Ect forum depression
SAMHSA’s National Helpline | SAMHSA
Your browser is not supported
Switch to Chrome, Edge, Firefox or Safari
Main page content
-
SAMHSA’s National Helpline is a free, confidential, 24/7, 365-day-a-year treatment referral and information service (in English and Spanish) for individuals and families facing mental and/or substance use disorders.
Also visit the online treatment locator.
SAMHSA’s National Helpline, 1-800-662-HELP (4357) (also known as the Treatment Referral Routing Service), or TTY: 1-800-487-4889 is a confidential, free, 24-hour-a-day, 365-day-a-year, information service, in English and Spanish, for individuals and family members facing mental and/or substance use disorders.
This service provides referrals to local treatment facilities, support groups, and community-based organizations.
Also visit the online treatment locator, or send your zip code via text message: 435748 (HELP4U) to find help near you. Read more about the HELP4U text messaging service.
The service is open 24/7, 365 days a year.
English and Spanish are available if you select the option to speak with a national representative. Currently, the 435748 (HELP4U) text messaging service is only available in English.
In 2020, the Helpline received 833,598 calls. This is a 27 percent increase from 2019, when the Helpline received a total of 656,953 calls for the year.
The referral service is free of charge. If you have no insurance or are underinsured, we will refer you to your state office, which is responsible for state-funded treatment programs. In addition, we can often refer you to facilities that charge on a sliding fee scale or accept Medicare or Medicaid. If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
The service is confidential. We will not ask you for any personal information. We may ask for your zip code or other pertinent geographic information in order to track calls being routed to other offices or to accurately identify the local resources appropriate to your needs.
No, we do not provide counseling. Trained information specialists answer calls, transfer callers to state services or other appropriate intake centers in their states, and connect them with local assistance and support.
-
Suggested Resources
What Is Substance Abuse Treatment? A Booklet for Families
Created for family members of people with alcohol abuse or drug abuse problems. Answers questions about substance abuse, its symptoms, different types of treatment, and recovery. Addresses concerns of children of parents with substance use/abuse problems.
Addresses concerns of children of parents with substance use/abuse problems.It's Not Your Fault (NACoA) (PDF | 12 KB)
Assures teens with parents who abuse alcohol or drugs that, "It's not your fault!" and that they are not alone. Encourages teens to seek emotional support from other adults, school counselors, and youth support groups such as Alateen, and provides a resource list.After an Attempt: A Guide for Taking Care of Your Family Member After Treatment in the Emergency Department
Aids family members in coping with the aftermath of a relative's suicide attempt. Describes the emergency department treatment process, lists questions to ask about follow-up treatment, and describes how to reduce risk and ensure safety at home.Family Therapy Can Help: For People in Recovery From Mental Illness or Addiction
Explores the role of family therapy in recovery from mental illness or substance abuse. Explains how family therapy sessions are run and who conducts them, describes a typical session, and provides information on its effectiveness in recovery.
For additional resources, please visit the SAMHSA Store.
Last Updated: 08/30/2022
Alcohol, Tobacco, and Other Drugs
Your browser is not supported
Switch to Chrome, Edge, Firefox or Safari
Misusing alcohol, tobacco, and other drugs can have both immediate and long-term health effects.The misuse and abuse of alcohol, tobacco, illicit drugs, and prescription medications affect the health and well-being of millions of Americans. NSDUH estimates allow researchers, clinicians, policymakers, and the general public to better understand and improve the nation’s behavioral health. These reports and detailed tables present estimates from the 2021 National Survey on Drug Use and Health (NSDUH).
Alcohol
Data:
- Among the 133.1 million current alcohol users aged 12 or older in 2021, 60.0 million people (or 45.1%) were past month binge drinkers.
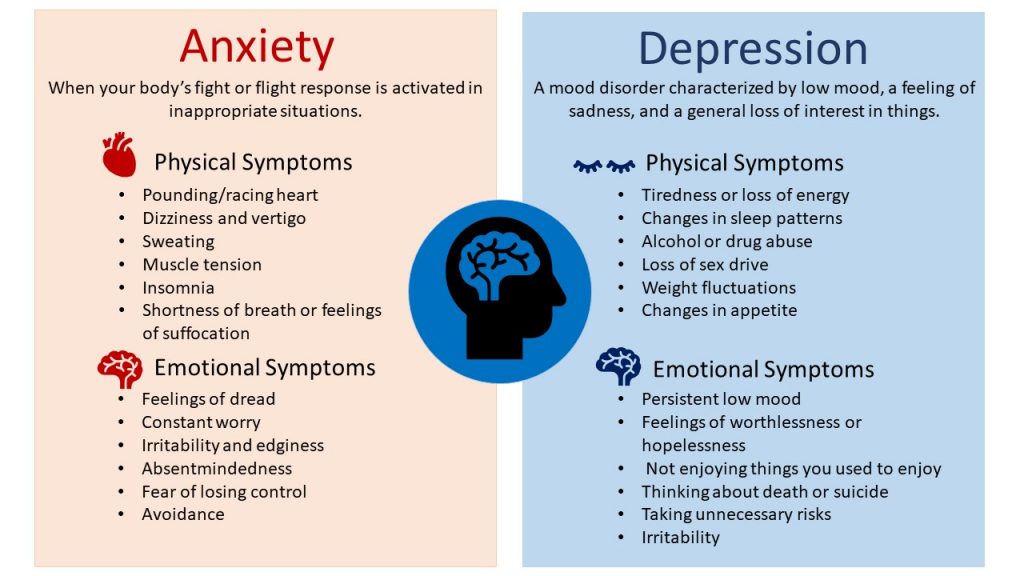 The percentage of people who were past month binge drinkers was highest among young adults aged 18 to 25 (29.2% or 9.8 million people), followed by adults aged 26 or older (22.4% or 49.3 million people), then by adolescents aged 12 to 17 (3.8% or 995,000 people). (2021 NSDUH)
The percentage of people who were past month binge drinkers was highest among young adults aged 18 to 25 (29.2% or 9.8 million people), followed by adults aged 26 or older (22.4% or 49.3 million people), then by adolescents aged 12 to 17 (3.8% or 995,000 people). (2021 NSDUH) - Among people aged 12 to 20 in 2021, 15.1% (or 5.9 million people) were past month alcohol users. Estimates of binge alcohol use and heavy alcohol use in the past month among underage people were 8.3% (or 3.2 million people) and 1.6% (or 613,000 people), respectively. (2021 NSDUH)
- In 2020, 50.0% of people aged 12 or older (or 138.5 million people) used alcohol in the past month (i.e., current alcohol users) (2020 NSDUH)
- Among the 138.5 million people who were current alcohol users, 61.6 million people (or 44.4%) were classified as binge drinkers and 17.7 million people (28.8% of current binge drinkers and 12.8% of current alcohol users) were classified as heavy drinkers (2020 NSDUH)
- The percentage of people who were past month binge alcohol users was highest among young adults aged 18 to 25 (31.
 4%) compared with 22.9% of adults aged 26 or older and 4.1% of adolescents aged 12 to 17 (2020 NSDUH)
4%) compared with 22.9% of adults aged 26 or older and 4.1% of adolescents aged 12 to 17 (2020 NSDUH) - Excessive alcohol use can increase a person’s risk of stroke, liver cirrhosis, alcoholic hepatitis, cancer, and other serious health conditions
- Excessive alcohol use can also lead to risk-taking behavior, including driving while impaired. The Centers for Disease Control and Prevention reports that 29 people in the United States die in motor vehicle crashes that involve an alcohol-impaired driver daily
Programs/Initiatives:
- STOP Underage Drinking interagency portal - Interagency Coordinating Committee on the Prevention of Underage Drinking
- Interagency Coordinating Committee on the Prevention of Underage Drinking
- Talk. They Hear You.
- Underage Drinking: Myths vs. Facts
- Talking with your College-Bound Young Adult About Alcohol
Relevant links:
- National Association of State Alcohol and Drug Abuse Directors
- Department of Transportation Office of Drug & Alcohol Policy & Compliance
- Alcohol Policy Information Systems Database (APIS)
- National Institute on Alcohol Abuse and Alcoholism
Tobacco
Data:
- In 2020, 20.
 7% of people aged 12 or older (or 57.3 million people) used nicotine products (i.e., used tobacco products or vaped nicotine) in the past month (2020 NSDUH)
7% of people aged 12 or older (or 57.3 million people) used nicotine products (i.e., used tobacco products or vaped nicotine) in the past month (2020 NSDUH) - Among past month users of nicotine products, nearly two thirds of adolescents aged 12 to 17 (63.1%) vaped nicotine but did not use tobacco products. In contrast, 88.9% of past month nicotine product users aged 26 or older used only tobacco products (2020 NSDUH)
- Tobacco use is the leading cause of preventable death, often leading to lung cancer, respiratory disorders, heart disease, stroke, and other serious illnesses. The CDC reports that cigarette smoking causes more than 480,000 deaths each year in the United States
- The CDC’s Office on Smoking and Health reports that more than 16 million Americans are living with a disease caused by smoking cigarettes
Electronic cigarette (e-cigarette) use data:
- In 2021, 13.2 million people aged 12 or older (or 4.7%) used an e-cigarette or other vaping device to vape nicotine in the past month.
 The percentage of people who vaped nicotine was highest among young adults aged 18 to 25 (14.1% or 4.7 million people), followed by adolescents aged 12 to 17 (5.2% or 1.4 million people), then by adults aged 26 or older (3.2% or 7.1 million people).
The percentage of people who vaped nicotine was highest among young adults aged 18 to 25 (14.1% or 4.7 million people), followed by adolescents aged 12 to 17 (5.2% or 1.4 million people), then by adults aged 26 or older (3.2% or 7.1 million people). - Among people aged 12 to 20 in 2021, 11.0% (or 4.3 million people) used tobacco products or used an e-cigarette or other vaping device to vape nicotine in the past month. Among people in this age group, 8.1% (or 3.1 million people) vaped nicotine, 5.4% (or 2.1 million people) used tobacco products, and 3.4% (or 1.3 million people) smoked cigarettes in the past month. (2021 NSDUH)
- Data from the Centers for Disease Control and Prevention’s 2020 National Youth Tobacco Survey. Among both middle and high school students, current use of e-cigarettes declined from 2019 to 2020, reversing previous trends and returning current e-cigarette use to levels similar to those observed in 2018
- E-cigarettes are not safe for youth, young adults, or pregnant women, especially because they contain nicotine and other chemicals
Resources:
- Tips for Teens: Tobacco
- Tips for Teens: E-cigarettes
- Implementing Tobacco Cessation Programs in Substance Use Disorder Treatment Settings
- Synar Amendment Program
Links:
- Truth Initiative
- FDA Center for Tobacco Products
- CDC Office on Smoking and Health
- National Institute on Drug Abuse: Tobacco, Nicotine, and E-Cigarettes
- National Institute on Drug Abuse: E-Cigarettes
Opioids
Data:
- Among people aged 12 or older in 2021, 3.
 3% (or 9.2 million people) misused opioids (heroin or prescription pain relievers) in the past year. Among the 9.2 million people who misused opioids in the past year, 8.7 million people misused prescription pain relievers compared with 1.1 million people who used heroin. These numbers include 574,000 people who both misused prescription pain relievers and used heroin in the past year. (2021 NSDUH)
3% (or 9.2 million people) misused opioids (heroin or prescription pain relievers) in the past year. Among the 9.2 million people who misused opioids in the past year, 8.7 million people misused prescription pain relievers compared with 1.1 million people who used heroin. These numbers include 574,000 people who both misused prescription pain relievers and used heroin in the past year. (2021 NSDUH) - Among people aged 12 or older in 2020, 3.4% (or 9.5 million people) misused opioids in the past year. Among the 9.5 million people who misused opioids in the past year, 9.3 million people misused prescription pain relievers and 902,000 people used heroin (2020 NSDUH)
- According to the Centers for Disease Control and Prevention’s Understanding the Epidemic, an average of 128 Americans die every day from an opioid overdose
Resources:
- Medication-Assisted Treatment
- Opioid Overdose Prevention Toolkit
- TIP 63: Medications for Opioid Use Disorder
- Use of Medication-Assisted Treatment for Opioid Use Disorder in Criminal Justice Settings
- Opioid Use Disorder and Pregnancy
- Clinical Guidance for Treating Pregnant and Parenting Women With Opioid Use Disorder and Their Infants
- The Facts about Buprenorphine for Treatment of Opioid Addiction
- Pregnancy Planning for Women Being Treated for Opioid Use Disorder
- Tips for Teens: Opioids
- Rural Opioid Technical Assistance Grants
- Tribal Opioid Response Grants
- Provider’s Clinical Support System - Medication Assisted Treatment Grant Program
Links:
- National Institute on Drug Abuse: Opioids
- National Institute on Drug Abuse: Heroin
- HHS Prevent Opioid Abuse
- Community Anti-Drug Coalitions of America
- Addiction Technology Transfer Center (ATTC) Network
- Prevention Technology Transfer Center (PTTC) Network
Marijuana
Data:
- In 2021, marijuana was the most commonly used illicit drug, with 18.
 7% of people aged 12 or older (or 52.5 million people) using it in the past year. The percentage was highest among young adults aged 18 to 25 (35.4% or 11.8 million people), followed by adults aged 26 or older (17.2% or 37.9 million people), then by adolescents aged 12 to 17 (10.5% or 2.7 million people).
7% of people aged 12 or older (or 52.5 million people) using it in the past year. The percentage was highest among young adults aged 18 to 25 (35.4% or 11.8 million people), followed by adults aged 26 or older (17.2% or 37.9 million people), then by adolescents aged 12 to 17 (10.5% or 2.7 million people). - The percentage of people who used marijuana in the past year was highest among young adults aged 18 to 25 (34.5%) compared with 16.3% of adults aged 26 or older and 10.1% of adolescents aged 12 to 17 (2020 NSDUH)
- Marijuana can impair judgment and distort perception in the short term and can lead to memory impairment in the long term
- Marijuana can have significant health effects on youth and pregnant women.
Resources:
- Know the Risks of Marijuana
- Marijuana and Pregnancy
- Tips for Teens: Marijuana
Relevant links:
- National Institute on Drug Abuse: Marijuana
- Addiction Technology Transfer Centers on Marijuana
- CDC Marijuana and Public Health
Emerging Trends in Substance Misuse:
- Methamphetamine—In 2019, NSDUH data show that approximately 2 million people used methamphetamine in the past year.
 Approximately 1 million people had a methamphetamine use disorder, which was higher than the percentage in 2016, but similar to the percentages in 2015 and 2018. The National Institute on Drug Abuse Data shows that overdose death rates involving methamphetamine have quadrupled from 2011 to 2017. Frequent meth use is associated with mood disturbances, hallucinations, and paranoia.
Approximately 1 million people had a methamphetamine use disorder, which was higher than the percentage in 2016, but similar to the percentages in 2015 and 2018. The National Institute on Drug Abuse Data shows that overdose death rates involving methamphetamine have quadrupled from 2011 to 2017. Frequent meth use is associated with mood disturbances, hallucinations, and paranoia. - Cocaine—In 2019, NSDUH data show an estimated 5.5 million people aged 12 or older were past users of cocaine, including about 778,000 users of crack. The CDC reports that overdose deaths involving have increased by one-third from 2016 to 2017. In the short term, cocaine use can result in increased blood pressure, restlessness, and irritability. In the long term, severe medical complications of cocaine use include heart attacks, seizures, and abdominal pain.
- Kratom—In 2019, NSDUH data show that about 825,000 people had used Kratom in the past month. Kratom is a tropical plant that grows naturally in Southeast Asia with leaves that can have psychotropic effects by affecting opioid brain receptors.
 It is currently unregulated and has risk of abuse and dependence. The National Institute on Drug Abuse reports that health effects of Kratom can include nausea, itching, seizures, and hallucinations.
It is currently unregulated and has risk of abuse and dependence. The National Institute on Drug Abuse reports that health effects of Kratom can include nausea, itching, seizures, and hallucinations.
Resources:
- Tips for Teens: Methamphetamine
- Tips for Teens: Cocaine
- National Institute on Drug Abuse
More SAMHSA publications on substance use prevention and treatment.
Last Updated: 01/05/2023
Official report: brutal psychiatric "treatment"
MAIN PAGE » PUBLICATIONS CCHR
Electroshock treatment, also known as electroconvulsive therapy (ECT), as well as psychosurgical "treatment measures", are reportedly gaining ground. From their inception until now, these procedures have been accompanied by conflict between psychiatrists who constantly recommend ECT and the many victims and their families whose lives have been completely destroyed by these procedures. nine0003
nine0003
So who is telling the truth? Anyone who has seen and felt sick while watching videos of ECT or psychosurgery knows the answer well. These procedures have all the hallmarks of physical torture befitting an NKVD (former Soviet Union's secret service) interrogator rather than a "medical worker." However, only a few people have seen such videos, including those who legislate for the mandatory use of such "treatments", and even fewer people have seen this procedure in reality. nine0003
Psychiatrists camouflage these procedures with medical practices: hospital environment, white-coated assistants, anesthetics, muscle relaxers, sophisticated equipment. The consequences of shock therapy are terrifying, but patients and their families are not fully warned about them. And what is even worse, when objections arise, they are rejected by the force of authority.
The fact that these procedures are extremely profitable for psychiatrists and their clinics, leading to a long and expensive "treatment" that guarantees the psychiatrist's future business and income, is not mentioned in conversations with those who do not suspect anything or do not want to be treated. nine0003
nine0003
According to Maria Garcia [name changed], if the belief that treatment is needed does not work, psychiatrists are willing to use coercion or intimidation to obtain "consent to treatment."
Maria, a middle-aged housewife, turned to a psychiatrist for advice after she felt that depression would not let her go. She was prescribed psychiatric drugs. When she began to experience uncontrolled body movements—a direct result of drug damage to her nervous system—the psychiatrist recommended ECT. She refused, but later, when she was admitted to the hospital for drug detoxification, ECT was recommended again. In response to her objections, the psychiatrist told her: “Your fears are just Cuban prejudices. You will die if you don't get this treatment." She underwent five sessions of electric shock. nine0003
Her husband recounts what happened: “After the ECT procedures, my wife's memory deteriorated greatly. Despite the fact that English was her second language for 42 years, she stopped speaking and understanding it.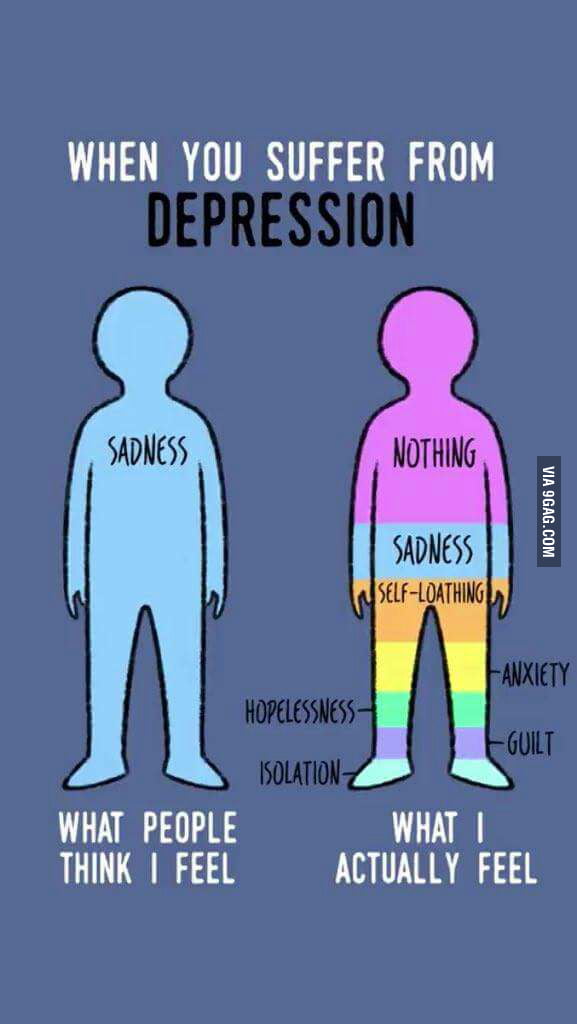 It was a complete scam. Her depression was not cured, and her memory became very bad ... we are both outraged by what happened. I feel like she was raped right in front of my eyes."
It was a complete scam. Her depression was not cured, and her memory became very bad ... we are both outraged by what happened. I feel like she was raped right in front of my eyes."
While ECT and psychosurgery generate billions of dollars in revenue, today there is a shocking amount of false information about them, much of which is spread by psychiatrists. Many scientists disapprove of these procedures. nine0003
John Friedberg, a neuroscientist who has studied the effects of ECT for more than 30 years, stated: “It is very difficult to articulate what exactly happens to people in general after shock treatment. It destroys their aspirations and ... desire to live. It makes people passive and lethargic. In addition to the loss of memory, apathy and loss of vitality are, in my opinion, the reasons why psychiatrists still get away with it.
Mary Lou Zimmerman knows what it's like to lose your drive and will to live in the hands of a psychiatrist. In June 2002, a jury ordered the Cleveland Clinic, Ohio, to pay a 62-year-old patient $7.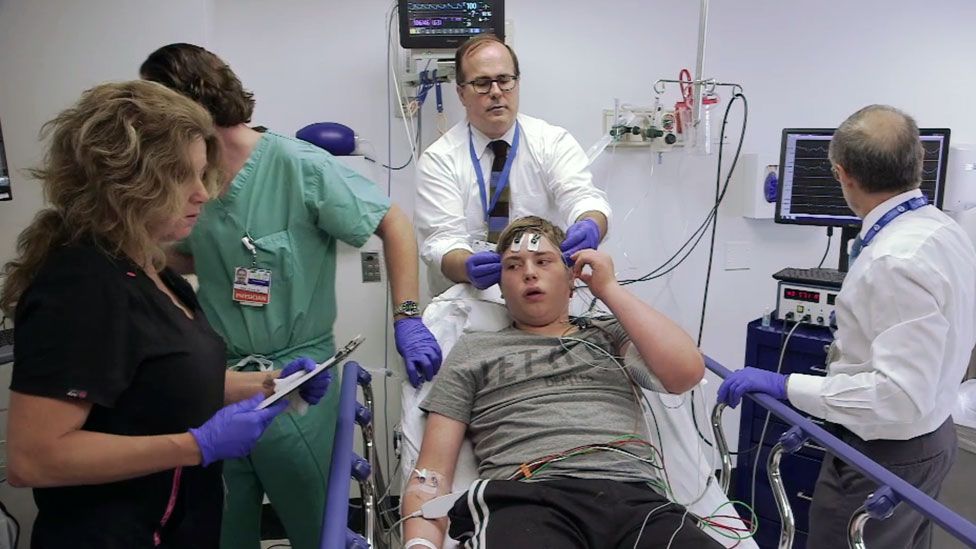 5 million after horrific brain surgery. Ms. Zimmerman came to the clinic about her obsessive handwashing habit after reading rave reviews about the operation on the clinic's website. However, in reality, the operation turned into a real nightmare. During this procedure, four holes were drilled into her skull, and cherry-sized sections of tissue were removed from her brain. As a result, she lost the ability to walk, stand, eat, and use the toilet on her own. Her lawyer, Robert Linton, stated: "She has lost everything - except for the understanding that she has changed ... She has become a complete invalid and needs constant care." nine0003
5 million after horrific brain surgery. Ms. Zimmerman came to the clinic about her obsessive handwashing habit after reading rave reviews about the operation on the clinic's website. However, in reality, the operation turned into a real nightmare. During this procedure, four holes were drilled into her skull, and cherry-sized sections of tissue were removed from her brain. As a result, she lost the ability to walk, stand, eat, and use the toilet on her own. Her lawyer, Robert Linton, stated: "She has lost everything - except for the understanding that she has changed ... She has become a complete invalid and needs constant care." nine0003
Today, the mental health industry in the United States alone is estimated to receive about $5 billion annually from ECT. 65-year-olds in the United States receive ECT treatments 365% more often than 64-year-olds because Medicare (the federal health insurance program) begins to work for people over 65 years old. This is evidence that the use of ECT is driven not by compassion on the part of the physician, but by profit and greed. Although psychosurgery is not as common today as it was in the past, up to 300 surgeries are still performed in the US each year, including the infamous prefrontal lobotomy. nine0003
Although psychosurgery is not as common today as it was in the past, up to 300 surgeries are still performed in the US each year, including the infamous prefrontal lobotomy. nine0003
Despite the intricate scientific intricacies, the brutality of ECT and psychiatric surgery confirms that psychiatry has not progressed beyond the cruelty and savagery of the original treatment measures. This report is written so that, like the whipping, bloodletting, and flogging of patients that are now outlawed, these "medical measures" should also be banned as a criminal offense against human health and prosecuted as such.
Sincerely,
Jan Eastgate
International CCHR President
Treatment of depression in women in St. Petersburg
- Home
- Psychotherapy
- Treatment of depression
- Depression in women
Depression in women is treated on an outpatient or inpatient basis at our clinic, depending on the complexity of the case. Mild forms of depression are removed with the help of psychotherapy sessions, without the use of medications. Protracted and severe depression require hospitalization and dynamic monitoring of health. nine0003
Outpatient medical treatment of depression in women with modern antidepressants with virtually no side effects, allows you to drive a car and carry out daily work.
Our psychiatrists and psychotherapists are doctors of the first and highest categories, candidates and doctors of sciences, with unique knowledge in the field of psychopharmacology. Our doctors will select an individual safe pharmacological treatment or, if the case allows, they will limit themselves to prescribing psychotherapy and supportive drug therapy. nine0003
Our doctors will select an individual safe pharmacological treatment or, if the case allows, they will limit themselves to prescribing psychotherapy and supportive drug therapy. nine0003
We take on even complex cases of drug resistance and cases where drug therapy is contraindicated (pregnancy, advanced age, etc.) with modified and innovative treatments:
- ECT;
- hemosorption;
- plasmapheresis;
- UV blood.
After discharge, our doctors accompany patients - consult and adjust maintenance therapy. An important role is also played by the help from relatives who are recommended to undergo training in behavior with a relative during the rehabilitation period. The knowledge that the doctor will give will help to better understand the nature of the disease and not provoke a relapse of a mental disorder. nine0003
Quiz: Beck Depression Scale
In each group, identify the one statement that best fits how you felt this week and today.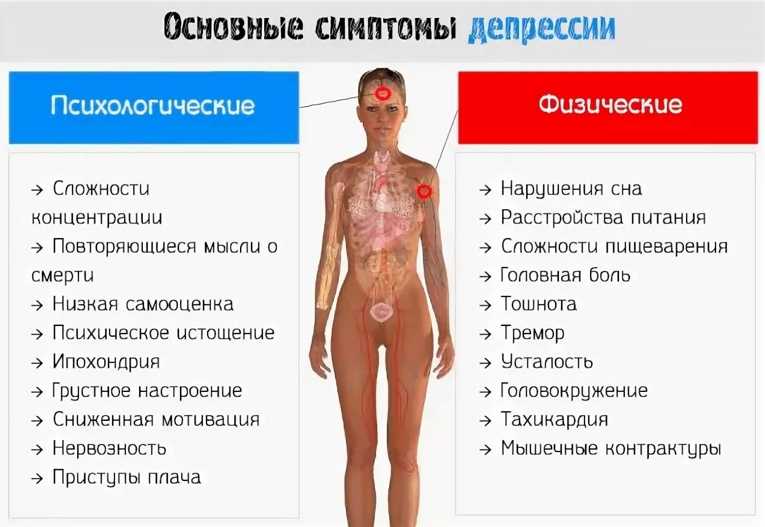 Before making your choice, make sure you read all of the statements in each group.
Before making your choice, make sure you read all of the statements in each group.
Doctor's consultation on the treatment of depression in women:
+7 (812) 407-18-00
Thank you for your trust!
- Outpatient and inpatient care nine0057 Expert level psychopharmacologists
- Post-discharge management
| Service | Price | |
|---|---|---|
| Psychotherapist appointment nine0099 | 5 000 ₽ | |
| Family Therapy | 10 000 ₽ | |
| Hypnotherapy | 8 000 ₽ | nine0095|
| Psychiatric consultation | 5 000 ₽ |
Reasons for the development of depression in women
Quarrels, parting with a loved one, dismissal from work and other life crises are triggers for the development of depression in women. Also, the development of a depressive state in women is influenced by a variety of biological factors, for example: hormonal fluctuations during puberty, the onset of the menstrual cycle, the onset of sexual activity, the first pregnancy and childbirth, as well as menopause and menopause. nine0003
Also, the development of a depressive state in women is influenced by a variety of biological factors, for example: hormonal fluctuations during puberty, the onset of the menstrual cycle, the onset of sexual activity, the first pregnancy and childbirth, as well as menopause and menopause. nine0003
| Genetics | The risk of developing severe depression increases if any of the female relatives suffered from depression. |
|---|---|
| Biochemistry | Clinical (“major”) depression may result from the side effects of drugs (eg, corticosteroids, benzodiazepines) or may arise from the abuse of alcohol, psychostimulants, hypnotics, etc. |
| Social environment | Clinical (“major”) depression may result from the side effects of drugs (eg, corticosteroids, benzodiazepines) or may arise from the abuse of alcohol, psychostimulants, hypnotics, etc. |
| Personal characteristics | Against the background of emotional outbursts, subject to their frequent repetitions, a stressful state inevitably arises, which can cause the development of depression. |
| Hormones | Puberty and growing up is a dangerous time in terms of the risk of developing depression. |
| Childbirth | About 15% of all women in labor suffer from postpartum depression. Mental disorder is dangerous with psychotic attacks, in which a young mother can harm a child. |
| Old age | Senile depression is a common mental disorder among older people caused by organic changes in the brain. Against the background of loneliness and various diseases, women in old age easily fall into a severe form of depression. nine0099 |
Symptoms of depression in women
Treatment of depression in women in our clinic
Many people are afraid of psychiatrists. But modern psychiatry has little to do with the eerie pictures that overly emotional cinema paints. In addition, if you seek help in advance, treatment of depression in women may be limited to working with a psychotherapist, without the use of pharmacotherapy. nine0003
nine0003
Severe cases of depression are treated in a hospital. Our experts in the field of psychopharmacology will select the necessary drugs and, through dynamic monitoring of the state of health, adjust the drug treatment. In addition, we prefer monotherapy, which avoids intoxication and side effects from pharmacotherapy.
The underlying problems that caused the development of depression must be worked out during psychotherapy sessions - this approach to the treatment of depression in women allows not only to get rid of the symptoms of the disease, but also to prevent relapses. nine0003
Our doctors prescribe only modern certified drugs with minimal side effects:
| Antidepressants | Normalize the balance of neurotransmitters and eliminate depression. Modern antidepressants have a selective principle of action and do not cause lethargy (you can drive a car and do full mental or physical work). |
|---|---|
| Nootropics | Increase the effectiveness of antidepressant treatment, restore the depleted nervous system. |