Ptsd flare up
Post-traumatic stress disorder (PTSD) - Symptoms and causes
Overview
Post-traumatic stress disorder (PTSD) is a mental health condition that's triggered by a terrifying event — either experiencing it or witnessing it. Symptoms may include flashbacks, nightmares and severe anxiety, as well as uncontrollable thoughts about the event.
Most people who go through traumatic events may have temporary difficulty adjusting and coping, but with time and good self-care, they usually get better. If the symptoms get worse, last for months or even years, and interfere with your day-to-day functioning, you may have PTSD.
Getting effective treatment after PTSD symptoms develop can be critical to reduce symptoms and improve function.
Products & Services
- Book: Mayo Clinic Family Health Book, 5th Edition
- Newsletter: Mayo Clinic Health Letter — Digital Edition
Symptoms
Post-traumatic stress disorder symptoms may start within one month of a traumatic event, but sometimes symptoms may not appear until years after the event. These symptoms cause significant problems in social or work situations and in relationships. They can also interfere with your ability to go about your normal daily tasks.
PTSD symptoms are generally grouped into four types: intrusive memories, avoidance, negative changes in thinking and mood, and changes in physical and emotional reactions. Symptoms can vary over time or vary from person to person.
Intrusive memories
Symptoms of intrusive memories may include:
- Recurrent, unwanted distressing memories of the traumatic event
- Reliving the traumatic event as if it were happening again (flashbacks)
- Upsetting dreams or nightmares about the traumatic event
- Severe emotional distress or physical reactions to something that reminds you of the traumatic event
Avoidance
Symptoms of avoidance may include:
- Trying to avoid thinking or talking about the traumatic event
- Avoiding places, activities or people that remind you of the traumatic event
Negative changes in thinking and mood
Symptoms of negative changes in thinking and mood may include:
- Negative thoughts about yourself, other people or the world
- Hopelessness about the future
- Memory problems, including not remembering important aspects of the traumatic event
- Difficulty maintaining close relationships
- Feeling detached from family and friends
- Lack of interest in activities you once enjoyed
- Difficulty experiencing positive emotions
- Feeling emotionally numb
Changes in physical and emotional reactions
Symptoms of changes in physical and emotional reactions (also called arousal symptoms) may include:
- Being easily startled or frightened
- Always being on guard for danger
- Self-destructive behavior, such as drinking too much or driving too fast
- Trouble sleeping
- Trouble concentrating
- Irritability, angry outbursts or aggressive behavior
- Overwhelming guilt or shame
For children 6 years old and younger, signs and symptoms may also include:
- Re-enacting the traumatic event or aspects of the traumatic event through play
- Frightening dreams that may or may not include aspects of the traumatic event
Intensity of symptoms
PTSD symptoms can vary in intensity over time. You may have more PTSD symptoms when you're stressed in general, or when you come across reminders of what you went through. For example, you may hear a car backfire and relive combat experiences. Or you may see a report on the news about a sexual assault and feel overcome by memories of your own assault.
You may have more PTSD symptoms when you're stressed in general, or when you come across reminders of what you went through. For example, you may hear a car backfire and relive combat experiences. Or you may see a report on the news about a sexual assault and feel overcome by memories of your own assault.
When to see a doctor
If you have disturbing thoughts and feelings about a traumatic event for more than a month, if they're severe, or if you feel you're having trouble getting your life back under control, talk to your doctor or a mental health professional. Getting treatment as soon as possible can help prevent PTSD symptoms from getting worse.
If you have suicidal thoughts
If you or someone you know has suicidal thoughts, get help right away through one or more of these resources:
- Reach out to a close friend or loved one.
- Contact a minister, a spiritual leader or someone in your faith community.
- Call a suicide hotline number — in the United States, call the National Suicide Prevention Lifeline at 1-800-273-TALK (1-800-273-8255) to reach a trained counselor.
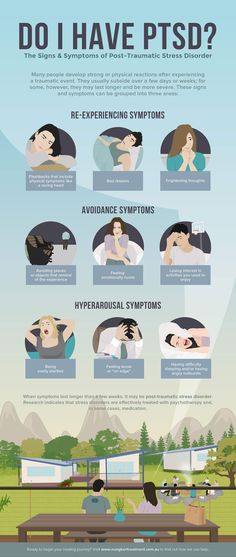 Use that same number and press 1 to reach the Veterans Crisis Line.
Use that same number and press 1 to reach the Veterans Crisis Line. - Make an appointment with your doctor or a mental health professional.
When to get emergency help
If you think you may hurt yourself or attempt suicide, call 911 or your local emergency number immediately.
If you know someone who's in danger of attempting suicide or has made a suicide attempt, make sure someone stays with that person to keep him or her safe. Call 911 or your local emergency number immediately. Or, if you can do so safely, take the person to the nearest hospital emergency room.
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which
information is beneficial, we may combine your email and website usage information with
other information we have about you. If you are a Mayo Clinic patient, this could
include protected health information. If we combine this information with your protected
health information, we will treat all of that information as protected health
information and will only use or disclose that information as set forth in our notice of
privacy practices. You may opt-out of email communications at any time by clicking on
the unsubscribe link in the e-mail.
If you are a Mayo Clinic patient, this could
include protected health information. If we combine this information with your protected
health information, we will treat all of that information as protected health
information and will only use or disclose that information as set forth in our notice of
privacy practices. You may opt-out of email communications at any time by clicking on
the unsubscribe link in the e-mail.
Causes
You can develop post-traumatic stress disorder when you go through, see or learn about an event involving actual or threatened death, serious injury or sexual violation.
Doctors aren't sure why some people get PTSD. As with most mental health problems, PTSD is probably caused by a complex mix of:
- Stressful experiences, including the amount and severity of trauma you've gone through in your life
- Inherited mental health risks, such as a family history of anxiety and depression
- Inherited features of your personality — often called your temperament
- The way your brain regulates the chemicals and hormones your body releases in response to stress
Risk factors
People of all ages can have post-traumatic stress disorder. However, some factors may make you more likely to develop PTSD after a traumatic event, such as:
However, some factors may make you more likely to develop PTSD after a traumatic event, such as:
- Experiencing intense or long-lasting trauma
- Having experienced other trauma earlier in life, such as childhood abuse
- Having a job that increases your risk of being exposed to traumatic events, such as military personnel and first responders
- Having other mental health problems, such as anxiety or depression
- Having problems with substance misuse, such as excess drinking or drug use
- Lacking a good support system of family and friends
- Having blood relatives with mental health problems, including anxiety or depression
Kinds of traumatic events
The most common events leading to the development of PTSD include:
- Combat exposure
- Childhood physical abuse
- Sexual violence
- Physical assault
- Being threatened with a weapon
- An accident
Many other traumatic events also can lead to PTSD, such as fire, natural disaster, mugging, robbery, plane crash, torture, kidnapping, life-threatening medical diagnosis, terrorist attack, and other extreme or life-threatening events.
Complications
Post-traumatic stress disorder can disrupt your whole life ― your job, your relationships, your health and your enjoyment of everyday activities.
Having PTSD may also increase your risk of other mental health problems, such as:
- Depression and anxiety
- Issues with drugs or alcohol use
- Eating disorders
- Suicidal thoughts and actions
Prevention
After surviving a traumatic event, many people have PTSD-like symptoms at first, such as being unable to stop thinking about what's happened. Fear, anxiety, anger, depression, guilt — all are common reactions to trauma. However, the majority of people exposed to trauma do not develop long-term post-traumatic stress disorder.
Getting timely help and support may prevent normal stress reactions from getting worse and developing into PTSD. This may mean turning to family and friends who will listen and offer comfort. It may mean seeking out a mental health professional for a brief course of therapy. Some people may also find it helpful to turn to their faith community.
Some people may also find it helpful to turn to their faith community.
Support from others also may help prevent you from turning to unhealthy coping methods, such as misuse of alcohol or drugs.
By Mayo Clinic Staff
Related
Associated Procedures
Products & Services
What Are PTSD Triggers?
Written by Mary Jo DiLonardo
In this Article
- How Do You Develop Triggers?
- What Are the Different Types of Triggers?
- How Can You Recognize Triggers?
When you have posttraumatic stress disorder (PTSD), your symptoms can come and go. You might feel fine until you hear a car backfire loudly. Suddenly, you become very afraid. Images of your time fighting in a war flood back.
Certain triggers can set off your PTSD. They bring back strong memories. You may feel like you’re living through it all over again. Triggers can include sights, sounds, smells, or thoughts that remind you of the traumatic event in some way.
Some PTSD triggers are obvious, such as seeing a news report of an assault. Others are less clear. For example, if you were attacked on a sunny day, seeing a bright blue sky might make you upset. Knowing your triggers can help you better cope with your PTSD.
How Do You Develop Triggers?
When faced with danger, your body gets ready to fight, flee, or freeze. Your heart beats faster. Your senses go on high alert. Your brain stops some of its normal functions to deal with the threat. This includes your short-term memory.
With PTSD, your brain doesn’t process the trauma the right way. It doesn’t file the memory of the event as being in the past. The result: You feel stressed and frightened even when you know you’re safe.
The brain attaches details, like sights or smells, to that memory. These become triggers. They act like buttons that turn on your body’s alarm system. When one of them is pushed, your brain switches to danger mode. This may cause you to become frightened and your heart to start racing. The sights, sounds, and feelings of the trauma may come rushing back. This is called a flashback.
The sights, sounds, and feelings of the trauma may come rushing back. This is called a flashback.
What Are the Different Types of Triggers?
Anything that reminds you of what happened right before or during a trauma is a potential trigger. They’re usually tied to your senses. You may see, feel, smell, touch, or taste something that brings on your symptoms. While triggers themselves are usually harmless, they cause your body to react as if you’re in danger.
A number of things can trigger your PTSD. Some of the most common include:
People: Seeing a person related to the trauma may set off a PTSD reaction. Or someone may have a physical trait that’s a reminder. For example, if someone with a beard mugged you, other bearded men may bring back memories.
Thoughts and emotions: The way you felt during a traumatic event (afraid, helpless, or stressed) could cause symptoms.
Things: Seeing an object that reminds you of the trauma can cue your PTSD symptoms.
Scents: Smells are strongly tied to memories. For instance, someone who survived a fire might become upset from the smoky smell of a barbecue.
Places: Returning to the scene of a trauma is often a trigger. Or a type of place, like a dark hallway, may be enough to bring on a reaction.
TV shows, news reports, and movies: Seeing a similar trauma often sets off symptoms. This includes scenes from a television show or movie, or a news report.
Feelings: Some sensations, such as pain, are triggers. For survivors of assault, a touch on a certain body part may lead to a flashback.
Sounds: Hearing specific noises, songs, or voices may bring back memories of the trauma. For example, hearing a car backfire may remind a veteran of gunfire.
Tastes: The taste of something, like alcohol, may remind you of a traumatic event.
Situations: You may tie scenarios with the trauma. For instance, being stuck in an elevator might remind you of feeling trapped after a car accident.
For instance, being stuck in an elevator might remind you of feeling trapped after a car accident.
Anniversaries: It’s often hard to go through a date marked by trauma without remembering it, as is the case for many survivors of the terrorist attacks on September 11, 2001.
Words: Reading or hearing certain words could cue your PTSD.
How Can You Recognize Triggers?
Some are obvious. Others are subtle. In fact, you may not realize something is a trigger until you have a reaction. It may seem like your PTSD symptoms come out of the blue. But they’re usually caused by an unknown trigger.
Feeling as if you’re in danger is a sign that you’ve experienced a PTSD trigger. A therapist can help you identify yours. They can also help you learn ways to cope.
PTSD: what is it, symptoms, treatment
Psychological trauma can sit inside us for years and decades, undermining strength and exacerbating pain from time to time. A practicing psychologist talks about the nature of post-traumatic stress disorder and explains what might help to cope with it.
A practicing psychologist talks about the nature of post-traumatic stress disorder and explains what might help to cope with it.
Arkady Volkov, psychotherapist, specialist of the service for the selection of psychologists Alter
Advertising on RBC www.adv.rbc.ru
What is PTSD
Each person has many mechanisms and resources at his disposal that allow him to live through difficult events, cope with difficulties, endure grief and loss, overcome disappointments and tragedies. Nevertheless, sometimes we are faced with an event that, for one reason or another, we cannot cope with: it does not fit into our personal experience at all and turns out to be an insurmountable shock. Such events, usually associated with a real or perceived risk to life and health, are usually called traumas, and they can cause post-traumatic stress disorder - a mental disorder as a result of encountering a traumatic situation.
Studies show that almost 4% of people suffer from PTSD at least once during their lives. At the same time, statistics in different countries differ significantly: in China, 0.3% of respondents faced the problem, in the Netherlands — 7.4%, in Canada — 9.2% [1], [2].
At the same time, statistics in different countries differ significantly: in China, 0.3% of respondents faced the problem, in the Netherlands — 7.4%, in Canada — 9.2% [1], [2].
Symptoms of PTSD
Currently, the two main medical diagnostic guidelines (DSM-5, the American Psychiatric Association's guidelines, and ICD-11, the World Health Organization's classification) state the following criteria to conclude that a person is suffering from PTSD:
- Encounter with a life or health threatening situation. At the same time, PTSD can develop in a situation where a person has become a victim of such an event, and if he was a witness to it, or if a similar event happened to his loved ones. This criterion also applies to professionals who, by the nature of their work, are faced with the consequences of traumatic events: doctors, firefighters, crisis psychologists, and so on.
- Presence of at least one of the symptoms of involuntary intrusive and disturbing memories of the event, nightmares, flashbacks, distressing experiences, or physical reaction in situations that are reminiscent of the event.

- Avoidance of memories and thoughts about the event or anything that might remind of it.
- Disturbances in thinking and emotional state due to the experienced event: inability to remember important aspects of what happened, negative thoughts and beliefs about oneself and the world around, blaming oneself or others that the traumatic event occurred, lowered mood and negative emotions, decreased interest in the world around , feelings of isolation and alienation, reduced ability to experience positive emotions.
- Changes such as irritability and outbursts of anger, aggressive and dangerous behavior to self or others, increased alertness, startle response to minor stimuli, problems concentrating and sleeping.
To be diagnosed, the listed symptoms must last more than one month and cause significant distress or social difficulties.
© shutterstock
It is important to note that PTSD is often accompanied by other disorders, primarily depressive ones.
Diagnosis of PTSD, like any other mental disorder, can only be diagnosed by a qualified specialist, but yes to the following questions may be a reason to seek advice and get help (or just be more attentive to yourself or a loved one).
- Have you experienced or witnessed any traumatic event in your life (such as an accident, fire, extreme disaster, physical attack on you or your loved ones)?
During the last month:
- Did you return to this event in your thoughts (not wanting it) or dreams?
- Did you make an effort not to think about this event and avoid being reminded of it?
- Were you more tense than usual?
- Have you ever been frightened for minor reasons?
- Did you feel alienated from your usual activities and loved ones?
- Did you feel guilty or blame yourself or others for the event?
Causes and risk factors
There is still no definite answer to the question of what exactly causes PTSD. But research has led to some important assumptions.
But research has led to some important assumptions.
At the physiological level, the development of PTSD can be triggered by:
Increased levels of stress hormones
In case of danger, our body produces stress hormones, such as adrenaline, in order to switch into an active mode and somehow escape from the threat (this reaction is often called "fight or flight"). PTSD victims continue to produce large amounts of stress hormones even when the danger is no longer around. This can cause hyperarousal and emotional changes, and can also cause long-term negative health effects, including migraines, pain, and an increased risk of heart, lung, and digestive problems.
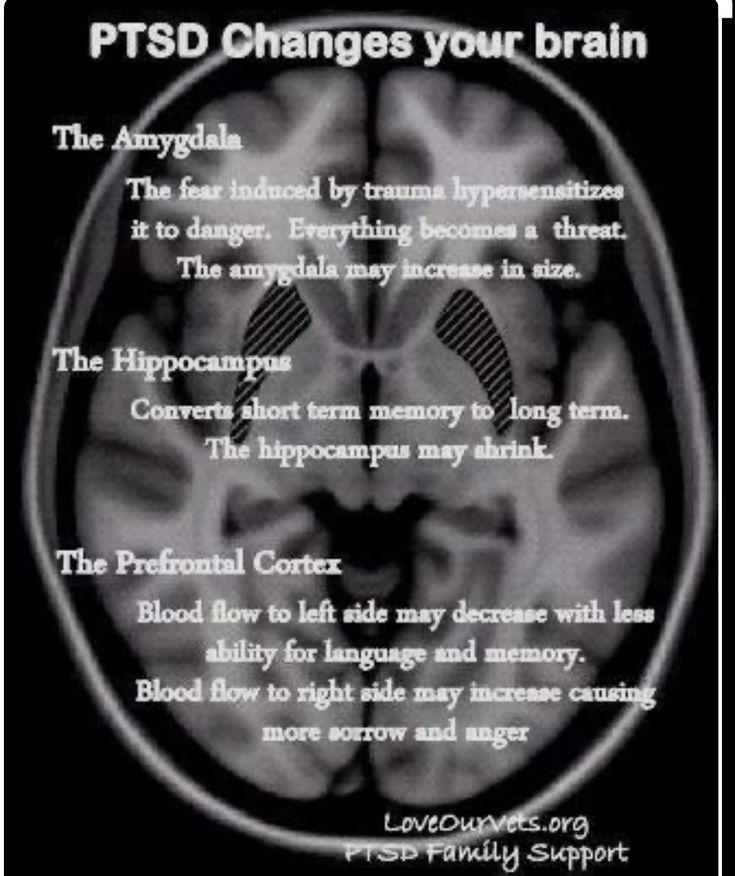
Changes in brain function
Trauma-induced stress can damage the hippocampus, the part of the brain involved in emotion and memory.
Disorders in the hippocampus can interfere with the proper processing of memories and dreams, so the anxiety they cause does not decrease over time. Such changes may explain the increased levels of fear and anxiety, memory and recall problems suffered by PTSD victims.
Such changes may explain the increased levels of fear and anxiety, memory and recall problems suffered by PTSD victims.
© shutterstock
Factors that can increase susceptibility to PTSD:
- Previous traumatic experiences. The stress of a trauma can have a cumulative effect, and a new traumatic experience can exacerbate the negative effects of a previous trauma.
- Experience of violence. People with a history of physical, emotional or sexual abuse tend to be more susceptible to post-traumatic stress.
- PTSD or depression in loved ones.
- Substance use experience.
- Lack of skills to cope with traumatic situations.
- Lack of social support. Good social and family relationships help mitigate the effects of stress and trauma. Conversely, people who lack supportive relationships and environments tend to be more vulnerable to stress and therefore more at risk for PTSD. Being in a social environment that cultivates shame, guilt, stigma, or self-hatred also contributes to the development of post-traumatic stress disorder.

- High level of stress in everyday life.
Treatment of PTSD
Approaches to the treatment of PTSD can be divided into two groups: medication and psychotherapy. Often methods of both groups are used in different combinations.
There are currently no medications specifically designed to treat PTSD, but there are many medications that work well for other conditions, such as depression and anxiety disorders, and have been shown to be effective in treating the symptoms of PTSD.
When it comes to psychotherapeutic methods, or "healing with a word", several approaches demonstrate the greatest (and research-supported) effectiveness.
Cognitive Process Therapy
In this approach, the therapist invites the client to talk about the traumatic event and its aftermath and describe the experience in detail in a diary, which allows them to better see how the trauma is reflected in thoughts and find new ways to deal with it [3 ].
© shutterstock
EMDR - Eye Movement Desensitization and Processing
This approach is based on the notion that trauma disrupts the natural coping mechanisms inherent in each person and cannot be built into their experience and memory. The person is asked to focus on an external stimulus (eye movements from side to side directed by the therapist) and in parallel work through complex memories, thoughts and emotions associated with the trauma [4].
The person is asked to focus on an external stimulus (eye movements from side to side directed by the therapist) and in parallel work through complex memories, thoughts and emotions associated with the trauma [4].
Body and creativity oriented approaches
Body Oriented Therapy aims to find resources through attention to bodily sensations, as well as gaining the opportunity to relive the traumatic experience from the position of an active actor, not a victim. Similar goals are set by approaches that use dance and participation in theatrical productions to gain the freedom and spontaneity that PTSD often deprives its victims of [5].
Living with PTSD
Trauma has a huge impact on many areas of our lives, but this does not mean that the problem cannot be solved, even if for one reason or another you do not have access to professional help.
Of particular difficulty in working with PTSD is the very pain and severity of the traumatic experience, which often makes it necessary to avoid any reminders of the trauma, excluding the possibility of talking about it, as well as the devastating consequences for the view of oneself and the world around. All this makes it extremely difficult to build close relationships, seek support and help.
All this makes it extremely difficult to build close relationships, seek support and help.
What can help you cope with PTSD
The very first and most important step is often the recognition of the traumatic experience, which opens up opportunities for conversation and subsequent rethinking. The devastating effect of trauma on the psyche is largely due to the fact that the traumatic event is completely knocked out of the normal course of our life, and it is extremely important to return, build it into our personal history.
Research demonstrates the effectiveness of such a simple tool as writing about your experience: writing down your thoughts and memories of a traumatic event, trying to talk about the impact it had on your life, thinking about the future.
Since trauma affects the body in one way or another, physical exercise, yoga (or regular stretching), meditation, dancing, and even theater classes can be an important help in overcoming its consequences [6].
The support of relatives and friends plays a huge role. It's important to open yourself up and find someone you can talk to about what's bothering you.
However, overcoming PTSD on your own is not easy and can take a long time. Therefore, at the first opportunity, it is worth contacting a psychotherapist.
If your loved one has PTSD
If you notice symptoms of PTSD in a loved one, you can become a support for him and help him. At the same time, it is important to take into account that it can be extremely difficult for him to talk about the trauma and even return to it in his thoughts, so it is important to indicate your willingness to help and be there without exerting any pressure. Your very understanding and supportive presence, your willingness to share activities that bring joy and pleasure, a sense of stability and confidence can be beneficial. At the same time, you should learn more about PTSD in general, and about the features of its manifestation in your loved one (including triggers - situations, words or objects that can provoke memories of a traumatic experience).
Books about PTSD
Tags: psychology
Post-traumatic stress disorder (PTSD) | English translation
However, most people realize what happened after a few weeks, sometimes a little longer, and then their symptoms will begin to disappear.
Research shows that certain groups of people are at increased risk of developing post-traumatic stress disorder. The risk of developing post-traumatic stress disorder is reduced when a person has:
Any traumatic event can cause PTSD, although the more severe the shock, the more likely it is to develop PTSD. For example, PTSD is more likely to develop if the event:
- is sudden and unexpected
- lasts for a long time
- happens when you are caught in a trap that you cannot get out of
- was caused by people
- causes a lot of death
- causes injury
- includes children
If you are still stressed and in an uncertain state, it will be difficult to get rid of the symptoms of PTSD.
How do I know that I have overcome a traumatic experience?
You may have already gotten over the traumatic event if you can:
- think about it without worrying
- not feel like you are under constant threat
- not think about it all the time
Why is PTSD not always diagnosed?
There are a number of reasons why a person with PTSD may not be diagnosed.
Stigma and misunderstanding
People with PTSD often avoid talking about their feelings to avoid thinking about the traumatic event.
Some people believe that the symptoms they are experiencing (such as avoidance or emotional numbness) help them cope and do not realize that they are caused by PTSD.
When people are very ill, they find it hard to believe that they are able to feel the way they did before the traumatic event. This may discourage them from getting help.
There is also a common misconception that only military personnel suffer from PTSD. In fact, PTSD can happen to anyone, and any experience of PTSD is real.
In fact, PTSD can happen to anyone, and any experience of PTSD is real.
Misdiagnosis
Some people with PTSD may be misdiagnosed with conditions such as anxiety or depression. Some people have other mental and physical health problems that make PTSD go unnoticed.
They may also experience medically unexplained symptoms such as:
- gastrointestinal disorders
- pain syndromes
- headaches
These symptoms may mean that their PTSD goes unnoticed.
Other difficulties
Some people with PTSD may also have other problems, such as difficulties in human relationships or addiction to alcohol and drugs. They may be caused by post-traumatic stress disorder, but these problems will manifest themselves more clearly than PTSD itself.
Can children develop PTSD?
PTSD can develop at any age. In addition to the symptoms of PTSD common to adults, children may also experience:
- Nightmares - In children, these dreams may or may not reflect an actual traumatic event.

- Repetitive play - some children act out a traumatic event during play. For example, a child who has been in a serious traffic accident may recreate the accident with toy cars.
- Physical symptoms - they may complain of abdominal pain and headaches.
- Fear of imminent death - they may find it hard to believe that they will live long enough to become adults.
What are the treatments for PTSD?
There are a number of different treatments for PTSD, including trauma-focused cognitive behavioral therapy (TF-CBT), eye movement desensitization and processing (EMDR), and medications.
Psychotherapy
Psychotherapy for PTSD will focus on the traumatic experience, not your past life. They will help you with the following:
- Acceptance - learn to accept the fact that although you cannot change what happened, you can think differently about the event, the world around you and your life.

- Remembrance of the event - remembering what happened, you will not feel fear or anxiety. You will be able to think about what happened when you yourself want it, and not through obsessive thoughts or memories.
- Explaining your experiences in words - by saying out loud what happened, your mind will be able to push the memories away and do other things.
- Finding a sense of security - helps you better control your feelings. This will make you feel more secure and eliminate the need to avoid memories.
All psychotherapy must be administered by a properly trained and accredited professional. Sessions are usually conducted by the same therapist at least once a week, with a total duration of at least 8-12 weeks.
Sessions usually last about an hour, sometimes they can last up to 90 minutes.
Therapy for PTSD includes:
Trauma-focused Cognitive Behavioral Therapy
A type of talking therapy that can help you change the way you think. Over time, this can help you feel better and behave differently. It is usually done individually, although there is evidence that CBT for trauma can also be done in groups.
Over time, this can help you feel better and behave differently. It is usually done individually, although there is evidence that CBT for trauma can also be done in groups.
Eye Movement Desensitization and Reprocessing (EMDR)
A technique that uses eye movements to help the brain process traumatic memories.
You will be asked to remember the traumatic event and what it made you think and feel. While you do this, you will be prompted to move your eyes or receive other "two-way stimulation" such as tapping your hand. It turns out that this reduces the emotional burden experienced in connection with the traumatic memory and helps to cope with the trauma.
The GERD must be carried out by a qualified person. EPDH usually requires 8-12 sessions, lasting from 60 to 90 minutes.
Some other forms of talking therapy may be useful for treating certain symptoms (eg, poor sleep) in people for whom EMRT or CBT have not been effective for trauma.
Medications
If you have tried various treatments for post-traumatic stress disorder and find that they do not work for you, your doctor may prescribe antidepressants.
Selective serotonin reuptake inhibitors (SSRIs) are antidepressants that can help reduce symptoms of post-traumatic stress disorder. They can also help you if you are suffering from depression.
If SSRIs are not working for you, you may be offered other drugs, but this should usually be done on the advice of a mental health professional.
Which treatment is more effective?
There is evidence that Cognitive Behavioral Therapy for Trauma and Eye Movement Desensitization and Reprocessing are the best first line treatments. Medication can help those who refuse talking therapy or cannot easily access it.
Which treatment should I take first?
Trauma-focused psychological therapy (TF-CBT or EMBT) should be offered prior to medication, to the extent possible. This is in line with the UK National Institute for Health and Clinical Excellence (NICE) guidelines.
How can I help myself?
There are some things you can do to help you get better if you develop PTSD. Your therapist will help with this and make sure you apply them in a timely manner:
Your therapist will help with this and make sure you apply them in a timely manner:
Stick to your daily routine - As far as possible, try to return to or maintain your normal daily routine. By continuing to lead a life as normal as possible, you can gain a sense of support.
Talk to someone you trust - Although you shouldn't feel like you need to talk to everyone about what happened, talking to someone you trust can help you sort out your feelings in a safe environment. It can also help to talk to someone who has gone through the same thing as you, or someone who has gone through something similar before, as long as it doesn't hurt you.
Try relaxation exercises - Try self-meditation and other relaxation exercises. Relaxing with PTSD can be challenging, so talk to your therapist about exercises or activities that can help you.
Return to work or school - if you feel empowered, it can help you return to work, school or university by giving you a sense of routine. However, you should try to avoid situations in which you may be subjected to further injury or severe stress. It is usually best to work in a supportive, low-stress environment before starting treatment.
However, you should try to avoid situations in which you may be subjected to further injury or severe stress. It is usually best to work in a supportive, low-stress environment before starting treatment.
Eat and exercise regularly - Try to eat at regular times, even if you don't feel hungry. If you feel fit, try to exercise regularly. It can also help you feel tired before bed.
Spend time with others - Spending time with people you care about will help you feel supported.
Expect to get better - Concentrating on thoughts that you will feel better over time will be useful for your recovery. Remember that you should not strain yourself in an attempt to recover faster.
Go back to where the traumatic event happened - If you feel you can do it, you may want to go back to where the traumatic event happened. Talk to your therapist or doctor if you are considering this so they can support you through this step.
There are also some things you should avoid while recovering. However, doing the "right things" can be very difficult, and you shouldn't feel guilty if you find yourself doing any of the following:
Self-criticism - PTSD symptoms are not a sign of weakness. This is a normal reaction to violent experiences.
Keep your feelings to yourself. If you have PTSD, don't feel guilty about sharing your thoughts and feelings with others. Talking about how you are feeling can help your recovery.
Expecting things to get back to normal quickly - PTSD can take some time to heal. Try not to demand too much of yourself in a short amount of time.
Stay away from other people. Spending a lot of time alone can increase your sense of isolation and make you feel less well.
Drink alcohol or smoke. While alcohol can help you relax, and coffee and nicotine can act as stimulants, they can make you feel worse over time if you experience symptoms associated with PTSD.
Overwork. Post-traumatic stress disorder can make it difficult to sleep, but as much as possible, try to stick to your normal sleep patterns and stay up late, as this can make you feel worse. You can learn more about good sleep in our resource.
Finally, you should be careful while driving. After a traumatic episode, people may have more accidents.
What is complex PTSD?
Some people develop complex post-traumatic stress disorder, caused by an experience or series of events that is extremely threatening or terrifying. These events can occur in childhood or adulthood.
Often such events are difficult or impossible to avoid. For example:
- torture
- slavery
- genocide
- living in war zones
- prolonged domestic violence
- repeated sexual and physical abuse
In addition to PTSD symptoms, people with complex PTSD may also:
- emotions and emotional reactions
- have difficulty maintaining relationships and feelings of closeness with other people
How do I recover from complex PTSD?
People with complex post-traumatic stress disorder are characterized by a lack of trust in other people and in the world at large.
Emotional stabilization
During the stabilization phase, you will learn to trust your therapist and to understand and manage feelings of distress and alienation.
As part of stabilization, you can familiarize yourself with the work with supports - "grounding techniques". This can help you focus on familiar physical sensations and remind you that you are living in the present, not the past.
Stabilization can help you "unplug" your feelings of fear and anxiety from the memories and the emotions they evoke, helping to make those memories less frightening.
The goal of stabilization is so that you can eventually live your life free from anxiety or memories.
Sometimes stabilization may be the only help needed.
Trauma Focused Therapy
Trauma Focused Therapy, including EMDR (Eye Movement Desensitization and Processing) or Trauma Focused Cognitive Behavioral Therapy, can help you deal with traumatic experiences. Other types of psychotherapy, including psychodynamic psychotherapy, may also be helpful. With complex post-traumatic stress disorder, care must be taken as these treatments can make things worse if not used properly.
Other types of psychotherapy, including psychodynamic psychotherapy, may also be helpful. With complex post-traumatic stress disorder, care must be taken as these treatments can make things worse if not used properly.
Reintegration and recovery
Reintegration into your normal life can help you get used to the real world at a time when you have emerged from the dangerous situation you were in before. This can help you begin to see yourself as a person with a choice.
Reintegration can help you:
- be compassionate towards yourself and others
- restore trust in yourself and others
- renew friendships, intimate relationships, and activities that promote your health and well-being
Medications
As with PTSD, antidepressants or other medications may be used along with psychotherapy. Medication may also be used if psychotherapy does not help or is not available to you. It would also be helpful to have a mental health professional help you oversee your medication.
Self Help
If you develop complex PTSD, it may be helpful to try to do ordinary things that have nothing to do with your past traumatic experience.
They can include:
- To make friends
- get a job
- to engage regular physical exercises
- Learn to relax
- Find the hobby
- Take a home animals
These things can help you gradually start the world around you . However, this can take time, and there is no need to be ashamed that at first these things will seem difficult to you or you will not be able to do them right away.
How do you know if someone has PTSD?
If you know someone who has just experienced a traumatic event, there are a few things you should be aware of. These moments can be signs that a person is not coping:
- Changes in behavior - low productivity at work, lateness, sick leave, minor accidents.
- Changes in emotions - anger, irritability, depression, lack of interest and lack of concentration.

- Changes in thought - preoccupation with threats or fears, negative outlook on the future
- Unexpected physical symptoms such as shortness of breath, nervousness or abdominal pain.
If you think a person may be showing signs of PTSD, you can suggest that they talk to their doctor. If you don't feel close enough to him for such a recommendation, talk to someone in his family or friends who could do it for you.
They may also find it helpful to refer to information about PTSD, such as this resource, to help identify the difficulties they face.
How can I help someone who has experienced a traumatic event?
For those who have experienced a traumatic event, the following actions may help:
- Be there - invite people to be with them. If they refuse, you can reassure them that you will be with them if they change their mind. Should not be imposed, but try to convince them to accept your help.

- Listen - try not to pressure people if they don't want something. If they want to talk, try to listen without interrupting or trying to share your own experience with them.
- Ask general questions - When you ask questions, try to keep them general and non-judgmental. For example, you might ask, "Have you talked about this with anyone else?" or “Can I help you find more help?”
- Offer real (practical) help - Some people may have difficulty taking care of themselves or doing daily activities. Offer help, such as cleaning the house or preparing meals;
Try not to tell people:
- That you know how they feel - even if you have experienced something like this, people experience situations differently. Comparing your experience with that of others is not always helpful;
- How lucky they are to be alive - people who have experienced traumatic events often don't think they are "lucky".
Learn more