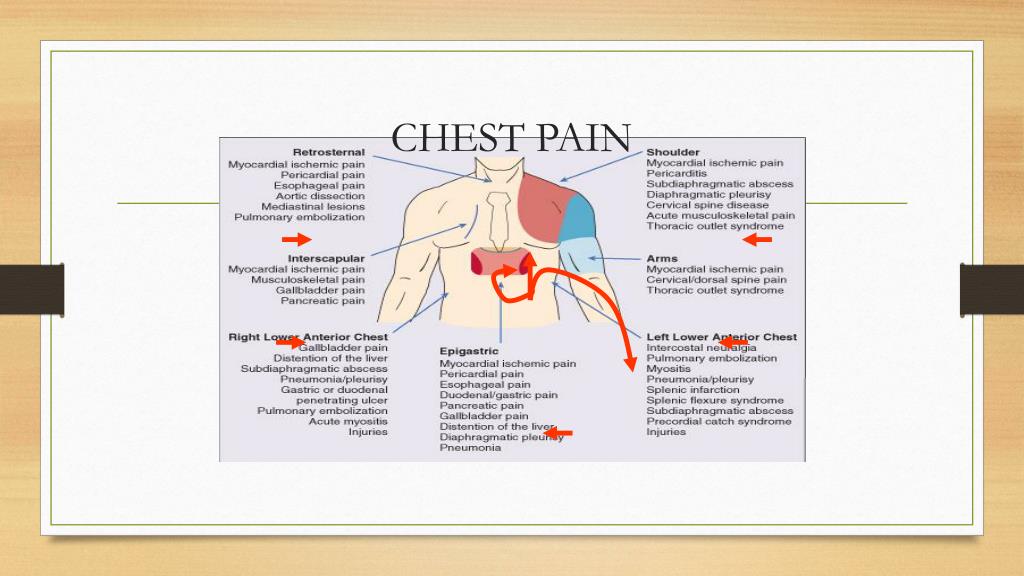
Constant pain in chest left side
15 Causes and When to Seek Emergency Help
We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Here’s our process.
If you have a pain in the left side of your chest, your first thought may be that you’re having a heart attack. While chest pain can indeed be a symptom of heart disease or heart attack, that’s not always the case.
Keep reading to learn more about the causes of pain in the left side of the chest, what the accompanying symptoms might be, and suggestions for actions you can take to address each.
Chest pain, or chest heaviness, in general is a concern for heart attack or other life-threatening condition for which every minute matters. Call 911 or your local emergency services if you or someone near you has unexplained left sided or generalized chest pain along with:
- feeling of pressure or tightening of the chest
- shooting pain, which is especially concerning down the left arm, left side of the neck, and left side of the jaw
- breathing difficulties
- weakness, lightheadedness, or dizziness
- nausea or vomiting
- chest heaviness
Several conditions can cause pain in the left side of your chest. They range from benign to potentially life threatening. If you’re ever in doubt about the potential cause of the pain in the left side of your chest, you should seek emergency medical services immediately.
Below are some common causes of left sided chest pain.
Angina isn’t a disease. Instead, it’s often a symptom of coronary heart disease, though other heart conditions may also cause it to occur. Angina is the chest pain, chest heaviness, discomfort, or pressure you get when your heart muscle isn’t getting enough oxygen from blood. The pain and discomfort typically include your left arm, left shoulder, left side of your neck, and left side of your jaw. You might also have discomfort in your back.
It’s crucial that the underlying condition is properly diagnosed and treated. Diagnostic testing may include:
- blood tests
- electrocardiogram (EKG)
- stress test
- echocardiogram
- angiogram/cardiac catheterization
Treatment will depend on the cause, and may include medication, lifestyle changes, and cardiac procedures as necessary.
A heart attack is when the heart muscle is damaged because it can’t get enough oxygen-rich blood. Some heart attacks start with mild chest pain that builds up slowly. They can also start quite abruptly, with intense pain on the left side or center of your chest. Other symptoms of heart attack can include:
- tightening, squeezing, or crushing pressure in your chest
- pain in your left arm, though it can also occur in your right arm
- shooting pain in your neck, jaw, back, or stomach
- shortness of breath
- heartburn, nausea, or vomiting
- lightheadedness, weakness, or dizziness
Heart attack symptoms in women
Symptoms of heart attack vary from person to person. Both men and women can experience chest pain or discomfort, gassiness or heartburn, shortness of breath, or pain and discomfort in the shoulders, arms, neck, or jaw. However, women are more likely to experience:
- unusual tiredness
- nausea
- lightheadedness
If you or someone near you experiences these symptoms, seek immediate medical attention. With a heart attack, every second counts. The longer the heart muscle is deprived of oxygen, the greater the chances that the damage will be permanent.
With a heart attack, every second counts. The longer the heart muscle is deprived of oxygen, the greater the chances that the damage will be permanent.
Emergency care can begin as soon as medical personnel arrive. After a hospital stay, you may need to continue medication. Lifestyle modifications can include:
- a heart-healthy diet
- some daily exercise
- maintaining a moderate weight
- not smoking
Myocarditis is a rare cause of cardiovascular disease that is caused by inflammation in the heart. Doctors often cannot identify a cause, but when they can, the cause is typically an viral infection.
Chest pain can be an indication that your heart muscle is inflamed. Other symptoms include:
- shortness of breath
- abnormal heart rhythm (arrhythmia)
- fatigue
Myocarditis can affect your heart’s electrical system, weakening your heart or causing permanent damage to the heart muscle. In some cases, a person can experience cardiac arrest or death.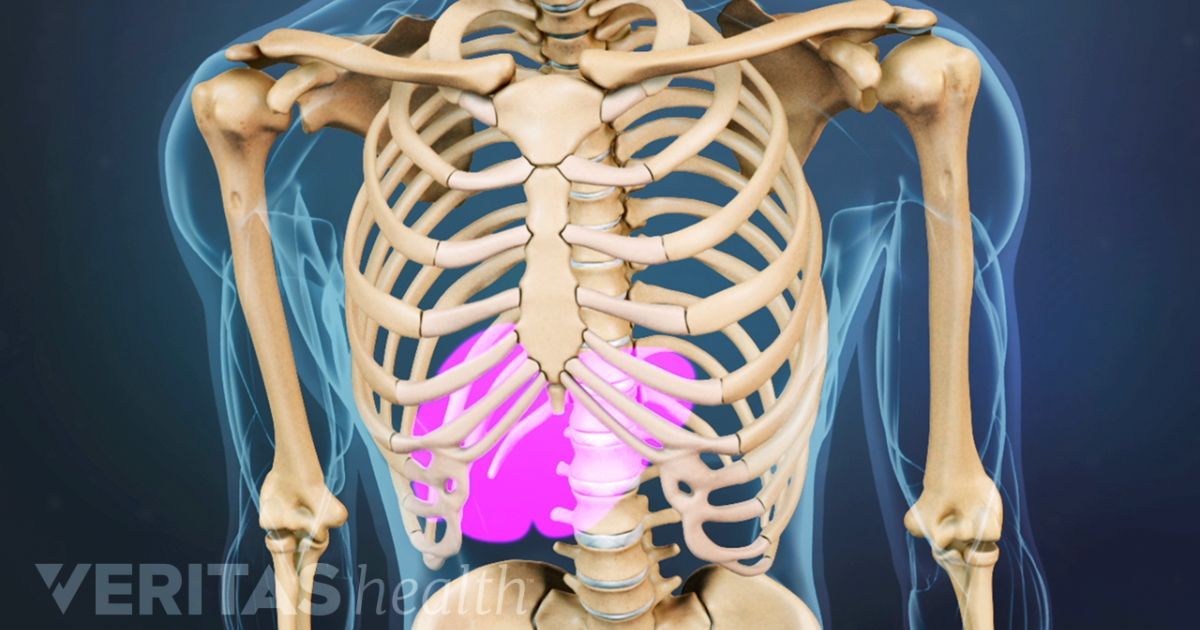
Mild cases sometimes improve without treatment, but severe cases may require medication. Treatment depends on the cause.
Cardiomyopathy is a disease of the heart muscle or enlarged heart. It’s possible to have cardiomyopathy without symptoms, but it can also cause chest pain. Other symptoms can include:
- shortness of breath
- dizziness or fainting
- heart palpitations
- fatigue
- swelling of your ankles, feet, legs, hands, or abdomen
Treatment involves medications, cardiac procedures, and surgery. Certain lifestyle changes may help, too. These can include:
- reducing salt intake
- maintaining a moderate weight
- avoiding alcohol
- engaging in light to moderate exercise on a regular basis
The pericardium is the two thin layers of tissue that surround your heart to help keep it in place. When this area becomes inflamed or irritated, it’s known as pericarditis.
Pericarditis can cause a sharp stabbing pain on the left side or middle of your chest. You might also have pain in one or both shoulders.
You might also have pain in one or both shoulders.
You may experience pericarditis due to infections, heart surgery, heart attack, injury, or medications.
It may be mild and even clear up on its own, but it can sometimes lead to heart abnormalities that can be fatal. Treatment depends on the underlying cause.
Panic attacks come on abruptly and tend to peak within 10 minutes. Due to chest pain, chest tightness, and other symptoms, a panic attack can simulate a heart attack. In addition to chest pain, some other symptoms are:
- shortness of breath
- rapid heartbeat
- shakiness or dizziness
- sweating, hot flashes, or chills
- nausea
- feelings of unreality or detachment
- feeling as though you might choke
- intense fear or sense of doom
If you think you’ve had a panic attack, see a doctor. Other health problems, such as heart and thyroid disorders, can produce similar symptoms, so you want to be certain of the diagnosis.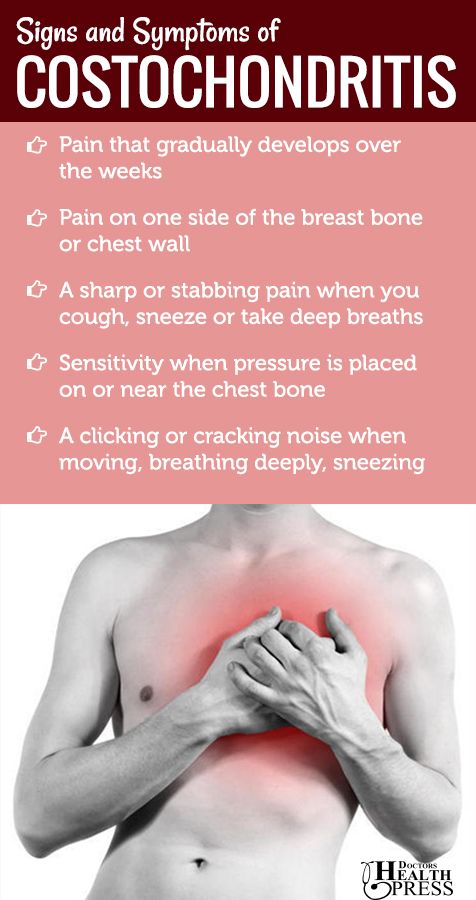
How to ease a panic attack
Panic disorder is a mental health problem that can be treated. Your doctor may recommend psychotherapy or cognitive behavioral therapy. If it’s an ongoing problem, there are some medications that might help.
In order to ease a panic attack, you might find it helpful to:
- practice stress management and relaxation techniques
- join a support group
- stay away from caffeine, tobacco, alcohol, and recreational drugs
- engage in regular physical activity
- make sure you get a full night’s sleep every night
Heartburn is the chest pain and discomfort you get when digestive acid flows up into your esophagus (acid reflux or gastroesophageal reflux). You might also have:
- a burning sensation in your upper abdomen and chest
- sour or metallic taste in your mouth
- stomach contents flowing up to the back of your throat
Heartburn generally happens fairly soon after you’ve eaten. It can also happen when you lie down within a few hours of eating. It can even wake you from a sound sleep.
It can also happen when you lie down within a few hours of eating. It can even wake you from a sound sleep.
Acid reflux can sometimes progress to a more severe form called gastroesophageal reflux disease (GERD). The main symptom of GERD is frequent heartburn. In addition to chest pain, GERD can also cause coughing, wheezing, and trouble swallowing.
Treating heartburn
You can usually ease heartburn with over-the-counter antacids. A doctor can prescribe a stronger medication if necessary. If you have frequent heartburn, it might help to:
- eat smaller meals
- avoid fried or fatty foods
- eat slowly
- avoid alcohol and tobacco
- maintain a moderate weight
- don’t eat food before bed
- avoid other foods that may be a trigger to you
A hiatal hernia is when the upper part of your stomach pushes through the large muscle between your abdomen and chest (diaphragm). Symptoms can include:
- chest pain
- abdominal pain
- heartburn
- regurgitation of food into your mouth
You can ease symptoms by:
- eating smaller meals
- avoiding foods that trigger heartburn
- not lying down after eating
- elevating the head of your bed
You may not need any treatment, but see a doctor if symptoms persist.
Chest pain can mean that there’s something wrong with your esophagus. For example:
- An esophageal muscle spasm can mimic the same type of chest pain as a heart attack.
- The lining of your esophagus can become inflamed (esophagitis), causing burning or sharp chest pain. Esophagitis can also cause pain after meals, swallowing problems, and blood in your vomit or stools.
- An esophageal rupture, or tear, lets food leak into your chest cavity, causing mild to severe chest pain. It can also lead to nausea, vomiting, and rapid breathing.
Treatment depends on cause. An esophageal rupture must be surgically repaired.
Chest pain can be the result of pulled, strained, or sprained muscles in your chest or between the ribs. Any injury to your chest can cause chest pain. This includes:
- bruising of your chest wall
- fractured breastbone (sternum)
- fractured ribs
This type of injury may also cause pain when you take a deep breath or cough.
If you believe you’ve broken a bone, see a doctor right away. It can take about 10 weeks to improve and even longer to fully recover. In the meantime, you’ll have to avoid strenuous activity.
Sudden and sharp pain on either side of your chest could be the result of a collapsed lung (pneumothorax). This can be due to disease or from trauma to your chest. Other symptoms can include:
- shortness of breath
- rapid breathing or heartbeat
- skin turning blue
- dry cough
- fatigue
Treatment will depend on the cause, but it’s important to seek medical help immediately.
Sharp or stabbing chest pain that worsens when you take a deep breath or cough could mean you have pneumonia, especially if you’ve recently had a respiratory illness such as bronchitis or influenza.
Other symptoms may include:
- cough, sometimes with mucus
- fever, chills, or shaking
- shortness of breath
- headache
- loss of appetite
- fatigue
See a doctor if you think you have pneumonia. In the meantime, get plenty of rest and drink a lot of fluids. Your doctor may prescribe antibiotics or antivirals. In severe cases, hospitalization may be necessary.
In the meantime, get plenty of rest and drink a lot of fluids. Your doctor may prescribe antibiotics or antivirals. In severe cases, hospitalization may be necessary.
Chest pain can sometimes be a symptom of lung cancer. Other and symptoms may include:
- intense coughing, coughing up mucus or blood
- pain in your shoulder or back, unrelated to pain from coughing
- shortness of breath
- recurring bouts of bronchitis or pneumonia
- loss of appetite or unexplained weight loss
Symptoms may not appear in early stage lung cancer. In general, the sooner you receive a diagnosis and treatment, the better the outcome.
Pulmonary hypertension is high blood pressure in your lungs. In addition to chest pain, it can cause:
- dizziness or fainting
- shortness of breath
- loss of energy
As the disease progresses, it can lead to irregular heartbeat and racing pulse. Untreated, it can lead to heart failure.
A sudden, sharp chest pain can be an indication of pulmonary embolism (PE). PE is a blood clot in your lungs. Other symptoms may include:
PE is a blood clot in your lungs. Other symptoms may include:
- back pain
- lightheadedness
- bluish tone to lips
- excessive sweating
- dizziness
- coughing
- shortness of breath
This is a medical emergency that calls for immediate treatment.
Several conditions share symptoms that include chest pain. If you have chest pain for no known reason, consult with a doctor so you can start working toward a diagnosis.
Sudden chest pain accompanied by symptoms such as trouble breathing, pressure on your chest, and dizziness could signal a life-threatening emergency. Get help immediately.
Symptoms, Causes, Treatment, and More
Your left ribs protect the organs that sit below them, like your heart and your stomach. Pain in this area can be caused by injury, infection, or an underlying condition.
If you have pain in your chest, you might worry about a serious condition, such as a heart attack. While it’s true that pain under your left ribs can be a heart attack symptom, discomfort in that area is not always related to your heart.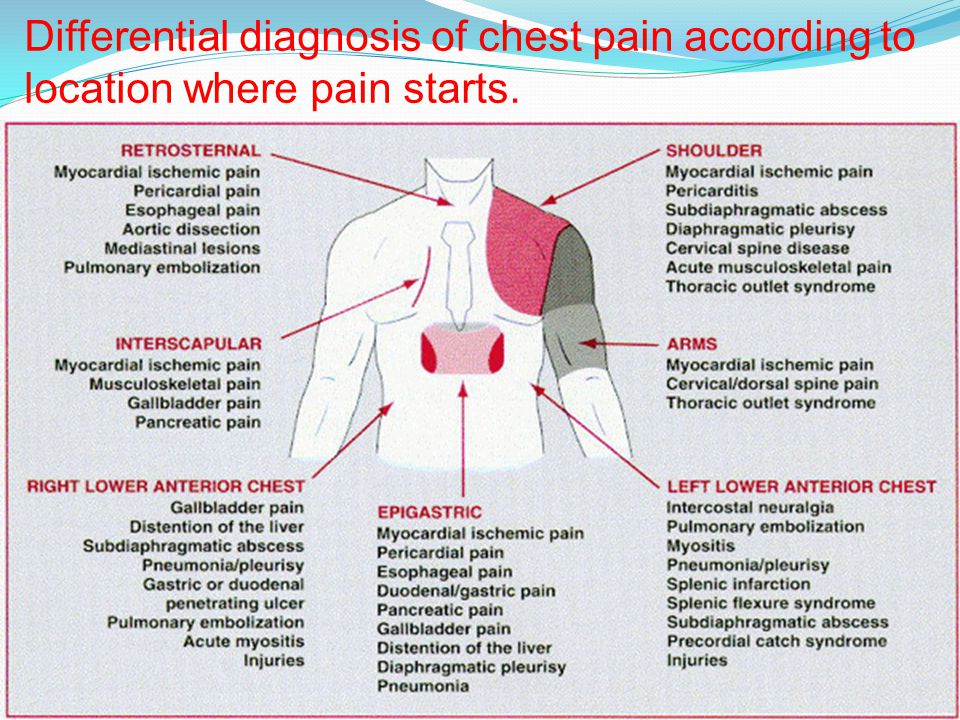
Depending on the cause, left rib pain might feel sharp and stabbing, or dull and aching. For many people, pain in this area is due to a benign (not harmful), treatable cause. But if you’re having chest pain, it’s best to see a doctor or healthcare professional to make sure it’s nothing serious.
Read on to learn about possible causes of left rib pain, diagnosis, and treatments.
Chest pain can sometimes signal a medical emergency, such as a heart attack. If you’re feeling pain in your left ribs, it’s best not to ignore it.
Heart attack symptoms include:
- pain, discomfort, or a heavy feeling in your chest, usually in the middle or on the left side
- pain or discomfort in your neck, jaw, shoulders, arms, back, or above your belly button
- shortness of breath
- sweating
- fatigue
- nausea and vomiting
- lightheadedness or dizziness
- fast or irregular heart rate
If you think you could be having a heart attack, call 911 or local emergency services right away.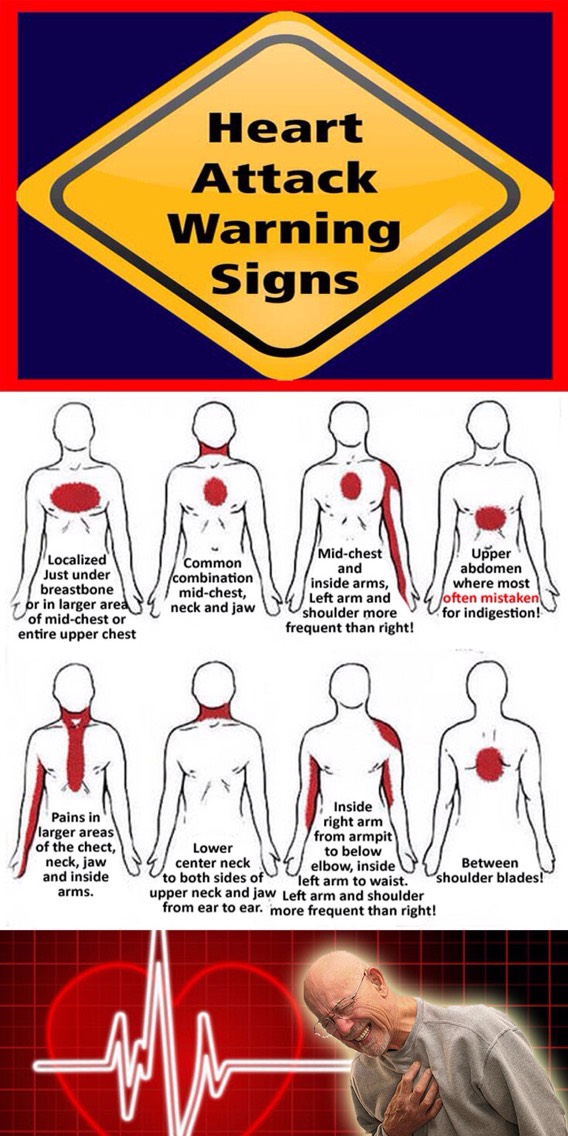
Your rib cage consists of 24 ribs — 12 on the left and 12 on the right side of your body. Their function is to protect your organs that lie beneath them.
On the left side, this includes your heart, left lung, pancreas, spleen, stomach, and left kidney. When any of these organs are infected, inflamed, or injured, pain can radiate under and around your left rib cage. It’s also possible to injure your ribs themselves.
Costochondritis refers to inflammation of the cartilage that attaches your ribs to your breastbone. This condition doesn’t always have a clear cause. It can happen for several reasons, such as:
- an infection
- an injury
- severe coughing
Costochondritis causes a sharp, stabbing pain that’s usually felt on the left side of your rib cage. It may get worse when you cough, sneeze, or press on your ribs.
A forceful blow or injury to your chest is the most common cause of bruised or broken ribs.
If you have a bruised rib, you’ll usually feel pain in your chest that’s worse when you inhale or move.
When a rib is broken, the pain is likely to be severe. It may make you feel like it’s hard to breathe in all the way. Broken ribs can sometimes cause serious complications, such as:
- a collapsed lung
- injuries to your blood vessels or organs, such as your spleen
- flail chest, which is a medical emergency that happens when you have many fractures in your ribs
Irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD) are two different digestive conditions. The causes of IBS and IBD aren’t fully known.
IBS and IBD both cause persistent, long-term pain in your abdomen, which is the area from your chest down to your hips. It’s possible for IBS or IBD to cause pain under your left ribs. These conditions also cause digestive symptoms, such as constipation, diarrhea, and gas.
Symptoms may come and go. IBS symptoms tend to improve after you have a bowel movement. IBD is a more serious condition that causes physical changes to your intestines. A doctor can see these changes using imaging tests.
A doctor can see these changes using imaging tests.
Your pancreas is a gland located near your small intestine, on the left side of your belly. It makes insulin, which your body uses to turn sugar into energy. It also releases digestive juices into your small intestine to help break down food you’ve eaten.
Pancreatitis refers to inflammation of your pancreas. It can have many causes, including:
- injury
- long-term heavy alcohol use
- gallstones
Pain caused by pancreatitis can happen suddenly (acute pancreatitis), or it can slowly get worse over time (chronic pancreatitis). Additional symptoms of pancreatitis include:
- fever
- fast heart rate
- nausea
- vomiting
- weight loss
- jaundice
It’s important to treat pancreatitis to prevent serious complications.
Your spleen also sits in the left side of your body, near your rib cage. This organ is an important part of your immune system. It produces white blood cells that fight infection, and it processes other parts of your blood.
An enlarged spleen, also called splenomegaly, can cause symptoms such as:
- pain or discomfort
- bloating
- feeling full after eating only a small amount of food
Several things can cause an enlarged spleen, including:
- viral infections, such as mononucleosis
- bacterial infections, such as syphilis
- parasitic infections, such as malaria
- blood diseases
- liver diseases
Sometimes, your spleen can rupture, usually as a result of trauma. It’s a medical emergency, and you should get medical attention immediately.
If your spleen ruptures, the area might feel tender when you touch it. In addition to pain, other signs and symptoms can include:
- low blood pressure
- dizziness
- blurry vision
- nausea
More rarely, a splenic infarct happens when a portion of your spleen necrotizes or “dies.” This happens when the blood supply is lowered or stopped, usually as a result of an injury or conditions that affect your blood.
Gastritis refers to inflammation of the lining of your stomach, which is also near the left side of your rib cage.
It doesn’t always cause symptoms, but possible symptoms include:
- pain in your upper abdomen
- feeling full after eating only a small amount of food
- nausea
- vomiting
The causes of gastritis include:
- Helicobacter pylori infection
- frequent use of nonsteroidal anti-inflammatory drugs (NSAIDs)
- long-term, heavy alcohol use
Your kidneys are part of your urinary tract. They’re located on either side of your spine, but when they become inflamed or infected, the pain can radiate to the front of your body. When your left kidney is involved, you might feel pain near the left side of your rib cage.
Kidney stones are hardened calcium and salt deposits that form into stones. They can cause a cramping pain as they move out of your kidneys and make their way toward your bladder. In addition to pain in your left rib cage, kidney stones can also cause:
- an urge to urinate, with little urine coming out
- bloody or cloudy urine
- pain in your side that radiates to the front of your body
Kidney infections occur when bacteria from your urinary tract make their way into your kidneys. This usually happens due to a bladder infection. Additional symptoms of a kidney infection can include fever and nausea.
This usually happens due to a bladder infection. Additional symptoms of a kidney infection can include fever and nausea.
If you’re having symptoms of a kidney problem, it’s important to see a doctor. You can get a diagnosis and start any treatment that may be needed.
Your heart is surrounded by a fluid-filled sac called the pericardium. Pericarditis refers to inflammation of this sac. This can cause a dull ache or a stabbing pain that’s usually worse when you’re lying down. Pericarditis can also cause a high fever.
Researchers aren’t sure why it happens, but it often occurs after you’ve had a viral infection.
Pericarditis can lead to complications if it is not treated.
Pleurisy happens when the tissue that surrounds your lungs becomes inflamed. Causes of pleurisy include:
- pneumonia
- blood clot in your lung
- injury
- cancer that has spread from another part of your body to the tissue surrounding your lungs
- cancers that specifically affect the tissue surrounding your lungs, such as mesothelioma
Pleurisy on your left side may cause pain under your left rib cage, but the main symptom is a sharp, stabbing pain when you breathe. Be sure to see a doctor if you experience any intense chest pain while breathing.
Be sure to see a doctor if you experience any intense chest pain while breathing.
To figure out what’s causing pain in your left rib cage, a doctor will give you a physical exam that includes feeling the affected area. This will help them check for any signs of swelling or inflammation that might be caused by conditions such as costochondritis.
If they suspect the pain could be due to a heart problem, a doctor might use an electrocardiogram to measure the electrical activity in your heart. This will help to rule out any serious underlying condition.
Next, they may take blood, stool, or urine samples for testing. Analyzing these results can alert a doctor to signs of kidney problems, pancreatitis, or gastritis.
If the cause of your rib cage pain still isn’t clear, you may need an imaging test, such as:
- ultrasound
- CT scan
- X-ray
- endoscopy
This will give a doctor a better view of your bones, organs, and tissues.
What kind of doctor should I see for left rib pain?
There are many possible causes of pain around your left rib cage. A primary care doctor can usually help you determine the cause. If needed, they can refer you to a specialist, such as an orthopedic doctor who treats bones, muscles, and joints.
A primary care doctor can usually help you determine the cause. If needed, they can refer you to a specialist, such as an orthopedic doctor who treats bones, muscles, and joints.
If you need help finding a primary care doctor, you can browse doctors in your area through the Healthline FindCare tool.
If you think you could be having a heart attack or other medical emergency, call 911 or your local emergency services right away.
Treating your left rib cage pain depends on what’s causing it. If it’s related to any type of inflammation, a doctor will likely recommend you take NSAIDs to lower your pain and swelling. In some cases, you may need an antibiotic to clear up a bacterial infection.
Bruised ribs will likely heal with rest, as will broken ribs, if there are no complications.
In rare cases, you may need surgery. For example, if a kidney stone is too large to pass through your body on its own, a doctor may need to surgically remove it.
Given the number of organs in the upper left part of your body, it’s not uncommon to feel pain under the left rib cage. It may be caused be an easily treatable condition.
It may be caused be an easily treatable condition.
But if you have pain in this area that’s severe, worsens over time, lasts more than 24 hours, or is associated with any of the serious symptoms above, you should get medical treatment immediately to rule out any underlying conditions.
Chest pain - causes, examination and treatment | Symptoms
Myocardial infarction or unstable angina
Signs: Represent an immediate danger to life. Sudden, pressing pain that spreads (radiates) to the jaw or arm, may be constant or transient. Sometimes shortness of breath or nausea. Pain that comes on with exertion and goes away with rest (angina pectoris). Abnormal heart sounds heard through a stethoscope. Frequent warning signs.
Thoracic aortic dissection (tear in the wall of the thoracic aorta)
Signs: Represent an immediate danger to life. Sudden, tearing pain that extends into or begins in the middle of the back. Sometimes dizziness, stroke, and pain, coldness, or numbness in the leg. Sometimes different pulse or blood pressure in the limbs. Usually in people over 55 with a history of high blood pressure. Warning signs.
Sometimes dizziness, stroke, and pain, coldness, or numbness in the leg. Sometimes different pulse or blood pressure in the limbs. Usually in people over 55 with a history of high blood pressure. Warning signs.
Pericarditis (inflammation of the lining around the heart)
Signs: Potentially life-threatening. Acute pain, constant or transient, aggravated by breathing, swallowing food, or lying on the back. Relaxes when leaning forward. Abnormal heart sounds heard through a stethoscope.
Spontaneous rupture of the esophagus
Signs: Represent an immediate danger to life. Sudden, sharp pain immediately after vomiting or after a medical procedure involving the esophagus (esophageal and gastric endoscopy or transesophageal echocardiography). Some warning signs.
Pancreatitis (inflammation of the pancreas)
Signs: Potentially life-threatening. Severe, persistent pain that: appears in the upper middle abdomen or lower chest. Often aggravated in the supine position, weakened by bending forward. Vomiting and soreness in the upper abdomen, sometimes shock. Often in people who abuse alcohol or have gallstones.
Often aggravated in the supine position, weakened by bending forward. Vomiting and soreness in the upper abdomen, sometimes shock. Often in people who abuse alcohol or have gallstones.
Peptic ulcers
Signs: Periodic vague discomfort that is felt in the upper middle of the abdomen or in the lower chest. Relief with antacids and sometimes after meals. Common in smokers and drinkers, or both. There are no warning signs.
Gastroesophageal reflux (GERD)
Signs: Periodic burning pain that spreads from the upper middle abdomen to the throat, worse when bending over or lying down. Relieves with antacids.
Diseases of the gallbladder and bile ducts (diseases of the biliary tract)
Signs: Intermittent discomfort, which is felt in the upper right side of the abdomen or in the lower middle of the chest, is observed after eating (but not after exercise).
Swallowing disorders (in which the peristalsis of food through the esophagus is impaired)
Signs: Pain that develops gradually over a long period of time may or may not appear during swallowing. Usually difficulty swallowing.
Usually difficulty swallowing.
Pulmonary embolism (blockage of the pulmonary artery by a blood clot)
Signs: Represent an immediate danger to life. Often severe pain when breathing, shortness of breath, rapid breathing and rapid heartbeat. Sometimes a slight fever, coughing up blood, or shock. More likely in patients with risk factors for pulmonary embolism (history of blood clots, recent surgery, especially leg surgery, prolonged bed rest, leg cast or splint, older age, smoking, or cancer).
Tension pneumothorax (collapse of the lung with increased air pressure in the chest)
Signs: Represent an immediate danger to life. Significant shortness of breath. Low blood pressure, swollen neck veins, and decreased breath sounds heard through a stethoscope on one side. It usually occurs only after a severe chest injury.
Pneumonia
Signs: Potentially life-threatening. Fever, chills, cough, and usually yellow or green sputum. Often shortness of breath. Sometimes pain when breathing. Palpitations and congestion in the lungs revealed during the examination.
Pneumothorax (collapse of the lung)
Signs: Potentially life-threatening. Sudden sharp pain, usually in one side of the chest. Sometimes shortness of breath, weakening of breath sounds heard through a stethoscope on one side.
Pleurisy (inflammation of the lining around the lung)
Signs: Sharp pain when breathing. Usually in patients who have recently had pneumonia or a viral respiratory infection. Sometimes cough. There are no warning signs.
Musculoskeletal chest wall pain
Signs: Pain that is usually persistent (lasting a few days or more). Increases with movement and/or breathing. May have no apparent cause or result from coughing or physical exertion. Soreness at one point on the chest. There are no warning signs.
Fibromyalgia
Signs: Pain that is almost constant, spreads to large areas of the body, is usually accompanied by fatigue and impaired sleep quality.
Shingles
Signs: Acute girdle pain in the middle of the chest, but only on one side. Rash in the form of numerous small vesicles, sometimes filled with pus, in the area of localization of pain, sometimes arising after the onset of pain.
Malignant tumors of the chest or chest wall
Signs: Sometimes pain that worsens with inspiration. Sometimes chronic cough, history of smoking, weight loss, swollen lymph nodes in the neck.
Cardiologist: chest pain is not always associated with heart disease
Chest pain often causes people to think that their heart hurts. But it can also be a sign of a completely different disease.
Cardiologist Dina Sulimanova told the viewers how to learn to distinguish exactly heart pain.
“We need to pay attention to the localization of pain,” advises Dina Rushanovna. - Heart pain occurs precisely behind the sternum or in the left half of the chest.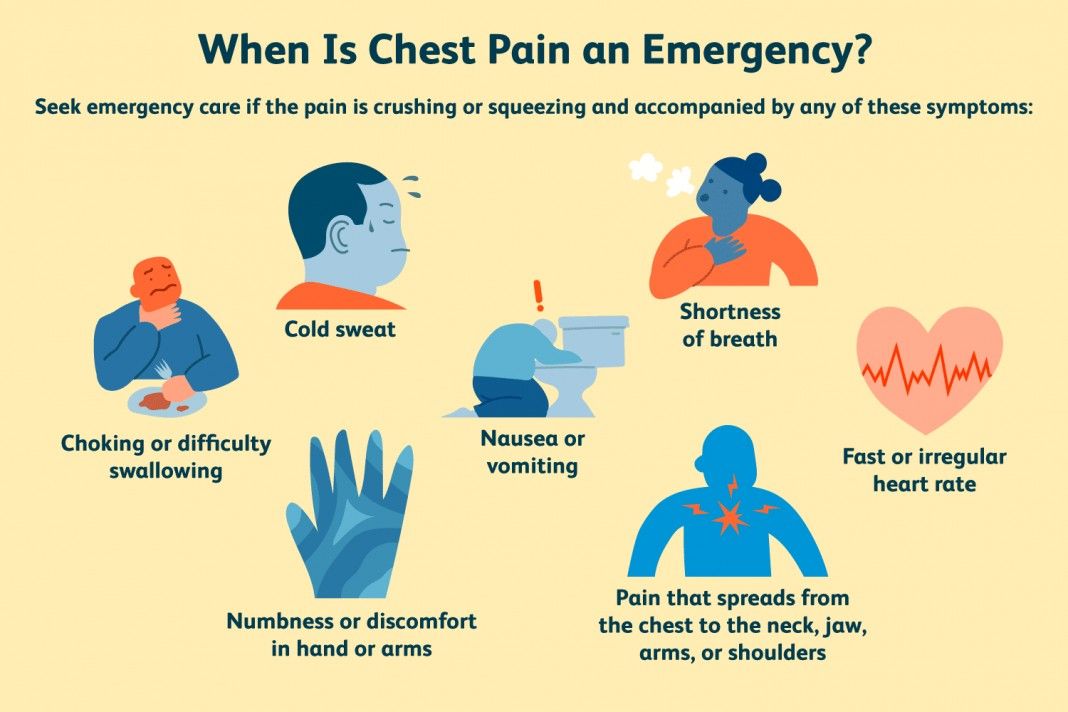 It appears with excessive physical exertion. For example, when a person climbs stairs faster, quickens their pace, or carries something heavy.
It appears with excessive physical exertion. For example, when a person climbs stairs faster, quickens their pace, or carries something heavy.
According to the description, heart pain is pressing, squeezing, burning. It can give to the lower jaw, left arm or under the left shoulder blade.
Such pain disappears if a person calms down, stops, catches his breath. Or if a patient who has already had a heart attack takes a nitroglycerin tablet.”
The cardiologist received a lot of questions from TV viewers and the presenter.
For example:
“It hurts in the left side of the chest, closer to the heart. When inhaling, the pain increases. Could it be heartache?
Doctor: “This pain is typical for osteochondrosis of the thoracic spine. It intensifies when inhaling, exhaling, changing the position of the body. You need to go to a neurologist for appointments and recommendations.”
“Do people often come to see you with what seems to be chest pain that turns out to be non-cardiac?”
“Yes, of course, because chest pain is a fairly significant symptom, and people most often visit a cardiologist to rule out a pathology of the cardiovascular system.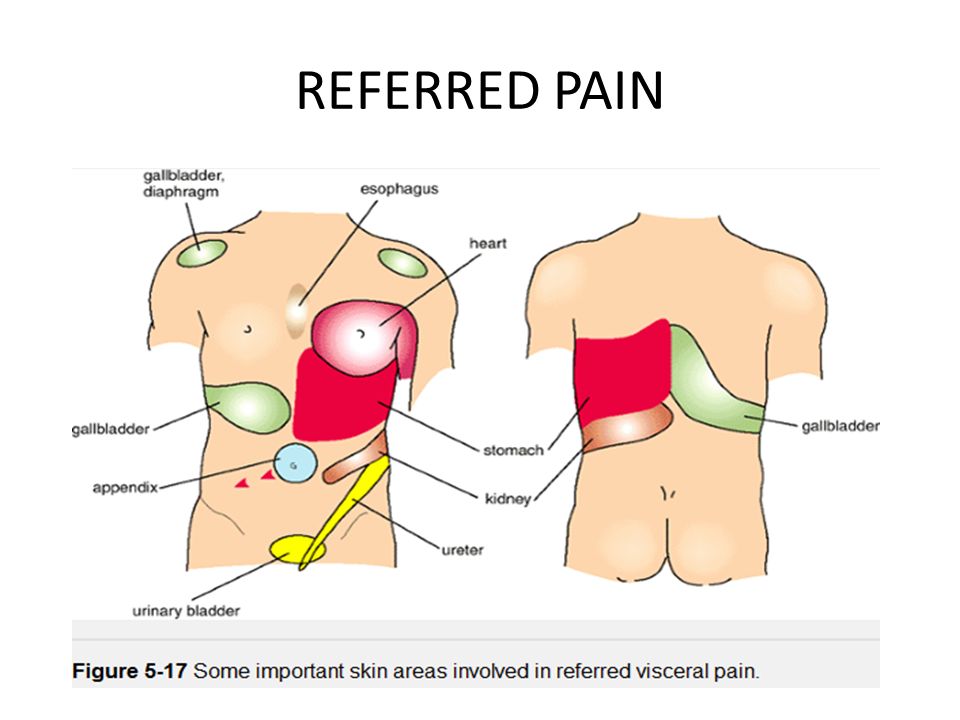 With a clear collection of anamnesis, complaints, we understand whether it is cardiological pain, or is it still osteochondrosis, diseases of the stomach or lungs. Further, we already recommend contacting a specialist who will help to cope with this pain. ”
With a clear collection of anamnesis, complaints, we understand whether it is cardiological pain, or is it still osteochondrosis, diseases of the stomach or lungs. Further, we already recommend contacting a specialist who will help to cope with this pain. ”
“I have anxiety and chest pain. Did an ultrasound of the heart. In conclusion, the doctor wrote "aortic sclerosis", but in words she said that everything was normal. Tell me, what is aortic sclerosis? Should I be worried about this?"
“Don't worry. Aortic sclerosis indicates thickening of the walls of the aorta. It occurs most often with a prolonged increase in pressure during hypertension. It is recommended to do an ultrasound of the heart once a year. You need to see a therapist in your area."
“Lifted the gas stove with a friend. It was light, carried away at a time. An hour later, when I got home, I felt pain in my chest. I have a heart defect, could it somehow affect? Or just pulled a muscle? The pain is acute: when tilting, turning, or moving the arm…”
“This pain is also associated with osteochondrosis. If the pain is associated with movement, it is not heart pain. When it is the heart that hurts in a person, he can lie down, sit, but the pain will not change the intensity, it will also be squeezing, squeezing, burning. Muscular or osteochondrosis pain will be with body movements, turns. If this worries you, you need to contact a therapist and a neurologist, take an x-ray of the thoracic spine.
If the pain is associated with movement, it is not heart pain. When it is the heart that hurts in a person, he can lie down, sit, but the pain will not change the intensity, it will also be squeezing, squeezing, burning. Muscular or osteochondrosis pain will be with body movements, turns. If this worries you, you need to contact a therapist and a neurologist, take an x-ray of the thoracic spine.
“Recently, while climbing the stairs at the entrance, I had pain and heaviness in the chest area on the left. The left hand was numb and burning. Came home, took nitroglycerin and lay down. Did I do the right thing?"
“You did the right thing, but in addition to taking glycerin, you should have called an ambulance. Your pain is very similar to cardiac pain. The paramedics would take a cardiogram. If the blood flow is disturbed, changes appear on the ECG that indicate a pre-infarction state and then you would be hospitalized. You need to see a cardiologist."
“Recently, I have been experiencing a sharp, squeezing pain in the center of my chest.