What to do for ocd
Obsessive-compulsive disorder (OCD) - Diagnosis and treatment
Diagnosis
Steps to help diagnose obsessive-compulsive disorder may include:
- Psychological evaluation. This includes discussing your thoughts, feelings, symptoms and behavior patterns to determine if you have obsessions or compulsive behaviors that interfere with your quality of life. With your permission, this may include talking to your family or friends.
- Diagnostic criteria for OCD. Your doctor may use criteria in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), published by the American Psychiatric Association.
- Physical exam. This may be done to help rule out other problems that could be causing your symptoms and to check for any related complications.
Diagnostic challenges
It's sometimes difficult to diagnose OCD because symptoms can be similar to those of obsessive-compulsive personality disorder, anxiety disorders, depression, schizophrenia or other mental health disorders. And it's possible to have both OCD and another mental health disorder. Work with your doctor so that you can get the appropriate diagnosis and treatment.
Care at Mayo Clinic
Our caring team of Mayo Clinic experts can help you with your Obsessive-compulsive disorder (OCD)-related health concerns Start Here
Treatment
Obsessive-compulsive disorder treatment may not result in a cure, but it can help bring symptoms under control so that they don't rule your daily life. Depending on the severity of OCD, some people may need long-term, ongoing or more intensive treatment.
The two main treatments for OCD are psychotherapy and medications. Often, treatment is most effective with a combination of these.
Psychotherapy
Cognitive behavioral therapy (CBT), a type of psychotherapy, is effective for many people with OCD. Exposure and response prevention (ERP), a component of CBT therapy, involves gradually exposing you to a feared object or obsession, such as dirt, and having you learn ways to resist the urge to do your compulsive rituals. ERP takes effort and practice, but you may enjoy a better quality of life once you learn to manage your obsessions and compulsions.
Exposure and response prevention (ERP), a component of CBT therapy, involves gradually exposing you to a feared object or obsession, such as dirt, and having you learn ways to resist the urge to do your compulsive rituals. ERP takes effort and practice, but you may enjoy a better quality of life once you learn to manage your obsessions and compulsions.
Medications
Certain psychiatric medications can help control the obsessions and compulsions of OCD. Most commonly, antidepressants are tried first.
Antidepressants approved by the U.S. Food and Drug Administration (FDA) to treat OCD include:
- Clomipramine (Anafranil) for adults and children 10 years and older
- Fluoxetine (Prozac) for adults and children 7 years and older
- Fluvoxamine for adults and children 8 years and older
- Paroxetine (Paxil, Pexeva) for adults only
- Sertraline (Zoloft) for adults and children 6 years and older
However, your doctor may prescribe other antidepressants and psychiatric medications.
Medications: What to consider
Here are some issues to discuss with your doctor about medications for OCD:
- Choosing a medication. In general, the goal is to effectively control symptoms at the lowest possible dosage. It's not unusual to try several drugs before finding one that works well. Your doctor might recommend more than one medication to effectively manage your symptoms. It can take weeks to months after starting a medication to notice an improvement in symptoms.
- Side effects. All psychiatric medications have potential side effects. Talk to your doctor about possible side effects and about any health monitoring needed while taking psychiatric drugs. And let your doctor know if you experience troubling side effects.
- Suicide risk. Most antidepressants are generally safe, but the FDA requires that all antidepressants carry black box warnings, the strictest warnings for prescriptions.
 In some cases, children, teenagers and young adults under 25 may have an increase in suicidal thoughts or behavior when taking antidepressants, especially in the first few weeks after starting or when the dose is changed. If suicidal thoughts occur, immediately contact your doctor or get emergency help. Keep in mind that antidepressants are more likely to reduce suicide risk in the long run by improving mood.
In some cases, children, teenagers and young adults under 25 may have an increase in suicidal thoughts or behavior when taking antidepressants, especially in the first few weeks after starting or when the dose is changed. If suicidal thoughts occur, immediately contact your doctor or get emergency help. Keep in mind that antidepressants are more likely to reduce suicide risk in the long run by improving mood. - Interactions with other substances. When taking an antidepressant, tell your doctor about any other prescription or over-the-counter medications, herbs or other supplements you take. Some antidepressants can make some other medications less effective and cause dangerous reactions when combined with certain medications or herbal supplements.
- Stopping antidepressants. Antidepressants aren't considered addictive, but sometimes physical dependence (which is different from addiction) can occur. So stopping treatment abruptly or missing several doses can cause withdrawal-like symptoms, sometimes called discontinuation syndrome.
 Don't stop taking your medication without talking to your doctor, even if you're feeling better — you may have a relapse of OCD symptoms. Work with your doctor to gradually and safely decrease your dose.
Don't stop taking your medication without talking to your doctor, even if you're feeling better — you may have a relapse of OCD symptoms. Work with your doctor to gradually and safely decrease your dose.
Talk to your doctor about the risks and benefits of using specific medications.
Other treatment
Sometimes, psychotherapy and medications aren't effective enough to control OCD symptoms. In treatment-resistant cases, other options may be offered:
- Intensive outpatient and residential treatment programs. Comprehensive treatment programs that emphasize ERP therapy principles may be helpful for people with OCD who struggle with being able to function because of the severity of their symptoms. These programs typically last several weeks.
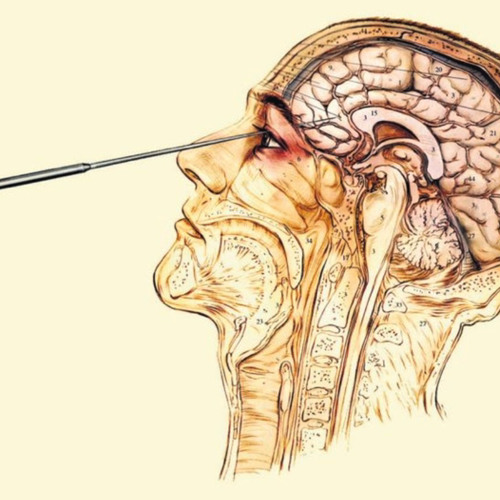
- Deep brain stimulation (DBS).
 DBS is approved by the FDA to treat OCD in adults age 18 years and older who don't respond to traditional treatment approaches. DBS involves implanting electrodes within certain areas of your brain. These electrodes produce electrical impulses that may help regulate abnormal impulses.
DBS is approved by the FDA to treat OCD in adults age 18 years and older who don't respond to traditional treatment approaches. DBS involves implanting electrodes within certain areas of your brain. These electrodes produce electrical impulses that may help regulate abnormal impulses. - Transcranial magnetic stimulation (TMS). The FDA approved a specific device (BrainsWay Deep Transcranial Magnetic Stimulation) to treat OCD in adults ages 22 to 68 years, when traditional treatment approaches have not been effective. TMS is a noninvasive procedure that uses magnetic fields to stimulate nerve cells in the brain to improve symptoms of OCD.
 During a TMS session, an electromagnetic coil is placed against your scalp near your forehead. The electromagnet delivers a magnetic pulse that stimulates nerve cells in your brain.
During a TMS session, an electromagnetic coil is placed against your scalp near your forehead. The electromagnet delivers a magnetic pulse that stimulates nerve cells in your brain.
Talk with your doctor to make sure you understand all the pros and cons and possible health risks of DBS and TMS if you're considering one of these procedures.
More Information
- Obsessive-compulsive disorder (OCD) care at Mayo Clinic
- Cognitive behavioral therapy
- Deep brain stimulation
- Electroconvulsive therapy (ECT)
- Psychotherapy
- Transcranial magnetic stimulation
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Lifestyle and home remedies
Obsessive-compulsive disorder is a chronic condition, which means it may always be part of your life. While OCD warrants treatment by a professional, you can do some things for yourself to build on your treatment plan:
While OCD warrants treatment by a professional, you can do some things for yourself to build on your treatment plan:
- Practice what you learn. Work with your mental health professional to identify techniques and skills that help manage symptoms, and practice these regularly.
- Take your medications as directed. Even if you're feeling well, resist any temptation to skip your medications. If you stop, OCD symptoms are likely to return.
- Pay attention to warning signs. You and your doctor may have identified issues that can trigger your OCD symptoms. Make a plan so that you know what to do if symptoms return. Contact your doctor or therapist if you notice any changes in symptoms or how you feel.
- Check first before taking other medications.
 Contact the doctor who's treating you for OCD before you take medications prescribed by another doctor or before taking any over-the-counter medications, vitamins, herbal remedies or other supplements to avoid possible interactions.
Contact the doctor who's treating you for OCD before you take medications prescribed by another doctor or before taking any over-the-counter medications, vitamins, herbal remedies or other supplements to avoid possible interactions.
Coping and support
Coping with obsessive-compulsive disorder can be challenging. Medications can have unwanted side effects, and you may feel embarrassed or angry about having a condition that requires long-term treatment. Here are some ways to help cope with OCD:
- Learn about OCD. Learning about your condition can empower you and motivate you to stick to your treatment plan.
- Stay focused on your goals. Keep your recovery goals in mind and remember that recovery from OCD is an ongoing process.

- Join a support group. Reaching out to others facing similar challenges can provide you with support and help you cope with challenges.
- Find healthy outlets. Explore healthy ways to channel your energy, such as hobbies and recreational activities. Exercise regularly, eat a healthy diet and get adequate sleep.
- Learn relaxation and stress management. In addition to professional treatment, stress management techniques such as meditation, visualization, muscle relaxation, massage, deep breathing, yoga or tai chi may help ease stress and anxiety.
- Stick with your regular activities. Try not to avoid meaningful activities. Go to work or school as you usually would. Spend time with family and friends. Don't let OCD get in the way of your life.
Preparing for your appointment
You may start by seeing your primary doctor. Because obsessive-compulsive disorder often requires specialized care, you may be referred to a mental health professional, such as a psychiatrist or psychologist, for evaluation and treatment.
Because obsessive-compulsive disorder often requires specialized care, you may be referred to a mental health professional, such as a psychiatrist or psychologist, for evaluation and treatment.
What you can do
To prepare for your appointment, think about your needs and goals for treatment. Make a list of:
- Any symptoms you've noticed, including the types of obsessions and compulsions youꞌve experienced and things that you may be avoiding because of your distress
- Key personal information, including any major stresses, recent life changes and family members with similar symptoms
- All medications, vitamins, herbal remedies or other supplements, as well as the dosages
- Questions to ask your doctor or therapist
Questions to ask might include:
- Do you think I have OCD?
- How do you treat OCD?
- How can treatment help me?
- Are there medications that might help?
- Will exposure and response prevention therapy help?
- How long will treatment take?
- What can I do to help myself?
- Are there any brochures or other printed material that I can have?
- Can you recommend any websites?
Don't hesitate to ask any other questions during your appointment.
What to expect from your doctor
Your doctor is likely to ask you a number of questions, such as:
- Do certain thoughts go through your mind over and over despite your attempts to ignore them?
- Do you have to have things arranged in a certain way?
- Do you have to wash your hands, count things or check things over and over?
- When did your symptoms start?
- Have symptoms been continuous or occasional?
- What, if anything, seems to improve the symptoms?
- What, if anything, appears to worsen the symptoms?
- How do the symptoms affect your daily life? Do you avoid anything because of your symptoms?
- In a typical day, how much time do you spend on obsessive thoughts and compulsive behavior?
- Have any of your relatives had a mental health disorder?
- Have you experienced any trauma or major stress?
Your doctor or mental health professional will ask additional questions based on your responses, symptoms and needs. Preparing and anticipating questions will help you make the most of your appointment time.
Preparing and anticipating questions will help you make the most of your appointment time.
By Mayo Clinic Staff
Related
Associated Procedures
Obsessive-compulsive disorder (OCD) - Symptoms and causes
Overview
Obsessive-compulsive disorder (OCD) features a pattern of unwanted thoughts and fears (obsessions) that lead you to do repetitive behaviors (compulsions). These obsessions and compulsions interfere with daily activities and cause significant distress.
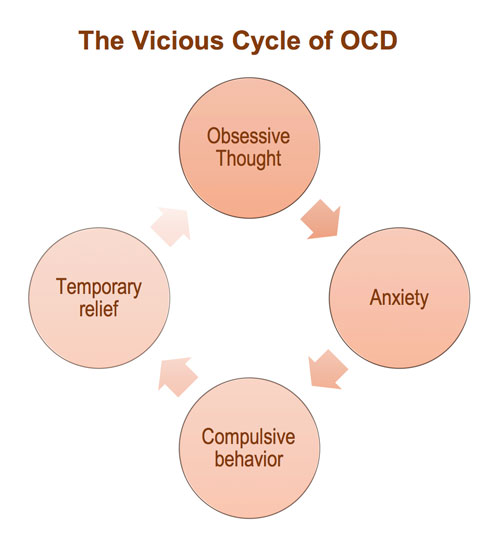
You may try to ignore or stop your obsessions, but that only increases your distress and anxiety. Ultimately, you feel driven to perform compulsive acts to try to ease your stress. Despite efforts to ignore or get rid of bothersome thoughts or urges, they keep coming back. This leads to more ritualistic behavior — the vicious cycle of OCD.
OCD often centers around certain themes — for example, an excessive fear of getting contaminated by germs. To ease your contamination fears, you may compulsively wash your hands until they're sore and chapped.
To ease your contamination fears, you may compulsively wash your hands until they're sore and chapped.
If you have OCD, you may be ashamed and embarrassed about the condition, but treatment can be effective.
Symptoms
Obsessive-compulsive disorder usually includes both obsessions and compulsions. But it's also possible to have only obsession symptoms or only compulsion symptoms. You may or may not realize that your obsessions and compulsions are excessive or unreasonable, but they take up a great deal of time and interfere with your daily routine and social, school or work functioning.
Obsession symptoms
OCD obsessions are repeated, persistent and unwanted thoughts, urges or images that are intrusive and cause distress or anxiety. You might try to ignore them or get rid of them by performing a compulsive behavior or ritual. These obsessions typically intrude when you're trying to think of or do other things.
Obsessions often have themes to them, such as:
- Fear of contamination or dirt
- Doubting and having difficulty tolerating uncertainty
- Needing things orderly and symmetrical
- Aggressive or horrific thoughts about losing control and harming yourself or others
- Unwanted thoughts, including aggression, or sexual or religious subjects
Examples of obsession signs and symptoms include:
- Fear of being contaminated by touching objects others have touched
- Doubts that you've locked the door or turned off the stove
- Intense stress when objects aren't orderly or facing a certain way
- Images of driving your car into a crowd of people
- Thoughts about shouting obscenities or acting inappropriately in public
- Unpleasant sexual images
- Avoidance of situations that can trigger obsessions, such as shaking hands
Compulsion symptoms
OCD compulsions are repetitive behaviors that you feel driven to perform. These repetitive behaviors or mental acts are meant to reduce anxiety related to your obsessions or prevent something bad from happening. However, engaging in the compulsions brings no pleasure and may offer only a temporary relief from anxiety.
These repetitive behaviors or mental acts are meant to reduce anxiety related to your obsessions or prevent something bad from happening. However, engaging in the compulsions brings no pleasure and may offer only a temporary relief from anxiety.
You may make up rules or rituals to follow that help control your anxiety when you're having obsessive thoughts. These compulsions are excessive and often are not realistically related to the problem they're intended to fix.
As with obsessions, compulsions typically have themes, such as:
- Washing and cleaning
- Checking
- Counting
- Orderliness
- Following a strict routine
- Demanding reassurance
Examples of compulsion signs and symptoms include:
- Hand-washing until your skin becomes raw
- Checking doors repeatedly to make sure they're locked
- Checking the stove repeatedly to make sure it's off
- Counting in certain patterns
- Silently repeating a prayer, word or phrase
- Arranging your canned goods to face the same way
Severity varies
OCD usually begins in the teen or young adult years, but it can start in childhood. Symptoms usually begin gradually and tend to vary in severity throughout life. The types of obsessions and compulsions you experience can also change over time. Symptoms generally worsen when you experience greater stress. OCD, usually considered a lifelong disorder, can have mild to moderate symptoms or be so severe and time-consuming that it becomes disabling.
Symptoms usually begin gradually and tend to vary in severity throughout life. The types of obsessions and compulsions you experience can also change over time. Symptoms generally worsen when you experience greater stress. OCD, usually considered a lifelong disorder, can have mild to moderate symptoms or be so severe and time-consuming that it becomes disabling.
When to see a doctor
There's a difference between being a perfectionist — someone who requires flawless results or performance, for example — and having OCD. OCD thoughts aren't simply excessive worries about real problems in your life or liking to have things clean or arranged in a specific way.
If your obsessions and compulsions are affecting your quality of life, see your doctor or mental health professional.
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Causes
The cause of obsessive-compulsive disorder isn't fully understood. Main theories include:
- Biology.
 OCD may be a result of changes in your body's own natural chemistry or brain functions.
OCD may be a result of changes in your body's own natural chemistry or brain functions. - Genetics. OCD may have a genetic component, but specific genes have yet to be identified.
- Learning. Obsessive fears and compulsive behaviors can be learned from watching family members or gradually learned over time.
Risk factors
Factors that may increase the risk of developing or triggering obsessive-compulsive disorder include:
- Family history. Having parents or other family members with the disorder can increase your risk of developing OCD.
- Stressful life events. If you've experienced traumatic or stressful events, your risk may increase. This reaction may, for some reason, trigger the intrusive thoughts, rituals and emotional distress characteristic of OCD.
- Other mental health disorders. OCD may be related to other mental health disorders, such as anxiety disorders, depression, substance abuse or tic disorders.
Complications
Problems resulting from obsessive-compulsive disorder may include, among others:
- Excessive time spent engaging in ritualistic behaviors
- Health issues, such as contact dermatitis from frequent hand-washing
- Difficulty attending work, school or social activities
- Troubled relationships
- Overall poor quality of life
- Suicidal thoughts and behavior
Prevention
There's no sure way to prevent obsessive-compulsive disorder. However, getting treatment as soon as possible may help prevent OCD from worsening and disrupting activities and your daily routine.
By Mayo Clinic Staff
Related
Associated Procedures
symptoms, how to get rid of and treat
Olya Selivanova
struggles with obsessive-compulsive disorder
Author profile
Since childhood, I have suffered from obsessive thoughts.
When I was nine years old, I was reading a book, when suddenly the thought occurred to me: “If you don’t finish reading today, your mother will die.” The thought frightened me, I put down the book and cried, but I had to return to reading so that my mother would not die.
From that moment on, the frightening thoughts were different. I could suddenly change the route, because the thought came to my mind: “It is not safe to go further. Get around." There were thoughts to harm loved ones: push, hit, pour over. At such moments, I thought that an evil force had entered into me, and I began to count to myself, imagined how the numbers increased in order in size and knocked bad thoughts out of my head.
By the time I was twelve, it all came to naught, and as a teenager, I decided that it was just childish oddities. But seven years later, the obsessive thoughts returned, and the doctor at the neuropsychiatric dispensary diagnosed me with Obsessive-Compulsive Disorder. I'll tell you how I was treated and how I live now.
Go see a doctor
Our articles are written with love for evidence-based medicine. We refer to authoritative sources and go to doctors with a good reputation for comments. But remember: the responsibility for your health lies with you and your doctor. We don't write prescriptions, we make recommendations. Relying on our point of view or not is up to you.
What is obsessive-compulsive disorder
Obsessive-compulsive disorder is a mental illness in which a person has obsessive thoughts and compulsive actions.
What is Obsessive-Compulsive Disorder - Mayo Clinic
Obsessive thoughts - obsessions - usually revolve around certain topics: fear of harming yourself and others, fear of germs and toxic substances, the need to organize everything. They appear suddenly or are provoked by external circumstances, such as a sharp object or the word "last".
Intrusive thoughts cannot be ignored, they cause anxiety or disgust. In response to them, a person has compulsions - a strong desire to perform certain actions that, according to his feelings, will get rid of such thoughts. Compulsions are difficult to resist: the anxiety will grow until the person gives up.
Compulsions are difficult to resist: the anxiety will grow until the person gives up.
For example, the obsessive thought that a person will become infected after touching a doorknob will provoke compulsive actions - repeated washing of hands, sometimes for several hours in a row.
/shizofreniya/
How much does it cost to support a relative with a mental disorder
I try not to touch doorknobs in public places and always make sure the door is closed. Do I have OCD?
Sergey Divisenko
psychotherapist
If a person's condition does not interfere with himself or others, then everything is in order, if it interferes, a disorder can be suspected. In the case of checking the door, one can say that checking if the door is closed once is not a problem, rechecking the door several times in a row and doing it systematically is already a problem.
To understand whether or not there is OCD, the doctor pays attention to how often the patient has obsessive thoughts and compulsive actions and how they affect his life. If symptoms occur more frequently in two weeks than in seven days and interfere with daily activities, it is probably OCD.
If symptoms occur more frequently in two weeks than in seven days and interfere with daily activities, it is probably OCD.
In this case, the symptoms should have the following characteristics:
- The person should evaluate them as his own thoughts and desires.
- There must be at least one thought or action that the person unsuccessfully resists.
- The thought of a person performing a compulsive action should not in itself be pleasurable. The fact that an action will help reduce anxiety is not considered pleasant in this sense.
- Thoughts or actions must be repeated.
How obsessive-compulsive disorder is treated
OCD is considered a lifelong disorder, but with treatment it is possible to achieve remission: to get rid of obsessive thoughts and compulsive actions for a long time or to reduce their number.
Medical treatment. The main drugs for the treatment of OCD are antidepressants of the SSRI group. They increase serotonin levels in the brain, making OCD symptoms less likely to occur.
They increase serotonin levels in the brain, making OCD symptoms less likely to occur.
Treatment options for OCD - NHS
Depending on the course of the disease and symptoms, along with antidepressants, the doctor may prescribe other drugs: tranquilizers, neuroleptics or mood stabilizers.
Cognitive behavioral therapy. This is a type of psychotherapy during which a person learns to control their emotional response to intrusive thoughts. As a result of therapy, obsessive thoughts cease to cause anxiety and compulsive actions.
Cognitive behavioral therapy - NHS
Order of the Ministry of Health of the Russian Federation of September 16, 2003 No. 438 "On psychotherapeutic care"
Psychiatrists, psychotherapists and psychologists are involved in the treatment of OCD in Russia. Psychiatrists prescribe prescription drugs. Psychotherapists and psychologists conduct psychotherapy sessions.
How I was diagnosed
At the age of 19, the development of the disease took a new turn. I was washing the kitchen knife and I had an obsessive thought that I was losing control and could cut myself and the guy who was nearby at that moment. So I began to avoid sharp objects, there was an irresistible desire to hide or throw them away.
I was washing the kitchen knife and I had an obsessive thought that I was losing control and could cut myself and the guy who was nearby at that moment. So I began to avoid sharp objects, there was an irresistible desire to hide or throw them away.
Obsessive thoughts revolved around the topic of death: drinking nail polish remover, bleach, vinegar, throwing yourself under a vehicle or jumping out of a window. Because of this, I removed all dangerous liquids from the house and stayed away from open windows, highways and train station platforms. I didn’t sleep well at night, suffered from anxiety, considered myself crazy and dangerous, and began to move away from everyone.
I also doubted everything. Even if I just performed an action, it seemed to me that it was not completed. I opened the door to make sure that it had been closed before, closed it again, pulled the handle, asked those around me if the door was exactly closed. I could wake up at night and see if the stove was turned on, although before going to bed I went up to it and stared without blinking - so that it would crash into my memory that it was definitely turned off. My young man, seeing all this, insisted that we try to see a psychologist.
My young man, seeing all this, insisted that we try to see a psychologist.
In Irkutsk, where I live, psychiatric care can be obtained free of charge at the regional psycho-neurological dispensary. I turned to the psychotherapeutic department of the dispensary for a consultation with a psychologist. At the reception, they brought me a card and said that there was no appointment with a psychologist for the next few days, but I could get to a psychiatrist: there are fewer people who want to see him.
/spravka/
How to get a certificate from the PND
At the appointment with the psychiatrist, I told about what was happening to me. The doctor was not surprised and said that it was an obsessive-compulsive disorder. It was the first time I heard my diagnosis, but I didn't believe it. On the Internet, I came across information that OCD is only pedantry, handwashing, fear of germs and perfectionism, and not the creepy things that come to my mind. The psychiatrist said that OCD was treated with antidepressants and offered to write a prescription, but I refused treatment because I thought they were serious drugs that would do more harm than help.
The psychiatrist said that OCD was treated with antidepressants and offered to write a prescription, but I refused treatment because I thought they were serious drugs that would do more harm than help.
How a visit to a neuropsychiatric dispensary with OCD will affect later life
Sergey Divisenko
psychotherapist
The patient could move freely, drive a car, use weapons and work.
With an OCD diagnosis, you can still work in any job, there are no legal barriers to this. With regard to cars and weapons, the situation has changed. In 2014 and 2015, government decrees appeared, according to which OCD became a contraindication for driving and owning weapons.
However, from a psychiatrist's point of view, a person diagnosed with OCD can drive a car and use a weapon. Doctors of the psycho-neurological dispensary still give a certificate about this, but they do it through a medical commission.
Treatment
First hospitalization My condition worsened, I tried to ignore obsessive thoughts. But the more I resisted them, the stronger they became. In addition, anger, irritability and constant fatigue appeared.
But the more I resisted them, the stronger they became. In addition, anger, irritability and constant fatigue appeared.
With new symptoms, I decided to see an endocrinologist, because I heard that this happens with problems with the thyroid gland. According to the results of ultrasound and hormone tests, the thyroid gland was in order. Then I made an appointment with a neurologist, but he also said that this was not his profile. Both doctors suggested that my constant fatigue, anger and irritability were symptoms of depression and advised me to seek psychiatric help.
Symptoms of clinical depression - NHS
I researched information about depression and realized that antidepressants could help, all I had to do was get a prescription. I came to the psychotherapeutic department again, but there was already another psychiatrist there. Since my condition worsened, instead of a prescription, he wrote out a referral for hospitalization in a day hospital. I had prejudices about a psychiatric hospital, so I did not want to visit the hospital. But there was no strength to argue with the psychiatrist.
But there was no strength to argue with the psychiatrist.
The next day I was already in the hospital. During the registration, the psychiatrist on duty asked what I was complaining about, measured the pressure and examined whether there were injuries on the body. It turned out to be difficult for me to talk about the symptoms: there was a feeling that they would not believe me, or vice versa, they would believe me so much that they would put me in a round-the-clock hospital. But everything was fine, the psychiatrist wrote down the data on the card, gave it to the orderly, and together with him sent me to the head.
The manager looked at the card, confirmed the diagnosis of OCD and depression, and prescribed treatment: an antidepressant, an antipsychotic, a mood stabilizer, tranquilizer tablets, and injections of B vitamins.
/guide/vitamins/
Vitamins: what foods contain and how to take supplements
The routine in the hospital was as follows: I arrived at eight in the morning, had breakfast and took the prescribed pills, took injections, dined and went home. Tablets were issued immediately for one day, but they could also be issued for two days, for example, before the weekend. Once after the injection, I went to an appointment with a clinical psychologist, he gave various tests and questionnaires that tested logic and intelligence.
Tablets were issued immediately for one day, but they could also be issued for two days, for example, before the weekend. Once after the injection, I went to an appointment with a clinical psychologist, he gave various tests and questionnaires that tested logic and intelligence.
About three times a week I went to see a psychiatrist in the same hospital. I told her about my condition and asked questions. I thought that as soon as I start taking medication, my mood will rise and my anxiety will go away. But this did not happen, so it seemed that everything was in vain and the treatment had to be abandoned. The psychiatrist explained to me that not all drugs begin to act instantly, she assured me that we were on the right track and we had to wait. These conversations made it easier. In my case, antidepressants began to work only on the third month of admission, when I no longer visited the day hospital.
These conversations made it easier. In my case, antidepressants began to work only on the third month of admission, when I no longer visited the day hospital.
Treatment at the day hospital lasted a month. All medications, medical consultations and meals were free. I spent money only on the road to the hospital and back - 600 R by public transport for the whole time.
/bye-depression/
“It reminded me of a strict regime sanatorium”: how much I spent on treating depression
After treatment, the symptoms of depression remained, but obsessive thoughts began to bother me less often: I stopped being afraid of open windows and was able to ride the escalator. Treatment had to be continued on an outpatient basis. Before I was discharged, the psychiatrist said that she would transfer my data to the psychiatric department. Now I will need to come to the local psychiatrist for prescriptions for medicines, and turn to him if the condition worsens or questions arise.
Treatment
Visiting a local psychiatristAfter I was discharged from the hospital, I came to the registration office of the psychiatric department with a passport and I was immediately sent to the district police officer. The doctor did not change the treatment and wrote out a prescription for the same medicines that were given in the day hospital. In the future, a referral to the district police officer was also not required. I just came to the appointment when I needed to update the prescription.
Government Decree of July 30, 1994 No. 890 with a list of categories of beneficiaries who are entitled to free medicines
District psychiatrists were different: some were polite, some were rude and rude. Using the brute force method, I found two normal specialists - when I made an appointment at the reception, I began to ask to be directed to them. Usually the registrar complied with my request.
Usually the registrar complied with my request.
Spent in six months of outpatient treatment — 8895 Р
| Preparation | Spending |
|---|---|
| Antidepressants | 5988 R |
| Normotimics | 2384 P |
| Antipsychotics | 419 P |
| Tranquilizers | 104 Р |
Antidepressants
5988 R
Normotimics
2384 R
neuroleptics
419 R
Transquilizers
104 R
Free medicines for the treatment of OCD are provided to certain privileged categories of people. I’m not a beneficiary, so I bought everything with my own money. Pharmacies don’t require a passport, but they put the date of issue of the medicine on the back and don’t sell more than prescribed by prescription. For example, according to a prescription for three months, I was given only three packs of an antidepressant. When I wanted to buy one more to have a supply, the pharmacist refused
When I wanted to buy one more to have a supply, the pharmacist refused Treatment
Second hospitalization and psychotherapyAfter six months of outpatient treatment, the district psychiatrist recommended to be treated again in the hospital. Antidepressants helped: my mood improved, I got energy and I wanted to live, but I felt a side effect from antipsychotics. I was terribly sleepy, my handwriting changed, it was difficult to write in class and generally follow the train of thought of the teacher. In addition, there were more intrusive thoughts.
In the day hospital, I was treated by the same psychiatrist as the first time. She adjusted the drug treatment so that I was not bothered by intrusive thoughts. She also said that a psychotherapist had appeared in the hospital and referred me to her for a consultation.
Unlike the psychiatrist's consultations during the first hospitalization, we did not discuss drugs and their effects with the psychotherapist. We talked about what is happening to me and what other methods can be used to combat this, in addition to drugs. At the first appointment, I briefly talked about my lifestyle, obsessive thoughts, compulsive actions, and how I tried to resist them even before the treatment. Then the doctor explained to me what obsessive-compulsive disorder is and how it manifests itself, why my struggle only worsened the condition and led to depression.
We talked about what is happening to me and what other methods can be used to combat this, in addition to drugs. At the first appointment, I briefly talked about my lifestyle, obsessive thoughts, compulsive actions, and how I tried to resist them even before the treatment. Then the doctor explained to me what obsessive-compulsive disorder is and how it manifests itself, why my struggle only worsened the condition and led to depression.
/psychotherapy-search/
How to choose a psychotherapist
We agreed that I would try to keep the number of compulsive acts to a minimum, and I would cope with anxiety from intrusive thoughts with the help of techniques.
Speak key phrases. Thoughts in themselves mean nothing, they can come to mind automatically. We agreed that when I had an obsessive thought, I would simply tell myself that it was a manifestation of OCD. Here are the two phrases that I used: “This is just my thought that…”, “I know that this thought is a manifestation of OCD…” So gradually I stopped identifying myself with my thoughts and realized that thinking about the bad is does not mean to be a bad person.
Separately, we discussed the issue of the materialization of thoughts. When terrible things are spinning in your head, and you hear from everywhere that thoughts are material, you get very worried. We discussed the fact that thoughts are intangible and you can’t invite trouble with them. This made it easier and the degree of emotions decreased.
Observe how the body reacts to anxiety. Every time I had anxiety from obsessive thoughts, I did not run away from it, but watched my body. I was shaking, my heartbeat increased, my breathing quickened, but I continued to live it. The psychotherapist said that I would not die from this. Yes, it is unpleasant and scary, but when you live emotions, you gradually learn to cope with them.
Keep a diary. In the course of the sessions, I became convinced that I cannot control the thoughts themselves - it is impossible, but I can control the reaction to them. So I started keeping a diary.
/psychotherapy/
How psychotherapy works
It was necessary to take notes according to the formula: A - situation, B - my thoughts, C - my emotions. Using such records, it is easier to track the thoughts that cause negative emotions and work them out. For example, when I could not fall asleep for a long time, I began to think that something was going wrong, and this caused anxiety. Then I wrote down the whole situation in a diary and instead of negative thoughts I formulated new ones: "My sleep does not depend on my will, and this is normal." It helped to get rid of anxiety, stop trying to sleep and go about your business. About half an hour later I went to bed and fell asleep peacefully.
Using such records, it is easier to track the thoughts that cause negative emotions and work them out. For example, when I could not fall asleep for a long time, I began to think that something was going wrong, and this caused anxiety. Then I wrote down the whole situation in a diary and instead of negative thoughts I formulated new ones: "My sleep does not depend on my will, and this is normal." It helped to get rid of anxiety, stop trying to sleep and go about your business. About half an hour later I went to bed and fell asleep peacefully.
| I also kept a mood diary. Before treatment, there was no point in monitoring the mood: it always turned out to be bad or indifferent | On antidepressants, I began to make entries in a diary every day and could track what affects my mood |
I also kept a mood diary. Before treatment, there was no point in monitoring the mood: it always turned out to be bad or indifferent. On antidepressants, I began to make entries in a diary every day and could track what affects my mood
Before treatment, there was no point in monitoring the mood: it always turned out to be bad or indifferent. On antidepressants, I began to make entries in a diary every day and could track what affects my mood
In the day hospital, I was treated for a month and a half, during which time I had only five sessions with a psychotherapist. All sessions, meals and drugs, as in the first hospitalization, were free. The only thing I had to spend money on was the road to the hospital and back, as well as the original antidepressant instead of the analogue provided in the dispensary. The doctor recommended the original, it suited me better.
3202 Р
spent on medicines and transport for a month and a half of treatment in the hospital
When I was discharged, the doctor told me that I was in a stable condition, the treatment helped me. I myself felt it: the mood was consistently good, and I quickly coped with obsessive thoughts. I was canceled all the drugs, except for antidepressants, then I had to continue taking them, be observed by the district psychiatrist and monitor my condition.
I was canceled all the drugs, except for antidepressants, then I had to continue taking them, be observed by the district psychiatrist and monitor my condition.
Spent one and a half months of treatment in a hospital — 3202 Р
| Expenditures | Spending |
|---|---|
| Antidepressants | 2422 R |
| Transport | 780 Р |
Antidepressants
2422 R
Transport
780 R
How do I feel after treatment
I stopped taking antidepressants a year and a month after discharge I spent another 14,640 R on them. Sometimes I have obsessive thoughts and compulsive actions, but I do not scold myself for this. I know that if I get upset, the symptoms will become more frequent. The psychiatrist warned me that OCD symptoms may appear periodically, but this is normal.
14,640 Р
spent on antidepressants for a year and one month
Coronavirus last spring was a test of strength for me. The condition worsened, compulsive actions resumed, I stopped leaving the house, I began to choke on the street, obsessive thoughts about death appeared. But I managed it on my own with the help of techniques taught to me by the therapist. I kept in my head the idea that if it worked then, it will work now.
The condition worsened, compulsive actions resumed, I stopped leaving the house, I began to choke on the street, obsessive thoughts about death appeared. But I managed it on my own with the help of techniques taught to me by the therapist. I kept in my head the idea that if it worked then, it will work now.
Before treatment, it was difficult for me to talk about my disorder. And now I openly talk about it and I can even joke about random manifestations of OCD. Almost everyone in my circle knows that I was being treated for OCD and depression. They help me notice compulsive actions and stop in time, treat me with understanding when I ask obvious things just in case - for example, did I close the door.
How often do people with OCD need to take drugs for life
Sergey Divisenko
psychotherapist
With the help of treatment, you can achieve remission - for a long time to get rid of the symptoms of OCD or reduce their number. Remission can occur both against the background of taking medications, and without them, against the background of psychotherapy.
Approximately 80% of patients with OCD stop taking medication sooner or later.
How much does OCD treatment cost?
In total, I treated OCD for one year and nine months. Of these, she was treated in a day hospital for two and a half months, and for a year and seven months - on an outpatient basis.
In the hospital, I only spent money on transport to and from the dispensary. Even during the second hospitalization, on the recommendation of the doctor, she bought antidepressants at the pharmacy and took them instead of those given in the hospital. The rest of the drugs, consultations and meals were free.
6 useful services for finding a psychotherapist
Most of the expenses are medicines during outpatient treatment.
Spent on OCD treatment for 1 year and 9 months — 27,337 R
| Expenditures | Spending |
|---|---|
| Antidepressants | 23 050 Р |
| Normotimics | 2384 P |
| Antipsychotics | 419 P |
| Tranquilizers | 104 Р |
| Transport during hospitalization | 1380 Р |
Save
- Obsessive Compulsive Disorder or OCD is a mental illness in which a person experiences obsessive thoughts and compulsive actions.

- OCD is considered a lifelong disorder, but remission can be achieved with the help of psychotherapy and drugs.
- OCD is treated in Russia by psychiatrists, psychotherapists and psychologists. Psychiatrists prescribe prescription drugs. Psychotherapists and psychologists conduct psychotherapy sessions.
- A visit to a neuropsychiatric dispensary will not prevent people with OCD from moving freely, driving a car, using weapons, or getting a job.
- Patients with OCD can receive care free of charge in state neuropsychiatric dispensaries or at their own expense in private clinics.
Did you also have an illness that affected your lifestyle or attitude? Share your story.
Tell
Personal experience: what to do when you have a million obsessive frightening thoughts in your head?
Health
Imagine that every second, frightening obsessive thoughts are born in your head: you are afraid to yell obscenities at a colleague, beat your mother, pierce your own eye with a fork during dinner. This is exactly what people with obsessive-compulsive disorder (OCD) experience. Sobaka.ru recorded a monologue of a journalist from St. Petersburg, whose life turned into hell because of such thoughts, but he managed to get out of it (and told how).
This is exactly what people with obsessive-compulsive disorder (OCD) experience. Sobaka.ru recorded a monologue of a journalist from St. Petersburg, whose life turned into hell because of such thoughts, but he managed to get out of it (and told how).
As a rule, most patients with obsessive-compulsive disorder have all sorts of intrusive and frightening thoughts in their heads. Such thoughts are actually called obsessions. And compulsions are rituals that supposedly help you cope with thoughts. The patient invents them himself: wash his hands 36 times so that nothing bad happens, pat his dog 15 times before leaving the house. I don’t know if I was lucky or not, but I didn’t have rituals (except for one - every time I closed my eyes for a second while driving, when I experienced an obsessive fear that I would now crash my car). But there were obsessions that ruined my life for years.
How it all began: a monster in a cap
I well remember the first obsessive thought - I was 13 years old, and my mother and I were on vacation in the Crimea. During the bus ride, I imagined a strange mythical creature with yellow teeth, a mouth like a hippopotamus, clawed paws and some completely wild grin. I imagined how this creature stuck to the glass of the bus. At the same time, the monster had a funny cap on its head - obsessions are often ridiculous, but at the same time very frightening. I couldn't get that image out of my head. He followed me throughout the rest. Later, I learned that in boys, the first symptoms of OCD appear exactly at the age of 13-15, and already at this age it is worth contacting a psychotherapist. However, I began to receive adequate treatment only after almost 10 years.
During the bus ride, I imagined a strange mythical creature with yellow teeth, a mouth like a hippopotamus, clawed paws and some completely wild grin. I imagined how this creature stuck to the glass of the bus. At the same time, the monster had a funny cap on its head - obsessions are often ridiculous, but at the same time very frightening. I couldn't get that image out of my head. He followed me throughout the rest. Later, I learned that in boys, the first symptoms of OCD appear exactly at the age of 13-15, and already at this age it is worth contacting a psychotherapist. However, I began to receive adequate treatment only after almost 10 years.
After that trip, the obsessions receded for a while and returned to me after finishing school, at the age of 17. They were the quintessence of all the most disgusting things my brain could generate. Evil and scary pictures, vulgar and depraved images associated with my friends and relatives ... The worst thing is that in real life I adhered to strict moral principles, but my thoughts made me doubt that I was a good person. Would a good person come up with the idea of standing up and yelling at colleagues, beating the chef of the restaurant where he works, hitting his mother? And all these thoughts visited me constantly. Of course, it never came to direct action - I was absolutely harmless to others, thoughts caused suffering only to me. In general, contrasting obsessions always have a very unpleasant content for a person; they contradict his ethical principles. For example, if a person is deeply religious, while suffering from OCD, blasphemous thoughts related to religion and images of saints climb into his head.
Would a good person come up with the idea of standing up and yelling at colleagues, beating the chef of the restaurant where he works, hitting his mother? And all these thoughts visited me constantly. Of course, it never came to direct action - I was absolutely harmless to others, thoughts caused suffering only to me. In general, contrasting obsessions always have a very unpleasant content for a person; they contradict his ethical principles. For example, if a person is deeply religious, while suffering from OCD, blasphemous thoughts related to religion and images of saints climb into his head.
How to live if you have OCD
By the age of 22, my illness had reached an acute phase - I had practically no episodes of respite, at least some kind of enlightenment during the day. Probably the best moment at that time was waking up: when I first opened my eyes, my head was still clear. But when faced with reality, the brain gave out flashes of obsessions. I could go into the kitchen and at the same moment the thought arose that now I would beat my mother. I was walking to the bathroom, and at that time an absurd word settled in my head. For example, a carburetor. I didn't know where it came from, but I couldn't throw it away. At some point, I began to spontaneously translate words into English. There doesn't seem to be anything wrong with that, but it bothered me a lot. English words brazenly climbed into my head, interfering with the normal train of thought.
I was walking to the bathroom, and at that time an absurd word settled in my head. For example, a carburetor. I didn't know where it came from, but I couldn't throw it away. At some point, I began to spontaneously translate words into English. There doesn't seem to be anything wrong with that, but it bothered me a lot. English words brazenly climbed into my head, interfering with the normal train of thought.
Tip #1: Separate yourself from the illness. She's just trying to hit you where it hurts the most. Would you like bad thoughts to come true? Most likely no. It turns out that you are not a scoundrel.
None of my acquaintances and friends knew exactly what was happening to me. But I behaved extremely strangely and began to avoid everyone. When you meet people, they talk about life, work, everyday affairs, girls, and obsessions swirl in your head (or you are completely afraid to yell obscenities at your interlocutors or hit them in the face), then communication turns out so-so. These thoughts greatly distracted me, they hit me on the head like hammers - bang, and complete disorientation sets in. In addition, I began to consider myself a very bad person, I was really ashamed of myself. It was only during the treatment that I realized that you are not your disease. And you should not think that you are a moral freak if, due to a mental disorder, frightening obsessions climb into your head. This is important knowledge for OCD patients that makes life easier.
These thoughts greatly distracted me, they hit me on the head like hammers - bang, and complete disorientation sets in. In addition, I began to consider myself a very bad person, I was really ashamed of myself. It was only during the treatment that I realized that you are not your disease. And you should not think that you are a moral freak if, due to a mental disorder, frightening obsessions climb into your head. This is important knowledge for OCD patients that makes life easier.
Loss of job and relationships
When I was 23, everything went to hell - first I was fired from a job that I really liked. I worked as a journalist, but I couldn't write tests anymore. I sat down for an interview, and a fear arose in my head that I would pierce my eyes with a pen or bite off my tongue. Contrasting obsessions are often aimed at harming oneself. You're afraid of losing control, afraid of self-mutilation. The quality of my texts fell to the bottom, problems began in the editorial office. I had to leave my place of work (I honestly told my editor-in-chief that I was crazy), a month later the girl I loved left me. She was aware of my illness, tried to treat it with understanding, but could not stand everything that happened to me. I tried to catch on for dubious part-time jobs, but due to obsessions I could not stay even as a loader. In fact, I lost all ability to work.
I had to leave my place of work (I honestly told my editor-in-chief that I was crazy), a month later the girl I loved left me. She was aware of my illness, tried to treat it with understanding, but could not stand everything that happened to me. I tried to catch on for dubious part-time jobs, but due to obsessions I could not stay even as a loader. In fact, I lost all ability to work.
It seemed to me that a huge tank fired at my inner world and blew it to pieces. Seeing no way out, I decided that I can safely put an end to it: after all, I will have to stay in this nightmare all my life. But later he began a long and serious treatment with a psychotherapist.
Unsuccessful attempts at treatment
In general, in my life there were three experiences of going to specialists. At the age of 17, my mother took me to a psychiatrist after I told her about my first obsessive thoughts. He prescribed neuroleptics for me, which most likely did not even suit me, and let me go. We did not do psychotherapy then - although, in my experience, it is it, and not drugs, that helps to bring the disease under control. But I found out about this later.
We did not do psychotherapy then - although, in my experience, it is it, and not drugs, that helps to bring the disease under control. But I found out about this later.
The second time I talked not with a psychiatrist, but with a psychotherapist. I came to him when I was 21, we worked with him for about two years. But in fact, he helped me cope with only one problem - he explained that if I have terrible thoughts due to illness, this does not mean that I am a bad person. I partially stopped self-flagellation, but the obsessions never left my head. Later, I realized that the doctor had little understanding of the treatment of OCD, and all our work with him was built incorrectly.
How to choose a competent doctor
The third doctor helped me cope with the disease - trips to him began just at the time when I hit the bottom. It seemed to me that my case was hopeless, but the initial trust in the specialist was still there: the psychotherapist I chose had a good education, authority in the professional environment, I liked talking to him. The doctor conducted a paid appointment, and at that time I was left without a job and, accordingly, money, so I turned to my family for help. This is an important tip for all patients with mental disorders: do not be afraid to tell your loved ones about your problem and together find money for adequate therapy. It is customary for us to collect funds for the treatment of physical illnesses, but for some reason, with a mental disorder, people are afraid to ask for help (and this is a big mistake).
The doctor conducted a paid appointment, and at that time I was left without a job and, accordingly, money, so I turned to my family for help. This is an important tip for all patients with mental disorders: do not be afraid to tell your loved ones about your problem and together find money for adequate therapy. It is customary for us to collect funds for the treatment of physical illnesses, but for some reason, with a mental disorder, people are afraid to ask for help (and this is a big mistake).
At the first appointment, I told the doctor about my problem, about all the painful obsessions. I was afraid that I would not be able to express what I feel, but the words literally poured out of me. The doctor listened and asked questions, structured information about me. At the end of the appointment, he summarized everything I had described and told me about a method that is considered effective in combating OCD - this is cognitive behavioral therapy (CBT)
Tip # 2: adequate treatment of OCD is possible only with the help of a competent doctor. The most effective method of treatment is CBT. If you are faced with a disease, then start working with a specialist in this area.
The most effective method of treatment is CBT. If you are faced with a disease, then start working with a specialist in this area.
If you have OCD or suspect you have any other mental illness, seek out a competent professional immediately. Self-medication is most often useless and even dangerous. Ask a potential doctor directly if he has experience in treating patients with OCD and what kind of psychotherapy method he uses in his work. In my experience, cognitive-behavioral therapy provides the most consistent and high-quality results, so it's best to have your doctor work within CBT. From the side, you will be able to distinguish it by its special structure and system: you are not just chatting with the doctor, but moving along a clearly defined treatment plan. CBT involves independent homework, it is an educational form of psychotherapy. Having mastered the techniques, you can apply them yourself, for example, to avoid a recurrence of the disease.
Why work with thoughts
During my treatment, the doctor combined pharmacology and psychotherapy. I took neuroleptics and antidepressants. Pills can be a good safety cushion, but I don't think they're paramount. Hoping to defeat OCD by suppressing medication without going through psychotherapy is, in my opinion, a hopeless path.
I took neuroleptics and antidepressants. Pills can be a good safety cushion, but I don't think they're paramount. Hoping to defeat OCD by suppressing medication without going through psychotherapy is, in my opinion, a hopeless path.
Cognitive Behavioral Therapy helps to fundamentally change the way of thinking and through this to achieve recovery. See, our emotions are caused by our thoughts. That is, our emotional reaction and our state depend on how we mentally perceive the world around us. After all, it’s not even the obsessions themselves that cause problems with OCD – all people have them to some extent. And the fact that these obsessions seem realistic to the patient. For example, you have the idea that you can hit a person. If you are healthy, then most likely you will think: "Well, okay, I'm not going to do this." A person with OCD is likely to perceive this thought differently: “Oh, what a scoundrel I am! How can I even think about such a thing? What if I lose control of myself and really do it. He will experience fear, horror, disgust. But if you change your train of thought, recolor it from negative to neutral, then it will be easier to endure the symptoms of OCD. Obsessions will not be perceived as something terrible, but as just thoughts. Over time, they will disappear on their own.
He will experience fear, horror, disgust. But if you change your train of thought, recolor it from negative to neutral, then it will be easier to endure the symptoms of OCD. Obsessions will not be perceived as something terrible, but as just thoughts. Over time, they will disappear on their own.
Imagine all the worst
The core of my work was the exposure method. The doctor explained to me what it is: if frightening thoughts come, you need not to suppress them, but on the contrary, try to strengthen and purposefully think about it until they weaken. This is a rather intimidating exercise, so at the beginning of treatment it must be performed under the supervision of a specialist.
During the exercise, I imagined bullying my dog. How I tear my beloved dog apart, break his jaws, hurt him. At first it was very hard for me to think about it. But after a few minutes of practice, I noticed that the thought that I would kill the dog caused me less and less anxiety. Another time, I imagined how brutally I raped and perverted members of my family. This was the hardest part because I hated those thoughts more than anyone else. It was painful to focus on the disgusting images, but I got over myself and continued. At the end of the practice, I again noticed that the thought that I was abusing my relatives caused me less and less anxiety. I continued to do these practices every day. My work began to bear fruit.
This was the hardest part because I hated those thoughts more than anyone else. It was painful to focus on the disgusting images, but I got over myself and continued. At the end of the practice, I again noticed that the thought that I was abusing my relatives caused me less and less anxiety. I continued to do these practices every day. My work began to bear fruit.
Tip #4: Don't be afraid to lose control and do what the contrasting obsessions dictate. People with OCD never do all the crazy things that come into their heads. It is only a thought, and thought does not equal action.
The exposure was not the only exercise: to help me cope with the disorder, the doctor used a whole range of techniques. For example, we made tablets of obsessive thoughts - I wrote out the obsession, then the emotion that it evokes in me, I gave it an assessment. Later, the therapist told me about the method of selecting alternatives. First I described the negative thought, and then the alternative to it, that is, my objection to it. The most common objection was: "It's just OCD, my thought has nothing to do with reality, I won't do what I'm afraid of." Yes, indeed, a large number of studies confirm that people with obsessive-compulsive disorder never commit obsessive actions. None of the OCD patients bit off their tongue, turned the steering wheel into the oncoming lane, or shouted obscenities at the interlocutor. Absolutely no one. These are just their irrational thoughts that have nothing to do with reality.
The most common objection was: "It's just OCD, my thought has nothing to do with reality, I won't do what I'm afraid of." Yes, indeed, a large number of studies confirm that people with obsessive-compulsive disorder never commit obsessive actions. None of the OCD patients bit off their tongue, turned the steering wheel into the oncoming lane, or shouted obscenities at the interlocutor. Absolutely no one. These are just their irrational thoughts that have nothing to do with reality.
A person with OCD believes that his thoughts are material. We conducted a rather amusing experiment with the doctor. I advise everyone who is worried about the materiality of their thoughts to try it (after all, not only people with mental disorders sometimes suffer from this). Put a piece of paper on the table and try to move it to the side with the power of thought. Focus on this process. Repeat: "I order the piece of paper to move to the side." Nothing comes out? Does the paper stay in place? In general, this is not surprising. After all, thoughts do not determine our actions.
After all, thoughts do not determine our actions.
On the road to recovery
Another piece of advice is that when dealing with OCD, you need to prepare for a long job. Some patients hope to get the result quickly, but this is a big mistake, because of which many people abandon the treatment and lose hope. I didn't see a lasting positive effect for several months. But this is normal - the doctor was looking for a key to me, he understood my situation.
The effect of cognitive-behavioral therapy in severe cases of the disease (and mine was just like that) begins after 10-15 sessions. And I'm not talking about a complete recovery, but about positive changes. If the patient does not observe any positive effect even after so many meetings with the doctor, then it is worth discussing this with him directly.
Tip #4: Every job brings results. If you undergo adequate treatment under the guidance of a good specialist, you can defeat the disease. Are you doing nothing? OCD will only get worse and more and more poisonous to life.
Fighting OCD is a regular, monotonous job. You don't have to be a hero or a genius to do it. You will need diligence, patience, the ability to wait and the support of a competent therapist. I went to the doctor every week for six months. Then the sessions began to take place less frequently, but continued for two years.
I felt I had overcome my obsessions eight months after my first visit to my doctor. I was hired at my previous job, I began to feel confident, and the texts began to be written easily (of course, I was no longer afraid to bite off my tongue and fill my desktop with blood).
Do obsessive thoughts come into my head now
Having dealt with OCD, I really became a different person. Almost three years have passed since the moment when I felt free from obsessions, and a year ago the doctor completely canceled drug therapy. During the illness I was in a depressed state, and now I get real pleasure from life. I have a new job, I married a beautiful girl. Illness no longer poses any obstacle to my development.
Illness no longer poses any obstacle to my development.
An unexpected positive side of what I experienced: after such an experience, I seem to no longer be afraid of life's difficulties. A great thought popped into my head—if I can handle OCD, I can handle anything. It's like such a huge dragon that you defeated, so other dragons are not afraid of you. Before my recovery, I was a little man who had gone down with fear, now my character has been tempered and I have become impenetrable. Of course, I'm not an Ironman, but it's really hard to unsettle me.
Perfectionism is very common among people with OCD - they need to keep everything under control, they need everything to be perfect. If something is done wrong, it causes suffering to a person. At the same time, perfectionism reaches the point of absurdity. Patients arrange books alphabetically, and the pile on the carpet should be combed strictly in one direction. If the patient does not do everything “as it should”, he will be plagued by anxiety. I realized that perfectionism is a good feature of the disease, you just need to learn how to apply it in the right way. I started to use this trait in my work - I can’t do anything with my left heel and I take the process very seriously. Sometimes I go too far with my desire for excellence, but still a serious attitude to work affects life positively.
I realized that perfectionism is a good feature of the disease, you just need to learn how to apply it in the right way. I started to use this trait in my work - I can’t do anything with my left heel and I take the process very seriously. Sometimes I go too far with my desire for excellence, but still a serious attitude to work affects life positively.
In general, obsessive-compulsive disorder is a disease that is considered chronic. Therefore, people who have experienced a problem should remember that the symptoms may return. But once you've had a good CBT course, you already know how to deal with this flare-up. OCD is an insidious opponent, it can stealthily watch for you and punch you in the face. But if you are well trained, you will block first and then win. So now I have no fear that the disease will return.
You might be wondering if I have obsessive thoughts? Sometimes they come. As well as all the inhabitants of the planet Earth. Once I was talking to my mother, asked if obsessions come to her.