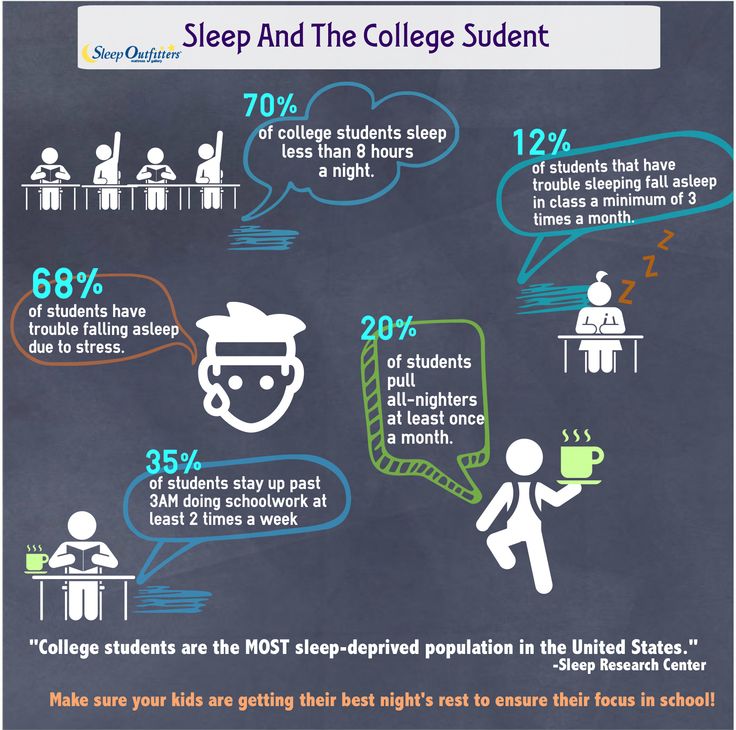
Men with ptsd and relationships
PTSD: National Center for PTSD
Available en Español
Support from family and friends is important for people with PTSD. At the same time, PTSD symptoms may create problems with trust or make it hard to talk through problems. Learn how PTSD affects relationships and read tips about how you can support someone with PTSD.
Reading time: minutes
Trauma survivors with PTSD may have trouble with their close family relationships or friendships. The symptoms of PTSD can cause problems with trust, closeness, communication, and problem solving. These problems may affect the way the survivor acts with others. In turn, the way a loved one responds to him or her affects the trauma survivor. A circular pattern can develop that may sometimes harm relationships.
How Might Trauma Survivors React?
In the first weeks and months following a trauma, survivors may feel angry, detached, tense or worried in their relationships. In time, most are able to resume their prior level of closeness in relationships. Yet the 5% to 10% of survivors who develop PTSD may have lasting relationship problems.
Survivors with PTSD may feel distant from others and feel numb. They may have less interest in social or sexual activities. Because survivors feel irritable, on guard, jumpy, worried, or nervous, they may not be able to relax or be intimate. They may also feel an increased need to protect their loved ones. They may come across as tense or demanding.
The trauma survivor may often have trauma memories or flashbacks. He or she might go to great lengths to avoid such memories. Survivors may avoid any activity that could trigger a memory. If the survivor has trouble sleeping or has nightmares, both the survivor and partner may not be able to get enough rest. This may make sleeping together harder.
Survivors often struggle with intense anger and impulses. In order to suppress angry feelings and actions, they may avoid closeness. They may push away or find fault with loved ones and friends. Also, drinking and drug problems, which can be an attempt to cope with PTSD, can destroy intimacy and friendships. Verbal or physical violence can occur.
They may push away or find fault with loved ones and friends. Also, drinking and drug problems, which can be an attempt to cope with PTSD, can destroy intimacy and friendships. Verbal or physical violence can occur.
In other cases, survivors may depend too much on their partners, family members, and friends. This could also include support persons such as health care providers or therapists.
Dealing with these symptoms can take up a lot of the survivor's attention. He or she may not be able to focus on the partner. It may be hard to listen carefully and make decisions together with someone else. Partners may come to feel that talking together and working as a team are not possible.
How Might Loved Ones React?
Partners, friends, or family members may feel hurt, cut off, or down because the survivor has not been able to get over the trauma. Loved ones may become angry or distant toward the survivor. They may feel pressured, tense, and controlled. The survivor's symptoms can make a loved one feel like he or she is living in a war zone or in constant threat of danger. Living with someone who has PTSD can sometimes lead the partner to have some of the same feelings of having been through trauma.
Living with someone who has PTSD can sometimes lead the partner to have some of the same feelings of having been through trauma.
In sum, a person who goes through a trauma may have certain common reactions. These reactions affect the people around the survivor. Family, friends, and others then react to how the survivor is behaving. This in turn comes back to affect the person who went through the trauma.
Trauma Types and Relationships
Certain types of "man-made" traumas can have a more severe effect on relationships. These traumas include:
- Childhood sexual and physical abuse
- Rape
- Domestic violence
- Combat
- Terrorism
- Genocide
- Torture
- Kidnapping
- Prisoner of war
Survivors of man-made traumas often feel a lasting sense of terror, horror, endangerment, and betrayal. These feelings affect how they relate to others. They may feel like they are letting down their guard if they get close to someone else and trust them. This is not to say a survivor never feels a strong bond of love or friendship. However, a close relationship can also feel scary or dangerous to a trauma survivor.
This is not to say a survivor never feels a strong bond of love or friendship. However, a close relationship can also feel scary or dangerous to a trauma survivor.
Do All Trauma Survivors Have Relationship Problems?
Many trauma survivors do not develop PTSD. Also, many people with PTSD do not have relationship problems. People with PTSD can create and maintain good relationships by:
- Building a personal support network to help cope with PTSD while working on family and friend relationships
- Sharing feelings honestly and openly, with respect and compassion
- Building skills at problem solving and connecting with others
- Including ways to play, be creative, relax, and enjoy others
What Can Be Done to Help Someone Who Has PTSD?
Relations with others are very important for trauma survivors. Social support is one of the best things to protect against getting PTSD. Relationships can offset feelings of being alone. Relationships may also help the survivor's self-esteem. This may help reduce depression and guilt. A relationship can also give the survivor a way to help someone else. Helping others can reduce feelings of failure or feeling cut off from others. Lastly, relationships are a source of support when coping with stress.
This may help reduce depression and guilt. A relationship can also give the survivor a way to help someone else. Helping others can reduce feelings of failure or feeling cut off from others. Lastly, relationships are a source of support when coping with stress.
If you need to seek professional help, try to find a therapist who has skills in treating PTSD as well as working with couples or families. For resources, please see our Get Help in a Crisis page.
Many treatment approaches may be helpful for dealing with relationship issues. Options include:
- One-to-one and group therapy
- Anger and stress management
- Assertiveness training
- Couples counseling
- Family education classes
- Family therapy
See Partners of Veterans with PTSD for more information and a list of recommended readings.
Go To Provider Version
6 Things I Learned from Dating Someone with PTSD
One lesson: Caring for yourself is essential.
How we see the world shapes who we choose to be — and sharing compelling experiences can frame the way we treat each other, for the better. This is a powerful perspective.
There’s nothing that can make you feel as powerless as living with a partner with post-traumatic stress disorder (PTSD).
For three years, I was in a relationship with a man who experienced PTSD symptoms daily. My ex, D., was a decorated combat veteran who served in Afghanistan three times. The toll it took on his soul was heartbreaking.
His flashbacks and dreams of the past drove him to be hypervigilant, fear strangers, and fend off sleep to avoid nightmares.
Being the partner of someone who has PTSD can be challenging — and frustrating — for many reasons. You want to take away their pain, but you’re also dealing with your own guilt at needing to care for yourself, too.
You want to have all the answers, but you often have to come to grips with the reality that this is a condition that can’t be loved out of someone.
That said, understanding the disorder can help make it easier for both you and your partner to communicate and set healthy boundaries.
I spent years trying to understand how PTSD affected my partner, and, ultimately, had to walk away from our relationship. Here’s what I learned.
PTSD is a debilitating anxiety disorder that occurs after a traumatic event, like war combat. Experts estimate 8 million adults have PTSD to varying degrees each year in the United States. Like depression or other mental and behavioral issues, it’s not something that a person can snap out of.
Symptoms arise anywhere from three months to years after the triggering event. In order to be characterized as PTSD, the person must exhibit these traits:
- At least one re-experiencing symptom (like flashbacks, bad dreams, or frightening thoughts). D. installed security cameras in his home to monitor threats and had terrible nightmares.
- At least one avoidance symptom.
 D. didn’t like crowds and would avoid activities that included a lot of people.
D. didn’t like crowds and would avoid activities that included a lot of people. - At least two arousal and reactivity symptoms. D. had a very short fuse and would get frustrated easily when he wasn’t understood.
- At least two cognition and mood symptoms, which includes negative self-esteem, guilt, or blame. D. would often say to me, “Why do you love me? I don’t see what you see.”
D. once described his PTSD to me like a constant waiting game for ghosts to jump from around the corner. It was a reminder that bad things happened, and that that feeling might never stop. Loud noises made it worse, like thunder, fireworks, or truck backfire.
There was a time we sat outside watching fireworks, and he held my hand until my knuckles turned white, telling me the only way he could sit through them was to have me next to him.
For us, these symptoms made basic relationship things difficult, like going out to dinner to a place that was new to him.
And then there was the skittishness and aggression, which are common for people with PTSD. I couldn’t come up behind him without first giving him warning — especially when he had headphones on.
He also had explosive outbursts of rage, which left me in tears.
He was the softest, most complimentary man 90 percent of the time. But when he felt wounded or scared, his cruel side became consuming. He knew my buttons to press — my insecurities and weaknesses — and he had no shame using them as a weapon when he felt angry.
D. is beautiful — inside and out. Not only is he strikingly handsome, he is smart, caring, and compassionate. But he didn’t feel he was deserving of love, or even remotely loveable.
“Traumatic experiences, in addition to being scary and impacting our sense of safety, very often have a direct effect on our cognition,” says Irina Wen, MD, a psychiatrist and director of the Steven A. Cohen Military Family Clinic at NYU Langone Health.
“Usually those effects are negative. As a result, the patient might start feeling undeserving and unlovable, or that the world is a dangerous place and people should not be trusted,” she explains.
As a result, the patient might start feeling undeserving and unlovable, or that the world is a dangerous place and people should not be trusted,” she explains.
Over time, these negative thoughts become generalized so that negativity permeates all aspects of life. They can also carry over into a relationship.
D. would often ask me what I saw in him, how I could love him. This deep insecurity shaped how I treated him, with more reassurances without prompting.
D. needed a lot of time and attention from me. Because he had lost so much in his life, he had an almost controlling grip on me, from needing to know every detail of my whereabouts and having meltdowns when the plan changed last minute, to expecting me to be loyal to him above my own parents, even when I felt he didn’t always deserve it.
But I obliged him. I walked out of the room on friends and stayed on the phone with him for hours. I took photos of who I was with to prove to him I wasn’t cheating or leaving him. I picked him over everyone in my life. Because I felt that if I didn’t, who would?
I picked him over everyone in my life. Because I felt that if I didn’t, who would?
In believing that he was unlovable, D. also created scenarios that cast him as such. When he was angry, he’d express it by taking horrific jabs at me.
I’d be left feeling torn apart, worried about the next time D. would try to verbally hurt me. At the same time, he often didn’t feel safe opening up to me, another symptom of his PTSD.
“I have seen plenty of situations where the partner doesn’t know that their significant other is suffering from PTSD. All they experience is the anger from their partner, when in reality this person has a psychological injury and is suffering and doesn’t know how to speak about it. This leads to more and more disconnection in the couple, and it becomes a vicious cycle,” Wen says.
Amid the feelings of hopelessness and isolation, people with PTSD do have options. The best way to tackle the mental health issue is with education and seeking the help of a professional.
“People with PTSD feel like they are going crazy and are all alone in their condition. And the partner feels exactly the same,” Wen says.
“Often what we see in our clinic is that couples therapy becomes a gateway into individual treatment,” Wen shares. “The veteran might not necessarily agree to individual treatment yet. They don’t want to feel like there is something wrong with them.”
To support my partner and my own mental health, I continued my established solo therapy routine. Beyond that, I researched and tried a few other treatment options as well.
Here are few that may help you or your partner with PTSD:
- Seek individual therapy as a partner of someone with PTSD.
- Encourage your partner to attend individual therapy with a PTSD specialist.
- Attend couples therapy.
- Find support groups for people with PTSD or their loved ones.
Many people who have relationships with someone with PTSD assume the role of caretaker. At least, this was the case with me.
At least, this was the case with me.
I wanted to be the one person who didn’t abandon D. I wanted to show him love can conquer all and that, with the right person, love could help him reinforce and reinstate a healthy lifestyle.
As heartbreaking as it is to admit, love often doesn’t conquer all. This realization came in waves over the three years we were together, mixed with intense feelings of guilt and inadequacy.
“It’s an illusion, this idea that we can save people,” Wen says. “It’s ultimately their responsibility as an adult to seek help, or to ask for help, even if it isn’t their fault that they experienced trauma. We cannot make anyone take the help.”
Caretakers in relationships with people with PTSD often forget to take care of themselves.
I developed guilt associated with personal fulfillment or enjoyment, because it’s easy to get sucked into an unhealthy cycle.
When I wanted to hang out with friends without having to spend an hour talking D. down or not check in consistently while I was traveling for work to let him know I was safe, I felt guilty.
down or not check in consistently while I was traveling for work to let him know I was safe, I felt guilty.
The partner of someone with PTSD will have to be strong a lot of the time. To do this, you must take care of your own mental health.
Wen agrees. “When you’re in a caretaker role, you have to put the mask on yourself first,” she says. “It must be a conscious effort to carve out time for yourself. The caretaker has to stay strong if they are to become a support system, and they need to have support and healthy outlets to maintain that.”
After years of baby steps forward and monumental steps back, I ultimately made the decision to end the relationship.
It wasn’t because I don’t love D. I love him and miss him every moment.
But the issues surrounding PTSD that needed to be addressed called for dedicated commitment, time, and the help of a professional — things he didn’t say he was opposed to. Still, he never made the choices to show he was ready.
The guilt, sadness, and feeling of defeat were all encompassing. For two months I barely left my apartment. I felt like I failed him.
It was a long time before I could accept it wasn’t my job to make someone seek help who wasn’t ready for it, and that it was OK for me to put myself first.
“We can’t make anyone take the help. Let go of guilt. You might feel sadness and grief over the loss of the relationship, but as much as possible, set aside guilt. It is going to be an unhelpful emotion in this situation,” Wen says.
“Say ‘I love you.’ Say ‘I would love for this to work and for you to get help because it affects me, you, and the relationship, but this is how far I’m able to go,’” she recommends.
As for me, I’m now spending time on healing myself and indulging in the fulfilling work and carefree fun that often made me feel guilty in the past.
Share on Pinterest
Meagan Drillinger is a travel and wellness writer. Her focus is on making the most out of experiential travel while maintaining a healthy lifestyle. Her writing has appeared in Thrillist, Men’s Health, Travel Weekly, and Time Out New York, among others. Visit her blog or Instagram.
Her writing has appeared in Thrillist, Men’s Health, Travel Weekly, and Time Out New York, among others. Visit her blog or Instagram.
Avicenna himself: 13 signs of post-traumatic disorder in entrepreneurs
The quarantine caused by the pandemic has a negative impact on health and leaves a deep mark on the psyche of many people - trauma. Psychologist, HSE teacher and consultant of the Ontology.one project Mikhail Stavissky tells how to recognize the symptoms of post-traumatic stress disorder in yourself
business. We begin to be haunted by constant stress from the need to make decisions, fear and anxiety for ourselves and loved ones, forced to engage in non-core activities, chronic fatigue from the inability to work and rest normally. Self-isolation and social distancing worsened the mental health of 55% of respondents, according to a Benenson Strategy Group survey. People of all generations report anxiety and symptoms of depression during the pandemic, with Millennials born in 19 years experiencing the most.81-1996, as well as Gen Z born 1997 and later, according to the NRC Health report.
People of all generations report anxiety and symptoms of depression during the pandemic, with Millennials born in 19 years experiencing the most.81-1996, as well as Gen Z born 1997 and later, according to the NRC Health report.
Lack of full-fledged government support, insecurity for one’s business and personal well-being, lack of an airbag, negative salvage value, the pursuit of luxury and living beyond one’s means, other stress factors are today’s business reality and a very serious mental health challenge. How to recognize the symptoms of mental trauma in yourself,
It is common in business even in calm times to expect "alarm ahead" when a person is worried "in advance". Business treats negative information with less criticism and healthy skepticism. But now, when, on the one hand, the disease, and on the other hand, economic problems come to a close circle, the threats are perceived as especially real. Now we see a triad of depression: a stressful traumatic situation, a psychologically understandable cause, a reaction and an outcome either in a mental disorder or in recovery. But there is an outcome in the form of post-traumatic disorders that will come later, we can afford to show this reaction.
Now we see a triad of depression: a stressful traumatic situation, a psychologically understandable cause, a reaction and an outcome either in a mental disorder or in recovery. But there is an outcome in the form of post-traumatic disorders that will come later, we can afford to show this reaction.
What is happening now with us and with our businesses has a negative impact on mental health and is very likely to leave a deep mark, trauma in the psyche of people. The consequence of this injury can be post-traumatic stress disorder, which can manifest itself for many months before the end of the quarantine and corona crisis.
In the book How to Live After Trauma, Benjamin Kolodzin, an American psychologist, founder and director of the Olympia Institute, which provides assistance to Vietnam War veterans, victims of crime and people who have suffered trauma, writes: “When a person does not have the opportunity defuse internal tension, his body and psyche find a way to somehow apply to this tension. This, in principle, is the mechanism of post-traumatic stress. His symptoms, which in the complex look like a mental disorder, are in fact nothing more than deeply rooted behaviors associated with extreme events in the past.
This, in principle, is the mechanism of post-traumatic stress. His symptoms, which in the complex look like a mental disorder, are in fact nothing more than deeply rooted behaviors associated with extreme events in the past.
One of the symptoms of negative changes in the emotional state is when an employee abruptly changes his usual behavior: this is a change in mood, lethargy or the opposite anxious fussiness, difficulty concentrating. The presence of at least one symptom should alert. After the crisis and the pandemic, many entrepreneurs will experience the following symptoms:
1. Excessive, unmotivated suspicion, incredulity. A person constantly experiences anxiety, tension, constant expectation of danger.
2. Hot temper, impulsiveness, and in "peaceful" time inherent in leaders, will interfere even more, knocking out of the resource state.
3. Emotional callousness, cynicism. It will become difficult for people to express themselves emotionally. It is difficult to establish collaborative, close and intimate ties with others, feelings of joy, love, admiration will become less available. It will be more difficult to feel creative, motivated, playful, light, spontaneous. It’s as if you don’t want to experience these feelings, they become dull, there is a feeling of embarrassment for manifestations of joy, openness.
It will become difficult for people to express themselves emotionally. It is difficult to establish collaborative, close and intimate ties with others, feelings of joy, love, admiration will become less available. It will be more difficult to feel creative, motivated, playful, light, spontaneous. It’s as if you don’t want to experience these feelings, they become dull, there is a feeling of embarrassment for manifestations of joy, openness.
4. Increased intolerance, aggressiveness. Negotiability decreases, there is a temptation to solve problems with the help of attacks, pressure, insults. This manifests itself both on the physical and on the mental, emotional level. A person begins to use aggression and pressure on others whenever he wants to achieve his goal, even if the goal is not so important for him.
5. Syndrome of memory loss and impaired concentration. A person cannot concentrate, finds it difficult to make a decision, find an answer to a simple task. Moreover, such difficulties appear under certain circumstances, when a stressful factor appears in a person’s field of vision, which begins to interfere with concentration, a person falls into a panic or stupor.
Moreover, such difficulties appear under certain circumstances, when a stressful factor appears in a person’s field of vision, which begins to interfere with concentration, a person falls into a panic or stupor.
6. In a state of post-traumatic stress disorder, depression develops, a person falls into despair, it seems that business, life, family - everything loses its meaning, becomes unimportant and useless. Against the background of depression, emotional exhaustion, apathy appear, suicidal thoughts develop.
7. At the psychological and physiological levels, high anxiety appears, which responds in psychosomatics with pain in the head, stomach, and heart. The person feels anxious and preoccupied. The already high paranoia, suspiciousness in business develops into persecution mania. Fear of annihilation, an oppressive feeling of fear, self-doubt, guilt, the syndrome of a loser become the leader's companion.
8. During such periods, any negative or even neutral events can cause outbursts of rage in people. It becomes easy to manipulate a person, infuriating him with a few words at the negotiating table or during the conclusion of an important deal.
During such periods, any negative or even neutral events can cause outbursts of rage in people. It becomes easy to manipulate a person, infuriating him with a few words at the negotiating table or during the conclusion of an important deal.
9. Dependence on alcohol, psychotropic substances, extreme entertainment, increased gambling addiction - through such abuse, we try to drown out the pain screaming inside him.
10. Obsessive memories appear. Manifestations of obsessive disorder and compulsive actions inspired by difficult thoughts are one of the important symptoms of post-stress disorder. Heavy dreams, nocturnal panic attacks. In reality, they appear in cases where the environment resembles the events that happened during quarantine. Images of the past evoke painful memories and stress. Such memories are accompanied by intense anxiety and fear.
11. Insomnia and interrupted sleep lead to nervous exhaustion. Poor sleep adds to the picture of PTSD symptoms. Insomnia can be caused by high levels of anxiety, an inability to relax, as well as feelings of fatigue and mental pain.
Poor sleep adds to the picture of PTSD symptoms. Insomnia can be caused by high levels of anxiety, an inability to relax, as well as feelings of fatigue and mental pain.
12. Thoughts about a dead end, uselessness, meaninglessness. The person begins to think about death. Business, family, the future seem more terrible than leaving them. There are thoughts of escapism, the end of all worries and anxieties. When a person reaches a state where there is no end, purpose, meaning, he begins to lose faith, hope, and involvement falls. Only passionate desire and perseverance can help a person get out of his "box" and see the prospects.
13. Even those who survived the crisis and the pandemic without much loss develop negative feelings. First of all, a feeling of guilt because I survived this period better than others. Many businessmen who have gone through difficult periods are ready to do anything to avoid being reminded of what they have experienced. Guilt provokes the behavior described by the classic when a non-commissioned officer's wife tries to flog herself. It is this that leads to emotional deafness, so a person is protected from unbearable thoughts.
Guilt provokes the behavior described by the classic when a non-commissioned officer's wife tries to flog herself. It is this that leads to emotional deafness, so a person is protected from unbearable thoughts.
It is important to know the symptoms of post-traumatic stress disorder not in order to be able to understand complex mental mechanisms or to look for all problems outside or in the past, but in order to realize for oneself the causal relationship between the “here and now” state and experienced events. From the point of view of therapy, it is important to study yourself, your life, to look into the hidden areas of the soul.
If you recognize yourself in the picture of PTSD symptoms, this means that you have taken an important first step, ready to take an honest look at some aspects of your life. By accepting the reality of your life with all its good and bad, you will be able to ask yourself the question: “What should I do today to make a difference?” The task of the leader is to become reflective, thinking, analyzing. Be able to understand yourself in order to demonstrate the best human qualities to the team. We cannot help an employee get rid of fears of illness or a mistake, but we can teach them how to endure traumatic feelings and how to cope with their consequences.
Be able to understand yourself in order to demonstrate the best human qualities to the team. We cannot help an employee get rid of fears of illness or a mistake, but we can teach them how to endure traumatic feelings and how to cope with their consequences.
Clinical experience teaches that one of the deepest human fantasies is the belief that somewhere there is an omnipotent, omniscient Other who can fix things. Some live their lives in a scenario in which they try to get an imaginary powerful mother to see how they suffer so that she intervenes and saves them. They come with this template to a psychologist and go through session after session, developing their pain and resisting attempts to help them understand that it is time to give up their childhood dream of an ideal parent in order to gain the ability to enjoy reality. Today, those leaders who are in touch with reality and tell the truth are better at helping to survive difficulties than those who resist reality, try to maintain the idea of their omnipotence and calm themselves with positive thinking, lies and illusions. The main task of psychologists in business today is to speak openly about how emotionally traumatic what is happening, to help create the most comfortable conditions for employees, in which they will feel as safe as possible, and to help restore peace of mind.
The main task of psychologists in business today is to speak openly about how emotionally traumatic what is happening, to help create the most comfortable conditions for employees, in which they will feel as safe as possible, and to help restore peace of mind.
The task of the employee is to realize the change in his condition and to contact a specialist in a timely manner. Thanks to the current situation, companies will become more responsible and conscious. We begin to understand that success accompanies those who know how to survive and enjoy life in conditions of uncertainty, understand their strengths and weaknesses and are ready to face reality. Responsible leaders who recognize themselves as the cause of everything that happens in their lives will win today. The higher the ability to be aware of oneself, the higher the responsibility. And the higher, in turn, the resilience in business. Quarantine is seen today as a difficult, but life-giving, cleansing procedure. At the end of it, for many, the question will be much more obvious: what are we really worth and how much does a business cost? Those who pass this exam will move to a new level and will definitely become stronger.
At the end of it, for many, the question will be much more obvious: what are we really worth and how much does a business cost? Those who pass this exam will move to a new level and will definitely become stronger.
The great healer Avicenna used to say: “A doctor has three means to fight a disease — a word, a plant, a knife,” and the word comes first. Paracelsus argued that faith works miracles, our health is a direct consequence of human thinking. Today, no one doubts that there is a direct connection between the emotional and physical state of people. The verbal expression of love, sympathy and support enhances the life energy of the one to whom it is addressed. Today we can safely say: we are what we say and hear. Learning to speak and hear words that make us stronger is the main work of a psychologist today.
The material was written as part of the Ontology.one project
About the Ontology. one online platform:
one online platform:
Today, it is vital for all of us to be able to quickly readjust, learn to relieve stress and anxiety, find an internal resource to move towards the goal . The Ontology.one online platform, created by the Forbes Ontology personal development club in partnership with Netology Group, allows everyone to find the perfect coach to solve personal, career and business problems quickly and efficiently.
You can sign up for a free online consultation here.
PTSD
") end if %>
Variant of Acrobat Samana Gaze | Acrobat Reader Samana Download
PTSD is a normal response
for severe traumatic events.
This booklet deals with signs,
symptoms and treatments for PTSD.
New York State
Department of Mental Health
Have you experienced a terrible and dangerous event? Note please, those cases in which you recognize yourself.
- Sometimes, out of the blue, everything that happened to me is happening again. I never know when to expect it again.
- I have nightmares and memories of that terrible incident which I have experienced.
- I avoid places that remind me of that incident.
- I jump on the spot and feel uneasy at any sudden movement or surprise. I feel alert all the time.
- It's hard for me to trust someone and get close to someone.
- Sometimes I just feel emotionally drained and deaf.
- I get angry very easily.
- I am tormented by guilt that others died, but I survived.
- I sleep poorly and experience muscle tension.
PTSD is a very serious condition that needs to be treated.
Many people who have experienced terrible events suffer from this disease.
It is not your fault that you fell ill, and you should not suffer from it.
Read this booklet to find out how you can be helped.
You can recover and enjoy life again!
What is post-traumatic stress disorder (PTSD/PTSD)?
PTSD is a very serious condition. PTSD symptoms may occur in a person who has experienced a terrible traumatic event. This disease is susceptible medical and therapeutic treatment.
PTSD can occur after you:
- Have been a victim of sexual abuse
- Have been a victim of physical or emotional domestic violence
- Victim of a violent crime
- Have been in a car accident or plane crash
- Survived a hurricane, tornado, or fire
- Were at war
- Survived a life-threatening event
- Witnessed any of the above events
If you have post-traumatic stress disorder, you often have nightmares or memories associated with the event. you try to hold on away from anything that might remind you of the experience.
You are bitter and unable to trust or care for others.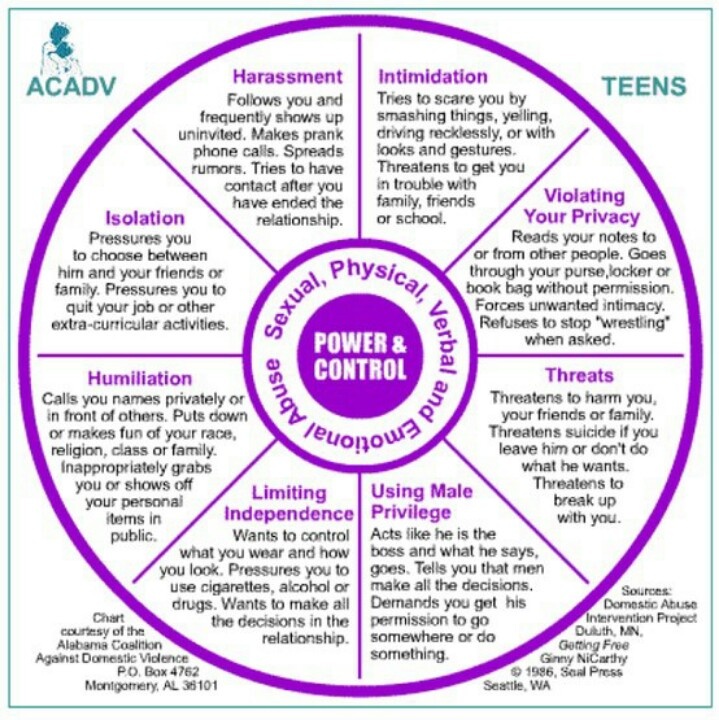 You are always on your guard and see a hidden threat in everything. You become not by itself, when something happens suddenly and without warning.
You are always on your guard and see a hidden threat in everything. You become not by itself, when something happens suddenly and without warning.
When does PTSD start and how long does it last?
In most cases, post-traumatic stress manifests itself approximately three months after the traumatic event. In some cases, signs Post-traumatic stress symptoms only show up years later. Post-traumatic Stress affects people of all ages. Even children are not immune from it.
Some get better after six months, others may suffer from it illness for much longer.
Am I the only one with this condition?
No, you are not alone. Every year, 5.2 million Americans suffer from PTSD.
Women suffer from this disease two and a half times more often than men. The most common traumatic events that cause PTSD in men are: rape, participation in hostilities, abandonment and abuse in childhood. The most traumatic events in women are rape, sexual molestation, physical assault, threat weapons and childhood abuse.
What other conditions can accompany PTSD?
Comorbid depression, alcohol and drug addiction, or other common anxiety disorders. The likelihood of successful treatment increases if these comorbidities to identify and treat in time.
Frequent headaches, gastroenterological problems, problems with the immune system, dizziness, chest pain or discomfort in other parts of the body. It often happens that a doctor treats physical symptoms, unaware that their cause lies in PTSD.
The National Institute of Mental Health (NIMH) recommends therapists to learn from patients about experiences of violence, recent losses and traumatic events, especially when symptoms persist are returning. After diagnosing PTSD, it is recommended to refer patient to a mental health specialist who has experience in the treatment of patients with PTSD.
What can I do to help myself in this situation?
Talk to your doctor and tell him about your experience, and how you feel. If you are visited by terrible memories, overcomes depression and sadness if you have trouble sleeping and constantly embittered - you should tell your doctor about all this. Tell him Are any of these conditions preventing you from doing your daily activities? lead a normal life. You may want to show this booklet to your doctor. This may help explain to him how you feel. Ask your doctor examine you to make sure there are no physical illnesses.
If you are visited by terrible memories, overcomes depression and sadness if you have trouble sleeping and constantly embittered - you should tell your doctor about all this. Tell him Are any of these conditions preventing you from doing your daily activities? lead a normal life. You may want to show this booklet to your doctor. This may help explain to him how you feel. Ask your doctor examine you to make sure there are no physical illnesses.
Ask your doctor if he has had patients with post-traumatic stress. If your doctor does not have a special preparation, ask him for directions to doctor with relevant experience.
How can a doctor or psychotherapist help me?
Your doctor may prescribe medication to help reduce your fear or tension. However, it should be borne in mind that usually several weeks before the medicine starts to work.
Many PTSD sufferers benefit from talking with a professional or other people who have experienced traumatic events. This is called "therapy". Therapy will help you get over your nightmare.
This is called "therapy". Therapy will help you get over your nightmare.
One man's story:
"After I was attacked, I He constantly felt fear and depression, became irritable. I couldn't sleep well and lost my appetite. Even when I tried not think about what happened, I was still tormented nightmares and terrible memories.
“I was completely at a loss and didn't know what to do. one buddy advised to see a doctor. My doctor helped me find a specialist in post-traumatic stress."
“I needed a lot of strength, but after medication and a course of therapy, I gradually come to my senses. It’s good that I called my doctor then.”
PTSD and the military
If you are in the military, you have probably been in combat. You, probably got into terrible and life-threatening situations. They shot at you you have seen your friend shot, you have seen death. experienced you events can cause PTSD.
Experts say PTSD occurs:
- Nearly 30% of Vietnam War veterans
- Nearly 10% of Gulf War veterans (Operation Desert Storm)
- Almost 25% of veterans of the war in Afghanistan (operations "Introducing freedom") and veterans of the war in Iraq (operations "Iraqi Freedom")
Other factors of the military environment can serve as an additional stress to and so stressful situation and can contribute to the development of PTSD and other mental problems. Among these factors are the following: your military specialty, the political aspects of the war, where the battle takes place and who your enemy is.
Another reason that contributes to PTSD in military personnel can be Military Sexual Assault (MST) – any form of sexual harassment or sexual abuse while serving in the military. MST can happen with men and women, and can occur in peacetime, during war training or during the war.
Among veterans with Veterans Affairs (VA) health care, approximately:
- 23 out of 100 women (23%) report sexual violence during military service
- 55 out of 100 women (55%) and 38 out of 100 men (38%) were exposed to sexual harassment while serving in the army
Although the trauma of sexual assault is more common in the military among women, more than half of veterans who have experienced sexual trauma violence in the army - it's men.
Remember, you can get the help you need right now:
Tell your doctor about your experience and how you feel. If your doctor does not have special training in the treatment of PTSD, ask him for a referral to a doctor who has relevant experience.
PTSD research
To help those suffering from PTSD, the National Institute of Conservation Mental Health (NIMH) supports research into the study of PTSD, as well as other thematically related to PTSD research on problems anxiety and fear. The challenge for research is to find new ways to help people cope with trauma, as well as find new treatment options and, The main thing is to prevent disease.
Research on possible risk factors for PTSD
Today, the attention of many scientists is focused on genes that play a role in having terrible memories. Understanding the mechanism of "creation" of scary memories can help improve or find new ways to alleviate symptoms of PTSD. For example, PTSD researchers have identified genes that are responsible for:
For example, PTSD researchers have identified genes that are responsible for:
Statmin - a protein involved in the formation of terrible memories. During one experiment, mice were placed in environment designed to instill fear in them. In this situation mice lacking the statmin gene, in contrast to normal mice were less likely to "freeze" - i.e. exercise natural defensive response to danger. Also in the environment designed to evoke innate fear in them, they demonstrated it to a lesser extent than normal mice, more willingly mastering the open "dangerous" space. 1
GRP (gastrin-releasing peptide/ GRP) - signal substance brain released during emotional events. At in mice, GWP helps control the fear response, and lack of GWP can lead to a longer memory of fear. 2
Scientists have also discovered a variant of the 5-HTTLPR gene that controls the level of serotonin (a brain substance associated with mood), which, as it turns out, feeds the fear response. 3 It seems that, like in the case of other mental disorders, in the development of PTSD different genes are involved, each of which contributes to the formation of the disease.
3 It seems that, like in the case of other mental disorders, in the development of PTSD different genes are involved, each of which contributes to the formation of the disease.
Understanding the causes of PTSD can also be helped by studying different areas brain responsible for fear and stress. One of these areas is cerebellar amygdala, responsible for emotions, learning and memory. It turned out that she plays an active role in the emergence of fear (or other words, "teaches" to be afraid of something, for example, to touch a hot stove), as well as in the early phases of fear repayment (or in other words, "teaches" Do not be scared). 4
The retention of faded memories and the weakening of the initial fear reaction are associated with the prefrontal cortex (PFC / PFC) of the brain, 4 responsible for decision making, problem solving and situation assessment. Each zone PFC has its own role. For example, when the PFC believes that a stressor is amenable to control, the medial prefrontal zone of the PFC suppresses the anxiety center deeply in the brainstem and controls the response to stress. 5 Ventromedial PFC helps maintain long-term fading of fearful memories, and her ability to perform this feature can be affected by its size. 6
For example, when the PFC believes that a stressor is amenable to control, the medial prefrontal zone of the PFC suppresses the anxiety center deeply in the brainstem and controls the response to stress. 5 Ventromedial PFC helps maintain long-term fading of fearful memories, and her ability to perform this feature can be affected by its size. 6
Individual differences in genes or characteristics of regions of the brain brain can only set the stage for PTSD, but by themselves do not cause no symptoms. environmental factors such as childhood trauma, head trauma or mental illness in family, favor the development of the disease and increase the risk of disease, affecting the brain in the early stages of its growth. 7 Except In addition, how people adapt to trauma is likely to be influenced by and characteristics of character and behavior, such as optimism and a tendency to consider problems in a positive or negative way, as well as social factors such as availability and use of social support. 8 Further investigations may show what combination of these factors or what other factors will allow ever predict who has a traumatic event cause PTSD, and who doesn't.
8 Further investigations may show what combination of these factors or what other factors will allow ever predict who has a traumatic event cause PTSD, and who doesn't.
Research on the treatment of PTSD
Currently, psychotherapy is used in the treatment of PTSD ("talk" therapy), drugs or drug-therapeutic combination.
Psychotherapy
Cognitive behavioral therapy (CBT) helps you learn differently think and react to frightening events that are the impetus for development PTSD, and can help bring the symptoms of the disease under control. There are several types cognitive behavioral therapy, including:
"Push" method - uses mental images, notes or visiting a place experienced trauma to help those affected face the overwhelming their fear and take control of it.
Behavior restructuring (cognitive restructuring) - encourages survivors of a traumatic event express depressing (often erroneous) thoughts about experienced trauma, challenge these thoughts and replace them with more balanced and appropriate.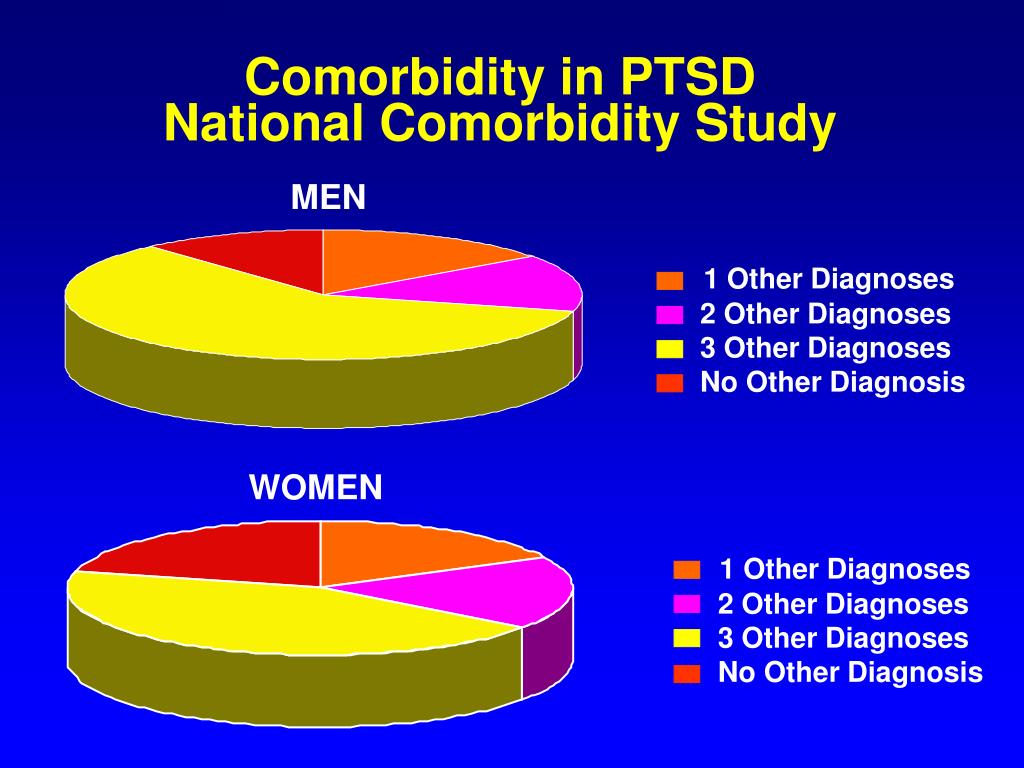
Implementation in a stressful situation - teaches ways to reduce anxiety and the ability to cope with it, helping to reduce the symptoms of PTSD, and helps to correct the erroneous train of thought associated with the trauma experienced. NIMH is currently conducting research to study the reaction brain response to cognitive behavioral therapy versus response sertraline (Zoloft) - one of two drugs recommended and approved US Food and Drug Administration funds (FDA) for the treatment of post-traumatic stress. This research may help find out why some people respond better to medications, and others for psychotherapy
Drugs
Recently, in a small study, NIMH scientists found that if patients who are already taking a dose of prazosin (Minipress) at bedtime, add a daily dose, then this weakens the general symptoms of PTSD and stress reaction to reminders of the trauma experienced. 9
Another drug of interest is D-cycloserine (Seromycin), which increases the activity of a brain substance called N-methyl-D-aspartate, needed to pay off fear. During the study, which was attended by 28 people suffering from a fear of heights, scientists found that patients who received "push" therapy before a session D-cycloserine, showed lower levels of fear during the session compared to those who did not receive the drug. 10 Currently scientists study the effectiveness of the combined use of D-cycloserine and therapy for the treatment of post-traumatic stress.
During the study, which was attended by 28 people suffering from a fear of heights, scientists found that patients who received "push" therapy before a session D-cycloserine, showed lower levels of fear during the session compared to those who did not receive the drug. 10 Currently scientists study the effectiveness of the combined use of D-cycloserine and therapy for the treatment of post-traumatic stress.
Propranolol (Inderal), a beta-blocker drug, also under study whether it can be used to reduce post-traumatic stress and break the chain of scary memories. First experiments gave consoling results: it was possible to successfully weaken and, it seems, prevent PTSD in a small number of victims of traumatic events. 11
For example, in one preliminary study, researchers created a website self-help, based on the use of a psychotherapeutic method implementation in a stressful situation. First, patients with PTSD meet in person with doctor. After this meeting, participants can go to the site to find more information about PTSD and how to deal with the problem; their doctors may also visit the site to give advice or briefing. In general, scientists believe that therapy in this form - promising treatment for a large number of people suffering from PTSD. 12
First, patients with PTSD meet in person with doctor. After this meeting, participants can go to the site to find more information about PTSD and how to deal with the problem; their doctors may also visit the site to give advice or briefing. In general, scientists believe that therapy in this form - promising treatment for a large number of people suffering from PTSD. 12
Scientists are also working to improve methods for testing early treatment and monitoring of survivors of massive trauma, on developing ways to teach them self-assessment skills and introspection and referral mechanism to psychiatrists (if necessary).
Prospects for PTSD research
In the last decade, rapid progress has been made in the study of mental and biological bases PTSD has led scientists to conclude that there is a need to focus on prevention, as the most realistic and important goal.
For example, in order to find ways to prevent PTSD, with funding NIMH conducts research to develop new and orphan drugs, aimed at combating the underlying causes of the disease.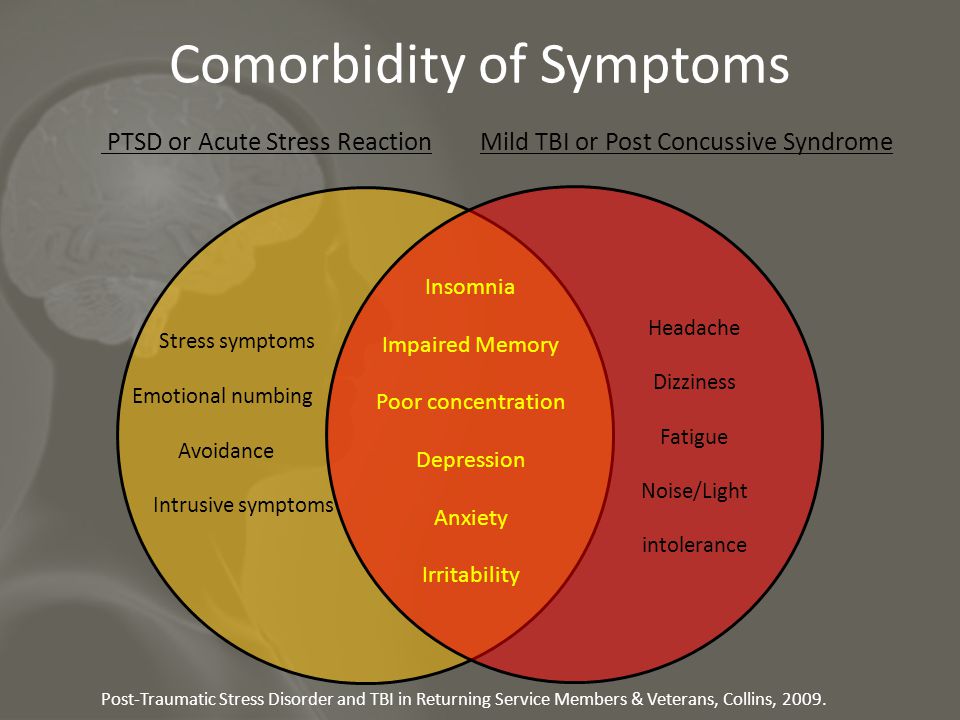 During another research scientists are looking for ways to enhance behavioral, personality and social protective factors and minimizing risk factors for prevent the development of PTSD after trauma. Another study is studying the question of what factors influence the difference in response to one or another method of treatment, which will help in the development of more individual, effective and productive methods of treatment.
During another research scientists are looking for ways to enhance behavioral, personality and social protective factors and minimizing risk factors for prevent the development of PTSD after trauma. Another study is studying the question of what factors influence the difference in response to one or another method of treatment, which will help in the development of more individual, effective and productive methods of treatment.
Where can I find more information?
MedlinePlus - resource from the American National Library of Medicine (U.S. National Library of Medicine and the National Institutes of Health) - offers the latest information on many health issues. Information about You can find PTSD at: www.nlm.nih.gov/medlineplus/posttraumaticstressdisorder.html.
National Institute of Mental Health
Office of Science Policy, Planning, and Communications
[National Institute of Mental Health
Science Policy Division research, planning and communications]
6001 Executive Boulevard
Room 8184, MSC 9663
Bethesda, MD 20892-9663
Phone: 301-443-4513; Fax: 301-443-4279
fax answering system Free answering machine: 1-866-615-NIMH (6464)
Text phone: 1-866-415-8051 toll-free
Email: nimhinfo@nih. gov
gov
National Center for Post-traumatic Stress Disorder
[National PTSD Center]
VA Medical Center (116D)
215 North Main Street
White River Junction, VT 05009
802-296-6300
www.ncptsd.va.gov
NOTES
- Shumyatsky GP, Malleret G, Shin RM, et al. Stathmin, a Gene Enriched in the Amygdala, Controls Both Learned and Innate Fear. cell. Nov 18 2005;123(4):697-709.
- Shumyatsky GP, Tsvetkov E, Malleret G, et al. Identification of a signal network in lateral nucleus of amygdala important for inhibiting memory specifically related to learned fear. cell. Dec 13 2002;111(6):905-918.
- Hariri AR, Mattay VS, Tessitore A, et al. Serotonin transporter genetic variation and the response of the human amygdala.Science. Jul 192002;297(5580):400-403.
- Milad MR, Quirk GJ. Neurons in medial prefrontal cortex signal memory for fear extinction.
 Nature. Nov 7 2002;420(6911):70-74.
Nature. Nov 7 2002;420(6911):70-74. - 5 Amat J, Baratta MV, Paul E, Bland ST, Watkins LR, Maier SF. Medial prefrontal cortex determines how stressor controllability affects behavior and dorsal raphe nucleus. Nat Neurosci. Mar 2005;8(3):365-371.
- Milad MR, Quinn BT, Pitman RK, Orr SP, Fischl B, Rauch SL. Thickness of ventromedial prefrontal cortex in humans is correlated with extinction memory. Proc Natl Acad Sci USA. Jul 26 2005;102(30):10706-10711.
- Gurvits TV, Gilbertson MW, Lasko NB, et al. Neurological soft signs in chronic posttraumatic stress disorder.Arch Gen Psychiatry. Feb 2000;57(2):181-186.
- Brewin CR. Risk factor effect sizes in PTSD: what this means for intervention. J Trauma Dissociation. 2005;6(2):123-130.
- Taylor FB, Lowe K, Thompson C, et al. Daytime Prazosin Reduces Psychological Distress toTrauma Specific Cues in Civilian Trauma Posttraumatic stress disorder.
 Biol Psychiatry. Feb 3 2006.
Biol Psychiatry. Feb 3 2006. - Ressler KJ, Rothbaum BO, Tannenbaum L, et al. Cognitive enhancers as adjuncts to psychotherapy: use of D-cycloserine in phobic individuals to facilitate extinction of fear. Arch Gen Psychiatry. Nov 2004;61(11):1136-1144.
- Pitman RK, Sanders KM, Zusman RM, et al. Pilot study of secondary prevention of posttraumatic stress disorder with propranolol.Biol Psychiatry. Jan 15 2002;51(2):189-192.
- Litz BTWL, Wang J, Bryant R, Engel CC.A therapist-assisted Internet self-help program for traumatic stress. Prof Psychol Res Pr. December 2004;35(6):628-634.
New York State Department of Mental Health expresses thanks to the National Institute of Mental Health for the information, used in this booklet.
Published by the State Department of Mental Health New York, June 2008.
New York State
Andrew M. Cuomo, Gov.
Department of Mental Health
Head of Department Michael F.