Neuropsychology of adhd
Neuropsychology of adults with attention-deficit/hyperactivity disorder: a meta-analytic review
Meta-Analysis
. 2004 Jul;18(3):485-503.
doi: 10.1037/0894-4105.18.3.485.
Aaron S Hervey 1 , Jeffery N Epstein, John F Curry
Affiliations
Affiliation
- 1 Department of Psychology, Duke University, Durham, NC 27705, USA. [email protected]
- PMID: 15291727
- DOI: 10.1037/0894-4105.18.3.485
Meta-Analysis
Aaron S Hervey et al. Neuropsychology. 2004 Jul.
. 2004 Jul;18(3):485-503.
doi: 10.1037/0894-4105.18.3.485.
Authors
Aaron S Hervey 1 , Jeffery N Epstein, John F Curry
Affiliation
- 1 Department of Psychology, Duke University, Durham, NC 27705, USA. [email protected]
- PMID: 15291727
- DOI: 10.1037/0894-4105.18.3.485
Abstract
A comprehensive, empirically based review of the published studies addressing neuropsychological performance in adults diagnosed with attention-deficit/hyperactivity disorder (ADHD) was conducted to identify patterns of performance deficits. Findings from 33 published studies were submitted to a meta-analytic procedure producing sample-size-weighted mean effect sizes across test measures. Results suggest that neuropsychological deficits are expressed in adults with ADHD across multiple domains of functioning, with notable impairments in attention, behavioral inhibition, and memory, whereas normal performance is noted in simple reaction time. Theoretical and developmental considerations are discussed, including the role of behavioral inhibition and working memory impairment. Future directions for research based on these findings are highlighted, including further exploration of specific impairments and an emphasis on particular tests and testing conditions.
Findings from 33 published studies were submitted to a meta-analytic procedure producing sample-size-weighted mean effect sizes across test measures. Results suggest that neuropsychological deficits are expressed in adults with ADHD across multiple domains of functioning, with notable impairments in attention, behavioral inhibition, and memory, whereas normal performance is noted in simple reaction time. Theoretical and developmental considerations are discussed, including the role of behavioral inhibition and working memory impairment. Future directions for research based on these findings are highlighted, including further exploration of specific impairments and an emphasis on particular tests and testing conditions.
Similar articles
-
Meta-analysis of intellectual and neuropsychological test performance in attention-deficit/hyperactivity disorder.
Frazier TW, Demaree HA, Youngstrom EA.
 Frazier TW, et al. Neuropsychology. 2004 Jul;18(3):543-55. doi: 10.1037/0894-4105.18.3.543. Neuropsychology. 2004. PMID: 15291732
Frazier TW, et al. Neuropsychology. 2004 Jul;18(3):543-55. doi: 10.1037/0894-4105.18.3.543. Neuropsychology. 2004. PMID: 15291732 -
Executive functions: performance-based measures and the behavior rating inventory of executive function (BRIEF) in adolescents with attention deficit/hyperactivity disorder (ADHD).
Toplak ME, Bucciarelli SM, Jain U, Tannock R. Toplak ME, et al. Child Neuropsychol. 2009 Jan;15(1):53-72. doi: 10.1080/09297040802070929. Child Neuropsychol. 2009. PMID: 18608232
-
Attention deficit hyperactivity disorder (ADHD): gender- and age-related differences in neurocognition.
Bálint S, Czobor P, Komlósi S, Mészáros A, Simon V, Bitter I. Bálint S, et al. Psychol Med. 2009 Aug;39(8):1337-45.
 doi: 10.1017/S0033291708004236. Epub 2008 Aug 20. Psychol Med. 2009. PMID: 18713489
doi: 10.1017/S0033291708004236. Epub 2008 Aug 20. Psychol Med. 2009. PMID: 18713489 -
Moderators of working memory deficits in children with attention-deficit/hyperactivity disorder (ADHD): a meta-analytic review.
Kasper LJ, Alderson RM, Hudec KL. Kasper LJ, et al. Clin Psychol Rev. 2012 Nov;32(7):605-17. doi: 10.1016/j.cpr.2012.07.001. Epub 2012 Jul 17. Clin Psychol Rev. 2012. PMID: 22917740 Review.
-
[Executive dysfunctions in adults with attention deficit hyperactivity disorder].
Rodriguez-Jiménez R, Cubillo A, Jiménez-Arriero MA, Ponce G, Aragüés-Figuero M, Palomo T. Rodriguez-Jiménez R, et al. Rev Neurol. 2006 Dec 1-15;43(11):678-84. Rev Neurol. 2006. PMID: 17133329 Review. Spanish.
See all similar articles
Cited by
-
Social Cognition in Adult ADHD: A Systematic Review.
Morellini L, Ceroni M, Rossi S, Zerboni G, Rege-Colet L, Biglia E, Morese R, Sacco L. Morellini L, et al. Front Psychol. 2022 Jul 11;13:940445. doi: 10.3389/fpsyg.2022.940445. eCollection 2022. Front Psychol. 2022. PMID: 35898990 Free PMC article.
-
Fast Tracking Assessment of Attention Deficit Hyperactivity Disorder in Tertiary Care.
Burrows K, Rysdyk S. Burrows K, et al. J Patient Exp. 2022 Jul 5;9:23743735221112210. doi: 10.1177/23743735221112210. eCollection 2022. J Patient Exp. 2022. PMID: 35832606 Free PMC article.
-
University students with attention deficit hyperactivity disorder (ADHD): a consensus statement from the UK Adult ADHD Network (UKAAN).

Sedgwick-Müller JA, Müller-Sedgwick U, Adamou M, Catani M, Champ R, Gudjónsson G, Hank D, Pitts M, Young S, Asherson P. Sedgwick-Müller JA, et al. BMC Psychiatry. 2022 Apr 22;22(1):292. doi: 10.1186/s12888-022-03898-z. BMC Psychiatry. 2022. PMID: 35459116 Free PMC article.
-
Longitudinal Cognitive Performance of Older Adults With ADHD Presenting to a Cognitive Neurology Clinic: A Case Series of Change Up to 21 Years.
Callahan BL, Shammi P, Taylor R, Ramakrishnan N, Black SE. Callahan BL, et al. Front Aging Neurosci. 2021 Nov 15;13:726374. doi: 10.3389/fnagi.2021.726374. eCollection 2021. Front Aging Neurosci. 2021. PMID: 34867269 Free PMC article.
-
Are attention and cognitive control altered by fMRI scanner environment? Evidence from Go/No-go tasks in ADHD.
Kolodny T, Mevorach C, Stern P, Ankaoua M, Dankner Y, Tsafrir S, Shalev L. Kolodny T, et al. Brain Imaging Behav. 2022 Jun;16(3):1003-1013. doi: 10.1007/s11682-021-00557-x. Epub 2021 Oct 27. Brain Imaging Behav. 2022. PMID: 34705186
See all "Cited by" articles
Publication types
MeSH terms
How do neuropsychologists diagnose ADHD?
Written by Dr. Nicole M. Vienna
December 23, 2021
Contrary to popular belief, there is no single test or checklist for diagnosing ADHD. Indeed, it is a complex neurobehavioral diagnosis and often misdiagnosed. To that end, ADHD shares many symptoms with other disorders, such as PTSD, personality disorders, anxiety, bipolar disorder, and depression. This article will give you a brief overview of the ADHD criteria, adults and ADHD, a neuropsychological approach to ADHD, and ADHD’s interaction in juvenile delinquency.
According to the DSM-5, ADHD is considered a neurodevelopmental disorder because symptoms begin in the developmental period. Individuals with ADHD have a persistent pattern of inattention and/or hyperactivity-impulsivity that interferes with life functioning. Inattentive symptoms can include:
- Difficulty sustaining attention on tasks or play activities
- Does not seem to listen when spoken to directly
- Trouble organizing tasks and activities
- Easily distracted
- Forgetful in daily activities
- Fails to give close attention to details.
Hyperactivity-impulsivity symptoms can include:
- fidgets with hands, arms, or legs, or squirms in place
- leaves the seat when expected to remain seated
- talks excessively
- often on the go or acts as if they are driven by a motor
- interrupts or intrudes in conversations or games
- blurts out the answers
- unable to turn, take or play games quietly.

In addition, symptoms must have been present prior to age 12, present in two or more settings, and cause clinically significant distress or interfere with daily life functioning (work, school, relationships, etc.). Last, the symptoms cannot be better described by another disorder such as depression, anxiety, or a personality disorder.
These symptoms can result in three different types of presentations:
- Predominately Inattentive Type– a qualifying number of inattentive symptoms are present for the last six months
- Predominately Hyperactive Type– a qualifying number of hyperactive symptoms are present for the last six months
- Combined Type– a qualifying number of both inattentive and hyperactive symptoms are present for the last six months
Brain Structure and ADHD
Numerous neuroimaging studies have found several morphological abnormalities in children’s brains with ADHD. Specifically, regional abnormalities include the reduced grey matter in the regions making up the frontostriatal circuits, atypical white matter volume in neural tracts (related to impaired communication between circuits), and cortical thinning. Still, over studies have found that ADHD is associated with reduced global brain volume. As such, ADHD is the result of complex abnormalities predominantly affecting the frontal lobes and other regions of the brain. In addition, it is important to note that genetic and adverse rearing association has been associated with reduced cortical volume in ADHD children. Thus, shining light on the role of parenting style and environmental influences on brain development.
Still, over studies have found that ADHD is associated with reduced global brain volume. As such, ADHD is the result of complex abnormalities predominantly affecting the frontal lobes and other regions of the brain. In addition, it is important to note that genetic and adverse rearing association has been associated with reduced cortical volume in ADHD children. Thus, shining light on the role of parenting style and environmental influences on brain development.
Adults and ADHD
While it has been thought to only exist in childhood, ADHD symptoms and impairments can persist into adulthood. Adult prevalence rates are estimated at 2.5% (Simon, et al. 2009). Still, other studies have found that over 10 million adults have ADHD.
Neuropsychological Approach to ADHD
Neuropsychologists are specifically trained in brain functioning, neuroanatomy, and brain-behavior relationships. Therefore, when assessing for ADHD, a neuropsychologist may use a variety of standardized cognitive tests and behavioral questionnaires. Depending on potential co-occurring issues, an ADHD evaluation can be very narrow-focused or broadly assessed to rule out or confirm cofounding problems. The tested cognitive domains can include intelligence, memory, learning, attention, problem-solving, organizational skills, and emotional regulation. Once the data is analyzed, the clinician will write a succinct report, including treatment recommendations to help improve daily life functioning.
Depending on potential co-occurring issues, an ADHD evaluation can be very narrow-focused or broadly assessed to rule out or confirm cofounding problems. The tested cognitive domains can include intelligence, memory, learning, attention, problem-solving, organizational skills, and emotional regulation. Once the data is analyzed, the clinician will write a succinct report, including treatment recommendations to help improve daily life functioning.
ADHD and Juvenile Delinquency
Children with ADHD have impairments that can result in various problematic behaviors that can get them mixed into the juvenile justice system. For example, their difficulties paying attention in class, excessive talking and disruption, inability to sit still, being unable to not be distracted (inattention problems), not being able to stop internal thoughts (impulsivity), or being unable to stop acting upon distractions and/or thoughts (hyperactivity) can get them into trouble with their parents or school officials which then can lead them into truancy and eventually dropping out altogether. And if these symptoms continue to go untreated, these children may turn to drugs/alcohol to self-medicate unremitted symptoms, thereby increasing their risk of poor decision making and asocial behavior and coming in contact with the legal system.
And if these symptoms continue to go untreated, these children may turn to drugs/alcohol to self-medicate unremitted symptoms, thereby increasing their risk of poor decision making and asocial behavior and coming in contact with the legal system.
Also, children with ADHD may have problems with self-talk (our ability to talk to ourselves), sense of time (in that time can seem to go by very slow or very fast), and shifting from plan A to Plan B. Lastly, they are more likely than their peers to struggle with separating emotion from fact, again, increasing their risk of asocial behavior and engaging in behavior that is not well thought out.
Final Thoughts
ADHD is a complex neurobehavioral diagnosis that shares overlapping symptoms with bipolar disorder, PTSD, anxiety, depression, and even some personality disorders. While most thought to exist in children, some studies have shown upwards of 10 million adults have ADHD. A neuropsychological evaluation can help assess executive functioning systems among other cognitive domains implicated in ADHD. This includes standardized cognitive paper-pencil testing as well as behavioral and symptom questionnaires. Untreated or mismanaged symptoms can lead to self-medicating with drugs or alcohol, thereby increasing their risk of asocial behavior, which is not well thought out.
This includes standardized cognitive paper-pencil testing as well as behavioral and symptom questionnaires. Untreated or mismanaged symptoms can lead to self-medicating with drugs or alcohol, thereby increasing their risk of asocial behavior, which is not well thought out.
If you would like to learn more about ADHD, contact our office to speak with Dr. Vienna. Call us at (626) 709-3494.
How to help a child with ADHD?
Attention deficit hyperactivity disorder (ADHD) is a behavioral developmental disorder. How as a rule, it is diagnosed in children. Child with ADHD has difficulty concentrating, he becomes hyperactive, poorly controlled and impulsive. Unfortunately, many parents and educators in schools do not take this disorder seriously and associate child's behavior with pampering and bad manners. Children with ADHD are often subjected to pressure from both parents and from other children. All this is fertile ground for further mental illness and the formation of criminogenic behavior in adulthood. How to determine in time Does your child need professional help? What are the reasons for the appearance syndrome? And what if your child is diagnosed with ADHD? Says the leading researcher of the Ural Federal University Sergey Kiselev.
How to determine in time Does your child need professional help? What are the reasons for the appearance syndrome? And what if your child is diagnosed with ADHD? Says the leading researcher of the Ural Federal University Sergey Kiselev.
Sergey Yuryevich Kiselev – Candidate in Psychology, Leading Researcher at the Ural Federal University, Head of the Laboratory of the Brain and neurocognitive development.
- I remember how 13 years ago my cousin brother was diagnosed with Attention Deficit Disorder and hyperactivity. Then in Russia, almost no one knew about it. diagnosis. Tell us what is known today?
In fact, we still don't fully know what it is. disorder. There is a definition in the International classification of diseases, where deficiency syndrome is separately distinguished attention and separately - hyperactivity syndrome. However, often we We are faced with two sets of symptoms. Such a manifestation commonly referred to as Attention Deficit Hyperactivity Disorder or ADHD.
Such a manifestation commonly referred to as Attention Deficit Hyperactivity Disorder or ADHD.
However, there is still no generally accepted concept of causes of ADHD, about the mechanisms that cause syndrome symptoms. We have at our disposal only a number of different models that attempt to explain externally observed symptoms. I view this disorder from a neuropsychological point of view in within the framework of the Lurie approach. Russian psychologist and neuropathologist Alexander Romanovich Luria created a national neuropsychology, which is known throughout the world precisely as Luriev neuropsychology. His followers and students developed their own concept of the nature of behavioral disorders and mental health in children with ADHD.
It's not just about attention problems or hyperactivity. These children have a range of symptoms associated with a disorder. different mental functions, for example, they often have specific memory impairment, increased exhaustion, difficulties of inclusion in tasks, activity fluctuation, etc. Before modern specialists are faced with the task of explaining the causes and mechanisms of this set of symptoms.
Before modern specialists are faced with the task of explaining the causes and mechanisms of this set of symptoms.
Why is it important? If we know the mechanism of disorder, then we can more effectively help children deal with them. it will allow us to correctly build a correction for the development of children with ADHD diagnosis, which will work with the mechanism of the disorder, not outward symptoms. Suppression or withdrawal of symptoms often does not mean that we act on the mechanism of disorder, Therefore, such a correction has a short-term effect. For example, if a person has a cough that is associated with tuberculosis, then cough pills, of course, will not cure this disease. AT In this case, it is necessary to treat tuberculosis, then cough, as one of the symptoms of this disease will disappear. Also with behavioral disorders. It is necessary to influence the mechanism of the disorder, and not "remove symptoms".
Unfortunately, there is still no generally accepted understanding what the variants of ADHD might be. Most likely, There are different kinds and types of this syndrome. For example, modern research shows that under such a disorder How does ASD (Autism Spectrum Disorder) fall under the plethora of different variants of this disorder, including Asperger's syndrome, Kanner syndrome, RDA (early childhood autism), etc. It is obvious that ADHD also includes different varieties.
Most likely, There are different kinds and types of this syndrome. For example, modern research shows that under such a disorder How does ASD (Autism Spectrum Disorder) fall under the plethora of different variants of this disorder, including Asperger's syndrome, Kanner syndrome, RDA (early childhood autism), etc. It is obvious that ADHD also includes different varieties.
It is also important to understand that there are individual differences course of this disease.
Professionals should not just diagnose ADHD, thereby putting a label on the child. They must clearly understand which variant of ADHD you need to work with in a particular situation. It is necessary to understand the individual characteristics of the course of ADHD every child.
One of the serious tasks of modern child neuropsychology and neurology — development of an algorithm for helping children with ADHD, taking into account type of disorder, age, gender, individual and typological features of the child.
- Describe key symptoms that may indicate ADHD in its early stages?
- If we talk about the most rude version of ADHD, then there is a number of basic sets of symptoms.
The first set of symptoms is associated with behavioral characteristics. One of the key symptoms is increased exhaustion. Such children as a rule, they cannot engage in any one activity for a long time. At school, for example, children with ADHD cannot sit still 40 minutes of the lesson, listen to the teacher, complete assignments. They are fast exhausted and switched to other activities. Exhaustibility this kind of thing greatly interferes with successful learning, and in a broader sense, effectively adapt to the world.
The second key symptom is related to the inability to turn on quickly. into a certain activity. A simple example: the beginning of the lesson after change. The typical child quickly enters the appropriate learning activity pace of activity, begins to listen to the teacher, complete study assignments. A child with ADHD cannot change quickly level of brain activity. At recess, when he ran, jumped, played with other children, he had increased activity, but for it is not suitable for learning activities. Enhanced Level brain activity can not decrease to a suitable level for educational activity. Hence the serious problems with success learning, frequent comments from the teacher, etc.
A child with ADHD cannot change quickly level of brain activity. At recess, when he ran, jumped, played with other children, he had increased activity, but for it is not suitable for learning activities. Enhanced Level brain activity can not decrease to a suitable level for educational activity. Hence the serious problems with success learning, frequent comments from the teacher, etc.
The third symptom manifests itself in the form of peculiar waves of activity. At in such children, there is an effect of either increased activity, or its sharp decline. Similar undulating activity also manifests itself in school during the lesson. Against the backdrop of these fluctuations in activity, a specific effect occurs - at the peaks hyper- and hypoactivity children with ADHD are not successful in performing educational tasks. At such moments, their brain activity is not corresponds to learning activities. But when for a short period of time, their brain activity stabilizes and enters agreement with learning activities, they easily respond to teacher's questions, can solve a difficult problem, etc.
That is why many teachers notice that children with ADHD often disobedient, chaotic, but at the same time they have a normal intelligence. Indeed, the cognitive resources of such children are often good enough. And against the background of an optimal level of activity brain they realize them to the maximum. When the activity level does not correspond to educational activities, they, of course, show poor results.
In fact, each of us has waves of activity. During We go through periods of growth and decline every day. This characterizes normal feature of our nervous system. She demands period of rest, rest and activity. But in children with ADHD, this feature manifests itself in a hypertrophied form. Waves activities change more often and more noticeably.
The fourth symptom is hyperactivity, which manifests itself in the form increased motor activity, restlessness, the number of unnecessary movements, speech incontinence, etc. There is such a thing as synkinesis - involuntary extra movements during the performance of some activity or motor activity. For example, a child writes something in notebooks, and at this time his tongue moves, his shoulders move or legs move.
There is such a thing as synkinesis - involuntary extra movements during the performance of some activity or motor activity. For example, a child writes something in notebooks, and at this time his tongue moves, his shoulders move or legs move.
According to such key symptoms in the behavior of the child, specialists identify the presence of attention deficit disorder and hyperactivity.
Although there are situations when the diagnosis is made when the presence of only one of these symptoms. And this is wrong. For example, increased exhaustion may not be in the context of ADHD, and manifest as a result of dystonia or another disease. Therefore, it must be clearly understood that ADHD is always set of symptoms.
In addition to the group of behavioral symptoms, there are a number of secondary manifestations. Children with ADHD often have cognitive Problems. For example, they do not solve problems well against the background of fluctuations. activity. An experienced diagnostician will immediately understand that the reason lies not in the cognitive abilities of the child, and in the presence of increased exhaustion during the task. Therefore, often such children, to Unfortunately, many unnecessary symptoms are attributed. In this case, you need clearly distinguish between primary and secondary symptoms.
activity. An experienced diagnostician will immediately understand that the reason lies not in the cognitive abilities of the child, and in the presence of increased exhaustion during the task. Therefore, often such children, to Unfortunately, many unnecessary symptoms are attributed. In this case, you need clearly distinguish between primary and secondary symptoms.
Another interesting phenomenon has to do with memory. Often in children with ADHD there is an increased erasure of traces of memory in conditions interference, that is, interfering activity. Like this shows up? Imagine that you have to remember two text. First you read and, as you think, remember the first text. Then you are given a second text. Memorizing the second material, you forget the first one. This is a natural feature of our memory. But children with ADHD this manifests itself in an abnormal form. For example, we ask the child to remember first the first 3 words, and then the second 3 the words. He repeats the second group of words clearly, but the first 3 do not can remember. Similar memory problems also interfere with children's educational activity.
He repeats the second group of words clearly, but the first 3 do not can remember. Similar memory problems also interfere with children's educational activity.
In addition, these children have problems with voluntary control. Within the framework of the Luriev model for arbitrary control answers the so-called "third functional block in operation brain."
— Tell us more about this model.
— According to Luriev's model, there are three blocks of the brain. The first functional block is responsible for the level of brain activity. Second the block is cognitive. It is associated with processing, perception and remembering information coming from the outside world. Third the block is called the “programming, regulation and control block for the course of mental activity.
Children with ADHD often have secondary developmental delays. frontal cortex. This leads to derivative control problems and derived attention. For example, these children cannot focus on the task, can't control their behavior. This symptomatology of ADHD is especially pronounced in preschool children. It is clear that due to age the level of derivative control in these children is very immature. AT older age, closer to 9 years, in children with ADHD due to improvement of voluntary control over one's behavior occurs a decrease in the symptoms of this disorder, that is, it begins have a compensatory effect. However, ADHD does not go away, but only goes into a latent (hidden) form.
For example, these children cannot focus on the task, can't control their behavior. This symptomatology of ADHD is especially pronounced in preschool children. It is clear that due to age the level of derivative control in these children is very immature. AT older age, closer to 9 years, in children with ADHD due to improvement of voluntary control over one's behavior occurs a decrease in the symptoms of this disorder, that is, it begins have a compensatory effect. However, ADHD does not go away, but only goes into a latent (hidden) form.
And, finally, another secondary symptom is connected precisely with involuntary attention disorder. It's a symptom for the most part. refers to biology and the so-called orienting reflex for new incentives. When we hear an unexpected loud sound, we involuntarily pay attention to the source of the sound. This one is pure biological response allows us to respond effectively to potentially dangerous external influences.
Children with ADHD have a peculiar heightened sensitivity to all external influences, for example, to various soft sounds. A child with ADHD has an effect orienting reflex to both strong stimuli and weak. Outwardly, this manifests itself as increased distractibility. child. It is important to note that the child is not in the least is to blame - it is the indicative reflexes.
Imagine that you are walking through a forest at night. Your nervous system is this situation will become very sensitive. You will pay attention to any rustles and sounds. However, under normal conditions, when there is no danger, we react only to strong incentives. A child with ADHD constantly feels like he or she is is, figuratively speaking, in such a "dark and terrible forest." it leads to big problems at school, in communication with teachers and classmates.
So the symptoms of ADHD are quite complex and complex. To understand how a child with ADHD feels, imagine this situation. You are at the railway station, around various events are unfolding, many sounds, people flash before you, you are pushed, etc. And in these conditions you are offered to solve some problem. It is clear that you everything will be distracting and you will not be able to quickly and efficiently To solve the task. Of course, if you were asked to solve the same task at home in a calm environment, then you would have coped with it much faster. So, a child with ADHD seems to be all the time is in the situation of a railway station where its all distracts.
To understand how a child with ADHD feels, imagine this situation. You are at the railway station, around various events are unfolding, many sounds, people flash before you, you are pushed, etc. And in these conditions you are offered to solve some problem. It is clear that you everything will be distracting and you will not be able to quickly and efficiently To solve the task. Of course, if you were asked to solve the same task at home in a calm environment, then you would have coped with it much faster. So, a child with ADHD seems to be all the time is in the situation of a railway station where its all distracts.
In addition, orienting reflexes are accompanied by an increase child's anxiety.
The situation is aggravated by the fact that others react to the behavior of these children is inappropriate. Teachers shout at them parents, peers. Children with ADHD are under severe pressure from the outside world. And that just makes them bigger.
anxiety.
These kids are really hard. In life they are constantly face adaptation problems, even when they become adults. With age, the syndrome does not disappear anywhere. He only passes into a latent form, in which external symptoms do not appear clearly, but at the same time it is difficult for such a person concentrate on some work, he is overcome by a swarm of thoughts, he constantly distracted by various external and internal events.
— Are the causes of the syndrome known in children?
Almost all behavioral disorders in children are related to genetics. However, we cannot say for sure whether a child with genetic predisposition will form ADHD. The fact, that any phenotypic trait, including behavior, develops under the influence of two factors - genotype and environment. AT certain environmental conditions, a genetic predisposition to ADHD can lead to the development of this disorder, and in others conditions are not.
As risk factors that may lead to the development Attention Deficit Hyperactivity Disorder (ADHD) is traditionally referred to as birth trauma, hypoxia during childbirth, prematurity. However not always these factors lead to the development of ADHD. Especially if you have the child is not genetically predisposed to it disorder.
ADHD is always associated with a combination of genetic factors. predisposition and external adverse influences, especially in the first year of life. At this time, actively formed mechanism of neurodynamics in the brain, and external risk factors may lead to the development of this disorder. For example, emotional negative experiences of the child associated with the absence of the mother, may be such a risk factor.
In addition, children in the first year of life should develop in conditions of adequate sensory load. Level violation sensory information leads to adverse effects on reticular formation of the brain, which can lead to impaired neurodynamics and formation of ADHD.
- If the disorder is not given due attention, what could this lead to in the future?
- Imagine the world in which a child with deficiency syndrome lives attention and hyperactivity. At school, he most often does not succeed, on he is pressured by teachers, parents. This kid is trying to defend himself. often due to aggressive reactions. This, after all, may escalate into criminal behavior. And increased anxiety further may provoke the development of serious mental diseases, such as pathological depression. That is, at such children are at risk of developing adverse scenarios in life.
Therefore, it is necessary to treat them correctly already in the early childhood, to build the right atmosphere around such children, adequately respond to the manifestation of certain features, be more tolerant of them. This will reduce the risk development of deviant behavior.
— What practices are used to help such children? Are there any medications?
- If we talk about attention deficit disorder and hyperactivity in its gross form, it is necessary here comprehensive support. It includes three elements intervention.
It includes three elements intervention.
First, medical support is needed, especially when severe form of ADHD.
The second element is behavioral modification. There are many different techniques. But one of the most effective has to do with learning the so-called deep diaphragmatic breathing. A business is that the reticular formation, which is responsible for the general the level of activity of our brain, is sensitive to the lack of oxygen. Each of us has experienced severe exhaustion and inefficient work when in a stuffy room. If we improve the supply of oxygen to the reticular formation, the brain will work better. In a child with ADHD, breathing is often irregular and shallow. This impairs the supply of oxygen to the brain. situation can be improved if the child is taught the technique of correct diaphragmatic breathing.
By the way, children with ADHD are well helped by sports where deep breathing is practiced, for example, swimming.
Michael Phelps, a 23-time Olympic swimming champion, is also in actually suffered from ADHD. Phelps dealt with this disorder thanks in large part to swimming.
Stories like these inspire parents who reach out to me. for advice on ADHD. Such children are helped not only swimming, and any other sport where breathing plays an important role - kayaking, canoeing, skiing, running and other rhythmic and aerobic sports. Proper breathing brought to automatism is one of the most important helpers for children with ADHD.
The third direction is aimed at working with the family. This is about family therapy and creating the right atmosphere in which he lives child. As a rule, children with ADHD show inadequate forms of behavior from the point of view of the parents themselves. Moms, dads, grandmothers, brothers and sisters can be aggressive, punish child for inappropriate behavior. And this, as I said above, only exacerbates the already problematic anxiety in these children. Therefore, it is important that within the family, a child with ADHD develops harmonious and tolerant relationships. Under these conditions, higher the probability that he will form a mechanism of arbitrary regulation and control, and he will gradually get rid of bright manifestations of ADHD symptoms.
Therefore, it is important that within the family, a child with ADHD develops harmonious and tolerant relationships. Under these conditions, higher the probability that he will form a mechanism of arbitrary regulation and control, and he will gradually get rid of bright manifestations of ADHD symptoms.
The most unfavorable parenting strategy that leads to aggravation of ADHD symptoms - this is an authoritarian upbringing. At preschool age, it gives rise to a child increased infantilism, shifting responsibility to adult. A mature parenting strategy is to mother gradually transferred responsibility to the child in conditions joint activities.
- Tell us what you are working on today?
— Our laboratory of brain and neurocognitive development operates in several directions. One of the important areas of research employees of our laboratory is associated with the influence parent-child interaction on the development of young children and preschool age. We're trying to figure out what strategies and styles upbringing has the most beneficial effect on the development of the child, and which ones can increase the risk of developing various disorders, for example, ADHD.
We're trying to figure out what strategies and styles upbringing has the most beneficial effect on the development of the child, and which ones can increase the risk of developing various disorders, for example, ADHD.
Another important area is devoted to the study of digitalization, influence of virtual space and computer addiction on children development. In the international classification of diseases has already been introduced diagnosis called digital addiction or digital addiction. Unfortunately, this is how the modern environment works - it provokes a situation in which the child is immersed early in the virtual space and becomes dependent on it. Some studies show that the child's early interaction with digital environment negatively affects the development of many basic brain mechanisms. It is clear that digitalization is a reality, from which is now nowhere to go. However, it is very important to correctly to introduce the child to the digital environment in a timely manner, to adapt him to this new reality.
The third aspect of research is devoted to the formation of a unified system diagnosis of preschool children, which in Russia so far no. Unfortunately, we do not have a generally accepted standard for which we can assess the development of children at preschool age, in order to timely detect atypical manifestations and the risk of deviant behavior. The fact is that preschool age is a period in which during which most of the basic brain cells are formed mechanisms. Therefore, any mistakes are fraught with serious consequences. in future. We must learn to quickly identify the causes deviant behavior and deviant development of children, which will basis for the development of effective methods of correction. Necessary time to change the environment of a child with the risk of developing deviant behavior, adjust the parameters of its development in order to mitigate the risks of various disorders. That's why we need a unified system of sensitive diagnostics that will allow to identify not only gross violations in development, but also minimal deviations in order to help the child in time.
Preschool age is a very important period in development, because the child's brain is sensitive both to adverse external influences as well as favorable ones. Quickly noticing the deviation the specialist can change the child's environment, which will lead to to the rapid restoration of development mechanisms.
Therefore, at this age it is so important to create for the child the most favorable environment for the development of basic brain mechanisms.
Today, unfortunately, many parents focus on the formation of school skills in preschool age - reading, letters, bills. It is not right. So the parents ahead of events. Figuratively speaking, they build the roof of the house, not completing the foundation and walls. We must strictly follow a certain sequence of brain development, take into account individual characteristics of the child, including psychological.
The basic mechanisms of the brain must be formed in preschool age with the help of a variety of motor activities: gymnastics, dancing, sports, drawing, classes music and so on. And only then, when the foundation has been created, can it is easy to switch to the formation of a variety of school skills - letters, readings, bills, etc.
And only then, when the foundation has been created, can it is easy to switch to the formation of a variety of school skills - letters, readings, bills, etc.
Today, together with Tomsk State University, we we are working on creating a unified diagnostic system that is easy to fit into the system of preschool education. It is necessary that she allowed to effectively identify risks at an early stage and gave the ability to quickly correct the development of the child.
— What advice would you give to parents whose children Have you been diagnosed with ADHD?
- Unfortunately, sometimes it happens that a child is diagnosed ADHD, but he doesn't really have that syndrome. I often I am facing this kind of overdiagnosis.
Therefore, it is important not to rely on the opinion of only one specialist. It is necessary to re-diagnose with another doctor, to make sure if the child really has a syndrome attention deficit and hyperactivity.

If the syndrome is confirmed by at least two specialists, then the child comprehensive support is required. Unfortunately, parents often rely on drugs. Of course, the effect of drugs is, but it short-term. If the child stops using them, then symptoms will return, and in some cases even worsen. Therefore, it is important to solve the problem comprehensively. Together with right built medical support must be carried out behavioral therapy, in particular, using the technique diaphragmatic breathing.
And, of course, parents should not forget that often their own misbehavior exacerbates the situation. AT In some cases, parents need to work even harder on yourself and your own behavior. Sometimes shown and personal therapy, which involves a change of position in relation to to kid. Sometimes, such changes give a stronger effect, than other influences or interventions.
Causes of ADHD. Neuropsychological approach | Defectology Prof.
Attention deficit hyperactivity disorder is a neurological-behavioral developmental disorder that begins in childhood.
ADHD causes a lot of controversy. From a neurological point of view, ADHD is seen as a persistent and chronic syndrome for which no cure has been found. According to some reports in the United States population, this disorder is present in 3-5% of people, including both children and adults. According to the current diagnostic criteria, ADHD can be diagnosed starting in late preschool or school age, since assessment of the child's behavior in at least two settings (for example, at home and at school) is necessary to meet the requirements for diagnosis. The presence of learning disabilities and social functioning is a necessary criterion for establishing a diagnosis of ADHD.
The etiology of ADHD is not well understood. Most researchers suggest the genetic nature of the syndrome. Families of children with attention deficit hyperactivity disorder often have close relatives who had similar disorders at school age. In the pedigrees of children with ADHD, there is also often a burden for obsessive-compulsive syndrome, tics, and Gilles de la Tourette's syndrome. Probably, there is a genetically determined relationship of neurotransmitter disorders in the brain in these pathological conditions.
Families of children with attention deficit hyperactivity disorder often have close relatives who had similar disorders at school age. In the pedigrees of children with ADHD, there is also often a burden for obsessive-compulsive syndrome, tics, and Gilles de la Tourette's syndrome. Probably, there is a genetically determined relationship of neurotransmitter disorders in the brain in these pathological conditions.
It is assumed that ADHD is determined by mutations in 3 genes that regulate dopamine metabolism - the D4 receptor gene, the D2 receptor gene, and the gene responsible for dopamine transport. The carriers of the mutant gene are children with the most pronounced hyperactivity. Along with genetic factors, family, perinatal and perinatal risk factors for the development of attention deficit hyperactivity disorder are distinguished.
Based on H.H. Zavadenko /5/, the occurrence of ADHD due to early damage to the central nervous system during pregnancy and childbirth occurs in 84% of cases, due to genetic causes - in 57%, the negative effect of family factors can be traced in 63%.
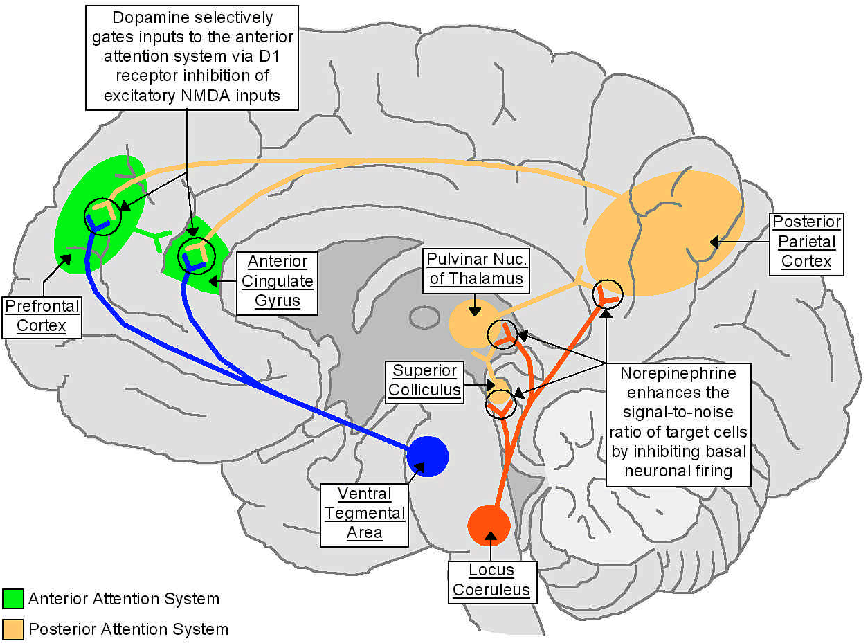
It is assumed that the pathogenesis of the syndrome is based on disturbances in the activating system of the reticular formation, which contributes to the coordination of learning and memory, the processing of incoming information and the spontaneous maintenance of attention. Violations of the activating function of the reticular formation, apparently, are associated with a lack of norepinephrine in it. The impossibility of adequate processing of information leads to the fact that various visual, sound, emotional stimuli become redundant for the child, causing anxiety, irritation and aggressiveness. Violations in the functioning of the reticular formation predetermine secondary disorders of the neurotransmitter metabolism of the brain. The theory of the relationship of hyperactivity with dopamine metabolism disorders has numerous confirmations, in particular, the success of the treatment of attention deficit/hyperactivity disorder with dopaminergic drugs. It is possible that disorders of neurotransmitter metabolism leading to hyperactivity are associated with mutations in genes that regulate the functions of dopamine receptors. Separate biochemical studies in children with attention deficit/hyperactivity disorder indicate that the metabolism of not only dopamine, but also other neurotransmitters, serotonin and noradrenaline, is disturbed in the brain.
Separate biochemical studies in children with attention deficit/hyperactivity disorder indicate that the metabolism of not only dopamine, but also other neurotransmitters, serotonin and noradrenaline, is disturbed in the brain.
Neuropsychological studies show heterogeneity in the manifestations of ADHD and allow us to identify several variants of this syndrome. Thus, a longitudinal study of children from 5 to 9 years old by E.A. Osipova and N.V. Pankratova showed 4 types of deviations of higher mental functions.
The first type occurred in 42% of cases and was associated with a deficit in the basal structures of the brain, a delay in the formation of functional left hemispheric dominance, and a lack of cortical-subcortical regulation. In the process of growing up, children with this type of ADHD are characterized by a decrease in symptoms and normalization of behavior. In ontogenesis, there was a delay in determining the dominant hand, difficulties in the formation and retention of motor programs, violations of mnestic activity in the selectivity link.
The second type of ADHD, identified in 20% of the examined, was characterized by dysfunction of the right hemisphere in combination with deficiency of the basal (subcortical) structures of the brain. This variant of ontogeny was distinguished by pronounced instability of age dynamics. The development of children and the acquisition of cognitive and social skills were accompanied by periodic failures and increased hyperactivity. The peak of hyperactivity and disturbances in interaction with peers in this group of children was at the age of 5 years. At the age of 7-8 years, there was a positive trend, and at 9years - recurrence of symptoms. The children showed polymodal disturbances in mnestic activity in the link of selectivity and a deficiency in the implementation of motor functions, as in the children of the first group.
The third type of ADHD development was detected in 29% of the examined. They had a primary functional deficiency of the basal brain structures, which slowed down the formation of spatial functions (posterior parts of the right hemisphere), as well as programming and control functions (frontal lobes of the left hemisphere), intellectual indicators were reduced. However, children of this type often showed slow but positive age dynamics.
However, children of this type often showed slow but positive age dynamics.
The fourth type of ADHD was identified in 9% of cases and was characterized by the preservation of the basal structures of the brain with a pronounced unformed regulatory structures (frontal lobes of the left hemisphere). There was a lack of speech programming and control in ensuring the consistent execution of serial actions, inertia in reproducing the material being learned, perseveration, instability of social contacts, aggression, and uncontrollability.
Research results T.G. Goryacheva and A.S. Sultanova /12/ allowed to divide children with ADHD into 3 groups. The first group (70%) consisted of children with primary dysfunctions of the brain stem and subcortical structures, in whom the functional development of the prefrontal cortex areas suffers for the second time. The second group (about 20%) included children with primary dysfunctions of the stem and subcortical structures of the brain, in whom the functional development of the cortex, predominantly in the basal frontal regions, suffers secondarily. The third group of children (about 10%) was characterized by primary functional insufficiency of the prefrontal sections of the cerebral cortex. The authors emphasize that attention disorders in children of the first two groups are direct manifestations of an activation deficit, characterized by increased exhaustion and the absence of an increase in attention and a decrease in hyperactivity in a game situation. In contrast to them, the children of the third group managed to overcome their distractibility with a special organization of the material that increases motivation, or with the introduction of a game context when performing tasks.
The third group of children (about 10%) was characterized by primary functional insufficiency of the prefrontal sections of the cerebral cortex. The authors emphasize that attention disorders in children of the first two groups are direct manifestations of an activation deficit, characterized by increased exhaustion and the absence of an increase in attention and a decrease in hyperactivity in a game situation. In contrast to them, the children of the third group managed to overcome their distractibility with a special organization of the material that increases motivation, or with the introduction of a game context when performing tasks.
Comparing these two studies, it can be noted that we are talking mainly about two types of deficiency: dysfunction of I and III structural-functional blocks of the brain according to A.R. Luria. The weakness of the block of regulation and maintenance of mental tone and wakefulness (block I) is manifested in the imbalance of the background components of movements provided by the upper sections of the extrapyramidal system: intensity, pace, spontaneity of motor reactions.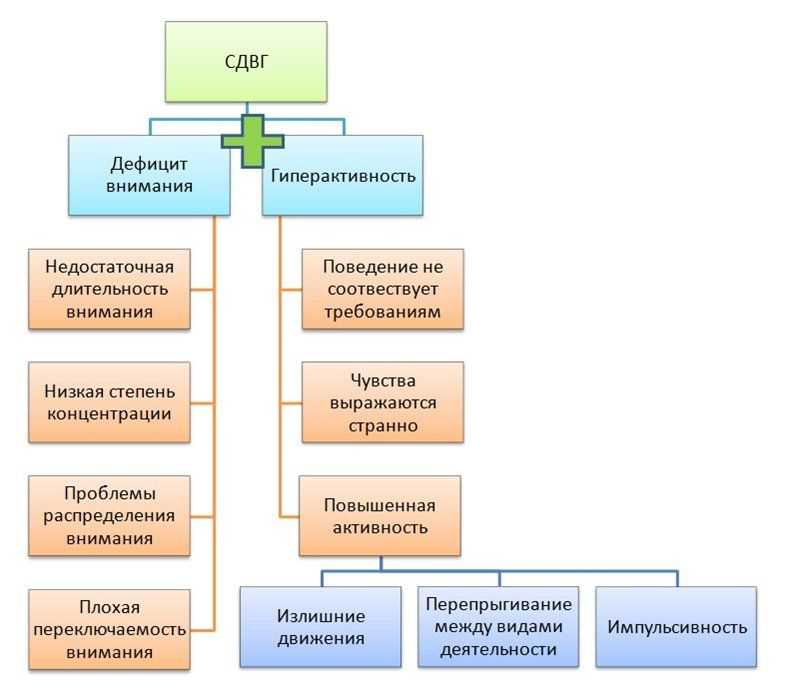 The weakness of the block of regulation, programming and control (block III) manifests itself in the form of difficulties in voluntary inhibition of impulsivity and downward cortical control over the background components of movements.
The weakness of the block of regulation, programming and control (block III) manifests itself in the form of difficulties in voluntary inhibition of impulsivity and downward cortical control over the background components of movements.
The main cause of damage to parts of the child's brain is hypoxia during childbirth, that is, a decrease in the supply of a sufficient amount of oxygen to the brain. Moreover, hypoxia is dangerous, which occurs quickly within a few minutes (acute hypoxia or fetal distress), with which the defense mechanisms of the fetus cannot cope. Acute hypoxia can cause suffering and death of areas of the white matter of the brain. Such hypoxia can occur, first of all, during childbirth.
During cerebral hypoxia during childbirth, the cells of the cerebral cortex (neurons of the cerebral cortex) suffer least of all, since they begin to work only after the birth of a child, during childbirth they need a minimum of oxygen.
During hypoxia during childbirth, blood is redistributed and, first of all, goes to the cells of the brain stem, where the most important centers for life are located - the center for regulating blood circulation and the center for regulating respiration. (From it, after the birth of the child, a signal will come to take a breath.) Thus, the most sensitive to hypoxia in the fetus are neuroglial cells (oligodendrocytes), which are in large numbers between the cortex and the brain stem, in the subcortical zone - the White Matter region of the brain (BVM).
(From it, after the birth of the child, a signal will come to take a breath.) Thus, the most sensitive to hypoxia in the fetus are neuroglial cells (oligodendrocytes), which are in large numbers between the cortex and the brain stem, in the subcortical zone - the White Matter region of the brain (BVM).
Neuroglial cells after the birth of a child must ensure the process of myelination. Each cell of the cerebral cortex - a neuron - has processes that connect it to other neurons, and the longest process (axon) goes to the neurons of the brain stem. As soon as myelination occurs - covering these processes with a special sheath, the neurons of the cerebral cortex can send signals to the subcortex and brain stem and receive response signals.
The more neuroglial cells suffer from hypoxia during childbirth, the greater the difficulties for the neurons of the cerebral cortex in establishing connections with the subcortex and brain stem, since the myelination process is disrupted. That is, the neurons of the cerebral cortex cannot fully and during (according to the program recorded in their genes) regulate and control the underlying parts of the brain. Part of the neurons of the cortex simply die when it is impossible to perform their functions.
That is, the neurons of the cerebral cortex cannot fully and during (according to the program recorded in their genes) regulate and control the underlying parts of the brain. Part of the neurons of the cortex simply die when it is impossible to perform their functions.
Impaired regulation of muscle tone and reflexes. By the age of 1-1.5 years, cortical neurons usually establish enough connections for muscle tone and reflexes to normalize and the child to walk on its own (as recorded in the gene program for the development of the organism). In the development of movements, not only the frontal, but also other parts of the brain are involved, which provides great compensatory opportunities for the normalization of movement disorders.
Social development of the child begins at the age of 1.5 - 2 years. The child has a genetically inherent fear of adults (parents), the desire to repeat actions and words after adults, obey the comments of adults, understand the word “no” (albeit not always obey), be afraid of punishment and enjoy praise from adults (parents).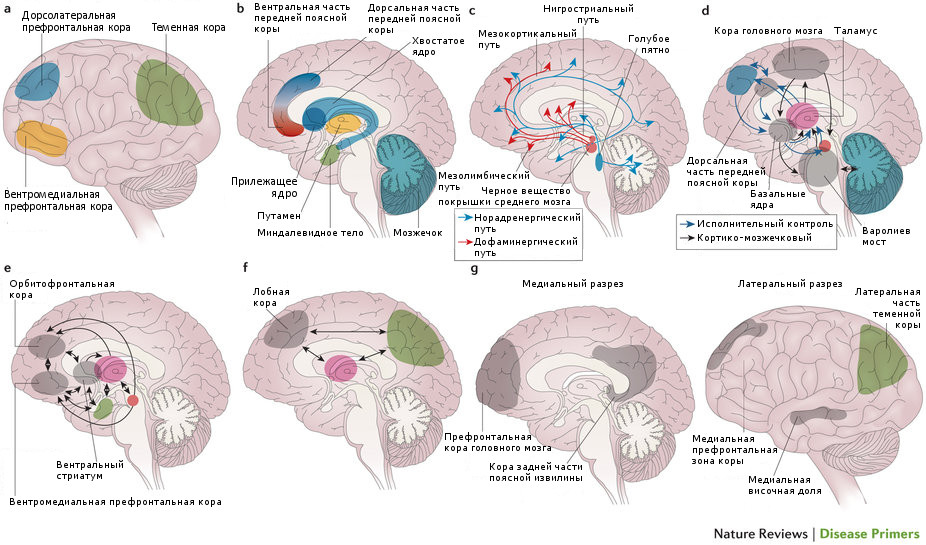 That is, the possibility of raising a child is provided at the genetic level in the program for the development of the child's central nervous system. Moreover, this genetic program for the development of social maturation (social adaptation and behavior) is evolutionarily honed and selected, otherwise the child would not be able to survive among the world around him, full of real dangers for maintaining health and life itself.
That is, the possibility of raising a child is provided at the genetic level in the program for the development of the child's central nervous system. Moreover, this genetic program for the development of social maturation (social adaptation and behavior) is evolutionarily honed and selected, otherwise the child would not be able to survive among the world around him, full of real dangers for maintaining health and life itself.
In case of insufficiency of connections in the neurons of the cortex responsible (according to the gene program) for this social development, behavioral disorders that do not correspond to the age norm appear - violations of social adaptation. Conduct disorders may in some cases be simply inherent in a given child, due to its individual characteristics, or be a reflection of certain periods of the child's development.
Behavioral disorders include: problems with education, communication, behavioral discipline, eating, sleeping, difficulties in acquiring tidying skills, hyperactivity. A high degree of activity and a tendency to noisy games is typical for children from 2 to 4 years old, and, as it were, is considered the age norm. But hyperactivity, combined with inattention and impulsivity, persisting in a child after 4 years of age, indicates the presence of ADHD.
A high degree of activity and a tendency to noisy games is typical for children from 2 to 4 years old, and, as it were, is considered the age norm. But hyperactivity, combined with inattention and impulsivity, persisting in a child after 4 years of age, indicates the presence of ADHD.
First of all, the regulation of one's emotions and sensations is disturbed. Children are emotionally labile (unstable), irritable, quick-tempered. But, on the other hand, they are characterized by increased vulnerability and low self-esteem.
The intellect usually develops successfully, but its implementation is hampered by poor concentration of attention: children cannot fully listen to the conditions of the problem, impulsively make rash decisions. They quickly get bored with monotonous work, mechanical memorization of a large amount of material, they often do not complete the work they have begun...
The main cause of violations of the development of the central nervous system of a child are damage (infarctions) of the BVM (white matter of the brain) during acute hypoxia (distress) and birth trauma of the fetus during childbirth (intranatal period).
The main threat and cause of the development of acute hypoxia and birth trauma of the fetus during childbirth is the medicinal and mechanical “preparation” of the cervix and stimulation of labor, contractions and attempts.
As Bortsov A.V. /20/, only a strict, complete ban on obstetricians, the use of “modern” medications in childbirth and medical manipulations to induce and stimulate labor, can reduce the threat of brain damage to newborn children, and dramatically reduce the number of newborns with brain damage.
Only the refusal of obstetricians from active aggressive labor management will return our women to natural childbirth without induction and stimulation.
Natural childbirth is the only safe childbirth that gives the greatest chance of preserving the undamaged central nervous system of the newborn baby!
Literature:
1. LS Chutko et al. “Principles of helping children with attention deficit hyperactivity disorder”. Institute of the Human Brain RAS, St. Petersburg, Journal of Neurology Pharmacotherapy of Cognitive Impairments in Childhood. Clinic of Nervous Diseases of the Moscow Medical Academy named after I.M. Sechenov, Moscow, Journal “Farmateka”, No. 15, 2008
Institute of the Human Brain RAS, St. Petersburg, Journal of Neurology Pharmacotherapy of Cognitive Impairments in Childhood. Clinic of Nervous Diseases of the Moscow Medical Academy named after I.M. Sechenov, Moscow, Journal “Farmateka”, No. 15, 2008
2. A.I. Zakharov. "Prevention of deviations in the child's behavior", St. Petersburg, 1997.
3. B.R. Yaremenko, A.B. Yaremenko, T.B. Goryainov. "Minimal dysfunctions of the brain in children", St. Petersburg, 2002.
4. Gasanov R.F. "Modern ideas about the etiology of attention deficit disorder (literature review)." Journal No. 1, 2010, “Review of Psychiatry and Medical Psychology. Bekhterev." Research Institute of Psychoneurological them. V.M. Bekhtereva, St. Petersburg.
5. Zavadenko, N.N. Hyperactivity and attention deficit in childhood / N.N. Zavadenko. — M.: Academy, 2005. — 256 p.
6. Wallets, D.A. Features of voluntary regulation of activity in children aged 5-6 years with signs of attention deficit and hyperactivity / D. A. Wallets, O.A. Semenova // Almanac "New Research". - M., 2009. - No. 2 (19). - S. 47-48.
A. Wallets, O.A. Semenova // Almanac "New Research". - M., 2009. - No. 2 (19). - S. 47-48.
7. Developmental psychology / ed. T.D. Martsinkovskaya. — M.: Academy, 2008. — 528 p.
8. Lokhov, M.I. Analysis of the features of the electroencephalogram in children with attention deficit disorder and hyperactivity / Lokhov, Yu.A. Fesenko, L.P. Rubina // Journal of Review of Psychiatry and Medical Psychology named after. V.M. Bekhterev. - T. 2. - No. 2. - 2005. - S. 27-38.
9. Flor-Henry, P. Cerebral basis of psychopathology / P. Flor-Henry. - Wright, Boston etc., 1983. - 254 p.
10. Itil, T.M. The significance of quantitative pharmacy EEG in discovery and classification of psychotropic drugs / T.M. Itil // EEG Drug Res. - N. Y., 1982. - P. 131-150.
11. Agris, A.R. Neuropsychological and neurophysiological studies of variants of attention deficit hyperactivity disorder / A.R. Agris, O.I. Egorova, E.Yu. Matveeva, A.A. Romanova // Modern foreign psychology. - 2012. - No. 1. - P. 39-46.
- 2012. - No. 1. - P. 39-46.
12. Goryacheva, T.G. Neuropsychological features of the mental development of children with hyperactivity syndrome / T.G. Goryacheva, A.S. Sultanova // V.M. Bekhterev and modern psychology. - Vol. 2, no. 3. - Kazan, 2005. - S. 74-79.
13. Barkley, R.A. ADHD and the Nature of Self-Control / R.A. Barkley. - New York: Guilford Press, 1997. - 266 p.
14. Petrukhin, A.S. Neurology of childhood / A.S. Petrukhin. - M .: Medicine, 2004. - 414 p.
15. Pylaeva, N.M. Attention School. Methods of development and correction of attention in children 5-7 years old. Methodological guide / N.M. Pylaeva, T.V. Akhutin. — M.: Linka-Press, 2005. — 48 p.
16. Actual problems of childhood neuropsychology / ed. L.S. Tsvetkova. — M.: MPSI, 2010. — 320 p.
17. Korsakova, N.K. Underachieving children: neuropsychological diagnosis of learning difficulties / N.K. Korsakova, Yu.V. Mikadze, E.Yu. Balashova. - M .: Pedagogical Society of Russia, 2001.