Infant feeding methods
Methods: Breastfeeding and Infant Feeding Practices | Breastfeeding
Infant Feeding Practices Study II and Its Year Six Follow-Up
The Infant Feeding Practices Study II (IFPS II) was a longitudinal survey about infant feeding and care. Data were collected approximately monthly beginning in the third trimester of pregnancy and through the infant’s first year.
The Participants: Women and Their Children During the First Year of Life
Between May and December 2005, approximately 4,000 pregnant women from across the nation were recruited to participate in the Infant Feeding Practices Study II (IFPS II). To maximize participation rates, the study selected the sample from a national consumer opinion panel consisting of 500,000 households from throughout the United States.
To qualify for the IFPS II, the mother had to be at least 18 years old and the infant had to be a singleton born at ≥35 weeks gestation, weighing at least 5 lbs, and without medical conditions that would affect feeding. About 2,000 mother-infant dyads qualified and completed mail surveys of IFPS II.
Data Collection
With the exception of a brief telephone interview near the time of the infant’s birth, all IFPS II data were collected using mailed questionnaires.
Measures
The IFPS II provides detailed information about the following:
- Foods fed to infants, including breast milk, infant formula and solid foods.
- Factors that may contribute to infant feeding practices and to breastfeeding success.
- Mothers’ intrapartum hospital experiences, sources of support, and postpartum depression.
- Mothers’ employment status and child care arrangements.
- Infant sleeping arrangements.
- Other issues such as food allergies, experiences with breast pumps, and WIC participation.
- Diets of pregnant and postpartum women.
Study methods are described in this publication:
Fein SB, Labiner-Wolfe J, Shealy KR, Li R, Chen J, Grummer-Strawn LM. Infant Feeding Practices
Infant Feeding Practices
Study II: Study Methods. Pediatrics. 2008;122(suppl 2):S28–S35. [PDF-284KB]external icon Accessed July 13, 2017.
Top of Page
Year Six Follow-Up Study
Methods
The Year Six Follow-Up Study (Y6FU) of the mothers and children who participated in the IFPS II was a cross-sectional study conducted to characterize the health, development, and dietary patterns of the children at 6 years of age.
The Participants: Women and Their Children at Six Years of Age
Between March and June of 2012, when children from IFPS II were 6 years of age, mothers were re-contacted to participate in a cross-sectional mail survey for a follow-up. To qualify for Y6FU, the mother had to have answered at least the prenatal and neonatal IFPS II questionnaires and not have been disqualified afterwards due to some medical reasons that affected infant feeding. Of 2,958 mothers who qualified for Y6FU using the IFPS II, 1,542 women participated in the follow-up study yielding a response rate of 52 percent.
Data Collection
For Y6FU, two methods were used to collect the data to maximize the response rate. Mothers were first sent a questionnaire through the mail; however, those who did not respond after two attempts of mailed questionnaires were contacted by telephone to obtain the same information by telephone interview.
Measures
The Y6FU provides detailed information about the following:
- Child’s weight and height.
- Child’s physical, oral health, behavioral, and development outcomes.
- Child’s food allergy.
- Child’s dietary practice and use of herbal or botanical remedies.
- Child’s eating behaviors.
- Home food environment.
- Home environment and exposure to inhaled contaminants.
- Child’s physical activity level, screen time, and sleep patterns.
- Information about mothers, such as anthropometry, physical activity, weight, height, any present or past depression, pregnancy and breastfeeding history, work status, and maternal feeding style.
Study methods are described in this publication:
Fein SB, Li R, Chen J, Scanlon KS, Grummer-Strawn LM.
Methods for the year 6 follow-up study of children in the Infant Feeding Practices Study II. Pediatrics. 2014;134(suppl 1):S4–S12. pdf icon[PDF_655KB]external icon Accessed July 12, 2017.
Top of Page
Baby-Led Weaning is a New Way of Feeding Your Baby - Learn More About it
Every parent remembers when they first introduced their baby to solid foods. This momentous occasion of spoon-feeding them pureed food is considered a major milestone for babies and their parents.
Today however, more and more parents are opting to skip the applesauce and mashed sweet potatoes and instead are adopting a new feeding technique called “baby-led weaning” ( or BLW) for their babies. This alternative approach to feeding, first introduced in the UK a decade ago, involves introducing solid chunks of foods much earlier on by placing them on the baby’s high chair and letting them grasp the food and feed themselves directly.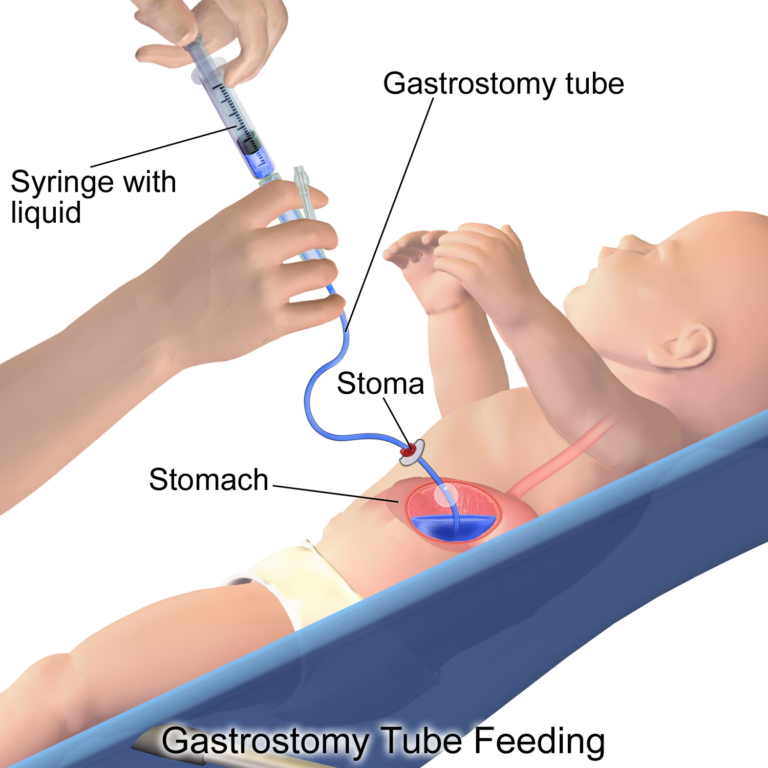 As the name implies, feeding time is led by the baby as they determine the pace and the amount of food they consume; basically, baby-led weaning puts the baby in charge.
As the name implies, feeding time is led by the baby as they determine the pace and the amount of food they consume; basically, baby-led weaning puts the baby in charge.
While children all develop at different paces, advocates of baby-led weaning agree that this method of eating shouldn’t be introduced until the baby is ready. Cues to begin BLW include making sure that your baby can sit up straight unassisted, have good neck strength and be able move food to the back of their mouth with up and down jaw movements. Most babies develop these skills by the sixth month, but some babies may not fully develop them until they are nine months old.
Proponents of BLW believe that it holds many benefits, including enhancing baby’s hand-eye coordination and other fine motor skills, including using their thumb and index finger to grasp their food. They also feel that it will produce healthier eaters than spoon-fed babies because BLW eaters get to choose how much they eat as opposed to traditional feeding methods, which sometimes results in force feeding. Other advantages that BLW supporters claim to be true is that it creates a more enjoyable feeding experience for babies and less stress on their parents.
Other advantages that BLW supporters claim to be true is that it creates a more enjoyable feeding experience for babies and less stress on their parents.
Detractors of baby-led weaning feeders point out that these babies are generally underweight as compared to spoon-fed babies because they simply do not ingest that much when they are first introduced to this way of eating due to difficulties grabbing food. BLW babies also tend to be iron-deficient because they aren’t consuming the iron-fortified cereals that spoon–fed babies typically eat. Lastly, a big concern for many parents is the increased choking hazards associated with BLW, and while the American Academy of Pediatrics doesn’t have opinion of BLW, they do state that babies are ready for solid food once they are ready to sit up on their own and bring their hand to their mouth.
If you are considering baby led weaning for your child, here are a few tips:
- Continue breast feeding and / or formula feeding as this will continue to be your baby’s biggest source of nutrition until they are 12 months old.
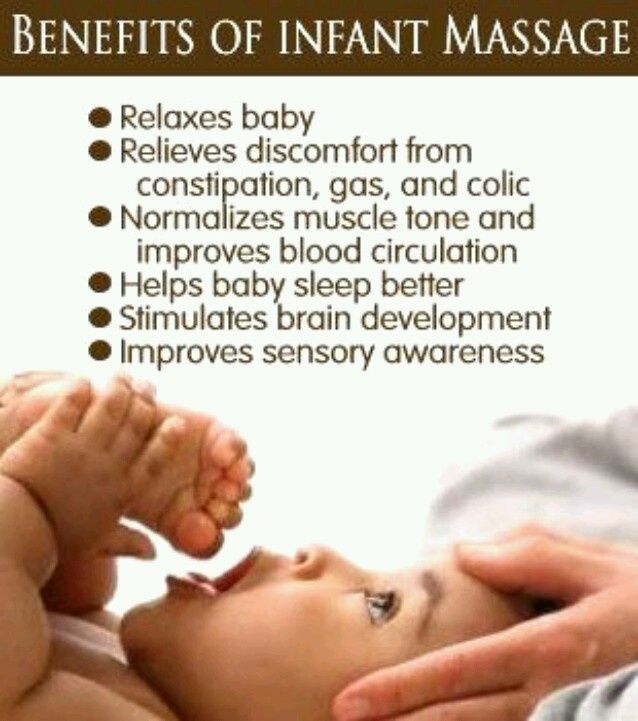
- Begin BLW feedings with softer foods, such as ripe fruits, cooked egg yolks, and shredded meats, poultry and fish.
- Avoid foods that can pose as choking hazards, such as nuts, grapes, popcorn, or foods cut into coin shapes, like hot dogs.
- Do not leave your child unattended during BLW feeding times. Continue to supervise and socialize with them while they eat and to have them eat when the rest of the family does.
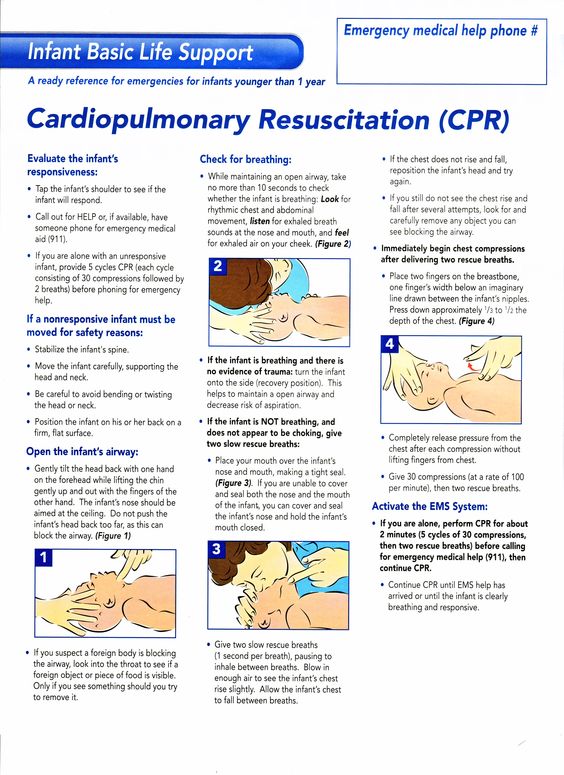
- Don’t panic if your baby gags as it is a safe a natural reflex. Instead of overreacting, prepare for a choking event by familiarizing yourself with the infant-specific Heimlich maneuver.
- Introduce new foods one at a time to pinpoint potential food allergies. A recommended length of time is three to four days between foods.
- The goal of BLW is to let your baby explore eating at their own pace. This may include the smashing, smearing, or dropping of food, so prepare for a mess.
Before you decide to adopt BLW to your child, it is a good idea to discuss with your child’s pediatrician as it may not be a good idea for all babies, especially those babies with known developmental delays or neurological issues.
To make an appointment with a pediatrician at Flushing Hospital’s Ambulatory Care Center, please call 718-670-5486.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.
Sitemap
State autonomous professional
educational institution
Republic of Bashkortostan
"Salavat Medical College"
453261 Republic of Bashkortostan
Salavat, st. Furmanova, 4
Phone/fax: (3476)-38-78-83
e-mail: [email protected]
- College information
- Basic information nine0013 Structure and governing bodies of the college
- Documents
- Education
- Educational standards and requirements
- Manual.
 Teaching staff
Teaching staff - Logistics and equipment of the educational process
- Scholarships and other financial support
- Paid educational services
- Financial and business activities
- Vacancies for reception (transfer)
- Personal data processing nine0013 Anti-corruption
- Legal framework for combating extremism and terrorism
- Vacancies
- Information security
- Olympics
- Mentoring nine0013 Available environment
- International cooperation
- Applicant
- Control figures for the reception of citizens
- Admission Rules nine0013 Regulations on Individual Achievements
- Fundamentals
- Regulations
- Culture and sports
- Dormitory
- Student Council nine0013 Life safety
- Reference information
- Educational and methodical work
- Additional education
- Republican information and training pedagogical seminars
- Hotline
- Feedback
- Contacts of controlling organizations
This page does not exist.
|
Breastfeeding technique
Milk composition
During breastfeeding, the composition of milk changes. In the first days after childbirth (and for some women even at the end of pregnancy), the so-called colostrum appears, it differs from later milk in the content of proteins, fats, carbohydrates, water and other substances, which facilitates the transition from intrauterine nutrition to extrauterine. On the 3-5th day there is a "rush" of milk, and within 10-15 days transitional milk is formed, which later becomes mature. nine0006
In the first days after childbirth (and for some women even at the end of pregnancy), the so-called colostrum appears, it differs from later milk in the content of proteins, fats, carbohydrates, water and other substances, which facilitates the transition from intrauterine nutrition to extrauterine. On the 3-5th day there is a "rush" of milk, and within 10-15 days transitional milk is formed, which later becomes mature. nine0006
Ideally, first breastfeeding should occur within 20 minutes of delivery. During this period of time, the area of the nipple and areola is the most sensitive, which facilitates the start of milk production (lactation).
| Nutrients | Unit | Colostrum | Transitional milk | Mature milk |
| Proteins | g | 22 | 17. | 10 |
| Fats | g | nine0007 25 | 44 | 45 |
| Carbohydrates | g | 57 | 64 | 73 |
| Calories | kcal | Day 1 to Day 5 | 700 | 700 |
Comparative composition of some components of colostrum, transitional and mature human milk (per 1 liter)
Technique
It is necessary to put the baby to the breast in such a way that not only the nipple itself, but also the areola area is in the baby’s mouth. This prevents the appearance of cracks in the nipple. The baby's nose should be open at the same time. During feeding, you need to pay attention not only to the activity of sucking movements, but also to the sound characteristic of swallowing. nine0006
nine0006
Twin feeding technique: The twins are placed alternately on the breast. The more restless baby is first placed on the breast, the second baby is placed on the same breast, and then the other breast is fed. The next feeding should begin with the breast from which the second child was fed.
Some mothers practice feeding two babies at once, leaning over them.
After feeding, the baby should be held in an upright position for a while so that he burps the swallowed air. nine0006
After you have fed and held your baby upright, he can be put to bed.
Currently, many positions on the method of breastfeeding have been revised. Most nutritionists recommend feeding on demand (including nighttime hours) rather than on a schedule. The free-feeding regimen stimulates lactation, a rush of milk, prevents stagnation of milk in the mammary gland (lactostasis), as well as nervous breakdowns in family members due to hungry crying of the child. At first, newborns feed irregularly, the number of attachments to the breast and the intervals between feedings can vary greatly, but then the child will develop his own regimen and the process of breastfeeding will go much easier.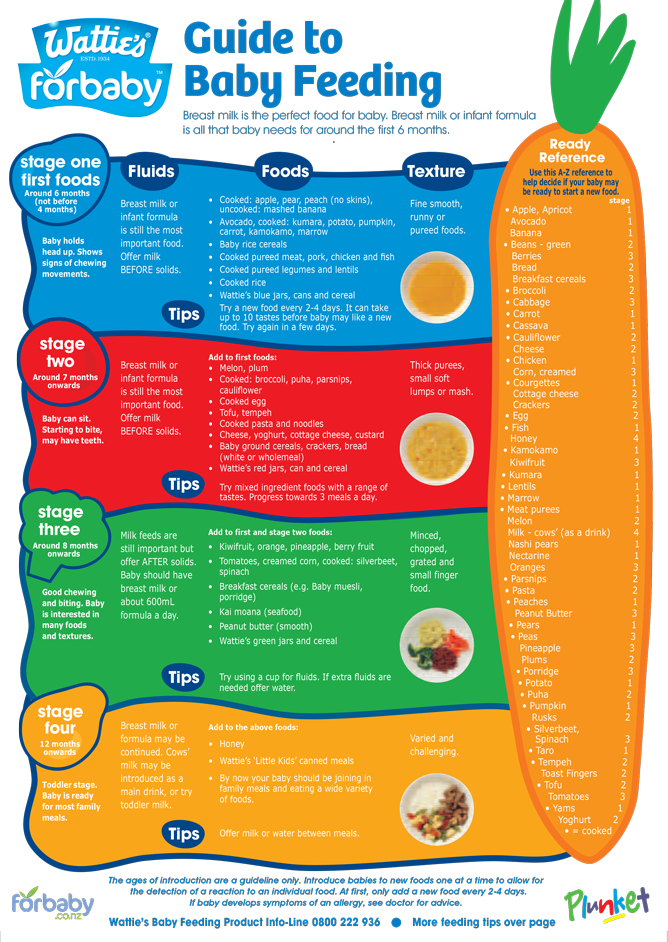 The time spent at the breast is not recommended to be artificially limited, since during feeding, early or foremilk, which contains a large amount of water, is first released, and then later or hindmilk, which is rich in fat and other nutrients. Thus, at first the need for water is provided, and then the child is saturated. That is why one should not prematurely take one breast and offer another. It is better if the child suckles one breast at each feeding. If one breast has already been completely emptied, and the child has not yet been satiated, then another can be offered, while the next feeding should be started from the breast that ended the previous one. With an on-demand feeding regimen and frequent attachment to the breast, there is usually no need to pump. You need to express if there is too much milk and the baby is not able to completely empty the breast (prevention of milk stasis), or if you want to leave milk for feeding the baby in your absence. Expressed milk can be stored in the refrigerator for 24 hours and in the freezer for up to two weeks.
The time spent at the breast is not recommended to be artificially limited, since during feeding, early or foremilk, which contains a large amount of water, is first released, and then later or hindmilk, which is rich in fat and other nutrients. Thus, at first the need for water is provided, and then the child is saturated. That is why one should not prematurely take one breast and offer another. It is better if the child suckles one breast at each feeding. If one breast has already been completely emptied, and the child has not yet been satiated, then another can be offered, while the next feeding should be started from the breast that ended the previous one. With an on-demand feeding regimen and frequent attachment to the breast, there is usually no need to pump. You need to express if there is too much milk and the baby is not able to completely empty the breast (prevention of milk stasis), or if you want to leave milk for feeding the baby in your absence. Expressed milk can be stored in the refrigerator for 24 hours and in the freezer for up to two weeks. nine0006
nine0006
Expressed milk can be pasteurized if necessary. This is done as follows: milk bottles are closed with clean cotton-gauze plugs and placed in a pot of water (the water level in the pan should be higher than the milk level), after which they are boiled for 3–5 minutes. It is better to pasteurize milk just before feeding. If necessary, milk is stored in the refrigerator for no more than a day.
In our opinion, it is better not to accustom children to pacifiers, as difficulties may arise when sucking the breast, since when sucking pacifiers, the muscles of the cheeks work mainly, and when sucking the breast, the tongue and jaws. nine0006
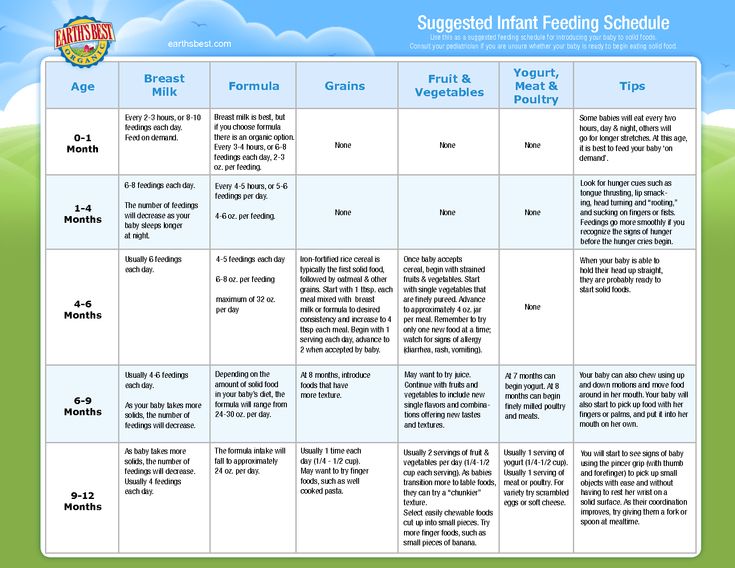
Is it necessary to supplement the baby with water when breastfeeding
When breastfeeding, it is not necessary to supplement the baby with water without medical indications. When supplementing, the baby will suck out less milk, and this will lead to a decrease in its [milk] formation.
Is it necessary to give vitamins to the baby when breastfeeding
If the baby is fed mainly by mother's milk, then, provided that the nursing woman is adequately fed, the only vitamin that needs to be supplemented is vitamin D.
 5
5