Obsessive compulsive disorder paranoia
Paranoia And How It Is Linked To OCD
Content
- Overview
- What Is OCD?
- What Is paranoia?
- The link between OCD and paranoia
- Treatment options for OCD
- When to see a doctor
- The lowdown
Most people have heard the terms "paranoia" and "OCD." Both terms come with numerous misconceptions, which can be harmful to a person suffering from them. Paranoia and OCD can make everyday life more difficult, especially when it comes to maintaining friendships and relationships.
OCD and paranoia may be related, and it is possible to experience both at the same time. Learn more about what OCD and paranoia are and how they may be linked.
Have you considered clinical trials for Obsessive compulsive disorder (OCD)?
We make it easy for you to participate in a clinical trial for Obsessive compulsive disorder (OCD), and get access to the latest treatments not yet widely available - and be a part of finding a cure.
Check your eligibility
OCD, or obsessive-compulsive disorder, is a mental disorder characterized by obsessive or repeating thoughts and rituals or compulsive behaviors. People with OCD may have fears about various things, including germs or getting sick, acting impulsively and hurting themselves or others, or doing something wrong that leads to harm.
OCD can be diagnosed in people from all backgrounds, though there does appear to be a genetic link. Families with OCD are approximately four times¹ more likely to develop OCD than families without a history of the condition. However, having a family member with OCD doesn't guarantee that you will also develop it.
Paranoia can be described as feelings or thoughts that someone or something is threatening you, even if you don't have evidence that you are in danger. People experiencing paranoia may not even worry about physical threats, like someone wanting to harm them. Instead, they may have fears that people purposely upset them or that others are striving to make them look bad.
It can be difficult to determine whether you are experiencing paranoia or actually in danger. Thoughts are typically paranoid when nobody else shares suspicion, there is no evidence for the thought, but there is evidence against it, and your suspicions are based more on feelings than facts. Paranoia may be mild, or it can become incredibly severe, making it difficult to operate daily. Paranoia may also stem from other mental illnesses such as paranoid schizophrenia, paranoid personality disorder, and delusional disorder.
OCD and anxiety are commonly diagnosed together, as OCD is an anxiety-based disorder. People with OCD develop real fears of a range of things, which can cause anxiety when they are exposed to their fears. As a result, they rely on compulsive behaviors to try to keep their fears at bay, but they often worsen their condition.
Paranoia is also related to anxiety, as having untreated anxiety can cause paranoid thoughts and feelings. Paranoid thoughts can also make you anxious. Anxiety tends to make people feel more on edge and wonder if they are in danger at any given moment, which is consistent with paranoia. OCD and anxiety produce extreme worries that can be difficult to contain, leading to paranoia.
Anxiety tends to make people feel more on edge and wonder if they are in danger at any given moment, which is consistent with paranoia. OCD and anxiety produce extreme worries that can be difficult to contain, leading to paranoia.
If, however, you can address your OCD and/or anxiety, your paranoia should begin to decrease in severity. The treatment options for all three conditions are similar. In some cases, OCD can trigger paranoia.
Because paranoia can be attributed to OCD, getting the right treatment for your OCD should help to resolve your issues with paranoia too.
Some of the most common treatment options for OCD include:
Cognitive-behavioral therapy
Cognitive-behavioral therapy, or CBT, is a type of psychotherapy that involves discussions with a trained therapist about your thought patterns and compulsive behaviors. Your therapist may ask questions about why you think you feel or think certain things, and they may help you develop new coping strategies when you feel your thoughts getting out of hand.
CBT for OCD² often also includes exposure and response prevention (ERP), which involves facing your fears in a safe and controlled environment, so you can eventually overcome them.
Medication
Medications can also prove helpful for OCD, especially if CBT is too difficult at first. Antidepressants can help slow your mind and lessen some of the obsessive thoughts you experience, which can make you more open and available to CBT and ERP.
Your doctor may start you off on a small dose and gradually increase it until you see results, or you may have to try a few different medications until you find the one that works best for you. It can take several weeks to feel the effects of medications, but they can make a big difference in OCD symptoms over time.
Support groups
Support groups can provide a space for people with OCD to come together and share their experiences. They also offer a space where people with the condition can share different strategies that have helped them cope and seek advice from their peers about how to deal with certain situations.
Talk to your doctor or therapist about joining a support group near you, or check the International OCD Foundation's support group database.³
If you believe you have OCD, scheduling an appointment to talk with your doctor may be helpful. If your symptoms have begun to interfere with your work, school, or home life, including difficulties maintaining relationships, you should see a doctor immediately.
If you are noticing more paranoid thoughts, regardless of OCD, it may be helpful to speak with your doctor about your symptoms. They may be able to refer you to a specialist that can run more evaluations and offer treatment options.
OCD is a challenging condition that can make life incredibly complicated for the person suffering from it, as well as the loved ones trying to support them. With proper treatment, people with OCD can overcome their fears, obsessions, and compulsions, and they can still live happy and fulfilling lives. If you think you or a loved one may be experiencing OCD or paranoia, you should speak to a doctor to discuss your concerns.
Is it Anxiety, OCD, or Psychosis?
Recently someone asked me a question regarding the relationship between anxiety and paranoia. They reported feeling paranoid and were wondering if treatment for anxiety would help them feel better. Being paranoid means very different things to people with anxiety, Obsessive-Compulsive Disorder (OCD), or psychosis and it's helpful to know the difference.
What does paranoia mean?
Sometimes people use the word paranoia to mean someone is worried, preoccupied, or fearful of something happening. Other times paranoia is used to describe a mental illness where someone has lost touch with reality.
Let's get a few definitions out of the way thanks to the Merriam-Webster dictionary.
Paranoia:
1. Mental illness characterized by systematized delusions of persecution or grandeur usually without hallucinations
2. A tendency on the part of an individual or group toward excessive or irrational suspiciousness and distrustfulness of others
Delusion:
1. Something that is falsely or delusively believed or propagated
Something that is falsely or delusively believed or propagated
2. A persistent false psychotic belief regarding the self or persons or objects outside the self that is maintained despite indisputable evidence to the contrary
Compulsion:
An irresistible persistent impulse to perform an act (such as excessive hand washing)
If you know someone who is paranoid or are curious about the best ways to provide support, download this free PDF guide: 21 Guidelines on how to help someone with psychosis
Anxiety and paranoia
People with anxiety can be worried and fearful. They may feel paranoid that something bad is going to happen but they are not psychotic. Their anxious response may be out of proportion to the risk of the feared event but that doesn't mean they are delusional.
A person with anxiety has worries that are grounded in reality. This means that what they are worried about COULD happen even though it may be unlikely (or even highly unlikely) to happen.
Examples of paranoia: Anxiety and paranoia
- "I don't want to leave the house because I'm paranoid that I may need a bathroom. I won't be able to find one and will have an accident."
- "I'm paranoid I have germs and I'm going to spread them. I have to wash my hands before and after I touch anything."
- "I'm so paranoid about losing the keys I've hidden copies all around."
- "I installed an alarm system, video camera, and deadbolt on my front door because I'm paranoid about being robbed."
- "I'm paranoid that if I go to that party everyone will stare at me and no one will talk to me. I will stand there alone looking dumb and humiliate myself."
- "I'm paranoid that if I get on a train I will have a panic attack and not be able to get off."
For people with anxiety, paranoia and fear can lead to avoidance and isolation. Anxiety can take over and control peoples lives if it isn't treated. For more information about how to manage and control anxiety read these posts:
5 Ways to Stop a Panic Attack,
Do What You are Afraid Of: Stop Letting Anxiety Control You,
Anxiety: The Best Websites, Books, and Apps to Treat It.
OCD and paranoia
This can get a bit more complicated when someone has anxiety associated with Obsessive Compulsive Disorder (OCD). With OCD, people can have fears about a bad thing happening if they don't do a particular action (ie. their compulsion). The link between the two events may be illogical and not reality-based but the person is not psychotic. A person with OCD has not lost touch with reality even if the things they worry about aren't always rational.
Someone with OCD knows that following a regimented routine to wash dishes will not really prevent a loved one from getting in a car accident. They know it makes no sense but the anxiety is too intense for them to easily stop their ritual.
OCD is a "disease of doubt" where people feel they can't quite trust their brains. They often think "What if I didn't actually check it correctly? What if I thought I did but I looked at the wrong knob?"
It doesn't matter if they already rechecked it 10 or 20 times, some people with OCD will continue to feel anxious they left a stove on, the door unlocked, or the car running.
Despite the strength of these worries, people with OCD know that the obsessions and compulsions are irrational. However, just knowing they aren't real doesn't mean a person can stop them without getting treatment.
Examples of paranoia: OCD and paranoia
- They may convince themselves they ran over someone on the way to work and retrace their drive for hours. Unable to eliminate the worry, they may later scour the news for any reports of a hit and run or even call the police to ask if anyone was hit.
- "If I don't tap this object 4 times and start walking with my left foot first something bad may happen. A train may crash."
- "If I don't look at that sculpture first when I walk in the room and cross myself 3 times, someone in my family may get cancer and it will be my fault."
Psychosis and paranoia
Psychotic paranoia is a worry that is not grounded in reality. The thoughts are delusional and cannot possibly happen. The reasoning may be bizarre and illogical.
The reasoning may be bizarre and illogical.
A person with psychotic paranoia isn't aware their thoughts are not real. It is not helpful to tell them they don't make sense or argue with them that it cannot happen.
Psychosis can be terrifying. Some people with paranoia feel constantly under attack and scrutiny. Everything feels unsafe. They may feel close family members have been replaced with imposters, or even their own bodies are being controlled by outside entities.
It can be difficult to know the best way to support someone who is in the midst of psychosis. I put together a list of 21 recommendations to keep communication lines open and increase the chance to be helpful.
Get your free PDF: 21 Guidelines on how to help someone with psychosis
Examples of paranoia: Psychosis and paranoia
- "There are people breaking into my house every night and sprinkling dust all over my house to poison me."
- "My skin is being peeled off in my sleep by aliens and replaced by other peoples skin.
 "
" - "The government is trying to capture and kill me. They have implanted me with tracking devices so I cannot escape. Everywhere I go there is someone following me. They are listening to us right now."
- "The wiring in my house is set to a particular frequency that causes my food to spoil."
- "My body was replaced by someone else's body that I don't recognize."
Paranoia, Fear, and Worry
Paranoia can be upsetting and scary regardless if the source is anxiety, OCD, or psychosis. If you are struggling to overcome paranoia, fear, and worry; seek help from your psychiatric physician. Together you can come up with a treatment plan, find a way to help feel more at peace, and free yourself from the limitations set on your life because of the fear.
Get my future articles emailed directly to you by signing up here. To submit your questions, ideas, find resources, or to simply learn more about optimizing mental health visit my blog.
Looking for additional mental health resources? Visit the Mental Health Bookstore to see a list of doctor-recommended books on many different health topics.
A version of this article was first published here, on the blog of Dr. Melissa Welby
OCD: what is obsessive-compulsive mental disorder, diagnosis, treatment
In our time, obsessive-compulsive mental disorder is faced by those who knew this disease only by hearsay. Surprisingly, psychologists note that many OCD patients can find advantages in their illness. Still, it is better to diagnose the disease and try to cope with it. The statistics are disappointing - up to 3% of the world's population is faced with a violation.
What is OCD (obsessive compulsive disorder)? nine0005
OCD, or obsessive-compulsive disorder, is a mental disorder characterized by obsessive thoughts (obsessions) and actions (compulsions). Striking examples include the desire for perfect cleanliness, the fear of catching various diseases, a manic attachment to certain rituals (for example, pressing the doorbell three times, washing hands after each handshake, etc. ).
).
Often, the manifestation of obsessive-compulsive disorder is accompanied by bodily harm to oneself or other people. It is important to diagnose the disease in time so that it does not develop into a pathology. nine0003
Obsessive-compulsive disorder is also called obsessive-compulsive disorder. The disease can be chronic, episodic or progressive. Equally, the disease is present in both men and women. Sometimes the patient himself understands that his thoughts in their manifestation are absurd, and the behavior that follows them is very ineffective. But resisting them is useless. Suppressing these actions only increases the anxiety state.
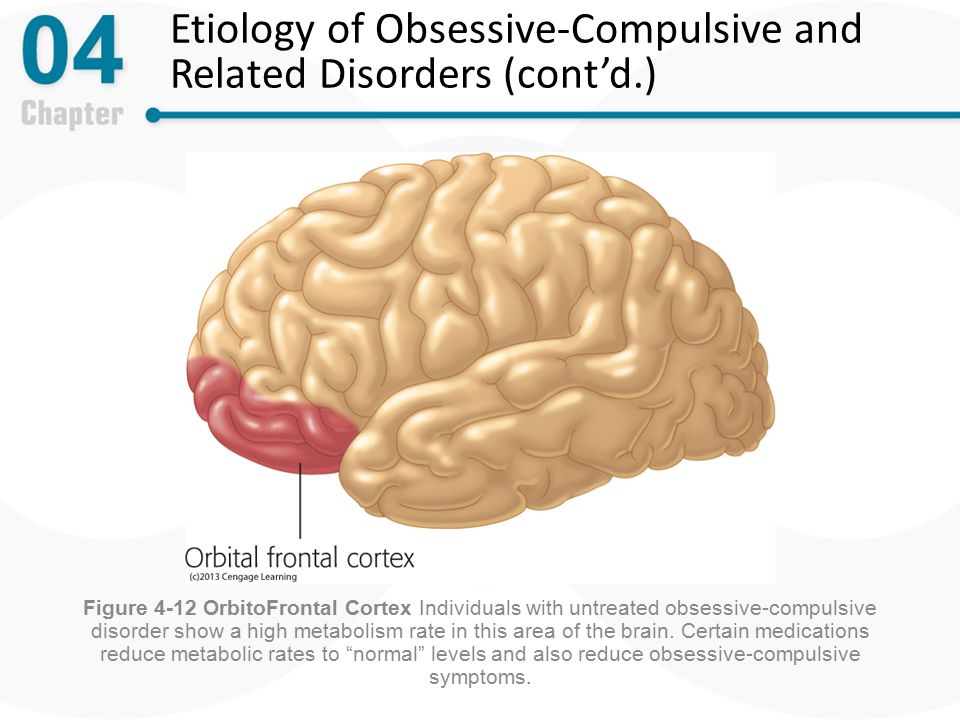
If we consider the disease from the side of physiology, then it leads to functional disorders in the following parts of the brain: nine0003
- basal ganglia;
- frontal part;
- caudate nucleus;
- amygdala.
The severity of obsessive-compulsive personality disorder in patients can vary and most often depends on the presence of stressful situations in a person's life. Violation can change life for the worse, reduce communication with society. A distinctive feature of obsession can be considered the absence of rationalism, and compulsions - that they cannot be abandoned. nine0003
Violation can change life for the worse, reduce communication with society. A distinctive feature of obsession can be considered the absence of rationalism, and compulsions - that they cannot be abandoned. nine0003
Patients, realizing their situation, are afraid of going crazy, they begin to worry about their relatives, about their own and their safety. In practice, such neuroses do not lead to serious consequences or mental disorders, and aggressive thoughts do not lead to subsequent actions.
This is what distinguishes a person with OCD from mentally deranged or hallucinating patients. A patient with OCD has the following symptoms:
- high intelligence;
- adequate thinking; nine0016
- conscientiousness and anxiety;
- high sense of responsibility;
- pedantry;
- desire to be the best.
Symptoms of obsessive-compulsive disorder
The most obvious symptoms include the obsessive and compulsive disorders already mentioned, that is, obsessive thoughts and a manic desire to perform any action. Thoughts can manifest as images, delusional ideas, inexplicable drives. Obsessive-compulsive disorder and its symptoms are observed in the form of the inability to make decisions regarding everyday situations. nine0003
Thoughts can manifest as images, delusional ideas, inexplicable drives. Obsessive-compulsive disorder and its symptoms are observed in the form of the inability to make decisions regarding everyday situations. nine0003
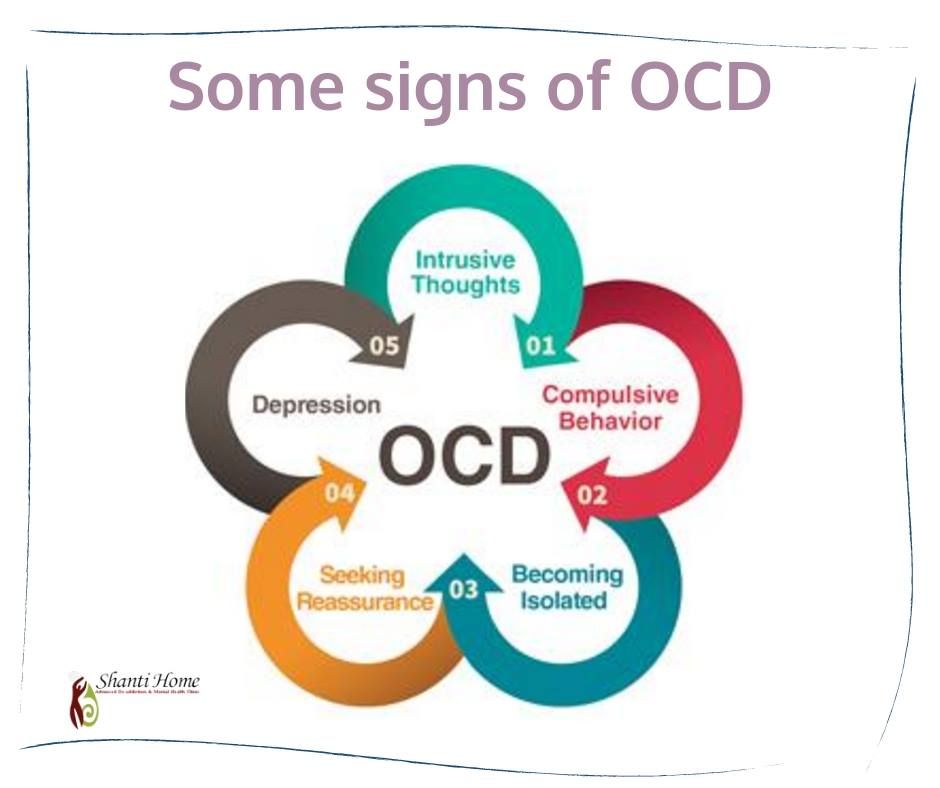
Of the main signs of OCD, the following can be distinguished: obsessive-compulsive disorder:
- intrusive thoughts;
- anxiety and various fears;
- the same rituals that a person performs daily.
Among the mental symptoms in patients, the following are observed:
- fear of catching an infection;
- causeless anxiety;
- maniacal desire for order and cleanliness; nine0016
- excessive superstition.
With OCD, the patient appropriates all incoming thoughts, in contrast to the disease of a split personality, when a person hears "foreign" voices.
These actions themselves do not bring pleasure to a person, but they can reduce the level of anxiety and stress. This does not last long and after a while the obsession returns, a phobia sets in and everything starts in a circle. Outwardly, compulsions can resemble ordinary work, for example, a person lays out things, constantly cleans the house, although the house can be perfectly clean anyway. nine0003
This does not last long and after a while the obsession returns, a phobia sets in and everything starts in a circle. Outwardly, compulsions can resemble ordinary work, for example, a person lays out things, constantly cleans the house, although the house can be perfectly clean anyway. nine0003
Sometimes the manifestation of obsessive-compulsive disorder manifests itself physically. A person does not sleep well, he has headaches, heartaches, blinking becomes more frequent, nervous tics and convulsions occur, pressure rises, appetite is disturbed, and sexual desire decreases.
The manifestations of obsessive-compulsive disorder are constant and manic in nature, they cause inconvenience to a person.
Causes of obsessive-compulsive disorder nine0005
Scientists are still conducting various studies to establish the exact causes of the violation. But there are no exact data in this area. Despite this, it is customary to single out several areas that can cause obsessive-compulsive disorder syndrome, the reasons are:
But there are no exact data in this area. Despite this, it is customary to single out several areas that can cause obsessive-compulsive disorder syndrome, the reasons are:
- Psychological. OCD occurs when a person develops aggression towards an object. It also includes stressful situations that provoke a violation. The state appears as an exit of emotions, as a marker of anxiety. nine0016
- Biological. The disorder is the result of a disease of the brain or nervous system. It can be provoked by various kinds of injuries, hormonal disorders or anatomical features.
- Genetic. The disease can be inherited.
- Sociological. They arise as a response of the body to external factors.
- Exogenous. They manifest themselves in the form of traumatic situations that can happen at work or in personal life. nine0023
- "Mental chewing gum" or rumination. When a person sets himself unsolvable questions and tasks.
- Arrhythmia. Obsession, which is manifested by the constant re-reading of various objects.
- Intrusive reproduction. It manifests itself in the painful formation of a person to remember everything that is not related to a given period of time, event or conversation. nine0016
- Onomatomania. An obsessive desire to remember all the words, titles and names.
- Misunderstanding. At this stage, intrusive thoughts are mild. A person feels a violation of the habitual consciousness, anxiety, cannot understand the nature of the occurrence of manic impulses.

- Understanding. Accompanied by a visit to a specialist. The patient understands that disturbances are present, but cannot yet realize the changes. Often at this stage there is hope that the state will change and life will return to its previous course.
- Adoption. The patient comes to terms with the mental disorder, agrees to treatment. He ceases to regard obsession and compulsion as a temporary condition. At this stage, it is important to fully interact with the attending physician, to obtain comprehensive information about the disease. nine0016
- Suicidal behavior.
 In a severe stage, the patient may commit suicide or try to cause physical harm to another person.
In a severe stage, the patient may commit suicide or try to cause physical harm to another person. - From constant contact with soap and detergents that a person uses so actively, dermatitis can develop.
- Possible problems in the social sphere. Inability to communicate with society. A person falls out of society - he does not have a hobby, he is afraid to appear in public places, he cannot concentrate on work. nine0016
- There are conflicts with relatives and friends. Some people with OCD are unable to start a family and have difficulty raising children.
- The patient has intrusive thoughts. The frequency of their appearance in this case exceeds the permissible norm for two weeks.
- Obsessive thoughts and actions qualitatively worsen the life of the patient. nine0016
- The implementation of obsessions and compulsions causes discomfort in the patient.
- Actions and thoughts occur regularly and frighten the patient with their frequency.
- There is no specificity in thoughts and actions, their nature is associated with anxiety, generates stress in a person, internal tension.

- Primary. A person learns about a genetic predisposition, corrects his behavior with the help of a specialist, uses various methods to prevent the occurrence of a violation. Primary prevention also includes educational methods.
- Secondary. Used to prevent recurrence of OCD. In this case, you will also need the help of a specialist to correct behavior, calm and sufficient sleep, abstinence from alcoholic beverages and drugs. You can also follow a special diet that is aimed at producing serotonin. nine0016
- Erich Fromm, "The human soul, its capacity for good and evil"
- Karen Horney, Neurosis and Personal Growth: The Struggle for Self-Realization
- Goldsmith G.
 N. Approaches to the treatment of narcissistic disorders: Kohut and Kernberg nine0016
N. Approaches to the treatment of narcissistic disorders: Kohut and Kernberg nine0016 - Otto Friedmann Kernberg, “Severe personality disorders. Psychotherapy Strategies»
- Dadasheva K.N. 1 , Agafonov B.V. 2 , Dadasheva M.N. 1 , Podrezova L.A. GBUZ MO MONIKI them. M.F. Vladimirsky, Moscow - neurasthenic syndrome in general medical practice. The possibilities of therapy.
- McWilliams N., reflections on schizoid dynamics
- T.A. Solokhina, prof. V.S. Yastrebov, L.S. Shevchenko - A model for organizing socio-psychological care for patients with schizophrenia. nine0016
- Recurring thoughts that make you feel anxious - "obsessions" or "obsessions". It can be unpleasant words or phrases, mental pictures or doubts.
- The things you do over and over again that help you feel less anxious are 'compulsions'. You can try to correct or "neutralize" thoughts by counting over and over again, saying a special word, or performing certain rituals. nine0016
- In some cases, OCD is inherited, so sometimes the disorder can run in the family.
- Stressful life events cause OCD in about a third of cases.
- Life changes in which you have to take on more responsibility, such as puberty, the birth of a child, or a new job. nine0016
- If you have OCD and it lasts for some time, you may develop an imbalance of serotonin (also known as 5HT), a brain neurotransmitter.
- You are a neat, pedantic, methodical person - but you go too far in this.
- If you have extremely high standards of morality and responsibility, you may feel especially bad about having unpleasant thoughts. To the point where you start to be wary and keep a close eye on them, which makes them even more likely to appear. nine0016
- If you regularly force yourself to think the thoughts that are bothering you, you will be able to control them better. You can write them down - on a recorder or on paper, and then listen to or reread.
 You should do this regularly, for about half an hour every day. At the same time, try to resist compulsive behavior.
You should do this regularly, for about half an hour every day. At the same time, try to resist compulsive behavior. - Do not use alcohol to control your anxiety.
- If your intrusive thoughts are about your faith or religion, discuss them with your religious leader to help you understand if OCD is a problem. nine0016
- Try using a self-help book.
- Initially, you can choose either CBT (up to 10 hours in contact with a therapist) or medication (up to 12 weeks). If you do not get better, you should try both treatments together. nine0016
- If you have severe OCD, it is best to use medication and CBT together from the start.
- Taking medication alone will help you if you don't feel able to face the anxiety that Exposure and response prevention will cause, but the chances of OCD coming back are higher - about one in two compared to one in four with psychotherapy treatment. The medicine must be taken for about a year and is obviously not ideal during pregnancy or breastfeeding. nine0016
Disease pathogenesis
Despite various theories of the occurrence of OCD, the pathogenesis of obsessive-compulsive disorder has a well-defined nature of occurrence, although not fully understood. These structures of the body interact with each other through serotonin. The lack of this hormone is due to the heightened effect of neurons on the cerebral cortex. This provokes a blockage of the nerve impulse, which does not reach the next neuron.
These structures of the body interact with each other through serotonin. The lack of this hormone is due to the heightened effect of neurons on the cerebral cortex. This provokes a blockage of the nerve impulse, which does not reach the next neuron.
Classification and stage of development of ROC nine0005
Obsessive-compulsive disorder has different degrees of severity and manifests itself in the following stages:
There are several variants of manifestation. For example, they can be expressed in simple symbolic actions. The patient can put a certain prohibition on performing actions, for example, counting steps for failure or success. They can also be expressed in physical actions aimed at self-harm: pulling out body hair and eating it. As a rule, an accurate diagnosis requires complete immersion in the disease in order to understand whether it is different from other mental disorders. nine0003
The patient can put a certain prohibition on performing actions, for example, counting steps for failure or success. They can also be expressed in physical actions aimed at self-harm: pulling out body hair and eating it. As a rule, an accurate diagnosis requires complete immersion in the disease in order to understand whether it is different from other mental disorders. nine0003
The manifestation of obsessive-compulsive disorder is equally observed in both men and women. It is much less common in children, although it is believed that the first signs may appear before the age of 11 years.
Obsessive-compulsive disorder is most common in adolescents. Studies have shown that the disorder affects mainly adolescents aged 11-17 years. Up to 85% of all patients are adolescents.
Each person, as a rule, goes through three stages that are inherent in OCD: nine0003
The obsessive-compulsive disorder scale was introduced to determine the stage of the disorder. It's called the Yale-Brown scale. It was developed at Yale University under the direction of Wayne Goodman. This manual is accepted throughout the world as a traditional method for identifying the stage of OCD.
Complications of obsessive-compulsive disorder
In obsessive-compulsive disorder, the consequences can be irreversible and cover completely different areas of life: nine0003
When to see a doctor?
At the slightest suspicion of the listed symptoms, you should immediately contact a specialist. Often a person with OCD is not able to independently realize and accept that his behavior and way of thinking has changed.
If you have problems with society and loved ones, then you should listen to their advice and make an appointment with a doctor. nine0003
Diagnostics
The violation is included in the International Classification of Diseases (ICD-10). Diagnosis of obsessive-compulsive disorder includes a mandatory visit to a specialist with subsequent diagnosis.
When making a diagnosis, the doctor relies on the following criteria:
The diagnosis is made if the patient has obsessive thoughts or ideas. They adopt an image that prompts them to impulsively perform some kind of action. nine0003
There is a mixed form of the disorder where the patient is equally haunted by obsessive thoughts and there is a manic execution of compulsions.
Treatment
Comprehensive treatment of obsessive-compulsive disorder includes an individual visit to a psychotherapist - a specialist identifies the causes of the disease, helps to recognize the signs of an obsessive-compulsive disorder, and accepts that the patient has OCD. The next step is the CBT method (Cognitive Behavioral Therapy). The psychotherapist teaches the patient to monitor the appearance of OCD, find ways to change negative thoughts, displace them and change them into optimistic actions. Medications in this case are prescribed with the consent of the patient. nine0003
Antidepressants and anxiolytics (drugs that relieve anxiety) are prescribed as medicines.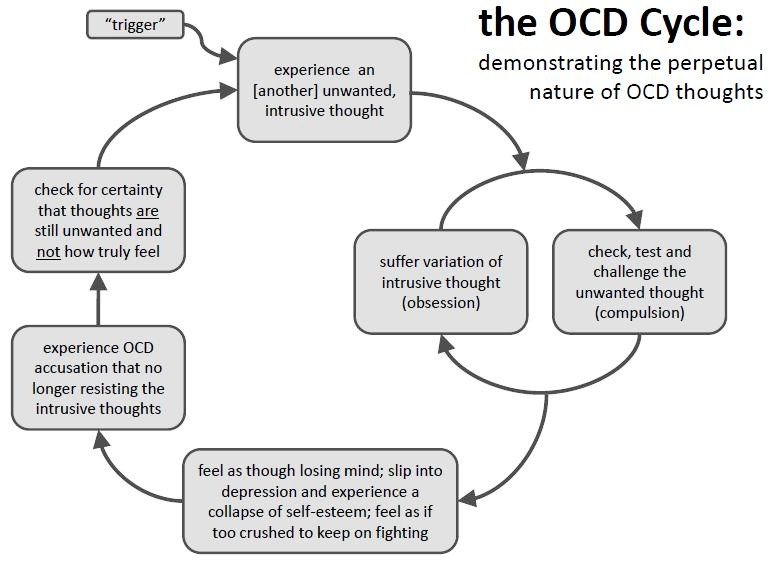 Treatment with sedatives is also possible, which helps relieve depressive thoughts, remove depressed mood.
Treatment with sedatives is also possible, which helps relieve depressive thoughts, remove depressed mood.
Therapy for obsessive-compulsive disorder may include biofeedback therapy. Sensors are installed on the patient, with the help of which breathing, muscle work and heart rate are monitored. This technique helps to control the condition and further cope with emerging obsessive thoughts and negative emotions. nine0003
You can get treatment from private practitioners, but it is better to choose clinics that specialize in the treatment of mental disorders. Doctors with many years of experience work in such institutions, who have been practicing and treating obsessive-compulsive disorder for many years.
+7 (495) 121-48-31
Prevention and recommendations for illness
OCD is typical for people who have any other mental disorders. Also, with a stable calm state of patients diagnosed with OCD, its recurrence is possible. Since the specific cause of the violation has not been established, then prevention is advisory in nature. nine0003
nine0003
For obsessive-compulsive disorder, recommendations in terms of prevention can be primary and secondary:
If any signs appear, it is better to consult a doctor, and not try to come to terms with unfamiliar conditions. It is useful to get comprehensive information about OCD from people who have suffered this disorder.
References:
Obsessive-Compulsive Disorder (OCD) - key facts in English
Obsessive-Compulsive Disorder (OCD)
See our disclaimer that applies to all translations available on this site.
What is obsessive-compulsive disorder?
At times we can all get hung up on things, but if:
Terrible thoughts come compulsively into your head, even if you try to get rid of them,
You have to count or touch things over and over again , or repeating some actions, for example, washing hands,
You may have obsessive-compulsive disorder (OCD).
Who gets OCD?
About 1 in 50 people will experience OCD at some point in their lives. Equally, it can be men and women. In the UK, their number is about 1 million people. OCD usually begins in adolescence or early adulthood. Symptoms of OCD may get worse or worse over time, but often people don't seek help for many years.
What are the signs and symptoms of obsessive-compulsive disorder?
What are the causes of OCD?
Many factors can play a role in the occurrence of OCD. One or more of the following could explain why you or someone you know has OCD.
How to help yourself
Professional help Various types of psychotherapy
Exposure and response prevention
Helps stop the mutual reinforcing of compulsive behavior and anxiety.
We know that if you stay in a stressful situation long enough, you will gradually get used to it and the anxiety will go away. In this way, you gradually face the situation that you fear (exposure), but stop yourself from doing your usual compulsive rituals of checking or clearing (avoiding a response) and wait for your anxiety to go away. nine0003
Cognitive therapy
Instead of getting rid of your thoughts, cognitive therapy helps you change how you react to them. It specifically targets unrealistic self-critical thoughts. Useful if you have intrusive thoughts but are not performing any rituals or activities to reduce your anxiety. Can be used with Exposure and Response Prevention.
It specifically targets unrealistic self-critical thoughts. Useful if you have intrusive thoughts but are not performing any rituals or activities to reduce your anxiety. Can be used with Exposure and Response Prevention.
Antidepressant treatment
Even if you are not depressed, SSRI (Selective Serotonin Reuptake Inhibitor) antidepressants can help. They may be used alone or with cognitive behavioral therapy for moderate to severe OCD. If the medicine doesn't help at all after three months of taking it, you can change it to another SSRI antidepressant or a medicine called Clomipramine (Anafranil). nine0003
How effective is the treatment?
Exposure and prevention of response
About three out of four people who completed this therapy did well, but one in four will return symptoms and require additional treatment. Approximately one in four people refuse to try this type of cognitive-behavioral therapy or do not complete it - they find it too hard for them.
Medications
About six out of 10 people feel better with medication and their symptoms lessen by about half. Medications do help prevent OCD from returning for as long as they are taken, even years later. Unfortunately, about half of those who stop taking the drug return symptoms within a few months afterward. This is less likely when drug treatment is combined with cognitive behavioral therapy. nine0003
Which approach is best for me?
Mild OCD
Exposure and response prevention can be done without professional help. This method is effective and has no side effects, but you will feel more anxious for a while. You must be motivated and ready for hard work. Cognitive therapy and drug treatment are equally effective.
Moderate or severe OCD
The original page produced by the RCPsych Public Education Editorial Board. Series Editor: Dr Philip Timms.
Information about treatments can change rapidly and the College updates its mental health information pages regularly.
Translated by: Maria Kadmenskaya
Translation date: August 2011
(c) February 2013. Royal College of Psychiatrists. This booklet may be downloaded, printed, copied and distributed free of charge provided that no profit is made from its use and that the Royal College of Psychiatrists is credited and credited as the author.