Bipolar disorder for dummies book
Bipolar Disorder For Dummies, 3rd Edition
Selected type: E-Book
$14.00
Candida Fink, Joe Kraynak
ISBN: 978-1-119-12187-9 October 2015 416 Pages
-
E-Book
Starting at just $14.00
-
Print
Starting at just $22.99
E-Book
$14.00
Paperback
$22.99
Download Product Flyer
Download Product Flyer
Download Product Flyer is to download PDF in new tab. This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description.
This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description. Download Product Flyer is to download PDF in new tab. This is a dummy description.
Description
Understand the realities of bipolar disorder
When one receives the diagnosis that they or a loved one has bipolar disorder, it can be a time of fear and worry. Bipolar Disorder For Dummies, 3rd Edition explains the brain chemistry behind the disease and covers the latest medications and therapies. You'll get reassuring, sound advice and self-help techniques that you and your loved ones, including kids and teens, can use to ease and eliminate symptoms, function in times of crisis, plan ahead for manic or depressive episodes, and feel a whole lot better. This new edition will include new and updated content on genetics, biochemistry, and imaging studies relevant to bipolar, expanded coverage on how to handle the high costs of treatment, and supporting a loved one (who may not want help, medications and treatment options, including DSM-5, ECT, and TMS along with new coverage on special populations (how bipolar affects different groups, like women and various ethnic groups and special populations, like seniors and expectant moms.
Bipolar disorder, which has also been called manic-depressive illness, is a brain disorder that causes unusual mood swings and shifting energy levels. The symptoms of bipolar disorder can, if not understood and handled properly, wreak havoc on personal and professional relationships. Though bipolar disorder is a serious condition, it's one that can be treated! With a firm understanding of what you're dealing with, you can navigate your way through the challenges of bipolar disorder, whether you or a loved one suffers from this illness.
- Recognize the warning signs of mania and depression, which may point to bipolar disorder
- Understand where to find the latest treatment options
- Stay on track with personal and professional aspects of life
- Effectively and compassionately respond to rants, depression, mania, and other behaviors associated with bipolar disorder
Bipolar Disorder For Dummies, 3rd Edition offers straightforward, reassuring information about bipolar disorder to help you or your loved one conquer the disease.
About the Author
Candida Fink, M.D. is a board-certified psychiatrist specializing in the diagnosis and treatment of bipolar disorder. Joe Kraynak is a professional writer/editor of many Dummies books and deals with bipolar in his family. Since publication of the first edition, the authors’ platform has grown: their Bipolar Blog has become a gathering place where visitors share their bipolar stories and support others; their blog on Psych Central averages thousands of visitors daily; and Dr. Fink regularly provides expert opinion on such news outlets as FoxNews.com and the Boston Globe.
Permissions
Request permission to reuse content from this site
Table of contents
Introduction 1
Part I: Getting Started on Your Bipolar Journey 5
Chapter 1: Grasping Bipolar Disorder: Symptoms and Diagnosis 7
Chapter 2: Finding the Cause: The Brain and Body Science of Bipolar Disorder 29
Chapter 3: Reining in Bipolar Disorder: Prognosis and Treatments 47
Part II: Obtaining a Diagnosis and Building a Treatment Plan and Team 61
Chapter 4: Diagnosis Step 1: Ruling Out Other Health Issues 63
Chapter 5: Diagnosis Step 2: Obtaining a Psychiatric Evaluation and Treatment Plan 75
Chapter 6: Building a Winning Mood-Management Team 93
Part III: Managing the Biology of Bipolar Disorder 107
Chapter 7: Leveling Moods with Medication 109
Chapter 8: Coming to Terms with Medications and Their Side Effects 141
Chapter 9: Expanding Your Biological Treatment Options 159
Chapter 10: Treating Bipolar Disorder in Women and Other Specific Populations 171
Part IV: Developing Essential Survival Skills 185
Chapter 11: Exploring Self-Help Strategies, Therapies, and Other Supports 187
Chapter 12: Making Lifestyle Adjustments 201
Chapter 13: Communicating Effectively 221
Chapter 14: Solving Problems and Resolving Conflict 233
Chapter 15: Planning Ahead for a Mood Episode 243
Part V: Dealing with the Fallout 253
Chapter 16: From Hospitalization to Recovery 255
Chapter 17: Returning to Work . . . or Not 269
. . or Not 269
Chapter 18: Overcoming Financial Setbacks 281
Part VI: Assisting a Friend or Relative with Bipolar Disorder 295
Chapter 19: Supporting Your Loved One 297
Chapter 20: Dealing with Crisis Situations 311
Chapter 21: Backing Your Bipolar Child or Teen 327
Part VII: The Part of Tens 353
Chapter 22: Ten Tips for Managing Bipolar 355
Chapter 23: Ten Ways to Help a Loved One with Bipolar Disorder 361
Index 367
Bipolar Disorder For Dummies by Candida Fink, Joe Kraynak - Ebook
Part I
Getting to Know Bipolar Disorder9781118338827-pp0101.eps
In this part . . .
In Part I, we provide a crash course in bipolar disorder. Here, you discover the similarities and differences among the different types of bipolar, including bipolar I, bipolar II, and cyclothymic disorder. You get to know the official signs and symptoms of depression, hypomania, and mania, and you discover how to distinguish between a bad day at work and a bona fide mood episode. You also find out where bipolar disorder comes from, what triggers it, and how likely or unlikely it is that you have it.
You also find out where bipolar disorder comes from, what triggers it, and how likely or unlikely it is that you have it.
To round out the part, we unveil the positive prognosis that accompanies the bipolar diagnosis and the various components that comprise an effective treatment plan — both medication and non-medication treatments that have proven to be effective to varying degrees.
Chapter 1 Understanding Bipolar Disorder: Diagnosis to Recovery In This Chapterarrow Navigating the wild mood episodes of bipolar disorder
arrow Receiving your official diagnosis and dealing with it
arrow Managing bipolar disorder your own way
arrow Supporting a loved one with bipolar disorder
arrow Considering a diagnosis of bipolar in children and adolescents
Bipolar disorder (sometimes referred to as manic depression) is characterized by episodes of mood and energy changes that range from high to low and are extreme enough to interfere with a person’s ability to function. At its best, bipolar disorder inspires brilliant insights and uninhibited joy. At its worst, it drapes the mind in debilitating depression, destroys relationships, empties bank accounts, and fuels suicidal thoughts. Doctors have no test for bipolar disorder and no cure, and many people experience symptoms for years before they receive a diagnosis. In fact, one of the main symptoms of bipolar is that the afflicted often deny they have it and resist treatment.
At its best, bipolar disorder inspires brilliant insights and uninhibited joy. At its worst, it drapes the mind in debilitating depression, destroys relationships, empties bank accounts, and fuels suicidal thoughts. Doctors have no test for bipolar disorder and no cure, and many people experience symptoms for years before they receive a diagnosis. In fact, one of the main symptoms of bipolar is that the afflicted often deny they have it and resist treatment.
Science knows few more elusive illnesses, yet mental health professionals are more skilled than ever at accurately diagnosing bipolar disorder and treating it with the right combination of medicine, therapy, and life changes. Many people with bipolar disorder can now live productive lives and achieve levels of happiness and fulfillment they never dreamed possible.
In this chapter, we reveal a few of the many manifestations of bipolar disorder and describe its most challenging aspects. We lead you on a brief journey through what a person with bipolar disorder can expect — from diagnosis through prognosis and on to treatment and recovery. And because successful treatment and recovery often involve the participation of loved ones, this chapter also shows you what you can do to support a friend, relative, or child who has bipolar disorder. Just keep in mind that recovery in this context doesn’t mean
And because successful treatment and recovery often involve the participation of loved ones, this chapter also shows you what you can do to support a friend, relative, or child who has bipolar disorder. Just keep in mind that recovery in this context doesn’t mean cure
but rather a way to manage the disorder so everyone involved can get back to living life.
Riding the Bipolar Waves
Some people are so persistently perky that you just want to slap them. Most others experience the normal ups and downs of life. When a person loses her job, she’s likely to feel dejected. Someone who just won the lottery probably feels ecstatic. Fluctuations in mood — even extreme feelings in response to major life events — are normal, as long as they don’t last too long or interfere with the ability to function and resume pre-event behavior patterns. A temporary bout of unhappiness can actually prompt a healthy person to make positive changes that lead to greater happiness and self-fulfillment.
remember.eps However, bipolar disorder causes extreme and lasting moods. If you suffer from bipolar disorder, you too experience the normal ups and downs of everyday living, but sometimes the ups and downs exceed healthy, adaptive limits and persist for inordinate amounts of time.
Seeking your elusive comfort levelMost people experience mood variations to some acceptable degree, but bipolar mood episodes are amplified and extend way beyond comfortable levels — to the point of impairing a person’s ability to function and enjoy life. Episodes associated with bipolar disorder make a person think, feel, speak, and behave in ways that are extremely uncharacteristic of the individual. Figure 1-1 illustrates how bipolar moods fluctuate outside the normal range.
Of course, intensity of mood alone, especially when it’s on the rise, isn’t always problematic. In fact, many people who experience hypomania — an elevated state of mood and energy — report that their creative drives and clarity of vision are quite exhilarating. Hypomania can often make you more extroverted, entertaining, and engaging. It can increase your sex drive, make you feel more powerful, energize and invigorate you, help you focus, and inspire creativity. To qualify as hypomania, the episode must last at least four days.
Hypomania can often make you more extroverted, entertaining, and engaging. It can increase your sex drive, make you feel more powerful, energize and invigorate you, help you focus, and inspire creativity. To qualify as hypomania, the episode must last at least four days.
Mania, on the other hand, is more severe both in intensity and duration (at least one week) and impairs your ability to function or requires hospitalization. Mania may also be accompanied by psychoses, while hypomania is not. (See Chapter 2 for more about the distinction between mania and hypomania.)
Figure 1-1: Normal mood variation versus bipolar mood episodes.
9781118338827-fg0101.eps
Illustration by Wiley, Composition Services Graphics
Some people with bipolar disorder experience symptoms of depression and mania at the same time. In these episodes with mixed features, people can feel depressed or hopeless while also feeling hyped up, irritable, and agitated.
remember.eps The trick to treating bipolar disorder isn’t to flat-line your moods and energy. The goal is to enable your brain to function as it does when it’s well so you don’t experience the extreme variations that characterize mood episodes.
Crashing on the rocksWith bipolar disorder, your mood fluctuates way beyond normal. A deep depression can wrap you in despair and sentence you to endless days in bed. A full-blown manic episode can buck you like a raging bull and then toss your exhausted carcass. Whether you soar high or plummet down, an extreme, prolonged mood episode can be devastating to your relationships, career, and other aspects of your life.
remember.eps Whether you crash via a wave of mania or get swept away by the undercurrents of depression, your doctor is likely to order medication, therapy, or a brief stay in the hospital (in extreme cases) as a first step toward recovery. However, the preferred method of living with bipolar disorder is to avoid the crash altogether by obtaining an accurate diagnosis and receiving preventive treatment and therapy.
Manic episodes seem to garner all the press because their stories are often titillating. In episodes of mania, people often rise above the monotony of the moment, pumped up with the following feelings and beliefs:
check.png I am amazing!
check.png Everything is wonderful!
check.png I can do anything and everything, and I will do it right now!
check.png I have all the answers! My ideas will change the world!
check.png No matter what bad things I do, I’m still a great person!
check.png Sleep is only for people who have nothing better to do!
check.png I’m always right!
check.png Everybody loves me!
check.png I’m the fastest at everything I do!
Full-blown manic episodes impair one’s ability to function, may be accompanied by paranoia and other psychoses, and usually require medical intervention. For example, a person may become consumed with thoughts of religious martyrdom or government plots. She may believe that family members, friends, or even strangers have ill or dangerous intentions against her. Angry and/or aggressive thoughts, moods, and behaviors can become major parts of the picture. Left to run its course, mania often results in a crash, leaving the individual feeling depressed and physically and mentally exhausted. The episode can also ruin personal and professional relationships and lead to serious financial and legal trouble.
She may believe that family members, friends, or even strangers have ill or dangerous intentions against her. Angry and/or aggressive thoughts, moods, and behaviors can become major parts of the picture. Left to run its course, mania often results in a crash, leaving the individual feeling depressed and physically and mentally exhausted. The episode can also ruin personal and professional relationships and lead to serious financial and legal trouble.
Depression is the opposite of thrilling. It can make you feel like you’re trudging through the quagmire of life in a lead suit. It dulls your senses and bars you from experiencing any of life’s pleasures. You become the resident party pooper, the proverbial wet blanket. If you had the energy to talk, you’d likely express your feelings as follows:
check.png I’m terrible.
check.png Everything is horrible.
check.png I can’t do anything.
check.png I’m a bad, evil person even when I don’t do anything bad.
check.png I can’t sleep.
check.png I can’t get out of bed.
check.png Even little things take forever to do.
check.png Nobody loves me.
check.png Everything’s my fault.
check.png Nothing feels good.
If you’re lucky, the depression eventually lifts like the morning fog. But if it deepens, it can lead to a crash, leaving you feeling even more depressed and physically and mentally exhausted. Self-harm or suicidal thoughts and behaviors can become dangerous parts of this story.
warning_bomb.eps When most people think of bipolar disorder, they think of the manic side. However, depression is the more common and more damaging of the two poles and is often the more difficult to treat.
Earning Your Bipolar Badge
To begin the process of treating and regulating bipolar disorder, you need an official diagnosis, and obtaining it can be quite a lengthy process.
Deciding to get helpThe first step toward getting a bipolar disorder diagnosis is to realize that something isn’t right. Awareness is usually the most time-consuming step. Most people with bipolar disorder live with it for an average of ten years before seeking help and receiving a correct diagnosis. Bipolar disorder is often misdiagnosed as depression, and people can receive incomplete or ineffective treatment for many years.
Awareness is usually the most time-consuming step. Most people with bipolar disorder live with it for an average of ten years before seeking help and receiving a correct diagnosis. Bipolar disorder is often misdiagnosed as depression, and people can receive incomplete or ineffective treatment for many years.
People with bipolar disorder may avoid seeking treatment for any number of reasons, including the following:
check.png Mania feels great. I’ve never felt so energized!
check.png Why bother? Nothing can possibly make me feel any better.
check.png I’m not ill. I’m just weak. I need to work harder at overcoming this.
check.png I can deal with this on my own.
check.png I can’t afford any more bills.
check.png I don’t want to be labeled.
remember.eps Both depression and mania can influence thought patterns that make a person avoid treatment. In a manic episode, you commonly feel all-knowing, all-powerful, full of energy, and at the top of your game. In such a state, few people think they need help. When you feel deeply depressed, you commonly lose hope in the future and begin thinking that nothing can improve your life, so seeking help may seem pointless. In many cases, a deep crash or a loved one’s intervention provides the motivation you need to seek professional help.
In such a state, few people think they need help. When you feel deeply depressed, you commonly lose hope in the future and begin thinking that nothing can improve your life, so seeking help may seem pointless. In many cases, a deep crash or a loved one’s intervention provides the motivation you need to seek professional help.
After you decide that you need professional help, you can begin the process of obtaining an accurate diagnosis. This process typically entails the following steps:
1. Visit your physician.
Some other health issue, such as thyroid malfunction, menopause, or a nutritional deficiency, can cause symptoms similar to those of bipolar disorder. Medications and other substances can also produce similar symptoms. Your family physician can help rule out these and other possible causes of your symptoms. (Flip to Chapter 4 for more on health problems with symptoms that are similar to those of bipolar disorder. )
)
2. Undergo a psychiatric evaluation.
A licensed psychiatrist can review your medical history, family history, and symptoms and offer an initial diagnosis and treatment plan. (See Chapter 5 for more on visiting a psychiatrist.) In some cases, a primary-care physician delivers the diagnosis and treatment.
warning_bomb.eps Unfortunately, the steps for obtaining an accurate diagnosis and a treatment plan that works aren’t always as linear as these steps make them seem. If you’re feeling deeply depressed, manic, or agitated, your physician or psychiatrist may prescribe medication to alleviate the symptoms immediately and work on refining the diagnosis later.
If you receive a diagnosis of bipolar disorder, your doctor typically narrows the diagnosis by specifying one of the following types of bipolar (see Chapter 2 for more details):
check.png Bipolar I: This diagnosis requires at least one full-blown manic episode that doctors can’t attribute to the direct physiological effects of another cause, such as a medication or substance abuse. If the manic episode is triggered by a substance or medicine but then persists well after the trigger is eliminated, a diagnosis of bipolar I is appropriate. Individuals often have one or more major depressive episodes as well, but depression isn’t required for a diagnosis of bipolar I.
If the manic episode is triggered by a substance or medicine but then persists well after the trigger is eliminated, a diagnosis of bipolar I is appropriate. Individuals often have one or more major depressive episodes as well, but depression isn’t required for a diagnosis of bipolar I.
check.png Bipolar II: People with bipolar II have had at least one major depressive episode and a hypomanic episode sometime during their life that doctors can’t attribute to the direct physiological effects of another cause such as medication. A diagnosis of bipolar II is not given if the person has ever had a full-blown manic episode. (Refer to the earlier section Seeking your elusive comfort level
for an explanation of the difference.)
check.png Cyclothymic disorder: This diagnosis requires multiple depressive and hypomanic episodes that aren’t extreme enough to warrant a diagnosis of bipolar I or II. This condition is chronic, so someone who’s been mood-symptom-free for more than two months in the past two years doesn’t qualify as having cyclothymic disorder.
check.png Substance-induced bipolar disorder or bipolar disorder associated with another medical condition: These types of bipolar disorder are diagnosed if a full manic episode is related to intoxication or withdrawal from drugs or alcohol or due to a physical illness such as thyroid disorder, dementia, or brain injury. As we explain in Chapter 4, a medical work-up is necessary to determine whether such conditions are the causes of the bipolar symptoms.
check.png Bipolar disorder not elsewhere classified (NES): This diagnosis describes bipolar symptoms that don’t fit into the major categories listed in the preceding bullets. The diagnosis is used in the following situations:
• The symptoms are too short in duration to meet the criteria for bipolar I or II.
• The symptoms aren’t numerous enough to meet the criteria for bipolar I or II.
• Insufficient information is available to make a diagnosis.
This diagnosis is similar to bipolar not otherwise specified (NOS) in DSM-IV. (DSM, which is short for Diagnostic and Statistical Manual of Mental Disorders, is published by the American Psychiatric Association in conjunction with many other professional, scientific, mental health, consumer, and provider groups. The manual describes criteria that doctors use to diagnose various mental illnesses, including bipolar disorder. Turn to Chapter 2 for more info.)
(DSM, which is short for Diagnostic and Statistical Manual of Mental Disorders, is published by the American Psychiatric Association in conjunction with many other professional, scientific, mental health, consumer, and provider groups. The manual describes criteria that doctors use to diagnose various mental illnesses, including bipolar disorder. Turn to Chapter 2 for more info.)
If you’re like most people, you shun labels — especially labels that carry negative connotations, such as bipolar. Used in a sentence, such as Pat is bipolar,
the label seems even more insensitive. It not only stigmatizes Pat but also reduces her to the illness itself. If Pat had cancer, nobody would say, Pat is cancer.
Yet people often play fast and loose with the term bipolar.
Your doctor doesn’t use the label bipolar disorder to label you or minimize your worth as a human being. The label provides a convenient way to refer to your condition, which requires treatment. It helps all the people involved in your treatment plan to quickly recognize the illness that afflicts you and to provide the appropriate medications and therapy. You are not bipolar disorder. Bipolar disorder is an illness you have, and you can manage it with the right treatments.
The label provides a convenient way to refer to your condition, which requires treatment. It helps all the people involved in your treatment plan to quickly recognize the illness that afflicts you and to provide the appropriate medications and therapy. You are not bipolar disorder. Bipolar disorder is an illness you have, and you can manage it with the right treatments.
Treating Bipolar Disorder Inside and Out
Treating bipolar disorder is usually best accomplished through a two-pronged approach that treats it inside and out. Medication and other biological treatments target the brain cells at the cellular level with the goal of returning normal brain function. But medication, even if effective, is rarely sufficient by itself. Sustained and robust management of this illness typically requires medication along with a focus on treating bipolar from the outside in — that is, targeting the brain and body at the level of function in addition to implementing self-help strategies and a range of therapies and supports, as we explain in the following sections.
Bipolar disorder is a physical illness that’s rooted in the biology of the brain (see Chapter 2), so it typically responds best to biological treatments that target the brain, including the following:
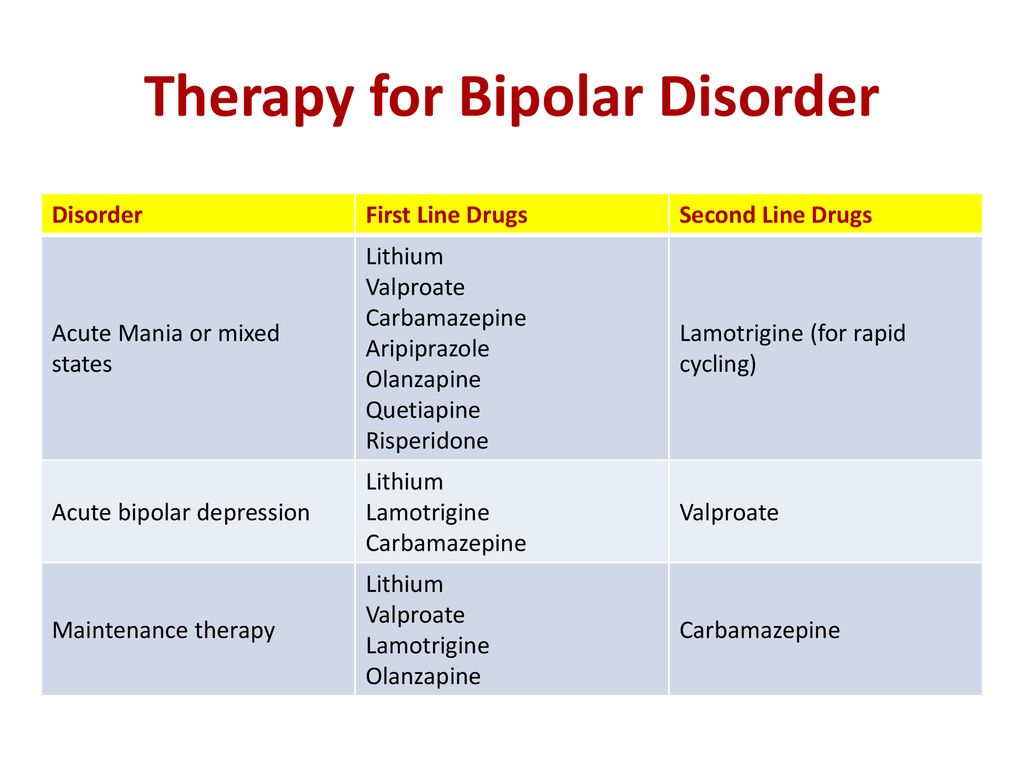
check.png Medication: Medication is usually the first line of treatment and consists of several different options for treating mania, depression, and accompanying symptoms, including anxiety and the inability to sleep. (For more about medications, see Chapter 7.)
remember.eps Doctors use medication to treat acute (severe) short-term symptoms and as a prophylaxis (preventive) to avoid further cycles. The medications your doctor prescribes will vary depending on your symptoms and past responses and reactions to medications.
check.png Vitamins and supplements: Omega-3 fatty acids may be useful in treating bipolar depression or mania. Other supplements, including folic acid, and N-acetylcysteine (NAC) are sometimes used, but there’s no clear evidence for their effectiveness.
warning_bomb.eps Proceed with caution when considering alternative treatments, including all-natural or herbal products. Having too much of a substance in your body can be as bad as or worse than having too little. In addition, some nutritional supplements can interact with prescribed medications, so make sure your doctor is aware of any supplements you’re using. Also, keep in mind that some natural remedies carry the same risks as pharmaceutical products, yet many of these products aren’t regulated by government-oversight agencies.
check.png Brain stimulation: Various methods of manipulating the inner workings of the brain by external means show promise in treating certain bipolar symptoms, especially depression that hasn’t responded to medication or therapy. Brain stimulation includes light therapy, electroconvulsive therapy (ECT), repetitive transcranial magnetic stimulation (rTMS), and deep brain stimulation (DBS).
For more about medication and other biological treatments, check out Part III.
Although bipolar disorder is a physical illness that affects the brain, referring to its cause as a chemical imbalance
is misleading. In many cases, restoring brain function through biological treatments isn’t enough to treat bipolar disorder because the brain is affected by much more than its inner workings, including how much sleep you get, what you eat and drink, how you interact with other people, how well you deal with stressful situations, and so on.
remember.eps Nature is nurture. Your experiences influence your brain as much as your brain influences your thoughts, words, and behaviors. And both your brain and your experiences affect your moods.
A robust recovery usually calls for medication along with the following self-help strategies, therapies, and other supports (see Chapter 11):
check.png Self-help: Self-help strategies consist of whatever you can do to make yourself feel better, and they often cost nothing but your time and effort. One of the most important self-help activities is monitoring your moods so you can respond to mood episodes early, before they get out of control. Another is identifying and trying to limit exposure to anything that causes you stress or tends to trigger an episode. Eating right, exercising, establishing healthy relationships, and engaging in other activities to support your overall health also help.
One of the most important self-help activities is monitoring your moods so you can respond to mood episodes early, before they get out of control. Another is identifying and trying to limit exposure to anything that causes you stress or tends to trigger an episode. Eating right, exercising, establishing healthy relationships, and engaging in other activities to support your overall health also help.
check.png Therapies: Certain therapies, including cognitive behavioral therapy (CBT), interpersonal and social rhythm therapy (IPSRT), marriage counseling or relationship therapy, and family therapy are common approaches to managing mood cycles and symptoms. CBT is well supported as being effective for depression and anxiety, but its effects on mania and bipolar disorder overall are still being evaluated. Working with a therapist is usually best, but if you don’t have access to a therapist for whatever reason, you can read up on these therapies and apply some of the strategies and principles in a self-help model.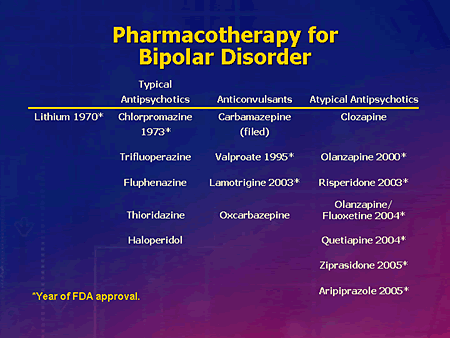
check.png Other supports: As with most things in life, the more support you have, the better. You may want to start building a support structure with your inner circle. Family members and friends can become the pillars by learning more about bipolar disorder, developing a sense of empathy, and teaming up with you to overcome the many challenges you face. Other supports may include local support groups, your community mental health center (CMHC), the Social Security Administration, free medication programs, your community, and your coworkers.
Reclaiming Your Life: Recovery
Experiencing a major manic or depressive episode is like getting T-boned by a freight train . . . but often without the physical evidence. If you could turn yourself inside out, though, you’d see your bruised and battered self and maybe garner a little well-deserved sympathy. Unfortunately, others may perceive you as a person who’s perfectly capable of returning to your home and job. To compound the problem, a major mood episode often leaves behind substantial collateral damage. Your loved ones may feel angry or alienated. Your boss may consider you a liability. And you may still be wrestling with the side effects of the most recent medication adjustment.
To compound the problem, a major mood episode often leaves behind substantial collateral damage. Your loved ones may feel angry or alienated. Your boss may consider you a liability. And you may still be wrestling with the side effects of the most recent medication adjustment.
At this point, you may feel that you have a responsibility as a loyal employee or family member to patch yourself up and return to service. And if that’s what you really want to do, it may be best for you. In most cases, however, taking some time off work to recuperate, allow your moods to stabilize, and pay attention to your emotional and psychological needs can lead to recovery with a much better long-term prognosis. To make your convalescence as successful as possible, consider the following tips and techniques:
check.png Find alternate living arrangements, if necessary. If you live alone or in a stressful environment, consider moving in with a close friend or relative until your moods and medications stabilize. A strong support person can help you monitor your moods, remind you to take your medications, and offer moral support.
A strong support person can help you monitor your moods, remind you to take your medications, and offer moral support.
check.png Take advantage of your job benefits. Contact your company’s human-resources department to find out if you’re eligible for a leave of absence during your recovery if your doctor prescribes it. Also be sure to check your health benefits. Don’t quit your job, even if you think it contributes to your illness. Get the benefits you deserve. Work the system. If you still feel like quitting, you can make that decision later, when you’re thinking more clearly.
check.png Enroll in intensive outpatient therapy. Many hospitals and clinics offer intensive outpatient therapy that can help you deal with the issues in your life while you recover physically from the trauma. If you take a leave of absence from work, intensive outpatient therapy keeps you busy during the day and provides all-important human contact.
Some people may consider this advice unrealistic. You have to work to earn enough money to survive and possibly support your family, right? So how can you possibly afford to take time off to recover? Well, the fact is that major mood episodes are extremely debilitating. Taking time to fully recuperate is an essential part of avoiding a series of incapacitating, demoralizing relapses. Ultimately, your financial health requires your medical recovery. So think of the situation like this: If you had a different health condition that prevented your return to work and family responsibilities, would you fret over making the choice to heal?
You have to work to earn enough money to survive and possibly support your family, right? So how can you possibly afford to take time off to recover? Well, the fact is that major mood episodes are extremely debilitating. Taking time to fully recuperate is an essential part of avoiding a series of incapacitating, demoralizing relapses. Ultimately, your financial health requires your medical recovery. So think of the situation like this: If you had a different health condition that prevented your return to work and family responsibilities, would you fret over making the choice to heal?
tip.eps Avoid making any major decisions during your convalescence, such as quitting your job or breaking off a relationship. Focus on becoming healthy. You can deal more effectively with your issues when you feel fully recovered.
remember.eps As we mention at the beginning of this chapter, recovery doesn’t mean cure
or necessarily a return to the way your life was before bipolar entered the picture.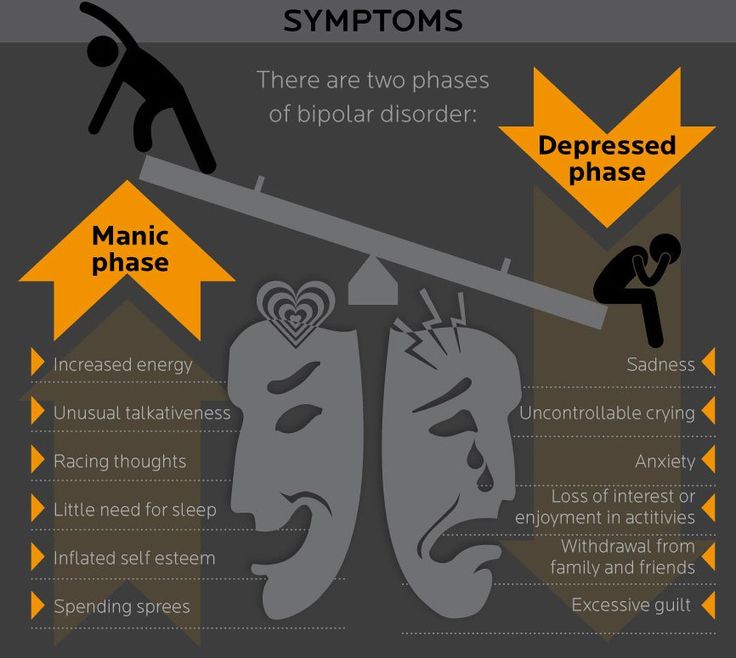 Recovering from a bipolar mood episode refers to finding a way to manage the illness. For some people, this sparks what becomes a rebirth to a new life. You may lose certain abilities you once had, gain knowledge and skills in other areas, and transition to a new career that you find just as or more rewarding than what you lost. Recovery is individual and personal.
Recovering from a bipolar mood episode refers to finding a way to manage the illness. For some people, this sparks what becomes a rebirth to a new life. You may lose certain abilities you once had, gain knowledge and skills in other areas, and transition to a new career that you find just as or more rewarding than what you lost. Recovery is individual and personal.
Supporting a Friend or Relative with Bipolar Disorder
Bipolar disorder can make or break a relationship. No question: The illness causes suffering, but it can also have benefits. People with bipolar are often the most creative, engaging, intelligent, life-affirming people around, and their zest for life is contagious. You can easily fall in love with them.
When someone you care about is in a deep depression, however, you may feel as though the disorder is swallowing you both into a bottomless pit of despair. During a full-blown manic episode, the arrogance, anger, self-righteousness, or emotional abuse your loved one displays may repel you. To maintain your own emotional stability and help the person you care about, try to keep the disorder in perspective and maintain a healthy state of mind. (Check out Chapter 19 for more details.)
To maintain your own emotional stability and help the person you care about, try to keep the disorder in perspective and maintain a healthy state of mind. (Check out Chapter 19 for more details.)
To support a friend or relative with bipolar disorder, the first step is to establish empathy and understand the level of control that the illness has over the person. Following are a few important points to keep in mind:
check.png Your loved one probably wants bipolar even less than you want him to have it.
check.png When your friend or relative spews abusive or cutting remarks, the disorder is talking. Don’t take it personally.
check.png Taking it personally is normal, so don’t feel guilty if you slip. Being a solid support person isn’t easy.
check.png The situation isn’t hopeless. With the right medication and therapy and your support, you can get your loved one back, and he may return even better than before!
check. png The more you know about bipolar disorder, the more you can accept it and provide proper support. By reading this book, you’re taking an important first step.
png The more you know about bipolar disorder, the more you can accept it and provide proper support. By reading this book, you’re taking an important first step.
Here are some ideas for more practical, hands-on things you can do to help a friend or relative with bipolar disorder:
check.png Attend a support group or class for friends or relatives of people with bipolar disorder.
check.png Ask your friend or relative how involved he wants you to be.
check.png Be helpful without being intrusive.
check.png During times of crisis, offer to cook, clean, or handle other necessities.
check.png Keep in touch. If your loved one is hospitalized, send a card or visit.
check.png Offer to drive your friend or relative to appointments.
check.png Listen.
check.png Treat your loved one as you used to — before you knew about the diagnosis.
Diagnosing and Treating a Child or Adolescent with Bipolar Disorder
The diagnosis of bipolar disorder in children (up to the age of 12) and adolescents (teenagers) has been an area of debate and controversy for more than a decade now. Even professionals in the field fundamentally disagree about some features of diagnosing this disorder in young age groups. The consensus that’s evolving, however, is straightforward: To be diagnosed with bipolar disorder, children need to exhibit the same patterns of energy and mood changes that adults do — at least one period of mania or hypomania, often associated with episodes of depression.
Even professionals in the field fundamentally disagree about some features of diagnosing this disorder in young age groups. The consensus that’s evolving, however, is straightforward: To be diagnosed with bipolar disorder, children need to exhibit the same patterns of energy and mood changes that adults do — at least one period of mania or hypomania, often associated with episodes of depression.
remember.eps Adolescents are more likely than younger children to show classic symptoms of bipolar — mania in particular. True mania does occur in children before puberty, but it’s infrequent. And recent research suggests that children who exhibit a lot of problems with mood dysregulation, particularly anger and irritability, aren’t more likely to exhibit bipolar disorder later in life. Instead, they often experience anxiety and/or depression when they get older.
The high energy and impulsivity that are prominent in manic episodes are core symptoms of one of the most common psychiatric conditions in children — attention deficit hyperactivity disorder (ADHD). The evolving diagnostic criteria for bipolar disorder in children don’t count high energy and impulsivity toward a manic episode diagnosis unless these symptoms become significantly worse during a sustained period of time (not just a few hours).
The evolving diagnostic criteria for bipolar disorder in children don’t count high energy and impulsivity toward a manic episode diagnosis unless these symptoms become significantly worse during a sustained period of time (not just a few hours).
This research is ongoing and the jury is still out on what bipolar disorder looks like in children and teens, but doctors now know that they must be cautious when evaluating young patients. The medications used to treat mania are powerful and have many side effects, and a diagnosis of bipolar may prevent the use of medications to treat ADHD or anxiety and depression. Therefore, a misdiagnosis in a child can have significant long-term consequences.
Obtaining an early, accurate diagnosis of a child’s difficulties and identifying whether the cause is bipolar disorder or something else is the most critical step in helping the child or adolescent manage a mood problem. See Chapter 21 for more about diagnosis and treatment options for children and teenagers who may be dealing with a mood disorder.
bipolarbio.eps
When I lost my mind, I lost my friendsDuring my battle with bipolar disorder, I was unaware of the consequences of my risky behavior — abusing substances, having promiscuous sex, staying up all night, and counterfeiting art — but I was high-functioning.
My diagnosis put me in a category of the population called bipolar. In my mind, I was a lunatic, freak, psycho, crack-up, and mental case. I had officially stigmatized myself, long before anyone else had the chance.
I invited my parents to dinner to tell them the news, and they had a ton of questions. Are you sure your doctor is right? Where did it come from? What’s going to happen to you? Is it genetic?
They struggled with the stigma of having a son with bipolar, and, even worse, they worried that it might run in the family — we might have more like me!
Family and friends didn’t come rushing to my side to support me in my battle. In 1993, the mere mention of bipolar disorder frightened people; someone with bipolar was crazy.
And because my insidious illness wasn’t tangible, like diabetes or MS, it was easier for people to blame it on me. At a time when I was most in need of support from my friends and family, stigma pushed them away. 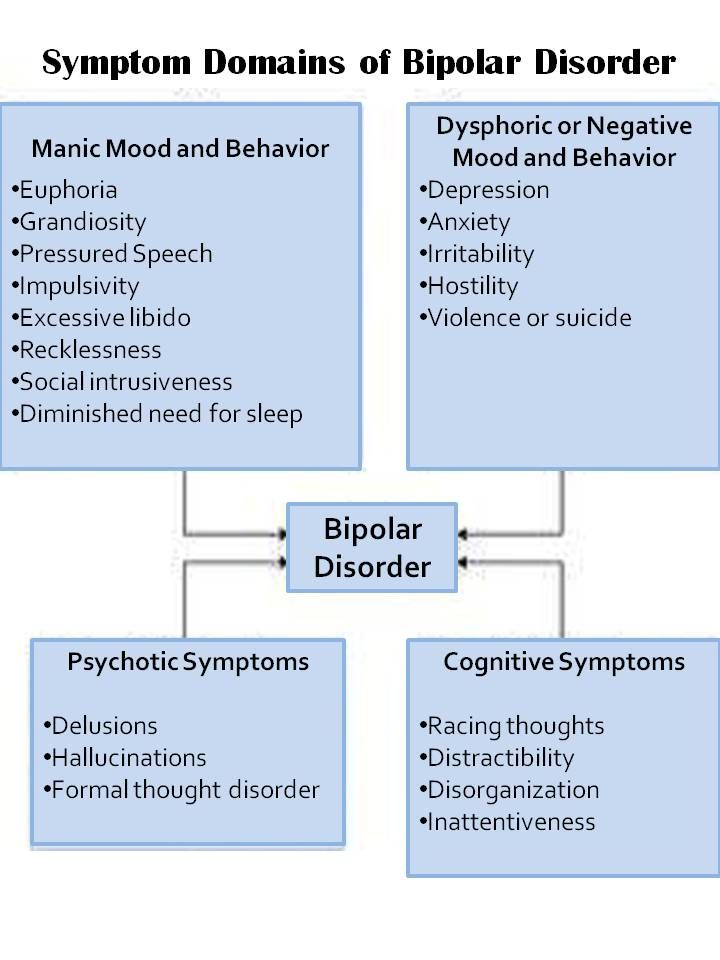
Most people thought I had the skills and strength to kick
my bipolar disorder and get better on my own because the symptoms didn’t show up on my body as a wound. Many people thought it was a figment of my imagination, that I was lazy or just seeking attention, and I started believing these ideas. But when symptoms surfaced, I was reminded that I really was suffering from bipolar disorder.
When medication didn’t quell the mania, I opted for the last resort — electroshock therapy. That decision in itself pretty much confirmed that I was officially mentally ill. It was too much for some of my friends to handle, and they simply disappeared. Nobody seemed to want a friend who was now a psychiatric patient and, after electroshock, a certifiable zombie.
Stigma prevents many us from seeking help and isolates us when we’re most in need of supportive friends and family. Even in my recovery today, when I speak openly about my diagnosis, I’m keenly aware that many people are uncomfortable and afraid. Stigma is a form of discrimination, and debunking the myths about bipolar disorder and disseminating the truths are critical to educating the public and creating a social environment that’s more conducive to mental health and recovery. — Andy Behrman (electroboy.com), author of Electroboy: A Memoir of Mania
Even in my recovery today, when I speak openly about my diagnosis, I’m keenly aware that many people are uncomfortable and afraid. Stigma is a form of discrimination, and debunking the myths about bipolar disorder and disseminating the truths are critical to educating the public and creating a social environment that’s more conducive to mental health and recovery. — Andy Behrman (electroboy.com), author of Electroboy: A Memoir of Mania
arrow Diagnosing bipolar disorder by the book — the diagnostic manuals
arrow Defining major depression, mania, hypomania, and psychosis
arrow Exploring bipolar I and II along with other forms of bipolar disorder
arrow Examining genetic vulnerabilities and other contributing factors
arrow Understanding the brain and the way in which it functions (and dysfunctions)
One of the more vexing aspects of bipolar disorder is that it manifests only through thoughts, emotions, perceptions, speech, and behavior.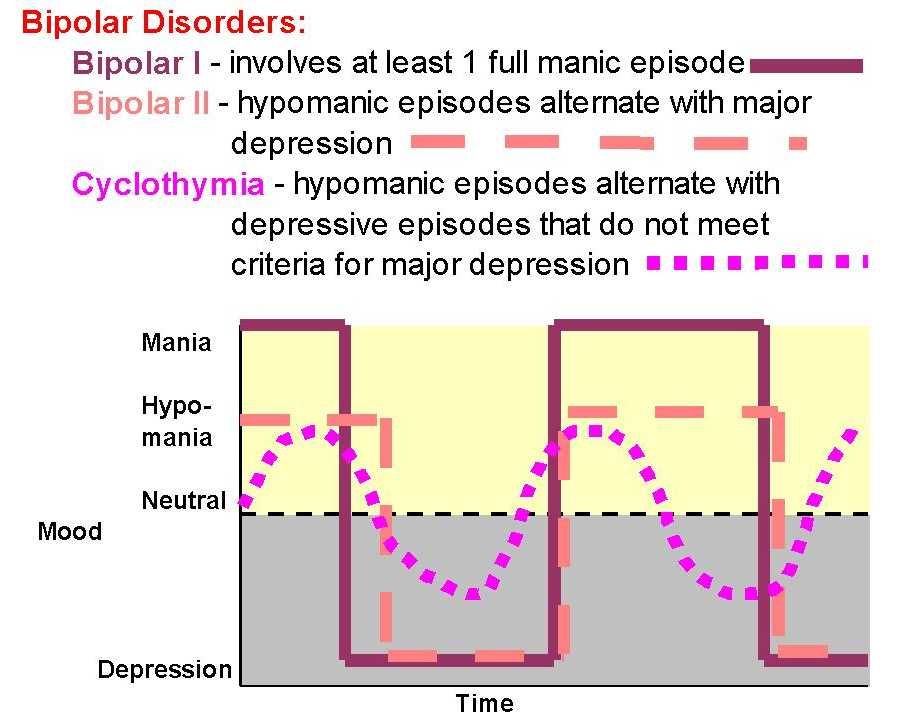 At the time of this writing, no medical test is available to prove beyond the shadow of doubt that you have bipolar disorder. Moreover, other medical conditions, such as thyroid malfunction, can produce symptoms that are similar to bipolar. The unfortunate result is that people often dismiss the illness as a character flaw or personality defect.
At the time of this writing, no medical test is available to prove beyond the shadow of doubt that you have bipolar disorder. Moreover, other medical conditions, such as thyroid malfunction, can produce symptoms that are similar to bipolar. The unfortunate result is that people often dismiss the illness as a character flaw or personality defect.
However, bipolar disorder is a very real physical illness. It just happens to affect the brain — one of the most complex parts of the human anatomy, one of the most difficult parts to test, and one of the areas most sensitive to emotional trauma and stress.
In this chapter, we define the terms that are the building blocks of the bipolar diagnosis, including depression, mania, and hypomania, and we look at how they come together to form principal bipolar diagnoses, including bipolar I and bipolar II. We also examine the biology of bipolar disorder, exploring the evolving picture of genetic vulnerability and brain physiology. We look at possible ways that medications work to alleviate symptoms. And because environmental stimuli contribute to the development of bipolar symptoms, we look at some other factors that can contribute to depression and mania.
We look at possible ways that medications work to alleviate symptoms. And because environmental stimuli contribute to the development of bipolar symptoms, we look at some other factors that can contribute to depression and mania.
Cracking Open the Diagnostic Manuals
To diagnose bipolar, doctors consult a manual that provides a list of criteria (symptoms) that must be present. In the U.S., doctors consult the Diagnostic and Statistical Manual of Mental Disorders (DSM). In the U.K. and throughout most of the world, doctors look to the International Classification of Diseases (ICD).
Diagnostic and Statistical Manual of Mental DisordersWhen a doctor in the U.S. diagnoses a mental illness, such as bipolar disorder, she relies primarily on the American Psychiatric Association’s (APA) Diagnostic and Statistical Manual of Mental Disorders (DSM). This manual defines numerous patterns of symptoms and illnesses that are supported by scientific research and consensus among a wide variety of experts. The DSM-IV has been used for many years, but the new edition, DSM-5, becomes official in May 2013. (Yes, that’s 5, not the Roman numeral V, as you may expect.)
The DSM-IV has been used for many years, but the new edition, DSM-5, becomes official in May 2013. (Yes, that’s 5, not the Roman numeral V, as you may expect.)
When talking about specific terms used in the diagnosis of bipolar disorder, we’ve tried to bridge the gap between DSM-IV and DSM-5, defaulting to expected changes in the soon-to-be-published update. Because some of these changes haven’t been fully defined as we write this book, be aware that the final version of DSM-5 may have some differences in language from what we use here. The major concepts and terms, however, are the same.
International Classification of DiseasesDoctors in countries throughout the world (not the U.S.) rely on the World Health Organization’s (WHO) International Classification of Diseases, a classification system for all health issues. Chapter V of the ICD specifically addresses mental and behavioral disorders.
The major difference between DSM-IV and ICD-10 is that the WHO’s manual doesn’t use the labels bipolar I and bipolar II as primary distinctions. Instead, ICD-10 refers to the disorder as bipolar affective disorder and then further classifies it by the current episode’s symptoms: currently hypomanic, currently manic, currently depressed, mixed disorder, or in remission. In addition, the ICD-10 requires two or more mood episodes, with at least one being manic or hypomanic, to qualify for a bipolar diagnosis, while the DSM requires only a single manic or hypomanic episode.
remember.eps The APA and WHO work together closely to coordinate their efforts. So in clinical practice, a doctor using one manual should arrive at a similar diagnosis as a doctor using the other.
Characteristics of Bipolar Disorder
Everyone experiences ups and downs, and some people are naturally a little moodier than others. That’s human nature, but it’s not what bipolar disorder is all about. If you drag yourself into a psychiatrist’s office singing the blues, he won’t (or shouldn’t) just hand you a prescription for an antidepressant. Likewise, if you stay up all night playing poker and howling at the moon with your buddies, don’t expect to receive a free sample of a mood stabilizer as a result of your one big night out. Major depression, mania, and hypomania are much more serious and more strictly defined than average mood
If you drag yourself into a psychiatrist’s office singing the blues, he won’t (or shouldn’t) just hand you a prescription for an antidepressant. Likewise, if you stay up all night playing poker and howling at the moon with your buddies, don’t expect to receive a free sample of a mood stabilizer as a result of your one big night out. Major depression, mania, and hypomania are much more serious and more strictly defined than average mood
5 books about bipolar disorder
22,097
This collection is addressed not only to those who have been diagnosed with this affective disorder, and there are many such people - there are more than 2 million of them in Russia alone, but also to everyone who wants to better understand their “ bipolar” friends and acquaintances, people who live as if on a rollercoaster – now experiencing ecstasy and “flights of the mind”, now plunging into darkness and impotence.
These books will help you to know yourself better, because each of us is different in some ways.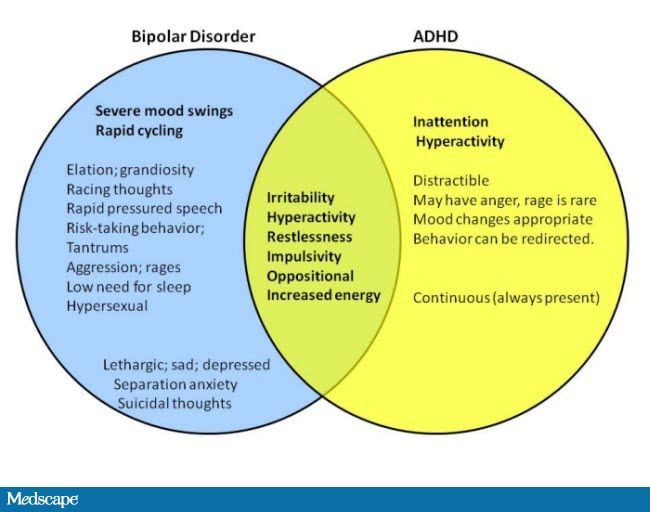 nine0003
nine0003
1. “A restless mind. My Victory Over Bipolar Disorder Kay Jamison
Kay Jamison is a psychiatrist and professor at Johns Hopkins University who has written several books on affective disorders, but this book is unique in that Kay talks about his personal experience. At the height of her scientific career, she realized that she herself suffered from a severe form of bipolar disorder. Nevertheless, she managed to create a clinic for the study of affective disorders and become a well-known specialist in this field. The reader will learn a lot about the causes of bipolar disorder, the history of the study of the problem and the methods of treatment. But first of all, about how you can live without giving up. Overcoming bouts of mania and then debilitating depression, Kay Jamison was able to make a serious contribution to the development of psychiatry and set an inspiring example for her patients. (Alpina Publisher, 2017)
2. “Confessions of a Normal Mad Woman” Olga Marinicheva
Turning a case history into a life story, Olga Marinicheva (who took the pseudonym Marina Zarechnaya) tells about unprecedented and unbearable love, visions and hallucinations, psychiatric hospitals and the fate of an entire generation. “Sometimes, in order to save the soul, she is forced to go into psychosis,” she writes in her poignant book. A diary, an autobiography, a human document (“human – and thanks for that,” the author comments on this characteristic) – it is impossible to determine the genre of this book. The text, like the life of the heroine herself, crumbles into fragments, but each page is filled with the talent of the author - a well-known journalist, writer and teacher. She knows very well why this book was written: “Now I just have nowhere but words,” and gives the reader a unique opportunity to see the experience of bipolar disorder described “from the other side”, from the inside. (Inapress, Novaya Gazeta, 2006)
“Sometimes, in order to save the soul, she is forced to go into psychosis,” she writes in her poignant book. A diary, an autobiography, a human document (“human – and thanks for that,” the author comments on this characteristic) – it is impossible to determine the genre of this book. The text, like the life of the heroine herself, crumbles into fragments, but each page is filled with the talent of the author - a well-known journalist, writer and teacher. She knows very well why this book was written: “Now I just have nowhere but words,” and gives the reader a unique opportunity to see the experience of bipolar disorder described “from the other side”, from the inside. (Inapress, Novaya Gazeta, 2006)
3. “Go crazy! A Guide to Mental Disorders for a City Resident Daria Varlamova, Anton Zainiev
Graduates of the Higher School of Economics, journalists Daria Varlamova and Anton Zainiev talk in a fascinating and accessible way about the most common mental disorders: depression, anxiety and bipolar disorders, schizophrenia and others. They also describe the methods of treatment, never getting tired of repeating: it is dangerous to use them on your own, without a visit to the doctor, and it is unlikely that it will work: you will need a psychiatrist's prescription to buy drugs. Most diseases do not impose special restrictions on life - no need to go on a diet, leave work, take toxic drugs and give up extreme entertainment. And at the same time, learning about your diagnosis is a great relief. “I perceived my problems with depression as personal shortcomings,” says Daria Varlamova. – I considered myself lazy, useless, useless. Knowing that you are sick and can be cured means that you can stop the destructive self-flagellation and start taking action.” (Alpina Publisher, 2016). nine0003
They also describe the methods of treatment, never getting tired of repeating: it is dangerous to use them on your own, without a visit to the doctor, and it is unlikely that it will work: you will need a psychiatrist's prescription to buy drugs. Most diseases do not impose special restrictions on life - no need to go on a diet, leave work, take toxic drugs and give up extreme entertainment. And at the same time, learning about your diagnosis is a great relief. “I perceived my problems with depression as personal shortcomings,” says Daria Varlamova. – I considered myself lazy, useless, useless. Knowing that you are sick and can be cured means that you can stop the destructive self-flagellation and start taking action.” (Alpina Publisher, 2016). nine0003
4. “Bipolar People: How People with Bipolar Disorder Live and Dream” Masha Pushkina
Journalist, editor of the bipolar.su portal Maria Pushkina has collected several personal stories – frank confessions of people with bipolar disorder. Among her heroes are the mathematical engineer Mikhail, who suffered his first attack of illness at the age of 25, and 35-year-old Asya, a graphic designer. Nastya, who fell in love with a man with the same diagnosis... They talk about how they first realized that they were sick, at what point they decided to seek help, and how they eventually learned to live with the disease. The characters' monologues are commented on by experts, psychiatrist and psychologists. They explain how to recognize the disease and what rules to follow in order to remain prosperous and productive. (Publishing Solutions, Ridero, 2017)
Among her heroes are the mathematical engineer Mikhail, who suffered his first attack of illness at the age of 25, and 35-year-old Asya, a graphic designer. Nastya, who fell in love with a man with the same diagnosis... They talk about how they first realized that they were sick, at what point they decided to seek help, and how they eventually learned to live with the disease. The characters' monologues are commented on by experts, psychiatrist and psychologists. They explain how to recognize the disease and what rules to follow in order to remain prosperous and productive. (Publishing Solutions, Ridero, 2017)
5. “Bipolar Toolkit”
Australian journalist and lawyer Sarah Freeman was diagnosed with bipolar disorder at the age of 40, but she managed to stabilize her condition, firstly, with the help of a diet, about which she wrote the book “The Bipolar Diet” (“ The Bipolar Diet, 2009), and secondly, using behavioral strategies aimed at developing awareness. Sarah Freeman details these strategies in a practical guide. There are only three of them: maintaining a mood chart, drawing up a recovery plan, and preparing a treatment agreement. The brochure is addressed to those who understand that therapy is the responsibility of not only the doctor, but also the patient. You can download the book for free here: http://bipolar.su/2016/06/instrumentarij-bipolyarnika-polezn/
There are only three of them: maintaining a mood chart, drawing up a recovery plan, and preparing a treatment agreement. The brochure is addressed to those who understand that therapy is the responsibility of not only the doctor, but also the patient. You can download the book for free here: http://bipolar.su/2016/06/instrumentarij-bipolyarnika-polezn/
Text: Alla Anufrieva Photo source: Getty Images
New on the site
Diet saboteurs: who and why prevents us from losing weight — 5 types of people
“The wife confessed to cheating… Now she has become more obedient, but what if everything happens again?”
“Is my husband an abuser? Help me understand”
Scientists have found out which men attract women the most
“Who gives life gives death”: how women perceive mother’s aging
Why do Russians run en masse to watch “Cheburashka”? Psychologist explains
Candid photos: how to loosen up in front of the camera - 6 secrets
"How can I help my husband prepare for the death of his beloved dog?"
Read the book “Bipolar Disorder.
 Survival guide for those who often don't see the white stripe" full online 📖 - Masha Pushkina - MyBook.
Survival guide for those who often don't see the white stripe" full online 📖 - Masha Pushkina - MyBook. Dedicated to the girl Alice, who was born together with the idea of this book
© Pushkina M., Kasyanov E., text
© Skochilenko A., ill.
© LLC AST Publishing House
The Chinese believe that before you kill a wild beast, you must see its beauty. I guess I tried to do it with a manic-depressive illness. She was to me a delightful but deadly beast, enemy and comrade. I was captivated by its complexity, an explosive mixture of the most beautiful and destructive in human nature. In order to conquer the disease, I had first to know it in all its countless forms, to understand its real and imagined power. nine0053
Kay Jamison, Restless Mind
Almost everyone has heard something about him, some even consider this diagnosis “fashionable”, because celebrities and TV series characters regularly talk about it.
At the same time, there is still very little verified and up-to-date information about bipolar disorder in Russian. nine0003
This book is the first in Russia written for people living with this disease and for those who care about them. For those who have to combine seemingly incompatible: unbridled fun and mortal longing, flight of thoughts and gray fog in the head, the desire to turn the world around and the inability to get out of bed in the morning.
There are more such people than we think.
According to global statistics, about 2% of all people suffer from bipolar disorder [1] . That is, there are almost three million bipolar people in Russia - half of the conditional St. Petersburg. And if we consider the whole spectrum of mood disorders, that is, disorders that lead to a chronically reduced emotional background or its sharp changes, then every tenth person suffers from them. This means that almost everyone, without even knowing it, encounters people in mania or depression in their life - if not in their family, then among friends or colleagues. nine0003
nine0003
Both of these conditions are dangerous, and above all for the patients themselves. Bipolar disorder is one of the most common causes of disability, almost on par with asthma and some cardiovascular diseases [2] .
According to various studies, from 25% to 50% of all bipolar people attempted suicide [3] .
And the number of broken destinies, ruined relationships, ruined abilities is impossible to count. This is despite the fact that the disease does not reduce mental abilities, does not deprive a person of the opportunity to be responsible for himself and responds well enough to treatment. nine0003
Many people do not seek help because they consider their features to be just a bad character. Or how psychiatrists are afraid of fire and the terrible words "put on record." In the end, they end up in hospitals in a rather serious condition, often after a suicide attempt.
Despite its popularity in mass culture, bipolar disorder is not yet a very "fashionable" diagnosis among Russian physicians. It is diagnosed dozens of times less often than in Europe, and is often confused with depression and schizophrenia. As a result - years of improper treatment, which can worsen the patient's condition. nine0003
It is diagnosed dozens of times less often than in Europe, and is often confused with depression and schizophrenia. As a result - years of improper treatment, which can worsen the patient's condition. nine0003
When a person nevertheless receives an F31 entry in the medical history, he can only guess: how to live on? And is it possible to live normally with this? The job duties of a psychiatrist do not include detailed explanations. Psychologists, for the most part, are only superficially familiar with psychiatry, and friends will most likely advise “not to bother” and “get more rest.”
With the most careful search, a new patient will find several books for doctors and a sea of conflicting information on the Internet. How to make a better scenario/algorithm/plan for the future life out of all this? nine0003
J Clin Psychiatry. (2000). Suicide and bipolar disorder (61 Suppl 9:47–51) [4]
Understanding and actively participating in treatment is essential for people with bipolar disorder, because their future depends on their lifestyle and habits as much than from medicines.
Four years ago, I started collecting bits and pieces of information about bipolar disorder from scientific research and foreign publications. First, she shared her findings in social networks, then, having thoroughly understood the issue, in educational articles in popular media. Over the years, I received a psychological education, met many creative and extraordinary bipolar people and a few psychiatrists who specialize in this field. We founded a patient community and opened support groups. We have accumulated a lot of useful experience. It's time to share it with a wide audience. nine0003
To create this book, I have assembled an extraordinary team of psychiatrists, psychologists and patients who have studied bipolar disorder not only in theory but in every possible aspect of practice.
In this guide, we provide up-to-date, reliable, and actionable information about bipolar disorder—the “pack of po- ss” you need to travel through life with this difficult diagnosis.