Can bipolar cause memory loss
How Does Bipolar Disorder Affect Memory?
People with bipolar disorder often report issues with their memory, thinking, and concentration. This is a mental health disorder that, like most others, can severely impair a person’s ability to carry out their responsibilities and daily routines. When something as frustrating as memory loss is added to the mix, finding relief from bipolar disorder can be crucial. So, how does bipolar disorder affect memory? What are the root causes?
What Is Bipolar Disorder?
Bipolar disorder is a mental health condition associated with episodes of mood swings ranging from depressive lows to manic highs. This condition is believed to occur due to a combination of genetics, environment, and altered brain structure and chemistry.
People with bipolar disorder experience both episodes of severe depression and episodes of mania, which include overwhelming joy, excitement, happiness, energy, reduced need for sleep, and reduced inhibitions. The signs and symptoms of bipolar disorder are unique to the individual, and no two diagnoses are the same.
These mood episodes can last for days to months at a time and may also be associated with suicidal thoughts, especially during depressive moods. These mood swings can be triggered by a variety of things, including lack of sleep, stress, changes to your daily routine, or jet lag when traveling.
How Does Bipolar Disorder Cause Memory Loss?
Scientists have found a distinct link between bipolar disorder and forgetfulness. What’s more, many people with bipolar disorder report memory loss and or difficulty remembering things.
These individuals may have trouble with short and long-term memory, struggle to think things through at a quick speed, and have difficulty thinking outside of the so-called box. But how does bipolar disorder affect memory? Why does it happen?
Well, researchers believe that depressive and manic episodes are the most common causes of memory loss in patients with bipolar disorder. During manic episodes, the individual may operate at high speeds, making it difficult for them to hard code new information into their memories.
During manic episodes, the individual may operate at high speeds, making it difficult for them to hard code new information into their memories.
It may also be equally as difficult to access older memories during these episodes. Research suggests that depressive phases of bipolar disorder can create problems with memory, as well.
When your mind is preoccupied with negative thoughts about yourself, the world, and the future, it can be difficult to concentrate. People in between these phases may also struggle with their memory.
For instance, depression causes memory loss both by occupying the mind and by inhibiting the connectivity between nerve cells. Although memory loss and bipolar disorder meds like lithium have also been linked, the evidence is scarce.
One study on people who are bipolar and memory issues analyzing a collection of data from similar studies found that people with bipolar disorder specifically struggle with verbal and visuospatial working memory loss.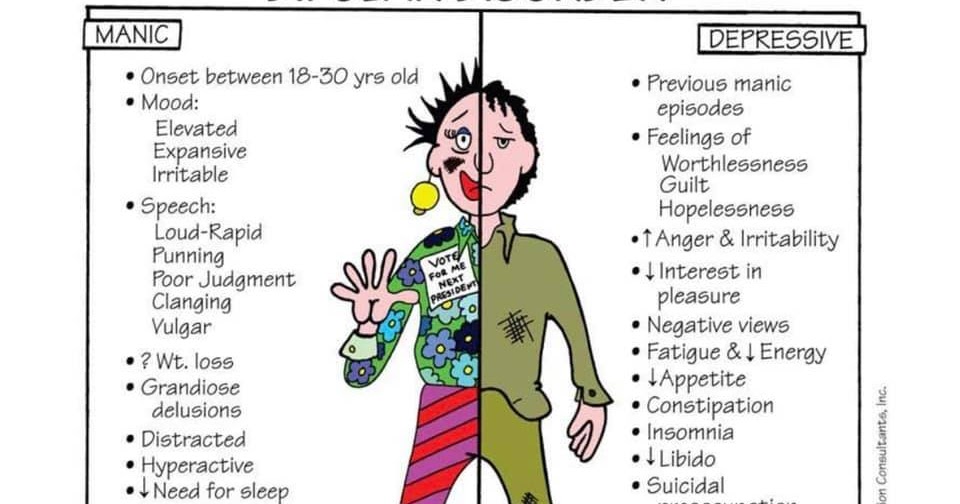 1 Verbal working memory involves the ability to remember something and to perform an activity using this memory.
1 Verbal working memory involves the ability to remember something and to perform an activity using this memory.
For instance, a person who developed bipolar disorder later in life may struggle to remember how to perform certain tasks in their jobs that they learned before developing this condition. Additionally, visuospatial working memory is the capacity to maintain a representation of visuospatial information for a brief period.
Visuospatial relates to the visual perception of the spatial relationships of objects, a skill that’s needed to identify and understand movement, depth, distance perception, and spatial navigation. Researchers also believe that a possible cause for memory problems in bipolar disorder patients is mood swings or episodes.
It’s common for people with this condition to experience cognitive deficits during manic or depressive episodes. Generally, people with bipolar disorder have shown problems in attention and memory during these episodes.
With that being said, impairment in attention or short-term memory can interfere with almost every area of a person’s life. Sustained attention, vigilance, and impulse control are often assessed in patients with bipolar disorder.
Research indicates that those who were in the middle of a depressed or manic phase of their illness produced more errors of attention compared to those who were not experiencing mania or depression.
Specifically, memory loss in bipolar disorder patients is also linked to deficits in regions of the brain like the prefrontal cortices, hippocampus, and caudate/putamen nuclei, each of which plays a role in memory as well as movement, learning, reward, motivation, emotion, and romantic interaction.
Reductions in brain volume and blood flow in certain regions – such as the hippocampus – in bipolar disorder patients are also associated with deficiencies in memory.
Bipolar Brain Fog
In addition to severe mood swings, people with bipolar disorder may also struggle with the ability to think coherently. Many complain of fuzzy or imprecise thought patterns. This symptom is otherwise referred to as “brain fog.”
Many complain of fuzzy or imprecise thought patterns. This symptom is otherwise referred to as “brain fog.”
Brain fog can occur in anyone with bipolar depression and is often characterized by symptoms like memory lapses, disorganization, groping for words, and difficulty learning new information.
Bipolar brain fog can also be considered a form of memory loss that people with bipolar disorder experience regularly. It can affect every area of a person’s life - from succeeding in school to correctly paying bills.
Bipolar Disorder Treatment
At our inpatient mental health rehab, we take all of our patients’ symptoms into consideration when treating their mental illnesses. Like others, bipolar disorder can be a difficult condition to manage without professional treatment and guidance.
Our Boca behavioral health center offers bipolar disorder treatment that involves a variety of modalities, including dialectical and cognitive behavioral therapy, group therapy, and more. We even offer family therapy to help the loved ones of our patients heal from the impact mental illness has had on them.
We even offer family therapy to help the loved ones of our patients heal from the impact mental illness has had on them.
Our mental health programs are multidimensional and effective forms of treatment that leave no detail behind. If you or someone you care about suspects that they have a mental illness or are searching for effective treatment and recovery resources, Banyan Mental Health is here to help.
Call our mental health treatment center today at 888-280-4763 to learn how to get started today.
Related Reading:
Dating Someone with Bipolar Disorder
How Does Bipolar Disorder Affect The Brain?
Famous People with Bipolar Disorder
Sources:
Bipolar disorder and memory: Effects, factors, and outlook
People with bipolar disorder can experience dramatic alterations in mood and activity levels, sleep disruption, and a range of other features and behavior patterns. The disorder may also affect the way a person thinks, and possibly their memory.
For some people with bipolar disorder, poor memory and difficulty concentrating can make it hard to function in everyday life, including at work and when studying.
However, this is not true for everyone.
The authors of a 2012 study have pointed out that one of the key features of bipolar disorder is the wide range of potential ability that exists among people with the condition.
Some people with bipolar disorder may find it harder to think, to reason, and to remember things.
Changes in thinking that can occur as people go through the different phases include:
- changes in attention span and focus
- racing thoughts during a high, or manic, phase
- anxiety
- difficulty remembering things
- in some cases, psychosis, including delusions and hallucinations
Studies report that some people with bipolar disorder have complained of memory impairment during high moods, low moods, and at times in between.
As a person’s mood shifts, they may report changes in their memory, too. As the mood becomes more extreme, memory problems can increase.
Scientists have suggested that some people with bipolar disorder experience memory problems due to changes in the brain.
These could involve changes in:
The prefrontal cortex, which plays a role in planning, attention, problem-solving, and memory, among other functions.
The hippocampus, which plays an essential role in storing memories.
The anterior cingulate cortex, which has links to both emotional and cognitive functions in the brain.
Imaging tests have shown that as a person’s mood shifts, variations in the way that blood flows into corresponding areas of the brain also occur.
Some people with bipolar disorder may find they face challenges with different kinds of memory function.
Here are some types of memory where problems might occur:
Working memory: This stores information for a short time while a person carries out a mental task.
Verbal learning and memory: This enables us to remember the words we see or hear.
Executive functioning: Is vital for planning and prioritizing tasks.
Declarative memory: Is necessary for recalling and explaining past events.
Spatial working memory: Enables people to recall shapes, colors, locations, and movements.
What does the research say?
A 2017 systematic review found that people may experience changes in the working memory processes of update and recall both during and between episodes of bipolar disorder. This can make it hard for people to function in work or study.
A study published in 2007 found that some people who experience psychosis in bipolar disorder may have difficulty with executive functioning. This can affect their ability to plan or carry out tasks.
Other researchers have described impairment in executive functioning as a “core dysfunction” that some people may experience when they are between high and low phases.
People with bipolar disorder who experience psychosis are more likely to experience problems with verbal-declarative memory and spatial working memory, compared with those who do not have psychosis. This can make it hard to recall and retell events and stories from the past.
The changes that occur with bipolar disorder may affect a person’s memory, but some of the treatments for the condition can also have an impact.
Lithium
Lithium is an important treatment for bipolar disorder. It can help to control moods, but it can also have adverse effects.
Some reports suggest that lithium can affect thinking and memory.
Newer drugs, such as lamotrigine, carbamazepine, valproate, topiramate, and zonisamide, may also impact a person’s cognitive ability. Research suggests that, of these drugs, lamotrigine may have less of a negative impact.
However, more studies are needed to confirm how these drugs affect thinking and memory.
If a person finds that a drug is affecting their memory, it is essential to speak to a doctor before stopping the treatment. they may be able to offer another option.
they may be able to offer another option.
Electroconvulsive therapy
If a person has severe symptoms that do not respond to other treatments, a doctor may recommend electroconvulsive therapy (ECT).
Research published in 2017 suggests that ECT is safe and effective for people with severe symptoms of bipolar disorder in any phase of the condition.
Out of 522 people with bipolar disorder who had not responded to other forms of treatment, two-thirds had a positive response to ECT, including almost 81 percent of those with catatonic depression.
However, one possible side effect of this treatment is memory loss.
Scientists have raised concerns about the impact on:
- remembering things that happened before the treatment
- forming new memories after the treatment
- remembering personal facts and events
- verbal and working memory
These impairments continued to affect people when they were between high and low moods.
More research is needed to find out exactly how ECT affects a person’s memory. However, for people who experience severe bipolar disorder, the benefits of this treatment may still outweigh the risks.
However, for people who experience severe bipolar disorder, the benefits of this treatment may still outweigh the risks.
Not everyone with bipolar disorder will experience problems with memory, but some people do. Early diagnosis and good medical management may help to minimize these effects in those who are at risk.
If a person is having difficulty with short term memory, the following tips may help.
- Record all appointments and contacts on a smartphone.
- Keep a book to record things you want to remember, for example, a record of spending.
- Make a to-do list each week or keep a wall calendar with space to write on.
- Stick post-it notes with reminders by the front door or other strategic places.
- Keep a chalk board, for example, in the kitchen, to write reminders on.
- Have a special place to keep important things like keys, glasses, and wallet.
- As far as possible, establish a routine, including regular bedtimes and mealtimes.
 This will also help to maintain healthful sleeping and eating habits.
This will also help to maintain healthful sleeping and eating habits.
Knowing what effects bipolar disorder can have on a person’s ability to think and remember, and understanding that mood changes are not the only feature of the disorder, may make it easier for individuals and their families to manage the many challenges that bipolar disorder presents.
A person who receives a diagnosis of bipolar disorder will have the condition for the rest of their life. However, they may not always experience mood alterations or show obvious symptoms. Symptoms often emerge sometime between the teenage years and the 30s.
The mood cycles and symptoms vary between individuals. One person may have more depressive symptoms, while another has mainly manic episodes.
A manic episode can involve the following:
- a high sense of self-esteem or the belief that the person is very important
- difficulty sleeping
- talking more than usual, with a rapid flow of speech that jumps suddenly between topics
- racing thoughts
- being easily distracted
- moving quickly from one focus of attention to another
- risk-taking behaviors, such as reckless driving or shopping sprees
During a low mood, the person may:
- lose interest in activities
- have no pleasure in things they usually enjoy
- be unable to focus
- sleep more or less than usual
- believe something terrible is going to happen or has happened
- talk about, think about, or attempt suicide
Some people may become completely inactive, or catatonic. If a person speaks about or attempts suicide, or if they become unable to move or react, someone should seek urgent medical help for the person.
If a person speaks about or attempts suicide, or if they become unable to move or react, someone should seek urgent medical help for the person.
Suicide prevention
If you know someone at immediate risk of self-harm, suicide, or hurting another person:
- Ask the tough question: “Are you considering suicide?”
- Listen to the person without judgment.
- Call 911 or the local emergency number, or text TALK to 741741 to communicate with a trained crisis counselor.
- Stay with the person until professional help arrives.
- Try to remove any weapons, medications, or other potentially harmful objects.
If you or someone you know is having thoughts of suicide, a prevention hotline can help. The 988 Suicide and Crisis Lifeline is available 24 hours a day at 988. During a crisis, people who are hard of hearing can use their preferred relay service or dial 711 then 988.
Click here for more links and local resources.
In either phase, a person may experience psychosis, involving delusions, hallucinations, or both. They may see, hear, or smell things that do not exist or believe that something is true when there is no evidence that it is.
They may see, hear, or smell things that do not exist or believe that something is true when there is no evidence that it is.
The causes of bipolar disorder remain unclear, but genetic, biochemical, and environmental factors probably play a role. Stress may trigger an episode, and using alcohol or other substances can make the symptoms and the impact of the condition worse.
Click here to find out more about possible links between alcohol and bipolar disorder.
Some people with bipolar disorder experience impairments in memory and thinking, although this is not true for everyone.
Memory problems may be more likely to develop if the person’s symptoms are severe, or if they experience many manic episodes, psychosis, or both.
Anyone who shows signs of bipolar disorder should seek medical help.
Treatment, including medication and counseling, can help a person to overcome the challenges of this condition.
Bipolar Disorder | Symptoms, complications, diagnosis and treatment
Bipolar disorder, formerly called manic depression, is a mental health condition that causes extreme mood swings that include emotional highs (mania or hypomania) and lows (depression).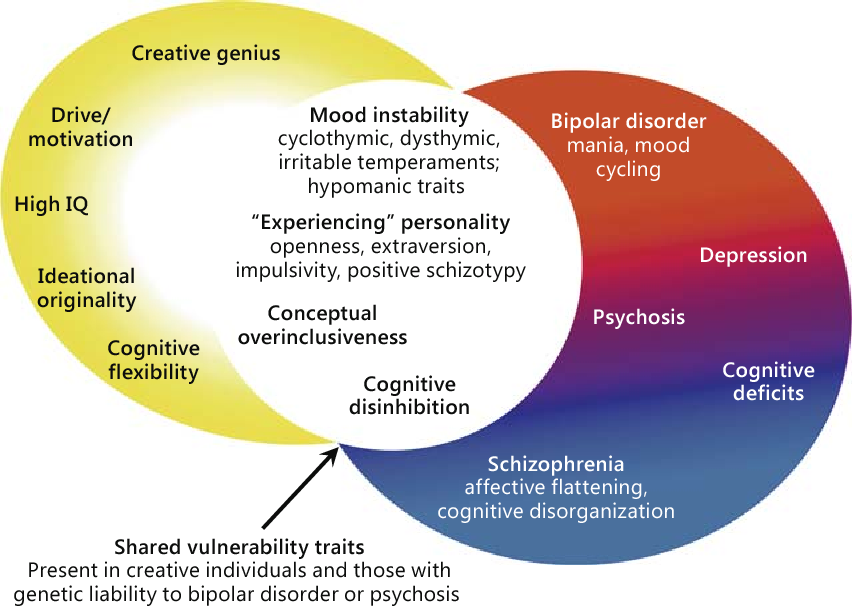 Episodes of mood swings may occur infrequently or several times a year.
Episodes of mood swings may occur infrequently or several times a year.
When you become depressed, you may feel sad or hopeless and lose interest or pleasure in most activities. When the mood shifts to mania or hypomania (less extreme than mania), you may feel euphoric, full of energy or unusually irritable. These mood swings can affect sleep, energy, alertness, judgment, behavior, and the ability to think clearly.
Although bipolar disorder is a lifelong condition, you can manage your mood swings and other symptoms by following a treatment plan. In most cases, bipolar disorder is treated with medication and psychological counseling (psychotherapy).
Symptoms
There are several types of bipolar and related disorders. These may include mania, hypomania, and depression. The symptoms can lead to unpredictable changes in mood and behavior, leading to significant stress and difficulty in life.
- Bipolar disorder I.
 You have had at least one manic episode, which may be preceded or accompanied by hypomanic or major depressive episodes. In some cases, mania can cause a break with reality (psychosis).
You have had at least one manic episode, which may be preceded or accompanied by hypomanic or major depressive episodes. In some cases, mania can cause a break with reality (psychosis). - Bipolar disorder II. You have had at least one major depressive episode and at least one hypomanic episode, but never had a manic episode.
- Cyclothymic disorder. You have had at least two years - or one year in children and adolescents - many periods of hypomanic symptoms and periods of depressive symptoms (though less severe than major depression).
- Other types. These include, for example, bipolar and related disorders caused by certain drugs or alcohol, or due to health conditions such as Cushing's disease, multiple sclerosis, or stroke.
Bipolar II is not a milder form of Bipolar I but is a separate diagnosis. Although bipolar I manic episodes can be severe and dangerous, people with bipolar II can be depressed for longer periods of time, which can cause significant impairment.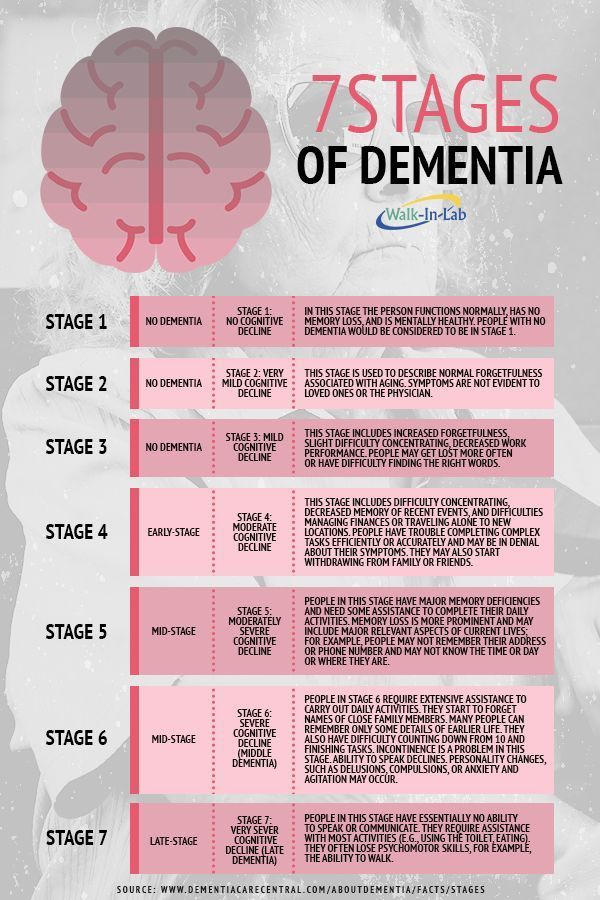
Although bipolar disorder can occur at any age, it is usually diagnosed in adolescence or early twenties. Symptoms can vary from person to person, and symptoms can change over time.
Mania and hypomania
Mania and hypomania are two different types of episodes, but they share the same symptoms. Mania is more pronounced than hypomania and causes more noticeable problems at work, school, and social activities, as well as relationship difficulties. Mania can also cause a break with reality (psychosis) and require hospitalization.
Both a manic episode and a hypomanic episode include three or more of these symptoms:
- Abnormally optimistic or nervous
- Increased activity, energy or excitement
- Exaggerated sense of well-being and self-confidence (euphoria)
- Reduced need for sleep
- Unusual talkativeness
- Distractibility
- Poor decision-making - for example, in speculation, in sexual encounters or in irrational investments
Major depressive episode
Major depressive episode includes symptoms that are severe enough to cause noticeable difficulty in daily activities such as work, school, social activities, or relationships. Episode includes five or more of these symptoms:
Episode includes five or more of these symptoms:
- Depressed mood, such as feeling sad, empty, hopeless, or tearful (in children and adolescents, depressed mood may manifest as irritability)
- Marked loss of interest or feeling of displeasure in all (or nearly all) activities
- Significant weight loss with no diet, weight gain, or decreased or increased appetite (in children, failure to gain weight as expected may be a sign of depression)
- Either insomnia or sleeping too much
- Either anxiety or slow behavior
- Fatigue or loss of energy
- Feelings of worthlessness or excessive or inappropriate guilt
- Decreased ability to think or concentrate, or indecisiveness
- Thinking, planning or attempting suicide
Other features of bipolar disorder
Signs and symptoms of bipolar I and bipolar II disorder may include other signs such as anxiety disorder, melancholia, psychosis, or others. The timing of symptoms may include diagnostic markers such as mixed or fast cycling. In addition, bipolar symptoms may occur during pregnancy or with the change of seasons.
The timing of symptoms may include diagnostic markers such as mixed or fast cycling. In addition, bipolar symptoms may occur during pregnancy or with the change of seasons.
When to see a doctor
Despite extreme moods, people with bipolar disorder often do not realize how much their emotional instability disrupts their lives and the lives of their loved ones and do not receive the necessary treatment.
And if you are like people with bipolar disorder, you can enjoy feelings of euphoria and be more productive. However, this euphoria is always accompanied by an emotional disaster that can leave you depressed and possibly in financial, legal, or other bad relationships.
If you have symptoms of depression or mania, see your doctor or mental health professional. Bipolar disorder does not improve on its own. Getting mental health treatment with a history of bipolar disorder can help control your symptoms.
People with bipolar disorder tell how to properly support them
March 30 is celebrated as Bipolar Day around the world. With this disease, it is important to monitor mood changes, which can be difficult to do alone. The founder of the Bipolar Association, Masha Pushkina, has collected stories of people who are helped by treatment partners.
With this disease, it is important to monitor mood changes, which can be difficult to do alone. The founder of the Bipolar Association, Masha Pushkina, has collected stories of people who are helped by treatment partners.
At the initiative of public organizations uniting scientists, doctors and activists, every year on March 30, World Bipolar Day is celebrated. The date chosen was the birthday of Vincent van Gogh, an artist who, according to researchers, was the embodiment of a "bipolar genius."
With bipolar disorder, a person lives either in a state of strong emotional upsurge and excitement (mania), or in depression. According to world statistics, about 2% of people suffer from bipolar disorder in various forms. This means that in Russia there are at least three million bipolar people - this is about half of St. Petersburg.
In most cases, this condition responds well to medication. But, unfortunately, many do not seek help or do not know how to find it. Without treatment, the disease progresses and ultimately leads to sad consequences: loss of family, job, disability in general, and in almost every seventh case, suicide.
These consequences can be avoided. The peculiarity of bipolar disorder is that the onset of remission depends not only on the doctor and medications, but also on the behavior of the patient himself. Very often, bipolar people provoke seizures "with their own hands." The mood of people with BAD (bipolar affective disorder. - Note ed. ) is very unstable, the balance is fragile, and mania or depression can be “started” in dozens of ways: the psyche is easily shaken by psychoactive substances, alcohol, lack of sleep, too intense work, travel, and even falling in love. So, a short time after the next course of treatment with powerful drugs, the person again ends up in the hospital. And each new attack reduces the chances of a long remission, affects social status, and even more painfully - self-esteem.
The experience of people with mental disorders around the world has proven that you are much more likely to cope with difficulties when you are supported by people who understand your problems and condition, but do not look at you as a patient. As practice shows, such a person can be not only a partner or close relative. An old friend, and even a person with whom you have never met in person, can help you get through the darkest times. Masha Pushkina, especially for Afisha Daily, spoke with several bipolar people about those in whom they found their support. The result is a story not about illness, but about friendship and trust, which can defeat even madness.
As practice shows, such a person can be not only a partner or close relative. An old friend, and even a person with whom you have never met in person, can help you get through the darkest times. Masha Pushkina, especially for Afisha Daily, spoke with several bipolar people about those in whom they found their support. The result is a story not about illness, but about friendship and trust, which can defeat even madness.
Yana, 31 years old
Housewife, collects books and is fond of confectionery
Purposefully, I didn't find out about the ways of support anywhere, everything turned out quite naturally. I have been sick for 15 years. The first person who looked after me was my best friend, and now it's my husband.
When my hypomania (a mild degree of mania, which is characterized by a constantly high mood. - Note ed. ) accelerated into a full-fledged mania (this state is also characterized by a one-sided attraction to some topic, sometimes accompanied by delirium. - Note ed. ), it became clear that I needed to be looked after. A friend began to pay attention to repetitive patterns of behavior in one phase or another, and we decided together to find out what helps in such cases. I think my friend was afraid to take responsibility for my condition, but she turned out to be generous and selfless. When I got married, a friend passed this knowledge on to her husband, and he already supplemented it, based on his own experience. The husband initially knew with whom he connects his life. He says it didn't scare him.
- Note ed. ), it became clear that I needed to be looked after. A friend began to pay attention to repetitive patterns of behavior in one phase or another, and we decided together to find out what helps in such cases. I think my friend was afraid to take responsibility for my condition, but she turned out to be generous and selfless. When I got married, a friend passed this knowledge on to her husband, and he already supplemented it, based on his own experience. The husband initially knew with whom he connects his life. He says it didn't scare him.
I have obsessions during my manic episodes. My husband does not argue with me at this time, but he also does not feed them, trying to redirect my stormy energy in a different direction. You can’t argue, because the result will be the opposite: I will finally get stuck on the idea, I will consider that I must prove it at all costs, even if the whole world is against me, and there are enemies and conspiracies around. If this does not help, the husband agrees to discuss all these things, but at the same time tries to slow down their implementation by offering to draw up a specific and detailed plan. Sometimes it takes me a long time.
Sometimes it takes me a long time.
For example, I always want to move somewhere. Right now, and why aren't we packing our things yet? My husband tries to make me write down what are the pros and cons of different cities, what attracts us to them. As a result, I sit for hours on different forums, make lists, think about how we will arrange our life, calculate the budget for different countries of the world. There is also a manic passion for travel, but after preparation, we usually implement these plans. And many years ago, in a fit of mania, I bought an apartment - with a mortgage, with hellish payments. Then it took a long time to resolve this situation, but, fortunately, everything worked out well.
My husband began to chart my mood. I also manage it, and we check the results so that they are objective. Quarrels due to the fact that the husband takes on the role of the elder often arise in the manic phase (never in depression). Then I become very suspicious, any attempts at control cause rage. But now the husband has learned from experience, so he does not react to attempts to unleash a conflict. With obvious attacks of rage and auto-aggression, he uses holding therapy (long strong hugs. - Note ed. ). We have seen this in autistic children, this is how their parents influence them.
But now the husband has learned from experience, so he does not react to attempts to unleash a conflict. With obvious attacks of rage and auto-aggression, he uses holding therapy (long strong hugs. - Note ed. ). We have seen this in autistic children, this is how their parents influence them.
When I'm depressed, he doesn't comfort me because it's pointless, but he tries to give reasonable arguments that this period has always ended and this time will also pass soon. We look at mood charts for the past months, discuss the duration of the attacks: two weeks have already passed and, judging by past experience, it should get better in a couple of weeks.
Such support from the husband helps in many ways. When I was being treated by two doctors, taking all the medicines, I didn’t have such support, everything was very bad. Over time, I stopped disappearing from home in a manic state and inflicting serious injuries on myself. All my super-ideas remain on paper in the form of graphs and tables, I don’t even have time to start putting them into practice, so that later I don’t have to deal with the consequences with the whole family.
Alisa, 27 years old
Biologist
To be honest, I don't always find understanding from my healthy environment, I often faced condemnation, devaluation of problems. But from a person who has a similar experience, you won’t hear “don’t invent”, “you can’t feel so bad”, “take a walk and it will pass”.
It just so happens that my best friend also suffers from bipolar disorder. I did not look for support in specialized communities where patients communicate, we met by chance. My friend is much older, he has much more life experience, and he was able to become a real mentor for me. Not once did his actions worsen my condition - I hope that he can say the same about me.
When I'm on the rise, I feel uncomfortable when he tries to slow me down and reduce my passions. But as soon as this state passes and I again take a sober look at the situation, each time I thank him for trying to stop the revelry and disgrace. My friend himself is currently not being treated, but he never imposed his position on me, and when I turn to doctors, he supports me in this.
I told the doctor about this source of support - he is all for it. Before meeting a friend, I had suicidal attempts, but during the entire time of our communication I never tried to say goodbye to life. When you know that there is a person who will understand everything and share warmth (while even my own family repels me), that there is a place where you can come in any condition and where they will accept me without unnecessary questions and teachings, this is a source of great strength. and hope.
When I was expecting my second child, I was depressed. My husband did not yet fully understand the features of the disease and did not want to admit obvious things - this added problems, and my emotional state became extremely difficult. It seems that only thanks to the participation of my friend, I did not do anything to myself and successfully endured the pregnancy. The child was named after him.
Sergey, 49 years old
Freelancer
At the height of the depression, I was looking for any available support and ended up in an online group of anonymous debtors (people who have taken on large loans). One of the participants drew attention to my condition and said that I urgently need medical help. Despite the fact that she lives in the USA, we began to communicate regularly via Skype. Olga literally brought me to the hospital and helped me prepare for the treatment.
Americans are a pragmatic people, many young and healthy people have folders with wills and instructions in case of their death. They also approach mental difficulties calmly and thoroughly. It is common practice for the patient to draw up detailed instructions in advance. In the United States, there is a practice of issuing Treatment Agreements for people with mental illness (Treatment Contract). This document is needed so that family, friends and doctors recognize the symptoms of deterioration in time and take into account your experience and wishes in the treatment. Typically, such a document contains: a list of trusted people; signs of a normal state; signs of an approaching episode; symptoms of mania and depression; actions that trusted people should take to help a person get better and keep him from destructive acts; plan of action in case of an emergency (for example, a suicide attempt). who and what will be done in case of his hospitalization, so that he can be treated without anxiety for household chores.
In a period of severe depression, there is a struggle inside a person between the craving for death and the desire to live - and many external things can outweigh in one direction or another. Every clue is important to help you get out. It is very difficult for one to cope with all this.
I madly didn’t want to go to the hospital and wouldn’t have made up my mind myself, until the last I hoped that somehow everything would go away on its own. But under the supervision of a friend, I drew up a preparation plan: warn the customer at work, arrange to look after my cats. Reported to her about every step. But then he could no longer simply “escape” [from hospitalization], because he felt obliged to both her and the doctor. During depression, one's own life has no value, but the people dear to me, the promises made to them, do.
At the most difficult moment, Olga became my “outer brain”, which told me what to do when I didn’t understand anything myself. After I was discharged from the hospital, I turned to four friends for support. Usually we call each other once a week, I tell what my condition is. It is important not only to chat online, but also to hear the voice, you can understand a lot from it. Friends immediately pay attention, if I suddenly disappear and stop calling, then something is wrong.
I think it is possible to find such a person if you set yourself such a goal. Take a closer look at people in support groups, religious or other communities - those who understand what compassion and mutual assistance are. This must be an internally mature person, ready to take responsibility for you in a difficult situation. If this person has similar problems, then he will better understand your experiences. For this reason, relatives are far from always suitable: they themselves can panic, seeing how bad you feel, choke you with their anxiety, overprotection.
It is necessary to establish the frequency of communication and observe it. And of course, in no case should you parasitize on someone else's kindness. The support system works when you yourself take responsibility for your life, and do not outweigh it completely on another.
Anna and Valeria, 21
Students
Anna: After a major depressive episode four years ago that almost ended in a suicide attempt, I started looking for information on [support]. I managed to find a guide in English for relatives and friends on how to behave with such a person. I have sent this list to all my friends so that they have an idea of what is happening to me. For the past few years, Lera has been monitoring my emotional state on a daily basis, and if, in her opinion, it goes beyond the norm, she tells me about it. Lera just asks every day how I'm doing, and if she sees that I'm reacting strangely, she wonders if something happened. At first, it was very difficult, because, in principle, I did not like to regularly share personal experiences. But by regularly receiving feedback, I can imagine the dynamics: do the pills help, how long do the side effects last, does the depressive phase go into a moderate and severe degree, do I lose my critical thinking during hypomania.
Valeria: We gradually established a very trusting relationship. Anya studied the topic of bipolar disorder up and down, and I read the articles that she sent me. The diagnosis did not change anything for me, because it remained the same. After that, we already discussed some formalities (for example, who to call in case of an emergency).
Anna: I asked Lera to watch for hypomanic manifestations in which I lose an adequate assessment of my actions: impulsive night walks, alcohol begin.
Valeria: My friend is a very responsible and conscious girl who takes care of herself, her health and her wallet. Before buying something expensive, she asks for my advice - and then we are already sorting out the situation. We can entrust accounts to each other and not worry. I also know where and to whom to run in cases of exacerbation.
Anna: I react badly to prohibitions and reminders of illness. Yes, I periodically have to turn to relatives for help, change treatment or take long breaks, but I expect mutual respect so that they don’t look at me through the prism of the disease.
When the mood is unstable, harsh phrases like “the disease speaks in you”, “these are not your real emotions” cause persistent rejection, even when they are true. The line between accepting a loved one's illness and identifying him with a diagnosis for healthy people is extremely thin. Therefore, those who were able to grope it deserve great respect.
Anna: In the last year, I go to see the doctor with my parents. When the doctor notices that I may not be able to do it alone, she duplicates the instructions and advice for them. I, in turn, am a friend. The doctor has repeatedly emphasized that the change of episodes is more noticeable from the outside.
Valeria: We don't have any kind of hierarchy in relationships, so there is no pressure when one makes decisions for another. This is not eating each other's emotional resources, but complementing and supporting.
Anna: The main danger in a relationship with a person with a serious illness is to fall into codependency. This format is equally bad for both the "controller" and the "subordinate". Unfortunately, I have been in such relationships before. It is worth maintaining mutual respect and treating each other as equals. Illness should not dominate a relationship. In difficult episodes, it temporarily comes to the fore, but you should always remember that you are not a disease.
Anna: I have memory problems: I don't remember some episodes. In such cases, I can ask Lera for help. If you remember the last weeks, then these are regular reminders to call the doctor. In mixed episodes, this becomes an acute problem, because I can suddenly change my mind or forget. Against the backdrop of a severe episode, I may develop psychosis, and this is the most dangerous thing in the disease. Thanks to our format, I manage to avoid such exacerbations almost always.
The advantages of observation from a loved one are an early response and the fact that he knows the patient's usual behavior very well and can notice even small changes. The main disadvantage is that normal friendly communication risks turning into constant monitoring of symptoms. Not every mentally healthy person is able to remain within the boundaries of reason.
It is important to agree in advance, before an attack, what is an undoubted sign of a worsening condition (for example, persistent insomnia), and what you do not need to pay special attention to (for example, loud indignation at something that you do not like). In a difficult situation, often a loved one begins to behave not as an equal, but as a “healthy” and “knowledgeable”. Not all relationships stand this test.
There is also a variant of "buddy" (when two people with mental disorders look after each other. - Note ed. ) - it is good precisely because it is the true request of the patient and more equal relations without mixing roles. But I don't know the buddy support system.
To choose a person you can rely on in a critical situation, take a closer look at your surroundings. Above all, a high level of trust is needed. Your assistant should be open to nonjudgmental and open dialogue and at the same time emotionally stable and resistant to stress.
Support is essential for every person - very often we as mental health professionals need it. And with bipolar disorder, this problem is especially acute. At the initial stages, those closest to you often ignore the presence of the disease, and friends advise you to either "pull yourself together" or, conversely, "relax", sometimes with the help of alcohol. When it becomes obvious to everyone that the “condition” will not go away on its own, urgent hospitalization is already required. The saved patient receives the "stigma".