Anorexia inpatient meal plan
The Importance of an Anorexia Recovery Meal Plan
by Kristin Jenkins, MS, RDN, LDN | Eating Disorders
Why do I need an anorexia recovery meal plan?
Anorexia nervosa is a serious and potentially deadly disorder. An anorexia recovery meal plan is a crucial tool to safely re-nourish the body and mind. If left untreated, anorexia can cause dangerous physical and mental effects including:
- Malnutrition
- Heart damage
- Bone loss
- Loss of menstrual cycle
- Tooth decay, hair loss
- Anemia
- Kidney damage
- Nerve damage
- Neurological dysfunction
The goal of an anorexia recovery meal plan is to restore a healthy body weight and establish consistency, adequacy, balance, and variety to your eating habits.
Is it safe to follow an anorexia recovery meal plan at home?
There are risks associated with following an anorexia recovery meal plan, especially without the guidance of a nutrition professional. Refeeding syndrome results from rapid re-nourishment when the body has been in a chronically starved state. Refeeding syndrome causes drastic shifts in fluids and electrolytes from the bloodstream into cells, which can result in heart failure, seizures, coma, or death.
Risk of refeeding syndrome increases if BMI is below 18, there has been low to no nutritional intake for 5 or more days, or the individual has lost 10% or more of their body weight in the last 3-6 months. Daily monitoring of blood tests and heart function tests by a doctor can help your dietitian determine an appropriate meal plan to avoid refeeding complications.
Choosing an appropriate level of care
Outpatient nutritional rehabilitation, like that offered by the dietitians at Rebecca Bitzer and Associates, is most appropriate for those individuals who are clinically stable and not at high risk of refeeding syndrome. Outpatient sessions are usually 30-60 minutes, 1-2 times per week or less. Your outpatient dietitian will monitor your weight restoration progress and help you make adjustments to your meal plan so you continue meeting your weight and intake goals.
Your outpatient dietitian will monitor your weight restoration progress and help you make adjustments to your meal plan so you continue meeting your weight and intake goals.
Higher levels of care include (in order of increasing clinical support) intensive outpatient (IOP), partial hospitalization (PHP), residential, and inpatient hospitalization. Everyone’s journey is different. It is not uncommon for someone recovering from anorexia to need different levels of care at different times in their recovery. Recovery is not linear.
Your outpatient dietitian will closely monitor your progress and make recommendations for higher levels of care if they are concerned about your health and safety.
How much do I need to eat on my anorexia recovery meal plan?
Your anorexia recovery meal plan’s calorie amounts are tailored to your specific body and needs by your dietitian to achieve weight restoration. There is no one-size-fits-all recovery meal plan.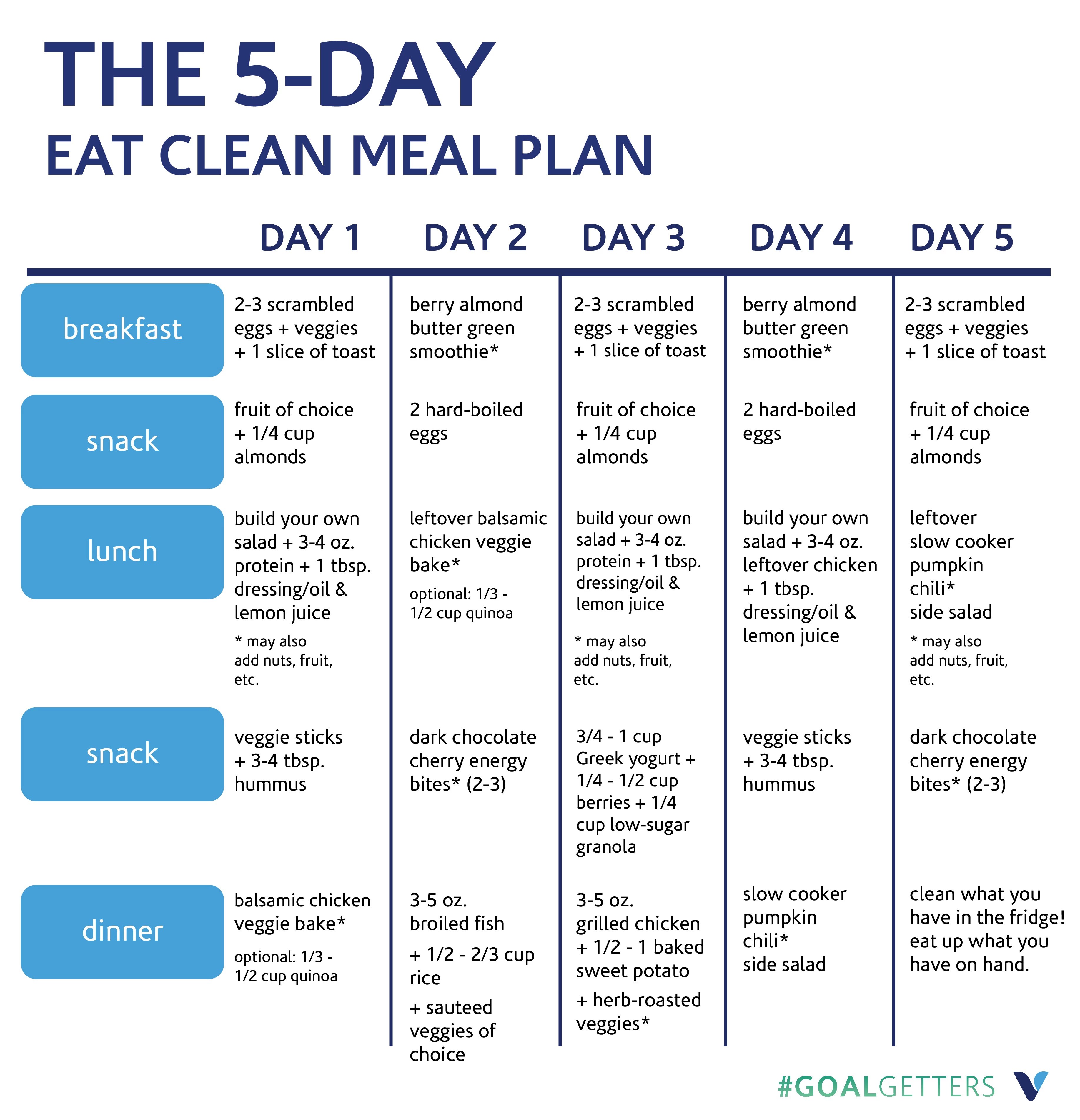
You may need to eat more food than you did prior to your eating disorder in order to restore a healthy body weight; This is normal. Your dietitian will help you determine a healthy goal weight range based on your growth charts (children and teens) and weight history (adults)
In general, an anorexia recovery meal plan will follow the “Rule of 3’s”: 3 meals, 3 snacks, no more than 3 hours apart. Meals will be structured around exchanges or fuel groups. In general, meals will include at least one portion of a carbohydrate or grain, a protein, and a fat. Snacks will include at least one portion of a carbohydrate and either a portion of a protein or a fat.
What about my fear foods/safe foods?
When you’re struggling with an eating disorder, the thought of eating some foods, or even whole food groups, can feel very challenging. We refer to these foods as “fear foods.” Fear foods can make it difficult to meet adequacy, balance, and variety goals.
Your dietitian will work with you to plan meals around foods that feel safer and less challenging to meet your energy needs. If you are unable to meet your energy needs with safe foods alone, your dietitian may recommend nutrition supplements like Ensure or Boost, to increase intake.
Your dietitian will also provide support in the planning and execution of food experientials to reintroduce fear foods into your diet to meet longer term goals of balance and variety. Challenging fear foods is an important and necessary part of anorexia recovery and establishing a healthy relationship with food.
Can my meal plan be vegetarian or vegan?
It is true that some individuals choose a vegetarian or vegan lifestyle for reasons pertaining to ethics or sustainability. It is also true that some individuals adopt a vegetarian or vegan lifestyle to further restrict their intake in accordance with their eating disorder.
Your dietitian will work with you to figure out how best to incorporate your values into your meal plan while still meeting your intake and weight restoration goals. If you are unable to meet your nutrition needs, your dietitian may recommend incorporating animal products at least until a healthy weight is restored.
If you are unable to meet your nutrition needs, your dietitian may recommend incorporating animal products at least until a healthy weight is restored.
What if I get too full too quickly to meet my meal plan?
Early fullness is to be expected after long periods of undereating. Your dietitian may work with you to plan smaller, more frequent meals and snacks. The sensation of fullness may feel very scary at first. Your dietitian and your therapist can work with you on how to manage difficult emotions at mealtimes.
The discomfort of early fullness may resolve on its own over time with consistency. In other cases, your dietitian may recommend a digestive enzyme or refer you to a GI specialist to address slow gastric emptying, or gastroparesis. This may be managed medically.
How can I be most successful in my anorexia recovery?
- Choose an appropriate level of care from a treatment provider/facility that aligns with your clinical, emotional, and spiritual needs
- Assemble a care team of providers who specialize in eating disorders, including a dietitian, a therapist, a psychiatrist, and a medical doctor
- Establish an eating plan with contingencies so you feel confident in what, when, where, and how you are nourishing yourself each day
- Identify your support system and include them in your treatment so they may offer support, encouragement, and accountability in your home environment
- Seek out resources that encourage, educate, and inspire you in your recovery including support groups, social media accounts, books, podcasts, and more
- Keep a list of your reasons why you want to recover; add your recovery wins and accomplishments to this list over time
- Identify when you are at risk of relapse, including times of transition, high stress, or the holidays, and recruit more support during these times
- Acknowledge that slips are not slides, and slides are not failures; relapsing does not mean you cannot fully recover from your eating disorder long term
Kristin Jenkins, MS, RDN, LDN
Kristin Jenkins, MS, RD is a Registered Dietitian Nutritionist. Kristin specializes in eating disorders and intuitive eating, and is an advocate for weight-inclusive care for all her clients.
Kristin specializes in eating disorders and intuitive eating, and is an advocate for weight-inclusive care for all her clients.
Eating Disorder Recovery Meal Plans
Table of Contents
Sharing is caring!
What Is The Purpose Of A Meal Plan In Eating Disorder Recovery?
Eating disorders, especially those involving very low caloric intake, will require a meal plan carefully constructed by a registered dietitian to re-nourish safely. Eating disorder recovery meal plans will vary from person to person.
There can be risks when we introduce food back into a very restrictive diet including digestive issues and refeeding syndrome.
An eating disorder meal plan will do several things for someone recovering from an eating disorder:
- Help them re-nourish safely
- Can help the person struggling with an eating disorder feel as though they have “permission” to eat (for example- my dietitian or doctor says I HAVE to eat this much)
- The prescriptive nature of an eating disorder meal plan can help soothe the eating disorder’s urge to restrict food
- Provides adequate nutrition for the body
- Can support weight restoration for patients that have lost significant amounts of weight.

Someone suffering from an eating disorder likely has a loud eating disorder voice which will make it very difficult to get adequate nourishment on their own. A meal plan can help.
An eating disorder meal plan can get rid of the confusion about when, where, and how much to eat for weight restoration and long-term ED recovery.
What Should I Eat In Recovery?
A balanced meal plan for eating disorder recovery will typically consist of:
- Grains and Starches: bread, english muffin, bagel, pita bread, grits, oatmeal, crackers, pretzels, popcorn, quinoa, bulgur, millet, polenta
- Meat or Meat Alternatives: chicken, fish, beef, pork, tofu, beans, tempeh, legumes
- Dairy or dairy alternatives: milk, soy milk, buttermilk, yogurt, cheese, cottage cheese, almond milk
- Vegetables: tomatoes, carrots, kale, broccoli, collard, artichokes, green beans, celery, cucumber, potatoes, winter squash, peas, corn
- Fruit: apricots, bananas, dates, grapes, oranges, juice, melons, strawberries, pineapple, raisins
- Fats and oils: butter, mayo, olive oil, salad dressing, olives, avocado, hummus
The amount of each of these food groups will vary greatly for each person.
Is It Safe To Initiate Eating Disorder Recovery Meal Plans At Home
This will highly depend on the level of restriction and total amount food a person is eating throughout the day at the time the meal plan is to be initiated.
If someone is consuming less than 500 calories a day (the equivalent of a peanut butter and jelly sandwich and a glass of milk) A recovery meal plan at home is not safe.
This level of malnutrition often requires a higher level of care such as an inpatient facility or medical monitoring at a hospital.
The decision to start a recovery meal plan at home should be carefully assessed by the eating disorder treatment team which includes a haes dietitian.
If a person is consuming very low nutrition they may require the following when refeeding:
- A comprehensive metabolic panel CMP(blood draw) with their physician two times a week.
- A DEXA scan (especially if the person has gone more than 6 months without a period)
- A magnesium test
- Monitoring blood pressure
- Monitoring heart rate
The comprehensive metabolic panel and magnesium test is intended to monitor for re-feeding syndrome, which can be life-threatening.
When food is re-introduced, it should be gradual.
Recovery Meal Plan For Anorexia
How Do You Start Eating After Starvation?
If it is deemed safe by your medical team you follow a meal plan in your home. It is very important to remember that for both anorexia and atypical anorexia, a meal plan is necessary and will most likely support weight restoration.
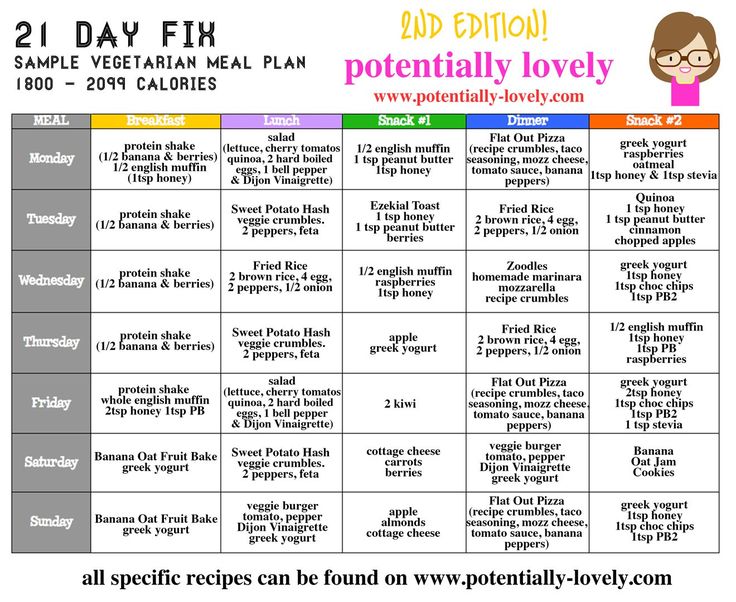
Here is a meal plan that will be safe to follow for most people.
Recovery Breakfast Portions:
- Grains-1
- Meat/alternatives-1
- Dairy/alternatives-1
- Fruits/Vegetables-1.5
- Fats/Spreads-1
Recovery Lunch Portions:
- Grains-2
- Meat/alternatives-1
- Dairy/alternatives-0.5
- Fruits/Vegetables-1
- Fats/Spreads-1
Recovery After Noon Snack Portions:
- Grains or Cereal Bar-1
Recovery Dinner Portions:
- Grains-2
- Meat/alternatives-2
- Dairy/alternatives-1
- Fruits/Vegetables-1.
 5
5
Recovery After Dinner Snack Portions:
- Dairy/Alternative-1
It’s important to consider that the recommendations for starting out with a recovery meal plan WILL NOT meet the actual nutrition needs for most people.
You should plan to gradually add to this plan weekly with the guidance of your treatment team. Typically an increase of 500 calories per week is appropriate.
A vegan eating disorder recovery meal plan will look slightly different in terms of food choices, but will include the same amount of calories.
Hypermetabolism in anorexia recovery can significantly increase the amount of energy one needs throughout the day and should be closely monitored for while someone follows an eating disorder recovery meal plan.
How Many Meals Does Someone Recovering From Anorexia Need?
People recovering from an eating disorder including anorexia should plan to have a meal or snack no more than 3 hours apart.
A typical recovery treatment plan will include at least 3 meals and 2 snacks per day for someone recovering from anorexia.
Bulimia Recovery Meal Plan
Bulimia can present with binging, restricting, or both.
A meal plan for bulimia recovery will vary somewhat based on the symptoms that a person is having. The primary goal of a meal plan in bulimia recovery is:
- Adequate intake
- To create meal structure throughout the day
- Provide permission to eat
For a bulimia recovery meal plan, the intention is to alleviate the restriction. A recovery plan for bulimia should consist of regular meals and snacks throughout the day (about 3 hours apart).
A bulimia recovery meal plan should consist of at least 3 meals and two snacks per day.
What Is The Rule Of Threes In Eating Disorder Recovery?
The rule of threes in eating disorder recovery is a simple way to remind ourselves when and how to nourish.
The rule of threes includes having this structure daily:
- Three meals
- Three snacks
- No more than three hours apart
While individual needs will vary and should be discussed with an eating disorder dietitian, a general eating disorder recovery meal will consist of:
- A grain
- A Fat
- A Protein
- A fruit or veggie
What Does The Plate By Plate Method Look Like In Eating Disorder Recovery?
The plate by plate approach focuses on the composition of each plate at every meal.
Some individuals can benefit from this approach as it does not require measuring individual portions or calorie counting.
The plate by plate approach focuses on:
- 1/2 plate of grains/starches
- 1/4 plate veggies/fruits
- 1/4 plate protein
- one fat
- 1 serving of dairy
This plate may be modified slightly for children or those with bulimia nervosa.
Have you Been Successful With A Recovery Meal Plan?
Easy disorder recovery is not easy. It’s reddened with many emotions and comes along with an abundance of physical discomfort. It is certainly something that no one should face alone.
Your support system can provide valuable meal support while this meal plan is carried out.
No one should begin to reintroduce food after restriction without proper guidance from an eating disorder treatment team.
An eating disorder recovery meal plan will vary from one person to the next. We can expect every recovery meal plan to include:
- variety
- balance
- Frequency in meal consumption
- Portion guidelines
I often refer people on the support team to the book “sick enough” by Jennifer Guadiani for additional support with the medical complications of eating disorders.
Reminder: The links below are affiliate links. As an Amazon Associate, I earn from qualifying purchases
For more support on safe refeeding guidelines, check out these other eating disorder recovery books.
Stop Humoring
Body Image Bullies!
Whether it’s your great aunt Sally or the itty bitty shitty committee in your own head- messages that threaten how you feel about your body suck.
Subscribe and i’ll send you the ultimate guide for battling the bullies that make us feel like our bodies are something to be “fixed.”
Ditch body checking and respond to weight focused comments like a champ.
Email address
Thank you for subscribing!
Is it safe to initiate eating disorder recovery meal plans at home?
It depends. Those with an energy intake less than 500 calories a day will likely need a higher level of care.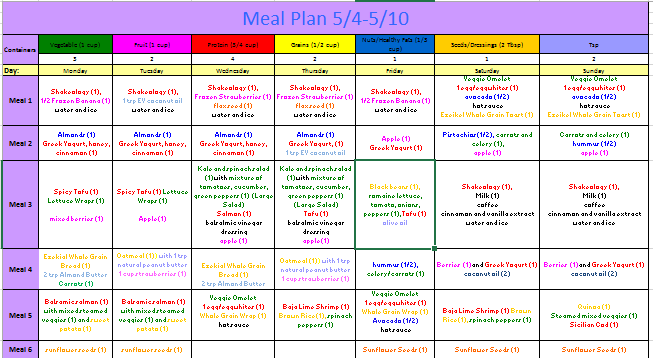
What is in a meal plan for ED recovery
Grains, proteins, fruits, vegetables, fats and oils
What are some anorexia recovery meal plan examples
Anorexia recovery meal plans typically consist of 3 meals and 3 snacks per day. They may start at 1600 calories and move up to the appropriate level of intake for the person.
What are the goals of the meal plan in ED recovery
balance, permission to eat, appropriate meal frequency, adequate nourishment
Diet for overcoming anorexia
Treatment of anorexia in our center.
Features of the treatment of anorexia in our center. ATTENTION!!! These tips will only work if you have begun to recover from anorexia. During anorexia itself, this advice is useless, because. the patient cannot follow the recommendations. Therefore, if in your case, anorexia has not yet passed - contact our center and get advice. The consultation will take place on a confidential note, no one will blame, frighten or shame you or your daughter. nine0005
Therefore, if in your case, anorexia has not yet passed - contact our center and get advice. The consultation will take place on a confidential note, no one will blame, frighten or shame you or your daughter. nine0005
Anorexia is a severe addiction that causes complete ruins in the body. Young girls are unable to resist it, just as an alcoholic cannot resist his addiction. The body of an anorexic patient is bound by a muscular shell, which indicates increased anxiety. In general, this tension and accompanying anxiety create unbearable conditions. from which a person seeks to escape by any means. Therefore, auto-aggression, thoughts of suicide are frequent companions of anorexia.
It is from these unbearable conditions that the obsessive thoughts of losing weight appear. Because after a weight loss of at least 100 grams, at least some decrease in tension appears in the patient's body. That is why the connection with reality is lost and only the world of the ideal and stereotypes remains.
At any stage of the development of the disease, a careful diet and adherence to strict limits must be observed. If the patient is not able to take food himself, then in such cases the doctor prescribes intravenous administration of minerals and vitamins, and the food in a puree-like form enters through special tubes directly into the intestines. Thus, the patient's body gradually gets used to eating and gradually begins to eat independently. With anorexia in the diet, the menu should be varied and consist of soft foods that will not irritate the stomach as much as coarse food. nine0005
The food menu to get out of anorexia should have:
- High-calorie foods.
- Foods with a high protein content.
- Fresh fruits and vegetables.
- Vitamins and minerals.
If you follow the right diet, which will help you gain weight and restore the body, then the disease will quickly go away and there will be no recurrence of the disease. It is very important not to pass and eat throughout the day in small portions. A balanced diet will enrich the body with nutrients and fill it with energy. The brain will work better, and will not give signals about a critical condition that food has entered the body. nine0005
A balanced diet will enrich the body with nutrients and fill it with energy. The brain will work better, and will not give signals about a critical condition that food has entered the body. nine0005
Recovery from anorexia will be much faster if the diet is properly compiled by a nutritionist. Compliance with such a diet is, in a way, the prevention of a subsequent disease. After all, when a person gets used to eating right, it already becomes a habit that is hard to change.
Do not forget to introduce fermented milk products into your diet, even if you don't like them, it's still worth consuming a little. So you saturate the body with calcium, a protein that is indispensable in the restoration of bone tissue and muscles. You should not introduce a lot of sweets into the diet, it will be enough to use dark chocolate, honey, ice cream. You need to eat fish, chicken, turkey, the preparation of which should be steamed or boiled. Fried food should not be consumed by an anorexic patient.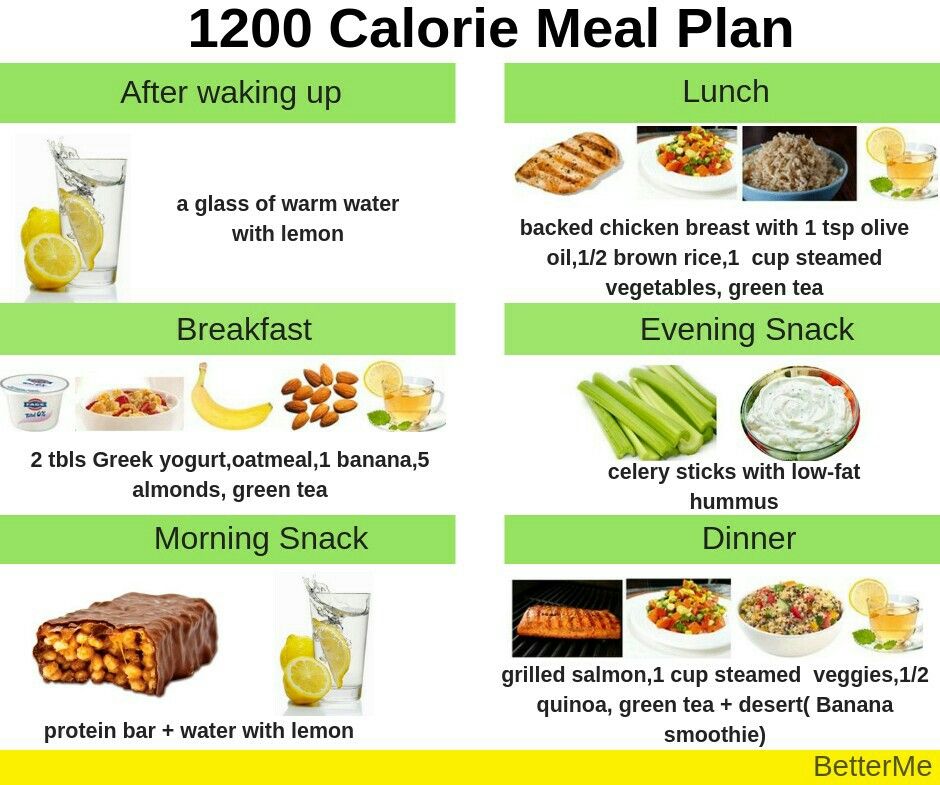 nine0005
nine0005
Fruit purees, vegetable soups and lean meats will improve the gastrointestinal tract and allow you to gradually gain weight. One has only to listen to the advice of a nutritionist and follow a diet.
How is treatment in our center different from others?
- Our center treats the condition of PTSD, which is not treated in other clinics and centers. PTSD, which is present in 100% of patients with RPP. And this condition is ignored in clinics by psychologists and psychotherapists, so it remains undeveloped. The state of PTSD in our center is worked out with the help of techniques: CBT, DPDH and the Gestalt approach. nine0030
- Our center uses methods of family systemic therapy, which gives good results, because. the climate in the environment of the patient with RPP changes. Which is rarely used in other clinics and centers.
- Our center uses "mom therapy". This is when we work with mom to cure our daughter. This technique is also practically not used in clinics for the treatment of ED.
Learn about the real causes of anorexia!
in clinics, even with hospitalization, the effectiveness of treatment is no more than 30%, due to the fact that only 30% of the channels for the appearance of anorexia causes are blocked, then in our center, due to the use of these additional techniques, 90% of the channels for the causes of anorexia, then the effectiveness of treatment is kept in the region of 90%. You will not find these methods in other clinics and centers for the treatment of ED, even the most famous and expensive ones. Therefore, in 70% of cases, after being discharged from medical clinics after a few months, patients with eating disorders again go into food addiction. And you need to go back to the clinic. And it turns out a vicious circle that sucks energy, money and time out of relatives, resulting in apathy and indifference to other treatment options. One often hears: "We have already tried everything, we were in the most famous clinics of RPP? Nothing helped us!". Such clients after 1 month of treatment in our center see improvements and they have hope. And after a few months they are cured and no longer get sick with RPP. nine0005
One often hears: "We have already tried everything, we were in the most famous clinics of RPP? Nothing helped us!". Such clients after 1 month of treatment in our center see improvements and they have hope. And after a few months they are cured and no longer get sick with RPP. nine0005
Feedback from Natasha.
Video review of a model treated via Skype. She has never even visited us in person.
Feedback from Svetlana.
Treatment of anorexia in our center.
Other Resources:
Book an Initial Anorexia Consultation.
If your daughter has anorexia, how should you deal with her? nine0005
The first exercise in the treatment of eating disorders.
A special case of anorexia.
Restoration of nutrition and weight in anorexia - treatment of eating disorders in the CIRP
Initial Consultation
What do Nutrition Counselors experience in an average initial consultation?
- patients come with a very limited range of foods they eat
- small servings
- unbalanced diet
- the patient is afraid to eat and gain weight
- food gives a terrible feeling - physical and emotional
- heaviness after eating
- bloating after eating as a result of eating only fruits and vegetables
- Voluntary vomiting and dehydration as a result of vomiting
- heartburn and belching after vomiting
- "safe food" presentation
- availability of a list of "forbidden foods" - high-calorie / "harmful"
- Edema after eating
- toilet problems (constipation due to lack of solid fiber in the diet and other carbohydrate-containing foods in the diet)
- taking laxatives and diuretics
What does a nutrition consultant tell a patient at the initial appointment? The concepts of basal and basal metabolism
Basic metabolism is the energy that the body needs to carry out vital functions, maintain blood circulation, endocrine system, respiration (we use this energy even at rest). This is the energy that we cannot influence. Approximately 70% of the energy received as a result of eating goes to the implementation of the basic metabolism.
This is the energy that we cannot influence. Approximately 70% of the energy received as a result of eating goes to the implementation of the basic metabolism.
Basic metabolism is the energy (conditional remaining 30%) that goes to the brain, physical activity (go to school, for example), maintaining the temperature regime to adapt to the temperature environment. nine0005
Catering in the hospital
In the hospital we have 6 meals a day: three main meals (breakfast, lunch and dinner) and three snacks (snack after dinner - milk or kefir).
There are different diets, "tables":
- First table
Food without salt, spices, everything boiled, fresh, without raw fruits and vegetables (such a sparing table helps reduce the aggression of unpleasant physical symptoms - bloating, constipation, heartburn, + so as not to provoke swelling, as well as adapt to a new diet, new products). nine0030 - Second table
Salts and spices, fruits and vegetables may be allowed, the heat treatment of food changes (baked foods), the diet becomes more varied (less dietary foods appear in the diet).
- Third table
Choice of two courses, the diet of an ordinary person: salts and spices, fruits and vegetables are used, as well as products initially "forbidden" by the patient - Fourth table
Choice of two courses and the patient himself determines the amount of food on the plate. Still sometimes it's going out to a cafe to test your new eating skills. nine0030
Organization of treatment
How is the treatment going?
Restoring nutrition
- Restoring the amount of nutrition to the standard: such an amount of nutrition that will provide the basic and main volume
- Restoring the balance of proteins, fats, carbohydrates, vitamins, minerals
- Restoring dietary diversity (gradually)
- We restore the disturbed feeling of satiety and hunger
- Restoring energy from food alone, without replacement nutrition
In case of bulimia, the menu is compiled in such a way that there are no sharp bouts of hunger - slow carbohydrates are included in the menu.
Restoring weight
Rapid weight gain is dangerous for health, it is also dangerous to gain weight rapidly solely due to a very large amount of food (the body is not ready to digest such an amount on the go).
We do not fatten patients on food, replacement therapy is used to restore weight:
- Enteral nutrition - nutritional mixtures in powder form, liquid is added to make a drink, Nutrison is used in our center
- Parenteral nutrition - formula drips (bypassing the GI tract)
Parenteral nutrition provides all the necessary nutrients while the patient gradually learns to eat again and builds a conscious relationship with food. The disadvantage of parenteral nutrition is the acceleration of metabolism (hypermetabolic status), metabolism returns to normal within a year. nine0005
Coming to health weight. Keeping the weight of health
Outpatient treatment: regular follow-up with a nutritional consultant. After discharge from the hospital, it is necessary to monitor your nutrition and weight - as there is a high risk of weight loss due to hypermetabolic status. The nutrition plan needs to be adjusted in a timely manner to maintain a healthy weight against the backdrop of a return to normal activities in the form of study, work and more physical activity than that which was in the hospital. nine0005
The nutrition plan needs to be adjusted in a timely manner to maintain a healthy weight against the backdrop of a return to normal activities in the form of study, work and more physical activity than that which was in the hospital. nine0005
After discharge
After discharge, a food diary is kept - what we eat and what we feel. If necessary, titration (correction) of the patients' menu is done with a nutrition consultant. Outpatient monitoring allows you to maintain the progress achieved during the hospitalization in the normalization of nutrition and weight, it is important to note that in addition to monitoring with a nutritionist, it is also necessary to regularly receive consultations from a psychologist and the attending physician.
Author: Korshunova Anna Aleksandrovna
Head of the Center for the Study of Eating Disorders,
psychiatrist, psychotherapist.
Learn more