-Ross has established hospices in many countries, the first in the Netherlands in 1999. Time magazine named her one of the 100 most important thinkers of the 20th century.
Professor Kübler-Ross' scientific reputation was shaken after she became fascinated with theories about the afterlife and began to experiment with mediums.
One of them, a certain Jay Barham, practiced non-standard religious-erotic therapy, in particular, he persuaded women to have sex, assuring that he was possessed by a person close to them from the afterlife. In 1979, because of this, a loud scandal arose.
In the late 1980s, she tried to set up a hospice for children with AIDS in rural Virginia, but faced strong local opposition to the idea.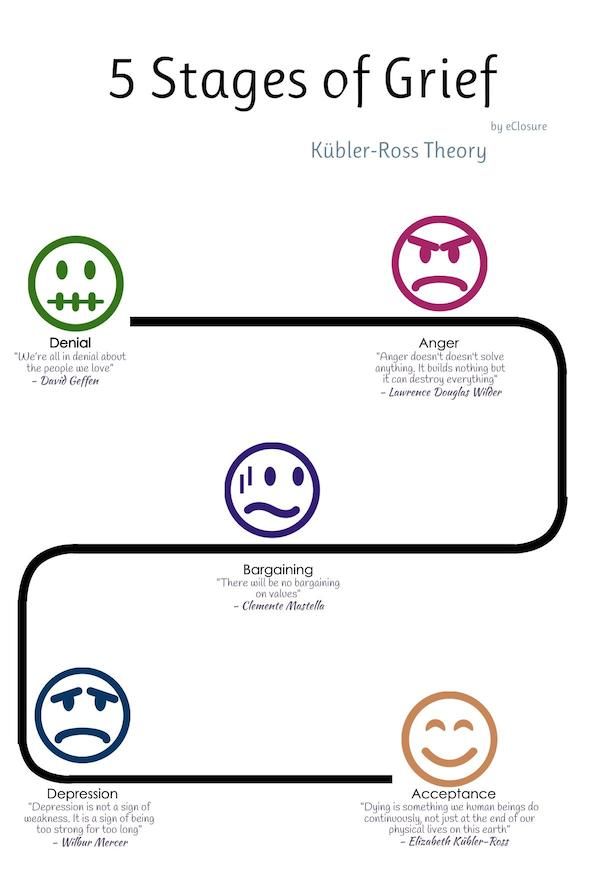
In 1995, her house caught fire under suspicious circumstances. The next day Kübler-Ross had her first stroke.
She spent the last nine years of her life with her son in Arizona, moving around in a wheelchair.
In her last interview with the famous TV presenter Oprah Winfrey, she said that at the thought of her own death she feels only anger.
"The public wanted the famed expert on death and dying to be some kind of angelic personality and quickly get to the stage of acceptance," says Ken Ross. "But we all deal with grief and loss as best we can."
The theory of the five stages of grief is not widely taught in medical schools these days. It is more popular at corporate trainings under the name "Curve of Change".
Since then, there have been many theories about how to deal with your grief.
David Kessler, with the consent of Kübler-Ross's family, added a sixth stage to the five: the understanding that everything that is done makes sense.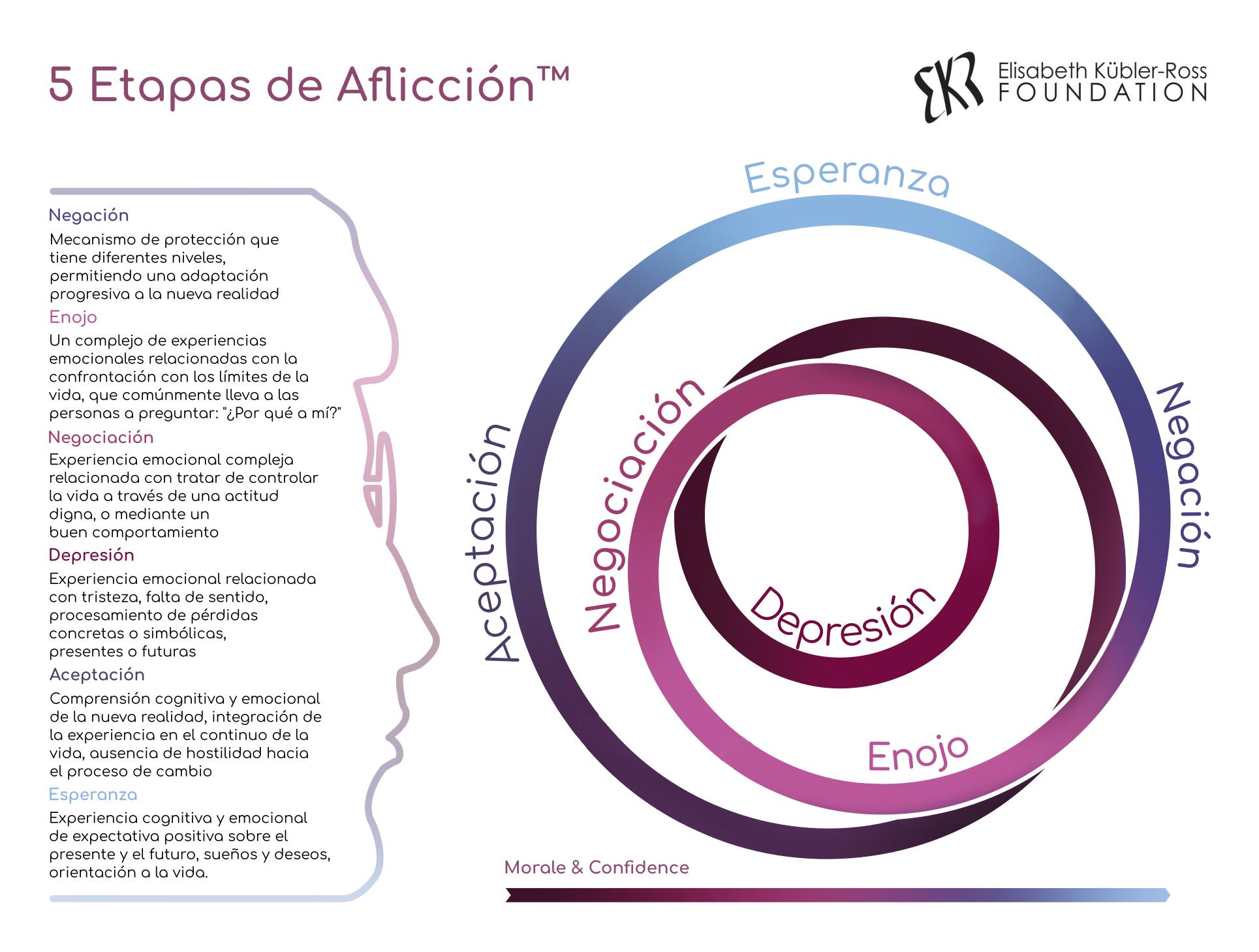
"Understanding can come in a million different ways. Let's say I've become a better person after losing a loved one. Maybe my loved one passed away in a different way than it should have happened, and I can try to make the world a better place to this has not happened to others," says David Kessler.
Charles Corr recommends the "double process model". It was developed by Dutch researchers Margaret Stroebe and Nenk Schut and suggests that a person in grief is simultaneously experiencing a loss and preparing himself for new things and life challenges.
George Bonanno talks about four trajectories of grief. Some people have great stamina and do not fall into depression, or it is weakly expressed in them, others remain morally broken for many years, others recover relatively close, but then a second wave of grief rolls over them, and finally, the fourth becomes stronger from the loss.
Over time, one way or another, it becomes easier for the vast majority.