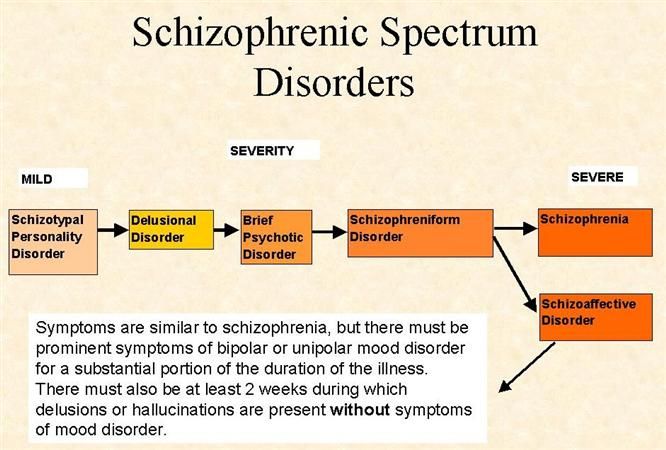
What is mild psychosis
Early Psychosis and Psychosis | NAMI: National Alliance on Mental Illness
In this 2-part podcast series, NAMI Chief Medical Officer Dr. Ken Duckworth guides discussions on early psychosis that offer insights from individuals, family members and mental health professionals. Read the transcript.
Note: Content includes discussions on topics such as suicide attempts and may be triggering.
Most people think of psychosis as a break with reality. In a way it is. Psychosis is characterized as disruptions to a person’s thoughts and perceptions that make it difficult for them to recognize what is real and what isn’t. These disruptions are often experienced as seeing, hearing and believing things that aren’t real or having strange, persistent thoughts, behaviors and emotions. While everyone’s experience is different, most people say psychosis is frightening and confusing.
Psychosis is a symptom, not an illness, and it is more common than you may think. In the U.S., approximately 100,000 young people experience psychosis each year. As many as 3 in 100 people will have an episode at some point in their lives.
Early or first-episode psychosis (FEP) refers to when a person first shows signs of beginning to lose contact with reality. Acting quickly to connect a person with the right treatment during early psychosis or FEP can be life-changing and radically alter that person’s future. Don’t wait to take the first step and prepare yourself with information by reviewing these tip sheets:
What is Early and First-Episode Psychosis?
Early Psychosis: What's Going on and What Can You Do?
Encouraging People to Seek Help for Early Psychosis
Early Intervention: Tips for School Staff and Coaches
Symptoms
Early warning signs before psychosis
Early psychosis or FEP rarely comes suddenly. Usually, a person has gradual, non-specific changes in thoughts and perceptions, but doesn't understand what's going on.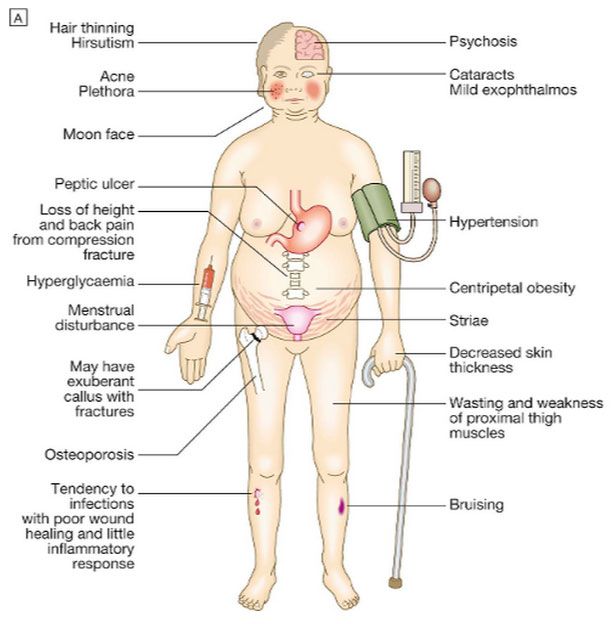 Early warning signs can be difficult to distinguish from typical teen or young adult behavior. While such signs should not be cause for alarm, they may indicate the need to get an assessment from a doctor.
Early warning signs can be difficult to distinguish from typical teen or young adult behavior. While such signs should not be cause for alarm, they may indicate the need to get an assessment from a doctor.
Encouraging people to seek help for early psychosis is important. Families are often the first to see early signs of psychosis and the first to address the issue of seeking treatment. However, a person's willingness to accept help is often complicated by delusions, fears, stigma and feeling unsettled. In this case, families can find the situation extremely difficult, but there are engagement strategies to help encourage a person to seek help.
It's important to get help quickly since early treatment provides the best hope of recovery by slowing, stopping and possibly reversing the effects of psychosis. Early warning signs include the following:
- A worrisome drop in grades or job performance
- Trouble thinking clearly or concentrating
- Suspiciousness or uneasiness with others
- A decline in self-care or personal hygiene
- Spending a lot more time alone than usual
- Strong, inappropriate emotions or having no feelings at all
Signs of early or first-episode psychosis
Determining exactly when the first episode of psychosis begins can be hard, but these signs and symptoms strongly indicate an episode of psychosis:
- Hearing, seeing, tasting or believing things that others don’t
- Persistent, unusual thoughts or beliefs that can’t be set aside regardless of what others believe
- Strong and inappropriate emotions or no emotions at all
- Withdrawing from family or friends
- A sudden decline in self-care
- Trouble thinking clearly or concentrating
Such warning signs often point to a person’s deteriorating health, and a physical and neurological evaluation can help find the problem.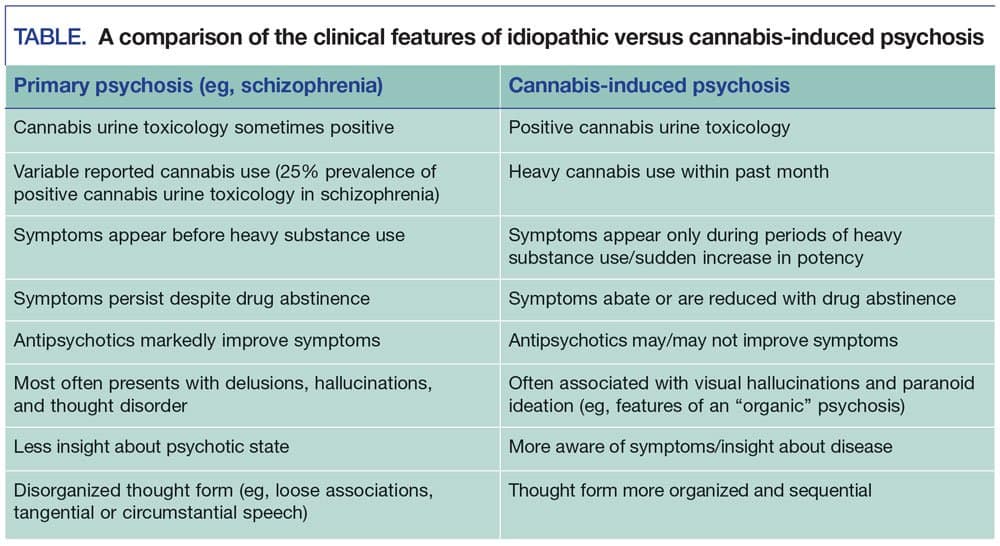 A mental health professional performing a psychological evaluation can determine if a mental health condition is involved and discuss next steps. If the psychosis is a symptom of a mental health condition, early action helps to keep lives on track.
A mental health professional performing a psychological evaluation can determine if a mental health condition is involved and discuss next steps. If the psychosis is a symptom of a mental health condition, early action helps to keep lives on track.
Psychosis
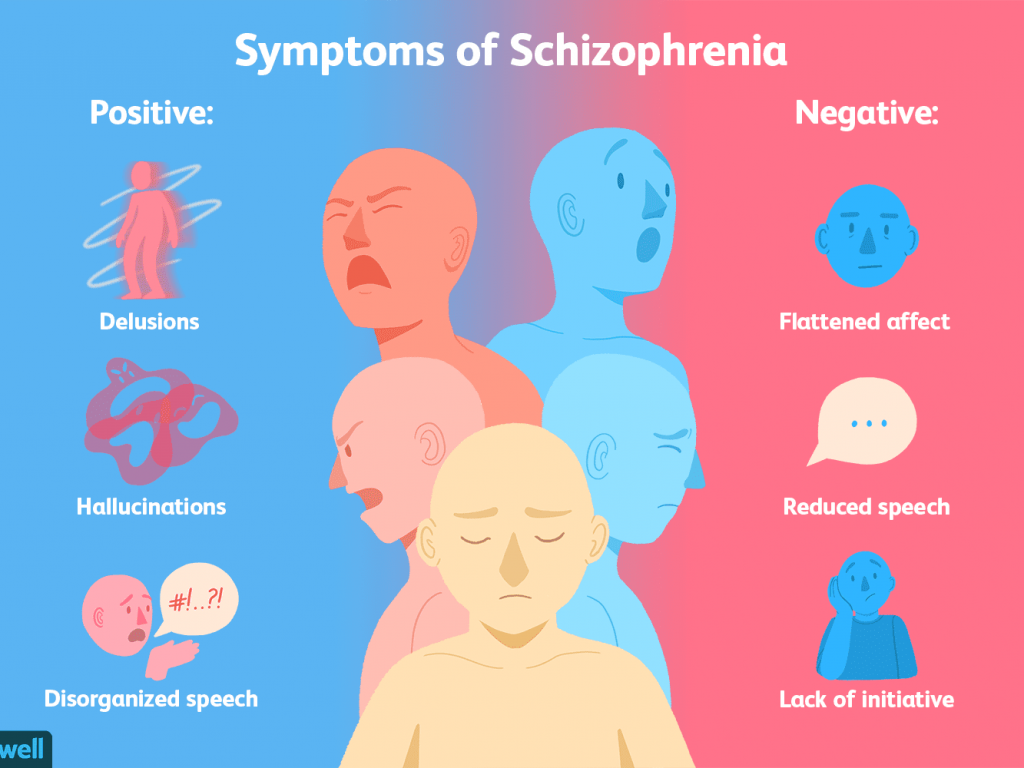
Psychosis includes a range of symptoms but typically involves one of these two major experiences:
Hallucinations are seeing, hearing or feeling things that aren’t there, such as the following:
- Hearing voices (auditory hallucinations)
- Strange sensations or unexplainable feelings
- Seeing glimpses of objects or people that are not there or distortions
Delusions are strong beliefs that are not consistent with the person’s culture, are unlikely to be true and may seem irrational to others, such as the following:
- Believing external forces are controlling thoughts, feelings and behaviors
- Believing that trivial remarks, events or objects have personal meaning or significance
- Thinking you have special powers, are on a special mission or even that you are God.
Causes
We are still learning about how and why psychosis develops, but several factors are likely involved. We do know that teenagers and young adults are at increased risk of experiencing an episode of psychosis because of hormonal changes in their brain during puberty.
Several factors that can contribute to psychosis:
- Genetics. Many genes can contribute to the development of psychosis, but just because a person has a gene doesn’t mean they will experience psychosis. Ongoing studies will help us better understand which genes play a role in psychosis.
- Trauma. A traumatic event such as a death, war or sexual assault can trigger a psychotic episode. The type of trauma—and a person’s age—affects whether a traumatic event will result in psychosis.
- Substance use. The use of marijuana, LSD, amphetamines and other substances can increase the risk of psychosis in people who are already vulnerable.

- Physical illness or injury. Traumatic brain injuries, brain tumors, strokes, HIV and some brain diseases such as Parkinson’s, Alzheimer’s and dementia can sometimes cause psychosis.
- Mental health conditions. Sometimes psychosis is a symptom of a condition like schizophrenia, schizoaffective disorder, bipolar disorder or depression.
Diagnosis
A diagnosis identifies an illness; symptoms are components of an illness. Health care providers draw on information from medical and family history and a physical examination to diagnose someone. If causes such as a brain tumor, infection or epilepsy are ruled out, a mental illness might be the reason.
If the cause is related to a mental health condition, early diagnosis and treatment provide the best hope of recovery. Research shows that the earlier people experiencing psychosis receive treatment, the better their long-term quality of life.
Treatment
Early or first-episode psychosis
Early treatment of psychosis, especially during the first episode, leads to the best outcomes.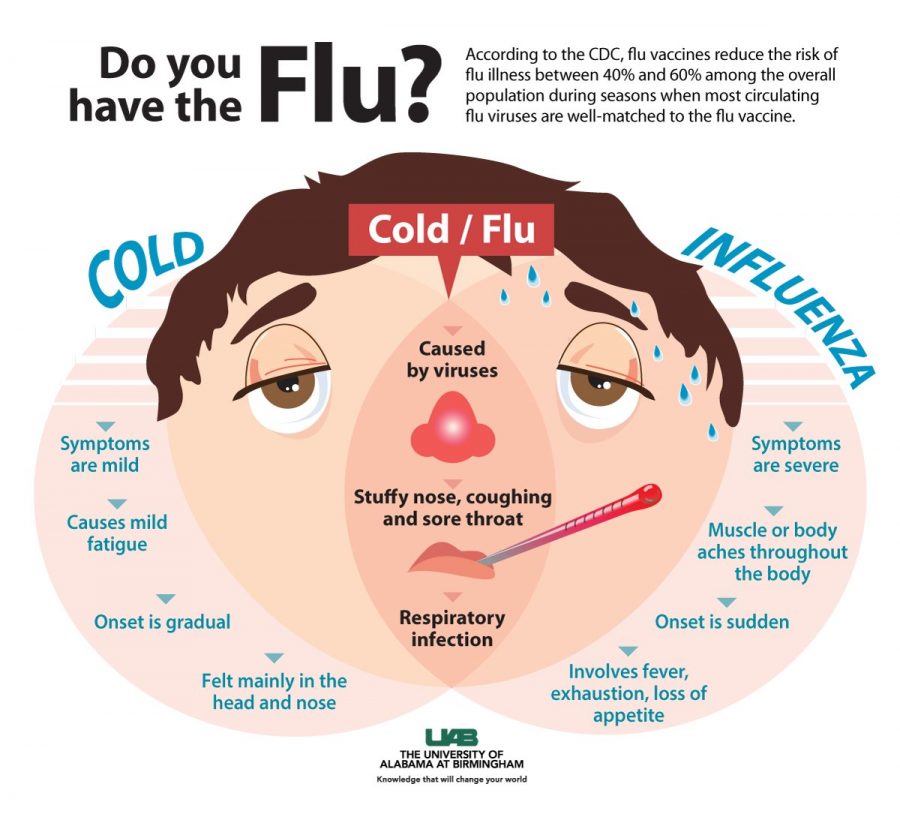
Research has shown significant success using a treatment approach called Coordinated Specialty Care (CSC). CSC uses a team of health professionals and specialists who work with a person to create a personal treatment plan based on life goals while involving family members as much as possible.
CSC has the following key components:
- Case management
- Family support and education
- Psychotherapy
- Medication management
- Supported education and employment
- Peer support
SAMHSA maintains an Early Serious Mental Illness (ESMI) Treatment Locator as a source of information for family members who are seeking CSC programs in the US. Portions of their website are available in Spanish.
Psychosis treatment
Traditional treatment for psychosis involves psychotherapy and medication. Several types of therapy have successfully helped individuals learn to manage their condition. In addition, medication targets symptoms and helps reduce their impact.
Related Conditions
Psychosis can be related to several mental health conditions:
- Bipolar Disorder
- Schizoaffective Disorder
- Schizophrenia
- Substance use disorders / Dual Diagnosis
Psychosis: Causes, symptoms, and treatments
Psychosis involves a loss of contact with reality. It is present in many conditions, including schizophrenia and bipolar disorder. Hallucinations and delusions are its most common symptoms.
People with psychosis may experience disruptions in their thoughts and perceptions, causing them to see their world differently. It is a common symptom in many medical and neurologic conditions.
Psychosis can affect anyone. According to the National Alliance on Mental Health (NAMI), 100,000 young people in the United States experience psychosis every year. At the same time, up to 3 in 100 people will have an episode in their lifetime.
In this article, learn more about psychosis, including what causes it and the treatment options available.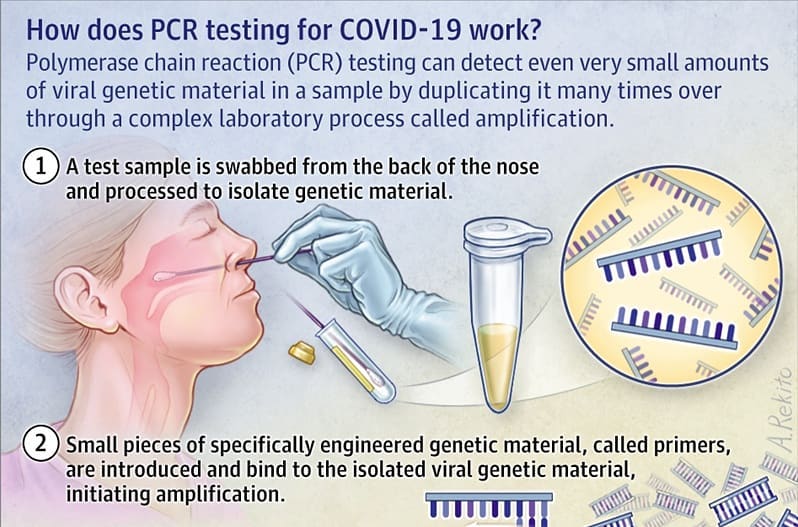
Psychosis affects a person’s thoughts and perceptions. It alters how they process information, making it difficult to determine what is real from what is not.
People with psychosis may hear, see, smell, taste, or feel things that are not there. They can also hold strong beliefs or bizarre ideas, such as that someone is out to get them or that someone is monitoring their activities when these are not the case.
Psychosis feels or appears real to a person. The Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) states that a person may not be aware that they have psychosis. It can be overwhelming and confusing.
Sometimes, the symptoms can cause the person to harm themselves. In rare cases, they may hurt another person.
Psychosis is one of the key symptoms of schizophrenia and other psychotic disorders. According to the DSM-5, it also co-occurs with many mood and substance use disorders.
Depending on the cause, psychosis can appear quickly or cause slow, gradual changes in a person’s thoughts and perceptions. It can also be mild or severe.
It can also be mild or severe.
In some cases, it may be mild when it first appears but become more intense over time. While psychosis includes a range of symptoms, it often involves one of two significant experiences.
The below sections explore the early signs of psychosis and two common symptoms in more detail.
Early signs
Early or first-episode psychosis (FEP) is the period when a person first begins to experience psychosis. The symptoms can be difficult to distinguish from typical behavior. These include:
- a significant drop in job performance or school grade
- difficulty concentrating or thinking clearly
- uneasiness or suspiciousness around others
- lacking emotions or having strong, inappropriate ones
- social withdrawal
- sudden decline in self-care or personal hygiene
The DSM-5 states that psychosis involves abnormalities in one of the following categories or domains:
- Hallucinations: Experiences a person perceives to be real despite the lack of stimulus to cause them.
- Delusions: False beliefs that a person holds despite a lack of evidence or proof.
- Disorganized thought: Having thoughts that are not logical, unrelated, or loosely connected. A person’s thought process may drift away from the topic. Their speech may make no sense to others.
- Catatonia: The person may become unresponsive or oppose stimuli (negativism) or present with unintentional movements or activities that lack purpose (catatonic excitement).
- Disorganized behavior: Unpredictable or inappropriate emotional responses that are not in line with the situation.
- Negative symptoms: A decline in emotions, words, movements, or motivation (anhedonia).
Hallucinations
Hallucinations may cause a person to see, hear, feel, taste, or smell something that is not there. Of these, auditory hallucinations appear to be the most common.
A person with auditory hallucinations hears things and believes them to be real when they do not exist.![]()
A person may hear incoherent sounds or distinct voices. They can perceive them to come through the ears, anywhere external to them, or in their mind.
Hearing voices may be very distressing, especially when they are commanding, derogatory, haunting, or threatening. It can affect a person’s actions and cause them to harm themselves or others. It may also cause a person to attempt suicide.
Suicide prevention
If you know someone at immediate risk of self-harm, suicide, or hurting another person:
- Ask the tough question: “Are you considering suicide?”
- Listen to the person without judgment.
- Call 911 or the local emergency number, or text TALK to 741741 to communicate with a trained crisis counselor.
- Stay with the person until professional help arrives.
- Try to remove any weapons, medications, or other potentially harmful objects.
If you or someone you know is having thoughts of suicide, a prevention hotline can help. The 988 Suicide and Crisis Lifeline is available 24 hours a day at 988. During a crisis, people who are hard of hearing can use their preferred relay service or dial 711 then 988.
The 988 Suicide and Crisis Lifeline is available 24 hours a day at 988. During a crisis, people who are hard of hearing can use their preferred relay service or dial 711 then 988.
Click here for more links and local resources.
Delusions
A person may also experience delusions during a psychotic episode. The most commonly encountered types of delusions include:
- Erotomanic delusions: The belief that another person is in love with them.
- Delusions of grandeur: A strong belief that the person has a special power or authority.
- Thought broadcasting: The belief that the person is broadcasting their thoughts and that others can perceive them.
A person may also experience:
- depression
- anxiety
- social withdrawal
- lack of motivation
- overall difficulty functioning
- difficulty focusing
- sleep problems
The length of a person’s psychosis varies depending on the type of psychosis.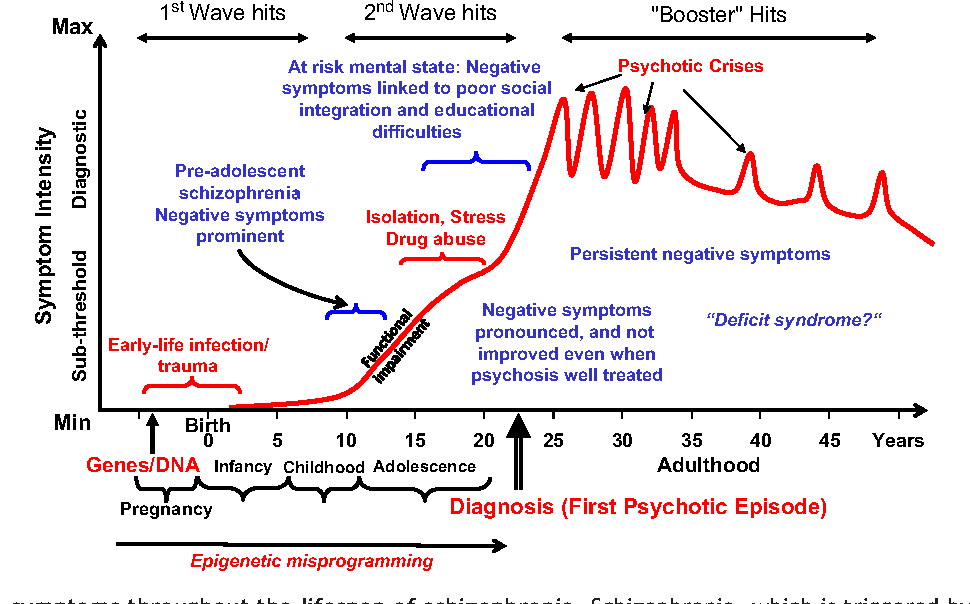
Substance or medication-induced psychosis tends to resolve shortly after the substance clears from a person’s system. But psychosis triggered by amphetamines, phencyclidine (PCP), and cocaine may last for several weeks.
Meanwhile, a brief psychotic disorder usually lasts for less than a month. According to the DSM-5, psychotic symptoms need to be present in people with schizophrenia for a significant portion of time during 1 month or longer.
Psychosis is not an illness in and of itself. It is often a symptom of another condition. To determine what may be causing the psychosis, a doctor will perform a thorough history.
This includes understanding the person’s personal, family, medical, cultural, social, and religious history. They will also ask about the person’s psychotic symptoms, including their course, duration, and severity.
The doctor will conduct a physical examination, including a mental and neurological exam.
If the signs and symptoms suggest an underlying medical condition, a doctor may request tests, including:
- complete blood count
- metabolic profile
- thyroid function tests
- urine toxicology testing
- measurement of parathyroid hormone, calcium, niacin, vitamin B12, and folate
The doctor may also consider testing for HIV and syphilis. Brain imaging is often not necessary except when the person presents with a new, severe headache, a history of recent significant head trauma, or focal neurological deficits.
Brain imaging is often not necessary except when the person presents with a new, severe headache, a history of recent significant head trauma, or focal neurological deficits.
They may also do tests to rule out other factors, including:
- the use of drugs or other substances
- a head injury
- other medical conditions, such as multiple sclerosis (MS) or a brain tumor
If the signs indicate a psychiatric cause, the doctor will refer to criteria from the DSM-5 to make a diagnosis.
Psychosis can happen due to several factors. It may be a symptom of a mental condition. Psychotic disorders such as delusional disorder and schizotypical disorder share psychosis as a symptom.
Studies show that a combination of genetic and environmental factors can lead to psychosis. Certain environmental factors may increase a person’s risk for psychosis, including:
- maternal infections and obstetric complications
- maternal stress and malnutrition
- child abuse
- head injury during childhood
- migration
- drug misuse
Other causes of psychosis include:
- brain changes
- alcohol and substance misuse
- general medical conditions
- certain psychiatric and neurological conditions
- certain prescription drugs
- sex hormones
- lack of sleep
Traumatic events such as war, sexual assault, or death can also trigger a psychotic episode.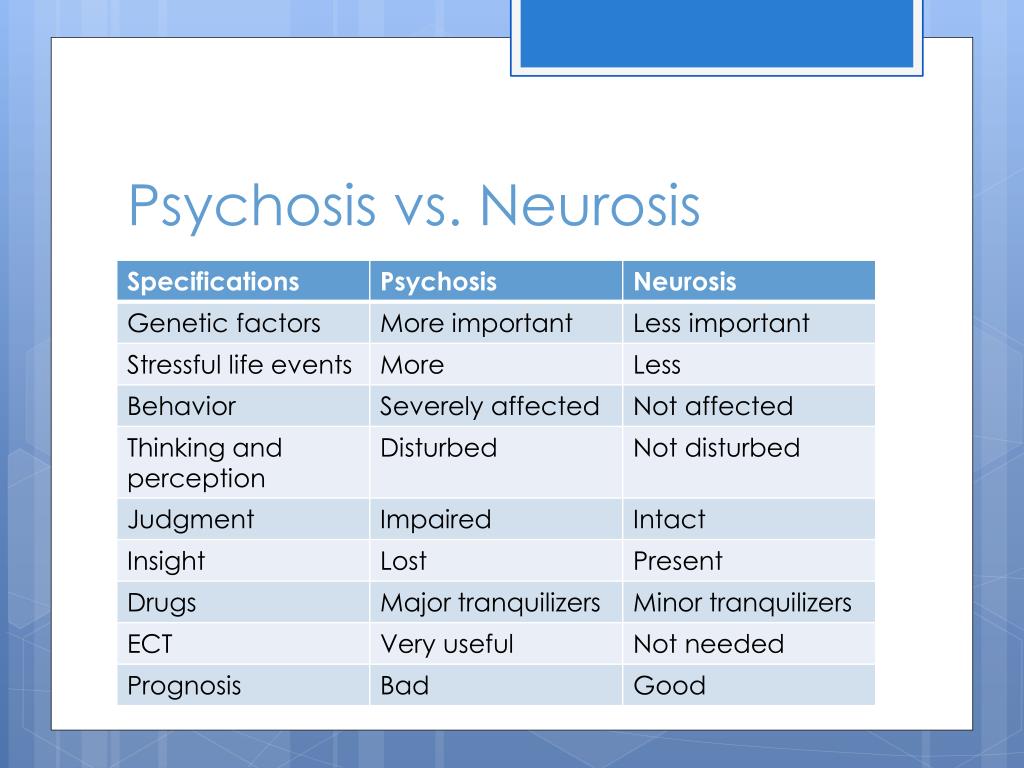
The mechanisms by which psychosis occurs are not entirely clear, but many studies point to imbalances in the brain’s chemicals.
The positive symptoms of psychosis are associated with excess dopamine activity (a neurotransmitter related to mood), as well as a decrease in the activity of receptors for glutamate (another neurotransmitter).
Some studies also point to imbalances in the activity of gamma-aminobutyric acid (GABA) and acetylcholine.
Anyone experiencing psychosis should receive urgent medical attention. Treatment can provide both short- and long-term help.
Antipsychotic drugs
Antipsychotic drugs are the primary treatment for people with psychotic illnesses.
Antipsychotics can reduce psychosis symptoms in people with psychiatric disorders, such as schizophrenia. However, they do not treat or cure the underlying condition.
Examples of these medications include:
- haloperidol (Haldol)
- chlorpromazine (Thorazine)
- clozapine (Clozaril)
A person can only use these drugs under supervision from a doctor as they can have adverse effects.
Learn more about antipsychotic drugs for schizophrenia here.
The doctor will also treat any underlying conditions responsible for the psychosis. Where possible, family support can also help.
Acute and maintenance phases of schizophrenia
In schizophrenia, there are two phases of antipsychotic treatment:
Acute phase
During the acute phase of schizophrenia, a person may need to stay in a hospital to receive care.
Sometimes, a doctor will prescribe rapid tranquilization. They will give the person a fast-acting medication that relaxes them to ensure they do not harm themselves or others.
Maintenance phase
In the maintenance phase, a person does not stay in the hospital, but healthcare professionals will prescribe antipsychotic drugs to help prevent further episodes. Stopping the medication can lead to relapses.
Psychotherapy interventions, including cognitive behavioral therapy (CBT) and supportive counseling, can also help people with schizophrenia and other psychotic disorders.![]()
Learn more about the stages of schizophrenia and treatment here.
Apart from schizophrenia, other psychotic disorders can cause psychosis. According to the DSM-5, these include:
- Schizoaffective disorder: This disorder is similar to schizophrenia but includes periods of mood disturbances.
- Brief psychotic disorder: Symptoms occur in response to a stressful life event, last less than 1 month, and do not return.
- Delusional disorder: The person strongly believes in something irrational and often bizarre with no factual basis.
- Bipolar psychosis: Some people with bipolar disorder experience psychosis during a very high or very low mood.
- Severe depression: Also known as major depressive disorder with psychotic features.
- Postpartum (postnatal) psychosis: This type of psychosis can present after giving birth.
- Substance-induced psychosis: The misuse of alcohol, some recreational drugs, and certain prescription drugs can cause this.

Psychosis can also result from other disorders, such as:
- a brain tumor or cyst
- dementia, including Alzheimer’s disease
- neurological conditions, such as Parkinson’s disease and Huntington’s disease
- HIV and other infections that can affect the brain
- some types of epilepsy
- malaria
- syphilis
- stroke
- low blood sugar
- MS
- stress
Psychosis is a collection of symptoms that makes a person out of touch with reality. Hallucinations and delusions often accompany it.
A person may experience psychosis for various reasons, including underlying mental health conditions, trauma, and infections.
While having a psychotic episode is distressing, treatment can help manage the symptoms.
If a person has concerns about someone experiencing psychosis, they should take them to the emergency room, if possible, or call 911.
Psychosis - Hadassah Medical Moscow
Psychosis is a mental illness. Under it, a person cannot adequately behave, he does not perceive the world around him and does not react to it. At the initial stages, psychosis can be recognized by changes in behavior, atypical reactions appear in a person, and the emotional background is disturbed. He cannot control his feelings
Under it, a person cannot adequately behave, he does not perceive the world around him and does not react to it. At the initial stages, psychosis can be recognized by changes in behavior, atypical reactions appear in a person, and the emotional background is disturbed. He cannot control his feelings
and expresses emotions that do not correspond to situations. If you or your loved ones experience these symptoms, you should immediately consult a doctor. The appearance of psychosis may indicate the development of schizophrenia, delirium tremens, senile dementia and other serious diseases. nine0003
Full text
Symptoms of psychosis
Psychosis is a group of psychotic disorders. Their manifestations depend on the specific type of violation. However, all of them are characterized by a gradual increase in signs, a change in behavior. You can recognize the symptoms of psychosis by the following manifestations:
- Hallucinations - can be auditory, visual, gustatory, tactile, olfactory;
- Delusional ideas - there are obsessive thoughts and judgments that do not correspond to reality.
 A person may feel that he is being watched; nine0018
A person may feel that he is being watched; nine0018 - Movement disorders - periods of excitement are replaced by a sharp stupor;
- Mood disorders - apathy, melancholy, indifference to everything;
- Manic disorders - excessive aggressiveness, building unrealistic plans, a sharp addiction to alcohol, promiscuity;
- Emotional disorders - a person cannot express his feelings, he does not correlate his feelings with what is happening.
Make an appointment
Leave your number, our operator will answer all your questions in detail
By clicking on the button, you agree to the rules for the use and processing of personal data
Causes of psychosis
Psychosis occurs due to problems in the work of neurons. Due to the violation of bonds in the molecules, they do not receive nutrition, they experience a lack of oxygen. This leads to the fact that neurons cannot transmit nerve impulses - multiple disorders occur in the central nervous system. The type of psychosis that occurs depends on which part of the brain suffered from a hunger strike. The causes of this disease are of 3 types:
The type of psychosis that occurs depends on which part of the brain suffered from a hunger strike. The causes of this disease are of 3 types:
- Endogenous, associated with internal processes. These can be endocrine, neurological disorders, bronchial asthma, vitamin B deficiency, conditions accompanied by acute pain (ulcer, heart attack, sarcoidosis), electrolyte imbalance, systemic diseases, genetic predisposition, age;
- Exogenous, or external: stress, intoxication with alcohol, drugs, drugs, consequences of infectious processes, mental trauma; nine0018
- Organic, when changes in the brain become the cause of psychosis: tumors, injuries, hemorrhages.
Psychosis diagnostic methods
Psychologist diagnoses psychosis. At the first appointment, he conducts a pathopsychological examination: he studies human behavior, asks questions to determine the process and course of thinking. It is necessary to understand how the patient reacts to the world around him.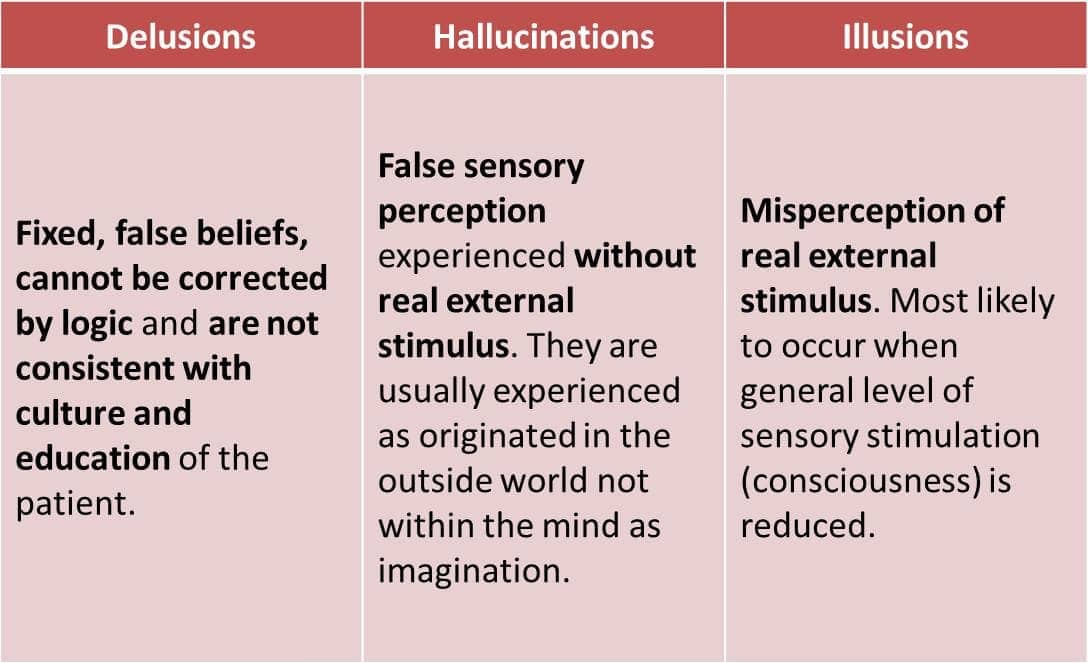 Relatives of a sick person are also involved in the diagnosis of psychosis - they will help to collect a complete clinical picture. Further diagnostics include
Relatives of a sick person are also involved in the diagnosis of psychosis - they will help to collect a complete clinical picture. Further diagnostics include
X-ray of the brain
MRI of the brain
Electroencephalogram
Blood test for hormones
Urinalysis for drugs and alcohol
Methods of treating psychosis
Psychosis is usually treated in a hospital setting. Such patients require hospitalization, as they cannot control their actions, they can harm themselves and others. The basis of therapy is taking medications, including:
- Antipsychotics - stop psychosis, relieve delirium and hallucinations;
- Atypical antipsychotics - restore neurochemical connections;
- Nootropics - restore brain function, improve mental activity;
- Normotimics - prevent the development of depressive and manic tendencies;
- Antidepressants - relieve symptoms of depression.
Treatment of psychosis necessarily includes psychotherapy. The patient will have to work with a psychologist for a long time in order to successfully return to society. In some forms of the disease, an electroconstrictive effect is shown, in which the current restores the metabolic processes of the nervous system in the brain. A good effect in the treatment gives physiotherapy: acupuncture, exercise therapy, reflexology. nine0003
The patient will have to work with a psychologist for a long time in order to successfully return to society. In some forms of the disease, an electroconstrictive effect is shown, in which the current restores the metabolic processes of the nervous system in the brain. A good effect in the treatment gives physiotherapy: acupuncture, exercise therapy, reflexology. nine0003
Prevention and treatment programs for psychosis at the Hadassah Clinic
Psychosis is a relapsing disease. With timely and comprehensive treatment, the prognosis will be favorable. However, the patient will have to undergo preventive examinations for several more years. If the patient follows all the recommendations of the doctor, the likelihood of exacerbations in the future will be minimal. To prevent the development of psychosis, you need to monitor your physical and mental health. For this:
- Eat right and balanced;
- Give up bad habits, especially alcohol and drug use;
- Avoid stressful situations;
- Avoid physical and psycho-emotional overload;
- Seek medical attention for all head injuries;
- See a therapist if needed;
- Observe the daily routine;
- Communicate more.
Psychosis is an insidious and dangerous problem. And it is very important to notice it in time and start treating it. If you see signs of approaching psychosis in yourself or loved ones, you should immediately consult a doctor. You can make an appointment at the Hadassah clinic in Moscow, where experienced specialists will determine the cause of psychosis and select an effective treatment regimen. nine0003
#DrunkOP
Drunk
Olga Pavlovna
Endocrinologist, dietitian, Ph.D.
Work experience: 11 years
Published: 25.12.2022
Department doctors
All doctors
Korobkina
Anna Sergeevna
Nephrologist, nutritionist
Work experience: 14 years
Cost of admission: from 6000 ₽
Make an appointment
Zavarzina
Natalya Pavlovna
Gastroenterologist-nutritionist
Work experience: 14 years
Appointment fee: from 6000 ₽
Make an appointment
Drunk
Olga Pavlovna
Endocrinologist, dietitian, Ph. D.
D.
Work experience: 11 years
Cost of admission: from 8000 ₽
Make an appointment
All doctors
Prices for nutrition services
02 By clicking on the button, you agree to the terms of use and processing of personal data
symptoms and treatment of acute psychosis, what to do with signs of psychosis?
How to deal with a psychotic person?
In order to avoid the dangerous consequences of psychosis for the patient and his environment, it is important to know how to behave with a person in a state of disorder. If the signs of psychosis are clearly visible, the first thing to do is to try to remain calm, demonstrate self-confidence and goodwill. In a conversation with a person in a state of psychosis, you cannot: nine0003
- argue;
- object;
- to sneer;
- scream;
- tease.
It is better to try to talk about the emotions and feelings of the person in this situation. You can ask about the help you can give him. If the patient is in an extreme degree of excitement, you need to hide all sharp and heavy objects and things that can injure him or others. It is also recommended to ensure that the patient does not get into the field of view: nine0003
You can ask about the help you can give him. If the patient is in an extreme degree of excitement, you need to hide all sharp and heavy objects and things that can injure him or others. It is also recommended to ensure that the patient does not get into the field of view: nine0003
- flammable substances;
- chemically active preparations;
- poisons.
If the patient in a state of psychosis is in the room, it is desirable to remove all unnecessary viewers. If possible, switch his attention, for example, ask a person for help, entrust him with hard physical work.
How dangerous is the patient to himself and others?
The disease can provoke irreversible consequences for the psyche. Progressing, acute psychosis constantly reduces the adequacy of the patient. A person rejects the help and advice of others, his world narrows, leading to self-isolation, negative habits arise. Loss of interest in life becomes dangerous for the patient himself. This is accompanied by: nine0003
This is accompanied by: nine0003
- sleep disorders;
- loss of appetite;
- increased fatigue;
- suicidal.
Extremely dangerous for the patient is the occurrence of auditory and visual hallucinations, obsessive and delusional states. A person is unable to distinguish fictional pseudo-reality from reality, he gradually deepens into the world of his fantasies, loses a sense of his own personality.
Patients in acute psychosis, defending themselves from imaginary threats, can commit acts that are dangerous for themselves and others. Often the disorder is accompanied by psychomotor agitation. The patient is chaotically rushing about, his movements are not purposeful. Fleeing from an imaginary danger, people in a state of psychosis can jump out of windows, balconies, and bridges. They can take the same actions, protecting loved ones and relatives. nine0003
Should I call an ambulance if I have symptoms of psychosis?
If a person is in a state of psychosis, others need to understand one way or another that they are not able to cope with the problem themselves. Urgent psychiatric help should be sought. If the symptoms of psychosis are relatively mild, the person makes contact, and the situation is under control, then you can not resort to an urgent call to the NPP team. But this does not mean that you do not need to contact a psychiatrist. It may be possible to convince the patient to consult a specialist. nine0003
Urgent psychiatric help should be sought. If the symptoms of psychosis are relatively mild, the person makes contact, and the situation is under control, then you can not resort to an urgent call to the NPP team. But this does not mean that you do not need to contact a psychiatrist. It may be possible to convince the patient to consult a specialist. nine0003
The mental health emergency team should be called when:
- affective disorders are increasing;
- there is a risk of self-harm;
- the patient commits suicidal acts;
- there is a threat to the lives of others.
The medics who arrived on the scene
- assess the complexity of the situation;
- immobilize the patient if necessary; nine0018
- will treat the condition;
- will decide on hospitalization.
Treatment in a psycho-neurological hospital may be agreed or compulsory. Consent to hospitalization can be given by the patient himself, and his relatives. Compulsory placement is determined by a psychiatrist in accordance with existing legislation.
Compulsory placement is determined by a psychiatrist in accordance with existing legislation.
Prophylaxis
Unfortunately, psychosis is a disorder characterized by relapses. Therefore, an important component of a favorable prognosis of the disease is prevention. The treatment of psychosis is long and laborious. And in the intervals of remission, you need to adhere to certain rules and prescriptions of doctors. nine0003
The main preventive methods include:
- maintenance therapy;
- compliance with the daily routine;
- avoidance of emotional shocks;
- getting rid of bad habits;
- constructive change of social circle;
- walks, sports, yoga.
Physiotherapy procedures are considered a good preventive method, including: nine0003
- electrosleep;
- acupuncture;
- massage;
- Su-Jok therapy;
- physiotherapy exercises.
Many of them help reduce emotional overstrain, normalize sleep, improve metabolism, and increase vitality.