Five stages of depression
SAMHSA’s National Helpline | SAMHSA
Your browser is not supported
Switch to Chrome, Edge, Firefox or Safari
Main page content
-
SAMHSA’s National Helpline is a free, confidential, 24/7, 365-day-a-year treatment referral and information service (in English and Spanish) for individuals and families facing mental and/or substance use disorders.
Also visit the online treatment locator.
SAMHSA’s National Helpline, 1-800-662-HELP (4357) (also known as the Treatment Referral Routing Service), or TTY: 1-800-487-4889 is a confidential, free, 24-hour-a-day, 365-day-a-year, information service, in English and Spanish, for individuals and family members facing mental and/or substance use disorders.
This service provides referrals to local treatment facilities, support groups, and community-based organizations.
Also visit the online treatment locator, or send your zip code via text message: 435748 (HELP4U) to find help near you. Read more about the HELP4U text messaging service.
The service is open 24/7, 365 days a year.
English and Spanish are available if you select the option to speak with a national representative. Currently, the 435748 (HELP4U) text messaging service is only available in English.
In 2020, the Helpline received 833,598 calls. This is a 27 percent increase from 2019, when the Helpline received a total of 656,953 calls for the year.
The referral service is free of charge. If you have no insurance or are underinsured, we will refer you to your state office, which is responsible for state-funded treatment programs. In addition, we can often refer you to facilities that charge on a sliding fee scale or accept Medicare or Medicaid. If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
In addition, we can often refer you to facilities that charge on a sliding fee scale or accept Medicare or Medicaid. If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
The service is confidential. We will not ask you for any personal information. We may ask for your zip code or other pertinent geographic information in order to track calls being routed to other offices or to accurately identify the local resources appropriate to your needs.
No, we do not provide counseling. Trained information specialists answer calls, transfer callers to state services or other appropriate intake centers in their states, and connect them with local assistance and support.
-
Suggested Resources
What Is Substance Abuse Treatment? A Booklet for Families
Created for family members of people with alcohol abuse or drug abuse problems. Answers questions about substance abuse, its symptoms, different types of treatment, and recovery. Addresses concerns of children of parents with substance use/abuse problems.
Answers questions about substance abuse, its symptoms, different types of treatment, and recovery. Addresses concerns of children of parents with substance use/abuse problems.It's Not Your Fault (NACoA) (PDF | 12 KB)
Assures teens with parents who abuse alcohol or drugs that, "It's not your fault!" and that they are not alone. Encourages teens to seek emotional support from other adults, school counselors, and youth support groups such as Alateen, and provides a resource list.After an Attempt: A Guide for Taking Care of Your Family Member After Treatment in the Emergency Department
Aids family members in coping with the aftermath of a relative's suicide attempt. Describes the emergency department treatment process, lists questions to ask about follow-up treatment, and describes how to reduce risk and ensure safety at home.Family Therapy Can Help: For People in Recovery From Mental Illness or Addiction
Explores the role of family therapy in recovery from mental illness or substance abuse.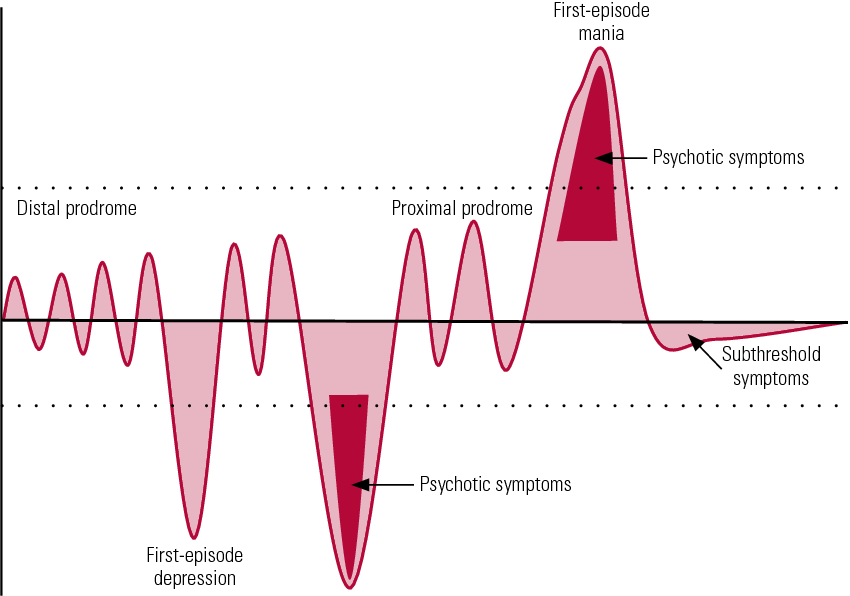 Explains how family therapy sessions are run and who conducts them, describes a typical session, and provides information on its effectiveness in recovery.
Explains how family therapy sessions are run and who conducts them, describes a typical session, and provides information on its effectiveness in recovery.For additional resources, please visit the SAMHSA Store.
Last Updated: 08/30/2022
Alcohol, Tobacco, and Other Drugs
Your browser is not supported
Switch to Chrome, Edge, Firefox or Safari
Misusing alcohol, tobacco, and other drugs can have both immediate and long-term health effects.The misuse and abuse of alcohol, tobacco, illicit drugs, and prescription medications affect the health and well-being of millions of Americans. NSDUH estimates allow researchers, clinicians, policymakers, and the general public to better understand and improve the nation’s behavioral health. These reports and detailed tables present estimates from the 2021 National Survey on Drug Use and Health (NSDUH).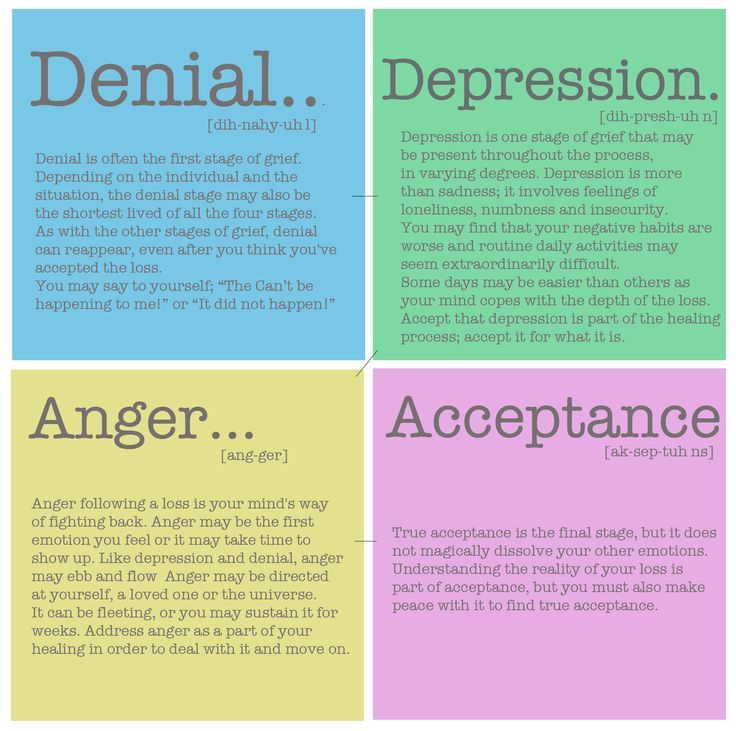
Alcohol
Data:
- Among the 133.1 million current alcohol users aged 12 or older in 2021, 60.0 million people (or 45.1%) were past month binge drinkers. The percentage of people who were past month binge drinkers was highest among young adults aged 18 to 25 (29.2% or 9.8 million people), followed by adults aged 26 or older (22.4% or 49.3 million people), then by adolescents aged 12 to 17 (3.8% or 995,000 people). (2021 NSDUH)
- Among people aged 12 to 20 in 2021, 15.1% (or 5.9 million people) were past month alcohol users. Estimates of binge alcohol use and heavy alcohol use in the past month among underage people were 8.3% (or 3.2 million people) and 1.6% (or 613,000 people), respectively. (2021 NSDUH)
- In 2020, 50.0% of people aged 12 or older (or 138.5 million people) used alcohol in the past month (i.e., current alcohol users) (2020 NSDUH)
- Among the 138.5 million people who were current alcohol users, 61.6 million people (or 44.
 4%) were classified as binge drinkers and 17.7 million people (28.8% of current binge drinkers and 12.8% of current alcohol users) were classified as heavy drinkers (2020 NSDUH)
4%) were classified as binge drinkers and 17.7 million people (28.8% of current binge drinkers and 12.8% of current alcohol users) were classified as heavy drinkers (2020 NSDUH) - The percentage of people who were past month binge alcohol users was highest among young adults aged 18 to 25 (31.4%) compared with 22.9% of adults aged 26 or older and 4.1% of adolescents aged 12 to 17 (2020 NSDUH)
- Excessive alcohol use can increase a person’s risk of stroke, liver cirrhosis, alcoholic hepatitis, cancer, and other serious health conditions
- Excessive alcohol use can also lead to risk-taking behavior, including driving while impaired. The Centers for Disease Control and Prevention reports that 29 people in the United States die in motor vehicle crashes that involve an alcohol-impaired driver daily
Programs/Initiatives:
- STOP Underage Drinking interagency portal - Interagency Coordinating Committee on the Prevention of Underage Drinking
- Interagency Coordinating Committee on the Prevention of Underage Drinking
- Talk.
 They Hear You.
They Hear You. - Underage Drinking: Myths vs. Facts
- Talking with your College-Bound Young Adult About Alcohol
Relevant links:
- National Association of State Alcohol and Drug Abuse Directors
- Department of Transportation Office of Drug & Alcohol Policy & Compliance
- Alcohol Policy Information Systems Database (APIS)
- National Institute on Alcohol Abuse and Alcoholism
Tobacco
Data:
- In 2020, 20.7% of people aged 12 or older (or 57.3 million people) used nicotine products (i.e., used tobacco products or vaped nicotine) in the past month (2020 NSDUH)
- Among past month users of nicotine products, nearly two thirds of adolescents aged 12 to 17 (63.1%) vaped nicotine but did not use tobacco products. In contrast, 88.9% of past month nicotine product users aged 26 or older used only tobacco products (2020 NSDUH)
- Tobacco use is the leading cause of preventable death, often leading to lung cancer, respiratory disorders, heart disease, stroke, and other serious illnesses.
 The CDC reports that cigarette smoking causes more than 480,000 deaths each year in the United States
The CDC reports that cigarette smoking causes more than 480,000 deaths each year in the United States - The CDC’s Office on Smoking and Health reports that more than 16 million Americans are living with a disease caused by smoking cigarettes
Electronic cigarette (e-cigarette) use data:
- In 2021, 13.2 million people aged 12 or older (or 4.7%) used an e-cigarette or other vaping device to vape nicotine in the past month. The percentage of people who vaped nicotine was highest among young adults aged 18 to 25 (14.1% or 4.7 million people), followed by adolescents aged 12 to 17 (5.2% or 1.4 million people), then by adults aged 26 or older (3.2% or 7.1 million people).
- Among people aged 12 to 20 in 2021, 11.0% (or 4.3 million people) used tobacco products or used an e-cigarette or other vaping device to vape nicotine in the past month. Among people in this age group, 8.1% (or 3.1 million people) vaped nicotine, 5.4% (or 2.1 million people) used tobacco products, and 3.
 4% (or 1.3 million people) smoked cigarettes in the past month. (2021 NSDUH)
4% (or 1.3 million people) smoked cigarettes in the past month. (2021 NSDUH) - Data from the Centers for Disease Control and Prevention’s 2020 National Youth Tobacco Survey. Among both middle and high school students, current use of e-cigarettes declined from 2019 to 2020, reversing previous trends and returning current e-cigarette use to levels similar to those observed in 2018
- E-cigarettes are not safe for youth, young adults, or pregnant women, especially because they contain nicotine and other chemicals
Resources:
- Tips for Teens: Tobacco
- Tips for Teens: E-cigarettes
- Implementing Tobacco Cessation Programs in Substance Use Disorder Treatment Settings
- Synar Amendment Program
Links:
- Truth Initiative
- FDA Center for Tobacco Products
- CDC Office on Smoking and Health
- National Institute on Drug Abuse: Tobacco, Nicotine, and E-Cigarettes
- National Institute on Drug Abuse: E-Cigarettes
Opioids
Data:
- Among people aged 12 or older in 2021, 3.
 3% (or 9.2 million people) misused opioids (heroin or prescription pain relievers) in the past year. Among the 9.2 million people who misused opioids in the past year, 8.7 million people misused prescription pain relievers compared with 1.1 million people who used heroin. These numbers include 574,000 people who both misused prescription pain relievers and used heroin in the past year. (2021 NSDUH)
3% (or 9.2 million people) misused opioids (heroin or prescription pain relievers) in the past year. Among the 9.2 million people who misused opioids in the past year, 8.7 million people misused prescription pain relievers compared with 1.1 million people who used heroin. These numbers include 574,000 people who both misused prescription pain relievers and used heroin in the past year. (2021 NSDUH) - Among people aged 12 or older in 2020, 3.4% (or 9.5 million people) misused opioids in the past year. Among the 9.5 million people who misused opioids in the past year, 9.3 million people misused prescription pain relievers and 902,000 people used heroin (2020 NSDUH)
- According to the Centers for Disease Control and Prevention’s Understanding the Epidemic, an average of 128 Americans die every day from an opioid overdose
Resources:
- Medication-Assisted Treatment
- Opioid Overdose Prevention Toolkit
- TIP 63: Medications for Opioid Use Disorder
- Use of Medication-Assisted Treatment for Opioid Use Disorder in Criminal Justice Settings
- Opioid Use Disorder and Pregnancy
- Clinical Guidance for Treating Pregnant and Parenting Women With Opioid Use Disorder and Their Infants
- The Facts about Buprenorphine for Treatment of Opioid Addiction
- Pregnancy Planning for Women Being Treated for Opioid Use Disorder
- Tips for Teens: Opioids
- Rural Opioid Technical Assistance Grants
- Tribal Opioid Response Grants
- Provider’s Clinical Support System - Medication Assisted Treatment Grant Program
Links:
- National Institute on Drug Abuse: Opioids
- National Institute on Drug Abuse: Heroin
- HHS Prevent Opioid Abuse
- Community Anti-Drug Coalitions of America
- Addiction Technology Transfer Center (ATTC) Network
- Prevention Technology Transfer Center (PTTC) Network
Marijuana
Data:
- In 2021, marijuana was the most commonly used illicit drug, with 18.
 7% of people aged 12 or older (or 52.5 million people) using it in the past year. The percentage was highest among young adults aged 18 to 25 (35.4% or 11.8 million people), followed by adults aged 26 or older (17.2% or 37.9 million people), then by adolescents aged 12 to 17 (10.5% or 2.7 million people).
7% of people aged 12 or older (or 52.5 million people) using it in the past year. The percentage was highest among young adults aged 18 to 25 (35.4% or 11.8 million people), followed by adults aged 26 or older (17.2% or 37.9 million people), then by adolescents aged 12 to 17 (10.5% or 2.7 million people). - The percentage of people who used marijuana in the past year was highest among young adults aged 18 to 25 (34.5%) compared with 16.3% of adults aged 26 or older and 10.1% of adolescents aged 12 to 17 (2020 NSDUH)
- Marijuana can impair judgment and distort perception in the short term and can lead to memory impairment in the long term
- Marijuana can have significant health effects on youth and pregnant women.
Resources:
- Know the Risks of Marijuana
- Marijuana and Pregnancy
- Tips for Teens: Marijuana
Relevant links:
- National Institute on Drug Abuse: Marijuana
- Addiction Technology Transfer Centers on Marijuana
- CDC Marijuana and Public Health
Emerging Trends in Substance Misuse:
- Methamphetamine—In 2019, NSDUH data show that approximately 2 million people used methamphetamine in the past year.
 Approximately 1 million people had a methamphetamine use disorder, which was higher than the percentage in 2016, but similar to the percentages in 2015 and 2018. The National Institute on Drug Abuse Data shows that overdose death rates involving methamphetamine have quadrupled from 2011 to 2017. Frequent meth use is associated with mood disturbances, hallucinations, and paranoia.
Approximately 1 million people had a methamphetamine use disorder, which was higher than the percentage in 2016, but similar to the percentages in 2015 and 2018. The National Institute on Drug Abuse Data shows that overdose death rates involving methamphetamine have quadrupled from 2011 to 2017. Frequent meth use is associated with mood disturbances, hallucinations, and paranoia. - Cocaine—In 2019, NSDUH data show an estimated 5.5 million people aged 12 or older were past users of cocaine, including about 778,000 users of crack. The CDC reports that overdose deaths involving have increased by one-third from 2016 to 2017. In the short term, cocaine use can result in increased blood pressure, restlessness, and irritability. In the long term, severe medical complications of cocaine use include heart attacks, seizures, and abdominal pain.
- Kratom—In 2019, NSDUH data show that about 825,000 people had used Kratom in the past month. Kratom is a tropical plant that grows naturally in Southeast Asia with leaves that can have psychotropic effects by affecting opioid brain receptors.
 It is currently unregulated and has risk of abuse and dependence. The National Institute on Drug Abuse reports that health effects of Kratom can include nausea, itching, seizures, and hallucinations.
It is currently unregulated and has risk of abuse and dependence. The National Institute on Drug Abuse reports that health effects of Kratom can include nausea, itching, seizures, and hallucinations.
Resources:
- Tips for Teens: Methamphetamine
- Tips for Teens: Cocaine
- National Institute on Drug Abuse
More SAMHSA publications on substance use prevention and treatment.
Last Updated: 01/05/2023
causes, types, stages, symptoms, signs, diagnosis, treatment in women and men
Causes
Classification
Symptoms
Complications
Diagnosis
Treatment
Depression is a common mental disorder, the main features of which are a persistent decrease in mood, problems with memory and concentration, and minimal physical activity.
The causes of such a painful condition for a person in most cases are neuropsychic shock or chronic stress. Depression can be accompanied by severe illness, sudden changes in life.
Depression can be accompanied by severe illness, sudden changes in life.
Treatment is based on the use of psychotherapeutic techniques. In some cases, it is supplemented by taking medications.
Reasons
Depending on the form, the disease is associated with external or internal factors. The causes of psychogenic reactive depression can be severe experiences, an acute psychotraumatic situation. Often, a violation develops after the loss of a loved one, loss of a job, divorce, relocation, injury.
Positively colored events, for example, finally gained wealth or popularity, can also cause upset. In this case, mental deviations are explained by the realization of a dream with the subsequent loss of the meaning of life, provided there are no other goals.
Neurotic depression is a consequence of chronic stress. In this state, it is usually not possible to establish a specific cause of experiences. A person finds it difficult to name any specific psycho-traumatic circumstance, sees his life as a whole as a series of losses and disappointments.
Depression in men often develops with regular use of alcoholic beverages, psychoactive substances.
Other risk factors for affective disorder in patients of either sex are:
- very high or extremely low financial status;
- impressionability, suspiciousness, poor resistance to stress;
- low self-esteem, a tendency to self-flagellation;
- pessimistic outlook on life;
- high psycho-emotional stress in professional activities;
- difficult childhood, psychotraumatic situations suffered at a young age;
- divorce of parents or loss of one of them, upbringing in an incomplete family, orphanage;
- the presence of mental or neurotic disorders, addictions among relatives;
- loneliness, lack of support in the family and social environment;
- economic and political instability in the country;
- physiologically determined changes in the hormonal background - the process of puberty, the postpartum period, menopause.
Endogenous depressions develop as a result of neurochemical abnormalities due to genetic mutation or aging of the body. This group of disorders includes involutional melancholia and senile depression. This form of pathology also occurs in manic-depressive psychosis, characterized by a change in the phases of mania, depression and mental stability.
The likelihood of depression in women is higher in the postpartum and menopause periods, when there is a change in the level of sex hormones, which is stressful for the body. In a young mother, neuropsychic disorders can occur with complicated childbirth, problems with breastfeeding or the health of the baby, and the appearance of excess weight.
Diseases of various organs can also be accompanied by depression. They are divided into the following groups:
- Pathologies of the cardiovascular system - myocardial infarction, hypertension, circulatory failure, heart rhythm disturbances.
- Brain damage due to stroke, neuroinfection or head trauma.
- Endocrine disorders - diabetes mellitus, hyper- or hypofunction of the thyroid gland.
- Violation of the digestive system - cirrhosis of the liver, colitis.
- Rheumatic diseases with prolonged pain syndrome - rheumatism, systemic lesions of the connective tissue, arthritis.
- Oncological processes, especially malignant neoplasms.
Classification
Depending on the severity and nature of manifestations, depression is of the following types:
- major or clinical;
- postpartum;
- atypical;
- recurrent;
- small;
- dysthymia.
Latent or "masked" depression is characterized by the absence of signs of neuropsychiatric disorders and symptoms characteristic of somatic diseases. The following options are distinguished:
- cardiology;
- abdominal;
- dermal.

Caused by an acute psycho-traumatic situation, reactive psychogenic depression proceeds in several stages:
- Denial. The psyche makes an attempt to isolate itself from the ongoing negative events, the patient stubbornly does not believe in what happened.
- Anger. Anger arises from a sense of injustice, and the search for the guilty begins.
- Trade. A person tries to negotiate in order to avoid consequences. This indicates active attempts to find a way out of the situation.
- Depression. There is a feeling of loss of control over what is happening, a feeling of powerlessness and the impossibility of correcting anything. This is accompanied by a depressed mood, apathy, laziness, sadness, pessimistic judgments.
- Acceptance. After a real assessment of the situation and the prospects that have opened up, a person resigns himself to his fate and mentally prepares for the consequences.
Symptoms
The main manifestations of the disease are united under the name "depressive triad" and include:
- a persistent decrease in mood, despair, melancholy, a sense of hopelessness for several weeks and even months;
- slowing down of thinking, problems with memorizing and analyzing information, fixation on one's own experiences;
- decreased motor activity, slowness, lethargy, prolonged stay in the same position.
The patient ceases to enjoy activities that previously brought positive emotions, becomes withdrawn and taciturn, can spend most of the day lying in bed or sitting, hunched over, bowing his head and resting his elbows on his knees. Feelings of guilt appear, self-esteem falls, suicidal thoughts arise. Fatigue is characteristic, the solution of simple everyday tasks requires great effort.
In some cases, depression may present with the following symptoms:
- nocturnal insomnia, often associated with drowsiness during the day;
- decreased appetite and weight loss;
- increased heart rate;
- constipation;
- dilated pupils;
- loss of sexual desire;
- menstrual disorders;
- intense pain in different parts of the body without objective causes;
- aggressive behavior, attacks and accusations against other people;
- dryness and flabbiness of the skin, the appearance of wrinkles;
- increased hair loss, brittle nails.

With endogenous depression, the intensity of symptoms peaks in the morning, gradually weakening during the day, and the manifestations of psychogenic affective disorders increase in the evening. A feature of postnatal depression is a decrease in the mother's interest in the child, irritation from the need to take care of him.
Clinical depression is severe, including all of the triad and many additional symptoms. The small form is characterized by only a couple of signs of the disease that persist for two or more weeks. The atypical variant proceeds with increased appetite, drowsiness, emotional arousal, and anxiety.
Recurrent depression is characterized by a short duration of several days with a monthly recurrence. Seasonal affective disorder is associated with the change of seasons, the symptoms begin and end at about the same time interval. With dysthymia, the mood is steadily reduced for several years, but negative emotions and experiences do not reach the intensity characteristic of clinical depression.![]()
Complications
The greatest danger is suicidal thoughts arising from the disease. They can provoke appropriate actions and lead to tragic consequences. With postpartum depression, a woman can harm not only herself, but also the child. In order to alleviate symptoms, the patient may resort to taking alcohol, drugs.
Diagnostics
With somatogenic or latent forms of the disease, a person can seek help from a general practitioner, cardiologist, neurologist, gastroenterologist and other doctors. In the case of psychogenic affective disorder, self-referral to a psychologist is possible. It is important that these specialists promptly refer the patient to a psychotherapist who diagnoses depression. It detects the disease by questioning the patient, during which complaints and symptoms are clarified, possible causative factors. Based on the data received, the doctor will tell you how to get out of depression as soon as possible and draw up a treatment plan.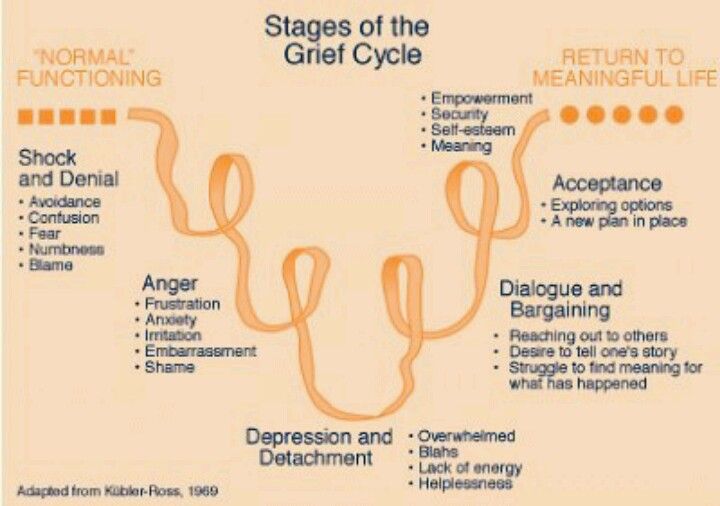
Special tests for depression are carried out to determine the severity of the process. They include standardized tasks designed and tested by experts. Thus, personal needs, character traits, emotional responses, intelligence levels, anxiety and stress are studied. The Beck Depression Scale with a test questionnaire is often used to identify and assess symptoms of the disease.
Treatment
With a mild course of the disease, it is possible to undergo only a course of psychotherapy without the use of medications. Additionally, massage, hydrotherapy and exercise therapy may be recommended. Moderate and severe affective disorders also require medication.
The essence of drug therapy for depression is to take drugs that affect the production of biologically active substances that cause the transmission of a neurochemical impulse through the neurons of the limbic system of the brain. For this purpose, antidepressants are used. A large clinical form of the disease, as a rule, requires hospitalization. According to indications for severe depression, pills for insomnia and anxiety are also prescribed - sedatives, tranquilizers.
A large clinical form of the disease, as a rule, requires hospitalization. According to indications for severe depression, pills for insomnia and anxiety are also prescribed - sedatives, tranquilizers.
Psychogenic reactive disorders are successfully treated, and soon after the onset of the disease comes the way out of depression. The clinical picture of the somatogenic form of the disease depends on the severity of the organic pathology. Endogenous disorders are not amenable to psychotherapy, but medication can often achieve long-term remission. Neurotic depression is prone to a long, chronic course.
The author of the article:
Ivanova Natalya Vladimirovna
therapist
reviews leave a review
Clinic
m. Sukharevskaya
Services
- Title
- Primary appointment (examination, consultation) with a general practitioner2300
- Repeated appointment (examination, consultation) with a general practitioner1900
- Initial appointment, consultation with a psychotherapist (up to 1 hour) 4400
- Repeated appointment, consultation with a psychotherapist (up to 1 hour)3000
Health articles
All articlesAllergistGastroenterologistHematologistGynecologistDermatologistImmunologistInfectionistCardiologistENT doctor (otolaryngologist)MammologistNeurologistNephrologistOncologistOphthalmologistProctologistPsychotherapistPulmonologistRheumatologistTraumatologist-orthopedistTrichologistUrologistPhlebologistSurgeonEndocrinologist 905 years.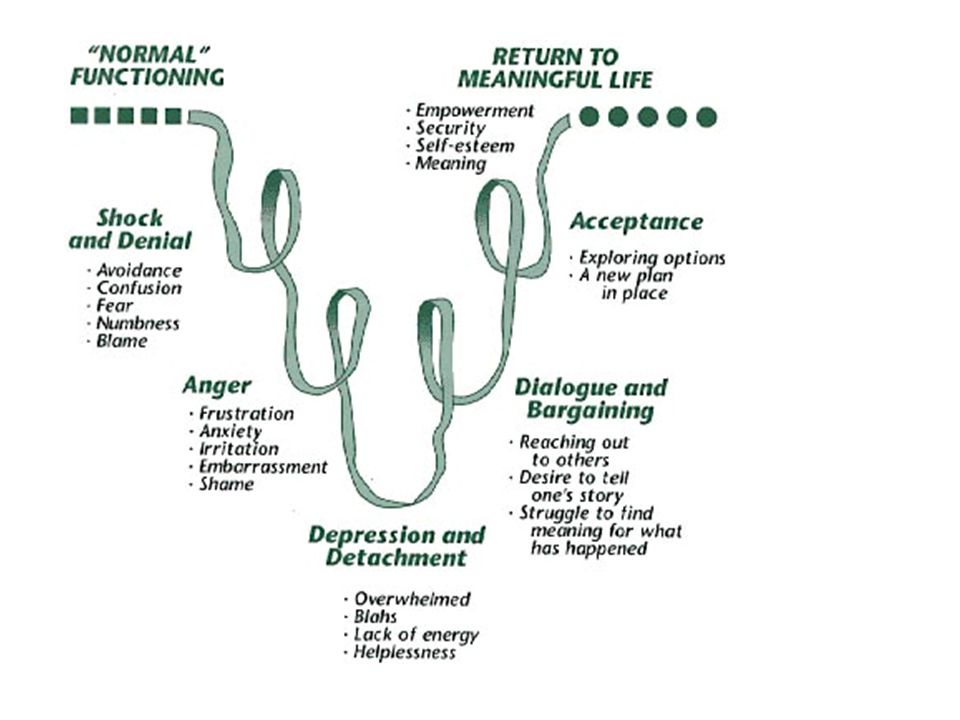 Red Gates. AvtozavodskayaPharmacy. Glades. Sukharevskaya. st. Academician Yangelam. Frunzenskaya Zelenograd
Red Gates. AvtozavodskayaPharmacy. Glades. Sukharevskaya. st. Academician Yangelam. Frunzenskaya Zelenograd Novikov Vladimir Sergeevich
psychotherapist, clinical psychologist, kmn, member of the Professional Psychotherapeutic League
reviews Make an appointment
Clinic
m. Frunzenskaya
Sorokin Maxim Vladimirovich
psychotherapist
reviews Make an appointment
Clinic
metro Frunzenskaya
Stages of accepting the inevitable: what are they and how to survive them
. And how to help them survive a loved one. Psychologists adviseUpdated November 16, 2022, 10:53
Shutterstock
Each person copes with difficult circumstances in their own way. One way to get through a difficult life period is to go through all the stages: denial, anger, bargaining, depression, and acceptance. However, according to psychologists, in practice this model is not so unambiguous. There is no single recipe. But there are ways to help yourself and loved ones during this difficult time. RBC Life talked to psychologists and found out the details.
However, according to psychologists, in practice this model is not so unambiguous. There is no single recipe. But there are ways to help yourself and loved ones during this difficult time. RBC Life talked to psychologists and found out the details.
Contents
- How We Accept the Inevitable
- Stages of Acceptance
- 5 Tips
- How to Help a Loved One
How We Accept the Inevitable
Shutterstock
The inevitable is unforeseen events of varying degrees of drama: illness, separation, layoffs, accidents, death of relatives and friends. During a lifetime, a person can experience such difficult situations several times - and not always the range of emotions will be the same. For example, while one will hide his head in the sand and refuse to make any decisions, the other may completely evade reality - there are many scenarios. Be that as it may, psychologists are unanimous: all these reactions are normal, since in a similar way the human psyche is looking for ways to protect itself and save itself.
One way to get through a difficult situation is to accept it. From an emotional point of view, this does not at all mean “to approve or support what happened.”
Acceptance is the recognition of a new objective reality as it is. To be at this point, a person needs time - for everyone it is different.
In psychology, there are at least ten models that describe the process of acceptance. Here are some of the more common examples.
- Sigmund Freud's theory of grief. The psychoanalyst saw the acceptance process as follows: breaking the connection, adjusting to new life circumstances and building new relationships [1].
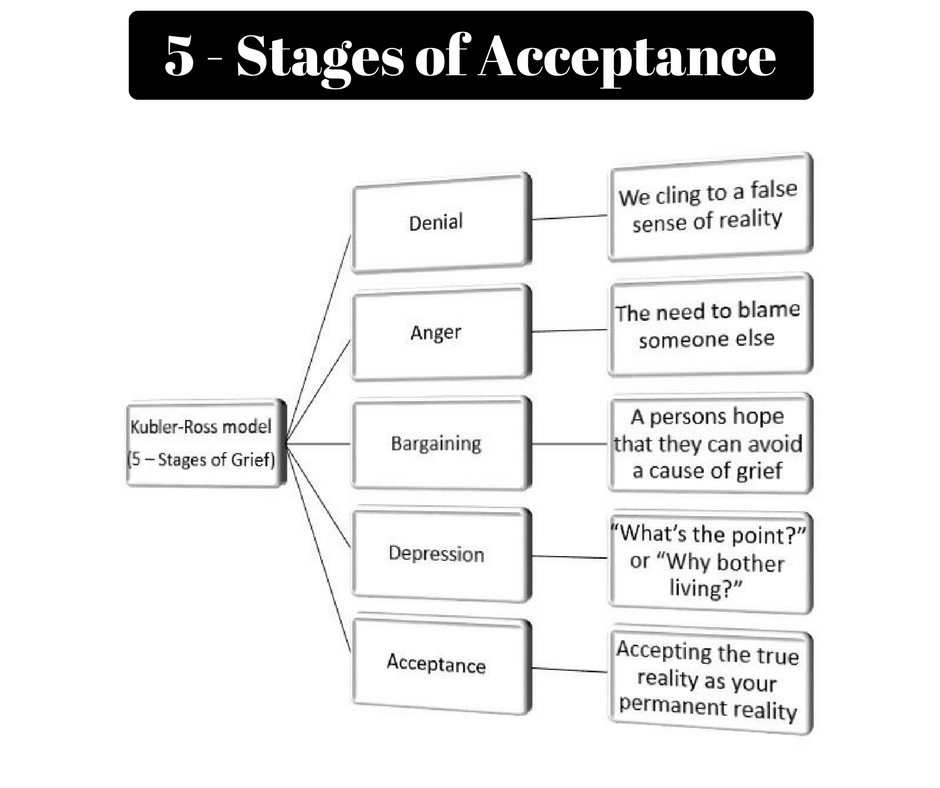
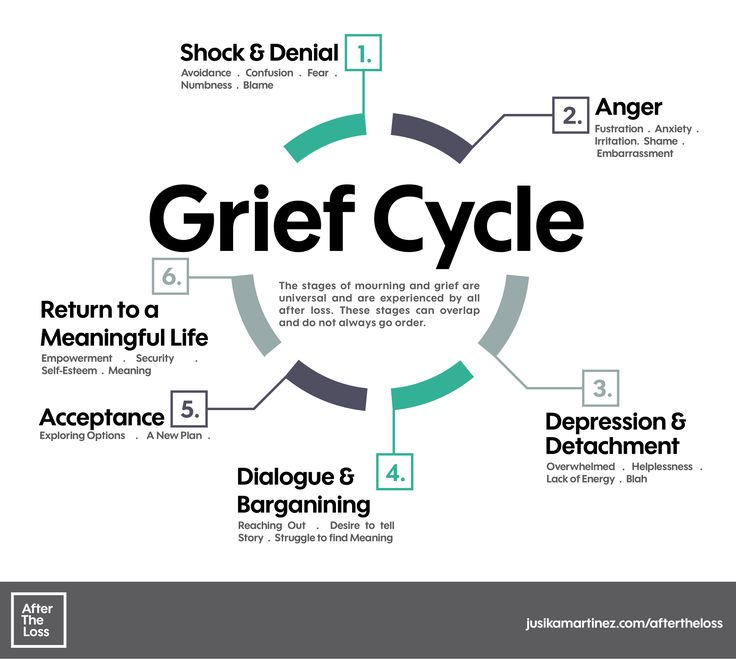
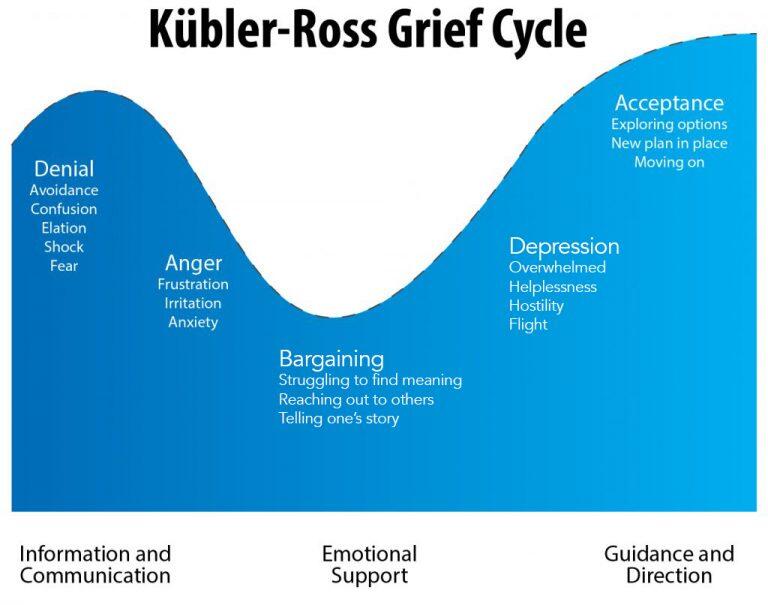
- Kübler-Ross acceptance stages. The most well-known theory of the five stages of acceptance is denial, anger, bargaining, depression, and acceptance. Often this model is perceived as linear, that is, a person sequentially goes through each of the stages. But Kübler-Ross herself noted that this is not her statement and that each individual stage may manifest itself in different ways or be completely absent [2].

- Model of two processes Strebe and Schut. An example of a cyclical model in which a person, as it were, oscillates between two states: recognizing a loss and experiencing pain, moving away from emotions and resolving practical issues caused by what is lost. These two processes are cyclically repeated, gradually healing the person [3].
- Six R Teresa Rando. Named after the first letter of each stage: Recognize, React to the separation, Recollect and re-experience, Relinquish old attachments, Readjust ) and reinvestment of emotional energy, the beginning of a new life (Reinvest) [4].
- Scott and Japhy change curve . In this model, experiences occur along a U-shaped trajectory. The high point at the beginning is characterized by almost manic denial, shock and anger, the low point by despair and depression, the high point at the end of the curve is a recovery of energy and morale. This approach is predominantly focused on accepting events before they happen.
 For example, an impending dismissal or something else that does not depend on us [5].
For example, an impending dismissal or something else that does not depend on us [5].
5 stages of acceptance
Shutterstock
Psychologists agree that it is often easier for the psyche of a person faced with severe grief or something inevitable to accept and experience something structured. “In modern practices, the Kubler-Ross stage model continues to be applied,” says Luiza Istomina, a medical psychologist at the European Medical Center. - It is used as a kind of support, helping to understand the principle of processes that replace each other. However, there is not enough empirical evidence to support or refute it. But, if it’s easier for you to accept what happened, you can focus on these stages. ”
1. Negation
A person unconsciously rejects events and begins to doubt them. For example, the laboratory mixed up the tests that confirmed a fatal illness, or the death of a loved one was reported by mistake.
Luiza IstominaMedical psychologist at the European Medical Center
“This state can last from a few seconds to several weeks, on average, by the seventh or ninth day, gradually changing to another.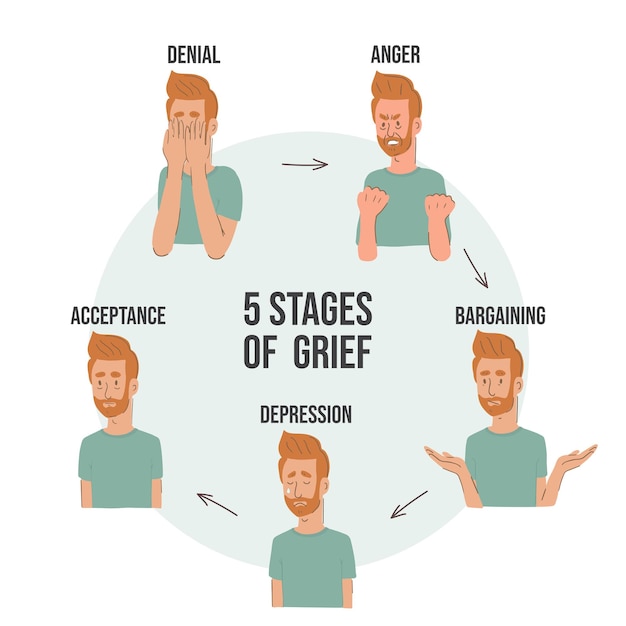 At this time, it is more important than ever to maintain your usual lifestyle: adhere to the sleep and wakefulness regimen, monitor nutrition, devote time to physical activity, and follow a daily routine. You can make a list of activities and activities that help relieve psycho-emotional stress: knitting, drawing, listening to music. It will be useful to use Mindfulness awareness techniques, since at the stage of denial a person may experience a feeling of detachment from the world, stupor, insensitivity.
At this time, it is more important than ever to maintain your usual lifestyle: adhere to the sleep and wakefulness regimen, monitor nutrition, devote time to physical activity, and follow a daily routine. You can make a list of activities and activities that help relieve psycho-emotional stress: knitting, drawing, listening to music. It will be useful to use Mindfulness awareness techniques, since at the stage of denial a person may experience a feeling of detachment from the world, stupor, insensitivity.
As soon as the denial and shock begin to fade, feelings that the person has previously suppressed come out.
2. Anger
Anger and anger at the moment of grief or a disturbing event is a natural reaction. Even if it seems that anger and anger are endless, these emotions will still dissipate - and the more you truly feel them, the faster this will happen [6]. At this stage, a person may have thoughts like “why me and not someone else?” or "life isn't fair." Redirecting anger to others is dysfunctional behavior.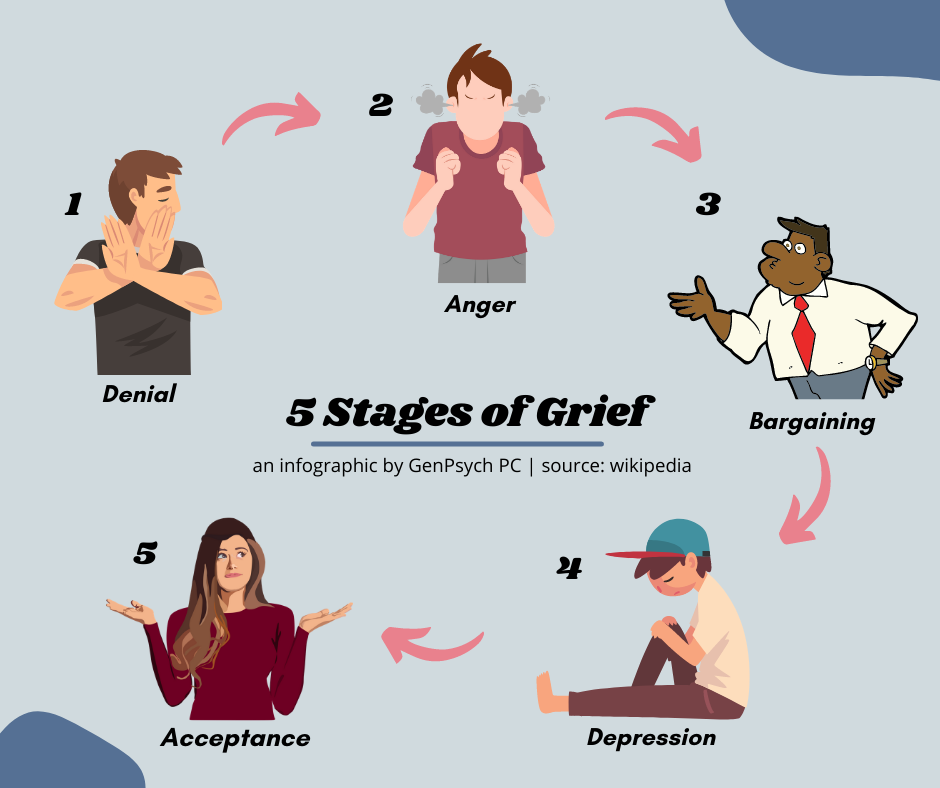
At this stage, as psychologists note, physical activity and sports will be especially useful. For example, Luiza Istomina recommends trying muscle relaxation techniques - Schulz's autogenic training or Ost's applied relaxation.
3. Bargaining
When something bad happens, a person can start an internal bargaining, promising to change something in himself and his life in order to improve the situation. Also at this stage, reasoning can torment, for example: "If I had left the house five minutes earlier, the accident would not have happened."
Shutterstock
To make it easier to pass this stage, it is useful to know about one non-obvious phenomenon. It turns out that it is easier for the psyche to accept the fact that a person is to blame and he could change something. This is a kind of trick of the psyche in response to a shock event. And this is worth remembering. In reality, such an attempt to bargain with oneself is nothing more than distortion and false hope.
To understand that what happened is not your fault, try to understand the reasons for what happened. If it is a disease, study it in more detail. Having read the necessary literature and received the necessary information, one can come to the conclusion that it was simply impossible to influence the course of treatment and its outcome.
4. Depression
Depression is the emptiness that a person feels when realizing that life will no longer be the same, for example, due to a sudden change in circumstances or loss. This is a phase of acute grief that lasts six to seven weeks from the onset of a tragic event. This is a period of despair and disorganization.
Luiza Istomina:
“At this step, separation begins, detachment from the object of loss, there is a gradual entry into reality, which will then allow you to combine the image of the lost, which remained in the past, with life in the present. At this stage, destructive and self-destructive coping strategies - dangerous behavior, the use of psychoactive substances, self-harm, the emergence of anti-vital and suicidal thoughts will be alarm bells. Support from loved ones and professional advice will help here. ”
Support from loved ones and professional advice will help here. ”
5. Acceptance of
At this point the emotions begin to stabilize as the person finally comes to terms with the fact that the new reality will now be different. In essence, we acknowledge the changes that have taken place. But this does not mean that a person evaluates them positively, just now you can live with it. To make it easier to move from depression to acceptance, you can try to learn constructive grief coping skills.
Luiza Istomina:
“Try writing down a negative automatic thought followed by cognitive restructuring (CBT approach). Example: “I can’t deal with this pain” is changed to “I have had suffering in my life, and I was able to cope with it, I need to give myself time.” Cognitive disconnection techniques (ACT-approach) can be applied. We track the depressive thought “My life will not be the same” and put it in a larger frame: “I have a thought that my life will not be the same. ”
”
The commit process may have some backtracking. It's demotivating and can be intimidating. However, it is possible to find ways to deal with regression.
In order to experience regression, according to Albina Borisenko, a psychotherapist in the ORCT approach (solution-oriented short-term therapy), a specialist in the Alter psychological platform, one can turn to an example with a metaphor. To do this, it is necessary to imagine that the process of acceptance is a kind of path: a road, a path or a ladder.
Albina Borisenkopsychotherapist in the ORCT approach, specialist in the psychological platform Alter
“Standing at some point on this path, you can turn around and see how far you have already traveled. To regress is only to take a step or a few steps back along a path that has already been traveled. That is, to be where you already were. So, you already absolutely know exactly how to move on and what can help. It is somewhat reminiscent of a computer game, where the completed levels are clear and understandable, and going through them again is not so scary, despite the difficulties that we know about. That means you're already on your way."
That means you're already on your way."
5 tips for accepting the inevitable
Shutterstock
Each of us is individual, so the same advice for someone will be healing, and for someone - absolutely useless. But each of us can listen to ourselves and understand what will help here and now. Here is what experts [7], [8], [9] advise.
1. Allow yourself to be sad
Expression of emotions can be an important part of the acceptance process. Don't judge yourself or compare yourself to others. Everyone mourns differently. If you suddenly feel like crying, give yourself that opportunity. There are many ways to express emotions: you can hit a punching bag or a ball for a healthy release of anger, or turn to creativity. For example, download a mobile application for music and art therapy. At the same time, write down all your feelings, experiences and thoughts in a diary. Over time, you will be able to see how your grief changes.
2. Ask for help
“Man is a social animal, and it is objectively difficult for us to survive without society,” says psychologist Borisenko. - Talking to a doctor, people in a support group, a relative or trusted friend can be a big help in a moment of grief. Don't be afraid to ask others for help and support. No, you will not be intrusive and will not lay responsibility on someone: a person always has the right to refuse. At the same time, you can always make a request – this is normal and part of human communication.”
- Talking to a doctor, people in a support group, a relative or trusted friend can be a big help in a moment of grief. Don't be afraid to ask others for help and support. No, you will not be intrusive and will not lay responsibility on someone: a person always has the right to refuse. At the same time, you can always make a request – this is normal and part of human communication.”
The same applies to offers of assistance. Do not rush to refuse if someone close to you decides to help you with house cleaning, grocery shopping or laundry. It won't make you weaker.
3. Take care of your health
Get regular exercise, eat as healthy as possible, and make sure you get enough sleep. Avoid excessive use of alcohol and other psychotropic substances. All this can not only contribute to the deterioration of mental health, but also directly affect your safety. For example, avoid self-driving and other potentially dangerous activities during times of intense emotion.
4.
 Set small goals
Set small goals Do not try to do everything at once - set small goals that are easy to achieve. “Make a list of different and most insignificant things: a cup of coffee in the morning, your favorite TV series or a walk in the park. Write down each item on how it helps the healing. Then, looking from the outside, you can see how much you do for yourself every day and how much more you can do,” says Albina Borisenko.
Also try to refrain from making major decisions, such as moving, for a while. But if this is inevitable, then, on the advice of a psychologist, the following technique will help.
Albina Borisenko:
“You shouldn't think of moving as one big “I'm moving” action. This is too big a step and therefore frightening. "I'm moving" consists of a lot of tiny steps: "I weigh the pros and cons," "I talk to my family," "I look at the list of required documents," and so on.
5. Stay Connected
Birthdays, anniversaries and holidays associated with a deceased person can cause a strong sense of grief. But do not completely cross out these days from your life. Celebrate a memorable date by lighting candles, meeting with family, or raising funds for charity. Simple rituals will maintain a sense of connection and emphasize that you continue to respect and appreciate the relationship that was. Keep a diary or write a letter to the person you have lost on an important date for both of you.
But do not completely cross out these days from your life. Celebrate a memorable date by lighting candles, meeting with family, or raising funds for charity. Simple rituals will maintain a sense of connection and emphasize that you continue to respect and appreciate the relationship that was. Keep a diary or write a letter to the person you have lost on an important date for both of you.
How to help a loved one accept the inevitable
Shutterstock
Some research suggests that the amount and quality of social support can affect the well-being of those who are grieving. The support of a loved one going through painful events can be critical to acceptance. But how to do it right? Here are some tips from experts [10].
1. Call a spade a spade
Do not be afraid, for example, to mention the name of a dead person or to talk about a situation the person is going through. This will avoid the unpleasant feeling that, for example, a loved one who has passed away is forever erased from memory. In such a situation, it is better to note that you will be bored than to say formally: "I'm sorry about the loss."
In such a situation, it is better to note that you will be bored than to say formally: "I'm sorry about the loss."
2. Give practical help
Do not ask how you can help, but act. Cook dinner, buy groceries, clean the house of the person you want to help. For many people, such as those who have lost a spouse, getting used to planning and living alone can be a big challenge.
3. Avoid annoying phrases
If you ask a grieving person how things are going, the answer is obviously "Bad." Instead, you can ask, “How are you feeling today?” Also, on the advice of experts, for some time it is better to refrain from the phrases “this is the will of God / the Universe / life” or “this is for the best”, until the person who has lost loved ones says it first.
4. Be a good listener
Listen carefully, but do not give advice or judge. Perhaps, on the path of acceptance, you will have to listen to your loved one the story of loss dozens of times in the smallest detail.