Vyvanse muscle pain
Side effects of Lisdexamfetamine dimesylate (Vyvanse)
Written by: Bronwen Watson
- Lisdexamfetamine (Vyvanse®)
- Precautions and considerations for taking Lisdexamfetamine dimesylate (Vyvanse)
- How to use Lisdexamfetamine dimesylate (Vyvanse)
- Side effects of Lisdexamfetamine dimesylate (Vyvanse)
- Lisdexamfetamine dimesylate (Vyvanse) FAQs
Lisdexamfetamine dimesylate (Vyvanse) can cause a number of adverse reactions or unwanted side effects. These may vary from person to person. Many potential problems which arise will need medical attention. Many may not. It is important to consult your doctor as soon as possible if you experience any side effects, especially if they persist or worsen.
Many side effects are merely your body’s way of adjusting to the medication and will stabilise over time. Your doctor will be able to work with you and your treatment dosages to reduce and alleviate side effects which may become bothersome, or prevent them altogether. Your doctor will generally prescribe this medication if its benefits outweigh any risks or side effects.
Common Lisdexamfetamine dimesylate (Vyvanse) side effects
- Headaches
- Nausea
- Decreased appetite
- Vomiting
- Upper abdominal pain (stomach)
- Weight loss
Less common side effects include:
- Uncontrolled or repeated vocal outbursts or body movements (tics, twitching or twisting)
- Peeling, blistering or loosening of the skin
- Cough
- Chills
- Diarrhoea
- Discouragements
- Dizziness or feeling faint
- Difficulties with breathing
- Difficulties with swallowing
- Increased heartbeat or pulse rate (fast, irregular, pounding or racing sensation)
- Depressive symptoms (feeling sad or empty, crying, irritability, agitation, aggression, mood swings, loss of interest or pleasure)
- Hives, welts, skin rashes, red skin lesions, inflammation of the skin or itching and swelling on the face, eyelids, tongue, throat, hands, legs, feet or sex organs
- Joint or muscle pain
- Lack of appetite
- Sore throat
- Sores, ulcers or white spots in the mouth or on the lips
- Swelling in the feet, ankles or lower legs
- Tightness in the chest
- Concentration problems
- Sleeping problems
- Fever
- Dysphoria (feeling of unease) or euphoria (elevated mood)
- Paranoia
- Hallucinations
- Blood flow problems (in the fingers and toes)
- Unusual wounds (on the fingers and toes)
- Frequent or prolonged erections (in males)
It is possible for your blood pressure to increase while on Vyvanse. Your doctor may check this regularly and help to manage any fluctuations.
Your doctor may check this regularly and help to manage any fluctuations.
It is imperative to seek immediate medical assistance if you experience serious side effects such as shortness of breath, sudden vision changes, fainting, seizures, weakness on one side of the body, chest / jaw / left arm pain, serious confusion, slurred speech or an allergic reaction.
Signs of Lisdexamfetamine dimesylate (Vyvanse) overdose
Signs of a possible overdose, which will require medical attention as soon as possible include:
- Blurred vision
- Abdominal pain or cramps
- Confusion
- Changes in consciousness or loss of consciousness
- Dizziness / light-headedness or feeling faint
- Dark-coloured urine
- Rapid breathing
- Muscle cramps and spasms
- Muscle pain or stiffness
- Overactive reflexes
- Nervousness
- Panic and anxiety
- Pounding sensation in the ears
- Seizures
- Hallucinations
- Profuse sweating
- Violent outbursts
- Shakiness or trembling in the legs, arms, hands or feet
PREVIOUS How to use Lisdexamfetamine dimesylate (Vyvanse)
NEXT Lisdexamfetamine dimesylate (Vyvanse) FAQs
Back to top
- Lisdexamfetamine (Vyvanse®)
- Lisdexamfetamine dimesylate
- Headache
- Nausea
- Vomiting
- Decreased appetite
- Abdominal pain
- Weight loss
If you have unexplained muscle pain and are taking Xyrem and stimulants, please read this.
 : Narcolepsy
: NarcolepsyHello, fellow narcs. I want to inform you of a serious medical condition I developed while being treated for narcolepsy It’s a long story so there’s a TLDR at the bottom; please read it if you or anyone you know is taking medication for ADHD.
It’s called rhabdomyolysis, here’s the link:
https://medlineplus.gov/ency/article/000473.htm
It’s something to be aware of, like serotonin syndrome with antidepressants. Not something to be scared of, as it’s only dangerous if it’s not addressed right away.
here is the link to report adverse side effects to the FDA: https://www.accessdata.fda.gov/scripts/medwatch/index.cfm?action=reporting.home
edited for clarity and less dramatic wording
SO. It’s 2017. I was 19, excited to start Xyrem. I’d taken Vyvanse for several years (for ADHD) with no issues.
August 27, 2017, I got my first shipment and started my first week. It was amazing, I could probably write a novel on how different my brain felt when rested. I felt so normal and it made me nearly euphoric. Everything felt possible and I felt capable again.
I felt so normal and it made me nearly euphoric. Everything felt possible and I felt capable again.
7 days in, it started as a strange tingly pain in my legs one evening while standing in place. An hour later, my knees felt like something had burst inside; there was a sensation like icy water and they were red and swollen. The pain came in several forms: muscle spasms up and down my legs; a crushing, rolling sensation across my kneecaps; severe cramps that inhibited me from standing or walking; and painful muscle stiffness. If I held onto my knee and moved it left to right I felt something grinding that also could be felt by others. I called my mom and met up with her for ER Trip #1. At this point, I wasn’t scared of what was wrong (I consulted the internet and figured I tore or dislocated something), I was scared of how bad it was going to hurt when they fixed it and if I could maybe be put under while they moved whatever back in place.
They did an X-ray and bloodwork. The doctor came in, told me everything was fine, and wrote me a script for pain meds and crutches.
The doctor came in, told me everything was fine, and wrote me a script for pain meds and crutches.
I was debilitated over the next few weeks and hospitalized many times as the condition worsened. It was a nightmare. Nobody could give me answers despite running every test they could think of; many doctors didn’t believe it was as excruciating as I said it was. It genuinely felt like someone was crushing my kneecaps, going back and forth over them with a steamroller, and stretching and snapping my muscles and tendons, especially my IT band. One hospital doctor told me it was psychosomatic and referred me to a therapist. (I am female and was 19-20 at the time.)
I stopped taking Xyrem because that seemed like the most logical cause. Nothing improved. I discontinued Vyvanse as well and nothing improved.
The pain spread to my upper back, shoulders, and elbows. I saw a physical therapist who noted how swollen my knees were and how atrophied my muscles had become (which makes no sense as I’ve always been fit and it had been less than a month since The Condition started at this point. )
)
After a month or so, I started taking my meds again since nothing got better and I couldn’t find anything online that sounded even remotely close to what I was experiencing. The pain was constant torture and never had any sort of rhythm or predictability about it.
I noticed one day I wasn’t urinating much and that my urine was dark. I went to the ER and mentioned other symptoms I had assumed were stress: tachycardia (resting hr over 160), nausea, vomiting; my legs were puffy and ached.
They ran tests, told me I had anemia, (no prior history) and that I was just dehydrated. The IV caused increased muscle pain and I asked the doctor to check my kidney function. He told me I was fine and discharged me; I went home.
I thought I was going to die that night, it was that deep sort of primal instinct/feeling that something was wrong. I was too afraid to take any medication because I was convinced it HAD to be meds, despite not having evidence.
That was December 2017.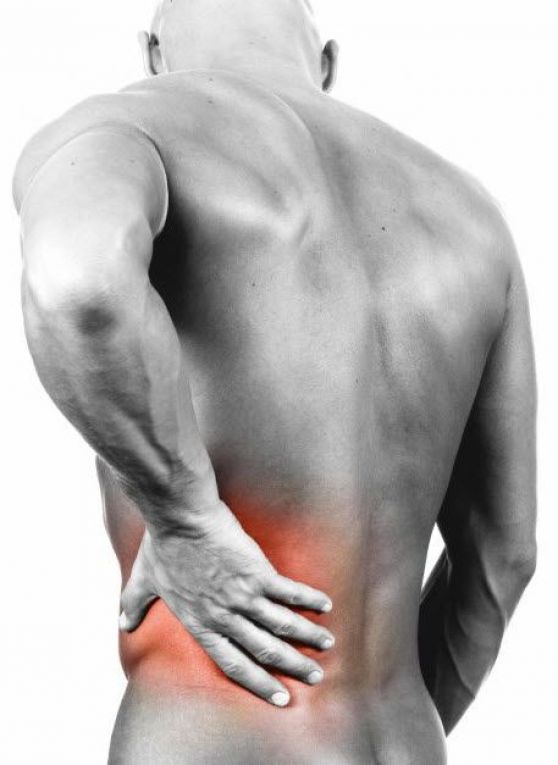 After two months of no meds, the mysterious muscle condition seemed to have gotten a bit better. I could walk across my apartment without braces, crutches, the broken swivel chair, or having to sit down. I wasn’t in constant pain and the pain I did experience was NOTHING compared to how it had been at the peak of it’s severity. Like, it was still bad enough I had to chew on ice and go to my mental happy place, but I didn’t fantasize about amputating my legs anymore.
After two months of no meds, the mysterious muscle condition seemed to have gotten a bit better. I could walk across my apartment without braces, crutches, the broken swivel chair, or having to sit down. I wasn’t in constant pain and the pain I did experience was NOTHING compared to how it had been at the peak of it’s severity. Like, it was still bad enough I had to chew on ice and go to my mental happy place, but I didn’t fantasize about amputating my legs anymore.
I began Xyrem again. No problems, the pain stayed consistently manageable and I decided Xyrem was safe to keep taking. (It was, thank god.) I still didn’t know what happened to my body. (It still hasn’t gone back to normal, I still experience pain and can’t do as much as I used to. I’m only 22.)
So a month ago, my new prescriber wrote me a script for 10 mg Vyvanse (for narcolepsy and ADHD, I was planning on going back to school, finally). I was a little nervous but figured, okay, it’s literally a pediatric dose.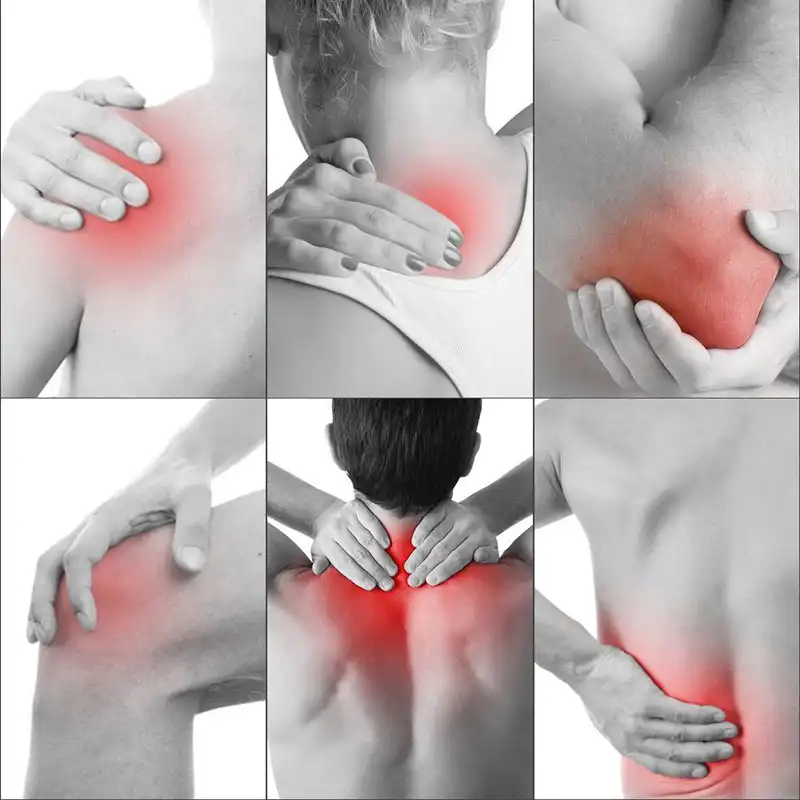 The Condition is getting better and was probably some one-time freak medical mystery.
The Condition is getting better and was probably some one-time freak medical mystery.
Within a week of taking Vyvanse, I felt it beginning exactly as it had the first time, tingly legs, sore knees, cold sensation. I had a panic attack, felt absolutely sick with terror and grief (I depend on stimulants quite a lot and can’t work or go to school without them) and went back to fervently researching via the internet.
And I found it. On this website, the FDA website, and a few other ones:
www.aboutlawsuits.com/adhd-drugs-rhabdomyolysis-warning-82002/
It’s called rhabdomyolysis, it’s extremely rare, and was only added to the warning label in 2015, which explains why doctors didn’t think of it during my battery of tests and examinations.
It applies to ALL ADHD MEDICATIONS, this includes Strattera. It is a life-threatening condition and if you begin experiencing symptoms, contact your doctor IMMEDIATELY.
Here is what is published on the site:
“Rhabdomyolysis is a side effect associated with several different types of medications, which causes muscle fibers to begin to break down, releasing a protein called myoglobin, which can damage the kidneys as they attempt to filter it out of the bloodstream.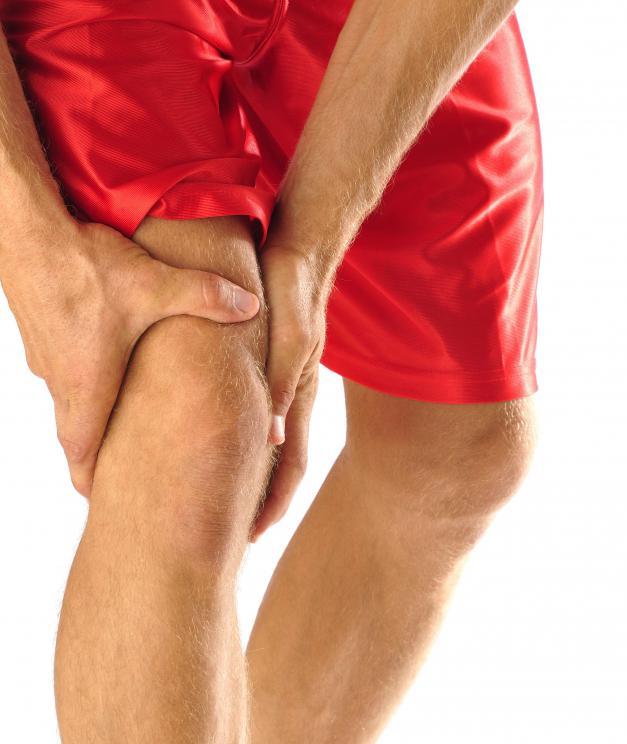
The illness is usually reported in patients over 65 years of age or those who have renal impairment or uncontrolled hypothyroidism, however these drugs are prescribed heavily to children and young adults. Over time, rhabdomyolysis can lead to kidney damage and even kidney failure. Some may require dialysis or a kidney transplant.
The list of drugs that must now carry the rhabdomyolysis warning includes Adderall, Adderall XR, Concerta, Daytana, Desoxyn, Dexedrine, Focalin, Focalin XR, metadate CD, Methylin, Quillivant XR, Ritalin, Ritalin LA, Ritalin SR, Strattera and Vyvanse.”
I’m writing this because back in 2017, I came HERE looking for answers. I messaged with a few other people who had the same exact symptoms. I don’t have my old account anymore, so I can’t check up on them, but I wanted to check up on all of you and bring more attention to this.
Sorry for the long post; take good care of yourselves, stay vigilant and knowledge about your health and medication.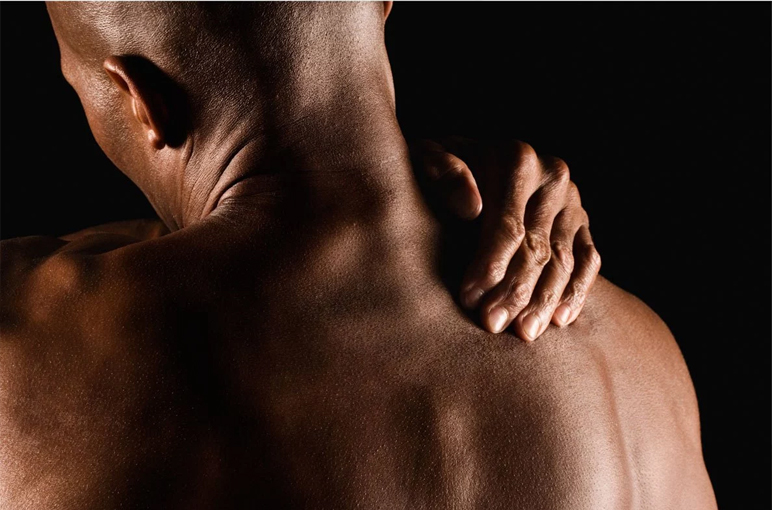
love u
TLDR:For some reason, after starting a new med, the stimulant I’d taken for years caused a life-threatening condition called rhabdomyolysis. Basically, it dissolves your skeletal muscles resulting in a protein being released into your bloodstream. This can cause kidney damage or failure and long term muscle pain/weakness.
Stimulants can cause non-serious muscle cramps, especially if you’re dehydrated, and rhabdomyolysis is extremely rare.
You can ask to get tested for it if you think you have symptoms.
https://medlineplus.gov/ency/article/000473.htm
Muscle pain - treatment, symptoms, causes, diagnosis
Muscle pain (myalgia) is a pulling, sometimes painful or spastic muscle pain : the term myalgia consists of the Greek words Myos muscle and Algos pain. Muscle pains can be localized both in a certain area of the body, and radiate or be diffuse. In principle, pain can occur in any of the more than 600 muscles in the body.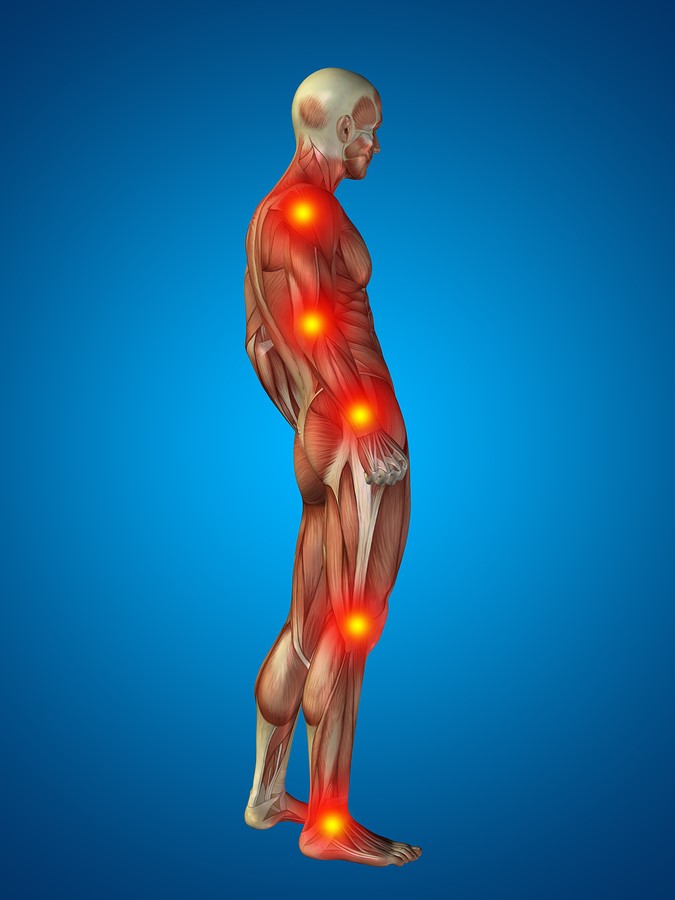
Muscle pain (myalgia) occurs most often in the area of the shoulders and neck in the back. Approximately 75 percent of adults in Europe suffer from back pain, one way or another having a muscular origin. Muscles are divided into skeletal and smooth. Skeletal muscles include muscles that provide human movement and connect bone structures. Quite often, the pain is caused not by skeletal muscle, but by smooth muscles (for example, problems in the smooth muscle of the heart can be a source of pain in the chest). Smooth muscles are located in the walls of the hollow organs of the body, such as the stomach, bladder, and blood vessels, and play a large role in the normal function of organs. The cardiac muscle, which forms the heart, is responsible for pumping blood throughout the body.
Muscles respond to commands from the brain and nervous system or other stimuli, for example reflexively when performing a neurological examination with a hammer. Muscles contract when stimulated and relax after contraction.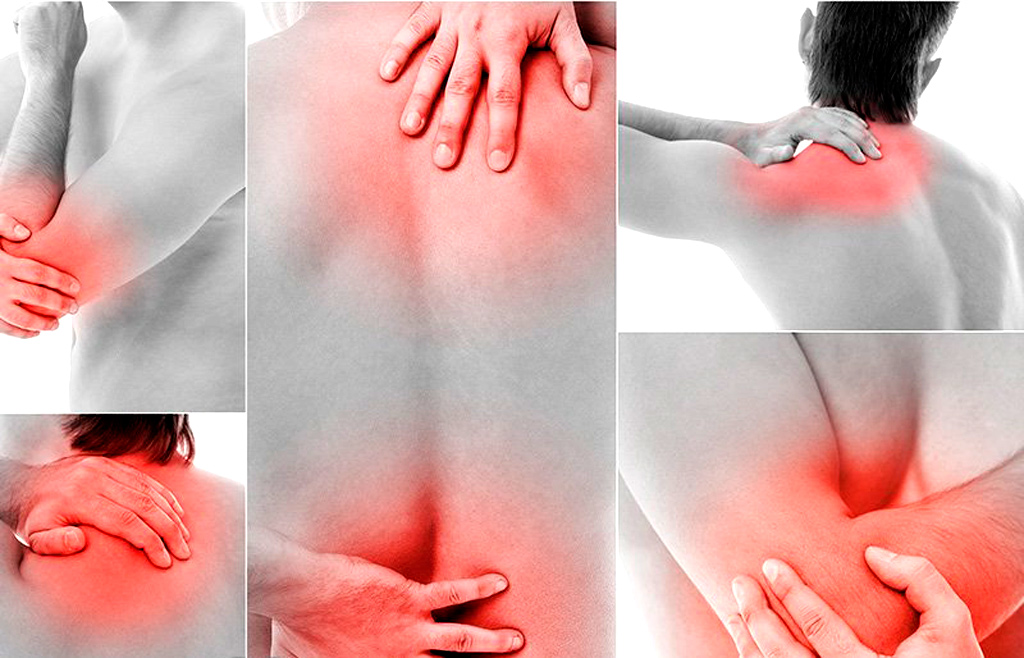 Muscles can become a source of pain due to various diseases and conditions, including infections, injuries, autoimmune diseases, neurological and muscle diseases, malignant tumors (cancer), and even after taking certain medications. Muscle pain can also involve ligaments, tendons, and fascia, which are soft tissues that connect muscles, bones, and organs.
Muscles can become a source of pain due to various diseases and conditions, including infections, injuries, autoimmune diseases, neurological and muscle diseases, malignant tumors (cancer), and even after taking certain medications. Muscle pain can also involve ligaments, tendons, and fascia, which are soft tissues that connect muscles, bones, and organs.
The person may feel muscle pain in certain muscles of the body, such as the muscles of the back or muscles of the legs, or the pain may be diffuse in all muscles, such as with the flu. In a patient during an angina attack, retrosternal pain is due to problems in the myocardium. Menstrual pain is pain caused by the smooth muscle of the uterus. Temporary skeletal muscle pain often occurs due to muscle tension due to awkward movement or excessive exercise. This type of pain often affects one or more muscles and is usually sharp and intense. Abstinence from the activity that caused the pain, rest, topical cold, and anti-inflammatory drugs usually help to reduce pain associated with overuse of the muscles.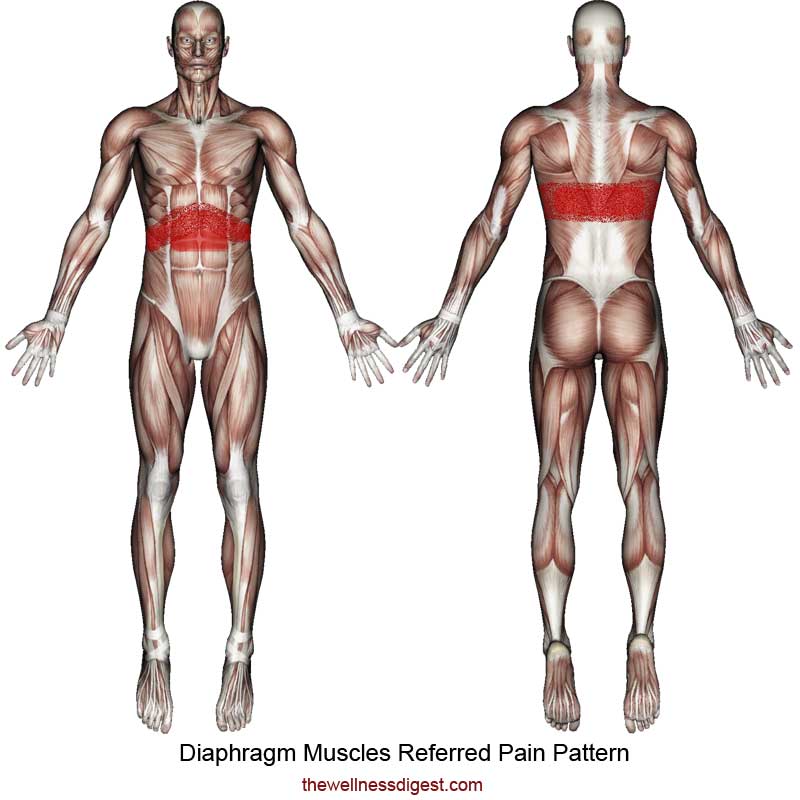 Muscle pain can be caused by serious conditions such as fibromyalgia, infections, or dermatomyositis.
Muscle pain can be caused by serious conditions such as fibromyalgia, infections, or dermatomyositis.
Muscle pain may be a symptom of a serious condition such as a muscle tear or infection. Therefore, you should immediately seek medical help if muscle pain is persistent or worsens.
Not only muscle pain , but any pain is an important signal for the body. Various stimuli can cause pain, such as heat or cold, pressure or shock, as well as electrical stimulation and chemicals. So-called pain receptors are responsible for transmitting these stimulating sensations. Pain receptors are free nerve endings that are located both on the surface in the skin and in depth - in muscles, tendons and ligaments, as well as in various organs. When pain receptors are stimulated, the signal from them goes to the central nervous system, where the signal is analyzed, and a protective response occurs, which is aimed at preventing further damage.
Symptoms
Muscle pain may occur along with other symptoms, which vary depending on the underlying disease.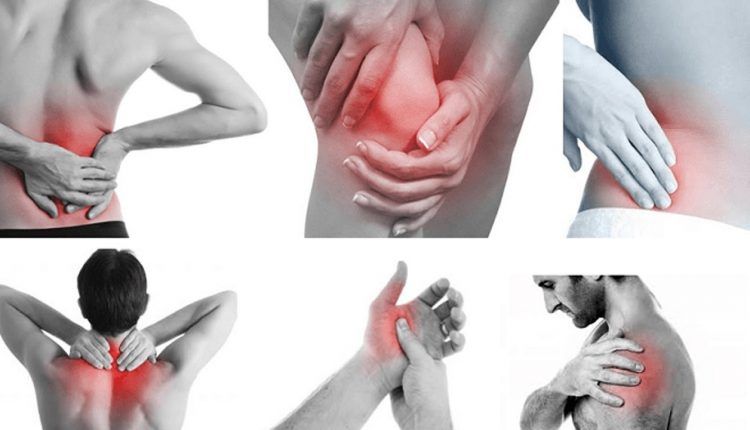 For example, muscle pain that is caused by an injury may be accompanied by bruising and swelling around the injury. Additional symptoms that may accompany muscle pain include:
For example, muscle pain that is caused by an injury may be accompanied by bruising and swelling around the injury. Additional symptoms that may accompany muscle pain include:
- Depression
- Diarrhea
- Acute respiratory symptoms (fever, chills, sore throat, fatigue, headache, cough)
- Attention disorder
- Loss of appetite
- Muscle cramps
- Numbness, tingling or burning (so-called paresthesias)
- Trouble walking
- Sleep disorders
- Swelling at the site of injury
- Abrupt weight loss
- Vomiting
Serious symptoms that may indicate a life-threatening condition
In some cases, muscle pain may occur in association with other symptoms that may indicate a serious or life-threatening condition, such as a heart attack (heart attack) or meningitis. Seek immediate medical attention if you experience any of these symptoms:
- Changes in consciousness or attention, such as loss of consciousness or severe impairment of memory
- Changes in mental status, such as impaired perception of the environment
- Chest pain radiating to the arm, shoulder, neck or jaw
- Difficulty breathing, shortness of breath
- Inability to move in any part of the body
- Violation (loss) of vision
- Lack of urine
- Progressive weakness and numbness
- Seizure
- Stiff neck with high temperature
Cause of pain
Skeletal muscle pain is most often caused by direct trauma or injury resulting from muscle strain or muscle strain. Muscle tension occurs when several muscle fibers are damaged, while when a muscle is torn, a large number of muscle fibers are torn. A tear (tear) in the tendon can also lead to muscle pain. Muscles and tendons have the ability to regenerate, but with a severe rupture of a muscle or tendon, prompt restoration of the integrity of the damaged structures is required. Muscle pain can be caused by cramps that occur due to overload or abnormal nerve impulses that lead to excessive muscle contraction. In some cases, muscle pain can be a symptom of a serious or life-threatening condition such as a heart attack, meningitis, or cancer.
Muscle tension occurs when several muscle fibers are damaged, while when a muscle is torn, a large number of muscle fibers are torn. A tear (tear) in the tendon can also lead to muscle pain. Muscles and tendons have the ability to regenerate, but with a severe rupture of a muscle or tendon, prompt restoration of the integrity of the damaged structures is required. Muscle pain can be caused by cramps that occur due to overload or abnormal nerve impulses that lead to excessive muscle contraction. In some cases, muscle pain can be a symptom of a serious or life-threatening condition such as a heart attack, meningitis, or cancer.
Traumatic causes of muscle pain
Muscle pain can be associated with any injury, including:
- Blunt force
- Muscle strain or tear
- Excessive or repetitive movements
- Nerve compression (due to disc herniation, spinal stenosis)
Neuromuscular diseases and conditions
- Amyotrophic lateral sclerosis (ALS, Charcot's disease) is a severe neuromuscular disease that causes muscle weakness and disability
- Injury to the brain or spinal cord
- Dermatomyositis (a condition characterized by muscle inflammation and skin rash)
- Lyme disease (inflammatory bacterial disease transmitted by ticks)
- Multiple sclerosis (a disease that affects the brain and spinal cord and causes weakness, incoordination, balance and other problems)
- Muscle breakdown (rhabdomyolysis)
- Muscle infections such as abscess
- Parkinson's disease (disease of the brain leading to impaired movement and coordination)
- Polymyalgia rheumatica (disease characterized by muscle pain and stiffness)
- Polymyositis (inflammation and muscle weakness)
- Stroke
Other possible causes of muscle pain
Many other diseases and conditions can cause muscle pain, including:
- Cancer
- Depression
- Fibromyalgia
- Angina pectoris or myocardial infarction
- Hypothyroidism
- Influenza or other respiratory diseases
- Renal failure
- Electrolyte disorders (impaired levels of potassium or calcium in the blood).

- Pregnancy
- Systemic lupus erythematosus
- Vitamin B12 or vitamin D deficiency
Medicines and substances that can cause muscle pain, include:
- ACE inhibitors (used to lower blood pressure)
- Cocaine
- Statins (cholesterol-lowering drugs)
Questions to help find the cause of muscle pain include:
- Are there other symptoms such as a sore throat or fever?
- Do you feel pain in one specific area or throughout your body?
- How long does this condition last?
- In what parts of the body are the pains localized?
- What reduces pain or increases pain?
- What medications are currently taken or have been taken recently
Potential complications of muscle pain
Complications associated with muscle pain depend on the underlying disease or condition. For example, muscle pain associated with fibromyalgia or degenerative disease can lead to reduced motor activity and related complications.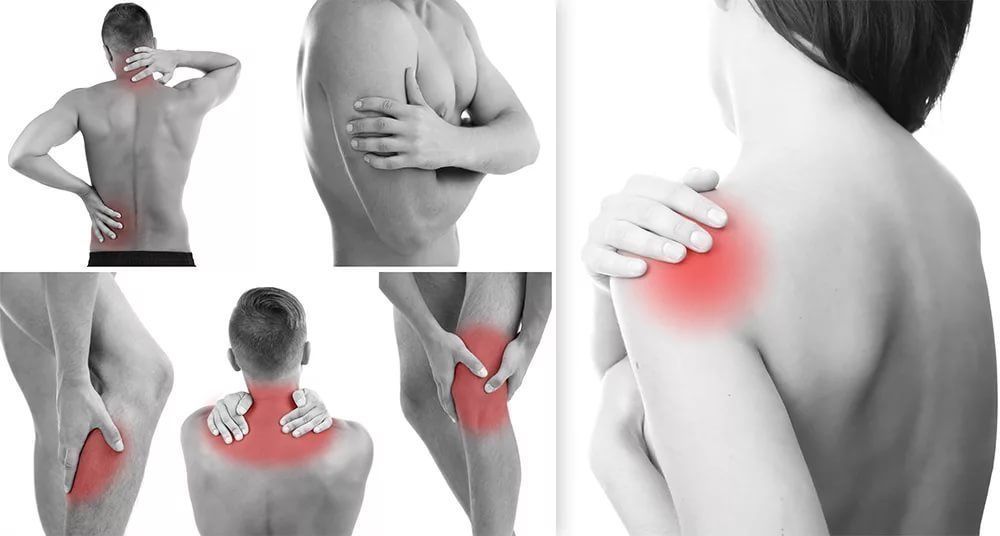 Many skeletal muscle pains, however, respond well to treatment. However, if muscle pain prolonged and associated with a systemic disease, this may lead to the following complications, including:
Many skeletal muscle pains, however, respond well to treatment. However, if muscle pain prolonged and associated with a systemic disease, this may lead to the following complications, including:
- Chronic pain
- Immobility and associated complications (such as bedsores and thrombosis)
- Persistent pain refractory to treatment
- Muscle atrophy
- Muscle contracture
- Permanent muscle or nerve injury (most commonly due to nerve compression), including paralysis.
- Decreased quality of life
Diagnosis
Diagnosis of muscle pain (myalgia) is primarily based on the history of the disease and symptoms. Most muscle pain is associated with muscle tension (eg, due to poor posture or a sedentary lifestyle) or injury (eg, sprains, bruises, or muscle soreness from sports). Instrumental research methods, such as ultrasound or X-ray, CT, MRI, help confirm or differentiate cause of muscle pain .
Medical history (anamnesis).
The physician will be interested in the type of pain, the location of the pain, and the intensity of the muscle pain. This information can be key to finding out what causes leg pain. Information about the presence of muscle injuries, the presence of bruises, factors that lead to an increase or decrease in muscle pain, or the pain is persistent, for example, with a herniated disc, the time of occurrence of pain (day or night), is very important.
Inspection. A doctor's examination can look for areas of pain, changes in skin color, range of motion in muscles or joints, muscle strength, local tenderness in the tendon area, or identification of trigger points (for example, fibromyalgia). In addition, reflex activity, sensitivity and other neurological tests are important, which can detect the presence of neurological disorders. The time of occurrence of pain in the muscles is also relevant, as, for example, with osteoporosis or Bechterew's disease. Alcohol or drug abuse can be a possible cause of muscle pain and information about this is important in understanding the causes of muscle pain. Some medications can also have the side effect of muscle pain.
Alcohol or drug abuse can be a possible cause of muscle pain and information about this is important in understanding the causes of muscle pain. Some medications can also have the side effect of muscle pain.
Laboratory research methods.
Blood tests can determine the presence of an inflammatory process or infections, autoimmune processes; biochemical analyzes allow to determine violations of the functions of internal organs (for example, the liver or kidneys).
Ultrasound examination (ultrasound). This research method allows you to visualize the presence of inflammation of the muscles (myositis), ruptures of muscles, tendons.
Investigations such as CT or MRI are needed to visualize problems in deep muscles where ultrasonography is not helpful or where neurological conditions or traumatic injuries need to be visualized. Electrophysiological research methods (EMG or ENMG) allow you to determine the presence of inflammatory or degenerative muscle diseases or impaired conduction along the nerves due to compression of the nerve roots or other neurological diseases.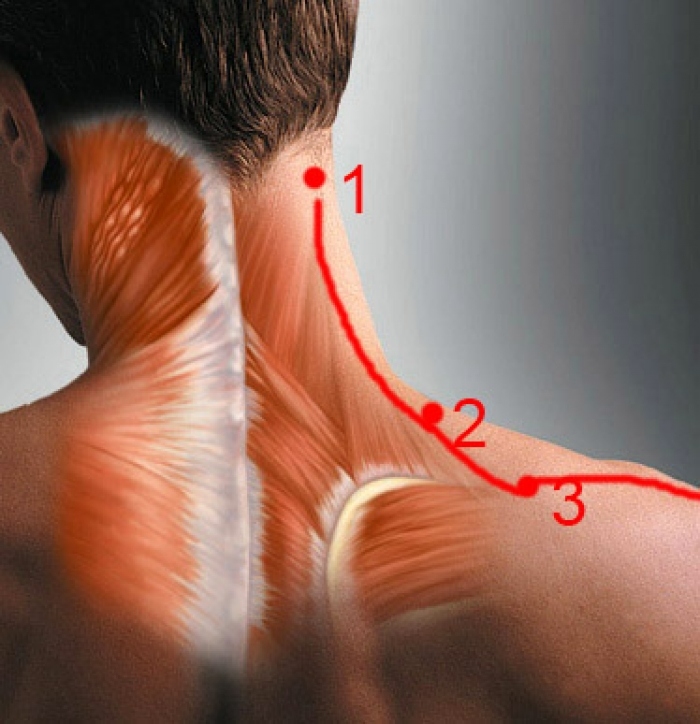
Muscle biopsy is usually used as the last step in the diagnosis of muscle diseases, and only if there are clear signs of such diseases.
Treatment
Treatment of muscle pain depends on the cause of the symptom. Therefore, the most important factor in determining treatment tactics is an accurate diagnosis. For example, if muscle pain is caused by taking certain drugs, then in such cases it may be enough to stop taking these drugs or replace them with other medicines. Medical treatment for muscle pain can include both NSAIDs or analgesics, and even opiates.
Acute muscle pain
Acute muscle pain after injury requires rest and unloading, in some cases immobilization. In addition, a good effect in such cases is given by local cooling with ice wrapped in a towel, which reduces swelling, inflammation, and pain. In addition, it is necessary to stop the load that led to muscle pain. It takes a lot of time to treat muscle injuries, since early restoration of normal loads can lead to chronic pain and excessive scarring of muscle tissue, and in severe cases, to the development of ossifying myositis.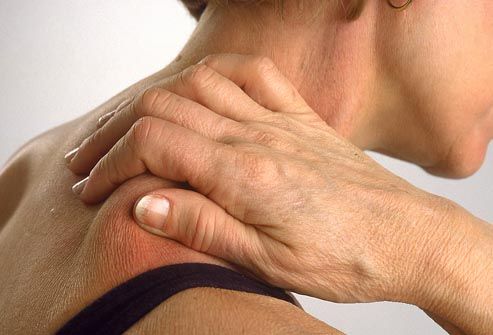
Chronic muscle pain
Treatment of chronic pain may include thermal treatments as well as other therapies such as:
- Acupuncture and acupressure
- Electrotherapy (therapy through electricity)
- Electromyostimulation
- Physiotherapy
- LFK
- Manual therapy
Systematic exercises (exercise therapy) are especially relevant when chronic pain is caused by degenerative diseases of the spine, such as osteochondrosis, spondylosis, disc herniation.
Surgical treatments are used for severe traumatic muscle injuries or nerve root compression.
Prevention of muscle pain consists in the following rules: maintaining a healthy lifestyle, sufficient physical activity, balanced nutrition, proper ergonomics of the workplace, avoiding alcohol abuse, smoking.
Causes of muscle pain - how to get rid of muscle pain
- Home
- /
- Publications
- /
- Muscle pain
Muscle pain (myalgia) is pain in the muscles that can occur not only in a tense state, but also at rest. Pain sensations of a pulling or spastic nature can be localized in one part of the body or several at once.
Pain sensations of a pulling or spastic nature can be localized in one part of the body or several at once.
Causes of muscle cramps after exercise
Discomfort due to pain in the shoulder, lower back, neck, or other parts of the body is a common occurrence when playing sports. Myalgia is often experienced by beginners who try to do a lot of exercises, barely starting classes. Experienced athletes are also susceptible to it, dramatically changing their training plan.
The causes of muscle pain in such cases lie in small ruptures of muscle fibers. Due to microscopic wounds, constantly increasing pain occurs in them. Intensive recovery begins in the body: protein is intensively synthesized and hormones are released.
Discomfort disappears after 2-3 weeks, when the athlete enters the rhythm and competently draws up a training program. But if the pain in the back and shoulder or in another area is sharp and throbbing, it is possible that the cause is an injury, so the athlete should consult a traumatologist.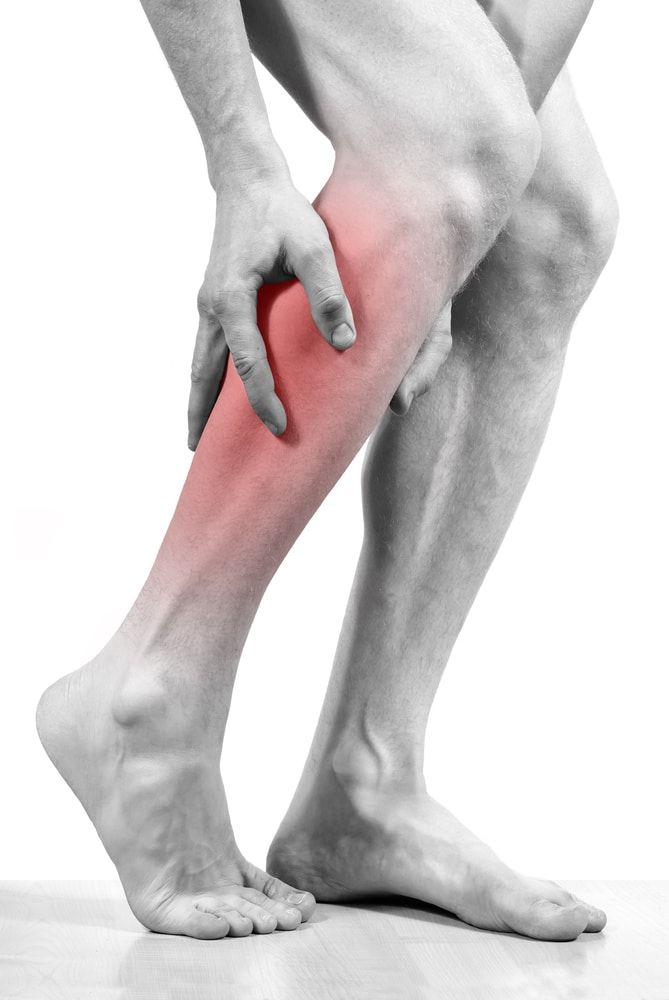
Types of myalgia
- Fibromyalgia. Arise in ligaments and tendons, appear in the neck, neck, lower back. Often manifested in women due to stress and men due to overload at work or in the gym.
- Myositis - inflammation of muscle tissue. It occurs due to injuries, heavy physical exertion, complications after the flu. Such muscle pain is localized in the legs, arms, torso, increases with movement and is aching in nature. Most often, it is required to treat a leg or arm in a hospital setting.
- Polymyositis. Serious illness. A person can have a severe pain in the neck, shoulders, then the pain passes to the pelvic girdle and legs. Sometimes leads to muscle dystrophy.
Muscle pain during pregnancy
During the period of expectation of a child, most women experience pain in the muscles. Moreover, if before pregnancy a woman was not engaged in maintaining a physical form, then they manifest themselves more strongly.
During pregnancy, muscles can hurt in different areas:
- back - due to the load of the growing body;
- abdomen due to painful muscle strains;
- lower back - due to increased load from increasing weight and natural displacement of internal organs;
- legs - the causes of pain in the legs are the same, pain is accompanied by cramps in the calves that develop at the beginning of sleep, at night or in the morning;
- chest - under the influence of changes in hormonal balance, increased blood circulation;
- vagina - under the influence of changes in venous hemodynamics, increased vascular load, decreased elasticity of muscle tissue.

Child's muscles hurt
Myalgia often manifests itself in children due to a lack of vitamins, calcium, magnesium in the body. It may be due to the fact that the child's bone skeleton grows, and the muscle tissues do not keep up with it and stretch.
If the child not only has pain in the legs or arms, but also the temperature has risen, swelling has appeared, it is urgent to consult a doctor to find out the cause of the disease. The doctor will prescribe treatment for muscle pain.
Treatment
Treatment for muscle pain depends on the cause of the pain, so an accurate diagnosis is important.
Treatment of muscle pain in the back and other areas is carried out using the following methods:
- drug therapy;
- physiotherapy exercises;
- physiotherapy procedures;
- manual therapy.
To avoid such problems, you should follow the rules of prevention: a healthy lifestyle, a balanced diet, moderate physical activity, an ergonomic workplace, avoiding smoking and alcohol abuse.
Publication date: 09/21/2017 | Modified date: 02/25/2022
| Article rating: | (Votes: 74, Rating: 3.36) |
Return to the list
From October 26, 2020, our center does not provide home care for adults...
Dizziness (vertigo) is a condition in which a person feels as if his body or objects ...
Return to the list
Pay attention
Requires a nephrologist
Requires a pulmonologist
adults
ASSISTICE DEMOTALS
Requires a dentist children
Relatives more ...
03.1 Many thanks to the cardiologist Oleg Vyacheslavovich Dymov!!! Helped me with high blood pressure and high cholesterol. Attentive, responsive and kind. It is a pleasure to communicate with him, he always listens and answers all questions. Very happy that I got to him.
24.10.2022 Victoria
I was sent from the antenatal clinic for a consultation and additional services.