Trauma for kids
About Child Trauma | The National Child Traumatic Stress Network
What Is a Traumatic Event?
A traumatic event is a frightening, dangerous, or violent event that poses a threat to a child’s life or bodily integrity. Witnessing a traumatic event that threatens life or physical security of a loved one can also be traumatic. This is particularly important for young children as their sense of safety depends on the perceived safety of their attachment figures.
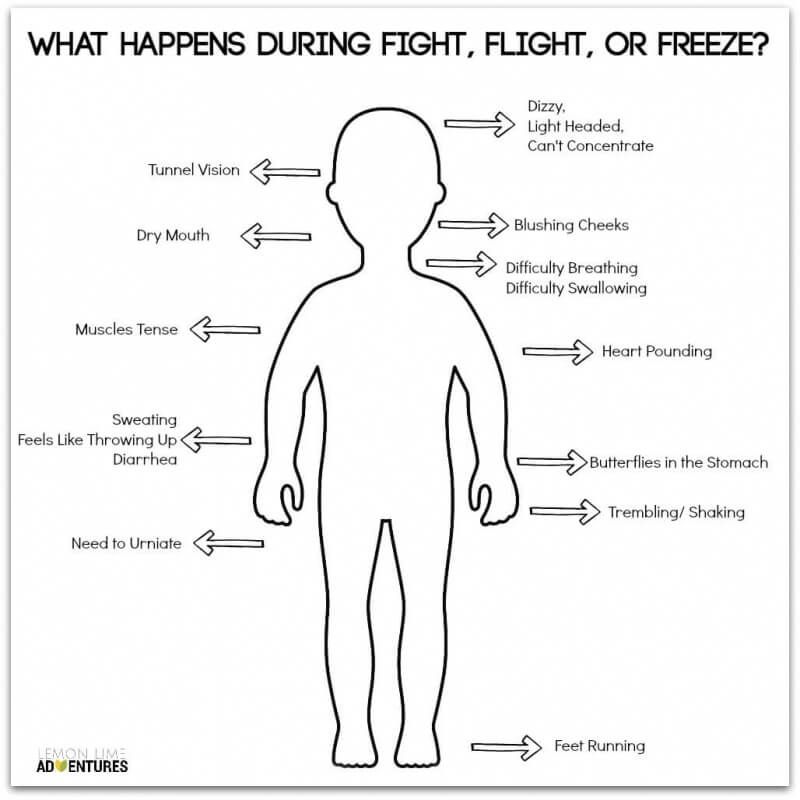
Traumatic experiences can initiate strong emotions and physical reactions that can persist long after the event. Children may feel terror, helplessness, or fear, as well as physiological reactions such as heart pounding, vomiting, or loss of bowel or bladder control. Children who experience an inability to protect themselves or who lacked protection from others to avoid the consequences of the traumatic experience may also feel overwhelmed by the intensity of physical and emotional responses.
Even though adults work hard to keep children safe, dangerous events still happen. This danger can come from outside of the family (such as a natural disaster, car accident, school shooting, or community violence) or from within the family, such as domestic violence, physical or sexual abuse, or the unexpected death of a loved one.
What Experiences Might Be Traumatic?
- Physical, sexual, or psychological abuse and neglect (including trafficking)
- Natural and technological disasters or terrorism
- Family or community violence
- Sudden or violent loss of a loved one
- Substance use disorder (personal or familial)
- Refugee and war experiences (including torture)
- Serious accidents or life-threatening illness
- Military family-related stressors (e.g., deployment, parental loss or injury)
When children have been in situations where they feared for their lives, believed that they would be injured, witnessed violence, or tragically lost a loved one, they may show signs of child traumatic stress.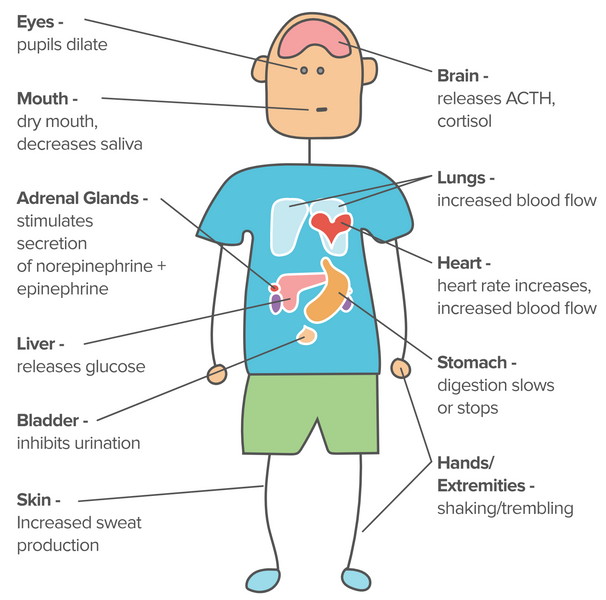
What Is Child Traumatic Stress?
Children who suffer from child traumatic stress are those who have been exposed to one or more traumas over the course of their lives and develop reactions that persist and affect their daily lives after the events have ended. Traumatic reactions can include a variety of responses, such as intense and ongoing emotional upset, depressive symptoms or anxiety, behavioral changes, difficulties with self-regulation, problems relating to others or forming attachments, regression or loss of previously acquired skills, attention and academic difficulties, nightmares, difficulty sleeping and eating, and physical symptoms, such as aches and pains. Older children may use drugs or alcohol, behave in risky ways, or engage in unhealthy sexual activity.
Children who suffer from traumatic stress often have these types of symptoms when reminded in some way of the traumatic event. Although many of us may experience reactions to stress from time to time, when a child is experiencing traumatic stress, these reactions interfere with the child’s daily life and ability to function and interact with others.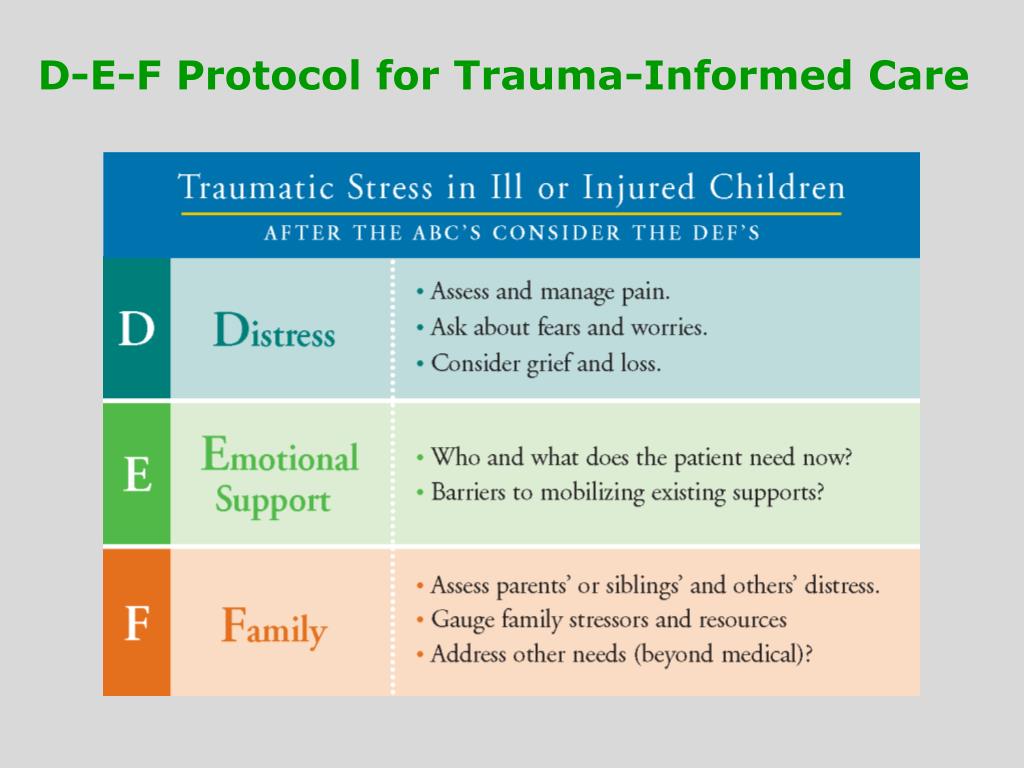 At no age are children immune to the effects of traumatic experiences. Even infants and toddlers can experience traumatic stress. The way that traumatic stress manifests will vary from child to child and will depend on the child’s age and developmental level.
At no age are children immune to the effects of traumatic experiences. Even infants and toddlers can experience traumatic stress. The way that traumatic stress manifests will vary from child to child and will depend on the child’s age and developmental level.
Without treatment, repeated childhood exposure to traumatic events can affect the brain and nervous system and increase health-risk behaviors (e.g., smoking, eating disorders, substance use, and high-risk activities). Research shows that child trauma survivors can be more likely to have long-term health problems (e.g., diabetes and heart disease) or to die at an earlier age. Traumatic stress can also lead to increased use of health and mental health services and increased involvement with the child welfare and juvenile justice systems. Adult survivors of traumatic events may also have difficulty in establishing fulfilling relationships and maintaining employment.
Reminders and Adversities
Traumatic experiences can set in motion a cascade of changes in children’s lives that can be challenging and difficult.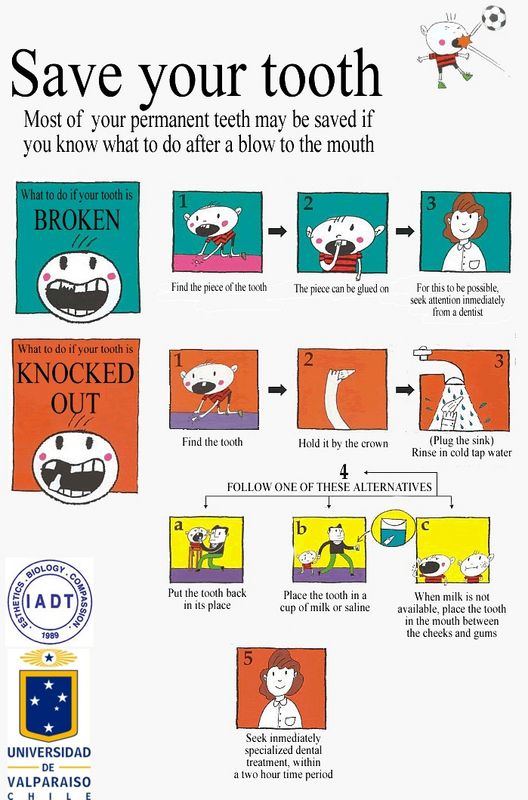 These can include changes in where they live, where they attend school, who they’re living with, and their daily routines. They may now be living with injury or disability to themselves or others. There may be ongoing criminal or civil proceedings.
These can include changes in where they live, where they attend school, who they’re living with, and their daily routines. They may now be living with injury or disability to themselves or others. There may be ongoing criminal or civil proceedings.
Traumatic experiences leave a legacy of reminders that may persist for years. These reminders are linked to aspects of the traumatic experience, its circumstances, and its aftermath. Children may be reminded by persons, places, things, situations, anniversaries, or by feelings such as renewed fear or sadness. Physical reactions can also serve as reminders, for example, increased heart rate or bodily sensations. Identifying children’s responses to trauma and loss reminders is an important tool for understanding how and why children’s distress, behavior, and functioning often fluctuate over time. Trauma and loss reminders can reverberate within families, among friends, in schools, and across communities in ways that can powerfully influence the ability of children, families, and communities to recover. Addressing trauma and loss reminders is critical to enhancing ongoing adjustment.
Addressing trauma and loss reminders is critical to enhancing ongoing adjustment.
Risk and Protective Factors
Fortunately, even when children experience a traumatic event, they don’t always develop traumatic stress. Many factors contribute to symptoms, including whether the child has experienced trauma in the past, and protective factors at the child, family, and community levels can reduce the adverse impact of trauma. Some factors to consider include:
- Severity of the event. How serious was the event? How badly was the child or someone she loves physically hurt? Did they or someone they love need to go to the hospital? Were the police involved? Were children separated from their caregivers? Were they interviewed by a principal, police officer, or counselor? Did a friend or family member die?
- Proximity to the event. Was the child actually at the place where the event occurred? Did they see the event happen to someone else or were they a victim? Did the child watch the event on television? Did they hear a loved one talk about what happened?
- Caregivers’ reactions.
 Did the child’s family believe that he or she was telling the truth? Did caregivers take the child’s reactions seriously? How did caregivers respond to the child’s needs, and how did they cope with the event themselves?
Did the child’s family believe that he or she was telling the truth? Did caregivers take the child’s reactions seriously? How did caregivers respond to the child’s needs, and how did they cope with the event themselves? - Prior history of trauma. Children continually exposed to traumatic events are more likely to develop traumatic stress reactions.
- Family and community factors. The culture, race, and ethnicity of children, their families, and their communities can be a protective factor, meaning that children and families have qualities and or resources that help buffer against the harmful effects of traumatic experiences and their aftermath. One of these protective factors can be the child’s cultural identity. Culture often has a positive impact on how children, their families, and their communities respond, recover, and heal from a traumatic experience. However, experiences of racism and discrimination can increase a child’s risk for traumatic stress symptoms.
Understanding Child Trauma - What is Childhood Trauma?
Fast Facts
At least 1 in 7 children have experienced child abuse and/or neglect in the past year, and this is likely an underestimate. In 2019, 1,840 children died of abuse and neglect in the United States.
Each day, more than 1,000 youth are treated in emergency departments for physical assault-related injuries.
In 2019, about 1 in 5 high school students reported being bullied on school property in the last year.
8% of high school students had been in a physical fight on school property one or more times during the 12 months before the survey.
Each day, about 14 youth die from homicide, and more than 1,300 are treated in emergency departments for violence-related injuries.
It’s important to recognize the signs of traumatic stress and its short- and long-term impact.
The signs of traumatic stress may be different in each child. Young children may react differently than older children.
Preschool Children
- Fear being separated from their parent/caregiver
- Cry or scream a lot
- Eat poorly or lose weight
- Have nightmares
Elementary School Children
- Become anxious or fearful
- Feel guilt or shame
- Have a hard time concentrating
- Have difficulty sleeping
Middle and High School Children
- Feel depressed or alone
- Develop eating disorders or self-harming behaviors
- Begin abusing alcohol or drugs
- Become involved in risky sexual behavior
The Body's Alarm System
Everyone has an alarm system in their body that is designed to keep them safe from harm. When activated, this tool prepares the body to fight or run away. The alarm can be activated at any perceived sign of trouble and leave kids feeling scared, angry, irritable, or even withdrawn.
Healthy Steps Kids Can Take to Respond to the Alarm
- Recognize what activates the alarm and how their body reacts
- Decide whether there is real trouble and seek help from a trusted adult
- Practice deep breathing and other relaxation methods
Impact of Trauma
The impact of child traumatic stress can last well beyond childhood. In fact, research has shown that child trauma survivors may experience:
In fact, research has shown that child trauma survivors may experience:
- Learning problems, including lower grades and more suspensions and expulsions
- Increased use of health and mental health services
- Increase involvement with the child welfare and juvenile justice systems
- Long-term health problems (e.g., diabetes and heart disease)
Trauma is a risk factor for nearly all behavioral health and substance use disorders.
There is hope. Children can and do recover from traumatic events, and you can play an important role in their recovery.
A critical part of children's recovery is having a supportive caregiving system, access to effective treatments, and service systems that are trauma informed.
Get Help Now
SAMHSA Behavioral Health Treatment Services Locator
The National Child Traumatic Stress Network: Get Help Now
Healthcare Toolbox: Basics of Trauma-Informed Care
Not all children experience child traumatic stress after experiencing a traumatic event.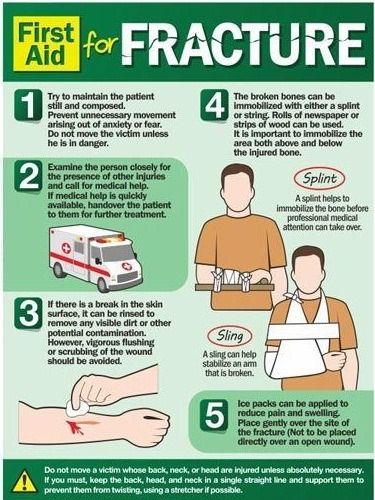 With support, many children are able to recover and thrive.
With support, many children are able to recover and thrive.
As a caring adult and/or family member, you play an important role.
Remember To:
- Assure the child that he or she is safe.
- Explain that he or she is not responsible. Children often blame themselves for events that are completely out of their control.
- Be patient. Some children will recover quickly while others recover more slowly. Reassure them that they do not need to feel guilty or bad about any feelings or thoughts.
- Seek the help of a trained professional. When needed, a mental health professional trained in evidence-based trauma treatment can help children and families cope and move toward recovery. Ask your pediatrician, family physician, school counselor, or clergy member for a referral.
Visit the following websites for more information:
- Trauma and Violence
- The National Child Traumatic Stress Network
Injuries in children.
 First aid and further actions - DMC UDP
First aid and further actions - DMC UDP Injuries in the summer are an integral part of childhood. Unfortunately, it is impossible to completely protect a child from injuries, but every adult is able to competently provide first aid. The most important rule is not to panic! If a child is injured, it is necessary to give him first aid and show him or consult a doctor. Depending on the nature of the damage, the scope of primary measures will be different. nine0003
The following types of injuries are distinguished:
Contusion in a child
The most common injury in children. As a result of a bruise, the skin is not damaged, but swelling and hemorrhage (bruising) appear at the site of impact. Ice or a chilled object must be applied to the injury site. You can do this several times during the first day in the form of applications for 5-7 minutes. With an increase in bruising, it is necessary to contact a traumatologist.
Dislocation in a child
This is an injury in which one of the bones that make up the joint is displaced outside the joint cavity. In childhood, dislocations often occur in the elbow joint and in the joints of the fingers. Any attempt to “set” a dislocation at the scene of an accident is strictly prohibited, even if a person with a medical education is trying to do it!
In childhood, dislocations often occur in the elbow joint and in the joints of the fingers. Any attempt to “set” a dislocation at the scene of an accident is strictly prohibited, even if a person with a medical education is trying to do it!
Ligament and tendon injury
This is a condition in which there is a partial rupture of the tendons or sprain of the ligaments. The most vulnerable places are the limbs. nine0003
Fracture
This is a type of injury that breaks the integrity of the bone. Distinguish between open and closed fractures. In the latter case, damage to the skin in the area of the fracture occurs.
First aid consists only in fixing the injured limb and transporting the child to the nearest medical facility. If the upper limb is damaged, the arm is fixed with a scarf bandage, if the lower limb is damaged, it is fixed with a splint along the entire length of the leg, using any available material for manufacturing. In case of an open fracture, it is necessary to cover the wound with a clean napkin; if possible, it is permissible to moisten the napkin with an antiseptic solution to avoid infection. It is optimal to fix the napkin with a band-aid or grab it with a bandage. nine0036 It is strictly forbidden to eliminate the displacement of bone fragments at the scene of the incident!
In case of an open fracture, it is necessary to cover the wound with a clean napkin; if possible, it is permissible to moisten the napkin with an antiseptic solution to avoid infection. It is optimal to fix the napkin with a band-aid or grab it with a bandage. nine0036 It is strictly forbidden to eliminate the displacement of bone fragments at the scene of the incident!
Abrasion
This is a superficial injury to the skin. In most cases, it is enough to treat the abrasion with any antiseptic solution. However, if redness occurs around the abrasion, swelling, fluid discharge of the child, it is necessary to show it to a pediatric surgeon.
Wounds
The most diverse type of injury. This is quite deep compared to an abrasion, skin damage, accompanied by bleeding. The main pre-medical measure for wounds is to stop bleeding. To do this, a pressure bandage is applied to the wound, previously, if possible, washing with water to remove foreign objects and treating with an antiseptic solution. It is forbidden to remove foreign bodies from the wound with your hands, since there is a possibility of displacing them inside the wound. nine0003
It is forbidden to remove foreign bodies from the wound with your hands, since there is a possibility of displacing them inside the wound. nine0003
In case of abrasions and wounds, the issue of emergency vaccination against tetanus must be resolved, the need and amount of which is determined by the doctor.
Bites
Bites come from insects and animals. With minor insect bites, the doctor prescribes antihistamines, with a bite of a stinging insect (wasp, bee) - you must contact a medical institution for possible removal of the insect sting and treatment of the wound.
In the event of a tick bite, contacting a pediatric surgeon or orthopedic traumatologist is mandatory. You should not attempt to remove the tick yourself, as this increases the risk of infection with tick-borne encephalitis or borreliosis. You can protect your child and get vaccinated against tick-borne encephalitis at our children's medical center. nine0003
If bitten by an animal, including a domestic animal, cover the bite with a clean bandage and seek immediate medical attention.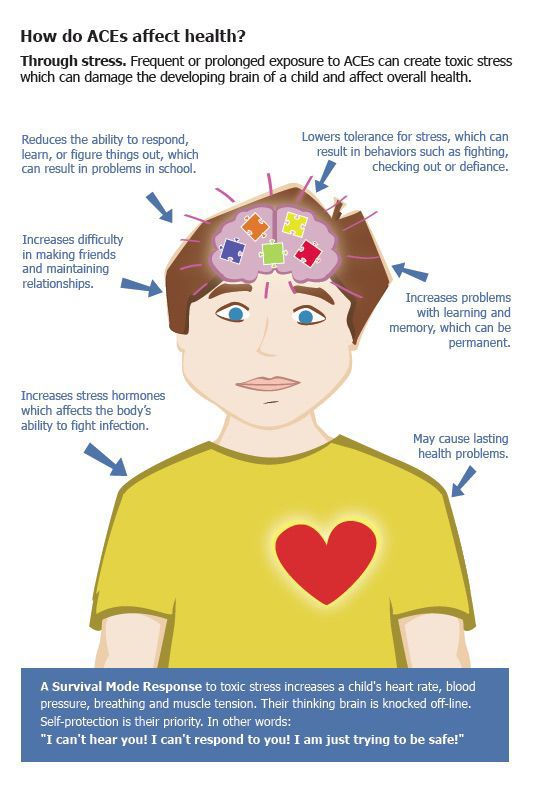 When bitten by animals, children are prescribed a course of vaccinations aimed at preventing rabies.
When bitten by animals, children are prescribed a course of vaccinations aimed at preventing rabies.
Burn
Type of injury resulting from skin exposure to very high temperatures, chemicals, or combinations thereof. Most often, children get burned by fire or boiling water. There are several degrees of burns from mild, characterized by reddening of the skin, to severe, in which deep lesions of soft tissues are noted. With these injuries, it is necessary to stop the action of heat and chemical compounds as soon as possible and cool the affected area either under a stream of cold water or with wet, cold, frequently replaced wipes. Regardless of the degree of the burn, the child must be shown to the pediatric surgeon. nine0003
Electric shock or electric shock
This type of injury occurs when a child comes into contact with sockets, electrical appliances and wires. With such an injury, along with the occurrence of a burn at the point of contact, there is a violation in the work of the cardiovascular system in the form of an arrhythmic heartbeat and intermittent breathing. If you receive an electrical injury, you must immediately call an ambulance. Such children require medical supervision for several days. nine0003
If you receive an electrical injury, you must immediately call an ambulance. Such children require medical supervision for several days. nine0003
What are childhood “traumas” and how to recognize them in adulthood
When a parent limits a child in contact with others and controls his social circle, the child may feel lonely, isolated from the outside world. Under such conditions, socialization and the development of independence are impossible. With verbal aggression and threats (for example, "I will refuse you"), the child will cease to trust the world and begin to perceive everything as hostile.
If parents themselves grew up in violence, then these destructive patterns can automatically be transferred to their attitude towards children. Therefore, it is first of all important to recognize and correct your own experience. nine0003
We are made up of the behavior patterns of our parents.
“Sexual abuse is not only a sexual act, but also a neglectful attitude of parents towards a child's sexuality,” explains Veronica. This can lead to rejection of one's body, cause repeated violence (a person can either commit it himself or again find himself in the role of a victim). “If the child’s physical and psychological boundaries are violated, this affects his entire adult life, and the negative experience will be repeated again and again,” says Irina. nine0003
This can lead to rejection of one's body, cause repeated violence (a person can either commit it himself or again find himself in the role of a victim). “If the child’s physical and psychological boundaries are violated, this affects his entire adult life, and the negative experience will be repeated again and again,” says Irina. nine0003
Why do we not remember some traumatic childhood events?
“When a person is traumatized in childhood, he represses it later in life. Thus, the psyche is protected, blocks painful information, ”explains Irina Mansurova. But even without remembering the causes of the injury, an adult will still feel its consequences - depression, guilt, etc. “The child also needs to somehow adapt, and one of the ways to do this is to dissociate the situation. For example, a child lives with parents who are addicted to alcohol. He has nowhere else to live - what will he do? Dissociate and anesthetize the affected part of the soul. It will block some memories, thoughts and images, as this reduces pain sensitivity. Subsequently, such people do not get hurt: they do not feel anything at all. The child gets used not to hear, not to feel and not to see: dissociation allows him to survive, and the psyche will use various methods so as not to collapse, ”says Veronika Doringer. nine0003
Subsequently, such people do not get hurt: they do not feel anything at all. The child gets used not to hear, not to feel and not to see: dissociation allows him to survive, and the psyche will use various methods so as not to collapse, ”says Veronika Doringer. nine0003
Repression
Often a severely traumatized person represses some or all of their past. He simply cannot remember events from his childhood, sometimes only some strongly emotionally charged events come up in his memory.
Loss of trust in the world
Avoidance of any trusting relationship. The logic of this choice is simple: "If there is no relationship, then I can avoid pain." Such a person eschews even friendship because of the anxiety that he will be betrayed, therefore he deliberately avoids intimacy, which over time can lead to loneliness and depression. Any harbinger of emotional intimacy that can cause psychic pain will be blocked. nine0003
Tendency to toxic relationships
People who were severely traumatized as children often enter into destructive relationships as adults. Their partners may be emotionally unavailable, married, violent, or have a narcissistic personality disorder. After ending one toxic relationship, a person will be drawn into others, attracting such partners over and over again. To get out of the vicious circle will help work through the trauma with a psychotherapist. nine0003
Their partners may be emotionally unavailable, married, violent, or have a narcissistic personality disorder. After ending one toxic relationship, a person will be drawn into others, attracting such partners over and over again. To get out of the vicious circle will help work through the trauma with a psychotherapist. nine0003
Difficulties with perception of other people's emotions
A person cannot recognize the true emotions and feelings of another person, because he projects his thoughts and feelings onto him.
How to start working with childhood trauma?
“When people with traumatic experiences raise their children, they are brought back to their traumas. They remember how their parents acted in any situations and do not understand their actions,” explains Veronica. Experiencing once again a painful experience, it is difficult to be emotionally included. Therefore, it is important that the parent first learns to help himself.