Seizures caused by anxiety
Anxiety and seizures: Here’s what you need to know
February 4, 2022
Lifestyle & Wellness
It is very common for people with epilepsy to experience anxiety. Find out about anxiety and seizures, diagnosis and ideas for coping.
Anxiety is a perfectly normal response to a stressful situation, and it often goes away when the problem has passed. People can sometimes feel excessively anxious - even when there is no obvious danger. This is known as an anxiety disorder.
Anxiety disorders are the most common mental health issue in the USA - almost 20% of Americans experience anxiety problems each year. Anxiety is particularly common for people with epilepsy - four people in 10 with epilepsy have an anxiety disorder.
Here is everything you need to know about anxiety and seizures.
What is an anxiety disorder?
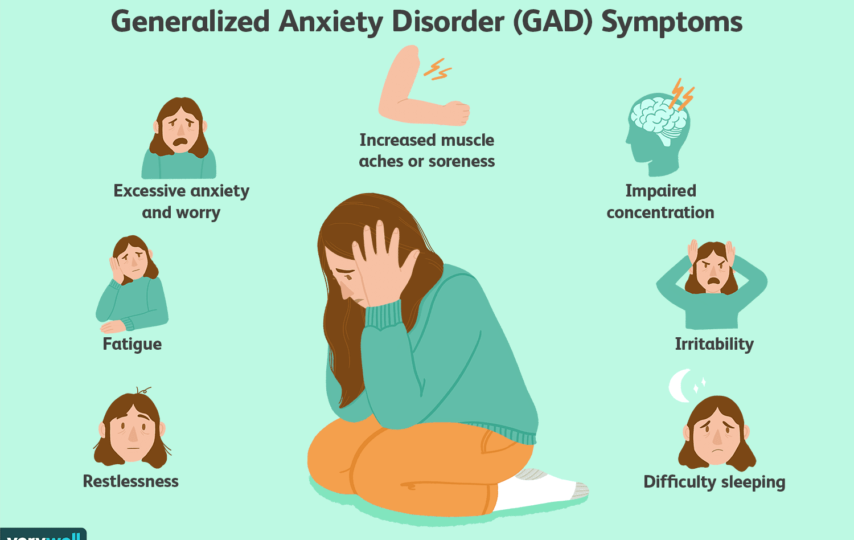
While feeling anxious is perfectly normal during stressful periods, sometimes people can feel anxious most - or even all - of the time. Anxiety disorders can cause many different kinds of symptoms:
Mind
- Constantly feeling worried
- Tiredness
- Inability to concentrate
- Poor sleep
- Feeling depressed
- Feeling easily annoyed
Body
- Fast or irregular heartbeats
- Dry mouth
- Sweating
- Muscle tension
- Numbness or tingling in fingers or toes
- Feeling sick or dizzy
Can anxiety cause seizures?
Maybe. If you have been diagnosed with epilepsy, intense feelings of anxiety could become a seizure trigger for you. Anxiety makes you feel stressed, and stress is widely believed to be a major cause of epileptic seizures.
Learn more: 7 common seizure triggers
Other articles you might like
February 3, 2022
Managing your condition
February 1, 2022
Epsy Community
October 27, 2022
Lifestyle & Wellness
Scroll down for the rest of the article
Anxiety and seizures: a complex relationship
It is very common for people with epilepsy to experience psychiatric disorders such as anxiety. There are several ways that anxiety and seizures feed into one another, and the exact relationship between the two is not always clear:
There are several ways that anxiety and seizures feed into one another, and the exact relationship between the two is not always clear:
- Anxiety after epilepsy diagnosis: People often feel anxious when they are diagnosed with a new medical condition.
- Fear of seizures: Seizures are highly stressful – and unpredictable - events. Not knowing when they might ‘strike’ can cause people to worry.
- Anxiety induced seizures: Feeling highly stressed is generally seen as a trigger for epileptic seizures. Feeling anxious increases stress levels and could therefore induce a seizure.
- Anxiety after seizures: It is also common for people to feel intense feelings of anxiety in the aftermath of a seizure. This could be because of chemicals released in the brain during the seizure. But it could also be related to social factors (people might feel embarrassed of losing control in front of others).
- Anti-seizure medication side effects: Some anti-seizure medications can cause people to feel anxious.
- Epilepsy syndrome and anxiety: Research suggests that people with certain kinds of epilepsy (particularly temporal and frontal lobe epilepsies) are more likely to have anxiety disorders - although anyone can have them.
Panic attack / anxiety or seizure?
A panic attack or anxiety attack is an extreme form of anxiety that causes severe physical reactions. These can include heart palpitations, sweating, trembling and shaking, headaches, dizziness, hot flashes and chills. They are accompanied with a feeling of intense fear.
Many of these symptoms can appear similar to epileptic seizures. However a panic attack is not the same as an epileptic seizure (seizures are caused by unusual electrical discharges in the brain).
If you are unsure if you are having panic attacks / anxiety or seizures it is important to seek medical help.
Related: The difference between epileptic and dissociative seizures
Anxiety and seizures treatment
If you notice that you are feeling highly anxious over a period of two weeks or more and there is no specific cause of the feelings, speak with your doctor. There are various treatments for people with epilepsy who have anxiety disorders, including:
- Counseling
- Cognitive Behavioral Therapy
- Medication
There are also several things you can do to treat yourself. These include talking about your worries with friends and family, going to epilepsy support groups, and using self-calming techniques - such as breathing methods, physical exercise and things like yoga.
Anxiety can feel overwhelming. But remember, it is treatable and with the right support you can overcome these feelings of panic and fear.
Can Stress Cause Seizures? Understanding the Link
Stress can cause seizures known as psychogenic nonepileptic seizures (PNES). PNES differ from neurological seizures with causes such as epilepsy. Learn about stress’s relationship to PNES, panic attacks, and more.
PNES differ from neurological seizures with causes such as epilepsy. Learn about stress’s relationship to PNES, panic attacks, and more.
For most people, feelings of stress are short-lived. For some people, stress can become chronic and greatly affect their quality of life.
Stress can cause a wide range of physical and mental symptoms, which may include psychogenic nonepileptic seizures (PNES). PNES were previously known as pseudoseizures, but that term is now outdated.
In this article, we’ll explain what PNES are, how they differ from neurological seizures, and the connection between stress and PNES.
A seizure is a brief period of uncontrolled electrical activity in the brain. Seizures can provoke a wide variety of changes in the body.
The chronic condition epilepsy causes unpredictable, recurrent seizures.
Epileptic seizures can occur due to a variety of triggers, including increased stress and anxiety. However, the Epilepsy Foundation suggests that it’s hard to know exactly how often stress triggers seizures. This is because stress has different meanings for different people.
This is because stress has different meanings for different people.
Stress and anxiety can also trigger PNES in people without epilepsy. PNES are physiologically different from the neurological seizures found in epilepsy.
PNES aren’t the same as neurological seizures that occur due to uncontrolled activity in the brain. Instead, PNES can be an extreme response to stress and anxiety. Doctors consider them psychiatric in nature.
According to a 2016 literature review, PNES are indicative of a functional neurological disorder (or conversion disorder). This type of disorder occurs when emotional stress causes physical symptoms that can’t be explained by an underlying health condition.
When certain emotions become overwhelming enough, the body may shut down as a defense mechanism. In some people, this can present as PNES.
PNES most often occur in people living with stress, anxiety, personality disorders, or other traumatic emotional conditions.
In addition, anxiety is common in people with PNES (and in people with stress).
Although PNES and neurological seizures may appear similar, there are some differences in symptoms between the two.
PNES symptoms that occur during other seizures
For example, PNES may feature some of the symptoms found in neurological seizures, such as:
- lowered awareness
- loss of body control
- flailing or thrashing
- head arching
- tongue biting
A distinguishing feature of PNES is that these symptoms tend to appear more gradually and last longer than in neurological seizures.
Symptoms unique to PNES
In addition to the symptoms above, PNES may also have symptoms that don’t traditionally occur in neurological seizures, such as:
- side-to-side head movements
- nonsynchronized body movements
- muscle contractions
- closed or fluttering eyes
- crying during the episode
- avoidant behaviors
- memory problems
Stress and mood changes
Stress affects everyone differently. In some cases, chronic stress can lead to rapid changes in your mood.
In some cases, chronic stress can lead to rapid changes in your mood.
A 2014 study on different types of psychosocial stress found that it can have a negative effect on mood.
A 2017 literature review concluded that people who experience stress-induced rapid mood changes might be more likely to experience PNES that last over 12 hours.
If you experience both rapid mood changes and PNES, it’s important to mention these when talking with a healthcare professional. This could help them make your diagnosis more precise and prescribe tailored treatment.
Anxiety symptoms can sometimes manifest as a sudden, intense episode called a panic attack.
Panic attack symptoms mimic many of the symptoms you may feel when you’re anxious. You may also notice other severe symptoms, such as:
- feelings of panic or dread
- feelings of disconnection from yourself or reality
- difficulty breathing or swallowing
- sharp chest pains
- chills or hot flashes
- numbness or tingling in the extremities
Panic attacks aren’t a known cause of neurological seizures in people without epilepsy. However, there may be a correlation between panic attacks and PNES.
However, there may be a correlation between panic attacks and PNES.
In one literature review from 2018, researchers analyzed 26 studies for a potential relationship between panic attacks, hyperventilation episodes, and PNES.
According to the results, between 17% and 83% of those who had PNES also reported having accompanying panic attacks. In addition, the researchers found that 30% of people with voluntarily induced hyperventilation also experienced PNES.
While these results seem to suggest that panic attacks and panic attack symptoms may be a trigger for PNES, more research is still necessary.
Panic attacks and PNES can both happen as a result of stress and anxiety. There are differences between the two experiences that distinguish them from each other, though.
Panic attacks feature many, if not all, of the characteristic symptoms of anxiety.
Panic attacks come on suddenly and usually pass within 10 minutes. Many people who have them are still able to retain some level of function during the attack.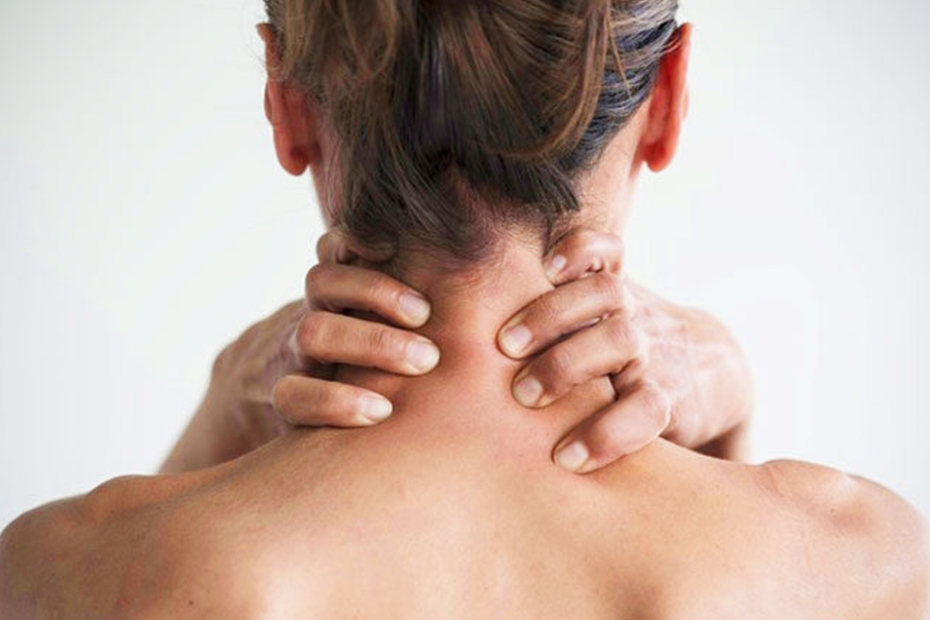 The severity of symptoms can vary from person to person.
The severity of symptoms can vary from person to person.
Many people who have PNES also experience panic symptoms, but some don’t. Episodes of PNES may not feature any symptoms of panic or anxiety at all. PNES also tend to come on gradually and last longer than panic attacks.
In some cases, panic attacks can even help a doctor differentiate between PNES and neurological seizures. In a 2014 study, researchers found that panic attack symptoms were more likely to appear in PNES than in epileptic seizures.
If you’ve been experiencing PNES, a doctor will most likely refer you to an inpatient setting for testing.
The following tests are important for building a full picture of why PNES are happening:
- Video-electroencephalography (vEEG): During your hospital stay, a doctor will connect you to an electroencephalography (EEG) machine and a video monitoring system. The EEG machine tracks electrical activity in the brain, while the video monitoring system records any physical symptoms.
 vEEG is the most common diagnostic test for PNES.
vEEG is the most common diagnostic test for PNES. - Seizure analysis: To determine the correct diagnosis, a healthcare professional may analyze any seizures that happen during your stay. If you appear to have a seizure but there’s no unusual brain activity, the most likely diagnosis is PNES.
- CT or MRI imaging: Your doctor may need to request further imaging of the brain with a CT scan or an MRI. They may also want to rule out any other underlying conditions, such as nutrient deficiency or infection.
- Psychological testing: They may also recommend additional psychological testing to narrow down potential causes or triggers.
Since PNES are often psychological in nature, it’s important to address the underlying causes and triggers. Treatment options for stress-induced PNES may include:
- psychotherapy
- medications
- lifestyle changes
Psychotherapy
Cognitive behavioral therapy (CBT) is the first-line treatment for anxiety disorders. With CBT, you can learn how to better cope with stressful or anxious thoughts, feelings, and behaviors. This may help lower the frequency of your PNES.
With CBT, you can learn how to better cope with stressful or anxious thoughts, feelings, and behaviors. This may help lower the frequency of your PNES.
In addition, trauma-focused therapy may be helpful for those who live with both trauma-based disorders and PNES.
Medications
Antiepileptic drugs aren’t effective for treating PNES, because the seizures aren’t neurological.
Instead, if you have anxiety, a healthcare professional may prescribe selective serotonin reuptake inhibitors (SSRIs) to help reduce the symptoms of anxiety and lower the number of PNES you have.
A 2017 literature review suggests that SSRIs may be most effective for anxiety when they’re used in conjunction with psychotherapy.
Lifestyle changes
Lifestyle changes can also help to reduce the symptoms of stress and anxiety.
Focusing on the following can further lower your stress and anxiety and greatly improve your quality of life:
- good sleep
- a balanced, nutritious diet
- daily exercise
- mindfulness practices such as yoga or meditation
You and a doctor can work together to come up with the best treatment approach for your personal situation.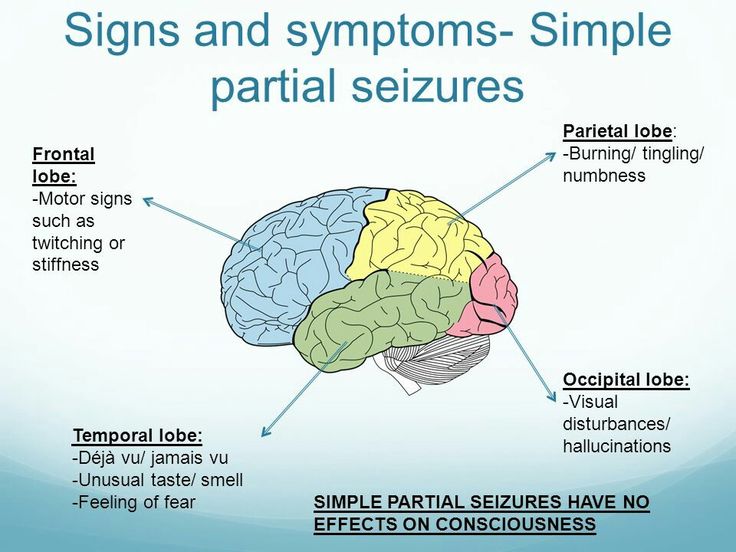
While stress and anxiety are unlikely to trigger neurological seizures in people without epilepsy, they can trigger PNES in individuals with underlying mental health conditions. Since these episodes have a psychiatric origin, addressing the underlying stress and anxiety can help reduce or eliminate these episodes.
If you’re concerned that you’ve been having PNES, reach out to a doctor for an appropriate diagnosis and treatment.
Pain and cramps in the muscles - possible causes and salvation | Health news
acmespb 02.02.2020 0 Comments
Who doesn't know about muscle discomfort? Or a sudden muscle spasm? I want to get rid of these symptoms as soon as possible. As a rule, muscle pains appear as a result of physical exertion. But is it always like this? When is pain just a harmless phenomenon, and when is it a sign of a serious illness?
Muscle spasms
Muscle spasms are the most common cause of muscle pain. Muscle spasm can develop for various reasons. It develops acutely or for a long time with chronic muscle strain. In this case, the pain can be dull, aching or, conversely, acute. It can last for several hours or months.
Muscle spasm can develop for various reasons. It develops acutely or for a long time with chronic muscle strain. In this case, the pain can be dull, aching or, conversely, acute. It can last for several hours or months.
The most common causes that lead to persistent muscle spasm:
- Prolonged muscle strain due to an uncomfortable posture in which a person works. This is the nature of back and neck pain in many office workers, leg pain in teachers and salespeople.
- Injuries where the muscles are forced to overexert themselves.
- Incorrect posture - as a result of this, certain muscle groups constantly have a large load and they are overstrained.
- Carrying the bag on one shoulder.
Muscle spasm is the most harmless cause of pain and the easiest to get rid of. Here you just need to remove the factor that led to the spasm, and do physical exercises. With persistent spasm, you will need a massage that will relieve muscle clamps.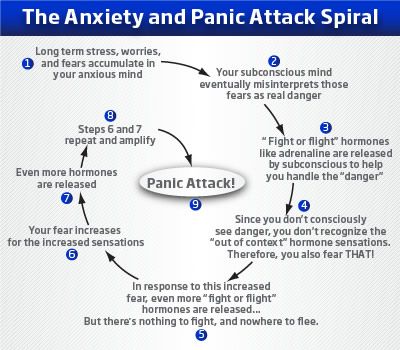
Lack of substances
Unpleasant sensations in the muscles can cause causes that a person is not even aware of. Who would think that his arms and legs hurt because there is a lack of potassium or calcium in the body, the role of which we have already written on our website a2news.ru? Meanwhile, this is a very common situation. The most unpleasant thing is that a lack of potassium can cause pain in the heart - after all, the heart is the same muscle. A person makes cardiograms, goes to doctors and gets annoyed because he is prescribed vitamins that mean nothing from his point of view. He begins to consider doctors as ignoramuses, but meanwhile all his problems can be solved by establishing electrolyte metabolism, for which it is necessary to take a complex of vitamins and minerals.
Potassium deficiency can be easily caused by taking diuretics (water pills). Needless to say, women often indulge in diuretics without advice, deciding to lose weight or get rid of puffiness under the eyes? Uncontrolled intake of diuretic herbs without supportive intake of trace elements causes incomprehensible pains in the muscles and heart.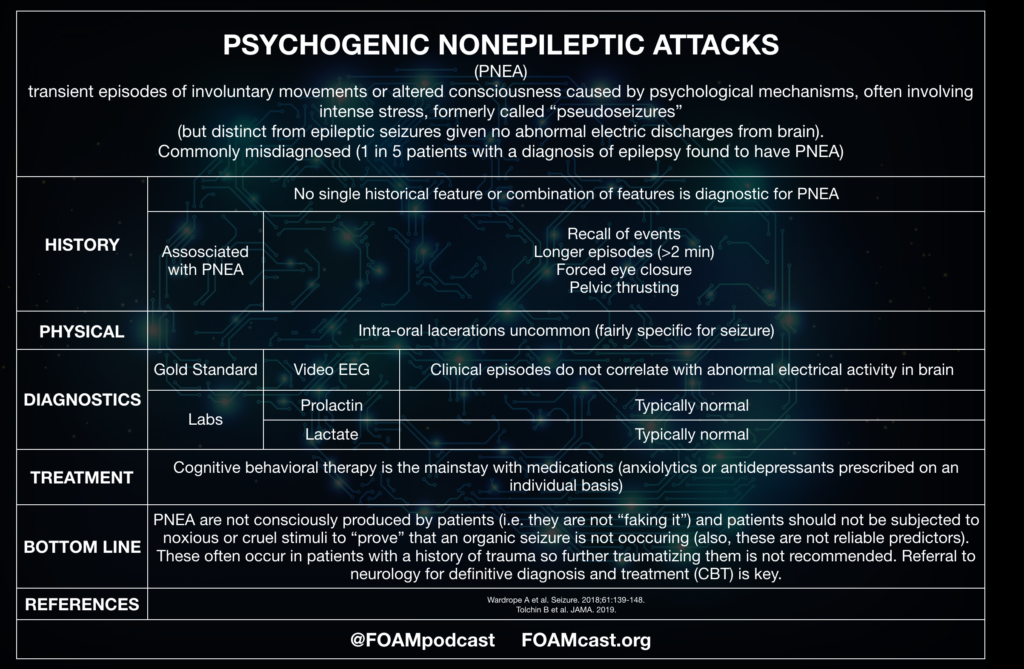
Calcium deficiency develops for various reasons. Very often it develops during the period of rapid growth of the body, during pregnancy and menopause. Osteoporosis is a more catastrophic and late consequence of calcium deficiency. And at first, you can begin to feel unpleasant aching pains in the muscles from time to time.
Mineral leaching is also possible in athletes and those who like to drive themselves in a fitness club.
This explains the way to get rid of the problem - start taking potassium and calcium as part of multivitamin complexes.
Myositis
Painful sensations in the muscles that increase with movement may be caused by myositis. Myositis is inflammation of the muscles. With it, aching pains that occur in the arms, legs, muscles of the body. Sometimes when probing the affected muscle, you can feel nodules or strands.
Myositis is caused by various causes. It appears as a result of injuries, muscle strain, as a complication after the flu. Some parasites, such as trichinella, also cause myositis. At the same time, with parasitic myositis, fever may develop.
Some parasites, such as trichinella, also cause myositis. At the same time, with parasitic myositis, fever may develop.
The nature of myositis will have to be clarified by a doctor. And only after that begin to eliminate the cause that led to it. But in any case, massage and taking vitamins will not be superfluous.
Fibromyalgia
Such pains are common - some doctors even claim that 75% of people have experienced them in one way or another. Most often, fibromyalgia affects the muscles of the shoulders, chest, neck, neck, lower back, hips near the knees. And also often these aching pains cause anxiety at night, insomnia, asthenia - weakness. The main difference between fibromyalgia is that the pain is diffused through the muscles. When pressed in areas of discomfort, you can even find the most painful points. The pain is diffuse - that is, it can appear and disappear in one place and flow to other parts of the muscles. The pain is constant and does not get worse with movement. A person has a lot of complaints, and there are almost no reasons for them in a detailed examination.
A person has a lot of complaints, and there are almost no reasons for them in a detailed examination.
Fibromyalgia can be caused by nervous and physical strain, frequent stress, trauma, lack of sleep, emotional stress, exposure to cold or dampness, rheumatic and autoimmune diseases. Interestingly, nervous and suspicious young women most often suffer from fibromyalgia. Even teenage girls can start to suffer from it. Enough to get nervous before exams. But in men, fibromyalgia often occurs due to nervous or physical overexertion. Hard workouts or rush at work are the main causes of men's suffering.
The treatment of fibromyalgia at first glance makes sufferers dumbfounded - for pain, the doctor prescribes ... valerian. But it is the use of sedatives that will be effective in this case, because the pain is more psychological in nature. If there is physical activity, it is necessary to revise the training program.
Colds, flu and other infectious diseases
Many infectious diseases (almost all!) are accompanied by muscle pain. This is explained by the fact that pathogenic microorganisms and viruses in the course of their life activity in our body cause its chronic poisoning - intoxication of the body. And with intoxication, pain in the muscles of varying intensity occurs. The more severe the cold is, the more the muscles of the body can hurt.
This is explained by the fact that pathogenic microorganisms and viruses in the course of their life activity in our body cause its chronic poisoning - intoxication of the body. And with intoxication, pain in the muscles of varying intensity occurs. The more severe the cold is, the more the muscles of the body can hurt.
Muscle pain caused by infections should not usually be confused with others. After all, the symptoms of the disease itself are obvious - temperature, chills, fever.
And there is only one treatment for pain - the treatment of the infection itself. And drinking plenty of water, which removes toxic substances from the body that cause intoxication.
Polymyalgia rheumatica
Rheumatic diseases can cause muscle pain. In this case, pain also occurs in different parts of the body.
Pain after exertion
The most natural muscle pain. It appears after a load on the muscles. Its nature is as follows: during exercise, lactic acid is produced in the muscle, which is a metabolic product of the working muscle. The more intense the workout, the more lactic acid is produced. It irritates the nerve endings in the muscles and causes a burning sensation. This process is due to physiology and is necessary for the body - acid accelerates the regeneration and restoration of muscles and destroys free radicals.
The more intense the workout, the more lactic acid is produced. It irritates the nerve endings in the muscles and causes a burning sensation. This process is due to physiology and is necessary for the body - acid accelerates the regeneration and restoration of muscles and destroys free radicals.
Lactic acid is gradually removed from the muscle through the bloodstream. To speed up this process, you can drink water with a pinch of soda.
In untrained people and with unusual or very strong exertion, muscle pain after exercise is caused not only by lactic acid, but also by microscopic ruptures of muscle fibers. Small wounds appear in the muscles, which provokes pain hours and days after the load. In principle, this is also useful for the body - the released hormones activate the healing processes and the work of the body, accelerate the metabolism of proteins and ultimately lead to muscle growth. What athletes want to achieve with training. Negative consequences occur when there are too many microtraumas - that is, when overtraining. Then the muscles are depleted, not grown.
Then the muscles are depleted, not grown.
Pain in the muscles of the legs
A very common situation with flat feet. Flat feet provokes a constant overstrain of the muscles of the lower leg, thigh and back, since these muscles are forced to take on the role of a shock absorber when walking and dampen impacts from steps, if the muscles of the foot cannot cope with this with flat feet. As a result, after a long walk or run, a person suffering from flat feet begins to hurt his legs. The pain is dull, aching, more reminiscent of heaviness.
If you are in an uncomfortable position, your legs may also ache due to circulatory disorders. Such pain disappears as soon as the posture changes and blood circulation is restored.
But pain in the legs can also be caused by more serious causes - for example, vascular disease and thrombophlebitis. Again, in this case, a chronic circulatory disorder develops, causing irritation of the nerve fibers and pain. With thrombophlebitis, the pain is characteristic - it is felt sharply along the diseased vein.
In atherosclerosis of the vessels of the lower extremities, the pain is felt like a vise.
Back pain
Back pain is not always provoked by the spine. A lot of times it's the muscles.
The most common cause of back and neck pain is osteochondrosis. There are many theories about its origin. And one of them says that compression of nerve endings is due to chronic muscle spasm.
Muscle pain is also provoked by scoliosis, wrong size of the shoulders, kyphosis, blockage of the joints. All these reasons lead to overstrain of the muscles and to an excessive load on certain muscle groups. The result is pain.
In this case, massage and supportive therapy for concomitant back diseases are useful. To avoid such problems, in childhood it is necessary to monitor the posture of the child and treat and correct the curvature of the spine in time.
Leg cramps
Everyone has experienced cramps at least once in their life. Especially often the muscles of the foot, fingers, calves are cramped. From a physiological point of view, cramps are a sharp contraction and spasm of muscles caused by impaired blood circulation or physical stress.
From a physiological point of view, cramps are a sharp contraction and spasm of muscles caused by impaired blood circulation or physical stress.
A common cause of convulsions may be an unsuccessful movement or monotonous repetitive movements. Such cramps develop in people who type a lot on a computer or play with a computer mouse, work on their feet, and exercise intensively.
Leg cramps are often caused by a lack of calcium and potassium salts in the body. This often occurs with intense training, taking diuretics, and dehydration.
Night cramps can be caused by circulation problems. And here we must look for the cause of this, which may lie in osteochondrosis and other diseases.
If the liver ceases to cope with its role as a neutralizer of toxins, then the body begins to accumulate harmful substances in tissues, including muscles. This can cause seizures.
Frequent seizures can be caused by epilepsy, neurosis, metabolic disorders, various endocrine disorders, varicose veins.
If convulsions recur frequently, you should consult a doctor and find out the cause of their occurrence. If the fault is just muscle strain and salt deficiency, then it’s enough just to normalize your diet and stop overloading your muscles too much.
Pain and cramps are always an indication that the body does not like something. Most often, eliminating their causes is not difficult. Enough rest and good nutrition. But if muscle pain becomes constant, then it is best to consult a doctor to find out the cause and eliminate it.
Source A2News.ru
90,000 Psychosomatics of diseases: Psychological causes of diseasesAuthor: Tsaru Evgeny Grigoryevich
[[Blockquote Text = "Studies show that physical disorders associated with mental stress arise due to the hyperactivity of nerve impulses sent from the brain to other parts of the body, which can cause the secretion of adrenaline into the blood, resulting in a state of anxiety. This state can be caused by various life factors. "]]
"]]
[[blockquote text="Lack of social support - in the form of a loved one with whom to share all difficulties or problems - also increases the likelihood of further heart attacks."]]
[[blockquote text="Doc.ua urges not physical or psychological ."]]
[[doctor text="Make an appointment with a doctor"]]
Since there is a belief that all emotional and psychological pain is reflected by various diseases of the body, and this phenomenon is called psychosomatics.
What is psychosomatics?
It was once believed that psychosomatic disorders (hereinafter referred to as psychosomatics) are a separate group of disorders in which stress and psychological stress lead to psychosomatic illness. Examples were peptic ulcer, arthritis and dermatitis. It is now recognized that the causes of psychosomatics may have social, psychological and behavioral aspects, as well as physical organic features.
The World Health Organization defines psychosomatic medicine as "the study of the biological, psychological and social variables in health and disease."
What causes psychosomatics?
Research shows that the physical disorders associated with mental stress are due to overactivity of nerve impulses sent from the brain to other parts of the body, which can cause the secretion of adrenaline into the bloodstream, resulting in a state of anxiety. This condition can be caused by various life factors.
The following causes of psychosomatic illness may make people more likely to experience somatic symptoms:
- Genetics: Several studies have suggested that certain genetic abnormalities in a person can directly cause this condition.
- irregular biological conditions: alteration of glucose metabolism, serum amino acid levels, etc.
 May cause psychosomatic disturbance.
May cause psychosomatic disturbance. - effects of stress: people who experience stressful events such as trauma, abuse, frequent illness, fear, depression, anger, guilt, insecurity and other difficult situations are also susceptible to this disorder.
- family circumstances: absence of parents, parental behavior towards the child and relationship difficulties are also the main causes of psychosomatic disorders.
Psychology and illness are directly linked, so psychosomatic illnesses resulting from stress can include hypertension, respiratory problems, gastrointestinal disorders, migraine and tension headaches, heart pain, and others.
This is best illustrated by heart disease, which is caused by many factors. These include:
congenital biological factors: age, sex and genetic characteristics that increase the likelihood of a heart attack;
physiological factors: high blood pressure, smoking, alcohol consumption and high blood cholesterol;
psychological and social factors: including depression, anxiety, and certain forms of stress that are associated with a risk of having a heart attack or an increased chance of dying thereafter.
Stress can cause anxiety or depressive disorders, which can lead to palpitations and an increased chance of irregular heartbeats, which can be fatal shortly after a heart attack.
Lack of social support - in the form of a loved one with whom you can share all the difficulties or problems - also increases the likelihood of further heart attacks.
Thus, the modern view of psychosomatic mechanisms includes the role of stress, depression and lack of social support along with biological factors in the causes or outcome of the disease. The relative importance of environmental stress varies across settings.
Main categories of psychosomatic disorders
There are three main categories of psychosomatic diseases.
In the first case, a person suffers from a mental and physical illness, the symptoms and treatment of which complicate each other.
The second category includes people suffering from mental disorders due to illness and treatment. For example, patients feel depressed because they have cancer and are being treated for it.
For example, patients feel depressed because they have cancer and are being treated for it.
The third type is called somatoform disorder. It is a condition in which a person with a mental illness experiences one or more physical symptoms, even if they do not have any associated illness.
Hypochondria: is a condition in which a person considers a minor physical symptom to be a serious illness. For example, the transformation of a temporary problem with flatulence into inflammation of the intestines psychosomatically and colon cancer.
Conversion disorder: when a person who does not suffer from any disease develops neurological symptoms such as psychosomatic speech problems, seizures and others that affect movement and feelings.
Somatization disorder: where the person experiences frequent headaches and diarrhea that is not associated with a serious illness.
Body Dysmorphic Disorder: a person experiences stress due to the appearance of their body, such as psychosomatic edema, wrinkles and obesity. Here a person suffers severely from anorexia.
Here a person suffers severely from anorexia.
Pain disorder: where the person experiences severe pain in any part of the body that can last from six months to one year without any physical cause - e.g. migraine, tension headaches, back pain, etc.
Risk factors for psychosomatic disorders
Doc.ua urges not to refuse treatment and seek medical help if any symptoms of the disease appear, physical or psychological .
Psychological factors can change the state of health to a certain extent. For example:
Diabetes: Type 2 diabetic patients are more susceptible to stress-related hypertension. The same stressors of hypertension exacerbate the diabetic condition.
Psychological causes of illness
Some illnesses are caused by mental stress, such as:
Cancer: Research has shown that psychological stress can affect the ability of tumors to grow and spread, thereby making cancer worse.
According to psychosomatics, oncological diseases testify to old grievances that you have harbored deep within yourself. The psychological causes of illness include feelings of dislike, hatred, remorse, some secret or grief that you have hidden deep within yourself.
- Neoplasms, cysts, tumors in psychosomatics - keeping old insults and upheavals in oneself, accumulating them in one place of one's body provokes the appearance of a malignant or even benign tumor in psychosomatics.
- Cancer psychosomatics is an old hidden grudge against someone or something, the feeling of revenge for which literally “devours” the body. A deep, unhealed spiritual wound that provokes an internal conflict with oneself and the outside world. Strong experiences on this basis can cause both heart cancer and other types of it, such as kidney cancer.
Hypertension: negative emotional state, frequent stress and social factors such as economic status and life events are indirectly related to blood pressure levels.
Heart disease: studies have shown that the development of coronary heart disease may be associated with depression, anxiety and stress.
Women's diseases according to psychosomatics (erosion, thrush, inflammation of the uterus, infectious diseases) occur when a woman does not accept something in herself, for example, her appearance, character or behavior. Diseases of the female genital organs can be associated with an unsatisfactory relationship with a man or with the avoidance and denial of men in general.
Breathing problems: emotional stress is a major factor in the development of asthma.
Bowel problems : peptic ulcer formation is associated with stressful life events in a person. For example:
- diarrhea psychosomatics - strong anxiety and fear, feeling of insecurity, fear of accepting future events out of fear, which is why the psychosomatics of this bowel disease often manifests itself before important events;
- flatulence (bloating) psychosomatics - occurs due to the inability of a person to “digest” some events that have happened.
 The psychosomatics of the stomach has similar causes: the inability to "digest" or "assimilate" new ideas and events. Fear and anxiety about this immediately affect the health of the stomach.
The psychosomatics of the stomach has similar causes: the inability to "digest" or "assimilate" new ideas and events. Fear and anxiety about this immediately affect the health of the stomach.
Allergy. According to psychosomatics, allergies occur in those who refuse to accept something in their lives. Allergy according to psychosomatics is a denial of one's strength. The psychosomatics of allergy is negative emotions, accumulating inside, lead the body to the denial of some external phenomenon.
Skin diseases (psychosomatic psoriasis, psychosomatic burns, acne, acne). Skin is the outer cover of the human body, which is designed to protect internal organs from direct external influences. Therefore, our subconscious associates this organ as a defense of individuality. The appearance of skin diseases and dermatological problems indicates the presence of psychosomatic problems.
Psychosomatics of kidney disease ( pain in the kidneys according to psychosomatics, inflammation of the kidneys, colic in the kidneys) occurs in those who in their lives often endured criticism, disappointment, perhaps they were disgraced by something. Remembering all their failures, such people often withdraw into themselves and live on their own failures, which leads to kidney disease.
Remembering all their failures, such people often withdraw into themselves and live on their own failures, which leads to kidney disease.
How is psychosomatic pain and other somatic symptoms treated?
People with somatic pain symptoms can benefit from several therapies, including:
- cognitive behavioral therapy;
- medicines, eg antidepressants;
- mind - fullness therapy;
- assistance from a psychiatrist or psychotherapist;
- regular contact with the attending physician.
5
Evgeniy Tsaruk
Doctor of the highest category
Effective treatment of working capacity disorders, depressive conditions, chronic fatigue syndrome, fears, anxiety, apathy and lethargy, sleep disturbance, schizophrenia, mental disorders in elderly and senile people. Therapeutic and preventive work among patients of psychiatric, narcological profiles. initial examination of the patient, the establishment of a preliminary diagnosis, the appointment of treatment, with further selection of supportive treatment.














