Ptsd most common age group
What Age Group Shows The Most PTSD? Statistics On Post-Traumatic Stress Disorder
Research indicates that 3.6% of those 18 and older in the United States alone live with post-traumatic stress disorder or PTSD per year. PTSD is considered a common mental health disorder, but there are some misunderstandings about post-traumatic stress disorder and what it is. There are many stereotypes and assumptions made about PTSD. One of the most common assumptions made about PTSD is that it affects adults in the military and does not affect anyone else. This could not be more or false; post-traumatic stress disorder is a disorder that can affect anyone who has experienced a traumatic event, and it affects people of all ages. So, what age group shows the most PTSD? In this article, we will go over the average age of onset for post-traumatic stress disorder and other PTSD statistics.
What Is PTSD?
Post-traumatic stress disorder or PTSD is a mental health condition or disorder that can develop after a traumatic event. Not all, or even most, survivors of traumatic events go on to develop post-traumatic stress disorder, but it is a disorder that is born out of trauma in some people
Symptoms or signs of post-traumatic stress disorder include but are not limited to:
- Hypervigilance
- Re-experiencing traumatic events, whether that is through flashbacks, nightmares, or something else
- Irritability or agitation
- Trouble sleeping or insomnia
- Social withdrawal or isolation from others
- Trouble focusing or concentrating
- Difficulty trusting other people
- Emotional detachment
- Feelings of guilt
- Self-destructive behaviors
Diagnostically speaking, to be diagnosed with post-traumatic stress disorder, you have to have experienced or witnessed a traumatic event. Symptoms of PTSD must affect your life and ability to function in social relationships or social situations, work, school, self-care, and so on to be diagnosed. It is normal to experience emotional consequences after trauma, but PTSD is more severe, and the impact is long-lasting. The good news is that post-traumatic stress disorder is a treatable condition. There are several studied treatments for post-traumatic stress disorder, including therapies such as cognitive-behavioral therapy or CBT and eye movement desensitization and reprocessing therapy or EMDR. For all information regarding specific treatments and therapies, make sure to speak with a medical or mental health professional who can give you individual medical or mental health advice.
It is normal to experience emotional consequences after trauma, but PTSD is more severe, and the impact is long-lasting. The good news is that post-traumatic stress disorder is a treatable condition. There are several studied treatments for post-traumatic stress disorder, including therapies such as cognitive-behavioral therapy or CBT and eye movement desensitization and reprocessing therapy or EMDR. For all information regarding specific treatments and therapies, make sure to speak with a medical or mental health professional who can give you individual medical or mental health advice.
What Age Group Shows The Most PTSD?
Statistics from the national institute of Mental Health NIMH suggest that individuals aged 45 to 59 have the highest prevalence of post-traumatic stress disorder, followed by those aged 18 to 29. Here are the percentages found in those studies:
- 4% of People ages 18 through 29 have post-traumatic stress disorder.
- 5% of people aged 30 to 44 have post-traumatic stress disorder.
- 3% of those 45 through 59 have post-traumatic stress disorder.
- 1% of those aged 60 or older have post-traumatic stress disorder.
It is important to note that children can also experience PTSD. Symptoms of PTSD and children can differ from those seen in adulthood with post-traumatic stress disorder PTSD. Though some symptoms are the same, children might experience other symptoms, such as reenacting traumatic events through play. Sources say that, out of the children who experience trauma, the development of post-traumatic stress disorder in kids is more likely to occur in girls than in boys. More specifically, 3%-15% of girls and 1-6% of boys develop PTSD after a traumatic event.
Other PTSD Facts and Statistics
Here are some other facts and statistics about post-traumatic stress disorder that might surprise you:
- Again, post-traumatic stress disorder impacts people of different genders disproportionately, in both children and adults—the reason why is unknown.
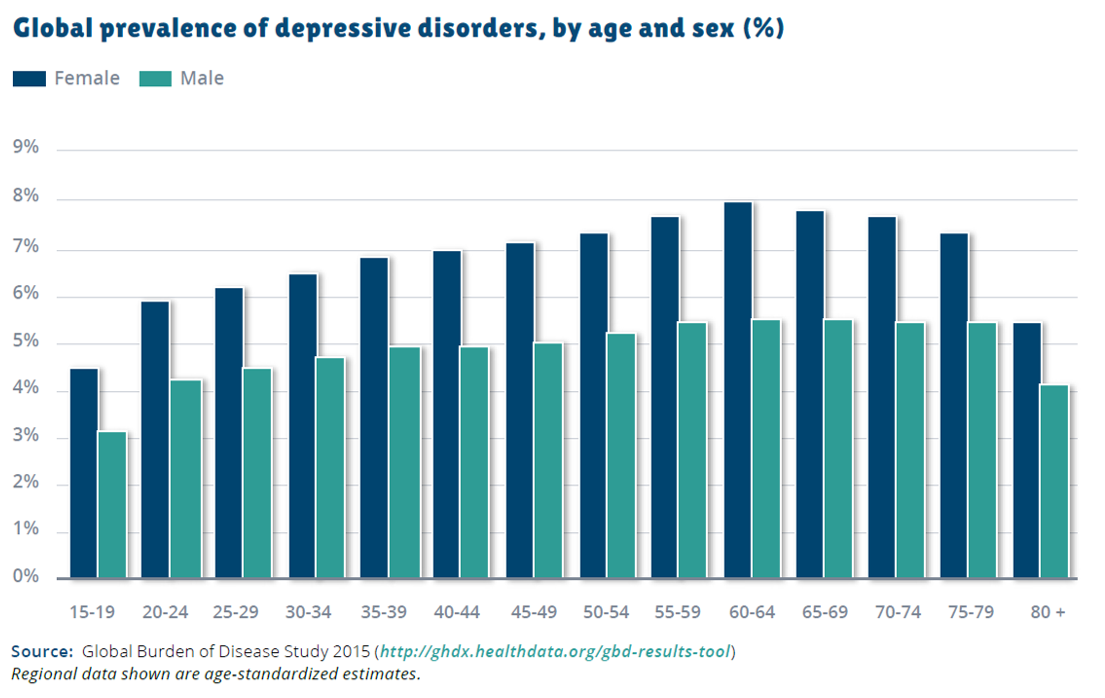
 Post-traumatic stress disorder is more common in females than in males, though it can affect all genders. More specifically, 5.2% of females experience PTSD, whereas 1.6% of males experience PTSD. That is where the statistic of 3.6% of all individuals is born.
Post-traumatic stress disorder is more common in females than in males, though it can affect all genders. More specifically, 5.2% of females experience PTSD, whereas 1.6% of males experience PTSD. That is where the statistic of 3.6% of all individuals is born. - Many people living with post-traumatic stress disorder have a comorbid mental health condition. Common comorbidities seen in post-traumatic stress disorder include anxiety disorders, substance use disorder, and depressive disorders.
- Before the most recent version of the diagnostic and statistical manual of mental disorders, the DSM-5, PTSD was diagnosed as an anxiety disorder. It is now diagnosed under a new category, which is called "trauma and stressor-related disorders."
- There are many different potential causes of PTSD. These causes include but are not limited to car accidents, illness or injury, sexual assault, natural disasters, domestic violence, witnessing violence, and more.
- According to the National Institute on Mental Health NIMH, 36.
 6% of those living with post-traumatic stress disorder experience serious impairment, while 30.2% experience moderate impairment, and 33.1% experience mild impairment. This statistic is derived from the prevalence of the impact of PTSD over a year, so the current numbers may differ.
6% of those living with post-traumatic stress disorder experience serious impairment, while 30.2% experience moderate impairment, and 33.1% experience mild impairment. This statistic is derived from the prevalence of the impact of PTSD over a year, so the current numbers may differ. - Roughly, 30%of veterans are said to have post-traumatic stress disorder.
PTSD Support
There are several ways that you can gain support for post-traumatic stress disorder or PTSD. Of course, treatment is the most important thing to pursue if you are experiencing post-traumatic stress disorder symptoms that are affecting your life. Peer support, in conjunction with therapy, can be highly beneficial as well. It is never a replacement for treatment, but peer support does have a special place because it provides individuals living with post-traumatic stress disorder or other mental health disorders with a sense of community and understanding.
Finding Peer Support
Here are some ways to find peer support for post-traumatic stress disorder:
Visit Post-Traumatic Stress Disorder Forums Online:
There are several support forums online that you can use. Where support groups meet at specific times, forums can often be used anywhere at any time, as long as you have an Internet connection. Here are some active online forums for people living with post-traumatic stress disorder:
My PTSD forum
My PTSD forum is an online forum-based community for those living with post-traumatic stress disorder.
The mentalhealthforum.net Post-Traumatic Stress Disorder Forum
Mentalhealthforum.net is a website with forums for various mental health conditions and concerns, including anxiety disorders, depression, post-traumatic stress disorder, and more.
The Beyond Blue PTSD and Trauma Forum
Beyond Blue is an Australian-based organization.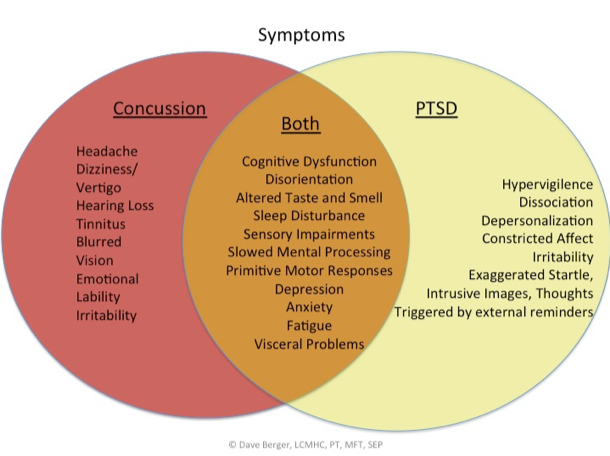 Their website has mental health forums, including one for post-traumatic stress disorder and trauma, among other resources. Click here to go to the Beyond Blue post-traumatic stress disorder forum.
Their website has mental health forums, including one for post-traumatic stress disorder and trauma, among other resources. Click here to go to the Beyond Blue post-traumatic stress disorder forum.
The psychforums.com Post-Traumatic Stress Disorder Forum
Like mentalhealthforum.net, psychforums.com is a website with various forums for many mental health conditions or concerns, including anxiety disorders, obsessive-compulsive disorder (OCD), depressive disorders, post-traumatic stress disorder, and more. Click here to go to the psychforums.com post-traumatic stress disorder forum.
Find a Support group In Your Area
To find a support group near you, you may ask a trauma-informed mental health provider who specializes in trauma or post-traumatic stress disorder for recommendations. Another way to find a support group in your area is to search for "trauma support groups near me" or "PTSD support groups near me" using your search engine of choice. In some cases, you will find support groups for PTSD or trauma surrounding specific sources of trauma. For example, if you have survived a car accident, you may be able to find a group of car accident survivors. The same is true for other traumas, like domestic violence and natural disasters.
In some cases, you will find support groups for PTSD or trauma surrounding specific sources of trauma. For example, if you have survived a car accident, you may be able to find a group of car accident survivors. The same is true for other traumas, like domestic violence and natural disasters.
No matter what route you take, make sure to remember that it is possible to heal from post-traumatic stress disorder. If you are searching for a counselor or therapist in your area, there are several ways that you can go about finding one. You may decide to go to your doctor and ask for a referral to a therapist or counselor. Another option is to search the web for "trauma therapist near me" or "PTSD counselors near me" using your search engine of choice. If you are interested in remote therapy or services, consider using an online therapy company like Better Help.
Take the Mind Diagnostics PTSD Test
Are you wondering if you could have symptoms of post-traumatic stress disorder or PTSD? If so, consider taking the Mind Diagnostics post-traumatic stress disorder test. Although taking the test is not a replacement for a diagnosis from a medical or mental health professional, the Mind Diagnostics post-traumatic stress disorder test can give your insight into your symptoms and what you're going through, and taking the test might just be the first step to getting the help that you need. While PTSD can affect people of all ages, the Mind Diagnostics post-traumatic stress disorder test is for those aged 18 and older.
Although taking the test is not a replacement for a diagnosis from a medical or mental health professional, the Mind Diagnostics post-traumatic stress disorder test can give your insight into your symptoms and what you're going through, and taking the test might just be the first step to getting the help that you need. While PTSD can affect people of all ages, the Mind Diagnostics post-traumatic stress disorder test is for those aged 18 and older.
To take the Mind Diagnostics post-traumatic stress disorder test, click the following link or copy and paste it into your browser: https://www.mind-diagnostics.org/ptsd-test.
Frequently Asked Questions (FAQs)
What are 5 statistics about PTSD?
What percent of the population has PTSD?
Who suffers from PTSD the most?
How much has PTSD increased over the years?
Why is PTSD more common now?
What age group is most affected by PTSD?
Is PTSD a mental illness or disorder?
Is PTSD a disability?
Is PTSD curable?
Why do psychologists believe PTSD is overdiagnosed?
51 PTSD Statistics & Facts: How Common Is PTSD?
Key PTSD Statistics & Facts
- An estimated 70% of adults in the United States have experienced at least one traumatic event in their lifetime.

- Up to 20% of these people go on to develop post-traumatic stress disorder.
- An estimated 5% of Americans – more than 13 million people – have PTSD at any given time.
- Around 8.7% of all adults – 1 in 13 people in the U.S. will develop PTSD at some point in their lifetime.
- Around 3.6% of adults in the U.S. suffer from PTSD in a given year.
- Approximately 1 in 9 women will get PTSD at some point in their lifetime, and women are around twice as likely as men to develop the disorder.
- Surprisingly, 23% of women in the military report being sexually assaulted. And 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.
- Researchers found the estimated prevalence of PTSD among veterans ranges from 1.09% to 34.84%.
- Post-traumatic stress disorder (PTSD) can occur after any traumatic event, not only trauma from wartime.
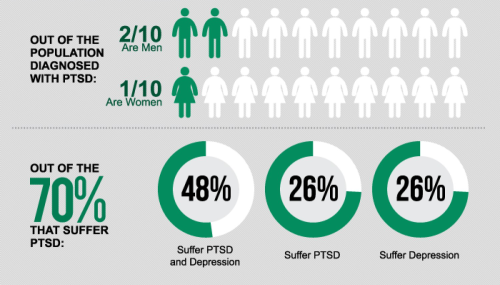
- 16% of emergency physicians meet diagnostic criteria of PTSD.
- Around 5% of adolescents experience PTSD.
PTSD Prevalence: How Common Is PTSD?
| Statistic | Data |
| % Of Americans Who’ve Experienced At Least One Traumatic Event | 70% |
| % Of Americans Who Have PTSD | 5% |
| % Of American Adults Who Have PTSD | 5% (More Than 13 Million) |
| % Of Americans Who Experience Trauma That Will Develop PTSD | 20% |
| % Of PTSD Cases That Are Severe | 36.6% |
| % Of PTSD Cases That Are Moderate | 33.1% |
| % Of PTSD Cases That Are Mild | 30.2% |
| % Of Women Who Will Get PTSD | 11% (1 in 9) |
| % Of Women Who Get Sexually Assaulted In The Military | 23% |
| % Of Male Veterans Who Experienced Sexual Harassment | 38% |
| PTSD Prevalence In 45- to 59-Year-Olds | 5. 3% 3% |
| PTSD Prevalence In Female Adolescents Aged 13 to 18 | 8% |
| PTSD Prevalence In Adults Aged 60 Or Older | 1% |
| PTSD Prevalence In Blacks | 8.7% |
| PTSD Prevalence In Hispanics | 7.0% |
| PTSD Prevalence In Whites | 7.4% |
| PTSD Prevalence In Asians | 4.0% |
Prevalence Of PTSD By Country
Source: Therecoveryvillage.comU.S PTSD Statistics
- Around 70% of adults in the United States have experienced at least one traumatic event in their lifetime.
- Up to 20% of these people go on to develop post-traumatic stress disorder.
- Approximately 5% of Americans – more than 13 million people – have PTSD at any given time.
- Approximately 8.7% of all adults – 1 in 13 people in the U.S. will develop PTSD at some point in their lifetime.
- Approximately 3.6% of adults in the U.S. suffer from PTSD in a given year.

- Of people in the U.S. who experience a traumatic event, 1 in 5 of them will develop the condition.
- 36.6% of PTSD cases are severe, 33.1% are moderate, and 30.2% are mild according to a study by Harvard Medical School in 2007.
Canada PTSD Statistics
- Canada has the highest rates of PTSD of 24 countries that were studied by the British Journal of Psychiatry in 2016.
- 9% of Canadians will suffer from PTSD in their lifetime.
PTSD Statistics By Gender
- Around 1 in 9 women will get PTSD at some point in their lifetime.
- Women are around twice as likely as men to develop the disorder.
- Surprisingly, 23% of women in the military report being sexually assaulted.
- 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.
PTSD Statistics By Age
- PTSD in adults was highest in 45- to 59-year-olds (5.3%) as of 2001-2003.
- PTSD in adolescents was highest in female adolescents aged 13 to 18 (8%) as of 2001-2004.
- PTSD prevalence was lowest in adults aged 60 or older (1%) as of 2001-2003.
PTSD Statistics By Race
- A study found that the lifetime prevalence of PTSD was highest among Blacks (8.7%), intermediate among Hispanics and Whites (7.0% and 7.4%) and lowest among Asians (4.0%).
PTSD Statistics By Trauma
Post-traumatic stress disorder is rooted in traumatic events, so we’ve compiled the latest data which illustrates the percentage of people who will likely develop the disorder after experiencing these traumatic events:
| Trauma | % Of People Who Will Likely Develop PTSD |
| Sexual assault | 49% |
| Severe physical assault | 32% |
| Serious accidents | 16.8% |
| Shoot and stabbing victims | 15.4% |
| The unexpected death of a loved one | 14. 3% 3% |
| Parents of children with life-threatening illnesses | 10.4% |
| Witnesses of violence | 7.3% |
| Natural disaster victims | 3.8% |
PTSD In Adults
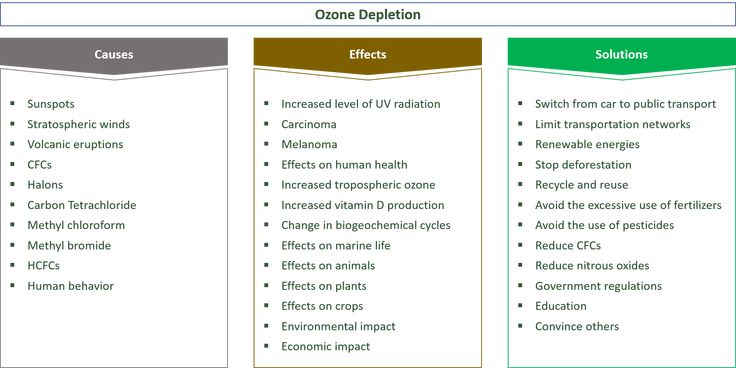
In the past year, PTSD affected around 3.6% of American adults over the age of 18 according to studies. The symptoms of PTSD in adults are grouped as serious, moderate or mild, and there are approximately 36.6% of adults who experience serious impairment, 33.1% of adults who experience a moderate impairment, and 30.2% of adults who experience mild impairment. All age groups can be affected even though most statistics focus on PTSD in adults.
Source: Cohen Veterans BioscienceIt’s possible for the disorder to occur in children, though sometimes childhood trauma doesn’t result in the disorder until after the brain has more time to develop in the individual’s early adulthood.
PTSD Among Adolescents
Around 5% of adolescents experience PTSD. Studies on PTSD in teenagers have found that just 1.5% experience severe impairment. Unsurprisingly, PTSD in adolescents is more than twice as prevalent in the later teen years, as the prevalence of PTSD for teens aged 13-4 is 3.7%. In the 17-18 age group, the PTSD prevalence increases to 7%.
Studies on PTSD in teenagers have found that just 1.5% experience severe impairment. Unsurprisingly, PTSD in adolescents is more than twice as prevalent in the later teen years, as the prevalence of PTSD for teens aged 13-4 is 3.7%. In the 17-18 age group, the PTSD prevalence increases to 7%.
PTSD & Domestic Violence
The connection between PTSD and domestic violence is clear even if PTSD might not always develop immediately following abuse. There are several factors which influence the probability of domestic violence victims developing post traumatic stress disorder, including the severity and duration of violence, and the age of the victim.
Whether or not someone feels their life is in danger can also influence the chance of PTSD developing in the victim. The intense emotional connection victims might have with the abuser is probably a big part of what makes the violence such a traumatic experience for the victim.
Veteran PTSD Statistics
Many researchers have worked to understand the prevalence of PTSD among military veterans. The result of their efforts are statistics that we’ve compiled. Estimates of prevalence in veterans vary widely because the field of psychiatry has defined and assessed PTSD in multiple ways over time.
The result of their efforts are statistics that we’ve compiled. Estimates of prevalence in veterans vary widely because the field of psychiatry has defined and assessed PTSD in multiple ways over time.
In one recent analysis of 32 scientific scientific articles, researchers found the estimated prevalence of PTSD among veterans ranges from 1.09% to 34.84%.
A 2017 study involving 5,826 U.S. veterans showed that 12.9% were diagnosed with PTSD. This is a shockingly high prevalence rate compared to the prevalence of PTSD among the general population: only 8.7% of the U.S. population will experience PTSD in their lives. And around 3.6% of adults in the U.S. suffer from PTSD in a given year.
Source: Hill & Ponton Disability AttorneysAnd in a 2014 study involving 3,157 U.S. veterans, 87% reported exposure to at least one potentially traumatic event in their lifetime. Veterans reported 3. 4 potentially traumatic events during their lifetime, on average.
4 potentially traumatic events during their lifetime, on average.
Surprisingly, nearly 1 in 4 women in the military report being sexually assaulted. And 55% of female veterans and 38% of male veterans experienced sexual harassment while in the military.
Source: Hill & Ponton Disability Attorneys- Around 30% of Vietnam veterans have had PTSD in their lifetime. (according to American Psychological Association in 1990)
- Approximately 354 million adult war survivors globally have PTSD and/or major depression. (according to European Journal of Psychotraumatology in 2019)
- PTSD prevalence of around 14% was present in veterans who served in Iraq in one study of 1,938 veterans. (according to U.S. Department of Veterans Affairs)
- A 10% prevalence of PTSD has been extrapolated for all Gulf War veterans in a 2003 report by American Journal of Epidemiology.
PTSD Symptoms
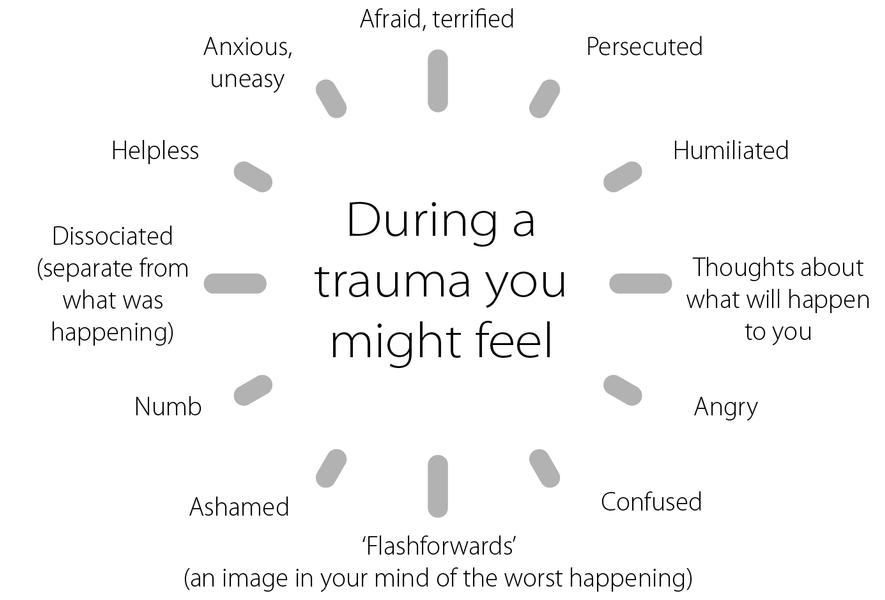
PTSD symptoms may include unwanted memories of the trauma, avoidance of situations that bring back memories of the trauma, nightmares, anxiety, depressed mood, or heightened reactions.
People may experience these symptoms:
- Intrusion of thoughts, flashbacks, memories, and dreams
- Avoidance of reminders of traumatic events
- Alterations in mood and cognition
- Alterations in reactivity and arousal
- Insomnia or nightmares
- Emotional detachment or unwanted thoughts
- Self-destructive behavior, social isolation, irritability, agitation
- Loss of interest in activities, loneliness, or guilt
PTSD & Co-Occurring Conditions
It’s possible for many mental health disorders to co-occur with PTSD in part, to the significant changes in brain functioning following trauma that leads to the disorder. The most common conditions someone with PTSD may experience include:
- Depression
- Suicidal thoughts
- Trauma
- Anxiety
- Substance use disorders
We’ll go into more detail on each condition in this section.
PTSD & Depression
Approximately 1 in 10 people have some form of depressive disorder every year, making it a common mental health condition. It’s more common among people who’ve experienced traumatic experiences.
As mentioned earlier, PTSD and depression frequently co-occur. Specifically, people with PTSD are 3-5 times more likely to have depression.
PTSD & Suicide
In general, people diagnosed with PTSD who struggle to express their emotions have a higher risk of suicide. Other common co-occurring conditions such as depression or anxiety can make a negative impact on the chances of suicide for someone with the disorder.
PTSD & Trauma
Disruptions and changes in brain chemistry caused by an individuals’ trauma is the main reason why PTSD and trauma are interconnected. The condition can occur in response to traumas besides military combat (example: sexual abuse).
However, there are other traumatic events which can happen in a person’s life that might lead to the disorder:
- 49% of rape victims will develop PTSD.
- Almost 32% of physical assault victims will develop PTSD.
- 16.8% of people involved in serious vehicle accidents develop PTSD.
- 15.4% of shooting and stabbing victims develop PTSD.
- 14.3% of people who unexpectedly and suddenly experience the death of a close loved one develop PTSD.
- 7.3% of people who’ve witnessed the murder or serious injury of another person will develop PTSD.
- 3.8% of people who experience natural disasters develop PTSD.
PTSD & Anxiety
Currently, PTSD is considered a separate type of disorder, but in the past it was categorized as an anxiety disorder because PTSD and anxiety disorders share some symptoms, many of which can impair sleep and other biological functions. For example, someone with anxiety related to PTSD can frequently feel on edge and be easily startled.
Similarly, anxiety caused by the disorder can make it challenging for an individual to concentrate, and it can also increase their agitation.
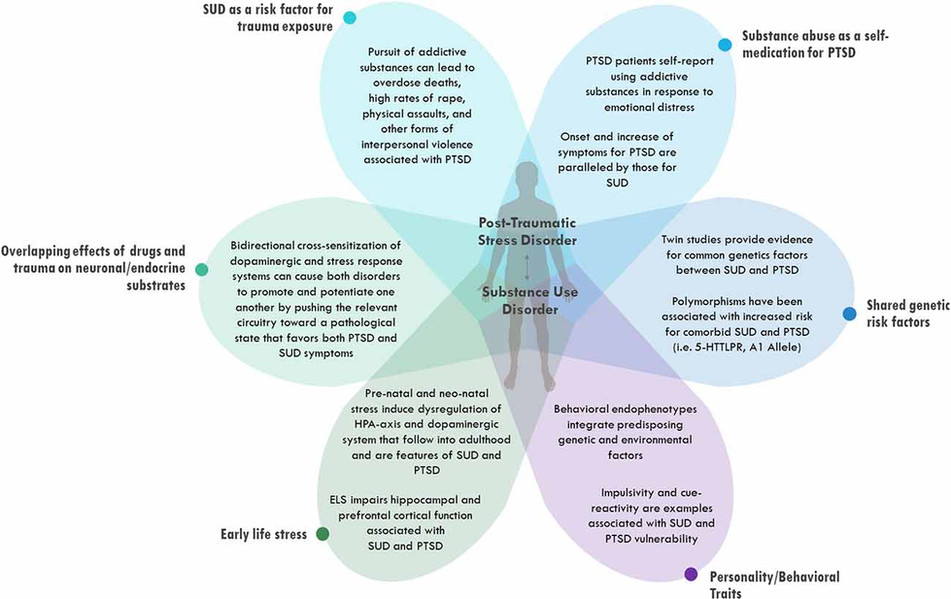
PTSD & Substance Abuse
One study estimates that 46.4% of people diagnosed with the disorder also meet the criteria for a substance use disorder. Another study found that women with the disorder were 2.48 times more likely to suffer from alcohol abuse, while men with the disorder were 2.06 times more likely.
PTSD Treatment Statistics
Medication, psychotherapy, or a combination of both can treat PTSD. Even though there’s more than one type of psychotherapy used to treat the disorder, trauma-focused psychotherapies with a mental healthcare professional are the most recommended.
That’s primarily because this type of treatment assists people to process their experiences by helping them focus on the memory of the traumatic event or the meaning behind it.
In fact, studies have demonstrated that up to 46% of people diagnosed with the disorder show improvement within the first six weeks of psychotherapy.
Another treatment option that can alleviate the symptoms of PTSD, including anxiety, are antidepressants. Interestingly, studies show up to 62% of people who receive medication for PTSD show improvement. (American Family Physician, 2003)
Interestingly, studies show up to 62% of people who receive medication for PTSD show improvement. (American Family Physician, 2003)
First Responder PTSD Statistics
If you’re wondering how common is PTSD among first responders, this section will show you the up-to-date stats.
Surprisingly, more than 80% of first responders experience traumatic events on the job. The challenging and dangerous situations they face cause them to be at a high risk of developing PTSD as a work-related injury or condition.
In fact, according to the Substance Abuse and Mental Health Services Administration, an estimated 30% of first responders develop behavioral health conditions including, but not limited to, depression and PTSD, as compared with 20% in the general population.
9/11 PTSD Statistics
More than 21% of residents enrolled in the WTC Health Registry reported new PTSD symptoms 5 to 6 years after the tragic day. PTSD among residents increased from more than 13% 2-3 years after the attacks to more than 16% 5-6 years later. The main risk factors associated with 9/11 were:
The main risk factors associated with 9/11 were:
- Intense dust cloud exposure
- Returning to a home with a heavy layer of dust
- Witnessing horror
- Job loss
- Lack of social support
Firefighter PTSD Statistics
Studies have shown that anywhere between around 7% and 37% of firefighters meet the criteria for a current PTSD diagnosis.
World War 2 PTSD Prevalence
Among individuals who had previously sought psychiatric treatment, 37% of the World War 2 veterans and 80% of the Korean War veterans had current PTSD. It was found that 54% of a group of psychiatric patients who had been in combat during World War 2 met criteria for PTSD. At the time, the prevalence for PTSD was 27%.
Frequently Asked Questions
What is PTSD?
PTSD stands for post-traumatic stress disorder, and the disorder develops in some who have experienced a dangerous or shocking event and have a challenging time recovering from the trauma the incident caused.
Life-threatening events are common risk factors for PTSD. For example, military personnel who have experienced violence, people who have lived through natural disasters, victims of sexual abuse, and those who were involved in a car accident have an unfortunate high chance for developing the disorder.
What does PTSD do to a person?
People diagnosed with PTSD have disturbing, intense thoughts and feelings related to their experience that can last long after the traumatic event occurred. They may even relive the event through nightmares or flashbacks, they may feel sadness or even depression, anger, fear, and they may feel detached from others.
What are 3 things that can lead to PTSD?
Here are the most common events that can lead to PTSD:
- Physical or sexual assault
- Serious accidents
- Abuse, including childhood or domestic abuse
How long does PTSD last for?
Some people with PTSD recover within just 6 months, while others have symptoms that can last much longer.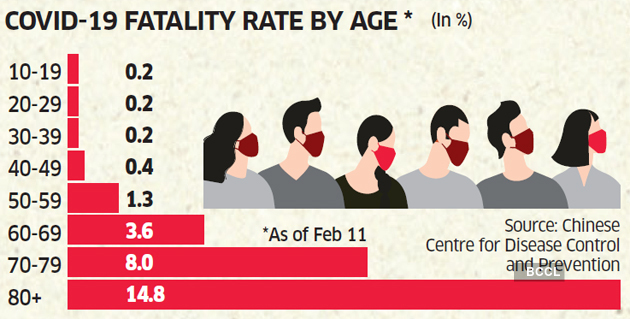 In some people, the condition becomes chronic and can result in depression and anxiety. A doctor, such as a psychologist or psychiatrist, who has experience helping people with mental illnesses can diagnose PTSD.
In some people, the condition becomes chronic and can result in depression and anxiety. A doctor, such as a psychologist or psychiatrist, who has experience helping people with mental illnesses can diagnose PTSD.
Is PTSD a cause of death?
Post-traumatic stress disorder more than doubles a veteran’s risk of death from any cause. It’s also an independent risk factor for cardiovascular disease, according to research presented in 2010 at the American Heart Association’s Scientific Sessions.
Can PTSD change your personality?
Yes, a study published by the National Library of Medicine concluded that PTSD is a risk of development enduring personality changes with serious individual and social consequences.
Can PTSD be cured?
As with the majority of mental illnesses, no cure exists for PTSD. However, it’s possible to effectively manage the symptoms to help the affected individual restore themself to normal functioning. A combination of therapy and medication is the best hope for treating the disorder.
Does PTSD affect memory?
If you have PTSD, you might notice that it’s challenging for you to concentrate or that you have memory issues such as memory loss. In fact, memory and concentration problems are common symptoms of PTSD.
Can PTSD last a lifetime?
As with the majority of mental illnesses, PTSD is very personal and no two cases are the same. In fact, according to Dr. Kriegeskotten, “When PTSD is not treated, it can last a very long time, perhaps a lifetime.”
PTSD Research & Sources
- Post-traumatic stress disorder
- National Center for PTSD
- Post-traumatic stress disorder
- Diagnosis and management of post-traumatic stress disorder
- Epidemiology of PTSD
- PTSD and Veterans: Exploring The Statistics
- Post Traumatic Stress
Post-traumatic stress disorder in children. What is Post Traumatic Stress Disorder in Children?
IMPORTANT
The information in this section should not be used for self-diagnosis or self-treatment.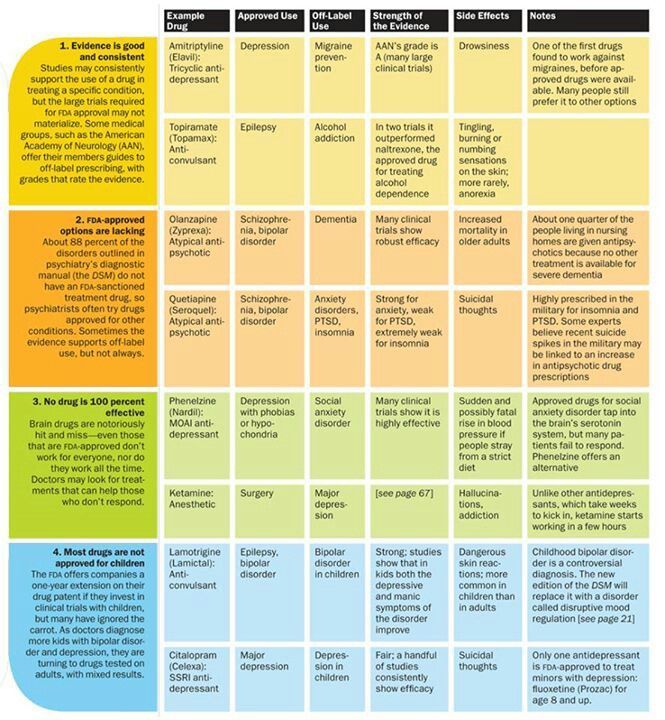 In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor.
In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor.
Post-traumatic stress disorder in children is a mental disorder that develops after an external psychologically traumatic event. It is manifested by repeated experience of the situation in nightmares and thoughts, the desire to get rid of memories, actual nervous tension, irritability, anxiety. For diagnosis, psychometric tests, projective techniques, observation, and conversation are used. Specific treatment includes family therapy, cognitive behavioral therapy, neuro-linguistic programming, auto-training. In complex forms, drug therapy is additionally used. nine0006
- Causes of PTSD in children
- Pathogenesis
- Classification
- Symptoms of PTSD in children
- Complications
- Diagnostics
- Treatment of PTSD in children
- Prognosis and prevention
- Prices for treatment
General
The term post-traumatic stress disorder (PTSD) has been around since the 1980s. Its synonym is post-traumatic syndrome. Initially, this nosology included emotional disturbances caused by extraordinary natural socio-political events: military operations, terrorist acts, natural disasters. Later, the boundaries of the concept were expanded, similar neurotic disorders after domestic, social violence began to be attributed to this pathology. The prevalence of PTSD in the general population is 7.8%. In children who have experienced traumatic events, the frequency of the syndrome ranges from 5 to 9eight%. The highest rates are noted after wars, persecution, repression; the lowest - after serious illnesses.
Its synonym is post-traumatic syndrome. Initially, this nosology included emotional disturbances caused by extraordinary natural socio-political events: military operations, terrorist acts, natural disasters. Later, the boundaries of the concept were expanded, similar neurotic disorders after domestic, social violence began to be attributed to this pathology. The prevalence of PTSD in the general population is 7.8%. In children who have experienced traumatic events, the frequency of the syndrome ranges from 5 to 9eight%. The highest rates are noted after wars, persecution, repression; the lowest - after serious illnesses.
Post-traumatic stress disorder in children
Causes of PTSD in children
Children are a group with a high age predisposition to post-traumatic syndrome. The risk of developing PTSD increases due to sensitivity, susceptibility, impressionability, insufficient formation of the adaptive mechanisms of the nervous system.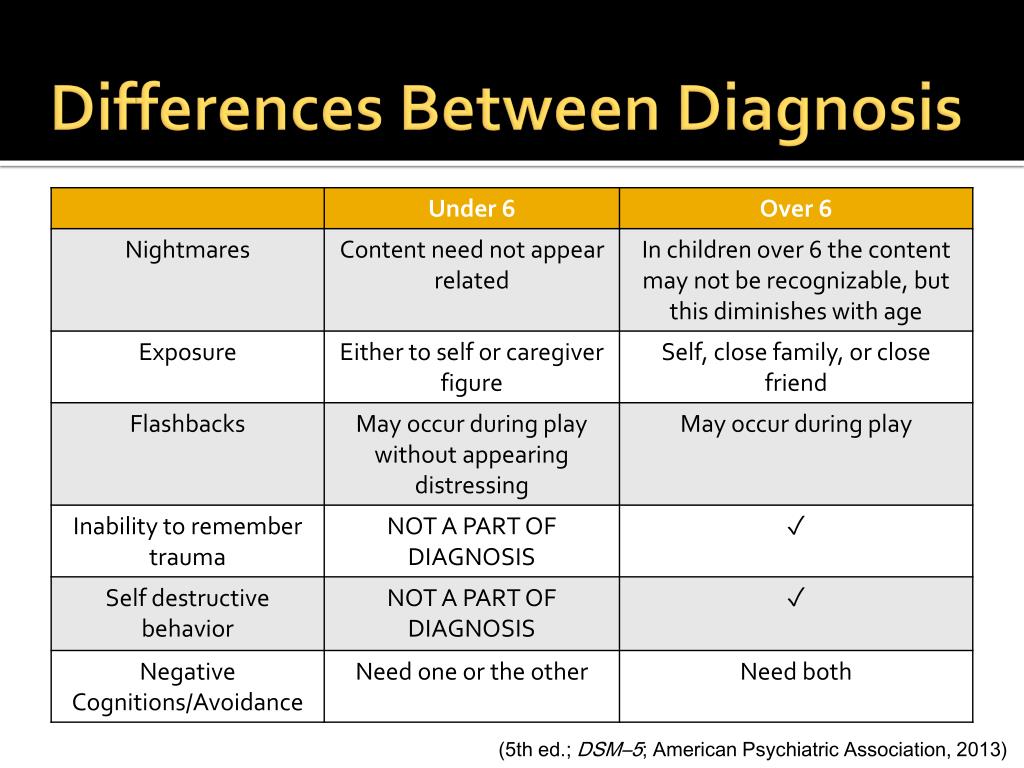 The causes of the disorder are: nine0006
The causes of the disorder are: nine0006
- Psychological trauma. The traumatic event becomes the basis of the syndrome. An extreme situation can be a serious illness, disability, prolonged separation from the mother, placement in a boarding school, illness or death of a loved one, physical, sexual and psychological abuse, man-made and natural disasters, wars, persecution.
- Unfavorable social conditions. The reason for the formation of post-traumatic syndrome is an unfavorable environment after a psychotrauma. Children who experience loneliness, who are not covered by social interactions, who do not have loved ones, who live in difficult material and living conditions, are more prone to frustration. nine0012
- Individual features. The likelihood of developing post-traumatic syndrome is higher with aggravated heredity - the presence of first-line relatives with mental disorders, suicides, alcoholism, drug addiction. PTSD is more often diagnosed in somatically weakened children with neurological, endocrine, and mental illnesses.
Pathogenesis
Post-traumatic stress disorder in children is a delayed reaction to trauma. It develops as a result of depletion of the adaptive reserves of the body, failure of emotional and volitional mechanisms. In an extreme situation, the body systems function in an enhanced mode - the resistance phase is activated. Danger, unpredictability of events do not allow to show weakness, emotionality. Own attitude, fear, humiliation, pain are forced out of consciousness, as they do not contribute to survival. As a result, after a certain period of time, the protective mechanisms are depleted, experiences are actualized, transforming into obsessive memories, nightmares, tension, anxiety, and depression. nine0006
Classification
A characteristic feature of post-traumatic stress disorder is staging. The syndrome develops some time after a psychological trauma, has a number of stages. The classification includes the following types of PTSD:
- Acute disorder.
 Characteristic manifestation of symptoms. Duration - up to 3 months.
Characteristic manifestation of symptoms. Duration - up to 3 months. - Chronic disorder. Symptoms are less noticeable, signs of central nervous system depletion are revealed, rudeness, selfishness, indifference to other people and events are noted. nine0012
- Deformations of the emotional-volitional sphere. Occur with a long chronic course of PSTR. Attacks of anxiety, fear, panic develop. Negative character traits are sharpened.
- Delayed syndrome. Symptoms appear six months or more after exposure to a traumatic situation.
Symptoms of PTSD in children
The behavior of children suffering from post-traumatic syndrome is aimed at avoiding situations that actualize memories of trauma. Random interaction with a trigger (a fragment of a traumatic situation) is accompanied by an emotional attack, manifested by anxiety, screams, panic, crying, inadequate impulsive actions. An example of a trigger is the screeching of brakes, the sound of a gunshot, the smell of certain drugs.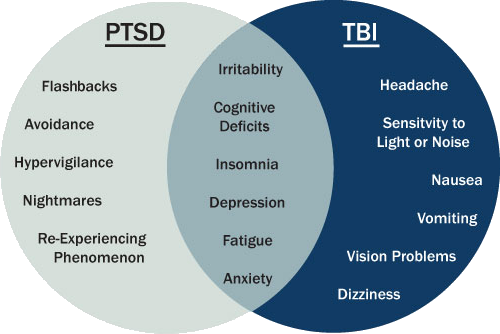 Memories often occur at night, are rare during the day, and are easier to bear. Often there are sleep disturbances, daytime sleepiness. Often there is a desire of the child to relive the traumatic situation again: the plot is reproduced in drawings, games, composed stories. nine0006
Memories often occur at night, are rare during the day, and are easier to bear. Often there are sleep disturbances, daytime sleepiness. Often there is a desire of the child to relive the traumatic situation again: the plot is reproduced in drawings, games, composed stories. nine0006
Children who have been physically abused become aggressive - they provoke conflicts, they are the first to start a fight. In preschoolers, against the background of PTSD, a regression of development is found: speech and play are simplified, previously learned self-care and hygiene skills disappear. Violations of emotional, volitional functions are manifested by isolation, capriciousness, irritability. There are problems of socialization, social adaptation. Severe forms are accompanied by illusions, hallucinations, reflecting fragments of a traumatic situation. nine0006
Constant emotional overstrain, insomnia lead to the development of cerebrasthenic syndrome - a complex of symptoms of exhaustion of nervous activity. The child quickly gets tired, does not cope with the study load, tries to avoid physical activity, and does not concentrate well. Gradually appear functional disorders of the cardiovascular, endocrine, digestive systems. Frequent symptoms are nocturnal enuresis, lethargy, weakness, drowsiness, epigastric, headache, heart pain. nine0006
The child quickly gets tired, does not cope with the study load, tries to avoid physical activity, and does not concentrate well. Gradually appear functional disorders of the cardiovascular, endocrine, digestive systems. Frequent symptoms are nocturnal enuresis, lethargy, weakness, drowsiness, epigastric, headache, heart pain. nine0006
Complications
The neurophysiological systems of children are developing rapidly. Psychological traumas are reflected in the process of physical and mental development. In the absence of timely diagnosis and adequate treatment, post-traumatic stress disorder in children becomes chronic, complicated by the development of secondary depression, the appearance of obsessive-compulsive disorder, panic disorder, and phobias. Agoraphobia, claustrophobia, fear of the dark predominate among the formalized fears. As they grow older, there is a risk of pathocharacterological, psychopathic development of the personality, isolation, anxiety, anger, and aggressiveness are observed.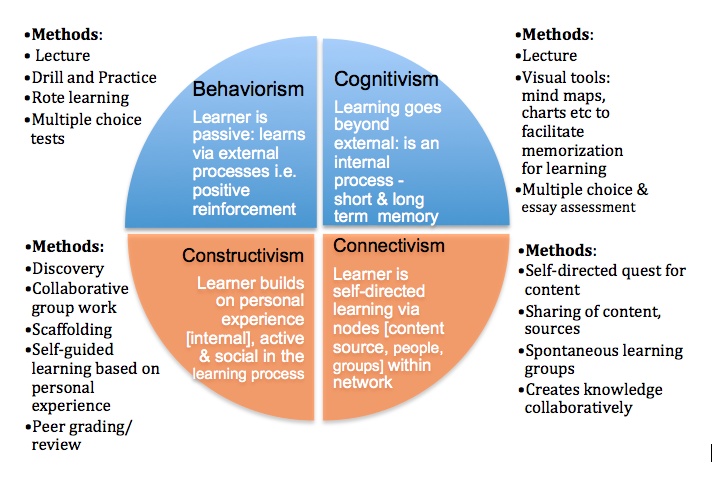 Behavioral disorders are associated with an increased risk of alcohol abuse, drug addiction, social maladaptation, and suicide. nine0006
Behavioral disorders are associated with an increased risk of alcohol abuse, drug addiction, social maladaptation, and suicide. nine0006
Diagnostics
Difficulties in diagnosing post-traumatic stress disorder are associated with the limited verbal capabilities of children, the tendency of parents to underestimate the child's symptoms. To identify the syndrome, clinical examination skills and special psychodiagnostic tools are used:
- Clinical conversation. Conducted by a child psychiatrist. The specialist finds out the nature of the traumatic event, the period before the onset of symptoms, the severity of the clinical picture. The emphasis is on three key points: the presence of a psychotrauma, an emotional outburst on the impact of triggers, frequent memories of a traumatic event, confirmed by reproduction in games, dreams, drawings, stories. nine0012
- Psychodiagnostics. The clinical psychologist offers parents to fill out questionnaires regarding the child's condition: the list of pediatric symptoms (PSC-17), the anxiety questionnaire of Lavrentieva, Titarenko.
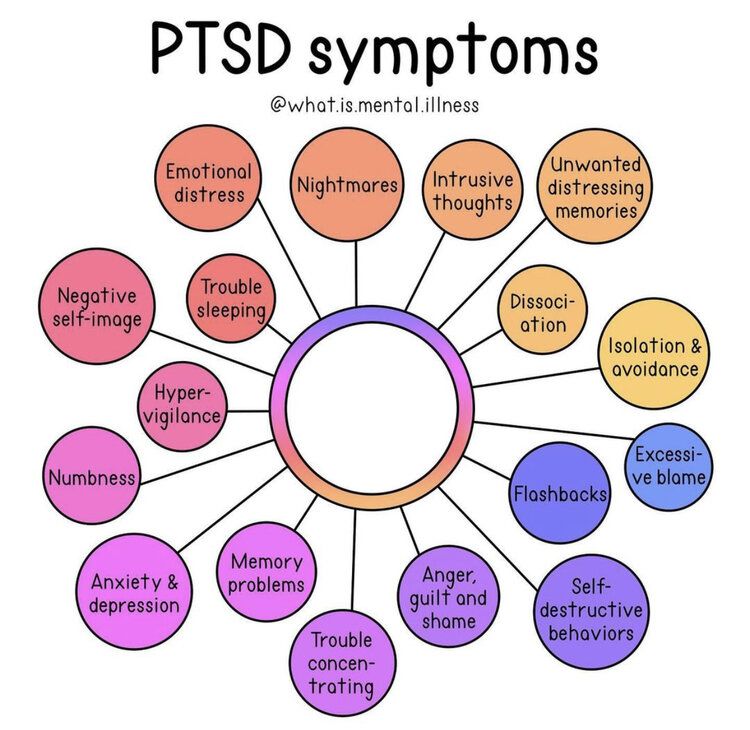 The emotional sphere of children under 8-10 years old is studied by projective methods: drawing tests "Non-existent animal", "Man in the rain", methods of interpreting situations (Rosenzweig test, thematic apperception test (TAT), children's apperception test (CAT), hand test). nine0029
The emotional sphere of children under 8-10 years old is studied by projective methods: drawing tests "Non-existent animal", "Man in the rain", methods of interpreting situations (Rosenzweig test, thematic apperception test (TAT), children's apperception test (CAT), hand test). nine0029 - Cognitive behavioral methods. Meetings with a specialist are aimed at understanding, re-experiencing psychotrauma. After that, key desensitization techniques are used. Several stimuli of the same type, but of different intensity, are selected. An emotional response is provoked (fear, crying) with a gradual increase, skills of coping with an attack are developed. Over time, the link between the trigger and the emotion breaks down.
- Psychocorrection of destructive feelings. By projective methods, game situations, the feeling of guilt is eliminated, bouts of aggression and self-aggression are corrected. nine0012
- Family psychotherapy. Working together with parents, close relatives is aimed at relieving anxiety and emotional stress. Situations are created thanks to which the child can express himself, be active, not be afraid.
- Medical treatment. It is prescribed for severe PTSD to relieve phobias, panic attacks, illusions.
 Sedatives, selective serotonin reuptake inhibitors (SSRIs) are used. The drugs relieve tension, obsessions, improve mood, eliminate anxiety, stabilize the central nervous system, and reduce aggressiveness. Severe anxiety is corrected with tranquilizers, asthenic manifestations - with nootropics, psychotic symptoms - with antipsychotics. nine0012
Sedatives, selective serotonin reuptake inhibitors (SSRIs) are used. The drugs relieve tension, obsessions, improve mood, eliminate anxiety, stabilize the central nervous system, and reduce aggressiveness. Severe anxiety is corrected with tranquilizers, asthenic manifestations - with nootropics, psychotic symptoms - with antipsychotics. nine0012 - In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor. nine0006
Post-traumatic stress disorder in young children
Alexandra De Young, PhD, Justin Kenardi, PhD
National Research Center for Disorders and Rehabilitation, School of Medicine, University of Queensland, Australia
(English).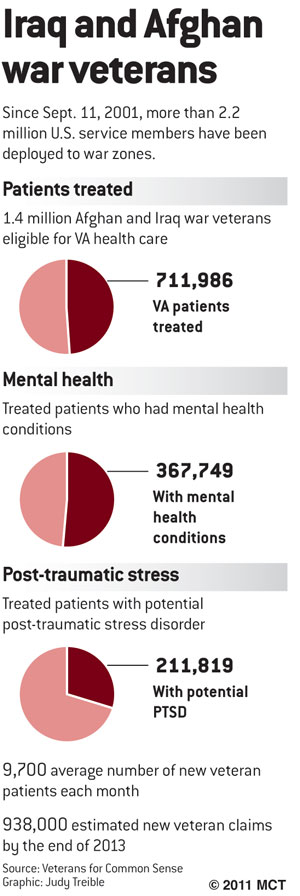 Translation: June 2015 nine0006 PDF Document
Translation: June 2015 nine0006 PDF Document Introduction
Post-traumatic stress disorder (PTSD) is one of the most severe and debilitating disorders associated with trauma. According to research, young children, as well as older children and adolescents, commonly exhibit three of the traditional symptoms of PTSD: re-experiencing the event (through nightmares or acting out traumatic events), seeking to avoid being reminded of the event, and psychological overexcitation (for example, , irritability, sleep disturbance, unmotivated shivering). nine0137 1 However, research suggests that the features of PTSD listed in The Diagnostic and Statistical Manual of Mental Disorders 2 do not adequately reflect the specificity of onset of symptoms in infants and preschool children. The Guidelines also underestimate the number of children experiencing post-traumatic stress and subsequent deterioration in health.
 nine0137 3 Accordingly, new research is encouraging the inclusion of a subtype of PTSD occurring in preschool children in the 5th edition of the Diagnostic and Statistical Manual. 4.5
nine0137 3 Accordingly, new research is encouraging the inclusion of a subtype of PTSD occurring in preschool children in the 5th edition of the Diagnostic and Statistical Manual. 4.5 Frequency, course and consequences of reactions to trauma months after the traffic accident (RTA) 6 or burn injuries 7 ; in 14.3–25% of cases, within two months after receiving various types of injuries (for example, burns, bullet wounds, road accidents, injuries during sports or during the game), 8.9 in 10% of cases, within six months after an accident or burn injuries 6.8 and in 13.2% of cases - within 15 months on average after burn injuries.10 Signs of age-specific PTSD appear in 26-60% 1,3,11 cases as a result of physical or sexual violence. Our study has shown that young children develop depression, separation anxiety disorder, oppositional defiant disorder (ODD), and specific phobias due to burn injuries, 8 , and that these disorders are highly co-morbid symptoms of PTSD.
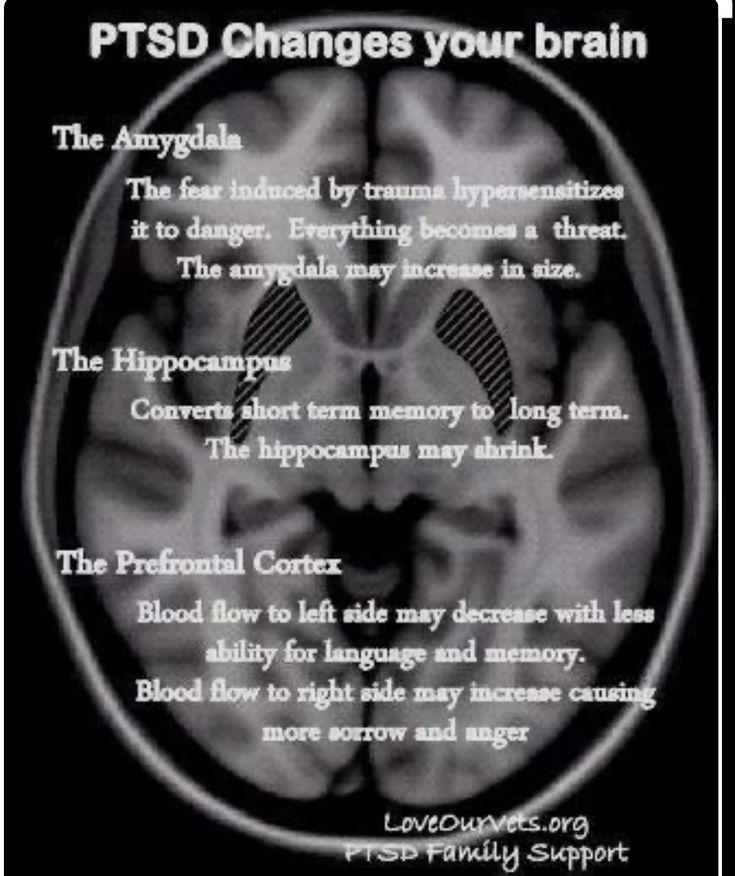
Studies in children of all ages have shown that, if left untreated, PTSD can develop into a chronic, debilitating form. nine0137 8,12,13 The results of this study are troubling given the fact that neurophysiological systems in young children, including stress modulation and emotion regulation, are still in rapid development. 14 In addition, childhood trauma is associated with permanent structural 15 and functional 16 brain damage, as well as with the onset of psychiatric disorders, 17 health risk behaviors and related physical health conditions in adults. 18 Thus, trauma in early childhood can have much more severe consequences on the developmental trajectory than trauma sustained later in development.
The role of parents
When working with children, it is very important to realize that the trauma itself and the child's reaction to it is a serious test for parents, which can also become a source of chronic stress.
 Research has shown that approximately 25% of parents experience clinically elevated levels of acute stress, PTSD, anxiety, depression, and stress within the first six months of a child's trauma. nine0137 19-21 Although most parents remain relatively resilient and their stress levels eventually return to clinical normal, parental distress during the acute stress stage contributes to the development and persistence of traumatic symptoms in affected children. 19,20,22
Research has shown that approximately 25% of parents experience clinically elevated levels of acute stress, PTSD, anxiety, depression, and stress within the first six months of a child's trauma. nine0137 19-21 Although most parents remain relatively resilient and their stress levels eventually return to clinical normal, parental distress during the acute stress stage contributes to the development and persistence of traumatic symptoms in affected children. 19,20,22 It is generally accepted that the quality of attachment of children and parents to each other, the mental health of parents and their parenting actions are key factors influencing a child's recovery from trauma. nine0137 14,23,24 For young children, relationships with parents are especially important because children do not have sufficient adaptive capacity to regulate strong emotions on their own. Thus, they depend on a sensitive and emotionally open educator who can help them regulate their emotional response in times of distress.
 14.23 In addition, young children especially rely on their parents' emotions to understand how to interpret or respond to an event. In the future, children can imitate their parents' reaction to fear and their inadequate adaptive reactions. nine0137 25 Parents can also directly influence the child's contact with the trauma reminders (for example, avoiding discussion of what happened) and thus hinder the child's adaptation to the event. 25
14.23 In addition, young children especially rely on their parents' emotions to understand how to interpret or respond to an event. In the future, children can imitate their parents' reaction to fear and their inadequate adaptive reactions. nine0137 25 Parents can also directly influence the child's contact with the trauma reminders (for example, avoiding discussion of what happened) and thus hinder the child's adaptation to the event. 25 The influence of adverse psychological reactions on the relationship between children and parents, the development of traumatic symptoms in the child, combined with the mental suffering of parents, are important arguments for paying more attention to the needs of parents in order to reduce their level of experience and stimulate their ability to support children in difficult times. Adequate measures aimed at alleviating the mental illness of the child and parents, as well as improving relations between them, will have a beneficial effect on the process of inhibiting the development of post-traumatic reactions in parents and children.
 However, there is only preliminary evidence to support these types of interventions during an exacerbation, and more research is needed on this issue. nine0006
However, there is only preliminary evidence to support these types of interventions during an exacerbation, and more research is needed on this issue. nine0006 Early prevention and correction measures
Unfortunately, most children and their parents who experience psychological difficulties after trauma are not diagnosed with characteristic symptoms, as a result of which both children and parents do not receive adequate support. Taking into account the prevalence of injuries, as well as the fact that early childhood is a sensitive period of brain development, it is necessary to introduce effective measures that can reduce the risk of developing chronic post-traumatic stress reactions in children and parents. It is advisable to take such measures in an environment with an increased risk of stress reactions, for example, in a medical institution. This solution would reduce the risk of traumatic stress reactions or even prevent them by conducting an examination and implementing a program of preventive measures.
 nine0137 26 Early diagnosis of severe symptoms and appropriate action in families at risk will help prevent problems from occurring and entrenching, or at least minimize the impact of these problems on the child, family and society. However, the primary task is to learn to distinguish between categories of patients experiencing a short-term mental disorder and those at risk of developing chronic PTSD, without creating additional overload for filled medical institutions. Psychometrically verified examination methods for very young children do not exist, which is a significant shortcoming in this area. nine0006
nine0137 26 Early diagnosis of severe symptoms and appropriate action in families at risk will help prevent problems from occurring and entrenching, or at least minimize the impact of these problems on the child, family and society. However, the primary task is to learn to distinguish between categories of patients experiencing a short-term mental disorder and those at risk of developing chronic PTSD, without creating additional overload for filled medical institutions. Psychometrically verified examination methods for very young children do not exist, which is a significant shortcoming in this area. nine0006 To date, most research has focused on the treatment of chronic PTSD rather than early prevention of its symptoms. Both in children's and adult literature, there is no data on which categories of patients need preventive measures at an early stage, what duration and content these measures should have. 27 To date, systematic reviews suggest that continuous cognitive behavioral trauma therapy (CBT) is most effective when administered within the first three months after the event.
 nine0137 27
nine0137 27 Studies involving children suggest that preventive action based on incident information up to two weeks after an injury can reduce anxiety symptoms in children at 1 28 and 6 months after the experience developments. 29 In addition, Landolt et al received a positive response to a single session of preventive therapy aimed at managing symptoms of depression and behavioral problems in a group of preteens (7-11 years old) affected by road traffic accidents. nine0137 30 Berkowitz and colleagues 31 created the only individualized prevention program (4 sessions for a child with a parent/guardian, including diagnostics, psychological self-help training and coping skills) for children 7-17 years old. The program has shown its effectiveness in reducing the manifestations of PTSD and various post-traumatic symptoms.
However, there are no published studies on the effectiveness of preventive post-traumatic psychological interventions for young children (under six years of age).
 However, Scheering's research has shown that 12 sessions of cognitive-behavioral therapy, built in accordance with a special plan for PTSD, conducted with children aged 3-6 years who experienced a variety of traumatic events, showed their appropriateness and effectiveness in reducing existing post-traumatic stress symptoms. nine0137 32
However, Scheering's research has shown that 12 sessions of cognitive-behavioral therapy, built in accordance with a special plan for PTSD, conducted with children aged 3-6 years who experienced a variety of traumatic events, showed their appropriateness and effectiveness in reducing existing post-traumatic stress symptoms. nine0137 32 Few studies look at the preventive therapy component for adults to prevent post-trauma disorders in children. Kenardy et al found that psychological self-help training provided to parents within 72 hours of an accident was effective in reducing parental post-traumatic symptoms up to 6 months after the accident. 28 Melnyk et al. 33 examined the effectiveness of a prevention program in parents of children aged 2-7 years under close supervision of pediatricians. The researchers found that parents in the prevention group had markedly reduced levels of stress, depression, and PTSD symptoms, and their children experienced fewer internalizing and externalizing behavioral problems after discharge.
 nine0006
nine0006 Evidence-based recommendations for the prevention of PTSD in young children require research. However, Landolt et al., based on the results of a recent meta-analysis, argue that early preventive measures help identify children at risk. These activities include several sessions of training in psychological self-help, individual adaptation skills, involvement of parents in the process and familiarization with various forms of traumatic phenomena. nine0137 34
Advice for parents, services and policy
The phenomenon of post-traumatic stress disorder in young children has received little attention so far. Health care providers should monitor children more closely for signs of post-traumatic stress disorder. This may require training and retraining of staff. Mass standardized screening is ideal, but diagnosing groups of children at risk may be more cost-effective. In addition, any screening program must be integrated with a clinical setting that provides opportunities for appropriate care.
 Parental distress is a significant factor influencing post-traumatic reactions in children. However, in medical institutions this criterion is given insufficient attention. The reason for this may be the fact that the distress of the parents against the background of the child's injury may not reach the level of clinical diagnosis, or the fact that it is customary to pay more attention to the needs of the child than the family as a whole. nine0137 22 Caregivers should pay more attention to the fact that the effects of trauma can have a greater impact on the family system as a whole.
Parental distress is a significant factor influencing post-traumatic reactions in children. However, in medical institutions this criterion is given insufficient attention. The reason for this may be the fact that the distress of the parents against the background of the child's injury may not reach the level of clinical diagnosis, or the fact that it is customary to pay more attention to the needs of the child than the family as a whole. nine0137 22 Caregivers should pay more attention to the fact that the effects of trauma can have a greater impact on the family system as a whole. Literature
- Scheeringa, M., et al., New findings on alternative criteria for PTSD in preschool children. Journal of the American Academy of Child and Adolescent Psychiatry , 2003. 42(5): p. 561-570.
- American Psychiatric Association, Diagnostic and statistical manual of mental disorders, (4th edition, Text Revision). nine0148 2000, Washington, DC: Author.

- Scheeringa, M.S., et al., Two approaches to the diagnosis of posttraumatic stress disorder in infancy and early childhood. Journal of the American Academy of Child and Adolescent Psychiatry , 1995. 34(2): p. 191-200.
- Scheeringa, M.S., C.H. Zeanah, and J.A. Cohen, PTSD in Children and Adolescents: Toward an Empirically Based Algorithm. Depression and Anxiety , 2011. 28(9): p. 770-782.
- De Young, A.C., J.A. Kenardy, and V.E. Cobham, Diagnosis of Posttraumatic Stress Disorder in Preschool Children. nine0147 Journal of Clinical Child and Adolescent Psychology , 2011. 40(3): p. 375-384.
- Meiser-Stedman, R., et al., The posttraumatic stress disorder diagnosis in preschool- and elementary school-age children exposed to motor vehicle accidents. American Journal of Psychiatry , 2008. 165(10): p. 1326-1337.
- Stoddard, F.J., et al., Acute stress symptoms in young children with burns. Journal of the American Academy of Child and Adolescent Psychiatry , 2006.
 45(1): p. 87-93.
45(1): p. 87-93. - De Young, A.C., et al., Prevalence, comorbidity and course of trauma reactions in young burn-injured children. Journal of Child Psychology and Psychiatry , 2012. 53(1): p. 56-63.
- Scheeringa, M.S., et al., Factors affecting the diagnosis and prediction of PTSD symptomatology in children and adolescents. American Journal of Psychiatry , 2006. 163(4): p. 644-651.
- Graf, A., C. Schiestl, and M.A. Landolt, Posttraumatic Stress and Behavior Problems in Infants and Toddlers With Burns. nine0147 Journal of Pediatric Psychology , 2011. 36(8): p. 923-931.
- Levendosky, A.A., et al., Trauma symptoms in preschool-age children exposed to domestic violence. Journal of Interpersonal Violence , 2002. 17(2): p. 150-164.
- Scheeringa, M.S., et al., Predictive validity in a prospective follow-up of PTSD in preschool children. J ournal of the American Academy of Child and Adolescent Psychiatry , 2005.
 44(9): p. 899-906.
44(9): p. 899-906. - Le Brocque, R.M., J. Hendrikz, and J.A. Kenardy, The Course of Posttraumatic Stress in Children: Examination of Recovery Trajectories Following Traumatic Injury. nine0147 Journal of Pediatric Psychology , 2010. 35(6): p. 637-645.
- Carpenter, G.L. and A.M. Stacks, Developmental effects of exposure to Intimate Partner Violence in early childhood: A review of the literature. Children and Youth Services Review , 2009. 31(8): p. 831-839.
- Carrion, V.G., C.F. Weems, and A.L. Reiss, Stress predicts brain changes in children: A pilot longitudinal study on youth stress, posttraumatic stress disorder, and the hippocampus. nine0147 Pediatrics , 2007. 119(3): p. 509-516.
- Perry, B.D., et al., Childhood trauma, the neurobiology of adaptation, and ''use-dependent'' development of the brain: How ''states'' become ''traits''. Infant Mental Health Journal , 1995. 16(4): p. 271-291.
- Green, J.G., et al.
 , Childhood Adversities and Adult Psychiatric Disorders in the National Comorbidity Survey Replication I Associations With First Onset of DSM-IV Disorders. Archives of General Psychiatry , 2010. 67(2): p. 113-123.
, Childhood Adversities and Adult Psychiatric Disorders in the National Comorbidity Survey Replication I Associations With First Onset of DSM-IV Disorders. Archives of General Psychiatry , 2010. 67(2): p. 113-123. - Felitti, V.J., et al., Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults - The adverse childhood experiences (ACE) study. American Journal of Preventive Medicine , 1998. 14(4): p. 245-258.
- De Young, A.C., Psychological impact of burn injury on young children and their parents: Implications for diagnosis, assessment and treatment (Unpublished Doctoral dissertation), 2011, School of Psychology, University of Queensland: Brisbane. nine0012
- Landolt, M.A., et al., The mutual prospective influence of child and parental post-traumatic stress symptoms in pediatric patients. Journal of Child Psychology and Psychiatry , 2012. 53(7): p. 767-774.
- Hall, E., et al.
 , Posttraumatic stress symptoms in parents of children with acute burns. Journal of Pediatric Psychology , 2006. 31(4): p. 403-412.
, Posttraumatic stress symptoms in parents of children with acute burns. Journal of Pediatric Psychology , 2006. 31(4): p. 403-412. - Le Brocque, R.M., J. Hendrikz, and J.A. Kenardy, Parental response to child injury: Examination of parental posttraumatic stress symptom trajectories following child accidental injury. nine0147 Journal of Pediatric Psychology , 2010. 35(6): p. 646-655.
- Lieberman, A.F., Traumatic stress and quality of attachment: Reality and internalization in disorders of infant mental health. Infant Mental Health Journal , 2004. 25(4): p. 336-351.
- Scheeringa, M.S. and C.H. Zeanah, A relational perspective on PTSD in early childhood. Journal of Traumatic Stress , 2001. 14(4): p. 799-815.
- Nugent, N.R., et al., Parental posttraumatic stress symptoms as a moderator of child's acute biological response and subsequent posttraumatic stress symptoms in pediatric injury patients. nine0147 Journal of Pediatric Psychology , 2007.
 32(3): p. 309-318.
32(3): p. 309-318. - Kazak, A.E., et al., An integrative model of pediatric medical traumatic stress. Journal of Pediatric Psychology , 2006. 31(4): p. 343-355.
- Roberts, N.P., et al., Systematic Review and Meta-Analysis of Multiple-Session Early Interventions Following Traumatic Events. American Journal of Psychiatry , 2009. 166(3): p. 293-301.
- Kenardy, J., et al., Information-provision intervention for children and their parents following pediatric accidental injury. nine0147 European Child & Adolescent Psychiatry , 2008. 17(5): p. 316-325.
- Cox, C.M., J.A. Kenardy, and J.K. Hendrikz, A Randomized Controlled Trial of a Web-Based Early Intervention for Children and their Parents Following Unintentional Injury. Journal of Pediatric Psychology , 2010. 35(6): p. 581-592.
- Zehnder, D., M. Meuli, and M.A. Landolt, Effectiveness of a single-session early psychological intervention for children after road traffic accidents: a randomized controlled trial.
 nine0147 Child and adolescent psychiatry and mental health , 2010. 4: p. 7.
nine0147 Child and adolescent psychiatry and mental health , 2010. 4: p. 7. - Berkowitz, S.J., C.S. Stover, and S.R. Marans, The Child and Family Traumatic Stress Intervention: Secondary prevention for youth at risk of developing PTSD. Journal of Child Psychology and Psychiatry , 2011. 52(6): p. 676-685.
- Scheeringa, M.S., et al., Trauma-focused cognitive-behavioral therapy for posttraumatic stress disorder in three-through six year-old children: a randomized clinical trial. nine0147 Journal of Child Psychology and Psychiatry , 2011. 52(8): p. 853-860.
- Melnyk, B.M., et al., Creating opportunities for parent empowerment: Program effects on the mental health/coping outcomes of critically ill young children and their mothers. Pediatrics , 2004. 113(6): p. E597-E607.
- Kramer, D.N. and M.A. Landolt, Characteristics and efficacy of early psychological interventions in children and adolescents after single trauma: a meta-analysis.

Learn more
In the presence of pronounced somatic symptoms, the child is referred to narrow specialists to exclude possible diseases. Differential diagnosis is carried out with primary depressive states, behavioral disorders, acute reactions to stress. The key point is the delay, staging of PTSD symptoms, the presence of triggers, and reactions to them.
Treatment of PTSD in children
Post-traumatic syndrome occurs when there is a violation of the processing of life experience of extreme situations - moments from the past exist in real life, change it. Therefore, treatment involves working with a child psychologist, psychotherapist - specialists who help to understand, survive, let go of traumatic events.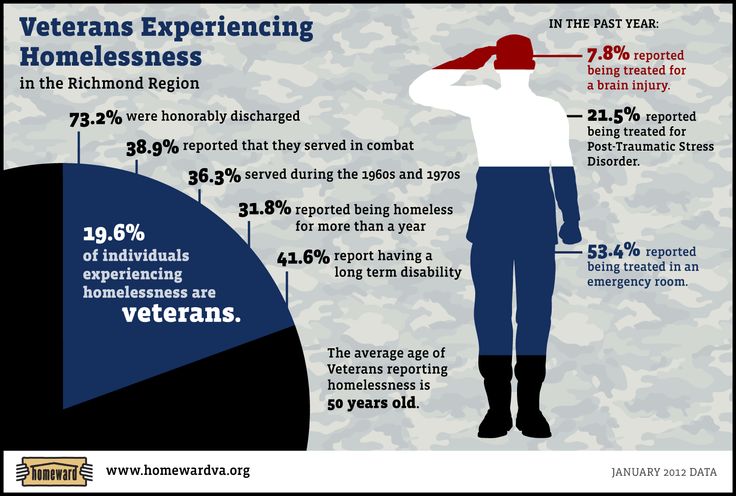 Comprehensive therapy for PTSD in children includes: nine0006
Comprehensive therapy for PTSD in children includes: nine0006
Prognosis and prevention
In the early stages of PSTR, the prognosis is favorable, the disorder can be eliminated with complex psychotherapeutic help, supplemented by medication. The chronic form of the syndrome is more difficult to treat - complications develop, psychopathization of the personality occurs. Pathological changes are more stable and require long-term medical supervision. You can reduce the likelihood of post-traumatic syndrome by proper organization of life. It is necessary to ensure the maximum involvement of the child in social relations: school attendance, friendly meetings, sports clubs, active family recreation.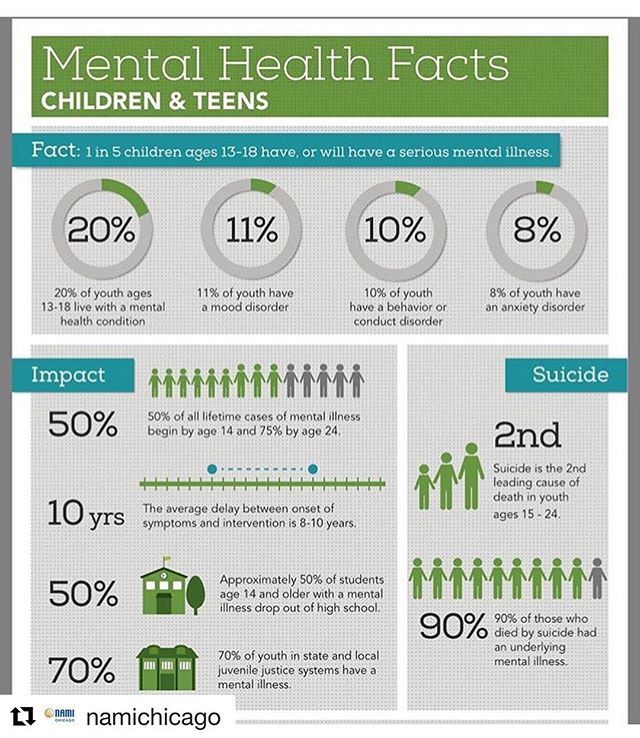 Enthusiasm for the present is important - meetings, studies, creativity, achievements. If a child wants to discuss a difficult event that has occurred, one cannot refuse, but it is worth talking about it as if it were a past experience. nine0006
Enthusiasm for the present is important - meetings, studies, creativity, achievements. If a child wants to discuss a difficult event that has occurred, one cannot refuse, but it is worth talking about it as if it were a past experience. nine0006
You can share your medical history, what helped you in the treatment of post-traumatic stress disorder in children.
Sources