Is hsp contagious
Kids Health Information : Henoch-Schönlein purpura (HSP)
Henoch-Schönlein purpura (hee-nok shon-line per-per-a), or HSP, is a condition where blood vessels become inflamed (irritated and swollen). HSP usually affects the small blood vessels in the skin, causing a rash that is called purpura. It can also affect blood vessels in the intestines and the kidneys. HSP can lead to complications in the lungs or brain, but this is extremely rare.
The cause of HSP is unknown, but it is most commonly triggered by a viral illness (e.g. a cold), and it occurs most often in the spring.
HSP usually affects children from two to 10 years of age, but it can happen in anyone. HSP itself is not contagious, but the infection that has triggered HSP may be contagious. There is no known way to prevent HSP.
Signs and symptoms of HSP
The signs of HSP can take days to weeks to fully develop. The distinctive rash almost always occurs in HSP, but is not always the first symptom to develop.
If your child has HSP, they may have:
- a skin rash, which looks like small bruises or small reddish-purple spots – it's usually seen on the bottom, legs and around the elbows
- swelling of the feet and hands, and the scrotum in male children
- pain in the joints, such as the knees and ankles
- stomach pain
- blood in the faeces (poo) or urine (wee), caused by the blood vessels in the bowel and the kidneys becoming inflamed.
In rare cases, an abnormal folding of the bowel (called intussusception) can occur. This causes a blockage in the intestines that may need surgery.
When to see a doctor
If you think your child has HSP, take them to see your GP.
Take your child back to the GP if they have HSP and they have increasing pain or swelling, blood in their stools or urine, or if you are worried at all.
If your child is unwell with a fever and a skin rash (small bright red spots or purple spots or unexplained bruises) that does not turn to skin-colour (blanch) when you press on it, this may be a sign of meningococcal infection (see our fact sheet
Meningococcal infection).
Treatment for HSP
Your child may not need any medicines; however, the GP may prescribe a drug called prednisolone to help with severe stomach pains or very painful joints. Prednisolone may also be helpful in preventing kidney problems. In some cases, your doctor may prescribe medicines to treat the infection that triggered HSP.
Care at home
HSP usually gets better on its own without causing lasting problems. You can give your child pain relief (e.g. paracetamol) or an anti-inflammatory pain reliever (e.g. ibuprofen) to help relieve the joint pain and general discomfort. See our fact sheet Pain relief for children.
Follow-up
Long-term follow-up with your doctor is very important. About 50 per cent of children who have had HSP will get it again. A few children will have kidney damage because of HSP, which may happen in the first week or so of illness, but there may be a delay of weeks or months before
it appears. Your child's doctor will want to test urine samples and blood pressure several times after the HSP goes away, and this is to check for kidney problems. These checks should continue for at least six months, with a final check at 12 months.
These checks should continue for at least six months, with a final check at 12 months.
Key points to remember
- HSP causes inflammation of the small blood vessels in the skin, causing a rash.
- HSP can also affect blood vessels around the kidneys and intestines.
- Paracetamol and anti-inflammatory medicines can help painful joints.
- See your GP if your child has increasing pain, swelling, blood in the stools or urine, or if you are worried at all.
- Long-term follow-up with your doctor is very important.
For more information
- Better Health Channel: Henoch-Schonlein purpura
- See your GP.
Common questions our doctors are asked
Are there any natural remedies you recommend for HSP?
No - there are no natural remedies that have been shown to be adequately effective in the treatment of HSP.
Is it safe to give my child prednisolone?
You may have heard about possible side effects from
prednisolone. These side effects happen when the medicine is given for months
at a time, and will not happen when the prednisolone is given for just a few
days.
These side effects happen when the medicine is given for months
at a time, and will not happen when the prednisolone is given for just a few
days.
Is my child likely to get HSP again?
In roughly half of patients, HSP will occur again, at least once – and usually within four months from the first episode. Each following episode is usually shorter and milder than the first.
How long will it take my child to recover from the symptoms of HSP?
In a simple, first
episode of HSP, symptoms should resolve within four weeks, with the rash being
the last symptom to disappear. Joint pain usually stops after three days, and
abdominal pain will usually stop after two days.
Developed by The Royal Children's Hospital General Medicine department. We acknowledge the input of RCH consumers and carers.
Reviewed March 2018.
This information is awaiting routine review. Please always seek the most recent advice from a registered and practising clinician.
Kids Health Info is supported by The Royal Children’s Hospital Foundation. To donate, visit www.rchfoundation.org.au.
Henoch-Schonlein Purpura - HealthyChildren.org
Log in | Register
Health Issues
Health Issues
Henoch-Schonlein purpura (HSP) is disease that causes small blood vessels to become swollen and irritated—a condition called vasculitis.
It is most common in children between the ages of 3 and 15 years old and is rarely seen in adults. HSP is not contagious and tends to affect boys more than girls.
Cause
The actual cause of HSP is not known. About half the time, however, children who get HSP have a cold or respiratory infection such as strep throat beforehand. HSP has also been linked to bug bites, cold weather, and some vaccinations.
Signs & Symptoms
Usually, the first sign of HSP is a rash called palpable purpura that appears as dark reddish splotches on the feet, legs, and buttocks. A child with HSP may also have joint pain, abdominal pain, and/or kidney problems.
Rash
Nearly every child diagnosed with HSP has a painless rash. The rash usually starts as raised wheals, reddish blotches, and little red dots (petechiae) around the feet and ankles. The rash may also be on the legs and buttocks. In smaller children—especially those who do not yet walk—the rash is often seen on the arms, trunk, and face. The rash usually takes about 10 days to fade.
Joint Pain
The majority of children with HSP experience joint pains. Children typically only have a few affected joints—hips, knees, and ankles. While the joints may swell for 1-3 days, there is no permanent damage.
Abdominal Pain
About 50% of children with HSP will have abdominal pain. Abdominal problems may be fairly mild (e. g., nausea, vomiting, and mild pain). In rare occasions, abdominal problems are much more serious and involve gastrointestinal bleeding or intussusception. Intussusception is when the intestine folds in on itself and may become blocked. Abdominal pain tends to come on about a week after the rash first develops.
g., nausea, vomiting, and mild pain). In rare occasions, abdominal problems are much more serious and involve gastrointestinal bleeding or intussusception. Intussusception is when the intestine folds in on itself and may become blocked. Abdominal pain tends to come on about a week after the rash first develops.
Kidney Problems
About 25% to 50% of children with HSP will have kidney problems. Usually, kidney problems due to HSP begin within days to 6 weeks after the rash first appears.
The most common kidney problem seen is blood in the urine. Blood is the urine is not usually visible to the naked eye. About 10% of the time, the urine becomes red or brown from blood. Up to 50% of patients also lose protein in the urine, and about 20% of the time protein lost is excessive.
Excessive loss of protein in urine requires the help of a pediatric nephrologist. Losing a lot of protein means a child is at risk for more serious problems—kidney damage and high blood pressure. Sometimes a pediatric nephrologist will perform a kidney biopsy to look at how severely a HSP affects a child's kidneys.
Sometimes a pediatric nephrologist will perform a kidney biopsy to look at how severely a HSP affects a child's kidneys.
Diagnosing HSP
The diagnosis of HSP is almost always based on symptoms. Your pediatrician may do blood and urine tests to help rule out other conditions and to check kidney function. There is not a specific blood test to diagnose HSP. An abdominal ultrasound may be done in patients with severe abdominal pain. In patients who have partial or unusual symptoms, a biopsy of the skin or the kidney may help make the diagnosis.
Treatment
HSP is a mild illness, so it is usually treated with rest, fluids, and over-the-counter pain medicines such as acetaminophen (Tylenol). In severe cases, a child may need to be hospitalized.
Once the symptoms of HSP disappear, children should have their urine checked for blood and protein for at least 6 months after they are first diagnosed—even if their urine was normal at first. This is to make sure that the disease did not damage a child's kidneys and that they are working properly. Sometimes, HSP in the kidneys persists or comes later and may need additional treatment.
Sometimes, HSP in the kidneys persists or comes later and may need additional treatment.
Outlook
Most of the time, HSP improves and goes away completely within a month. Sometimes HSP relapses; this is more common when a child's kidneys are involved. If HSP does come back, it is usually less severe than the first time.
The long-term prognosis of HSP largely depends on whether the kidneys have been involved and, if so, how severe the involvement is.
Additional Information from HealthyChildren.org:
What is a Pediatric Nephrologist?
Rashes and Skin Conditions
Blood in Urine (Hematuria)
When to Keep Your Child Home from Child Care
- Last Updated
- 3/9/2017
- Source
- Section on Nephrology (Copyright © 2017 American Academy of Pediatrics)
The information contained on this Web site should not be used as a substitute for the medical care and advice of your pediatrician.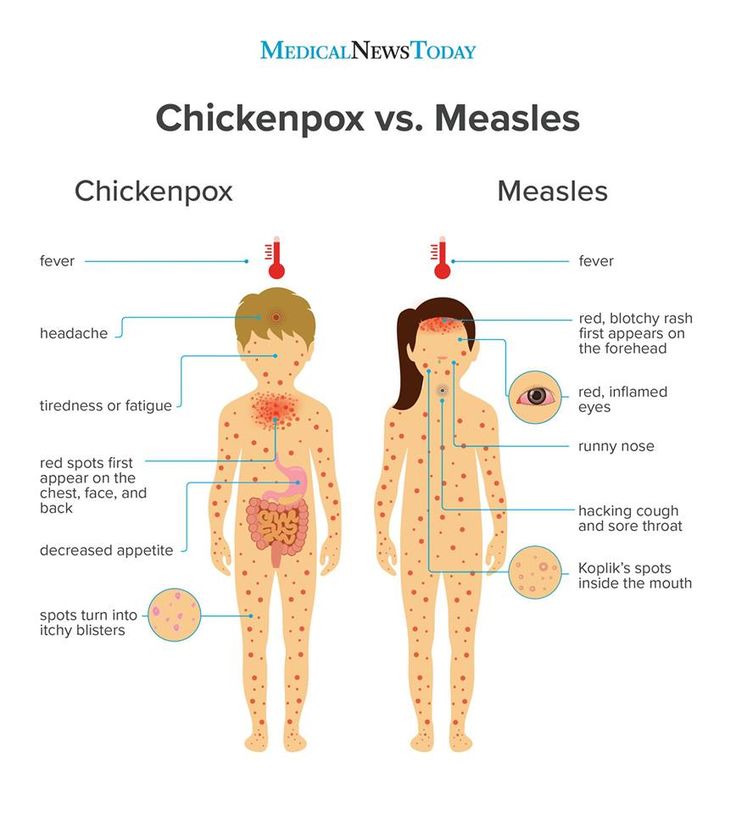 There may be variations in treatment that your pediatrician may recommend based on individual facts and circumstances.
There may be variations in treatment that your pediatrician may recommend based on individual facts and circumstances.
In all lungs: "Centaur" turned out to be more dangerous than other sub-variants of "Omicron"
Photo: Depositphotos
Foreign scientists have concluded that "Centaur" (BA.2.75) leads to more severe respiratory disease than other strains of "Omicron". According to a study in laboratory animals, this occurs through accumulation in the lower respiratory tract. In addition, this subvariant has an increased ability to enter human cells and resist antibodies, making it highly contagious. Rospotrebnadzor told Izvestia that the impact of the Centaur sub-option on the COVID-19 epidemiological processin Russia it is minimal, but experts warn: it is impossible to predict how the next subspecies of the virus will behave.
Very contagious
Japanese scientists from Kobe University and Toyama University have created a mathematical model to predict the infectivity of different variants of SARS-CoV-2. Based on it, they disassembled the risk of the spread of newly emerged variants of SARS-Cov-2. In particular, the researchers studied the coronavirus S-protein responsible for binding to the ACE2 enzyme, through which the pathogen enters the host's body. It is called a spike for its characteristic shape.
Based on it, they disassembled the risk of the spread of newly emerged variants of SARS-Cov-2. In particular, the researchers studied the coronavirus S-protein responsible for binding to the ACE2 enzyme, through which the pathogen enters the host's body. It is called a spike for its characteristic shape.
According to the authors of the work, two factors play a leading role in the level of infectivity of a strain - the ability of the variant to penetrate into cells and how effective neutralizing antibodies that appear naturally or after vaccination are against it.
It turned out that, firstly, the S-protein in BA.4/5 or BA.2.75 is significantly different from the wild Wuhan strain than in other variants of the coronavirus. The greater this difference, the higher the chance that the strain will cause a new outbreak of coronavirus, because the antibodies that people have against it will not work or their effect will be weaker. Secondly, the BA.2.75 spike proved to be the most effective in terms of docking with ACE2.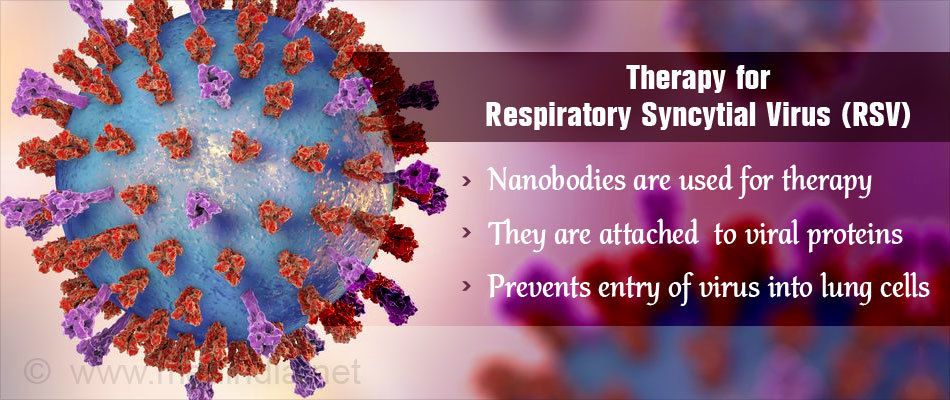
BA.2.75 has a high ability to penetrate human cells, while modern vaccines are much less effective in this variant. These results suggest that infection with BA.2.75 may be stronger than previously existing variants,” the authors conclude. named after M. V. Lomonosov Roman Zinovkin
This is how they gain a competitive advantage and crowd out other strains. Obviously, this is good for the virus, but bad for us,” the virologist added. "Hemotest", Doctor of Biology, Professor of the Department of Microbiology and Virology of the RUDN Medical Institute Oksana Gizinger Therefore, we can confidently say that "Centaur" is more resistant to the already existing immunity against coronavirus.0003
Seriously
on Syrian hamsters, which have become model animals for the study of coronavirus. The scientists compared the results with those obtained for strains BA.2 and BA.5.
Interestingly, most of the animals infected with BA.
2.75 gained weight during the six day experiment, as did the animals infected with BA.2, BA.5. The researchers measured virus titers in the animals' lungs and analyzed their samples using histology.
The replication capacity of BA.2.75 in hamster lungs was higher than that of BA.2 and BA.5. Of note, BA.2.75 caused focal viral pneumonia in hamsters, which was not observed in BA.5-infected rodents. Moreover, BA.2.75 replicated better than BA.5 in hamster lungs,” the authors concluded.
Where BA.5 and BA.2.75 circulate together, the prevalence of BA.2.75 grows faster. Thus, BA.2.75 is a likely candidate for worldwide dominance, unless a new variant emerges with even higher prevalence. In addition, BA.2.75 causes more severe respiratory illness by accumulating in the lower respiratory tract, according to studies in hamsters.
You can often hear that the virus gradually loses its pathogenicity and becomes less dangerous.This is true, but the process is not so fast, it usually takes decades. In addition, this is true rather for a virus with a high lethality - tens or more percent. For SARS-CoV-2, there is no particular difference: it will kill a little more people or a little less, it simply does not notice it. I think in the near future there will be small changes in terms of the danger of coronavirus. We were relatively lucky with Omicron - basically everyone carried it easily. It is impossible to predict what will happen with the next dominant option," Roman Zinovkin told Izvestiya.0035
Oksana Gizinger noted that such results give reason to think that infection with sub-variant BA.2.75 will be approximately the same in severity as from Stealth-Omicron.
A number of other researchers suggest that VA 2.75 may cause a milder disease, but at the expense of infectivity affect large groups of the population," the doctor added.
The VGARus database contains 35 sequences classified as sub-variant BA 2.
75 (Centaur), Rospotrebnadzor told Izvestia.0003
We emphasize that over the past two weeks, the sequences assigned to the indicated sub-strain of the Omicron strain have not been entered into the database. The influence of the Centaur subvariant on the epidemiological process for COVID-19 in Russia is minimal," the ministry said.
Omicron" (with a predominance of the sub-variant BA.5). Over the past two weeks, 1.6% of the total number of sequences were assigned to the previously dominant subline BA.2 of the strain "Omicron", more than 98%. New genomic sequences assigned to subline BA.2.75 ("Centaur") of strain "Omicron", as well as to the hybrid variant of COVID-19 "Deltacron", were not entered into the VGARus database.
To date, not a single laboratory in the Russian Federation detects this strain - there are no test systems. The exception is research laboratories accredited by the RPN, but they do not provide results to either patients or doctors.Thus, it is not possible to associate the course of the disease with the Centaur strain," explained Anna Safonova, director of product policy at the LabQuest medical laboratory, doctor of clinical laboratory diagnostics.
In Russia, the incidence of coronavirus has been on the rise since mid-July. At the same time, the mortality rate remains extremely low: for example, with almost 51 thousand new cases registered at the end of the week, 89 deaths were recorded.
In order to protect yourself from a serious illness, it is necessary, firstly, to strengthen your general health and immunity, advised Oksana Gizinger. The doctor's second recommendation is to follow a vaccination schedule to maintain an immune response against the new coronavirus.
Doctors of the Orenburg steppes - Our Urals and the whole world
- Poster
- Ural
Log in
Welcome! Log in to your account
Your username
Your password
Have you forgotten your password?
Privacy policy
Password recovery
Retrieve your password
Your email address
A long time ago, the Great Silk Road ran through the territory of the Orenburg steppes.
It carried goods that could be called the "currency" of the past - silk, spices, furs. But along its entire length there was also a cultural exchange, because not only merchants passed along this road. Among the travelers there were priests, teachers and even healers. Many of them started a new life in the villages they liked.
Wise books on the treatment of diseases, effective potions or medical instruments can be found today in local history museums of the Orenburg region. The guides say that each nomadic tribe had its own healers. The healers of nomadic peoples were well aware of the properties of steppe herbs, but at the same time they used conspiracies, rubbing, and even carried out operations.
author of the photo: Sergey Zhdanov. Other works of the author can be viewed here: https://www.facebook.com/profile.php?id=100006482532819Healers-nomads received their knowledge, among other things, through acquaintance with Arabic, Greek medicine, studies of human anatomy and physiology.
author of the photo: Sergey Zhdanov. Other works of the author can be viewed here: https://www.facebook.com/profile.php?id=100006482532819For the first time, the secrets of Kazakh folk medicine were described by the doctor A. Yamgin in the middle of the 19th century. He participated in the Russian-Kyrgyz expedition and saw with his own eyes the results when using certain steppe herbs. So, according to his observations, Kazakh healers use rhubarb for intestinal diseases, juniper used for urinary infections, and licorice roots for coughing. Interestingly, modern doctors prescribe these same herbs in addition to pharmaceuticals.
For centuries, healers of the steppes formed traditions in the treatment of certain diseases - this is how terms appeared, as well as the classification of diseases. They separated diseases of the organs (heart, lungs) or diseases from the cause: diseases from cold, diseases from heat, diseases from fatigue. One of the sayings of the ancient steppe healers has come down to us, which said: "Except for a fracture, everything is contagious.
author of the photo: Sergey Zhdanov. Other works of the author can be viewed here: https://www.facebook.com/profile.php?id=100006482532819" And this suggests that they had extensive knowledge in the field of virology. Kazakh physicians have long used natural antibiotics for wounds, ulcers and inflammations. Surprisingly, those diseases that in our time are treated only with the help of operations, the Kazakhs treated by other methods. For example, a diseased organ was covered with camel hair, previously moistened with cold water. The place was bandaged, and after some time the bandage was removed, the diseased organ was restored. (This is how the doctor A. Yamgin described the process.)
Koumiss was widely used for various diseases, which has bactericidal properties, including against Escherichia coli and other pathogenic microbes. It is known that this drink strengthens the immune system and activates many processes.
author of the photo: Sergey Zhdanov. Other works of the author can be viewed here: https://www.