Borderline personality disorder spouse
How Do People with BPD Act in Relationships?
When a partner lives with borderline personality disorder, your relationship may at times feel cyclic. Learning about the condition can help you cope.
If you’ve been in a relationship with someone with borderline personality disorder (BPD), you may know things can get emotional and intense at times.
A BPD relationship cycle often consists of some emotional highs and lows that may leave you confused and frustrated.
You might also see your partner experience unexpected bouts of anger, anxiety, or depression. They may love you and then suddenly reject you or get upset.
Borderline personality is a formal mental health diagnosis. It isn’t a personal choice.
But everyone experiences BPD differently, so being in a relationship with someone with BPD can bring its own challenges.
There are different ways to manage these challenges, though, and learning more about the condition could help.
Emotional episodes or cycles are often a reality for people living with borderline personality disorder. This can impact relationships.
“A BPD relationship cycle refers to a repeating, continuous series of highs and lows in a relationship,” explains Tabitha Cranie, a retired MD from St. Petersburg, Florida. “First, everything feels good, uplifting, and safe — they might think of you as their favorite person.”
At the start of the relationship, your partner with BPD might tend to idealize you and everything you do.
They may focus all their attention on you, singing your praises, and demanding your attention. They might see only the positives and feel you correspond to their interest and feelings.
As the relationship progresses, idealization may decrease and give room to devaluation.
Your partner may suddenly feel as though you’re not participating in the relationship, don’t care enough, or aren’t meeting them halfway. They may start focusing on negative aspects or having a hard time feeling safe in the relationship.
This idealization and devaluation often occur through what’s informally known as the BPD relationship cycle, or the BPD breakup stages.
This doesn’t mean that everyone with borderline personality disorder acts in the same ways or repeats the same patterns. But there’s a possibility that some of these behaviors and attitudes are present in a relationship with someone with BPD.
The borderline personality relationship cycle may include six stages:
Stage one
Your partner may view you as “the one,” see you as a perfect partner, and prioritize you over other things. This could happen shortly after you’ve met or established a relationship.
They may be demanding of your time and appear fully invested in the relationship.
Stage two
Feelings of anxiety and fear of abandonment may start to appear in your partner.
They may become hypersensitive to some incidents, like a missed text or postponed date.
Symptoms of BPD like fear of abandonment or stress-related paranoid thoughts can make your partner believe these isolated incidents mean you’re no longer interested in the relationship or want to leave.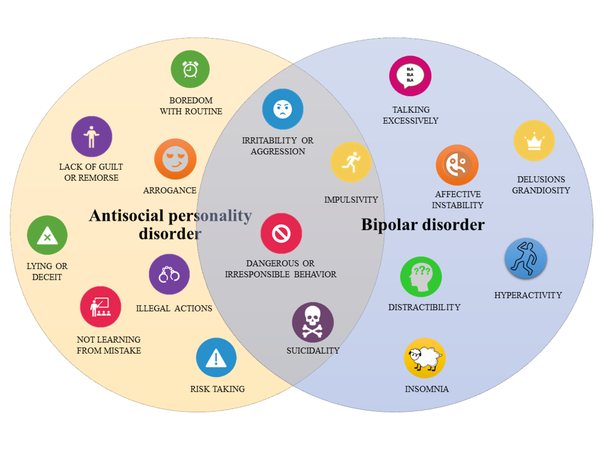
Stage three
In response to fears of abandonment, your partner may begin testing or pushing you away in small ways.
These tests can result in arguments and can be seen by your partner as a way of fighting for the relationship.
Stage four
Without satisfaction or sense of security from their efforts to test you, a partner living with BPD may resort to intentional distancing. They’ll try to emotionally leave you before you leave them.
This could be confusing for you and painful for them. It may even solidify their perception that the relationship is in trouble.
During this stage, your partner may fixate on thoughts that you’re going to leave, but they may hide these away, maintaining a façade that everything is OK. They could alternately ask you repeatedly to confirm your feelings and interest.
Stage five
If your partner lives with BPD but you remain unaware, this is the stage where the relationship may end.
You may not understand why things have been going downhill. You may feel significantly confused about the changes in your partner’s attitude and behavior.
You may feel significantly confused about the changes in your partner’s attitude and behavior.
Your partner living with BPD might try to suddenly explain everything as a last effort to save the bond.
Stage six
If the relationship is over, the partner living with BPD could spiral down into thoughts of low self-worth and experience symptoms of depression.
They may tell themselves they’re worthless or experience such volatile emotions that they engage in some behaviors that may put their safety in jeopardy.
They may also restart the relationship cycle, thinking about how perfect you were and wondering if they can get you back. They might attempt connecting again.
If the relationship doesn’t end, and you solve the challenges, they may also restart the cycle.
There is no set timeline for a BPD cycle.
It may take the person with borderline personality a few hours or a few days to go through stages. This doesn’t mean a BPD relationship will be short.
Cranie explains intense episodes of anxiety, depression, and anger may only last several hours and are then followed by a more emotionally stable period.
It may depend on:
- the support your partner has
- wherever or not they’re receiving formal treatment
- what other emotional resources they can rely on
Some BPD relationship cycles may take place over months or years, depending on the severity of symptoms.
The BPD relationship cycle isn’t a formal symptom of the condition. There’s also limited research on it.
However, clinical practice and literature have acknowledged it’s a common concern for both people with BPD and their partners.
These stages may not happen at all in a relationship or may be different in each relationship.
In fact, many people with BPD have healthy and successful relationships.
Formal symptoms of borderline personality disorder
To receive a diagnosis of BPD, five or more of these symptoms must be present across situations and over time:
- frantic efforts to avoid abandonment (real or imagined)
- intense, unstable relationship patterns of idealization and devaluation
- persistent and unstable sense of self or self-image
- potentially self-damaging impulsive behavior
- recurrent suicide attempts, suicide ideation, or self-harm
- intense, episodic mood instability
- chronic feeling of emptiness
- uncontrolled or intense, inappropriate anger response
- severe symptoms of dissociation or short-term, stress-related paranoia
Clinicians and researchers haven’t yet determined the exact causes of borderline personality disorder. They do know it’s not a personal choice, and it’s challenging for the person to manage.
They do know it’s not a personal choice, and it’s challenging for the person to manage.
Trauma, particularly childhood abuse, seems to be one of the contributing factors to the development of symptoms, as well as genetics and brain differences.
Cyclic behaviors are often how the symptoms of borderline personality disorder manifest.
They’re not your partner’s attempt to sabotage your relationship.
It’s a misconception that all people with BPD are attention seekers.
In fact, underneath these behaviors, there’s often a great deal of distress and pain.
They may evidence your partner’s difficulty regulating emotions and their persistently unstable self-image.
Quickly changing emotions may also contribute to the relationship cycle. Your partner with BPD may experience changes in mood going from feelings of elation and enjoyment to anxiety, insecurity, or distress.
Some people may believe that the borderline personality disorder relationship cycle is fueled by “self-sabotage.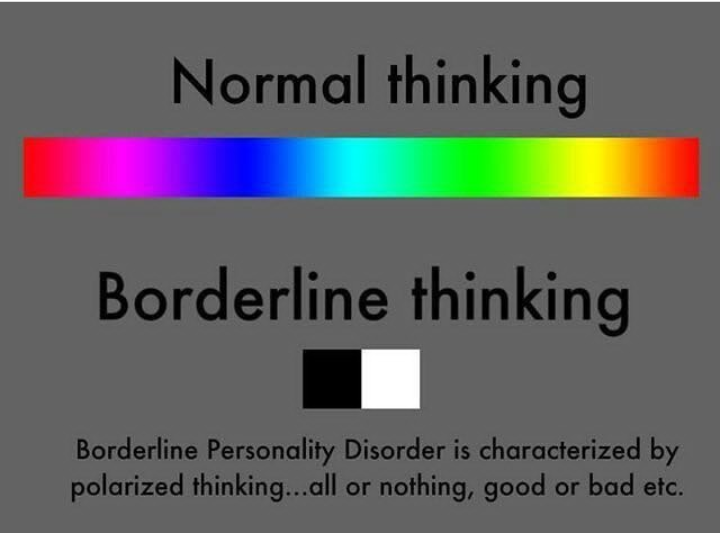 ”
”
Self-sabotage can in fact be a feature of some personality disorders. It was acknowledged as a fundamental psychodynamic trait of BPD by John Gunderson, MD, who expanded on it in his clinical guidebook.
According to Gunderson, and still considered relevant today, self-sabotage is one way some people with BPD can elicit the caring responses they need from those around them.
In a relationship, self-sabotage can garner displays of love and concern from the partner who has been blamed for not caring. Since the person with BPD might have a hard time expressing how they feel, these are attempts to receive reassurance that everything is well.
While this may temporarily meet the needs of the partner living with BPD, ultimately, self-sabotaging may repeat in a BPD relationship cycle.
Yes, it is possible. Living with BPD doesn’t mean you can’t establish stable and healthy relationships.
Still, relationships are a significant challenge to most people with BPD. These challenges can be managed, typically with professional support.
These challenges can be managed, typically with professional support.
A longitudinal marital study found that, while BPD was indicative of lower levels of marital satisfaction and higher levels of marital problems, it didn’t predict divorce.
“A romantic relationship with someone with BPD can be, in a word, stormy,” says Cranie. “However, people with BPD can be exceptionally caring, compassionate, and affectionate.”
You and your partner seeking guidance from a mental health professional can help support the possibility of positive change in your relationship.
BPD isn’t a determinant for lack of love or toxic relationships. It just may offer challenges to some people.
Tips to cope when your partner lives with BPD include:
- attending couple’s counseling together
- supporting and encouraging your partner’s desire to seek BPD treatment
- learning about BPD to better understand the symptoms and behaviors
- practicing support and patience during emotional moments
- staying calm during arguments
- setting and explaining boundaries to help prevent toxic behaviors
- making time for self-care and activities that bring you joy
- building a support network for those moments when your partner isn’t available
When your partner lives with borderline personality disorder, you may find yourself in a relationship cycle of highs and lows.
Your partner isn’t deliberately trying to hurt you or your relationship. Often, they’re internally critical, blaming themselves and not you. This is part of living with a mental health condition like BPD.
While relationships can be challenging when one or both partners have BPD, healthy bonds are still possible.
Learning more about the condition and seeking professional support can be helpful steps.
Tips for Couples Living With Borderline Personality Disorder
By Julie RevelantMedically Reviewed by Allison Young, MD
Reviewed:
Medically Reviewed
With compassion and good communication, borderline personality disorder doesn't have to signal doom for your romantic relationship.Brooke Cagle/UnsplashStephanie, of Jacksonville, Florida, has struggled with depression since she was a child. But in 2012, her mental health took a turn for the worse and her mood swings started to create conflict with her husband, Jerome. “At that time, I didn’t know what was going on. I would get angry for no apparent reason,” says Stephanie, whose last name has been withheld for her privacy.
“At that time, I didn’t know what was going on. I would get angry for no apparent reason,” says Stephanie, whose last name has been withheld for her privacy.
At first, Stephanie was diagnosed with bipolar disorder, but when she found another doctor who took the time to complete a thorough evaluation, she learned the true culprit was borderline personality disorder (BPD), which she was diagnosed with six months later.
The Challenges of Having a Partner or Spouse Diagnosed With BPD
Borderline personality disorder (BPD) is a mental illness that can cause affected individuals to have a negative self-image, make risky or impulsive choices, engage in self-harming behaviors, and have intense emotions and mood swings. Also, BPD, which is likely caused by a mix of environmental factors, brain activity, and genetics, can lead people to have trouble empathizing with others’ feelings and fear that they will be abandoned by their loved ones. (1)
More in Emotional Health
Could It Be Borderline Personality Disorder?
It goes without saying that these symptoms can create a perfect storm for a tumultuous relationship that in some cases may prove destructive.
In September 2018, SNL comedian Pete Davidson, who has been open about his struggles with BPD, said he had been concerned his diagnosis would prevent him from having a healthy relationship before getting together with then-fiancée Ariana Grande. “I was [afraid it could ruin relationships] until I met her,” he said, according to People. “I just think we are supposed to be together.” But in October 2018, TMZ broke the news that Davidson and Grande called off their engagement and broke up.
As of that month, the pair hadn't confirmed the cause of their split. But the truth is “it is challenging to be in a relationship with somebody who has BPD because one of the hallmarks is this fear of real or fantasy abandonment,” says Gail Saltz, MD, clinical associate professor of psychiatry at the NewYork Presbyterian Hospital Weill-Cornell School of Medicine in New York City.
That fear of abandonment can lead people with BPD to mistrust their partner. A study published in the journal Personality Disorders: Theory, Research, and Treatment found that after talking to their spouses about personal fears and possible reasons their relationship might end, women with BPD experienced a lower perception of trustworthiness in their spouse compared with women without BPD. (2)
(2)
For the person with BPD to manage the demands, closeness, and vulnerability of the relationship with his or her partner, “they have to work harder than other people at allowing themselves to choose to trust that person,” says Elizabeth Ochoa, PhD, chief psychologist at Mount Sinai Beth Israel in New York City.
The instability and unpredictability of the relationship itself can cause the partner without BPD to have trust issues as well.
For Stephanie, fear of abandonment was a familiar feeling from childhood. When she was a teenager, she says, her parents divorced, moved away, and left her and her brother on their own. With Jerome, Stephanie says those fears would also surface. “I always felt if he was going to go out, he would do something or find somebody better,” Stephanie says.
Unfortunately, that fear was realized when, while Stephanie was pregnant with one of their children, Jerome had an extramarital affair, further exacerbating her abandonment and trust issues. “I’m still dealing with it,” she says.
“I’m still dealing with it,” she says.
People with BPD are furthermore hypersensitive to every emotional nuance, usually in a negative way. “I can feel when there is something bothering him,” Stephanie says. “I can often tell before he even notices that something is bothering him.”
Dr. Saltz explains that people with BPD perceive emotion even in the absence of facial expressions. “That is their interpretation because that is what their brain is telling them,” Saltz says, “and that disconnect can of course make it hard for them to connect to and understand and feel safe with their partner.”
BPD can also cause extreme mood swings. “There can be this wonderful intensity, which may be delightful at the time with your partner, but it can quickly become unstable,” Saltz says.
One minute the person with BPD may idealize their partner and feel very close to him or her and the next, the person with BPD can get angry and put down his or her partner whether the partner did something wrong or failed to do something desired. “I had no clue when I would get angry. It would just come on all of a sudden,” Stephanie says. “If he left a dish on the counter, I would go off.”
“I had no clue when I would get angry. It would just come on all of a sudden,” Stephanie says. “If he left a dish on the counter, I would go off.”
Jerome says Stephanie’s extreme mood swings were challenging because he couldn’t anticipate what would cause her to get angry and trigger an argument, or how to prevent these episodes. “At the surface, we’re fighting over something that was kind of immaterial to the bigger picture of what was going on, and that kind of created a lot of noise,” he says.
Finding Relief if You’re Facing Relationship Problems Due to Borderline Personality Disorder
Gerry Surrency, a board-certified advanced practice psychiatric mental health nurse practitioner with North Florida Medical Associates in Orange Park, Florida, who provided therapy for the couple, says identifying Stephanie’s symptoms, validating them with Jerome, and then deciding on the best intervention was key in helping them improve their relationship.
Surrency and other experts say that despite the challenges BPD can bring to a relationship, communication skills and self-care are important for both partners. Here are some other tips for partners dealing with BPD:
Here are some other tips for partners dealing with BPD:
Seek out information. Learning as much as possible about BPD can increase empathy in a partnership. If you’re the partner affected by BPD, educating yourself about the disorder can help give an explanation for your feelings and behaviors and help ease your shame. Education can help the spouse without BPD understand that it’s an illness, not a choice. “When the person is responding out of fear, shame, or lack of self-worth, [the spouse can understand] this is not the whole person, this is a moment in time that will pass,” Dr. Ochoa says.
Get help. Seeking support from a mental health counselor or therapist — separately or as a couple — can help people affected by BPD gain insight, communicate more effectively, resolve conflict, and strengthen their relationships.
Because someone with BPD can also experience other conditions, such as anxiety disorders, post-traumatic stress disorder (PTSD), bipolar disorder, depression, eating disorders, and substance abuse, it’s important for both partners to keep their provider informed about changes in mood and behavior, Surrency says.
More in Emotional Health
What Finger Length May Say About Your Mental Health
Practice healthy communication. When you communicate, don’t say anything that could make the person with BPD feel slighted or uncared for. Actively listen and do your best to respond in a positive way. “Always do it in love as opposed to attacking or putting the person down,” Surrency says.
Ask open-ended questions. If you’re a partner to someone with the disorder, it’s important to speak objectively and keep in mind that BPD can cause people to misconstrue what others say to them. Asking open-ended questions can also help them feel that they’re being heard, such as "I think...."
“You may need to use your words in places where you would assume that your facial expression or the nuance in the room would make it clear,” Saltz says. “You may really need to spell it out.”
Talk only when your partner is calm. A severe episode of BPD is not the time to tackle potentially sensitive topics, like the cleanliness of your living room or your family budget. Doing so may lead your partner with BPD to make irrational decisions. He or she is also more likely to be defensive, pull away, or turn to self-harming behaviors when their symptoms are uncontrolled.
Doing so may lead your partner with BPD to make irrational decisions. He or she is also more likely to be defensive, pull away, or turn to self-harming behaviors when their symptoms are uncontrolled.
Offer support. Partners should provide the person with BPD understanding and emotional support and encourage and support their treatment. “I think it’s important for the partner to tell the person that they are there, that they understand it’s hard, and they want to help them in any way they can whether or not it’s rejected,” Ochoa says.
Avoid labeling or blaming. It’s important to be careful not to blame everything the person with BPD says or does on their mental illness because “then it starts to become sort of an insult or a put-down,” Saltz says.
Take threats seriously. Threats of self-harm or suicide should never become a form of blackmail in the relationship, but they must be taken seriously regardless of whether you believe the person plans to follow through. Call your spouse’s therapist, the National Suicide Prevention Hotline (1-800-273-8255), or 911. This isn’t only to protect them. “You also have to maintain your own sanity and safety,” Saltz says.
Call your spouse’s therapist, the National Suicide Prevention Hotline (1-800-273-8255), or 911. This isn’t only to protect them. “You also have to maintain your own sanity and safety,” Saltz says.
Prioritize self-care. Likewise, being in a relationship with someone who has BPD can feel all-consuming, but it’s important to seek out your own support system and have a healthy outlet to deal with stress.
Make healthy eating, fitness, and sleep a priority, and carve out time for friends, a hobby or enjoyable activities. Although a glass of wine for example, can help you relax, be aware that you can get drawn into substance abuse if your partner is abusing too, Saltz says.
Know that you can live a normal life with BPD. People with BPD often have risk-taking behaviors, such as overspending, drug use, reckless driving, or self-harm due to a lack of inhibition. Although these behaviors can be dangerous, and potentially life-threatening, many people with BPD are high-functioning individuals. “There are definitely different degrees of severity of BPD,” Saltz says.
“There are definitely different degrees of severity of BPD,” Saltz says.
Making Peace With Borderline Personality Disorder as a Couple
Once Stephanie was able to get an accurate diagnosis and the right medication, she says her illness became more manageable. “I don’t get those blowout anger episodes anymore,” she says.
Therapy and learning more effective ways to communicate has also helped her marriage. When Stephanie is struggling, for example, she’ll tell Jerome, “Today is an off day,” which helps him understand and not take things personally, but still offer support, even if it’s a simple hug.
Instead of letting an argument escalate, they’re able to neutralize a disagreement before it gets out of control. “Going down that path and going blow for blow isn’t going to get us anywhere,” Jerome says.
By subscribing you agree to the Terms of Use and Privacy Policy.
Editorial Sources and Fact-Checking
- Borderline Personality Disorder. National Institute of Mental Health.
 December 2017.
December 2017. - Miano A, Fertuck EA, Roepke S, Dziobek. Romantic Relationship Dysfunction in Borderline Personality Disorder-A Nautralistic Approach to Trustworthiness Perception. Personality Disorders. July 2017.
Show Less
The Case Against Food Morality: Why Foods Aren't ‘Good’ or ‘Bad’
By Christine ByrneWhat Is Agoraphobia? Symptoms, Causes, Diagnosis, Treatment, and Prevention
By Joseph Bennington-CastroIs Borderline Personality Genetic?
No single cause triggers a psychiatric illness, but genes play a bigger role than you may think.
By Jessica Migala
What Is Borderline Personality Disorder (BPD)? Symptoms, Causes, Diagnosis, Treatment, and Prevention
By Rena GoldmanHow to live with the "border guard" | PSYCHOLOGIES
21,633
A person among people
Life with a "border guard" is often compared to a "roller coaster" - ups and downs, good periods filled with love and happiness, then emotional outbursts, fits of rage or attempts at tight control . This causes confusion, helplessness, despair and the obvious question: “How to deal with this?”
This causes confusion, helplessness, despair and the obvious question: “How to deal with this?”
Stop walking on eggshells!
Authors of Stop Walking on Eggshells. Living with someone with borderline personality disorder Paul Mason and Randy Kroeger answer this question and more. They created a kind of instruction, a guide for those who live with the "border guards". nine0003
Reminding that diagnosis is the task of doctors, psychiatrists, Paul Mason and Randy Kroeger provide useful information about this type of disorder, not fully understood by specialists.
“The definition of a personality disorder implies that it causes suffering both for the person himself and for those who interact with him. The description of BPD seems so negative that people with this diagnosis often feel stigmatized.
It is extremely important to remember that borderline personality disorder and its owner are not the same thing. If you live with a borderline person, it can be difficult to separate the diagnosis from them. In fact, only a person with BPD can control his thoughts, feelings and behavior. And this is important to understand for the recovery of SPs and for yourself.” nine0003
In fact, only a person with BPD can control his thoughts, feelings and behavior. And this is important to understand for the recovery of SPs and for yourself.” nine0003
The following clearly structured chapters provide information about BPD itself and the inner world of a person with this disorder. The writing of the book was preceded by a long period of communication with the "border guards" and their relatives, the collection and systematization of information shared by real people.
That is why the "manual" covers such a large layer of problems - and each question is given a clear answer. In addition, the reader has the opportunity to look at the situations described from different angles - through the eyes of the people with BPD themselves, their parents, children or partners and experts. nine0003
How to regain control over your own life if there is a "border guard" next to you? How to resolve many specific issues? How to be guided in the search for a psychotherapist, what other literature on the topic can be read? And what exercises will help to cope with their own experiences and maintain balance? All the answers are in the book by Paul Mason and Randy Kroeger.
Here is a fragment of the text of chapter 2 “The inner world of the “border guard”: the definition of BPD. PRL Criteria".
"Desperate attempts to avoid real and imagined situations in which they will be abandoned"
Imagine the horror you would feel if you were lost as a child in Times Square in New York. A second ago, mom was there, holding your hand - and suddenly she was carried away by the crowd. You look around, panicking, trying to find her.
This is how people with BPD feel most of the time - isolated, anxious, terrified at the thought of being alone. Caring, supportive people are like friendly faces in a crowd.
But if one takes a careless step, which can be interpreted as a sign of an impending departure, the SPs will panic and react. For example, an explosion of rage or a plea "Just don't leave!". It doesn't take much to trigger this reaction: One borderline woman stopped her neighbor from leaving her apartment to take her clothes to the laundry. nine0003
nine0003
Fear of abandonment can be so strong that it literally overwhelms an SP: when a man told his SP wife that he probably had a deadly disease, she lashed out at him for going to the doctor.
If your SPs experienced neglect as children or grew up in a highly dysfunctional environment, they may have learned to deal with fear by denying or suppressing it. They had plenty of opportunities to practice, so the original emotion might not be felt. nine0003
If SPs get upset or angry, try to remember if some circumstance could have triggered the fear of abandonment.
Armin (not borderline)
If I'm five minutes late on my way home from work, my wife will call me. She constantly sends messages to the pager. I can't go out with my friends anymore because she reacts so strongly to it. Messages on the pager came, even if we were going to the movies. It was so stressful that I stopped seeing my friends without her. nine0003
Sometimes people with BPD will immediately warn about their fear of being abandoned. However, no less often this fear is expressed in other forms, for example, through rage. Feeling vulnerable and out of control provokes anger.
However, no less often this fear is expressed in other forms, for example, through rage. Feeling vulnerable and out of control provokes anger.
Tess (borderline)
If I feel like I've been abandoned, a whole range of feelings arise: isolation, horror, loneliness. I panic. I think that I was betrayed, used. I think I will die. One day I called my young man, and he replied that he would call back later, as he is now watching TV. nine0003
I took up ironing to pass the time. But he didn't call. I waited. He didn't call. And the terrible feeling that I was abandoned returned. It hurt so much, because just the day before, I caught myself thinking that I believed in his love for me.
By the time the phone rang at ten o'clock, I had already decided that we needed to break up, I wanted to leave him before he left me. And all this time he was just watching the movie. I felt so stupid; but the pain, the fear like a knife in the heart - it was all real. nine0003
nine0003
Photo Source: Getty Images
New on the site
No matter how much you drink: how personality type affects hangover severity networks without damaging the psyche: 4 rules
Swine flu: what is important and everyone needs to know
"Dangerous" pills: why we are afraid to take psychotropic drugs - 2 main myths
“I broke up with my ex due to emotional swings. And now I miss and suffer”
“I lost interest in people, I don’t care about everyone”
What’s wrong with weight loss after 50 years: an unexpected answer from scientists
How to live with borderline personality disorder
Daria Batyrshina
lives with BPD
Author profile
The correct diagnosis could not be made for me for several years, and then it completely changed my life.
To describe borderline personality disorder, or BPD, psychologist Marsha Linehan's well-known statement is perfect: “People like that just don't have 'emotional skin'. Even the slightest touch or movement can cause the most severe suffering.” nine0003
Even the slightest touch or movement can cause the most severe suffering.” nine0003
Share my path to getting the correct diagnosis, symptoms, and tips for dealing with people with BPD.
Go see a doctor
Our articles are written with love for evidence-based medicine. We refer to authoritative sources and go to doctors with a good reputation for comments. But remember: the responsibility for your health lies with you and your doctor. We don't write prescriptions, we make recommendations. Relying on our point of view or not is up to you. nine0003
What is borderline personality disorder
Borderline personality disorder is characterized by permanent changes in mood, self-image and behavior. This can lead to problems in relationships with other people and impulsive actions of all kinds.
BPD - Mayo Clinic
BPD - National Institute of Mental Health, USA
In the International Classification of Diseases, 10th Revision, or ICD-10, there is in fact no diagnosis of "borderline personality disorder", there is an emotionally unstable personality disorder, which two types: borderline and impulsive. In ICD-11, this is already a separate diagnosis, which is called borderline personality disorder. nine0003
In ICD-11, this is already a separate diagnosis, which is called borderline personality disorder. nine0003
The disorder has several main features.
So what? 01/12/22
Transition to the new International Classification of Diseases has begun in Russia: what will change and when
Self-injurious and risky behavior. For example, a person may injure themselves or use psychoactive substances - borderline disorder increases the risk of developing various addictions.
Black and white thinking: it seems to a person that there can only be good and bad, there are no halftones. nine0003
Criteria for diagnosing BPD - Medscape
Problems with self-esteem. People with this disorder are overly sensitive to the opinions of others, enter into dependent relationships, have a strong fear of being alone, and may take desperate actions to keep a loved one or get their attention.
The manifestations of borderline personality disorder are similar to those of adolescence: outbursts of anger, mood swings, aloofness, so this diagnosis is made after 18 years. nine0003
What are the symptoms of borderline personality disorder
Aleksey Pribytkov
psychotherapist, psychiatrist, Ph.D. It happened.
 Usually these are short, from a few hours to a few days, but intense emotional experiences. Depression and depression can be replaced by an upbeat, euphoric mood. Such drops can occur for no apparent reason or in minimal life situations. For example, the partner did not respond to the message.
Usually these are short, from a few hours to a few days, but intense emotional experiences. Depression and depression can be replaced by an upbeat, euphoric mood. Such drops can occur for no apparent reason or in minimal life situations. For example, the partner did not respond to the message. Why borderline personality disorder develops
Why borderline personality disorder develops is not exactly known.
NHS
Biological factors. There is evidence that the development of personality disorders, including BPD, may depend on genetic factors. nine0003
BPD may also be associated with changes in some parts of the brain responsible for controlling emotions. Its development can be affected by disturbances in the functioning of the system of neurotransmitters - compounds with the help of which brain neurons communicate with each other, in particular serotonin.
Its development can be affected by disturbances in the functioning of the system of neurotransmitters - compounds with the help of which brain neurons communicate with each other, in particular serotonin.
Social factors. For example, unstable relationships with significant adults, lack of love in childhood, neglect by parents, loss of a loved one.
Emotional or physical abuse, as well as intense fear experienced in childhood, greatly increase the risk of any psychological problems. In this case, BPD can be combined with another diagnosis - post-traumatic stress disorder, or PTSD. It is manifested by constant frightening memories of a traumatic event and increased anxiety. The more unstable the environment around and the more traumatized the child, the more likely it is to get PTSD. nine0003
How I treated depression and anxiety for several years
I first saw a doctor almost eight years ago. I had an eating disorder - it often accompanies BPD, but I didn't know about it yet.
My gastroenterologist at some point realized that my constant pain in the abdomen was most likely connected not with physical problems, but with mental ones. My mother took me to a government clinic, where I came across incompetent doctors.
/eating-disorders/
How to cure eating disorders
The psychiatrist said that I have anorexia, I look terrible and I won't be able to find a partner because "men don't throw bones." Then I realized that it was not worth waiting for help from him.
I coped with eating disorders myself, having lived through all the stages from anorexia to bulimia and compulsive overeating in two years. After solving the problem with food, depression came. Here, I couldn't manage on my own.
My days were similar to each other: constant fatigue, apathy, I didn’t have enough strength even to eat and brush my teeth, and there was only fog in my head and no thoughts. My circle of contacts narrowed greatly, because those around me saw only aggression or received no answers at all. So several years passed, then I realized that I needed help. nine0003
So several years passed, then I realized that I needed help. nine0003
On the Profi-ru website, I found a psychologist who lived next to me. Then I did not yet know how psychiatrists differ from psychologists and psychotherapists, so I did not receive the necessary help.
/psychotherapy-search/
How to choose a psychotherapist
Psychologists usually do not work with mental disorders, besides, in the sessions I just told what was bothering me, there was no other support. Sometimes I couldn't find words and we just kept silent.
I went to the specialist for about a month and paid 1300 R for each meeting. In total, we held nine meetings. The only thing I got was the fog left my head. Despite my condition and the fact that the psychologist could not do anything about it, she persuaded me to stay in therapy. She said that it helps, although I did not feel any relief.
11,700 R
I spent on a psychologist who did not help me
As a result, I did not want to spend more money on myself and lost confidence in doctors. Then I learned that in Moscow you can get free psychological help at the Moscow Service for Psychological Assistance to the Population. nine0003
Then I learned that in Moscow you can get free psychological help at the Moscow Service for Psychological Assistance to the Population. nine0003
Moscow Service for Psychological Assistance to the Population
I had to wait for an appointment, but I had nowhere to hurry. About six months later, I was able to get to a psychologist. I told her what worries me - at that time they were symptoms of depression and apathy. She immediately said that I should talk to a psychotherapist, and I made an appointment with another specialist in the same clinic.
The psychotherapist referred me to a psychiatrist, suggesting several doctors she trusts. She said that I most likely had depression and needed medication. Psychiatrists are not accepted at MSPPN, so I went to a private clinic, where I had to pay 4000 R for an appointment.
The amount of free assistance in the ISPP is limited, but it is enough to get started. Source: MSPPN A psychiatrist in a private clinic diagnosed me with depression, prescribed an antidepressant and a tranquilizer. I was lucky that my doctor saw not only in a private clinic, but also in a state one, so I went to all subsequent appointments for free.
I was lucky that my doctor saw not only in a private clinic, but also in a state one, so I went to all subsequent appointments for free.
The second time I managed to find the right medicines. We fixed the changes not only with the help of conversations. The psychiatric clinic had a simulator on a computer, where the patient was asked to pass several tests: attentiveness, reaction speed, the ability to distinguish faces, and much more. I took tests at intervals of about once a month. nine0003
This testing is not necessarily and does not always reflect the effectiveness of the treatment, but I liked that the results got better every time. At that time, about 1,500 R per month was spent on medicines.
/list/antidepressant-myths/
8 myths about antidepressants
During the same period, I tried cognitive behavioral therapy. In a year I started and quit three times, nothing worked out for me. The mood diary was empty, because I do not distinguish between emotions, the diary of situations that concern me and their analysis, too. I did not understand why this or that situation became important to me. In total, I had five meetings with a psychotherapist, the cost of one was 3000 R.
I did not understand why this or that situation became important to me. In total, I had five meetings with a psychotherapist, the cost of one was 3000 R.
At that time, the doctor and I did not yet know that I had more than just depression with panic attacks and anxiety, so we did not follow my emotions and feelings much, which is important in BPD.
At some point, I abruptly stopped taking the prescribed pills and coped with the withdrawal syndrome for another week. I refused the pills, because it seemed that I could manage without them, besides, they helped for a short time, then everything started all over again.
/panic attack/
How to cope with a panic attack: recommendations from a psychotherapist
A month or two after the withdrawal, I felt fine and even started to exercise. Then anxiety and depression symptoms returned, I suffered for a few more months and went to a new doctor.
Over the next year and a half or two, I changed three doctors in one private clinic, I was prescribed different types of medicines in different combinations and dosages. Primary appointments cost 4000-5000 R, repeated - 2400 R. I went to psychiatrists once a month to control my condition. I bought medicines either generics or original ones, they spent about 2000-3000 R per month. nine0003
Primary appointments cost 4000-5000 R, repeated - 2400 R. I went to psychiatrists once a month to control my condition. I bought medicines either generics or original ones, they spent about 2000-3000 R per month. nine0003
The pills made me feel better for a short time, about a month. During this period, I was already diagnosed with "emotional personality disorder", but they did not tell me about it. I later found out from the medical record, which I requested before changing the clinic.
At the same time, I also turned to Gestalt therapy for help - this is one of the areas of psychotherapy aimed at developing self-awareness. For me, the sessions were an opportunity to cry, acknowledge problems, and receive support. For three months, I called a psychologist every two weeks. One session cost 2000 R.
107,100 R
I spent on specialists before I was given the correct diagnosis
I spent on treatment before the correct diagnosis was made 177,100 R
| Expenses | |
|---|---|
| Medicines in the last two years of treatment | 55 000 R |
| Regular visits to psychiatrists | 50 400 R |
| Medicines in the first year of treatment | 15 000 R |
| Cognitive behavioral therapy, 5 sessions | 15 000 R |
| Three initial appointments with the following psychiatrists | 14 000 R |
| Gestalt therapy sessions, 6 sessions | 12 000 R |
| Psychologist sessions with "Profi-ru" | 11 700 Р |
| First psychiatrist appointment | 4000 R |
Medicines in the last two years of treatment
55 000 R
Regular visit to psychiatrists
50 400 R
Medicines in the first year of treatment
15 000 R
Cognitive-behavioral therapy, 5 sessions
15 000 P
Three initial appointments with the following psychiatrists
14,000 R
Gestalt therapy sessions, 6 sessions
12,000 R
Psychologist sessions with Profi-ru
R 11,7000004 Appointment with the first psychiatrist
4000 Р
How borderline personality disorder is diagnosed
Aleksey Pribytkov
psychotherapist, psychiatrist, Ph. D. In the first place is always the clinical picture, that is, manifestations of mental disorders.
D. In the first place is always the clinical picture, that is, manifestations of mental disorders.
There is an interesting story with borderline personality disorder in Russia. We still use the International Classification of Diseases of the 10th revision, where in fact there is no such diagnosis, which means that for a long time it was out of sight of psychiatrists. But the absence of a diagnosis in the classification does not mean the absence of violations, because more than 30 years have passed since the adoption of the ICD-10 - it was adopted by WHO in 1990 - and the understanding of mental disorders during this period has noticeably changed.
Now many modern doctors are guided by other criteria when making a diagnosis. They are most clearly formulated in the American classification of psychiatric disorders DSM-5. Similar criteria are used in ICD-11, which is adopted by WHO and should come into force in Russia in 2024.
The above are nine criteria that are specific to BPD. The task of the psychiatrist is to identify them during a conversation with the patient. The basis for the diagnosis of "borderline personality disorder" is the presence of at least five of the nine criteria. nine0003
The task of the psychiatrist is to identify them during a conversation with the patient. The basis for the diagnosis of "borderline personality disorder" is the presence of at least five of the nine criteria. nine0003
How I was correctly diagnosed and treated
After many unsuccessful attempts at treatment, I decided to change doctors again and went to a new psychiatrist at another clinic. The first appointment there cost 7,000 R, and repeated appointments already cost 6,000 R.
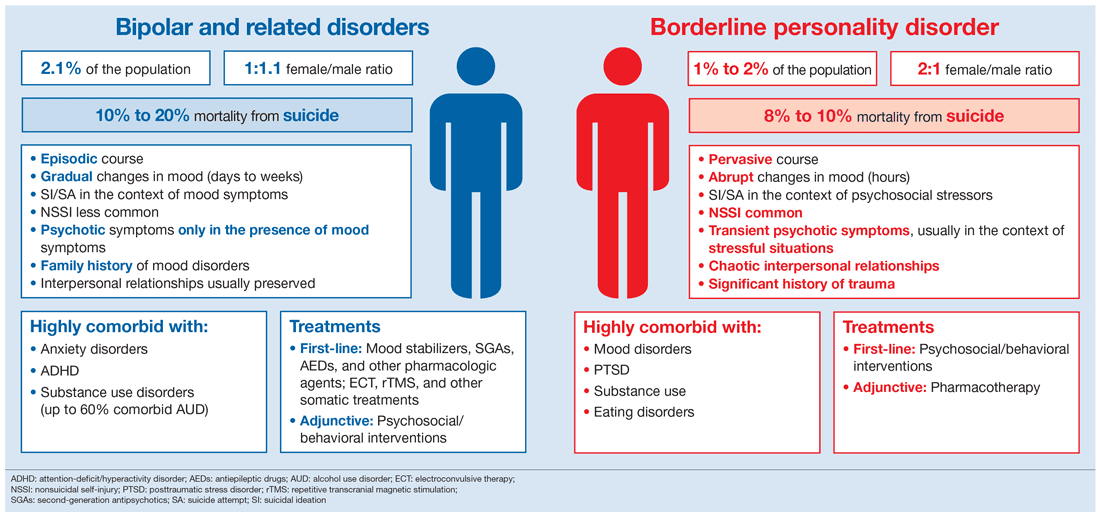
The drug treatment was corrected for me. And with the final diagnosis, they rushed between bipolar affective disorder, or BAD, and borderline personality disorder.
/bipolarnoe-rasstroystvo/
How much does it cost to treat bipolar affective disorder
They are similar in symptoms. BAD also occurs with alternating periods of depression and high spirits, but they are usually long and can last several months.
In BPD, periods of different moods change over several hours, less often over several days, that is, the mood is constantly unstable. Moreover, these two disorders can occur simultaneously in one person.
Moreover, these two disorders can occur simultaneously in one person.
As a result, the psychiatrist diagnosed me with borderline personality disorder. Now, once every one and a half to two months, I go to him to monitor the condition. nine0003
Since that time, I began to go to schema therapy - this is a therapy focused on making a person change their behavior patterns. I go to a psychotherapist every week, one session costs 6000 R. I feel that it helps me.
BPD - MSD Handbook
My maladaptive patterns of behavior that my therapist and I identified at our first meeting. In the lower left corner are the schemes to be achieved It is difficult to treat BPD. My doctors never know in what condition I will come to them and whether I will come at all. Meetings are held online from time to time. I am often late, I call specialists from different places: it can be a park or my workplace, a stop on the street or someone else's apartment, a noisy highway or a food court. Sometimes I don't want to see my doctor because it seems that he is wrong about everything. nine0003
Sometimes I don't want to see my doctor because it seems that he is wrong about everything. nine0003
Sometimes I felt disgusted and decided that I needed another doctor: I abruptly go from idealizing a person to hating him. For this reason, many doctors refuse patients with borderline disorder. In addition, people with BPD tend to discount their own problems, so many may not seek help for a long time.
/list/antidepressant-facts/
10 facts you should know before taking antidepressants
Over the years, I have developed several rules for choosing a doctor for myself:
- At the reception, they listen to me attentively.
- Everything that I consider important is important to a doctor. He should not wave his hand and say that there is no point in talking about something.
- The doctor speaks honestly about the diagnosis, does not hide anything, describes the treatment regimens.
- I am informed about the drug I will be taking.
 They explain exactly how it works, why it was prescribed, what side effects.
They explain exactly how it works, why it was prescribed, what side effects. - If I don't like something, I change doctors.
Unfortunately, there are no rules that help fight mood swings. I try to turn to the facts at such moments and tell the doctors how I feel. Psychiatrists, as a rule, treat the frequent change of doctor normally. I have never faced condemnation. nine0003 One of the latest treatment regimens My prescriptions for drugs, there are a lot of them due to different dosages
How borderline personality disorder is treated
Alexey Pribytkov
psychotherapist, psychiatrist, PhD in medicine
The main method of treating borderline personality disorder is psychotherapy. It is necessary to achieve a stable result. Medications only alleviate some of the symptoms of the disorder.
Dialectical Behavioral Therapy, or DBT, has the most evidence of effectiveness in treating BPD. Other directions can be applied: schema therapy, transference focused therapy - TFP. nine0003
nine0003
However, medications are also prescribed for most BPD patients. Three groups of drugs are usually used:
- Mood stabilizers, or mood stabilizers, are drugs that smooth out emotional fluctuations and help maintain an even mood.
- Antidepressants - they help reduce the severity of emotional instability. BPD often accompanies depressive and anxiety disorders, obsessive-compulsive disorder - antidepressants are also used to treat them. nine0138
- Antipsychotics, or second-generation neuroleptics, are prescribed in low doses to correct impulsivity and aggression.
The choice of treatment regimen depends on the individual patient's symptoms. Drug therapy usually lasts at least a year, more often several years.
How do I deal with borderline personality disorder
Insomnia. I have suffered from sleep problems since childhood. I tried everything: from hot milk at night to being very tired during the day.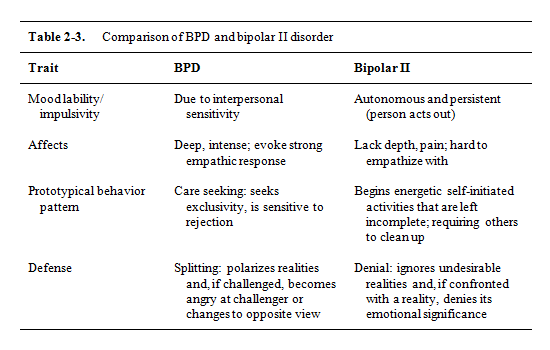 nine0003
nine0003
Unfortunately, I do not have a universal solution to this problem. I only save myself with pills: psychiatrists prescribed tranquilizers for sleep, now I have an antidepressant with a strong sedative effect - or I just don’t sleep.
/insomnia/
How to deal with insomnia
Anxiety and panic attacks. It often overtakes unexpectedly and at the most calm moments. Just talking to a friend, I can start twitching my leg, nervously breaking my nails, scratching my skin with my nails, or sticking to my phone. This is also manifested by a rapid heartbeat, trembling in the body, a desire to move, and strong fear. nine0003
To get rid of this feeling, I knit, switch to TV series, listen to meditation practices, start moving more, turn to metaphorical associative cards or Tarot. Metaphorical associative cards are cards with pictures that you can interpret based on your experience.
I use cards when my anxiety is about the future. I am extremely afraid of uncertainty, and this is a chance to decide at least a little, albeit somewhat irrational.
I am extremely afraid of uncertainty, and this is a chance to decide at least a little, albeit somewhat irrational.
Feeling of loneliness and abandonment. Feels like an unfilled hole in the chest. At such moments, I am sure that I have no one to turn to, no one will help. The feeling that I am alone in the whole world.
Saves background noise such as a movie or TV series. I also have three cats that periodically ask for attention, and I am no longer alone. During periods when I feel very lonely, my friends help, who, if they cannot come, then at least call or write.
Sometimes, in order to feel that I am not alone, I look for meetings with different men. I tend to dive into the person who gives me attention, as if I'm trying to close the inner "hole". If I don’t get enough attention, then I show aggression, and subsequently I change the “victim”. I'm trying to deal with this with the help of psychotherapy. nine0003
Mood swings, anger and aggression. In an hour I can experience a huge range of emotions, it is very tiring. Moreover, anything can become a trigger: an incorrect statement on the part of the interlocutor, just an action that seemed wrong to me, or an opinion that is the opposite of mine. I can be aggressive even to banal questions about my well-being.
In an hour I can experience a huge range of emotions, it is very tiring. Moreover, anything can become a trigger: an incorrect statement on the part of the interlocutor, just an action that seemed wrong to me, or an opinion that is the opposite of mine. I can be aggressive even to banal questions about my well-being.
I try to warn people about the peculiarities of my behavior, I leave the dialogue if I feel that I am jumping into aggression, I try to distract myself. My psychotherapist advises to live through aggression and give it a way out: tear a sheet of paper, go in for sports, beat a pillow, shout. nine0003
/list/psychoterapevt/
10 important questions for psychotherapist Sergey Divisenko
Changes in interests, hobbies and desires. I don't have one hobby, they are constantly changing. I can't say what my favorite movie or music is. Because today I like one thing, and tomorrow I'm already interested in absolutely polar things.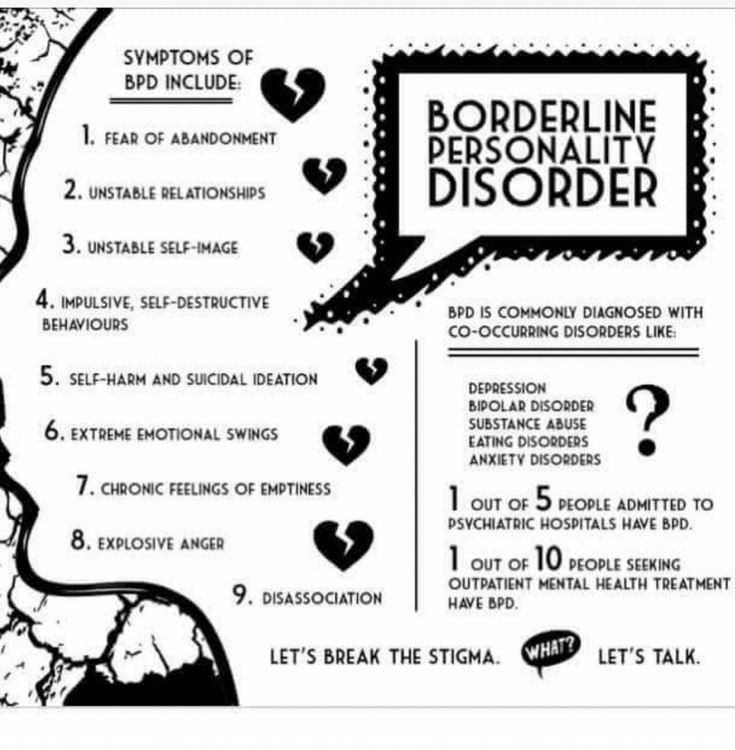 I never know in advance what awaits me the next day.
I never know in advance what awaits me the next day.
Suicidal thoughts and destructive behavior. For the first time I thought about suicide at the age of 14. Then these thoughts haunted me throughout my life. Somehow I lived with a gas leak in my apartment for several months, knowing full well about it. I drown my negative emotions in alcohol. I used to cut myself, but then I replaced this ritual with getting tattoos on my body. nine0003
Such thoughts are difficult to deal with. Medication, mindfulness and constant support from a psychotherapist help a little. I also sometimes go outside in the cold or take a shower: it's sobering.
Unstable self-esteem. I need a permanent evaluation from the outside. I doubt whether I am doing the right job, whether I look right if I do not receive feedback from people. Every mistake is a tragedy for me, but from praise I can feel capable of anything. I can spend weeks thinking that I did some wrong action, although it did not suffer consequences. nine0003
nine0003
To cope with this, I try to compliment myself, remind myself what I'm doing and why, and look at the results of my work. This does not always work, but here you need to take small steps and learn to focus on your feelings, and not just on others.
11 types of psychotherapy that work
Communication difficulties. I'm thrown from love to hate. I often conflict and change because of this place of work. In no relationship have I lasted more than a few months, and communication with friends is reduced to a couple of meetings a year. If I feel that I may be rejected or denied something, then I do it first to avoid emotions. nine0003
Everything that happens is always a disaster: vivid emotions, strong feelings of guilt. If I feel like I'm getting less attention, I'm hysterical. I immediately feel abandoned and abandoned. Considering my peculiarities of behavior, I always try to warn friends and relatives about my condition and tell how not to run into even more negativity.
How to better communicate with people who have borderline disorder
As with many people with BPD, the SET-UP method works well for me. There is about him in the book “I hate you, just don’t leave me. Borderline Personalities and How to Understand Them by Kreisman and Strauss. nine0003
6 useful services for finding a psychotherapist
SET stands for support, empathy, truth - support, sympathy, truth.
It is important that none of the parts can be thrown out of this triangle of communication, otherwise a person with BPD will go into conflict or completely stop communication:
- Support should be expressed in the form of concern in the first person: “I worry about how you you feel." The main thing is to express your own feelings and sensations. nine0138
- Sympathy: "You must be feeling upset." It is important to validate the feelings of the person with BPD. Don't try to show pity or talk about how you feel the same way.
 Most likely, this is not the case. And the phrase "I know how bad you feel" will only cause ridicule and anger.
Most likely, this is not the case. And the phrase "I know how bad you feel" will only cause ridicule and anger. - Truth: you need to rely on the facts about the situation and not go into accusation. For example: “You quit, you have enough money for a couple of months. I can help by preparing your resume, and you will look for a new job.” nine0138
UP is understanding, perseverance, or understanding and perseverance. These are goals that both participants must achieve.
A person with BPD must become aware of the causes of his actions and their consequences. Understand that he influences his life and can change it. He needs perseverance in order not to give up treatment, because any changes are difficult.
For those close to a person with BPD, understanding is the recognition of a person's feelings and emotions. That is, the acceptance that negative statements and aggression are behavioral features. They need perseverance in order to continue communicating with a person with borderline disorder, not to stop reminding him of his readiness to help, to sober him up and help him find the true cause of events, rely on facts, and not let him focus only on emotions. nine0003
nine0003
/shizofreniya/
How much does it cost to support a relative with a mental disorder
Communication with a person with BPD is always stressful, so people around need to take more care of themselves. It will take a lot of patience and strength to withstand sudden mood swings and maintain relationships.
The main thing is to understand that it is not your fault and you cannot influence BPD. However, if you remain in a stable state and support a person with a disorder, he will eventually cease to see his relatives as a potential threat, which means that there will be fewer outbreaks of aggression. nine0003
In Russia there is a resource center "Borderline Personality Disorder". It is designed for Muscovites, but on the site you can find personal stories of people with BPD, literature on the topic and features of this disorder.
How much does it cost to treat borderline personality disorder? The psychotherapist told me that we would manage in a year.
I need to visit a psychotherapist every week, an appointment costs 6,000 R. In addition, every one and a half to two months I visit a psychiatrist, whose appointment also costs 6,000 R.
/prl/
How much does borderline personality disorder treatment cost? Since I have severe depressive episodes, I need to take pills for a long time: from the moment my condition becomes stable on the background of psychotherapy, it is another 6-12 months.
About 2000 R per month is now spent on drugs. I often change pills, so the cost is approximate. nine0003
Drug treatment can remove symptoms that interfere with a normal life, and with the help of a course of psychotherapy, it will be possible to go into remission and significantly improve the quality of life. Relapses are extremely rare and are associated with affective states.
I spend 372,000 R per year for the treatment of borderline disorder
| Treatment | Expenses |
|---|---|
| Weekly psychotherapist visit | 312 000 R |
| Psychiatrist visit every 2 months | 36 000 R |
| Medicines | 24 000 R |
Visit of a psychotherapist every week
312 000 R
Visit a psychiatrist once every 2 months
36 000 R
Medicines
24 000 R
Is it possible to cure a border personality disorder
003
psychotherapist, psychiatrist, MD
We cannot completely eliminate the symptoms of borderline personality disorder.