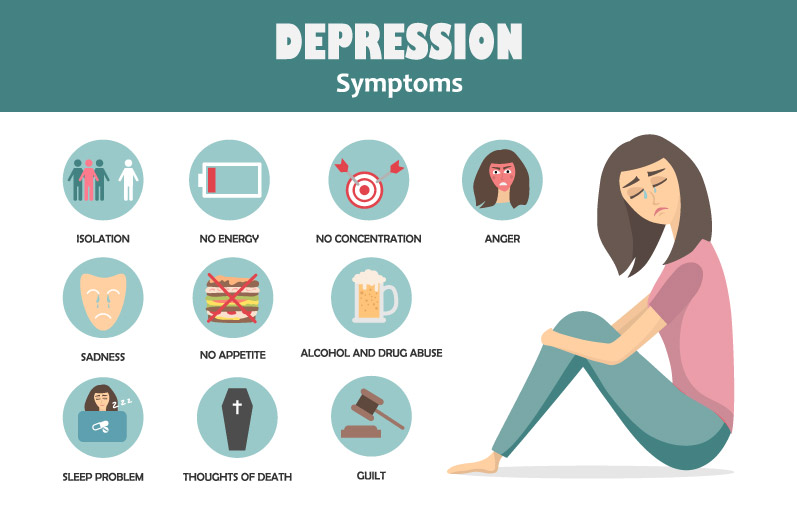
Definition of depression disorder
Depression (major depressive disorder) - Diagnosis and treatment
Diagnosis
Your doctor may determine a diagnosis of depression based on:
- Physical exam. Your doctor may do a physical exam and ask questions about your health. In some cases, depression may be linked to an underlying physical health problem.
- Lab tests. For example, your doctor may do a blood test called a complete blood count or test your thyroid to make sure it's functioning properly.
- Psychiatric evaluation. Your mental health professional asks about your symptoms, thoughts, feelings and behavior patterns. You may be asked to fill out a questionnaire to help answer these questions.
- DSM-5. Your mental health professional may use the criteria for depression listed in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5), published by the American Psychiatric Association.
Types of depression
Symptoms caused by major depression can vary from person to person. To clarify the type of depression you have, your doctor may add one or more specifiers. A specifier means that you have depression with specific features, such as:
- Anxious distress — depression with unusual restlessness or worry about possible events or loss of control
- Mixed features — simultaneous depression and mania, which includes elevated self-esteem, talking too much and increased energy
- Melancholic features — severe depression with lack of response to something that used to bring pleasure and associated with early morning awakening, worsened mood in the morning, major changes in appetite, and feelings of guilt, agitation or sluggishness
- Atypical features — depression that includes the ability to temporarily be cheered by happy events, increased appetite, excessive need for sleep, sensitivity to rejection, and a heavy feeling in the arms or legs
- Psychotic features — depression accompanied by delusions or hallucinations, which may involve personal inadequacy or other negative themes
- Catatonia — depression that includes motor activity that involves either uncontrollable and purposeless movement or fixed and inflexible posture
- Peripartum onset — depression that occurs during pregnancy or in the weeks or months after delivery (postpartum)
- Seasonal pattern — depression related to changes in seasons and reduced exposure to sunlight
Other disorders that cause depression symptoms
Several other disorders, such as those below, include depression as a symptom. It's important to get an accurate diagnosis, so you can get appropriate treatment.
It's important to get an accurate diagnosis, so you can get appropriate treatment.
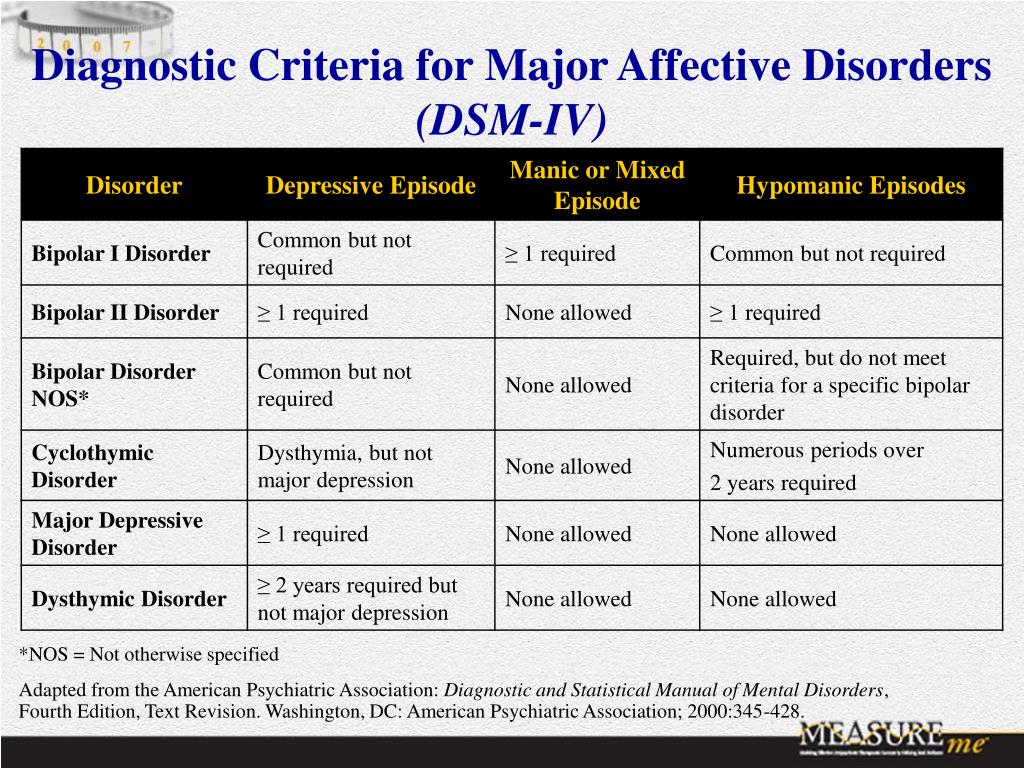
- Bipolar I and II disorders. These mood disorders include mood swings that range from highs (mania) to lows (depression). It's sometimes difficult to distinguish between bipolar disorder and depression.
- Cyclothymic disorder. Cyclothymic (sy-kloe-THIE-mik) disorder involves highs and lows that are milder than those of bipolar disorder.
- Disruptive mood dysregulation disorder. This mood disorder in children includes chronic and severe irritability and anger with frequent extreme temper outbursts. This disorder typically develops into depressive disorder or anxiety disorder during the teen years or adulthood.
- Persistent depressive disorder. Sometimes called dysthymia (dis-THIE-me-uh), this is a less severe but more chronic form of depression. While it's usually not disabling, persistent depressive disorder can prevent you from functioning normally in your daily routine and from living life to its fullest.
- Premenstrual dysphoric disorder. This involves depression symptoms associated with hormone changes that begin a week before and improve within a few days after the onset of your period, and are minimal or gone after completion of your period.
- Other depression disorders. This includes depression that's caused by the use of recreational drugs, some prescribed medications or another medical condition.
Care at Mayo Clinic
Our caring team of Mayo Clinic experts can help you with your depression (major depressive disorder)-related health concerns Start Here
More Information
- Depression (major depressive disorder) care at Mayo Clinic
- Complete blood count (CBC)
Treatment
Medications and psychotherapy are effective for most people with depression. Your primary care doctor or psychiatrist can prescribe medications to relieve symptoms. However, many people with depression also benefit from seeing a psychiatrist, psychologist or other mental health professional.
However, many people with depression also benefit from seeing a psychiatrist, psychologist or other mental health professional.
If you have severe depression, you may need a hospital stay, or you may need to participate in an outpatient treatment program until your symptoms improve.
Here's a closer look at depression treatment options.
Medications
Many types of antidepressants are available, including those below. Be sure to discuss possible major side effects with your doctor or pharmacist.
- Selective serotonin reuptake inhibitors (SSRIs). Doctors often start by prescribing an SSRI. These drugs are considered safer and generally cause fewer bothersome side effects than other types of antidepressants. SSRIs include citalopram (Celexa), escitalopram (Lexapro), fluoxetine (Prozac), paroxetine (Paxil, Pexeva), sertraline (Zoloft) and vilazodone (Viibryd).
- Serotonin-norepinephrine reuptake inhibitors (SNRIs). Examples of SNRIs include duloxetine (Cymbalta), venlafaxine (Effexor XR), desvenlafaxine (Pristiq, Khedezla) and levomilnacipran (Fetzima).

- Atypical antidepressants. These medications don't fit neatly into any of the other antidepressant categories. They include bupropion (Wellbutrin XL, Wellbutrin SR, Aplenzin, Forfivo XL), mirtazapine (Remeron), nefazodone, trazodone and vortioxetine (Trintellix).
- Tricyclic antidepressants. These drugs — such as imipramine (Tofranil), nortriptyline (Pamelor), amitriptyline, doxepin, trimipramine (Surmontil), desipramine (Norpramin) and protriptyline (Vivactil) — can be very effective, but tend to cause more-severe side effects than newer antidepressants. So tricyclics generally aren't prescribed unless you've tried an SSRI first without improvement.
- Monoamine oxidase inhibitors (MAOIs). MAOIs — such as tranylcypromine (Parnate), phenelzine (Nardil) and isocarboxazid (Marplan) — may be prescribed, typically when other drugs haven't worked, because they can have serious side effects. Using MAOIs requires a strict diet because of dangerous (or even deadly) interactions with foods ― such as certain cheeses, pickles and wines ― and some medications and herbal supplements.
 Selegiline (Emsam), a newer MAOI that sticks on the skin as a patch, may cause fewer side effects than other MAOIs do. These medications can't be combined with SSRIs.
Selegiline (Emsam), a newer MAOI that sticks on the skin as a patch, may cause fewer side effects than other MAOIs do. These medications can't be combined with SSRIs. - Other medications. Other medications may be added to an antidepressant to enhance antidepressant effects. Your doctor may recommend combining two antidepressants or adding medications such as mood stabilizers or antipsychotics. Anti-anxiety and stimulant medications also may be added for short-term use.
Finding the right medication
If a family member has responded well to an antidepressant, it may be one that could help you. Or you may need to try several medications or a combination of medications before you find one that works. This requires patience, as some medications need several weeks or longer to take full effect and for side effects to ease as your body adjusts.
Inherited traits play a role in how antidepressants affect you. In some cases, where available, results of genetic tests (done by a blood test or cheek swab) may offer clues about how your body may respond to a particular antidepressant. However, other variables besides genetics can affect your response to medication.
However, other variables besides genetics can affect your response to medication.
Risks of abruptly stopping medication
Don't stop taking an antidepressant without talking to your doctor first. Antidepressants aren't considered addictive, but sometimes physical dependence (which is different from addiction) can occur.
Stopping treatment abruptly or missing several doses can cause withdrawal-like symptoms, and quitting suddenly may cause a sudden worsening of depression. Work with your doctor to gradually and safely decrease your dose.
Antidepressants and pregnancy
If you're pregnant or breast-feeding, some antidepressants may pose an increased health risk to your unborn child or nursing child. Talk with your doctor if you become pregnant or you're planning to become pregnant.
Antidepressants and increased suicide risk
Most antidepressants are generally safe, but the Food and Drug Administration (FDA) requires all antidepressants to carry a black box warning, the strictest warning for prescriptions. In some cases, children, teenagers and young adults under age 25 may have an increase in suicidal thoughts or behavior when taking antidepressants, especially in the first few weeks after starting or when the dose is changed.
In some cases, children, teenagers and young adults under age 25 may have an increase in suicidal thoughts or behavior when taking antidepressants, especially in the first few weeks after starting or when the dose is changed.
Anyone taking an antidepressant should be watched closely for worsening depression or unusual behavior, especially when starting a new medication or with a change in dosage. If you or someone you know has suicidal thoughts when taking an antidepressant, immediately contact a doctor or get emergency help.
Keep in mind that antidepressants are more likely to reduce suicide risk in the long run by improving mood.
Psychotherapy
Psychotherapy is a general term for treating depression by talking about your condition and related issues with a mental health professional. Psychotherapy is also known as talk therapy or psychological therapy.
Different types of psychotherapy can be effective for depression, such as cognitive behavioral therapy or interpersonal therapy. Your mental health professional may also recommend other types of therapies. Psychotherapy can help you:
Your mental health professional may also recommend other types of therapies. Psychotherapy can help you:
- Adjust to a crisis or other current difficulty
- Identify negative beliefs and behaviors and replace them with healthy, positive ones
- Explore relationships and experiences, and develop positive interactions with others
- Find better ways to cope and solve problems
- Identify issues that contribute to your depression and change behaviors that make it worse
- Regain a sense of satisfaction and control in your life and help ease depression symptoms, such as hopelessness and anger
- Learn to set realistic goals for your life
- Develop the ability to tolerate and accept distress using healthier behaviors
Alternate formats for therapy
Formats for depression therapy as an alternative to face-to-face office sessions are available and may be an effective option for some people. Therapy can be provided, for example, as a computer program, by online sessions, or using videos or workbooks. Programs can be guided by a therapist or be partially or totally independent.
Programs can be guided by a therapist or be partially or totally independent.
Before you choose one of these options, discuss these formats with your therapist to determine if they may be helpful for you. Also, ask your therapist if he or she can recommend a trusted source or program. Some may not be covered by your insurance and not all developers and online therapists have the proper credentials or training.
Smartphones and tablets that offer mobile health apps, such as support and general education about depression, are not a substitute for seeing your doctor or therapist.
Hospital and residential treatment
In some people, depression is so severe that a hospital stay is needed. This may be necessary if you can't care for yourself properly or when you're in immediate danger of harming yourself or someone else. Psychiatric treatment at a hospital can help keep you calm and safe until your mood improves.
Partial hospitalization or day treatment programs also may help some people. These programs provide the outpatient support and counseling needed to get symptoms under control.
These programs provide the outpatient support and counseling needed to get symptoms under control.
Other treatment options
For some people, other procedures, sometimes called brain stimulation therapies, may be suggested:
- Electroconvulsive therapy (ECT). In ECT, electrical currents are passed through the brain to impact the function and effect of neurotransmitters in your brain to relieve depression. ECT is usually used for people who don't get better with medications, can't take antidepressants for health reasons or are at high risk of suicide.
- Transcranial magnetic stimulation (TMS). TMS may be an option for those who haven't responded to antidepressants. During TMS, a treatment coil placed against your scalp sends brief magnetic pulses to stimulate nerve cells in your brain that are involved in mood regulation and depression.
More Information
- Depression (major depressive disorder) care at Mayo Clinic
- Antidepressants: Selecting one that's right for you
- Antidepressants: Side effects
- Atypical antidepressants
- Monoamine oxidase inhibitors (MAOIs)
- Selective serotonin reuptake inhibitors (SSRIs)
- Serotonin and norepinephrine reuptake inhibitors (SNRIs)
- Treatment-resistant depression
- Tricyclic antidepressants and tetracyclic antidepressants
- Antidepressant withdrawal: Is there such a thing?
- Antidepressants and alcohol: What's the concern?
- Antidepressants and weight gain: What causes it?
- Antidepressants: Can they stop working?
- MAOIs and diet: Is it necessary to restrict tyramine?
- Electroconvulsive therapy (ECT)
- Psychotherapy
- Transcranial magnetic stimulation
- Vagus nerve stimulation
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Depression generally isn't a disorder that you can treat on your own. But in addition to professional treatment, these self-care steps can help:
- Stick to your treatment plan. Don't skip psychotherapy sessions or appointments. Even if you're feeling well, don't skip your medications. If you stop, depression symptoms may come back, and you could also experience withdrawal-like symptoms. Recognize that it will take time to feel better.
- Learn about depression. Education about your condition can empower you and motivate you to stick to your treatment plan. Encourage your family to learn about depression to help them understand and support you.
- Pay attention to warning signs. Work with your doctor or therapist to learn what might trigger your depression symptoms. Make a plan so that you know what to do if your symptoms get worse. Contact your doctor or therapist if you notice any changes in symptoms or how you feel.
 Ask relatives or friends to help watch for warning signs.
Ask relatives or friends to help watch for warning signs. - Avoid alcohol and recreational drugs. It may seem like alcohol or drugs lessen depression symptoms, but in the long run they generally worsen symptoms and make depression harder to treat. Talk with your doctor or therapist if you need help with alcohol or substance use.
- Take care of yourself. Eat healthy, be physically active and get plenty of sleep. Consider walking, jogging, swimming, gardening or another activity that you enjoy. Sleeping well is important for both your physical and mental well-being. If you're having trouble sleeping, talk to your doctor about what you can do.
More Information
- Depression (major depressive disorder) care at Mayo Clinic
- Depression, anxiety and exercise
Alternative medicine
Alternative medicine is the use of a nonconventional approach instead of conventional medicine. Complementary medicine is a nonconventional approach used along with conventional medicine — sometimes called integrative medicine.
Make sure you understand the risks as well as possible benefits if you pursue alternative or complementary therapy. Don't replace conventional medical treatment or psychotherapy with alternative medicine. When it comes to depression, alternative treatments aren't a substitute for medical care.
Supplements
Examples of supplements that are sometimes used for depression include:
- St. John's wort. Although this herbal supplement isn't approved by the Food and Drug Administration (FDA) to treat depression in the U.S., it may be helpful for mild or moderate depression. But if you choose to use it, be careful — St. John's wort can interfere with a number of medications, such as heart drugs, blood-thinning drugs, birth control pills, chemotherapy, HIV/AIDS medications and drugs to prevent organ rejection after a transplant. Also, avoid taking St. John's wort while taking antidepressants because the combination can cause serious side effects.
- SAMe.
 Pronounced "sam-E," this dietary supplement is a synthetic form of a chemical that occurs naturally in the body. The name is short for S-adenosylmethionine (es-uh-den-o-sul-muh-THIE-o-neen). SAMe isn't approved by the FDA to treat depression in the U.S. It may be helpful, but more research is needed. SAMe may trigger mania in people with bipolar disorder.
Pronounced "sam-E," this dietary supplement is a synthetic form of a chemical that occurs naturally in the body. The name is short for S-adenosylmethionine (es-uh-den-o-sul-muh-THIE-o-neen). SAMe isn't approved by the FDA to treat depression in the U.S. It may be helpful, but more research is needed. SAMe may trigger mania in people with bipolar disorder. - Omega-3 fatty acids. These healthy fats are found in cold-water fish, flaxseed, flax oil, walnuts and some other foods. Omega-3 supplements are being studied as a possible treatment for depression. While considered generally safe, in high doses, omega-3 supplements may interact with other medications. More research is needed to determine if eating foods with omega-3 fatty acids can help relieve depression.
Nutritional and dietary products aren't monitored by the FDA the same way medications are. You can't always be certain of what you're getting and whether it's safe. Also, because some herbal and dietary supplements can interfere with prescription medications or cause dangerous interactions, talk to your doctor or pharmacist before taking any supplements.
Mind-body connections
Integrative medicine practitioners believe the mind and body must be in harmony for you to stay healthy. Examples of mind-body techniques that may be helpful for depression include:
- Acupuncture
- Relaxation techniques such as yoga or tai chi
- Meditation
- Guided imagery
- Massage therapy
- Music or art therapy
- Spirituality
- Aerobic exercise
Relying solely on these therapies is generally not enough to treat depression. They may be helpful when used in addition to medication and psychotherapy.
More Information
- Depression (major depressive disorder) care at Mayo Clinic
- Natural remedies for depression: Are they effective?
Coping and support
Talk with your doctor or therapist about improving your coping skills, and try these tips:
- Simplify your life. Cut back on obligations when possible, and set reasonable goals for yourself.
 Give yourself permission to do less when you feel down.
Give yourself permission to do less when you feel down. - Write in a journal. Journaling, as part of your treatment, may improve mood by allowing you to express pain, anger, fear or other emotions.
- Read reputable self-help books and websites. Your doctor or therapist may be able to recommend books or websites to read.
- Locate helpful groups. Many organizations, such as the National Alliance on Mental Illness (NAMI) and the Depression and Bipolar Support Alliance, offer education, support groups, counseling and other resources to help with depression. Employee assistance programs and religious groups also may offer help for mental health concerns.
- Don't become isolated. Try to participate in social activities, and get together with family or friends regularly. Support groups for people with depression can help you connect to others facing similar challenges and share experiences.

- Learn ways to relax and manage your stress. Examples include meditation, progressive muscle relaxation, yoga and tai chi.
- Structure your time. Plan your day. You may find it helps to make a list of daily tasks, use sticky notes as reminders or use a planner to stay organized.
- Don't make important decisions when you're down. Avoid decision-making when you're feeling depressed, since you may not be thinking clearly.
Preparing for your appointment
You may see your primary care doctor, or your doctor may refer you to a mental health professional. Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, make a list of:
- Any symptoms you've had, including any that may seem unrelated to the reason for your appointment
- Key personal information, including any major stresses or recent life changes
- All medications, vitamins or other supplements that you're taking, including dosages
- Questions to ask your doctor or mental health professional
Take a family member or friend along, if possible, to help you remember all of the information provided during the appointment.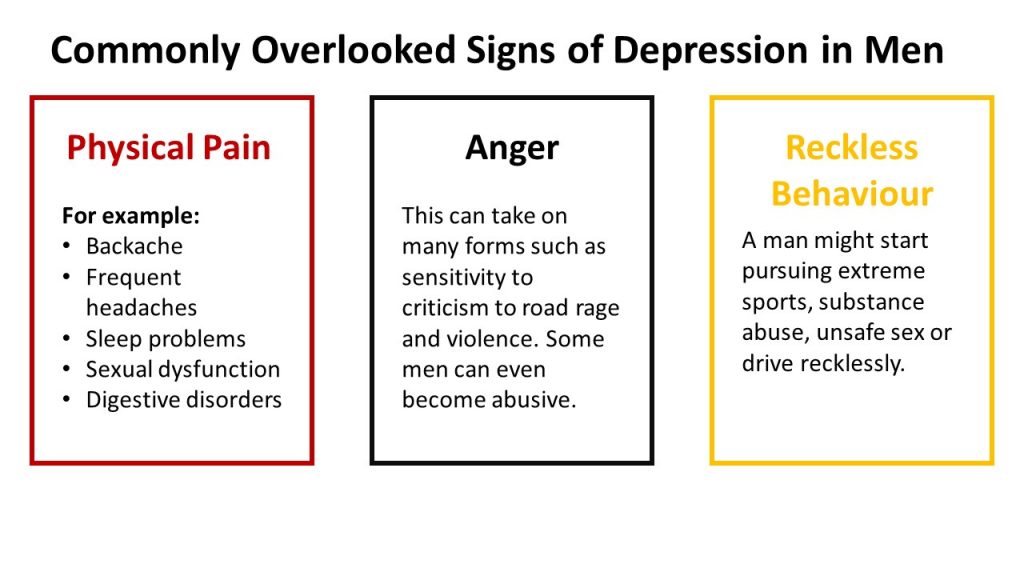
Some basic questions to ask your doctor include:
- Is depression the most likely cause of my symptoms?
- What are other possible causes for my symptoms?
- What kinds of tests will I need?
- What treatment is likely to work best for me?
- What are the alternatives to the primary approach that you're suggesting?
- I have these other health conditions. How can I best manage them together?
- Are there any restrictions that I need to follow?
- Should I see a psychiatrist or other mental health professional?
- What are the main side effects of the medications you're recommending?
- Is there a generic alternative to the medicine you're prescribing?
- Are there any brochures or other printed material that I can have? What websites do you recommend?
Don't hesitate to ask other questions during your appointment.
What to expect from your doctor
Your doctor will likely ask you a number of questions. Be ready to answer them to reserve time to go over any points you want to focus on. Your doctor may ask:
Be ready to answer them to reserve time to go over any points you want to focus on. Your doctor may ask:
- When did you or your loved ones first notice your symptoms of depression?
- How long have you felt depressed? Do you generally always feel down, or does your mood fluctuate?
- Does your mood ever swing from feeling down to feeling intensely happy (euphoric) and full of energy?
- Do you ever have suicidal thoughts when you're feeling down?
- Do your symptoms interfere with your daily life or relationships?
- Do you have any blood relatives with depression or another mood disorder?
- What other mental or physical health conditions do you have?
- Do you drink alcohol or use recreational drugs?
- How much do you sleep at night? Does it change over time?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
By Mayo Clinic Staff
NIMH » Depression
Overview
Depression (also called major depressive disorder or clinical depression) is a common but serious mood disorder.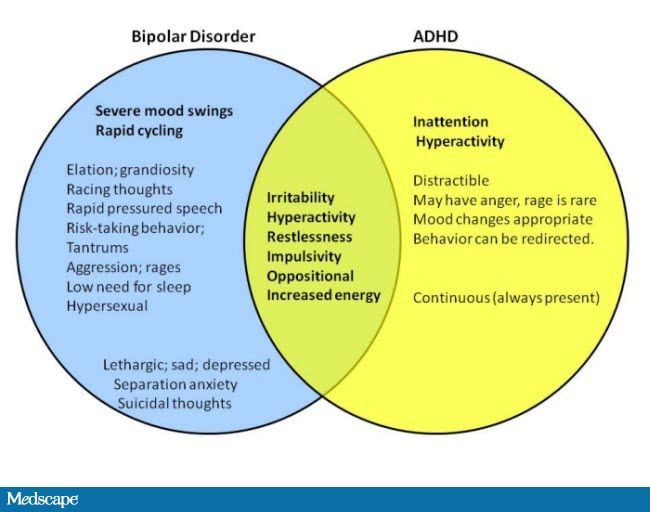 It causes severe symptoms that affect how you feel, think, and handle daily activities, such as sleeping, eating, or working.
It causes severe symptoms that affect how you feel, think, and handle daily activities, such as sleeping, eating, or working.
To be diagnosed with depression, the symptoms must be present for at least two weeks.
There are different types of depression, some of which develop due to specific circumstances.
- Major depression, which includes symptoms of depression most of the time for at least 2 weeks that typically interfere with one’s ability to work, sleep, study, and eat.
- Persistent depressive disorder (also called dysthymia), which often includes less severe symptoms of depression that last much longer, typically for at least 2 years.
- Perinatal depression, which occurs when a woman experiences major depression during pregnancy or after delivery (postpartum depression).
- Seasonal affective disorder, which comes and goes with the seasons, typically starting in late fall and early winter and going away during spring and summer.

- Depression with symptoms of psychosis, which is a severe form of depression where a person experiences psychosis symptoms, such as delusions (disturbing, false fixed beliefs) or hallucinations (hearing or seeing things that others do not see or hear).
Individuals with bipolar disorder (formerly called manic depression or manic-depressive illness) also experience depressive episodes, in which they feel sad, indifferent, or hopeless, combined with a very low activity level. But a person with bipolar disorder also experiences manic episodes, or unusually elevated moods in which the individual might feel very happy, irritable, or “up,” with a marked increase in activity level.
Examples of other types of depressive disorders newly added to the diagnostic classification of Diagnostic and Statistical Manual of Mental Disorders (DSM-5) include disruptive mood dysregulation disorder (diagnosed in children and adolescents) and premenstrual dysphoric disorder (PMDD).
Signs and Symptoms
The Centers for Disease Control and Prevention (CDC) has recognized that having certain mental disorders, including depression and schizophrenia, can make people more likely to get severely ill from COVID-19. Learn more about getting help and finding a health care provider on NIMH's Help for Mental Illnesses webpage.
If you have been experiencing some of the following signs and symptoms most of the day, nearly every day, for at least two weeks, you may be suffering from depression:
- Persistent sad, anxious, or “empty” mood
- Feelings of hopelessness, or pessimism
- Feelings of irritability, frustration, or restlessness
- Feelings of guilt, worthlessness, or helplessness
- Loss of interest or pleasure in hobbies and activities
- Decreased energy, fatigue, or feeling "slowed down"
- Difficulty concentrating, remembering, or making decisions
- Difficulty sleeping, early morning awakening, or oversleeping
- Changes in appetite or unplanned weight changes
- Thoughts of death or suicide, or suicide attempts
- Aches or pains, headaches, cramps, or digestive problems without a clear physical cause that do not ease even with treatment
- Suicide attempts or thoughts of death or suicide
Not everyone who is depressed experiences every symptom. Some people experience only a few symptoms while others may experience many. Several persistent symptoms in addition to low mood are required for a diagnosis of major depression, but people with only a few – but distressing – symptoms may benefit from treatment as well. The severity and frequency of symptoms and how long they last will vary depending on the individual and his or her particular illness. Symptoms may also vary depending on the stage of the illness.
Some people experience only a few symptoms while others may experience many. Several persistent symptoms in addition to low mood are required for a diagnosis of major depression, but people with only a few – but distressing – symptoms may benefit from treatment as well. The severity and frequency of symptoms and how long they last will vary depending on the individual and his or her particular illness. Symptoms may also vary depending on the stage of the illness.
Risk Factors
Depression is one of the most common mental disorders in the United States. Research suggests that genetic, biological, environmental, and psychological factors play a role in depression.
Depression can happen at any age, but often begins in adulthood. Depression is now recognized as occurring in children and adolescents, although it sometimes presents with more prominent irritability than low mood. Many chronic mood and anxiety disorders in adults begin as high levels of anxiety in children.
Depression, especially in midlife or older adults, can co-occur with other serious medical illnesses, such as diabetes, cancer, heart disease, and Parkinson’s disease. These conditions are often worse when depression is present, and research suggests that people who have depression and another medical illness tend to have more severe symptoms of both illnesses. Sometimes medications taken for these physical illnesses may cause side effects that contribute to depression. A doctor experienced in treating these complicated illnesses can help work out the best treatment strategy.
Risk factors include:
- Personal or family history of depression
- Major life changes, trauma, or stress
- Certain physical illnesses and medications
Treatment and Therapies
Depression, even the most severe cases, can be treated. The earlier treatment begins, the more effective it is. Depression is usually treated with medications, psychotherapy, or a combination of the two.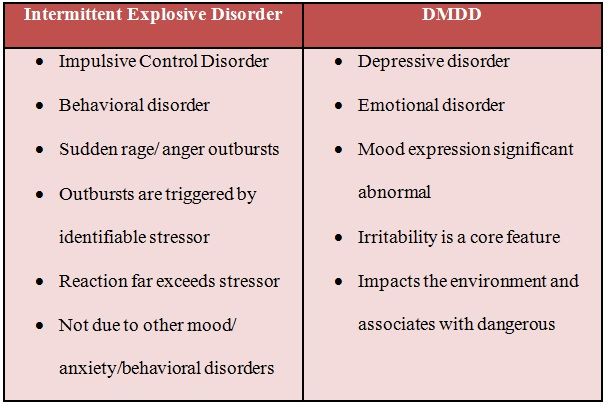 If these treatments do not reduce symptoms, electroconvulsive therapy (ECT) and other brain stimulation therapies may be options to explore.
If these treatments do not reduce symptoms, electroconvulsive therapy (ECT) and other brain stimulation therapies may be options to explore.
Quick Tip: No two people are affected the same way by depression and there is no "one-size-fits-all" for treatment. It may take some trial and error to find the treatment that works best for you.
Medications
Antidepressants are medicines commonly used to treat depression. They may help improve the way your brain uses certain chemicals that control mood or stress. You may need to try several different antidepressant medicines before finding the one that improves your symptoms and has manageable side effects. A medication that has helped you or a close family member in the past will often be considered.
Antidepressants take time – usually 4 to 8 weeks – to work, and often, symptoms such as sleep, appetite, and concentration problems improve before mood lifts, so it is important to give medication a chance before deciding whether it works.
If you begin taking antidepressants, do not stop taking them without talking to your health care provider. Sometimes people taking antidepressants feel better and then stop taking the medication on their own, and the depression returns. When you and your health care provider have decided it is time to stop the medication, usually after a course of 6 to 12 months, the health care provider will help you slowly and safely decrease your dose. Stopping them abruptly can cause withdrawal symptoms.
Please Note: In some cases, children, teenagers, and young adults under 25 may experience an increase in suicidal thoughts or behavior when taking antidepressants, especially in the first few weeks after starting or when the dose is changed. This warning from the U.S. Food and Drug Administration (FDA) also says that patients of all ages taking antidepressants should be watched closely, especially during the first few weeks of treatment.
If you are considering taking an antidepressant and you are pregnant, planning to become pregnant, or breastfeeding, talk to your health care provider about any increased health risks to you or your unborn or nursing child.
To find the latest information about antidepressants, talk to your health care provider and visit the FDA website.
Psychotherapies
Several types of psychotherapy (also called “talk therapy” or "counseling") can help people with depression by teaching new ways of thinking and behaving and how to change habits that contribute to depression. Examples of evidence-based approaches specific to the treatment of depression include cognitive-behavioral therapy (CBT) and interpersonal therapy (IPT). More information on psychotherapy is available on the NIMH Psychotherapies webpage.
Brain Stimulation Therapies
If medications do not reduce the symptoms of depression, electroconvulsive therapy (ECT) may be an option to explore. Based on the latest research:
- ECT can provide relief for people with severe depression who have not been able to feel better with other treatments.
- Electroconvulsive therapy can be an effective treatment for depression. In some severe cases where a rapid response is necessary or medications cannot be used safely, ECT can even be a first-line intervention.

- Once strictly an inpatient procedure, today ECT is often performed on an outpatient basis. The treatment consists of a series of sessions, typically three times a week, for two to four weeks.
- ECT may cause some side effects, including confusion, disorientation, and memory loss. Usually these side effects are short-term, but sometimes memory problems can linger, especially for the months around the time of the treatment course. Advances in ECT devices and methods have made modern ECT safe and effective for most patients. Talk to your doctor and make sure you understand the potential benefits and risks of the treatment before giving your informed consent to undergoing ECT.
- ECT is not painful, and you cannot feel the electrical impulses. Before ECT begins, a patient is put under brief anesthesia and given a muscle relaxant. Within one hour after the treatment session, which takes only a few minutes, the patient is awake and alert.
Other more recently introduced types of brain stimulation therapies used to treat medicine-resistant depression include repetitive transcranial magnetic stimulation (rTMS) and vagus nerve stimulation (VNS). Other types of brain stimulation treatments are under study. You can learn more about these therapies on the NIMH Brain Stimulation Therapies webpage.
Other types of brain stimulation treatments are under study. You can learn more about these therapies on the NIMH Brain Stimulation Therapies webpage.
Natural Products
FDA has not approved any natural products for depression. While research is ongoing, some people find natural products, including vitamin D and the herbal dietary supplement St. John’s wort, to help depression. Do not use St. John’s wort or other dietary supplements for depression before talking to your provider. For more information, visit the National Center for Complementary and Integrative Health website.
How can I find help?
If you think you may have depression, start by making an appointment to see your health care provider. This could be your primary care practitioner or a health provider who specializes in diagnosing and treating mental health conditions. Visit the NIMH Find Help for Mental Illnesses webpage if you are unsure of where to start.
Beyond Treatment: Things You Can Do
Once you begin treatment, you should gradually start to feel better. Here are other tips that may help you or a loved one during treatment for depression:
Here are other tips that may help you or a loved one during treatment for depression:
- Try to get some physical activity. Just 30 minutes a day of walking can boost mood.
- Try to maintain a regular bedtime and wake-up time.
- Eat regular, healthy meals.
- Do what you can as you can. Decide what must get done and what can wait.
- Try to connect with other people, and talk with people you trust about how you are feeling.
- Postpone important decisions, such as getting married or divorced, or changing jobs until you feel better.
- Avoid using alcohol, nicotine, or drugs, including medications not prescribed for you.
Join a Study
Clinical trials are research studies that look at new ways to prevent, detect, or treat diseases and conditions. The goal of clinical trials is to determine if a new test or treatment works and is safe. Although individuals may benefit from being part of a clinical trial, participants should be aware that the primary purpose of a clinical trial is to gain new scientific knowledge so that others may receive better help in the future.
Researchers at NIMH and around the country conduct many studies with patients and healthy volunteers. We have new and better treatment options today because of what clinical trials have uncovered. Talk to your health care provider about clinical trials, their benefits and risks, and whether one is right for you.
To learn more or find a study, visit:
- NIMH’s Clinical Trials webpage: Information about participating in clinical trials
- Clinicaltrials.gov: Current Studies on Depression: List of clinical trials funded by the National Institutes of Health (NIH) being conducted across the country
- Join a Study: Depression – Adults: List of studies currently recruiting adults with depression being conducted on the NIH Campus in Bethesda, MD
- Join a Study: Depression – Children: List of studies currently recruiting children with depression being conducted on the NIH Campus in Bethesda, MD
- Join a Study: Perimenopause-Related Mood Disorders: List of studies on perimenopause-related mood disorders being conducted on the NIH Campus in Bethesda, MD
- Join a Study: Postpartum Depression: List of studies on postpartum depression being conducted on the NIH Campus in Bethesda, MD
Learn More
Free Brochures and Shareable Resources
- Chronic Illness and Mental Health: Recognizing and Treating Depression: This brochure provides information about depression and mental health for people living with chronic illnesses, including children and adolescents.
 It discusses symptoms, risk factors and treatment options.
It discusses symptoms, risk factors and treatment options. - Depression: This brochure provides information about depression including the different types of depression, signs and symptoms, how it is diagnosed, treatment options, and how to find help for yourself or a loved one.
- Depression in Women: 5 Things You Should Know: This brochure provides information about depression in women including signs and symptoms, types of depression unique to women, treatment options, and how to find help.
- Men and Depression: Men and women may experience depression very differently. This brochure describes common signs and symptoms, and treatment options for depression in men.
- Perinatal Depression: This brochure provides information about perinatal depression including how it differs from the “baby blues”, causes, signs and symptoms, treatment options, and how you or a loved one can get help.
- Seasonal Affective Disorder: This fact sheet includes a description of seasonal affective disorder (SAD), signs and symptoms, how SAD is diagnosed, causes, and treatment options.

- Seasonal Affective Disorder: More Than the Winter Blues: This infographic provides information about how to recognize the symptoms of SAD and what to do to get help.
- Teen Depression: More Than Just Moodiness: This fact sheet is intended for teens and young adults and presents information about how to recognize the symptoms of depression and how to get help.
- Shareable Resources on Depression: Help support depression awareness and education in your community. Use these digital resources, including graphics and messages, to spread the word about depression.
Federal Resources
- Depression (MedlinePlus - also en español)
- Moms’ Mental Health Matter: Depression and Anxiety Around Pregnancy (National Institute of Child Health and Human Development)
Research and Statistics
- Journal Articles: This webpage provides information on references and abstracts from MEDLINE/PubMed (National Library of Medicine).

- Statistics: Major Depression: This webpage provides information on the statistics currently available on the prevalence and treatment of depression among people in the United States.
Multimedia
- NIMH Experts Discuss the Menopause Transition and Depression: Learn about the signs, symptoms, treatments, and latest research.
- Mental Health Minute: Depression: Take a mental health minute to watch this video on depression.
- NIMH Expert Discusses Seasonal Affective Disorder (SAD): Learn about the signs, symptoms, treatments, and latest research on SAD.
- Discover NIMH: Personalized and Targeted Brain Stimulation Therapies: Brain stimulation therapies can be effective treatments for people with depression and other mental disorders. NIMH is supporting studies exploring how to make brain stimulation therapies more personalized while reducing side effects.
 This video describes transcranial magnetic stimulation and electroconvulsive therapy for treatment-resistant depression.
This video describes transcranial magnetic stimulation and electroconvulsive therapy for treatment-resistant depression. - Discover NIMH: Drug Discovery and Development: One of the most exciting recent breakthroughs from research funded by the NIMH is the development of a fast-acting medication for treatment-resistant depression based on ketamine. This video shares the story of one of the patients participating in a NIMH clinical trial, and how ketamine infusions changed her life and gave her a sense of purpose. In addition, Dr. Carlos Zarate, a senior clinical investigator in NIMH’s Intramural Research Program, describes his groundbreaking research on ketamine.
Last Reviewed: September 2022
Unless otherwise specified, NIMH information and publications are in the public domain and available for use free of charge. Citation of NIMH is appreciated. Please see our Citing NIMH Information and Publications page for more information.
Depression is not just a constant decline in mood, pessimism and a desire for solitude. This is a mental disorder that leads to serious consequences. The patient loses the ability to enjoy life, he is not given the solution of difficult problems, he is prone to negative outcomes from any situation. But this condition can be corrected, depression is curable.
Vidkriti Zgornuti
Types of depression
Depression is not always perceived as a disease not only by the patient's relatives, but also by himself. A bad mood lasts for weeks, everything is seen in gloomy colors, you don’t want to move, but you want to hide in a corner and just lie. The patient is accused of deterioration of character, selfishness and laziness. And he needs help. Help of a specialist. nine0003
Such help can be needed at any age. Five out of a hundred teenagers and children are familiar with this condition.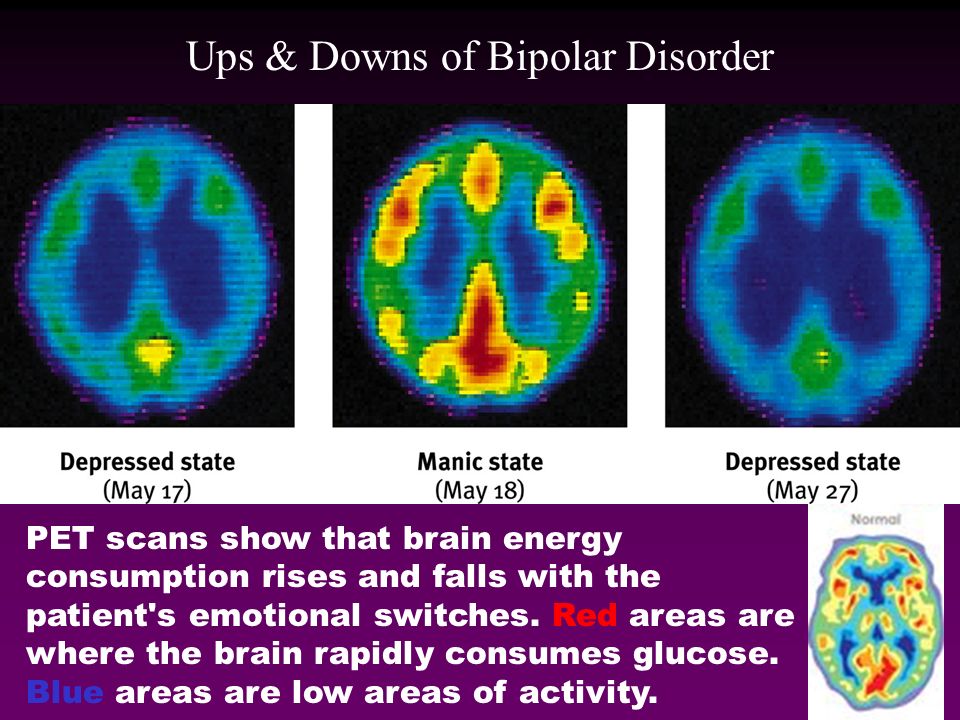 With age, the number of cases also increases among young people - from 15 to 40%. Among adults, depressive disorders occur in one in ten, and women are twice as likely to experience this disorder. At an older age, about 30% of people have ever been depressed.
With age, the number of cases also increases among young people - from 15 to 40%. Among adults, depressive disorders occur in one in ten, and women are twice as likely to experience this disorder. At an older age, about 30% of people have ever been depressed.
Depression as an illness can take many forms.
Depressive episode
This is the most common form of the disorder. Its duration is from two weeks to a year. If such a disorder is recorded only once, it is called unipolar. About 33% of patients experience this condition only once in their lives. As a rule, a depressive disorder is accompanied by a decrease in working capacity. Lack of treatment can lead to relapse.
Periodic depressive disorder
Characterized by recurring episodes. It is also called recurrent, as well as classical or clinical depression. It usually first occurs in childhood or adolescence. Duration from several months to several years. Phases of the disease alternate with remission. Seriously affects working capacity and requires an appeal to a child psychologist in the early stages of the development of the disease. nine0003
Seriously affects working capacity and requires an appeal to a child psychologist in the early stages of the development of the disease. nine0003
Dysthymia
Duration from two years to decades. Although the symptoms are less severe than in recurrent disorder, they last longer. Dysthymia is also called chronic depression. The transition of this type to a severe form is called a double depression.
Bipolar depression type I
It is characterized by a change in the phases of the disease, remission and manic phases. This disorder is also called manic-depressive psychosis. When the patient goes through the last phase, he is characterized by hyperactivity, combined with a good mood, but at the same time with anxiety and insomnia. The patient loses the ability to think critically. As a result - financial problems, the risk of casual sex. After this phase, the patient becomes depressed. This is bipolar disorder. nine0003
Bipolar II depression
Similar to depressive episodes.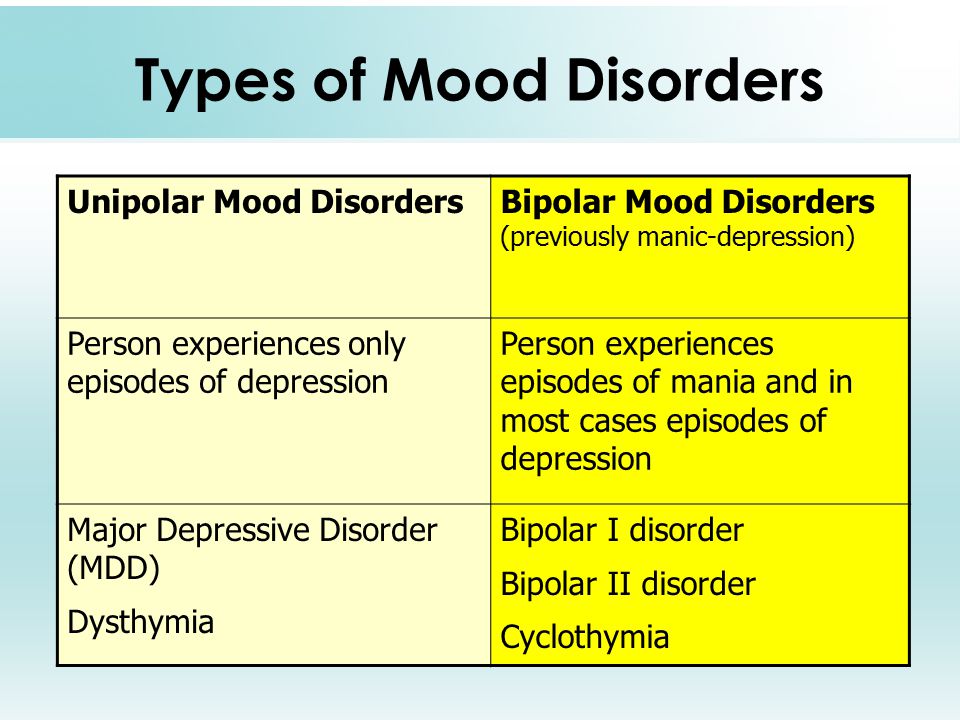 Changes of phases are also observed, but without an excessive increase in mood. During remission, there is an illusion of recovery.
Changes of phases are also observed, but without an excessive increase in mood. During remission, there is an illusion of recovery.
Depressive psychotic episode
With this disorder, hallucinations, delusions are observed. Such patients in most cases require hospitalization.
Atypical depression
A mild type of depression, accompanied by drowsiness and excessive eating, mood swings, hypersensitivity, a tendency to panic attacks. nine0003
Seasonal depressive disorders
Occur most often in autumn or winter. They pass when the season changes.
Vidkriti Zgornuti
Causes of depression
There is no single point of view among doctors on the causes of depression. Allocate the influence of heredity, as well as the environment. Nearly half of people with depression have close relatives with the same condition. There is a high probability of illness of one of the identical twins if the second is sick. nine0003
nine0003
Depression can also be caused by external factors. It can be stress caused by the loss of a loved one, loss of a job, divorce. Those who have previously suffered from depression are also at risk. People with a passive life position, with increased anxiety, with mental disorders are also more likely to get sick.
A high risk of depression in women is associated with stress and increased emotionality. And also, with some features of female physiology, for example, a tendency to thyroid dysfunction, hormonal changes during the menstrual cycle and menopause. Also, pregnancy and the postpartum period due to increased stress on the body can lead to postpartum depression. nine0003
Vidkriti Zgornuti
Depression can also be caused by a number of diseases, such as:
- Thyroid diseases
- Diseases of the adrenal glands
- Brain tumors
- Stroke
- AIDS
- Multiple sclerosis
- Parkinson's disease, etc.

Vidkriti Zgornuti
The development of the disease can be caused by uncontrolled intake of certain drugs, alcoholism and drug addiction. nine0003
Signs and symptoms of depression
Signs of depression are divided into 4 groups:
1. Emotional.
Depressed mood, impaired activity, decreased interest in life, insomnia or hypersomnia, psychomotor agitation or lethargy, fatigue, loss of energy, recurrent thoughts of death or suicide, suicide attempts, low self-esteem, impaired concentration, difficulty making decisions, hopelessness .
2. Physiological.
Cognitive, psychomotor and other types of dysfunctions, increased fatigue, decreased sexual desire, loss of interest or pleasure in previously enjoyable activities, sleep disturbances, decreased or increased appetite, body pain, constipation.
3. Behavioral.
Anxiety, tension, nervousness, irritability, anger, mood swings, bouts of sadness, tearfulness, exacerbation of interpersonal conflicts, passivity, a tendency to solitude, abandonment of former hobbies, craving for alcohol and psychotropic substances. nine0003
nine0003
4. Thinking.
Inability to concentrate, make a decision, slow thinking, pessimism.
Vidkriti Zgornuti
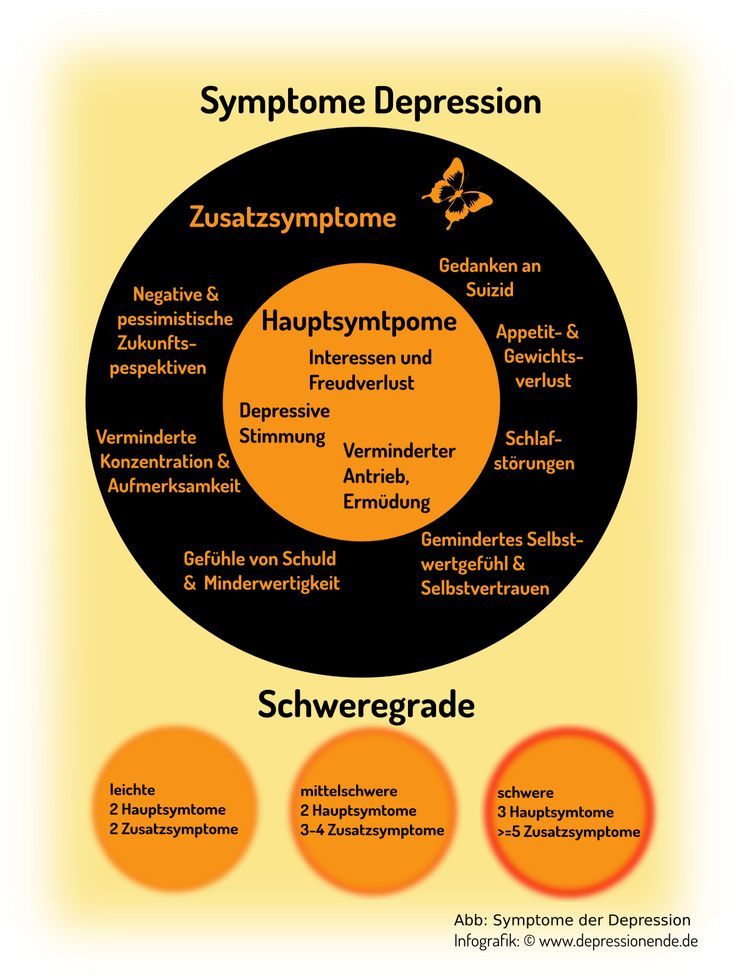
Symptoms of depression are divided into major and minor.
The main ones are:
- deterioration in mood without external causes for at least two weeks;
- increased fatigue for at least a month;
- persistent loss of interest from favorite activities. nine0077
- pessimism;
- suicidal thoughts;
- feelings of depression, attacks of fear or guilt;
- drop in self-esteem;
- any disturbance of sleep and appetite.
- sleep at least 8 hours, be sure to go to bed before midnight;
- diet with enough omega-3 fatty acids;
- sufficient physical activity;
- communication with friends, with people who are positive;
- it is highly desirable to receive psychotherapeutic assistance; nine0064
- maximum use of daylight hours, if necessary, light therapy.
- World Health Organization
- Ministry of Health of Ukraine
- Public Health Center of the Ministry of Health of Ukraine
Vidkriti Zgornuti
Additional symptoms of depression include:
Vidkriti Zgornuti
The presence of two main and three additional symptoms of depression in a patient allows making an appropriate diagnosis.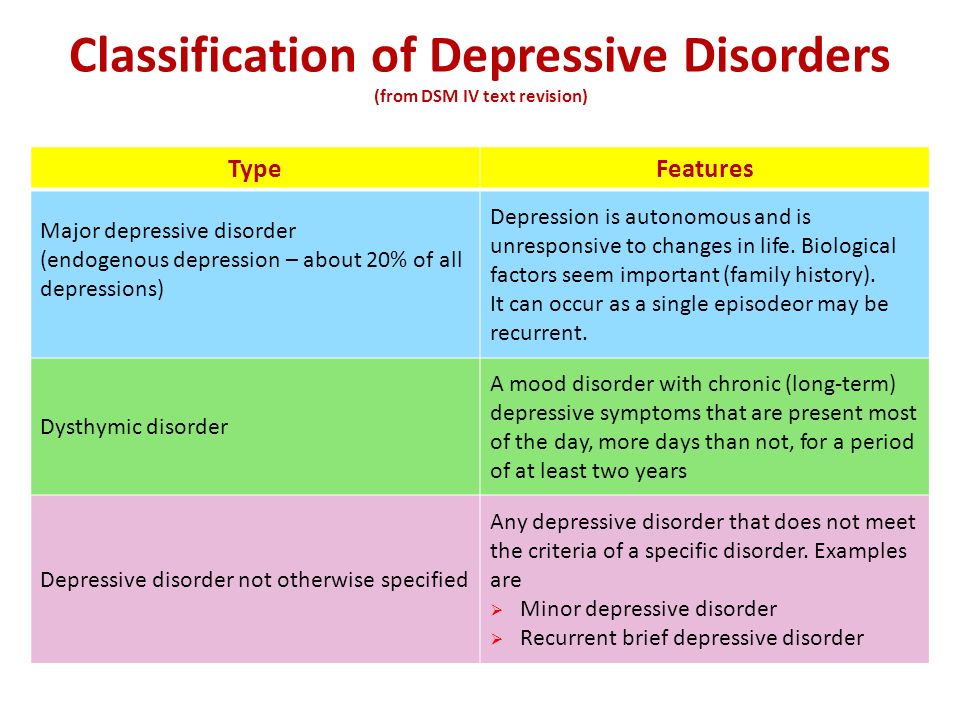
Depression in children has its own characteristics. Young children tend to feign illness in order to skip school or kindergarten, they are dependent on their parents and tormented by the fear of their death. Older children are constantly in a bad mood, their academic performance decreases, they perceive everything “with hostility” and complain of misunderstanding. The complexity of the diagnosis lies in the fact that sometimes it is not easy to separate the signs of depression and growth difficulties. In such cases, professional advice should not be abandoned. nine0003
Vidkriti Zgornuti
Sequelae of depression
If treatment is refused, the consequences of depression can be severe. With each episode of untreated depression, the risk of a recurrence of the disease increases. In addition, each subsequent episode will be more difficult, with greater loss of performance and negative impact on physical health. Episodes will occur with increasing frequency, and cases of prolonged depression are possible. If treatment for depression has been incorrect or incomplete, it can lead to the development of a form of the disease that is difficult to treat. nine0003
If treatment for depression has been incorrect or incomplete, it can lead to the development of a form of the disease that is difficult to treat. nine0003
Vidkriti Zgornuti
Diagnosis of depression
When diagnosing depression, it is important to rule out diseases that present with similar symptoms, such as viral infections. To do this, the patient must undergo a routine physical examination and pass tests.
After ruling out other problems, a psychological evaluation is carried out. The patient is being interviewed. Diagnosis of depression is carried out using special tests that reveal the level of anxiety, suicidal tendencies, anhedonia and other symptoms. nine0003
Vidkriti Zgornuti
Treatment of depression
Treatment of depression begins with psychological help. The patient is set up for an optimistic outlook on life, helps to get out of a state of constant fixation on negative aspects.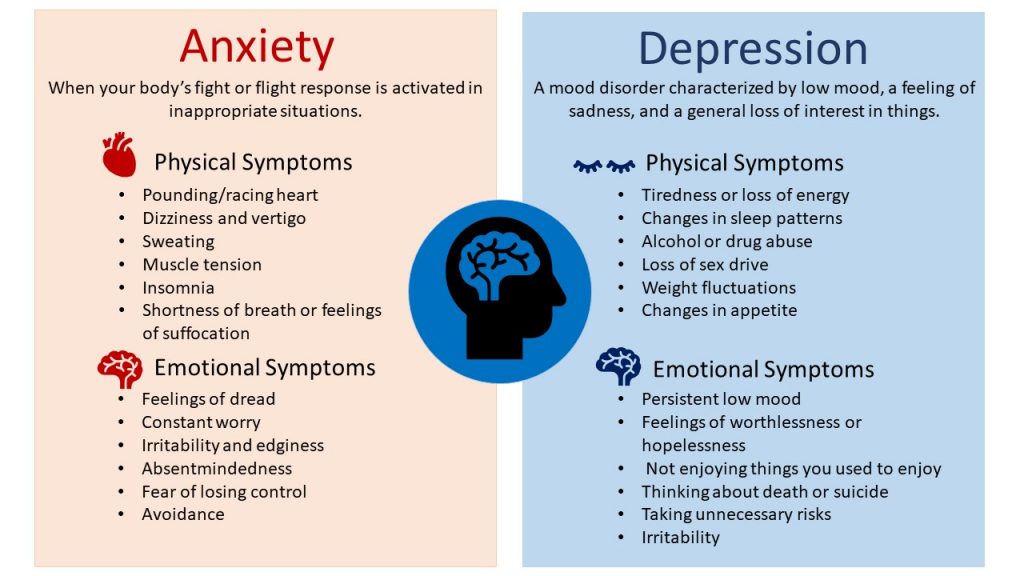 The doctor also works with family members. They must establish a benevolent climate, support the patient in everything.
The doctor also works with family members. They must establish a benevolent climate, support the patient in everything.
Tactics of treatment depends on the condition of the patient. Treatment is carried out on an outpatient basis or in a hospital. Treatment includes psychotherapy, drug therapy and social therapy. Antidepressants are used to treat depression. Only a doctor can choose the right drug. After all, the group under the general name of antidepressants includes drugs of different effects - stimulating, removing anxiety, sedatives. The dosage is selected by the doctor individually. The action of drug therapy begins two weeks after administration, and they cannot be canceled on their own. The duration of treatment is determined only by the doctor. nine0003
Also, auxiliary methods are used in the treatment - art therapy, hypnotherapy, aromatherapy, light therapy, magnetotherapy, meditation. For each patient, an individual course of treatment is selected.
Vidkriti Zgornuti
Prevention of depression
The support of family and friends plays an important role in the treatment of depression. They should avoid criticism of the patient, offer him joint activities. If the patient trusts them, then it is worth talking about his condition, emphasizing that his condition is temporary, and the treatment will definitely give a positive effect. nine0003
They should avoid criticism of the patient, offer him joint activities. If the patient trusts them, then it is worth talking about his condition, emphasizing that his condition is temporary, and the treatment will definitely give a positive effect. nine0003
Since some types of depression recur, it is important to know how to prevent them. Prevention of depression is simple actions that give great results. Doctors advise:
Vidkriti Zgornuti
The article is for informational purposes only. Please remember: self-medication can harm your health.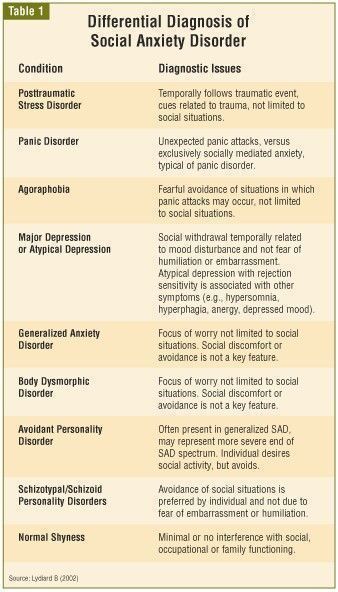
Vidkriti Zgornuti
Sources
Vidkriti Zgornuti
The author of the article:
Shulika Elena Valerievna
Psychotherapist, psychiatrist
Which doctor treats depression?
Where to go for help? Which doctor will help? It is better to start with a visit to a therapist. The general practitioner examines the patient, gives a referral for tests. The second specialist who will help is a psychotherapist.
Treatment of depression in Kyiv can be done at the MEDICOM clinic under the supervision of experienced specialists in comfortable clinics in Obolon and Pechersk. Do not stay with depression on your own. Contact the experts and return to a happy and healthy life as soon as possible! nine0003
show more
Certificates
Reviews
10/31/2022 16:35
Natalya Natalya
The article is built correctly, with a gradual disclosure of the topic. Disease is dealt with step by step. Forms of the disease, exemplary methods of treatment are indicated. For those who suspect that they have this disorder, the article gives a complete description in a brief form. This is of interest to start treatment with narrow specialists.
Disease is dealt with step by step. Forms of the disease, exemplary methods of treatment are indicated. For those who suspect that they have this disorder, the article gives a complete description in a brief form. This is of interest to start treatment with narrow specialists.
06/23/2022 10:15
Mary
Why do you have a psychologist and not a psychiatrist prescribing antidepressants in your clinic? Psychologists do not have the right to recognize whether they are medicines.
12.01.2022 01:16
Miroslava
My husband started having problems with his mood - everything is bad all the time, he is not interested in anything, he sees everything in a negative light. And I signed him up with a psychotherapist. At the consultation, pathopsychological and neuropsychological diagnostics were performed, after which it became clear that my husband had depression. Prescribed treatment with antidepressants, sessions of psychotherapy, magnetotherapy. Each case has its own treatment regimen. It's been a month and a half since the treatment started. Gradually, the negative and bad mood disappears, we will continue. nine0003
It's been a month and a half since the treatment started. Gradually, the negative and bad mood disappears, we will continue. nine0003
11/18/2021 20:22
Kubrak Masha
I liked the article, thank you! Very informative without complex medical terms, understandable for the perception of an ordinary person.
09/05/2021 09:06
To Svitlana
Depression is the greatest state of the soul, if nothing makes you happy. I experienced this stage a couple of times and I was helped several times to get a new one in the MEDIKOM clinic - my love psychologist Kulik Mariya Sergievna. Vaughn took antidepressants and gave psychological help. Shiro dyakuyu! nine0003
07/30/2021 19:27
Vladimir
Depression began after the death of his father, and was aggravated by a divorce from his wife. Became irritable, insomnia, always all in gloomy shades. Through the selection of drugs and work with a psychotherapist, colors began to appear in life.
05/07/2021 10:57
Love
I have postpartum depression after the birth of my long-awaited daughter. She couldn't figure it out on her own. A good psychologist works at the MEDICOM clinic. Without pills, I was able to help cope with depression - only herbal remedies and consultations. I begin to feel the happiness and joy of motherhood. Thanks a lot! nine0003
She couldn't figure it out on her own. A good psychologist works at the MEDICOM clinic. Without pills, I was able to help cope with depression - only herbal remedies and consultations. I begin to feel the happiness and joy of motherhood. Thanks a lot! nine0003
11.02.2021 17:17
Tetyana Oleksandrivna
The child began to notice a change in behavior and character development. No one knows anything, no wine is needed for anyone, everything is the opposite. I turned back to the psychologist for help, so that nothing bad happened. The doctor spent the interview with the son, prescribing calming preparations. Xing is slowly returning to normal.
04.11.2020 19:11
Nadya Reznichenko
For a long time I could not know the work behind the fah, problems with the person, my mother was sick. All in one compartment. Maria Sergievna Kulik helped me, I asked how you can change it, don’t pay attention to it, but look at it. I prescribed calmness, I relaxed, stopped sіpatisya and nervousness. You won't believe it after a couple of days, I knew the job! With a person, slowly getting better, trying to smooth out the kuti, even if it’s for the sake of strength. I took my mother to the Medicom to a good fakhivtsya, it was recognized as a likuvannya. Start thinking about yourself, hunt for help and help you! nine0003
You won't believe it after a couple of days, I knew the job! With a person, slowly getting better, trying to smooth out the kuti, even if it’s for the sake of strength. I took my mother to the Medicom to a good fakhivtsya, it was recognized as a likuvannya. Start thinking about yourself, hunt for help and help you! nine0003
Show 3 more
Total 9 reviews
give feedback
Types of depression - iFightDepression [EN]
There are different types of depression, which are different.
Signs and symptoms vary in number, time, severity and frequency, but are generally very similar. Because different types of depression are treated differently, it is important to pinpoint the type of depression. Depending on gender, age and cultural characteristics, people have different symptoms and severity of depression. nine0003
Neurotic, reactive (minor) depression is treated with psychotherapy.
Somatic and psychotic - medication. These terms are used by psychiatrists.
These terms are used by psychiatrists.
Studies have shown that depression has a phasic course. Periods of normal mood alternate with depressive episodes. Sometimes, instead of a depressive phase,
there may be a manic phase, which is manifested by irritability and high mood. If so, then it is not depression, but bipolar disorder (a more serious illness). nine0003
1. Depressive episode
The most common and typical form of depression is the depressive episode. An episode lasts from a few weeks to a year, but is always longer than 2 weeks. A single depressive episode is called a unipolar episode. Approximately one third of affected people experience only one episode, or "phase", during their lifetime. However, if a person does not receive appropriate treatment for depression, there is a risk of recurrent depressive episodes in the future. Depressive episodes always affect a person's performance to one degree or another. nine0003
2. Intermittent (recurrent) depressive disorder
When a depressive episode recurs, it is recurrent depressive disorder or major depressive disorder, which usually begins in adolescence or early adulthood.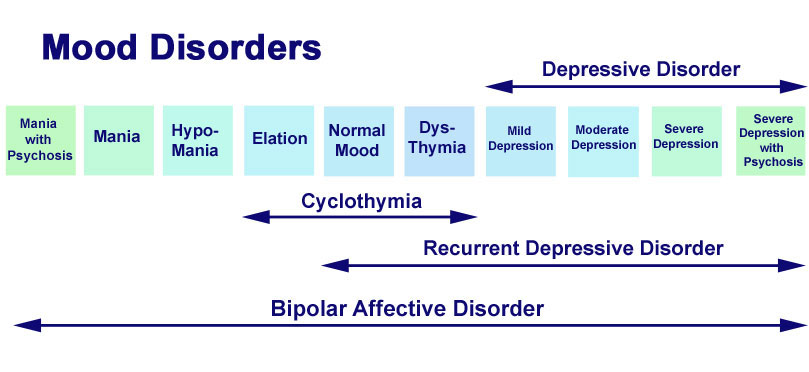 With this kind of depression, depressive phases, which can last from several months to several years, alternate with phases of normal mood. This type of depressive disorder can seriously affect performance and is unipolar in nature (no manic or hypomanic phase). This is the so-called "classic" or "clinical" depression. nine0003
With this kind of depression, depressive phases, which can last from several months to several years, alternate with phases of normal mood. This type of depressive disorder can seriously affect performance and is unipolar in nature (no manic or hypomanic phase). This is the so-called "classic" or "clinical" depression. nine0003
3. Dysthymia
Dysthymia presents with milder and less severe symptoms than a depressive episode or recurrent depression. However, the disorder is permanent, with symptoms lasting much longer, at least 2 years, sometimes decades, which is why it is called "chronic depression". This disorder is unipolar and also affects performance. This type of depression sometimes develops into a more severe form (major depressive episode) and if this happens it is called double depression. nine0003
4. Bipolar depression, type I
This is the type of depression in bipolar disorder, formerly called manic-depressive illness, and is less common than unipolar depression.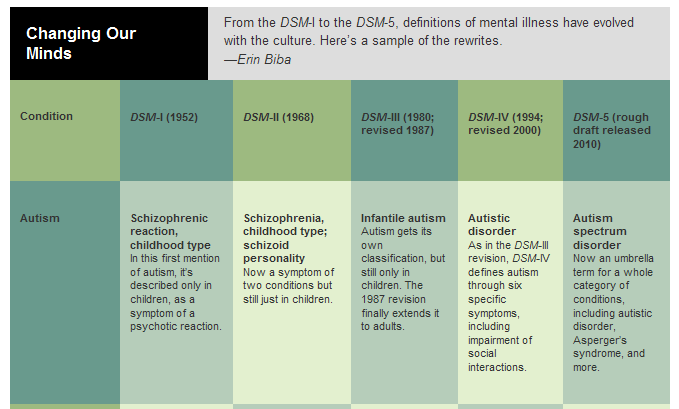 It consists of alternating depressive phases, phases of normal mood and so-called manic phases.
It consists of alternating depressive phases, phases of normal mood and so-called manic phases.
Manic phases are characterized by excessively high mood associated with hyperactivity, anxiety, and decreased need for sleep.
Mania affects thinking, judgment and social behavior causing serious problems and difficulties. When a person is in a manic phase, he makes frequent casual unsafe sex, makes unwise financial decisions. After a manic episode, such people often experience depression. nine0003
The best way to describe these "emotional upheavals" is "to be on top of the world and fall into the depths of despair".
Symptoms of the phases of depression in bipolar disorder are sometimes difficult to distinguish from unipolar depression.
5. Bipolar depression type II
More like recurrent depressive disorder than bipolar disorder. In this disorder, multiple depressive phases alternate with phases of mania, but with less pronounced euphoria. During these phases, family and loved ones may even mistakenly assume that the person is doing well. nine0003
nine0003
6. Mixed anxiety-depressive disorder
In anxiety-depressive disorder, the clinical picture is very similar to depression, however, in depression, depressive syndromes always come first. In this case, both anxious and depressive symptoms are evenly combined.
7. Depressive psychotic episode
A special form of depressive episode is psychotic or delusional depression. Psychosis is a condition in which people see or hear things that do not exist (hallucinations) and/or have false ideas or beliefs (delusions). There are various types of delusions such as self-accusation for no reason (delusion of guilt), financial ruin (delusions of poverty), feeling of an incomprehensible illness (hypochondriac delusions). People with delusional depression almost always require inpatient psychiatric treatment. Psychotic episodes can be either unipolar or bipolar. nine0003
8. Atypical depression
This type of depression is characterized by hypersensitivity and mood swings, overeating and drowsiness, panic attacks.