Stopping breastfeeding and hormones
After weaning – what next?
Breastfeeding always comes to an end – at some point, every breastfed baby or child stops breastfeeding. This article looks at what happens after your toddler or older child weans,1 how it feels for you and what it might mean for you going forward.
Sometimes, because of difficulties, breastfeeding your baby comes to an end much earlier than you thought it would or than you had hoped for. And with that can come feelings of anger, guilt, sadness, hurt and disappointment. If you are currently struggling with breastfeeding ending earlier than you had hoped, we would encourage you to talk to someone – your local LLL Leader would be pleased to support you. You may also find this article of interest:
Five ways to help when breastfeeding doesn’t go as expected. Amy Brown’s book Why Breastfeeding Grief and Trauma Matter which explores the deep feelings women have when breastfeeding doesn’t go to plan, may also be helpful.
Will weaning happen?
What is certain is that all children stop breastfeeding eventually. Children outgrow breastfeeding on their own, just as they outgrow other toddler and young child behaviours. For many families, taking the approach of being led by your child works well and the transition from breastfeeding to no longer breastfeeding is uneventful. It may all feel less noticeable if weaning takes place slowly and gently.
This process of ‘natural weaning’ allows a child to develop at their own pace, giving up breastfeeding according to their own natural timing. Rather than choosing a specific time to stop breastfeeding, many mothers just continue nursing while it is working well for them and see how it goes. That might mean breastfeeding for years beyond what you expected as you first breastfed your newborn.
Once weaning has happened
If you are following your child’s lead, it is unlikely they will wean suddenly or overnight, especially if they are under one year old (see our article on Nursing Strikes if you are concerned this is happening). It is really common for the natural weaning process to take a long time and feel like a few steps forward and a few back. This can feel confusing at times.
It is really common for the natural weaning process to take a long time and feel like a few steps forward and a few back. This can feel confusing at times.
It’s not uncommon for children to look like they are weaning, only to come back – often with renewed energy – to breastfeed when you least expect it or when you thought they had weaned. A new baby, an unsettled family time, a change in their days such as whenstarting preschool or school, or illness can often lead to an increase in breastfeeding just when you thought they were stopping. That can be unsettling if you are trying to decide if you are still breastfeeding or not – one day you might not be, and then the next you are again. One mother said: “I thought she was weaning and I was starting to feel the grief of it around three years old, but we are still going at four.”.
‘The Last Breastfeed’ might not be a significant event. For some, weaning happens so gradually, that suddenly you realise your child hasn’t asked to nurse for a while, and you can’t remember your last breastfeed – or at least, you didn’t know it was the last time.
This is often the time mothers wish they had captured more photographic memories of their toddler or child breastfeeding, not realising that soon it might be the last breastfeed. Taking photos of you and your child nursing can be really special, so you may want to consider taking more at this stage.
Emotional change
The topic of what it feels like after weaning isn’t talked about much and so you might be wondering if what you are feeling is normal. It almost always is.
For many, weaning is an emotional adjustment
As breastfeeding comes to end it can be an emotional time and mothers can experience a wide range of feelings. For some it might be a time of sadness – a sense of loss for the time that’s gone before and a sorrow that your special ‘baby days’ are passing and behind you. For others it might be a huge relief and a time you had longed for and thought would never come.
Or it might be a mix of both.
Perhaps one moment you may feel a sense of relief that the intensity of breastfeeding is passing and the next moment sad that this stage of motherhood is drawing to a close when it has been so important to you.
The Womanly Art of Breastfeeding says: “You may revel in your non-nursing status but also feel weepy or supersensitive for a time.”2
One mother described the time of her two year old weaning as a confusing time of feeling a sense of loss but also happiness: grief and relief. Another, as her four year old weaned, said that she was completely ready to stop (and was desperate to), but then realised it meant she had to redefine how she viewed herself as she always thought of herself as a breastfeeding mother.
This huge mix of emotions around your breastfeeding journey coming to an end is common. Especially if you worked so hard to make it happen in the early days. When breastfeeding has been such a central part of how you have mothered your child, it can feel like a new and perhaps uncertain stage.
Distress around weaning is more likely the earlier it happens, or where it happened before you wanted or had intended. Where weaning has happened very early on, mothers can be left with deep feelings of anger, grief, sadness and disappointment. Where weaning has happened suddenly, or has been stressful, it is more likely that the emotional impact may be greater. How old your child is when they wean may not be as important to how you feel about weaning, rather the sense that things ended well. As Diane Bengson says: “Mothers who wean gradually, or who feel that weaning happened at a time when both they and their child were ready, often feel peace and contentment when weaning is complete3
Where weaning has happened suddenly, or has been stressful, it is more likely that the emotional impact may be greater. How old your child is when they wean may not be as important to how you feel about weaning, rather the sense that things ended well. As Diane Bengson says: “Mothers who wean gradually, or who feel that weaning happened at a time when both they and their child were ready, often feel peace and contentment when weaning is complete3
But even if you initiated weaning or encouraged your child to wean, you may still find moments of sadness. Even when weaning is a positive experience for both of you, ‘letting go’ can still feel emotional. Some mothers and parents describe it as nostalgia for the early times of breastfeeding your baby. Perhaps this is even more apparent if you know this is your last baby and you know you won’t be a nursing mother again.
If you felt that your child initiated weaning rather than you did, and it was sooner than you had hoped for, those feeling of sadness can be stronger. Or if your toddler or older child weaned quickly, you may feel a sense of hurt or rejection. In The Nursing Mother’s Guide to Weaning, Kathleen Huggens says:“ Even if you had planned to wean soon, you may feel surprised and a little disappointed when your child rejects you in favour of a cup or bottle.”4
Or if your toddler or older child weaned quickly, you may feel a sense of hurt or rejection. In The Nursing Mother’s Guide to Weaning, Kathleen Huggens says:“ Even if you had planned to wean soon, you may feel surprised and a little disappointed when your child rejects you in favour of a cup or bottle.”4
Or you may actually feel nothing but relief – that you are pleased to be moving on from the intensity of the early days and years and enjoying a sense of having your body back. You might be relieved to finally ditch your nursing bras and look forward to wearing clothes that no longer need easy access. You may find a sense of relief that you can sit down without being asked to nurse, and that maybe that intense need for you is easing a little – and that feels good.
The key is that whatever you are feeling emotionally about weaning – it’s normal. What one mother experiences won’t necessarily be the same as another. Talking about it with others who have weaned at LLL groups (in person or online), might help.
Hormonal Changes
When weaning happens, there is also a physical and hormonal adjustment which, despite limited studies on the subject, seems to reflect across the experience of many. This adjustment can lead to a short time of feeling quite low, as your hormones settle down.
It can be really common to feel down or weepy – or even depressed – after weaning. And for some, the feelings are strong and may mean there is a sense of anxiety, insomnia, anger, swings between high and low moods. In part, this is because of hormonal changes happening in your body as you adjust to reducing, and then no longer, making milk or having the repeated closeness of your child at your breast. Your breasts may still continue to produce milk, but gradually they will stop and for some mothers it might be months before they can no longer squeeze a few drops out.
There is little research on the topic, but we know that the hormones so important in breastfeeding – prolactin (milk making hormone) and oxytocin (the hormone of love and responsible for the milk ejection reflex) – play an important role in how we feel emotionally. Both oxytocin and prolactin contribute to feelings of calm, love, relaxation, closeness and contentment. As breastfeeding ends, both prolactin and oxytocin levels will lower – and so may your mood and sense of wellbeing. It may last a few days, or it may go on for longer.
Both oxytocin and prolactin contribute to feelings of calm, love, relaxation, closeness and contentment. As breastfeeding ends, both prolactin and oxytocin levels will lower – and so may your mood and sense of wellbeing. It may last a few days, or it may go on for longer.
So if you are feeling low or weepy after weaning, it can be reassuring to know that it is likely that your body is also dealing with hormonal changes, as well as any emotions you may have around weaning. Even if you are totally at peace with weaning and know the time is right for you both, there are changes happening in your body that might have an impact on how you feel.
It has often been described as similar to how you feel hormonally as part of your menstrual cycle, but more intense and more long lasting. Others may go further and say that they feel really sad and depressed for a few weeks after weaning. Often your hormones settle within a few weeks and you and your child adjust to a new rhythm where breastfeeding is no longer part of your current story.
These feelings of sadness and general lowness that can happen after weaning are normally temporary. Being gentle and patient with yourself is important. If you have ongoing low mood or depression after the initial weeks, it may be helpful to talk to your GP.
How do I do ‘this’ without breastfeeding?
If your child has stopped breastfeeding gradually or they have led the weaning process, you may see this as all part of the bigger picture of watching your child grow into an independent little person. Your role of mothering ‘your baby’ is changing. Perhaps your child is spending longer away from you, may be sleeping longer or on their own, and maybe there is a sense that their need for you isn’t quite so intense. That can be both a relief and an adjustment.
You may feel proud of how they have grown and how much you have learnt about parenting through breastfeeding, but perhaps wonder what it means for you if you no longer have breastfeeding in the picture. Perhaps you are relieved that your breasts are no longer the focal point of your child’s day?
Where breastfeeding has been important to you both, it can sometimes feel a bit uncertain about how things might go without nursing as a go-to or back-up for when parenting is tricky. How will you get them back to sleep if they wake with a bad dream in the middle of the night? How will you calm them down when the emotional whirlwind takes over them? What will you do when they bump themselves? How will you get some extra time in bed in the morning if your breast no longer offers the oasis of calm it once did?
How will you get them back to sleep if they wake with a bad dream in the middle of the night? How will you calm them down when the emotional whirlwind takes over them? What will you do when they bump themselves? How will you get some extra time in bed in the morning if your breast no longer offers the oasis of calm it once did?
Often looking back at all your breastfeeding relationship gave you and your child, can help shape your ‘new’ picture of parenting without breastfeeding. Many mothers would say that breastfeeding their baby beyond babyhood is one of their proudest and greatest achievements. If that is the case, it might feel right to celebrate or mark the event in some way for you that feels significant – for both you and and your child. Be proud!
And if you are feeling low, or missing that physical closeness, sometimes finding other ways to connect on a physical level with your child can help. If your arms are feeling “empty” without your child nursing at the breast, cuddling lots, having baths together and playing physical games with them climbing on you or rolling around together, can help with getting a hormone boost. Simple cuddles and touch, or sniffing or nuzzling your child’s head, can work wonders for having a surge of oxytocin.
Simple cuddles and touch, or sniffing or nuzzling your child’s head, can work wonders for having a surge of oxytocin.
It’s likely your breasts and chest will be a special place for your child for a long time. Many mothers have commented how their older child still likes to place their head or hand near their breast, or when upset, will cuddle into a breastfeeding position without actually breastfeeding.
Looking ahead
As you watch your child wean – be it entirely on their own, or with some gentle encouragement from you – you may find that you swing between various emotions and thoughts. Whether weaning passed uneventfully and feels like a natural end to your breastfeeding journey, or you found it an emotional and challenging time, looking back and acknowledging what you achieved and what you have given your child is something you can be rightly proud of.
Breastfeeding has taught you so much about recognising your child’s needs and emotions, their demands and their wants. Your ability to nurture them, to read their cues and respond to them hasn’t changed, but it might be that instead of offering the breast, you now meet those needs in different ways. And while your baby may no longer need comfort at your breast, they still need you.
Your ability to nurture them, to read their cues and respond to them hasn’t changed, but it might be that instead of offering the breast, you now meet those needs in different ways. And while your baby may no longer need comfort at your breast, they still need you.
Many mothers and parents look at their older children, even grown-up children, and know that the shape of their relationship has its foundation back in their nursing days. The closeness, understanding and connection that you grew together at the breast over the years, will continue – in new and different ways but shaped by your breastfeeding journey.
Endnotes
- Weaning here describes the process of stopping breastfeeding, not the introduction of family foods which takes place around the middle of your baby’s first year.
- La Leche League International. The Womanly Art of Breastfeeding. 8th Edition, 2010: 337.
- Bengson, D. How weaning happens. La Leche League International, 2000: 137.
- Huggins, K and Ziedrich, L. The Nursing Mother’s Guide to Weaning. 2007: 177.
Further reading
Still Nursing
Thinking about weaning
Breastfeeding beyond Infancy
Breastfeeding beyond one year
Nursing strike
A sudden end to breastfeeding
The goodness goes on
LLLI articles:
Weaning: How to
Written by Justine Fieth, LLL Cambridge, October 2020.
Thanks to Ginnie Sullivan and the Leaders of LLL Cambridge for their help writing this.
What Happens to Our Hormones When We Stop Breastfeeding? – Perelel
Meet
The Expert:
Stephanie Cortner, founder of Root & Branch, is a licensed Acupuncturist, herbalist and Functional Medicine practitioner. Her practice specializes in hormone balancing, fertility, autoimmune disease, GI health and sports medicine. Stephanie’s goal is to combine Eastern and Western studies to offer integrative healthcare options so patients can fully achieve their potential by leading happier and healthier lives.
We nursed on the idyllic beaches of Malibu, sandy and serene; we nursed on the hot asphalt parking lot of Trader Joe’s, sweaty and angry; I pumped on the 405 freeway, on the couch, in the bed. It was tender bonding, it was never-ending physical exertion, and after eight and half months (don’t short me those last two weeks, thank you very much) and several spine-shivering experiences with four razor-sharp baby teeth, our breastfeeding journey came to an end. Making the decision to stop breastfeeding was hard enough—there’s the mom guilt; the unfulfilled expectations; the frustrated baby—but what I did not expect was that the process would send me into a hormonal tailspin flooded with tears, anxiety, fatigue and inexplicably greasy hair.
I probed my peers to find out: Does weaning from breastfeeding make one crazy? Is something wrong with me? The anecdotes flooded in. “When I was weaning it was the worst anxiety I’ve ever had.” “I felt horrible.” “I cried all day.” I marinated; were we all suffering through rock hard chests and cabbage leaves in silence? What was chemically happening here?
To make sense of the hormonal changes that happen with weaning, I spoke with Stephanie Cortner, founder of Root and Branch and licensed Acupuncturist, herbalist and Functional Medicine practitioner.
Keep reading for her tips on how to wean from breastfeeding.
Can weaning from breastfeeding affect your hormones? How so?
“Yes! There are hormonal changes during pregnancy and postpartum, but what a lot of women don’t expect is the huge hormonal shift throughout the process of weaning. Throughout breastfeeding there is an abundance of two very important hormones, prolactin and oxytocin. Prolactin is known as the hormone that tells the body to produce milk and keeps mom feeling calm and relaxed, but that's not its only role. Prolactin also produces a hormone called oxytocin; the hormone that you might know of as the ‘love hormone.’ Oxytocin is the reason why we feel so content and happy when we are breastfeeding. As we start to wean, prolactin levels drop, which stops the production of oxytocin as well,” Cortner explains. “From an Eastern Medicine point of view, postpartum and breastfeeding women are extremely blood deficient or as we say, liver blood and yin deficient, due to losing fluid while breastfeeding and blood during childbirth. ” That doesn’t sound ideal.
” That doesn’t sound ideal.
“With prolactin and oxytocin levels lowering, progesterone and estrogen levels will begin to rise, which in turn sparks ovulation and our menstrual cycle to start up once again. We are not only managing the decrease in all the ‘feel good’ hormones but we are also dealing with the hormonal shifts that come with our menstrual cycles. If you had a difficult time with hormonal fluctuations before pregnancy, this might be a rather challenging time for you,” Cortner says.
Symptoms of Weaning from Breastfeeding
- sadness
- anxiety
- breast engorgement
- weight gain
- difficulty with concentration or "mom brain"
- dry mouth
- guilt
“Please know that you are not alone. The majority of symptoms should only last for a month or two and should fully subside after three months. If these manifestations go beyond that or feel unmanageable during the weaning, please reach out to your therapist or OB for further help.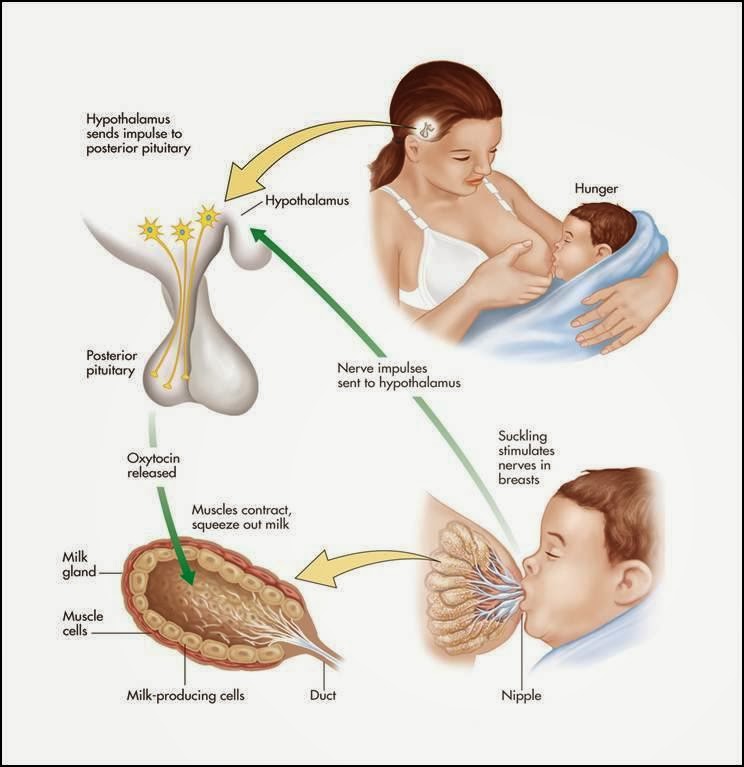 ”
”
“Remember to wean slowly! Dropping one feeding a week, if possible, will make the symptoms less intense. This, of course, will also depend on your hormones and how your body responds to the weaning. Oxytocin is released through breastmilk but it is also released through cuddling. Even though your little one is spending less time on your breast, you can still take the same amount of time for cuddles, which will continue the release of oxytocin,” Cortner suggests.
Looking for a postnatal vitamin to support you postpartum? We recommend our Mom Multi Support Pack specifically formulated by a team of OB/GYNs to support moms while breastfeeding.
Ways to Support Your Body While Weaning Off Breastfeeding
- Wean slowly by dropping one feeding a week.
- Release oxytocin by cuddling with your baby.
- Try to get adequate sleep, which we know is no easy fete with a new baby at home.
- Eat a fiber-rich diet to support your microbiome.
- Be sure to eat plenty of nutritious whole foods. Cortner especially recommends:
- seaweed
- black beans
- fish
- black sesame seeds
- Add replenishing supplements and herbs like:
- postnatal vitamins
- fish oil
- iron
- magnesium
- adaptogenic herbs
- nettle and dandelion teas to restore calcium and iron
- Meditate to calm your nervous system.
- Exercise when you can, even if it's just a few minutes of moving your body each day.
By the way, these are the four foods a nutritionist wants you to avoid while breastfeeding.
How long after weaning will it take for hormones to balance and your cycle to recalibrate?
“Any changes to our body’s systems typically takes up to three months. This is the time for our hypothalamic-pituitary-ovarian (HPO) axis, which is the communication from brain to ovaries, to recalibrate. Acupuncture can greatly decrease the amount of time it takes your body to adjust and can also help with the transition in hormones as well as to help your body create endorphins naturally. If you still don’t feel like yourself after a few months, functional medicine lab tests are great at finding where the root of the imbalance lies so we can supplement your body with the right precursors and cofactors instead of simply chasing symptoms,” Cortner says.
Acupuncture can greatly decrease the amount of time it takes your body to adjust and can also help with the transition in hormones as well as to help your body create endorphins naturally. If you still don’t feel like yourself after a few months, functional medicine lab tests are great at finding where the root of the imbalance lies so we can supplement your body with the right precursors and cofactors instead of simply chasing symptoms,” Cortner says.
“Unfortunately, anxiety and depression can definitely be a part of the weaning process. Identifying where the feelings are coming from is important. There is a lot of guilt that comes up when weaning, and there are therapists that are specifically trained in postpartum and post weaning blues. If it is purely hormonal, again, herbal formulas are really powerful. Sometimes we need a little extra and that is where the functional labs come in handy to see if specific neurotransmitters such as dopamine and serotonin levels are low and then giving precursors to these neurotransmitters so we are telling our brains how to properly operate and fire again. Other times it can be as simple as taking a strong B complex vitamin a couple times a day on top of our prenatal. B vitamins are really important! These guys are cofactors in so many different systems in the body and when we are deficient in them, those systems, such as our mitochondria, or energy creators in our cells, don’t have the fuel they need to be powered correctly. The good news is that there are many supportive measures to ease the weaning transition and the most important thing is to be kind to yourself, listen to what your body is telling you and ask for help,” Cortner says.
Other times it can be as simple as taking a strong B complex vitamin a couple times a day on top of our prenatal. B vitamins are really important! These guys are cofactors in so many different systems in the body and when we are deficient in them, those systems, such as our mitochondria, or energy creators in our cells, don’t have the fuel they need to be powered correctly. The good news is that there are many supportive measures to ease the weaning transition and the most important thing is to be kind to yourself, listen to what your body is telling you and ask for help,” Cortner says.
Are you currently breastfeeding? Get more tips for feeding your baby. Plus, support yourself with Perelel Mom Multi Support Packs formulated for postpartum and beyond throughout motherhood.
This article is for informational purposes only. It is not, nor is it intended to be, a substitute for professional medical advice, diagnosis, or treatment and we recommend that you always consult with your healthcare provider. To the extent that this article features the advice of physicians or medical practitioners, the views expressed are the views of the cited expert and do not necessarily represent the views of Perelel.
To the extent that this article features the advice of physicians or medical practitioners, the views expressed are the views of the cited expert and do not necessarily represent the views of Perelel.
Written by Jessica Lopez. Jessica Lopez is a freelance writer, digital content creator, and new mother. She has covered all lifestyle topics ranging from bridal to beauty for publications including Brides Magazine, Byrdie, THE/THIRTY, and more. Walking wide-eyed into motherhood has inspired her to connect with other parents through her writing and shared experience. You can follow more of her journey @Jessica.H.Lopez.
Cessation of breastfeeding for medical reasons
Cessation of breastfeeding is the process of transferring a child from mother's milk to other sources of nutrition. In rare cases, abrupt cessation of breastfeeding may be required due to illness of the mother, medication, or prolonged separation from the child. Unlike gradual weaning by the mother or refusal to breastfeed by the baby over several months, abrupt cessation of breastfeeding can be psychologically difficult for both mother and baby. In addition, it can cause significant chest discomfort and put the mother at risk of mastitis. If possible, abrupt cessation of breastfeeding should be avoided and the baby should be weaned gradually so that he himself refuses it. nine0003
In addition, it can cause significant chest discomfort and put the mother at risk of mastitis. If possible, abrupt cessation of breastfeeding should be avoided and the baby should be weaned gradually so that he himself refuses it. nine0003
Share this information
Physiological changes during the abrupt cessation of breastfeeding
In the process of cessation of breastfeeding, the composition of milk changes greatly, especially if it happens at the same time. Despite the fact that the secretory capacity of the mammary glands decreases, in the process of involution, the breast tissue partially retains its functions for quite a long time (about 45 days). Between days 1 and 45, the concentration of lactose and potassium decreases, while the concentration of sodium, fat and total protein increases. In addition, milk becomes more salty due to an increase in the content of proteins (lactoferrin, immunoglobulins A, G and M, albumin, lactalbumin and casein).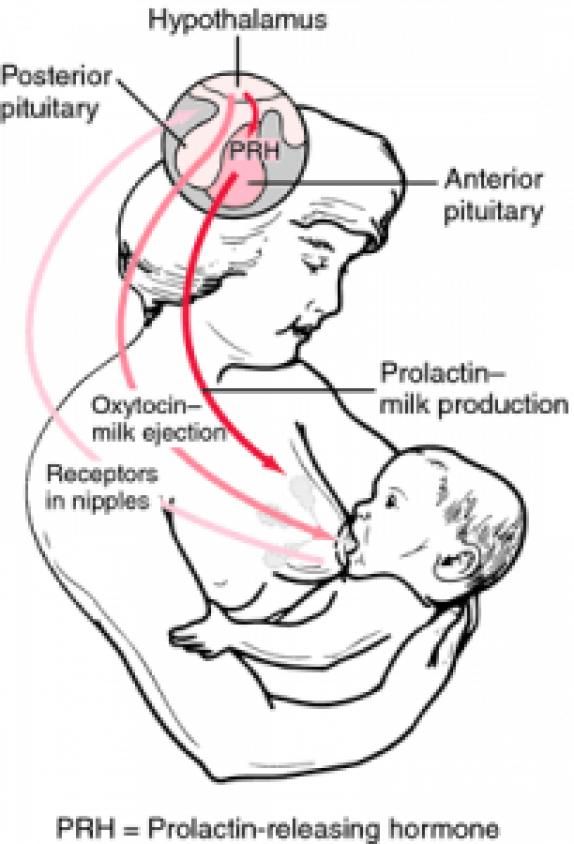 nine0003
nine0003
Abrupt cessation of breastfeeding can cause dramatic hormonal changes, especially in the first month after birth when prolactin levels are extremely high.
General guidelines for stopping breastfeeding for medical reasons
- If you need to stop breastfeeding for medical reasons, it is recommended that you seek support from a qualified lactation specialist. He should help determine if there are other options (for example, if other medications for the mother can be used). nine0018
- Mothers should express milk manually or with electric breast pumps to relieve the feeling of fullness and feel comfortable, but the amount of expressed milk should be minimal so as not to stimulate further production.
- Other methods may be helpful, including wearing a comfortable supportive bra and monitoring for signs of blocked milk ducts or breast infection.
- Some mothers, especially those prone to depression, may need emotional and social support during the transition from breastfeeding.
 nine0018
nine0018 - Do not neglect the instructions for stopping breastfeeding for physiological reasons.
Literature
Lawrence, R. A. and Lawrence, R. M. Breastfeeding: a guide for the medical profession (Elsevier Mosby, Maryland Heights, MO, 2011). - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." (Maryland Heights, Missouri, USA: Elsevier Mosby; 2011.)
Li, R., Fein, S.B., Chen, J., Grummer-Strawn, L.M. Why mothers stop breastfeeding: mothers' self-reported reasons for stopping during the first year. — Lee R, Fane S.B., Chen J., Grummer-Stroane L.M., "9
Hartmann, P.E., Kulski, J.K. Changes in the composition of the mammary secretion of women after abrupt termination of breast feeding. J Physiol 1978 Feb ;275:1–11 - "Changes in the composition of the breast secretion in women after the end of breastfeeding" Zh Physiol 1 ? - How long? "... when a woman is no longer breastfeeding and menstruation is full, the so-called "free" prolactin circulates in the blood - the body cannot abruptly stop its production... "Free prolactin", imagine! I am already exhausted by these hormonal changes in the body. But what to do. Phytosed, vitamins Vitrum Prenatal, get enough sleep and often walk in the open air. So far, it’s nonsense with nutrition, because from permanent stress it always draws on chocolate and coffee. It seems that his scent alone can lift me up. The help of a psychologist or a nutritionist would be real, but there is no money for them and there won’t be, so I’m looking for affordable recommendations.
Categories:
The article is devoted to nutrition and hormonal balance of women. But I was attracted by some individual answers of the dietitian Anokhina Olga Vyacheslavovna about what happens at the hormonal level after the cessation of breastfeeding.
In particular:
"From a nutritional point of view, the first months after breastfeeding is critical for women in terms of weight gain.
After all, while a woman was intensively breastfeeding, not only incoming substances, but also the resources of her own body - everything was directed to maintaining lactation. Milk production itself is already a rather complex, energy-intensive process, and often nursing mothers, on the contrary, lose weight. But at the end of breastfeeding, a woman, finally, can not limit herself and leans on sweets, chocolate ... But her energy consumption no longer corresponds to the previous level - and everything received is deposited in fat depots. "
But at the end of breastfeeding, a woman, finally, can not limit herself and leans on sweets, chocolate ... But her energy consumption no longer corresponds to the previous level - and everything received is deposited in fat depots. "
At first I got an unexpected effect, and then I literally rushed to look for answers. Unexpected, because all the doctors told me during breastfeeding that the weight would return to normal after the cessation of breastfeeding by itself.
And here, still, the main thing, in my opinion.
"When you finish breastfeeding, you do not need to actively change everything in your life on the same day - a woman should gradually part with the lifestyle of a nursing mother. Having finished breastfeeding, well, do not run to work that day, let the body adapt to new conditions life! And if we say that a nursing mother should rest more, be in the fresh air and eat well (that is, in fact, set herself a certain spa regimen ), then we recommend that women observe this very regimen for some time after the end of lactation.
It often happens in women that after quite a long time after the end breastfeeding prolactin persists in the blood, and this is accompanied by irregular periods, emotional instability, irritability. "