Triggers for narcolepsy
Narcolepsy - Causes - NHS
Many cases of narcolepsy are thought to be caused by a lack of a brain chemical called hypocretin (also known as orexin), which regulates sleep.
The deficiency is thought to be the result of the immune system mistakenly attacking parts of the brain that produce hypocretin.
But a lack of hypocretin is not the cause in all cases.
Immune system problem
Normally, antibodies are released by the body to destroy disease-carrying organisms and toxins.
When antibodies mistakenly attack healthy cells and tissue, it's known as an autoimmune response.
In 2010, scientists in Switzerland discovered that some people with narcolepsy produce antibodies against a protein called trib 2.
Trib 2 is produced by an area of the brain that also produces hypocretin. This results in a lack of hypocretin, which means the brain is less able to regulate sleep cycles.
These research results may help explain the cause of narcolepsy in many cases, but it does not explain why some people with the condition still produce near-normal levels of hypocretin.
Possible triggers
A number of factors may increase a person's risk of narcolepsy or cause an autoimmune problem.
These include:
- an inherited genetic fault
- hormonal changes, including those that take place during puberty or the menopause
- major psychological stress
- a sudden change in sleep patterns
- an infection, such as swine flu or a streptococcal infection
- having the flu vaccine Pandemrix
Research is yet to confirm whether all of these play a role in narcolepsy.
Pandemrix vaccine
Research carried out in 2013 found an association between the flu vaccine, Pandemrix, which was used during the swine flu epidemic of 2009 to 2010, and narcolepsy in children.
The risk is very small, with the chance of developing narcolepsy after having a dose of the vaccine estimated to be around 1 in 52,000.
Pandemrix is no longer used in the UK for flu vaccination.
Impact of narcolepsy on sleep
The total time someone with narcolepsy spends sleeping is not necessarily different from that of people who do not have the condition.
But narcolepsy can significantly affect sleep cycles and decrease the quality of sleep.
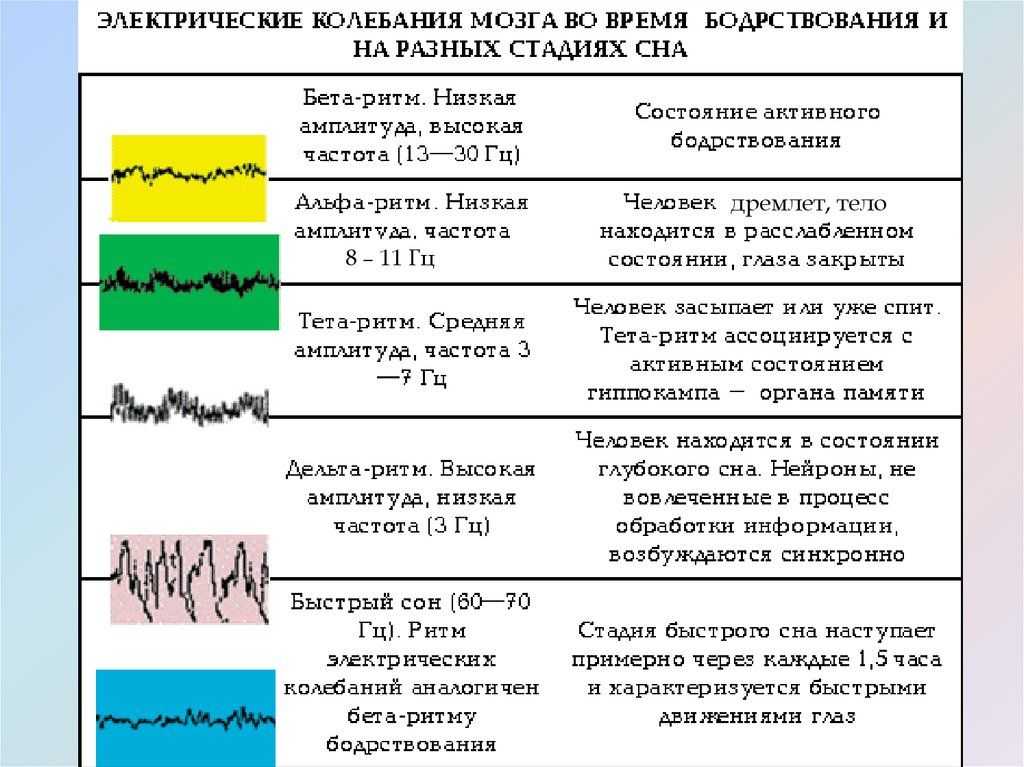
Sleep is made up of cycles of different brain activity known as non-rapid eye movement (NREM) and rapid eye movement (REM).
During REM sleep, your brain activity increases and you may dream. Normal sleep starts with 3 stages of NREM sleep at first, followed by a short period of REM sleep.
NREM and REM sleep then alternates throughout the night. During the latter part of the night, REM sleep is more prominent.
If you have narcolepsy, this pattern is much more fragmented and you may wake several times during the night.
You may also experience REM sleep much earlier than normal after falling asleep, and the effects of REM sleep, such as dreaming and paralysis, while you're still conscious.
Secondary narcolepsy
Narcolepsy can sometimes be the result of an underlying condition that damages the areas of the brain that produce hypocretin.
For example, narcolepsy can develop after:
- a head injury
- a brain tumour
- multiple sclerosis (MS)
- encephalitis
Narcolepsy resulting from an identifiable underlying condition is called secondary narcolepsy.
Page last reviewed: 30 December 2022
Next review due: 30 December 2025
Narcolepsy - NHS
Narcolepsy is a rare long-term brain condition that can prevent a person from choosing when to wake or sleep.
The brain is unable to regulate sleeping and waking patterns normally, which can result in:
- excessive daytime sleepiness – feeling very drowsy throughout the day and finding it difficult to concentrate and stay awake
- sleep attacks – falling asleep suddenly and without warning
- cataplexy – temporary loss of muscle control resulting in weakness and possible collapse, often in response to emotions such as laughter and anger
- sleep paralysis – a temporary inability to move or speak when waking up or falling asleep
- excessive dreaming and waking in the night – dreams often come as you fall asleep (hypnogogic hallucinations) or just before or during waking (hypnopompic hallucinations)
Narcolepsy does not cause serious or long-term physical health problems, but it can have a significant impact on daily life and be difficult to cope with emotionally.
In an attempt to avoid attacks, some people may become emotionally withdrawn and socially isolated.
Find out more about the symptoms of narcolepsy.
What causes narcolepsy
Narcolepsy is often caused by a lack of the brain chemical hypocretin (also known as orexin), which regulates wakefulness.
The lack of hypocretin is thought to be caused by the immune system mistakenly attacking the cells that produce it or the receptors that allow it to work.
But this does not explain all cases of narcolepsy, and the exact cause of the problem is often unclear.
Things that have been suggested as possible triggers of narcolepsy include:
- hormonal changes, which can occur during puberty or the menopause
- major psychological stress
- an infection, such as swine flu, or the medicine used to vaccinate against it (Pandemrix)
Find out more about the causes of narcolepsy.
Who's affected
It's difficult to know exactly how many people have narcolepsy because many cases are thought to go unreported.
But it's estimated to affect about 30,000 people in the UK.
Men and women are thought to be affected equally by narcolepsy, although some studies have suggested the condition may be more common in men.
The symptoms of narcolepsy often begin during adolescence, although it's usually diagnosed between the ages of 20 and 40.
Diagnosing narcolepsy
See a GP if you think you may have narcolepsy. They may ask about your sleeping habits and any other symptoms you have.
They may also carry out tests to help rule out other conditions that could be causing your excessive daytime sleepiness, such as sleep apnoea, restless legs in bed and kicking during sleep, or an underactive thyroid gland (hypothyroidism).
If necessary, you'll be referred to a specialist in sleep disorders, who'll analyse your sleep patterns.
This will usually involve staying overnight in a specialist sleep centre so various aspects of your sleep can be monitored.
Find out more about diagnosing narcolepsy.
Treating narcolepsy
There's currently no cure for narcolepsy, but making changes to improve your sleeping habits and taking medicine can help minimise the impact the condition has on your daily life.
Taking frequent, brief naps evenly spaced throughout the day is one of the best ways to manage excessive daytime drowsiness.
This may be difficult when you're at work or school, but a GP or specialist may be able to devise a sleep schedule that will help you get into a routine of taking naps.
Keeping to a strict bedtime routine can also help, so you should go to bed at the same time each night whenever possible.
If your symptoms are particularly troublesome, you may be prescribed medicine that can help reduce daytime sleepiness, prevent cataplexy attacks and improve your sleep at night.
These medicines are usually taken as daily tablets, capsules or drinkable solutions.
Find out more about treating narcolepsy.
Narcolepsy and driving
If you're diagnosed with narcolepsy, it may affect your ability to drive.
Stop driving immediately and inform the Driver and Vehicle Licensing Agency (DVLA).
You'll need to complete a medical questionnaire so your individual circumstances can be assessed.
You'll usually be allowed to drive again if your narcolepsy is well controlled and you have regular reviews to assess your condition.
Narcolepsy UK's information about driving and narcolepsy
Tell the DVLA about your condition at GOV.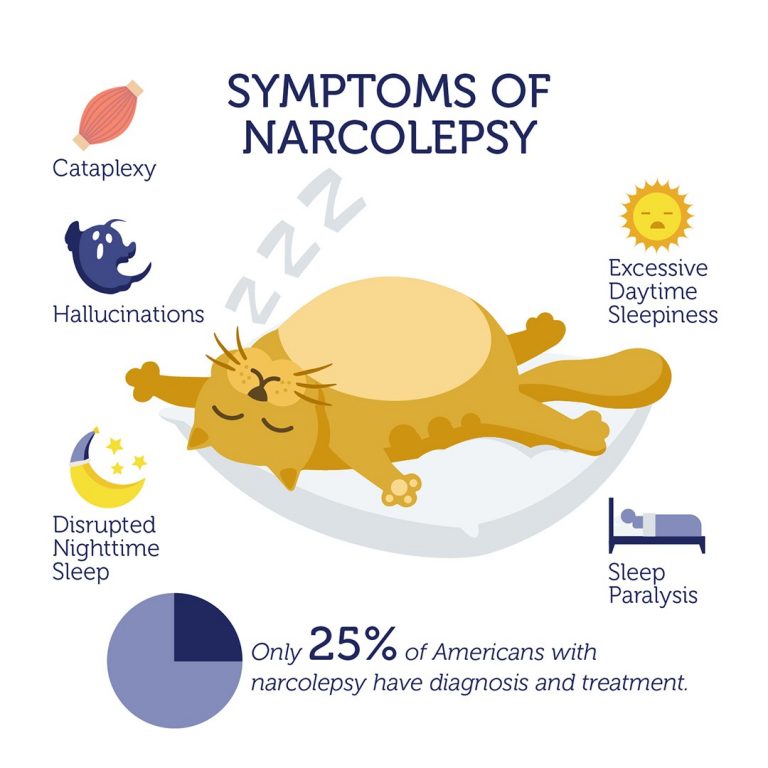 UK: Narcolepsy and driving
UK: Narcolepsy and driving
Page last reviewed: 30 December 2022
Next review due: 30 December 2025
search for drugs, prices and availability of drugs in pharmacies of Ukraine
Save up to 30% when booking goods in pharmacies.
Pharmacy chains of Ukraine
- Pharmacy chain 9-1-1, Kharkiv
- Merezha Pharmacy Plantain, Lviv
- Low Price Pharmacy, Zaporozhye
- Pharmacy chain "Pharmacy Good Day", Kyiv
- Pharmacy chain D.
 S., Lviv
S., Lviv
Alphabetical search
Last news
My Pharmacy is the fastest and most convenient way to find the necessary medicines in any pharmacy throughout Ukraine. We provide up-to-date pricing and availability information drugs in pharmacies of Ukraine. Here you can buy medicines at low prices by comparing prices or making an online reservation.
Our database contains data on more than 11,000,000 product offerings of medicines and related products in 3,000 pharmacies in Kyiv and other settlements of Ukraine.
Updating the product range database every 20 minutes allows you to always provide the most up-to-date and reliable information about medicines.
In addition, the user can get acquainted with the work schedule and contacts of each pharmacy point presented on our resource, find the addresses of round-the-clock pharmacies 24 hours and build to them route on the map.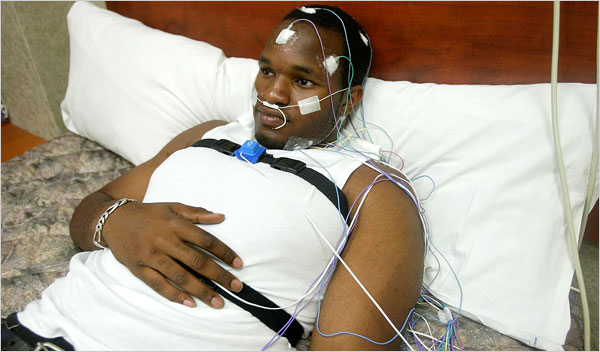
The goal of this project is to enable each user to search for medicines as simply and efficiently as possible, and to order pills online quickly and conveniently.
User benefits
My Pharmacy has a number of advantages that distinguish us from competitors, thanks to which customers choose us.
We offer:
- Ability to quickly search for drugs in pharmacies in Kyiv and other cities of Ukraine;
- Find out about the availability of medicines in Ukrainian pharmacies;
- View the current price of medicines in various pharmacies;
- Compare prices in pharmacies for the drug of interest and find out where it can be purchased at the most profitable;
- We provide an opportunity to get an additional discount when ordering medicines online;
- Find analogues of expensive drugs by comparing drugs by active substance;
- Read manufacturer's instructions for use;
- Find out about the availability of medicines in the nearest pharmacies, and independently build a route on the map online;
- On our website you can find out the exact address, contact numbers and working hours of any pharmacy and find the closest pharmacy to you.
- Read useful publications about health, learn the latest news from the field of medicine;
- Share your feedback on the quality of service of a particular pharmacy;
Ordering and searching for medicines in pharmacies on the website
On the main page of the site there is a line for a quick search for the necessary medicines. According to the full name or its fragment, the resource will offer you a list of drugs found with relevant prices. To purchase the drug at the lowest cost, you just need to compare prices in pharmacies or place a reserve for it to receive an additional discount.
Using filters by price, distance, work schedule will make your search results more targeted and useful.
The functionality of the service will be useful not only to ordinary users, but also to employees of medical institutions. Selection is available on the advanced search pages medicines according to specialized indicators:
- ATC code
- Active ingredient
- Pharmacotherapeutic group
- International non-proprietary name
For each drug, the site contains the original instructions for use from the manufacturer, which indicates everything about the product: active ingredients, purpose, contraindications and adverse reactions. Please read this information carefully before purchasing. On the same page, you can quickly find drug analogues by simply clicking the Analogues button. Here you will see everything options that can replace the drug of interest. And to order pills online, you need to click on the green button next to the price.
Please read this information carefully before purchasing. On the same page, you can quickly find drug analogues by simply clicking the Analogues button. Here you will see everything options that can replace the drug of interest. And to order pills online, you need to click on the green button next to the price.
DEAR USER!
ADMINISTRATION OF THE SERVICE "MY PHARMACY" WARNING: SELF-HEALING CAN BE DANGEROUS TO YOUR HEALTH! INFORMATION ON THIS RESOURCE IS PRESENT FOR INFORMATIONAL PURPOSES ONLY AND IS NOT MAY REPLACE A DOCTOR'S CONSULTATION.
Not just drowsiness. How to live with narcolepsy and why there is still no cure for it - Knife
At one of my first jobs, I stood on a lion's nix. There are activities that are not suitable for a person with narcolepsy, and this is probably one of them. I was 22, recently graduated from the Faculty of Zoology and studied meerkats in the Kalahari Desert in South Africa.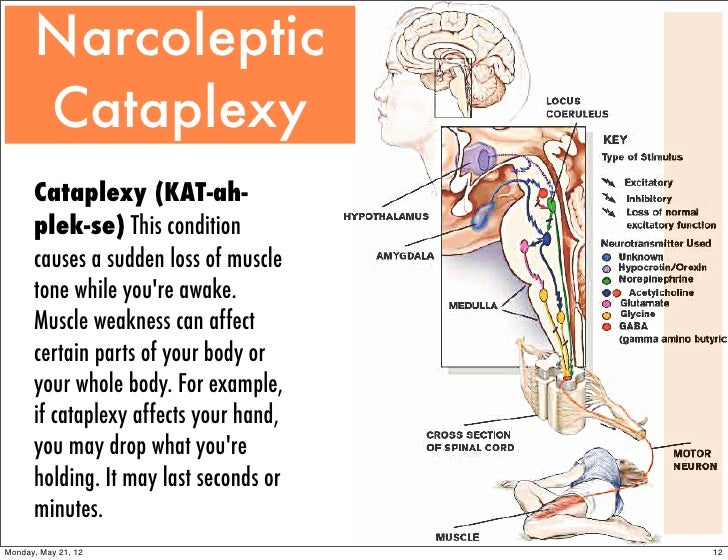 My colleague and I worked in pairs: one on the move walking with meerkats, and the other in a jeep scanning the horizon for the danger of a lion. Many times I woke up with a steering wheel imprint on my forehead and the realization that I had overlooked a colleague and meerkats. I searched the surrounding landscape for signs of life, and as the panic grew, for signs of death. Now I can tell this story only because no one was devoured after all.
My colleague and I worked in pairs: one on the move walking with meerkats, and the other in a jeep scanning the horizon for the danger of a lion. Many times I woke up with a steering wheel imprint on my forehead and the realization that I had overlooked a colleague and meerkats. I searched the surrounding landscape for signs of life, and as the panic grew, for signs of death. Now I can tell this story only because no one was devoured after all.
I wasn't always like this. I slept well for the first twenty years of my life, but shortly after my 21st birthday, I began to experience symptoms of narcolepsy, a rare (but not uncommon) disorder that affects about one in 2,500 people.
Narcolepsy is common knowledge, that the sufferer experiences frequent bouts of uncontrollable drowsiness. This is true, but the disease is much more serious: it is often accompanied by cataplexy (a condition where strong emotions cause loss of muscle tone and the person falls like a rag doll), psychedelic dreams, sleep paralysis and frightening hallucinations.

No medicine. Bye.
In the Kalahari in 1995, these symptoms were new to me. I didn't realize the damage the endless struggle with sleep would do to my body and mind. I was not alone in my ignorance. Few family doctors have heard of this disorder, let alone seen even one patient live. Some neurologists knew what to look for, but many did not. Even sleep experts could not explain why I suddenly had this condition.
A lot has changed since then. Evidence is mounting that the most common cause of narcolepsy is an autoimmune malfunction, in which the immune system misinterprets an upper respiratory tract infection and mistakenly clears out about 30,000 neurons in the center of the brain.
The brain is made up of 100 billion cells, and there doesn't seem to be much to worry about.
But these are not simple cells, these are cells of the hypothalamus, a small, evolutionarily ancient, and incredibly important device that helps regulate many basic body functions, including the daily swing between sleep and wakefulness.

They are also the only cells in the brain that synthesize orexins (also known as hypocretins).
This pair of peptides—short chain amino acids—was unknown to science at the time of my diagnosis in 1995. The story of their discovery, which began in the 1970s, is a beautiful parable of luck and luck, fantasy and foresight, risk and rivalry, and besides, it features a colony of narcoleptic Dobermans.
There are medications now available to help manage the worst symptom of narcolepsy, but none come close to correcting the underlying brain damage. The answer to my problems seems simple - I just need to put orexins (or something equivalent) in my brain. So why am I still waiting for my cure to be invented?
In 1972, a poodle puppy was born in Canada, he was named Monique. When Monique tried to play, she suddenly suddenly fell. It didn't feel like sleep, more like partial paralysis. Veterinarians suspected narcolepsy with symptoms of cataplexy. Monique was moved to California, where she was studied by sleep specialist and Stanford University professor William Dement. Word began to spread, and soon Dement and his colleague Merrill Mitler were watching not only Monique, but several other dogs as well.
Word began to spread, and soon Dement and his colleague Merrill Mitler were watching not only Monique, but several other dogs as well.
The fact that narcolepsy was more common in certain dog breeds suggested that there was a genetic basis for the disorder.
Then the breakthrough came: Dement was informed of a Doberman litter of seven puppies, all with narcolepsy and cataplexy. “During the first day, each of the puppies collapsed to the ground once,” says Mitler.
It turned out that the disease was inherited in Labradors and Dobermans. Dement decided to focus on Dobermans, and by the end of the 70s he was already the proud owner of an entire colony of dogs of this breed. He established that narcolepsy in Dobermans is caused by the transmission of a single recessive gene. By the 1980s, genetic analysis methods had advanced enough to try to track down the defective Doberman gene.
I will never be able to reconstruct the combination of factors that led to my narcolepsy, but the main thing happened at the moment of my conception in 1972 - around the same time Monique was born in the Canadian province of Saskatchewan. I have inherited a special version of a gene (known as HLA-DQB1*0602) that is involved in a process that helps the immune system distinguish friend from foe.
I have inherited a special version of a gene (known as HLA-DQB1*0602) that is involved in a process that helps the immune system distinguish friend from foe.
The HLA-DQB1*0602 gene is quite common - about one in four Europeans boast a copy - and it plays a key role in many cases of narcolepsy and is present in about 98% of patients with narcolepsy and cataplexy.
In addition to genetics, time also seems to play a role. People with narcolepsy are often born in March (like me). This "birth effect" is also seen in other autoimmune disorders and is likely due to seasonal infections. In the case of narcolepsy, apparently those born in March are just a little more vulnerable than everyone else.
Although other childhood infections, hormonal imbalances and stress may also have contributed, I encountered a key pathogen in late 1993 years old - I was overtaken by the flu virus or possibly a strep infection. It was an autoimmune tipping point that resulted in the rapid destruction of my orexin system. In short, most cases of narcolepsy are the result of an unfortunate set of circumstances that created the ninth immunological wave, the perfect storm.
In short, most cases of narcolepsy are the result of an unfortunate set of circumstances that created the ninth immunological wave, the perfect storm.
Around this time, the Doberman project at Stanford was close to solving the mystery of narcolepsy in this breed. The mutation was hunted down by Emmanuel Mignot, who later succeeded Dement as director of the Stanford Sleep Center. We meet in his office, Mignota accompanies Watson, a narcoleptic chihuahua. “Such a stupid breed,” he says. “I would never choose such a dog for myself.”
At first, Watson is wary of me, keeping his distance. I get down on the floor, he yips and jumps at me, pretending that he is angrier than he is.
I feel empathy, even though his view is an abyss from mine. I know what severe daytime sleepiness is. I know what cataplexy is, I know what it's like when emotions short circuit the neurological network in the brain stem and cause muscle collapse (this happens in REM sleep, that's when we dream most often).
I wonder if Watson is afraid of sleep paralysis and the supernatural hallucinations that often accompany sleep paralysis. The dog's eyelids close and then open again, and I recognize the lethargy in his gaze. He climbs into the basket and curled up asleep during the entire interview.
In the 1980s, the idea of finding the gene responsible for canine narcolepsy seemed extremely ambitious. Breeding narcoleptic Dobermans is a more difficult task than it seems at first glance, since such dogs can fall in the middle of intercourse, temporarily paralyzed by cataplectic trembling (the so-called orgasmolepsy, also happens in humans). And even without taking into account this inconvenience, it was necessary to find a gene whose sequence is unknown in the genome, which at that time was not studied. “Most people said I was crazy,” Mignot recalls. In a way, they were right: it took him over ten years, hundreds of dogs, and over a million dollars. And he almost got ahead of himself.
In January 1998, just as Mignot's team was approaching the finish line, young neurologist Luis de Lecea of the Scripps Institute for Research in San Diego published a paper describing two new brain peptides. De Lecea and his colleagues named them hypocretins, from the hypothalamus where they were found, and from the word secretin, a hormone with a similar structure. These were chemical mediators that functioned exclusively within the brain.
A few weeks later, a team of scientists led by Masashi Yanagisawa from the University of Texas, independently of de Lecea and his colleagues, described the same peptides, but called them orexins, and also presented the structure of their receptors. They hypothesized that the interaction of these proteins with receptors could influence appetite regulation. “We didn’t think about sleep at all,” admits Yanagisawa.
At Stanford, Mignot learned about the publication of two papers, but there was no reason to believe that the discovery had anything to do with narcolepsy or sleep. However, by the spring of 1999, he and his team figured out that the recessive mutation must lie in one of the two genes. One is expressed in the foreskin. "It didn't look like a candidate for narcolepsy," Mignot says. There was a second gene that encoded one of the two orexin receptors. When he learned that Yanagisawa's team had created an orexin-free mouse, and that mouse was now showing symptoms of narcolepsy, the race was on.
However, by the spring of 1999, he and his team figured out that the recessive mutation must lie in one of the two genes. One is expressed in the foreskin. "It didn't look like a candidate for narcolepsy," Mignot says. There was a second gene that encoded one of the two orexin receptors. When he learned that Yanagisawa's team had created an orexin-free mouse, and that mouse was now showing symptoms of narcolepsy, the race was on.
A few weeks later, Mignot and his colleagues published their work in the journal Cell, where they talked about a defect in the gene encoding one of the orexin receptors. "This result suggests that hypocretins (orexins) are important sleep-influencing neurotransmitters, which opens the prospect of new approaches to the treatment of patients with narcolepsy," they wrote. Kalua, one of a litter of Dobermans named after spirits, lies lounging on the cover of the publication. Yanagisawa and colleagues published the results of their experiments two weeks later, also in the journal Cell.
Under normal circumstances, the chemical transmitter and its receptor act like a key and a lock. The key (transmitter) goes to the lock (receptor) to open the door (cause a change in the target cell). In the case of Mignot Dobermans, a large-scale mutation messed up the orexin receptor lock, rendering the orexin useless.
Either the lock does not work, as in this case, or there are no keys, as in the case of the Yanagisawa mice, but the outcome is the same - the door will not open. The orexin system is out of order. In the case of humans, there are many ways to break the orexin system. Sometimes the damage is caused by a brain tumor or a head injury. In most cases, however, narcolepsy is caused by an unfortunate set of circumstances, as described above.
Orexin neurons are a very important thing, and not only for those who have lost them. Almost all major classes of vertebrates have them and perform a very important function. When de Lecea first described orexins in 1998, he was not yet thirty and had just arrived from Barcelona to San Diego.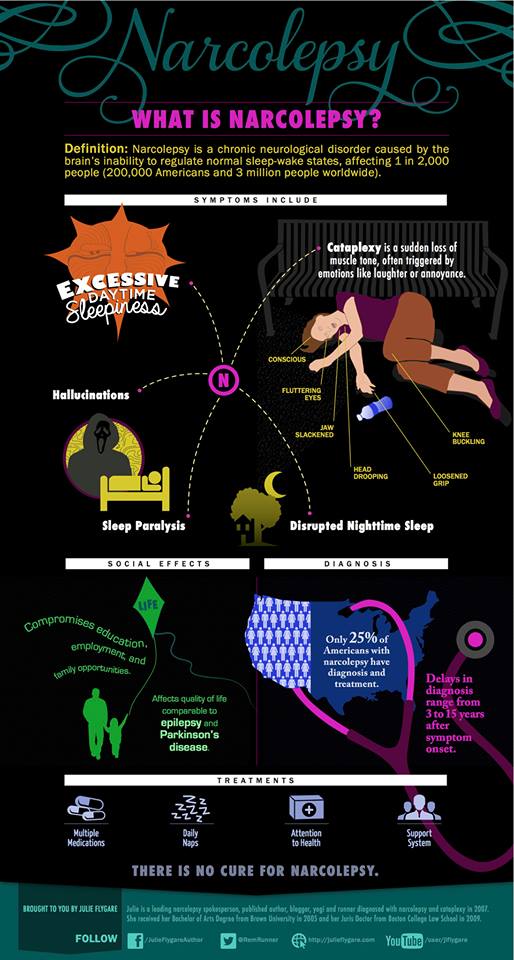 In 2006, he moved to Stanford to be closer to the science of sleep. “To be honest, I thought that now we will understand the system much better than we eventually understand it,” he says.
In 2006, he moved to Stanford to be closer to the science of sleep. “To be honest, I thought that now we will understand the system much better than we eventually understand it,” he says.
However, much has been learned, especially thanks to optogenetics. By introducing a virus, a promoter, and a gene from blue-green algae, it is possible to identify a specific group of light-sensitive neurons.
To illustrate this magic, de Lecea shows a video on his laptop. In the video, we see a mouse that has been genetically programmed to fire its orexin neurons in response to light. A thin fiber optic wire is led to the mouse brain. "The mouse is sleeping," he says, and at the top of the screen we see waves of electrical activity characteristic of deep sleep. The wire comes to life, a bluish flash lasts ten seconds. Light-sensitive orexin neurons release neuropeptides and suddenly the rodent wakes up. When the light is turned off, the mouse falls asleep as quickly as it woke up.
Suddenly my tear ducts tingle, and for a fraction of a second I almost envy this mouse.
Using optogenetics and other methods, de Lecea was able to prove that orexins play an important role in many neurological networks. Sometimes they function as neurotransmitters and help neurons release norepinephrine into the cerebral cortex. In other cases, orexins act more like hormones. This is how orexins affect other chemicals in the brain, including dopamine (which plays a key role in the reward system, in planning and motivation), serotonin (strongly associated with mood and involved in depression), and histamine (an important warning signal).
“Most other neural networks have parallel and multiple layers of security,” de Lecea says. “So if something goes wrong, other systems turn on and take over. In the case of orexins, however, there is little or no safety net.
That is, manipulating this system gives a clear response that scientists can work with. This is an excellent model for understanding how neural networks work in a more general sense.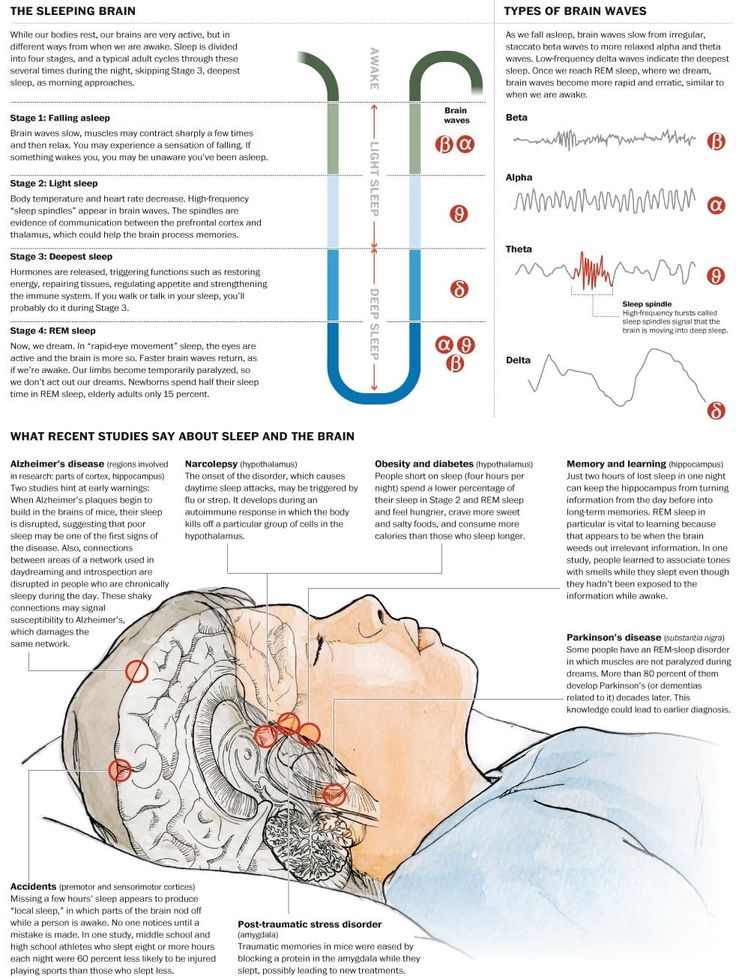 ”
”
What we now know about orexins also helps to explain why the loss of just a few tens of thousands of cells can lead to such a serious multi-symptom disease as narcolepsy, which affects wakefulness and sleep, body temperature, metabolism, appetite, motivation and mood. These proteins give us an exceptional insight into how the human brain works.
And that turns the orexin story into an archetypal double helix tale, and a great illustration of how science works. There is a mystery (narcolepsy), a primordial story (Monique), foresight (Dement), aspiration (Mignot), technological discoveries (genetics), a photogenic animal (Dobermans), a race (with Yanagisawa), looks like science (optogenetics), and yet has high goal (sleep and brain).
It's elements like these that can turn current scientific events into compelling cultural narratives, says Stephen Kasper, a neuroscience historian at Clarkson University in New York. “Here are all the ingredients for what physiologists and neurologists at the beginning of the 20th century were looking for and hoped to find - something that would unite heredity, biochemistry, biophysics, neurology and psychology.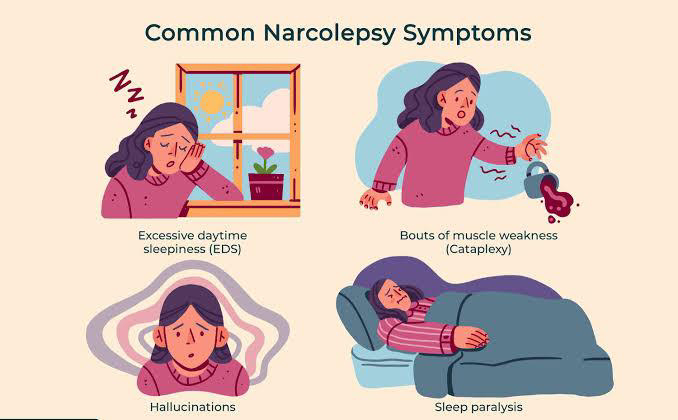 ”
”
“However, there is a tendency in biochemical studies of niche disorders that they are often promising, but never help the patients themselves,” Kasper adds. Something is missing in the narrative around narcolepsy, he says: “A good story should have a clear happy ending.”
We are still waiting for that happy ending.
Even if I could get a bottle of orexin-A and orexin-B, how would I put them in my brain? If I swallowed them in solution, the enzymes in my intestines quickly dealt with them, plucking the amino acids like beads off a necklace. If you inject into a muscle or blood vessel, only a few will pass blood-brain barrier .
Experiments have been done with nasal delivery - it has been suggested that inhaling orexins might be a way to smuggle some of them into the hypothalamus via the olfactory nerve, but no one has made much investment in this approach.
This does not mean that the pharmaceutical industry has ignored the discovery of orexins. Not at all. Fifteen years after Mignot's publication, Merck received approval from the US Food and Drug Administration to market the drug suvorexant (commercial name Belsomra). The substance crosses the blood-brain barrier and blocks orexin receptors. And it is sleeping pills.
Not at all. Fifteen years after Mignot's publication, Merck received approval from the US Food and Drug Administration to market the drug suvorexant (commercial name Belsomra). The substance crosses the blood-brain barrier and blocks orexin receptors. And it is sleeping pills.
Sleeping pills are not exactly what people with narcolepsy needed. By preventing orexins from binding to receptors, the drug provides a completely narcoleptic onset - but the fog from it dissipates in the morning. Sleeping pills, commonly used to treat insomnia, depress the nervous system as a whole, says Paul Coleman, a chemist at Merck's Philadelphia lab. “Suvorexant differs in that it very selectively blocks wakefulness without affecting systems that control balance, memory, and thought processes,” he says.
Coleman developed drugs to treat a number of different infections, diseases, and disorders, but the orexin system stands apart. “Narcolepsy has given us a thread that we can pull and unravel the tangle of knowledge about what is behind the system that controls sleep and wakefulness,” says the chemist.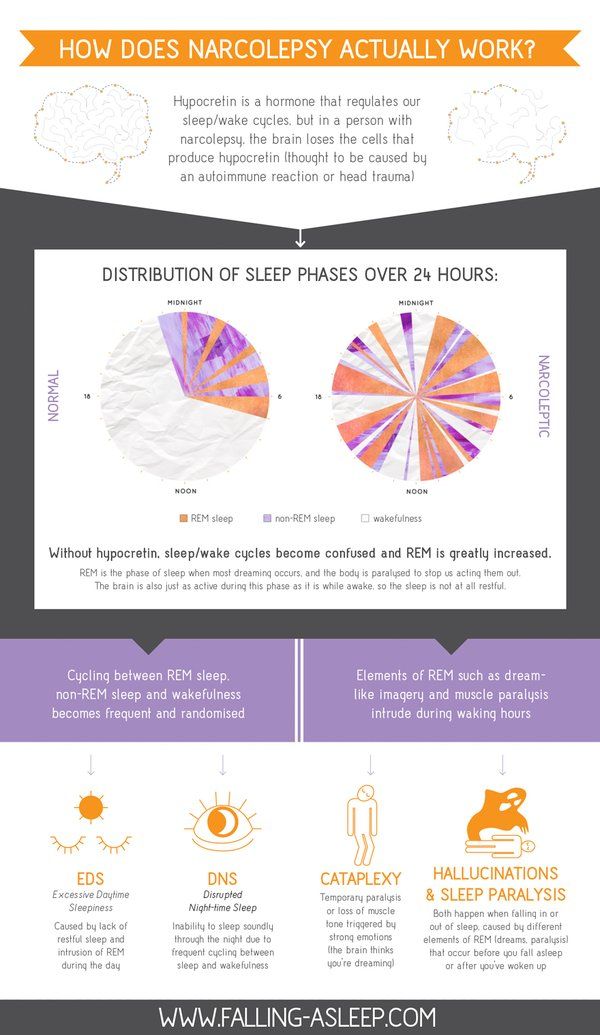 “Waking is a pretty key process for all of us, whether you are healthy or have insomnia or narcolepsy. It's the most interesting thing I've ever worked on."
“Waking is a pretty key process for all of us, whether you are healthy or have insomnia or narcolepsy. It's the most interesting thing I've ever worked on."
The use of suvorexant could be expanded, with clinical trials planned for its ability to provide quality daytime sleep for shift workers, improve sleep for Alzheimer's patients, help those suffering from post-traumatic disorder and drug addiction, and alleviate the symptoms of panic disorder.
I'm glad to see this news, but we, millions of people with narcolepsy, are still waiting for a drug that will shake up rather than subdue the orexin system.
Masashi Yanagisawa has been working on this for a long time, who competed with Mignot 20 years ago to link orexins to narcolepsy. But designing and synthesizing a substance that will pass intact through the gut—which is exactly what it takes to get it from the blood to the brain—and that has the perfect configuration to activate one or both of the orexin receptors—“is a very, very big challenge,” he says.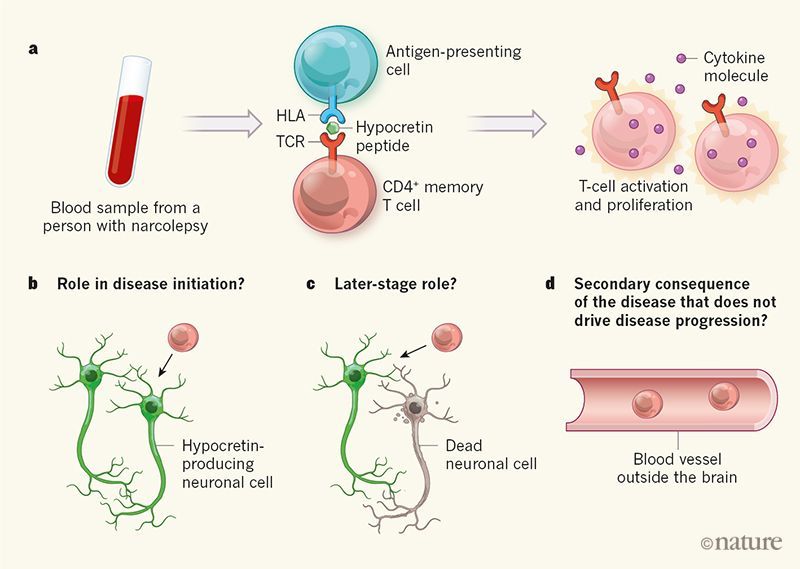 This is "significantly" more difficult than finding a compound that inhibits the receptor, as suvorexant does.
This is "significantly" more difficult than finding a compound that inhibits the receptor, as suvorexant does.
Earlier this year, Yanagisawa and his colleagues published data on the most powerful such compound to date, the small molecule YNT-185. The introduction of this molecule into narcoleptic mice significantly improves their wakefulness and reduces the excess of REM sleep (this is one of the characteristics of narcolepsy). And while the affinity of YNT-185 (how strongly it binds to the orexin receptor) is not enough to warrant clinical trials, Yanagisawa's team has already identified a number of other potential candidates. “The best of them is almost a thousand times stronger than YNT-185,” he boasts. Although the symptoms of narcolepsy can vary widely from person to person, the underlying pathology—the absence of orexins—remains the same. “If this compound works, it will work for all patients. In that sense, it will be a relatively simple clinical trial compared to many other disorders,” says Yanagisawa.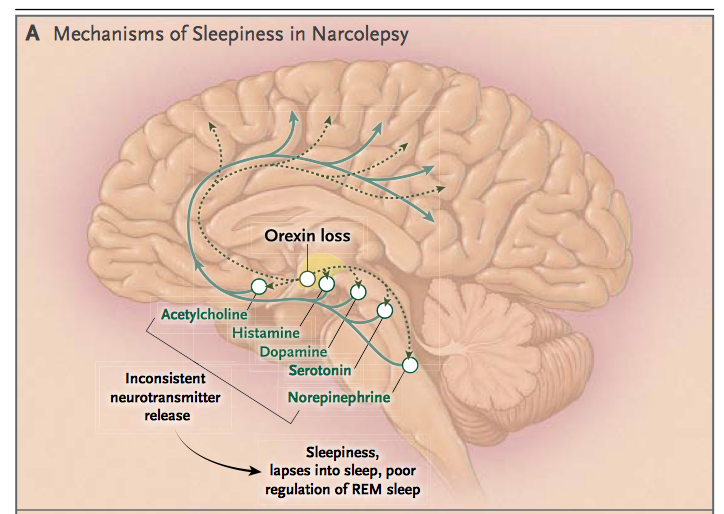
An even more futuristic perspective involves stem cells.
Sergiu Pasca occupies the office next to Emmanuel Mignot at Stanford, and in 2015 he and colleagues developed a way to take induced pluripotent stem cells made from skin cells and send them to a new life as brain cells.
In theory, an orexin neuron could be grown and transplanted into the brains of people with narcolepsy. However, everything is not so simple. Firstly, it is unlikely that the cells themselves will be exactly the same as orexin cells, secondly, the introduction of a needle into the brain is a risk, and thirdly, there is always a chance that the immune system will make another attack - now on transplanted cells.
So, will the orexin tale have a happy ending? Translating basic research into clinics is difficult and expensive, Kasper notes.
The cost of the optimally available drug for narcolepsy - sodium hydroxybutyrate - is such that not every patient can afford it, although the drug is one of those that can qualitatively change the lives of many people.

It is widely believed that narcolepsy is a rare disorder with a small market, so any pharmaceutical research and development in this area is unlikely to generate significant revenue. This view ignores the fact that narcolepsy is likely to be undiagnosed for many people, and that a person who develops narcolepsy as a teenager and lives to be 80 years old will need approximately 25,000 doses of medication in their lifetime.
An orexin-stimulating drug may also be useful in any disease characterized by excessive daytime sleepiness, not to mention a myriad of other situations where low orexin levels play a role—including obesity, depression, post-traumatic stress disorder, and dementia.
I believe there is another reason why this story has not yet come to an end.
For far too long we have underestimated sleep as an uncomfortable distraction from being awake. With this mindset, sleep research does not seem to be a priority. But this is far from a rational approach.