Increasing prozac dosage
Relapse in patients on long-term fluoxetine treatment: response to increased fluoxetine dose
Clinical Trial
. 1995 Feb;56(2):52-5.
M Fava 1 , S M Rappe, J A Pava, A A Nierenberg, J E Alpert, J F Rosenbaum
Affiliations
Affiliation
- 1 Depression Research Program, Massachusetts General Hospital, Boston 02114.
- PMID: 7852252
Clinical Trial
M Fava et al. J Clin Psychiatry. 1995 Feb.
. 1995 Feb;56(2):52-5.
Authors
M Fava 1 , S M Rappe, J A Pava, A A Nierenberg, J E Alpert, J F Rosenbaum
Affiliation
- 1 Depression Research Program, Massachusetts General Hospital, Boston 02114.
- PMID: 7852252
Abstract
Background: Although several studies have examined the long-term efficacy of antidepressants, relatively little attention has been paid to the management of relapses or recurrences during continued antidepressant treatment. This study examined whether depressed patients who had recovered and then relapsed on fluoxetine 20 mg/day would benefit from an increase in fluoxetine dose.
Method: Eighteen patients who relapsed on fluoxetine 20 mg/day during long-term treatment with fluoxetine as part of a placebo-controlled study had their fluoxetine dose raised to 40 mg/day and were followed for at least 1 month (mean time = 4.7 months).
Results: Twelve (67%) were full responders, 3 (17%) partial responders, and 3 (17%) dropped out because of side effects (e.g., insomnia and agitation). Of those patients who had either full or partial response (N = 15; 83%), 3 complete responders had a recurrence on 40 mg/day after a mean of 5.8 months and 1 partial responder had a recurrence 11 months later. Overall, 11 (61%) of 18 patients maintained their response during their follow-up while taking the higher dose of fluoxetine.
Conclusion: An increase in dose of fluoxetine to 40 mg/day appears to be an effective strategy in the treatment of relapse among depressed patients who had initially responded to fluoxetine 20 mg/day.
Similar articles
-
Eighteen months of drug treatment for depression: predicting relapse and recovery.

Mulder RT, Frampton CM, Luty SE, Joyce PR. Mulder RT, et al. J Affect Disord. 2009 Apr;114(1-3):263-70. doi: 10.1016/j.jad.2008.08.002. Epub 2008 Sep 20. J Affect Disord. 2009. PMID: 18805590 Clinical Trial.
-
Efficacy in long-term treatment of depression.
Montgomery SA. Montgomery SA. J Clin Psychiatry. 1996;57 Suppl 2:24-30. J Clin Psychiatry. 1996. PMID: 8626360 Review.
-
Early fluoxetine treatment of post-stroke depression--a three-month double-blind placebo-controlled study with an open-label long-term follow up.
Fruehwald S, Gatterbauer E, Rehak P, Baumhackl U. Fruehwald S, et al. J Neurol. 2003 Mar;250(3):347-51. doi: 10.1007/s00415-003-1014-3. J Neurol.
 2003. PMID: 12638027 Clinical Trial.
2003. PMID: 12638027 Clinical Trial. -
Use of low-dose fluoxetine in major depression and panic disorder.
Louie AK, Lewis TB, Lannon RA. Louie AK, et al. J Clin Psychiatry. 1993 Nov;54(11):435-8. J Clin Psychiatry. 1993. PMID: 8270588 Clinical Trial.
-
[Value of fluoxetine in obsessive-compulsive disorder in the adult: review of the literature].
Etain B, Bonnet-Perrin E. Etain B, et al. Encephale. 2001 May-Jun;27(3):280-9. Encephale. 2001. PMID: 11488259 Review. French.
See all similar articles
Cited by
-
Failure to Respond after Reinstatement of Antidepressant Medication: A Systematic Review.

Bosman RC, Waumans RC, Jacobs GE, Oude Voshaar RC, Muntingh ADT, Batelaan NM, van Balkom AJLM. Bosman RC, et al. Psychother Psychosom. 2018;87(5):268-275. doi: 10.1159/000491550. Epub 2018 Jul 24. Psychother Psychosom. 2018. PMID: 30041180 Free PMC article. Review.
-
Current Perspectives on the Diagnosis and Treatment of Double Depression.
Hellerstein DJ, Little SA. Hellerstein DJ, et al. CNS Drugs. 1996 May;5(5):344-57. doi: 10.2165/00023210-199605050-00004. CNS Drugs. 1996. PMID: 26071047
-
Identification and treatment of antidepressant tachyphylaxis.
Targum SD. Targum SD. Innov Clin Neurosci. 2014 Mar;11(3-4):24-8. Innov Clin Neurosci. 2014. PMID: 24800130 Free PMC article.
 Review.
Review. -
Treatment-resistant depression: therapeutic trends, challenges, and future directions.
Al-Harbi KS. Al-Harbi KS. Patient Prefer Adherence. 2012;6:369-88. doi: 10.2147/PPA.S29716. Epub 2012 May 1. Patient Prefer Adherence. 2012. PMID: 22654508 Free PMC article.
-
The clinical pharmacology of depressive states.
Schulz P, Macher JP. Schulz P, et al. Dialogues Clin Neurosci. 2002 Mar;4(1):47-56. doi: 10.31887/DCNS.2002.4.1/pschulz. Dialogues Clin Neurosci. 2002. PMID: 22034133 Free PMC article.
See all "Cited by" articles
Publication types
MeSH terms
Substances
Prozac® Dosage Guide | hims
Fluoxetine, commonly sold as Prozac®, is an antidepressant that’s used to treat several mental health conditions.
As a selective serotonin reuptake inhibitor, Prozac and generic fluoxetine work by increasing the amount of serotonin in your brain.
Many people who use Prozac and similar types of medication find that they’re effective at controlling their symptoms and improving their mood.
Prozac is prescribed in a range of dosages to treat several conditions, including depression and certain anxiety disorders.
Below, we’ve explained what Prozac is and how it works as an antidepressant.
We’ve also listed typical dosages of Prozac for conditions such as major depressive disorder, panic disorder and obsessive-compulsive disorder (OCD).
Finally, we’ve listed the key side effects and potential interactions that you should be aware of if you’re prescribed Prozac or generic fluoxetine.
What Is Prozac?Prozac is a brand name for fluoxetine, a selective serotonin reuptake inhibitor (SSRI). Prozac is prescribed to treat a range of mental health conditions, including the following:
Major depressive disorder (MDD, or major depression)
Obsessive-compulsive disorder (OCD)
Panic disorder, with or without agoraphobia
Bulimia nervosa
In some cases, Prozac may be combined with other medications to treat specific conditions. For example, a combination of Prozac and olanzapine (Zyprexa®) is often used to treat depressive episodes associated with bipolar disorder, as well as treatment-resistant depression.
For example, a combination of Prozac and olanzapine (Zyprexa®) is often used to treat depressive episodes associated with bipolar disorder, as well as treatment-resistant depression.
If you’ve been diagnosed with any of the conditions mentioned above, your healthcare provider may recommend Prozac or a similar medication to manage your symptoms and help you make progress towards recovery.
Our guide to SSRIs goes into more detail about how Prozac and other medications in this class work to treat depression, anxiety and other mental health conditions.
Prozac DosagesProzac is used to treat several mental health conditions. Your dosage of Prozac may vary based on the specific mental health issue you’re facing and the severity of your symptoms.
We’ve listed the typical dosages of Prozac for depression, obsessive-compulsive disorder, panic disorder and other conditions below.
Prozac Dosage for DepressionProzac is most commonly used to treat depression. The standard dosage for major depressive disorder is 20mg per day, taken in the morning.
The standard dosage for major depressive disorder is 20mg per day, taken in the morning.
Research shows that this dosage produces an improvement for most people with depression.
As with other SSRIs, the effects of Prozac aren’t instant. It may take several weeks for Prozac to produce a noticeable improvement in your mood and other depression symptoms.
If you don’t experience any positive change in your mood after taking Prozac at this dosage for several weeks, your healthcare provider may adjust your dosage up to a maximum of 80mg of Prozac (or generic fluoxetine) per day.
At dosages of 20mg or more per day, your healthcare provider may instruct you to take Prozac in the morning and later in the day in separate doses.
In children, Prozac is typically used at a lower dosage of 10mg per day. This may be adjusted over time based on the child’s response to the medication.
online counseling
the best way to try counseling
Prozac Dosage for Obsessive-Compulsive Disorder (OCD)Prozac is prescribed to treat obsessive-compulsive disorder (OCD) at a starting dosage of 20mg per day, taken in the morning.
If this dosage isn’t effective after several weeks, it may be adjusted up to a maximum dosage of 60mg per day.
If you’re prescribed Prozac at a dosage greater than 20mg per day, you may be instructed to take your medication twice daily (for example, in the morning and at noon).
In children and adolescents with OCD, Prozac is typically used at a starting dosage of 10mg per day.
This may be adjusted over time based on the child or adolescent’s symptoms and overall response to the medication.
Prozac Dosage for Panic DisorderProzac is typically prescribed to treat panic disorder at a starting dosage of 10mg per day. This may be increased to 20mg per day after one week.
If you do not experience improvements from Prozac at a daily dosage of 20mg, your healthcare provider may increase your dosage up to a maximum of 60mg per day.
Prozac Dosage for Bulimia NervosaProzac is prescribed at a dosage of 60mg per day to treat bulimia nervosa, or bulimia. If you’re prescribed Prozac for this purpose, your healthcare provider may instruct you to slowly increase your dosage up to 60mg per day over several days or weeks.
If you’re prescribed Prozac for this purpose, your healthcare provider may instruct you to slowly increase your dosage up to 60mg per day over several days or weeks.
Currently, research shows that lower dosages of Prozac (for example, dosages similar to those used to treat depression) are not effective at treating bulimia nervosa
Prozac vs. Prozac Weekly™Prozac comes in two forms: daily-use Prozac and Prozac Weekly. The weekly version of Prozac contains a larger dosage of fluoxetine and has an enteric coating that slows down its absorption and release into your bloodstream.
Each Prozac Weekly capsule contains 90mg of fluoxetine. As its name suggests, you’ll need to take this form of Prozac one time per week.
Your healthcare provider may prescribe this long-acting version of Prozac if you’ve shown good results with the daily-use version of Prozac.
Make sure to closely follow your healthcare provider’s instructions and use Prozac Weekly only as prescribed.
Currently, the brand name medication Prozac is only manufactured in capsule form as Prozac or Prozac Daily.
Generic fluoxetine (the active ingredient in Prozac and Prozac Daily) is available as a capsule, a tablet and as a liquid solution for oral use.
If you use generic fluoxetine, it’s important to check the dosage form and verify that you’re using the correct amount of this medication.
Prozac Side Effects & InteractionsProzac is a common medication that’s used by millions of people in the United States. Although it’s a safe and effective medication for most people when used as directed, it can cause a range of side effects.
Common side effects of Prozac and generic fluoxetine include:
Abnormal dreams
Abnormal ejaculation (difficulty ejaculating)
Anorexia
Anxiety
Asthenia (physical weakness or lack of energy)
Decreased libido
Diarrhea
Dry mouth
Dyspepsia (indigestion)
Flu-like symptoms
Impotence (erectile dysfunction)
Insomnia
Nausea
Nervousness
Pharyngitis (sore throat)
Rash
Sinusitis (sinus inflammation)
Somnolence (drowsiness or sleepiness)
Sweating
Tremor (involuntary shaking)
Vasodilation
Yawning
These side effects may first start to occur during the first few weeks of treatment and improve on their own over time.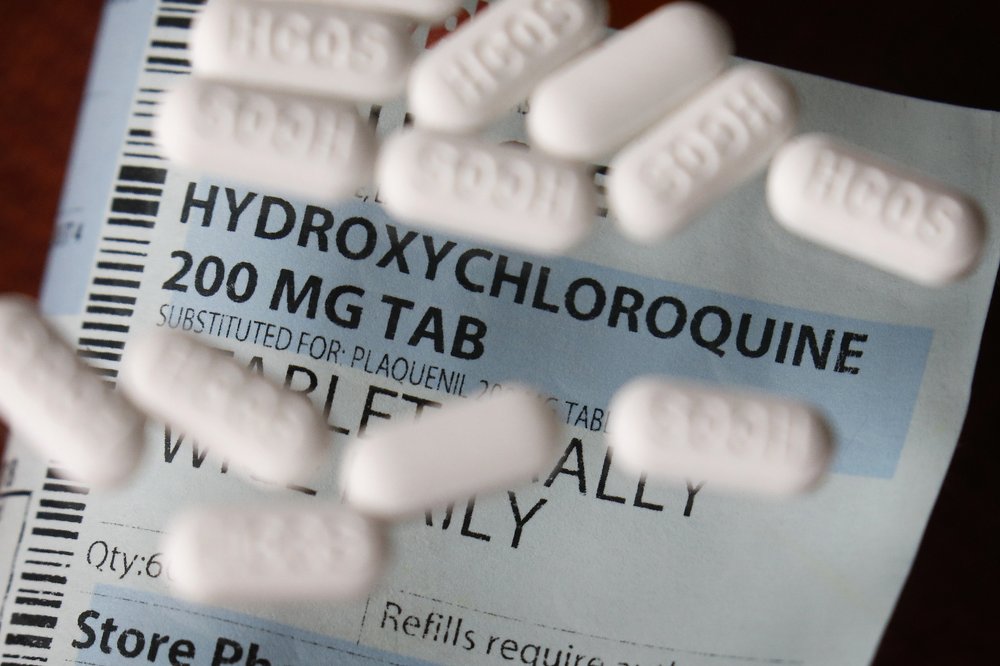
If you experience persistent side effects after you start treatment with Prozac, it’s important to inform your healthcare provider.
They may suggest making changes to the way you take your medication, such as using it in the morning only or with a meal.
Although rare, Prozac can cause more serious side effects, including worsening of depression symptoms, seizures, mania and, in some cases, allergic reactions that may involve swelling in the face, mouth, tongue and eyes, rash, itching and difficulty breathing or swallowing.
Like other SSRIs, Prozac carries a black box warning from the FDA notifying of an increase in the risk of suicidal thoughts and behavior in adults up to 24 years of age.
Our guide to Prozac and generic fluoxetine side effects goes into these side effects and goes into more detail about how and why they can occur.
If you experience any severe side effects after using Prozac, contact your healthcare provider as soon as possible.
As an SSRI, Prozac may interact with other medications that affect serotonin levels, including other antidepressants. In some cases, this can lead to a life-threatening reaction referred to as serotonin syndrome.
In some cases, this can lead to a life-threatening reaction referred to as serotonin syndrome.
Prozac and other SSRIs are particularly dangerous to use with monoamine oxidase inhibitors (MAOIs), an older class of antidepressants.
These medications can linger inside the body for weeks at a time and cause severe and unsafe interactions.
Other medications and supplements, including pain medications and over-the-counter products such as St. John’s wort, can also interact with Prozac and other SSRIs used to treat depression, OCD, panic disorder and other conditions.
To avoid interactions, make sure to inform your healthcare provider about all medications you currently use or have recently used before using Prozac.
How to Use Prozac EffectivelyYour healthcare provider may prescribe Prozac if you’ve been diagnosed with depression, panic disorder, obsessive-compulsive disorder (OCD) or bulimia nervosa.
To get the best effects from Prozac, make sure to:
Take Prozac exactly as directed.
 If you’re prescribed Prozac for use once per day, take it in the morning. If you need to take Prozac twice per day, your healthcare provider will typically recommend taking one dose in the morning and the other at noon.If you’re prone to insomnia, your healthcare provider may suggest only taking Prozac in the morning.
If you’re prescribed Prozac for use once per day, take it in the morning. If you need to take Prozac twice per day, your healthcare provider will typically recommend taking one dose in the morning and the other at noon.If you’re prone to insomnia, your healthcare provider may suggest only taking Prozac in the morning.
Expect to wait several weeks for noticeable results. Prozac works, but results aren’t immediate. Keep using your medication every day, even if you don’t notice any changes in your symptoms during the first few weeks of treatment.
online psychiatrist prescriptions
talk to a psychiatry provider. it’s never been easier
Guide to Prozac DosagesProzac is one of the most well-known and widely-used medications for depression. It’s typically prescribed at a dosage of 10 to 80mg per day to treat mental health issues such as depression, panic disorder, obsessive-compulsive disorder and bulimia nervosa.
If you’re prescribed Prozac or generic fluoxetine, make sure to follow your healthcare provider’s instructions and only use your medication as directed.
You can learn more about Prozac and similar medications in our complete list of medications for depression. You can also access our complete range of mental health resources online to learn more about depression, anxiety, stress and other common conditions.
2 Sources
Hims & Hers has strict sourcing guidelines to ensure our content is accurate and current. We rely on peer-reviewed studies, academic research institutions, and medical associations. We strive to use primary sources and refrain from using tertiary references.
- PROZAC (fluoxetine capsules) for oral use. (2017, January). Retrieved from https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/018936s108lbl.pdf
- Fluoxetine. (2020, March 15). Retrieved from https://medlineplus.gov/druginfo/meds/a689006.html
This article is for informational purposes only and does not constitute medical advice. The information contained herein is not a substitute for and should never be relied upon for professional medical advice. Always talk to your doctor about the risks and benefits of any treatment. Learn more about our editorial standards here.
Always talk to your doctor about the risks and benefits of any treatment. Learn more about our editorial standards here.
| 💊 Ingredients of Prozac ® ✅ How to use Prozac ® Save Search for analogues Interaction Description of the active ingredients of the preparation Prozac ® (Prozac ® ) The scientific information provided is general and cannot be used to make decisions. Update date: 2020.06.09 Marketing authorization holder:ELI LILLY VOSTOK, S.A. (Switzerland)
Made:PATHEON FRANCE, S.A.S. (France) ATX code: N06AB03 (Fluoxetine) Active substance: fluoxetine (fluoxetine) Rec.INN WHO registered Dosage form
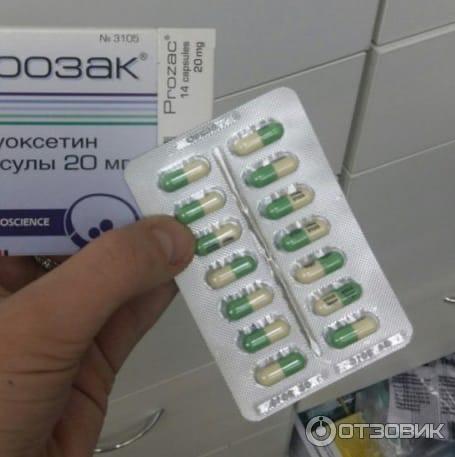
Release form, packaging and composition Prozac®Capsules hard gelatin capsules, size #3, opaque, green/cream, imprinted with the LILLY logo and the identification code "3105"; the contents of the capsules are white powder.0008
Excipients : starch, dimethicone. Composition of the capsule shell: patented blue dye (patent blue V dye), iron oxide yellow dye, titanium dioxide, gelatin, food ink (for identification printing). 14 pcs. - blisters (1) - packs of cardboard. Clinical and pharmacological group: Antidepressant Pharmacotherapeutic group: Antidepressant Pharmacological actionAntidepressant, propylamine derivative. The mechanism of action is associated with selective blockade of neuronal reuptake of serotonin in the CNS. Fluoxetine is a weak antagonist of cholino-, adreno- and histamine receptors. Unlike most antidepressants, fluoxetine does not appear to cause a decrease in the functional activity of postsynaptic β-adrenergic receptors. Helps improve mood, reduces feelings of fear and tension, eliminates dysphoria. Does not cause sedation. When taken in average therapeutic doses, it practically does not affect the functions of the cardiovascular and other systems. Pharmacokinetics Absorbed from the gastrointestinal tract. Weakly metabolized during the "first pass" through the liver. T 1/2 fluoxetine is 2-3 days, norfluoxetine is 7-9 days. Excreted by the kidneys 80% and through the intestines - about 15%. Indications of the active substances of the drug Prozac®Depression of various origins, obsessive-compulsive disorders, bulimic neurosis. Open list of ICD-10 codes
Dosage regimenThe method of administration and dosing regimen of a particular drug depends on its form of release and other factors. The optimal dosage regimen is determined by the doctor. Compliance of the dosage form of a particular drug with indications for use and dosing regimen should be strictly observed. Initial dose - 20 mg 1 time / day in the morning; if necessary, the dose can be increased after 3-4 weeks. The frequency of admission is 2-3 times / day. The maximum daily oral dose of for adults is 80 mg. Side effects From the side of the central nervous system: possible anxiety, tremor, nervousness, drowsiness, headache, sleep disturbances. From the digestive system: possible diarrhea, nausea. From the side of metabolism: may increase sweating, hypoglycemia, hyponatremia (especially in elderly patients and with hypovolemia). From the reproductive system: decreased libido. Allergic reactions: possible skin rash, itching. Other: joint and muscle pain, shortness of breath, fever. Contraindications for useGlaucoma, bladder atony, severe renal dysfunction, benign prostatic hyperplasia, simultaneous administration of MAO inhibitors, convulsive syndrome of various origins, epilepsy, pregnancy, lactation, hypersensitivity to fluoxetine. Use in pregnancy and lactationContraindicated in pregnancy and lactation. Use in hepatic impairmentUse with extreme caution in patients with hepatic impairment. Use in impaired renal function Contraindicated in severe renal impairment. Use in childrenThe safety of fluoxetine in children has not been established. Use in elderly patientsElderly patients require dosage adjustment. Special instructionsUse with extreme caution in patients with impaired liver and kidney function, with a history of epileptic seizures, cardiovascular diseases. In patients with diabetes mellitus, changes in blood glucose levels are possible, which requires correction of the dosing regimen of hypoglycemic drugs. When used in debilitated patients while taking fluoxetine, the likelihood of developing epileptic seizures increases. With the simultaneous use of fluoxetine and electroconvulsive therapy, the development of prolonged epileptic seizures is possible. Fluoxetine can be used no earlier than 14 days after discontinuation of MAO inhibitors. The period after the abolition of fluoxetine before the start of therapy with MAO inhibitors should be at least 5 weeks. Elderly patients require dosage adjustment. The safety of fluoxetine in children has not been established. Do not drink alcohol during treatment. Influence on the ability to drive vehicles and mechanisms During the period of treatment, one should refrain from potentially hazardous activities that require increased attention and rapid psychomotor reactions. Drug InteractionsWhen used simultaneously with drugs that have a depressant effect on the central nervous system, with ethanol, a significant increase in the inhibitory effect on the central nervous system, as well as an increase in the likelihood of convulsions, is possible. With simultaneous use with MAO inhibitors, furazolidone, procarbazine, tryptophan, serotonin syndrome may develop (confusion, hypomania, restlessness, agitation, convulsions, dysarthria, hypertensive crisis, chills, tremor, nausea, vomiting, diarrhea). With simultaneous use, fluoxetine inhibits the metabolism of tricyclic and tetracyclic antidepressants, trazodone, carbamazepine, diazepam, metoprolol, terfenadine, phenytoin, which leads to an increase in their concentration in blood serum, an increase in their therapeutic and side effects. With simultaneous use, inhibition of the biotransformation of drugs metabolized with the participation of the CYP2D6 isoenzyme is possible. When used simultaneously with hypoglycemic agents, their effect may be enhanced. There have been reports of increased effects of warfarin when co-administered with fluoxetine. When used simultaneously with haloperidol, fluphenazine, maprotiline, metoclopramide, perphenazine, periciazine, pimozide, risperidone, sulpiride, trifluoperazine, cases of extrapyramidal symptoms and dystonia have been described; with dextromethorphan - a case of the development of hallucinations is described; with digoxin - a case of increasing the concentration of digoxin in the blood plasma. When used simultaneously with lithium salts, an increase or decrease in the concentration of lithium in the blood plasma is possible. With simultaneous use, it is possible to increase the concentration of imipramine or desipramine in the blood plasma by 2-10 times (may persist for 3 weeks after fluoxetine is discontinued). When used simultaneously with propofol, a case is described in which spontaneous movements were observed; with phenylpropanolamine - a case is described in which dizziness, weight loss, hyperactivity were observed. Co-administration may enhance the effects of flecainide, mexiletine, propafenone, thioridazine, zuclopenthixol. Keep |
How we are treated: Prozac. From depression to bulimia
Medicine
16:00, December 14, 2017
Analysis of one of the popular antidepressants how it is customary to treat them and whether the antidepressant Prozac works, read in the new material of the heading “How we are treated”.
Prozac is on the list of the most important, safest and most effective (including from an economic point of view) drugs according to the World Health Organization. However, as we remember after the article with the analysis of Tamiflu, this does not guarantee its effectiveness.
Prozac is prescribed for the treatment of depression, obsessive-compulsive disorders, bulimia nervosa. If you know very well what it is, you can immediately skip to the “from what, from what” part.
When life is not nice
Depression is called depression, loss of interest in what used to make the patient happy. According to the international classification of diseases ICD-10, the main criteria by which such a diagnosis can be made include depressed mood for more than two weeks, loss of strength and consistently high fatigue (more than a month) and anhedonia (the inability to enjoy what used to bring joy). Doctors consider additional criteria for depression to be pessimism, low self-esteem, thoughts of death and suicide, appetite disturbances (weight loss or overeating), sleep problems, constant fears and anxieties, feelings of worthlessness and guilt, inability to concentrate, and a constant sweet taste in the mouth. These symptoms are unlikely to occur simultaneously (for example, fatigue and apathy may predominate in some cases, while anxiety and guilt may prevail in others), therefore, in order to diagnose depression, the patient's condition must meet at least two main criteria and three additional ones. At the same time, according to the definition of the US National Institute of Mental Health, such a state should last quite a long time (more than two weeks).
At the same time, according to the definition of the US National Institute of Mental Health, such a state should last quite a long time (more than two weeks).
Severe depression (clinical) includes a complex set of symptoms called major depressive disorder and may sometimes not be accompanied by low mood at all. However, because of her, the patient is physically unable to live and work normally, and the comments of those around him in the spirit of “he just can’t pull himself together” or “enough to turn sour that he spread snot” sound like a mockery. Such phrases stigmatize depression, blaming a person for his condition, while he himself will not be able to cope and needs treatment. To diagnose major depressive disorder, there is a whole questionnaire of major depression compiled by the World Health Organization. Also, depressive disorders include other conditions accompanied by depression, such as dysthymia (daily low mood and mild symptoms of depression for two years or more).
The causes of depression can be very different: somatic (due to diseases of the body), psychological (after strong dramatic experiences, such as the death of a relative) and iatrogenic (as a side effect of certain drugs). As strange as it would be to provide first aid to a victim of an electric shock without removing the wire from him, it is difficult to cure the symptoms of depression without eliminating its cause or changing the lifestyle that led the patient to such a state. If the patient lacks some essential substances (for example, tryptophan), it is important to make up for their lack, and not just fight the depressed mood with drugs. If he has some kind of psychological trauma, the help of a psychotherapist will be required. And for a person whose depression is provoked by hormonal disorders, neurological diseases, heart disease, diabetes, or even cancer (and this happens), it is more important to cure the disease itself, and symptomatic treatment of depression will be a secondary goal.
When you can't stop
Obsessive-compulsive disorder, or OCD (also called obsessive-compulsive disorder), consists of two mandatory components: obsessions (obsessive anxious or frightening thoughts) and compulsions (compulsive actions). A classic example is cleanliness-related OCD, where a person is afraid of contamination or contamination by microorganisms. Such thoughts and fears are called obsessions. In order to protect themselves from them, a person will worry too much about cleanliness, such as constantly washing their hands. Any contact with a non-sterile, according to the patient, object, plunges such a person into horror. And if you can’t wash your hands again, he will experience real suffering.
You can learn how to understand medicines on your own in the author's online course "How We Are Treated" by the editor of Indicator.Ru Ekaterina Mishchenko: https://clck.ru/Pnmtk
This "protective" behavior is called compulsion. The desire for cleanliness can be understood if a person is in conditions of complete unsanitary conditions or, on the contrary, wants to maintain sterile conditions somewhere in the operating room. But if the action loses its true meaning and becomes a mandatory ritual, it becomes a compulsion.
But if the action loses its true meaning and becomes a mandatory ritual, it becomes a compulsion.
However, OCD can manifest itself not only as a fear of pollution, but also as excessive superstition, fear of losing a necessary object, sexual or religious obsessive thoughts and related actions. Their reasons may lie in several areas: biological and psychological. The first includes diseases and features of the nervous system, lack of neurotransmitters (biologically active substances that ensure the transmission of a nerve impulse from one neuron to another, for example, dopamine or serotonin), genetic predisposition (mutations in the hSERT gene encoding the serotonin carrier protein and located on 17 -th chromosome).
There is also an infectious theory of the development of OCD, associated with the fact that in children it sometimes occurs after infection with streptococcus. This theory is called PANDAS - an abbreviation for the English Pediatric Autoimmune Neuropsychiatric Disorders Associated with Streptococcal infections, which translates as "Children's autoimmune neuropsychiatric disorders associated with streptococcal infections. " The cause of this syndrome may be an attack of its own antibodies produced against streptococcus on the patient's nerve cells. However, this theory has not yet been confirmed.
" The cause of this syndrome may be an attack of its own antibodies produced against streptococcus on the patient's nerve cells. However, this theory has not yet been confirmed.
Another group of explanations for the development of OCD is psychological. They go back to the theories of the beginning of the last century (from Freud to Pavlov). Mayakovsky's father died of blood poisoning after being injected with a binder, so it is believed that the poet also showed a pathological love for cleanliness. But you don't have to be a futurist poet to experience the full benefits of OCD: even dogs and cats suffer from it. Only in them this is expressed in the endless licking of wool and attempts to catch their tail.
The Yale-Brown scale is used to diagnose obsessive-compulsive disorder. In the fight against OCD, the method of psychological persuasion can be useful: patients are patiently explained that if they skip the “ritual” once, nothing terrible will happen. But drugs are also used in treatment.
When you are how you eat
Bulimia nervosa (third indication for Prozac) is a binge eating disorder. The main signs of bulimia are uncontrolled eating in large quantities, obsession with excess weight (calorie counting, attempts to induce vomiting after eating, fasting, use of laxatives), low self-esteem, low blood pressure. Other symptoms are sudden changes in body weight, kidney problems and dehydration, enlarged salivary glands, heartburn after eating, and inflammation of the esophagus. Due to provoking vomiting, hydrochloric acid from the stomach constantly enters the oral cavity of patients, which can lead to grinding of tooth enamel and ulcers on the mucous membrane. According to the DSM-5 classification of diseases, uncontrolled consumption of large amounts of food and the simultaneous use of various drastic measures for weight loss is the main criterion for diagnosing bulimia nervosa.
Video about bulimia on the educational medical resource Open Osmosis (USA)
The causes of bulimia can be either biological (incorrect levels of hormones or neurotransmitters, including serotonin) or social. The importance of the latter is highlighted, for example, in a high-profile study among teenage girls in Fiji, which showed a sharp increase in cases of intentional bowel cleansing for weight loss in just three years (from 1995 to 1998) after television appeared in the province. Perhaps the desire to be like models from the screens and covers really pushes for such behavior.
Bulimia can often be associated with other psychiatric disorders (depression, anxiety disorders, sleep disorders). According to a study by the New York State Psychiatric Institute and Columbia University, 70% of people with bulimia have ever experienced depression, compared with just over 25% in the general population.
Bulimia itself is not very common, and it can be more difficult to diagnose than the same anorexia, because changes in body weight in bulimia are less sharp and noticeable. For diagnosis, the food attitude test, developed by the Clark Institute of Psychiatry at the University of Toronto, and other tests based on it, are used. But (as with the tests for OCD and depression above), its result only indicates the likelihood that the patient has developed a disorder, but does not allow for a definitive diagnosis, especially for oneself.
For diagnosis, the food attitude test, developed by the Clark Institute of Psychiatry at the University of Toronto, and other tests based on it, are used. But (as with the tests for OCD and depression above), its result only indicates the likelihood that the patient has developed a disorder, but does not allow for a definitive diagnosis, especially for oneself.
From what, from what
What is a medicine that is prescribed for three types of disorders at once? The active ingredient in Prozac is fluoxetine. The patent for Prozac expired back in 2001, so many generics are available in pharmacies - cheaper copies that use the same active ingredient, but are not as well studied and may differ slightly from the original. These drugs include Fluoxetine, Prodel, Profluzak, Fluval.
Fluoxetine, discovered and marketed by Eli Lilly and Company, belongs to a group of antidepressants called selective serotonin reuptake inhibitors. This group is considered third-generation antidepressants, fairly well tolerated and without significant side effects.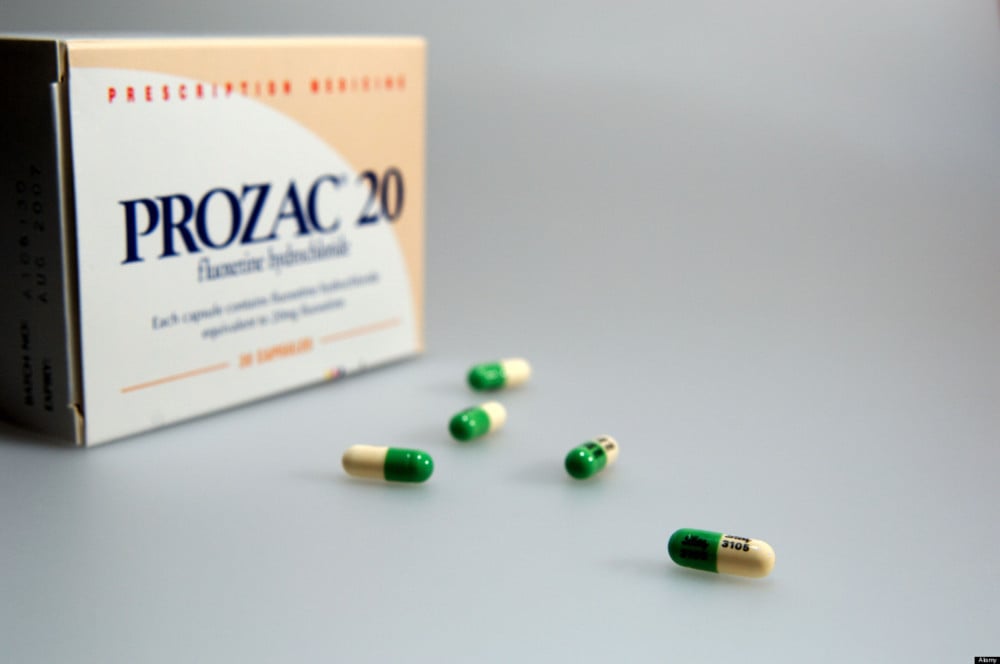
Fluoxetine is readily absorbed into the blood, can bind to plasma proteins and accumulate in body tissues. It also penetrates the blood-brain barrier, which protects the nervous system and brain from many substances circulating in the blood. There, in the nervous system, it works in the synaptic cleft we have already mentioned, preventing the excess serotonin ejected from the synapse from returning to the neurotransmitter. Because of this, serotonin is longer present in the synaptic cleft and can bind to receptors. How exactly fluoxetine achieves this effect is not clear even to manufacturers, but it is known that it has little effect on the work of other neurotransmitters. However, at high doses, fluoxetine increases adrenaline and dopamine levels, as studies in rat brain tissue show.
Fluoxetine and its metabolite, norfluoxetine, can interfere with each other's actions. Because of this, according to scientists from the Institute of Research Medicine in Barcelona, a constant concentration of fluoxetine in the blood is achieved only after four weeks of taking the drug. Similarly, the effects of taking the medicine do not disappear immediately. Associated with this is the difficulty in selecting the required dose for a particular patient.
Similarly, the effects of taking the medicine do not disappear immediately. Associated with this is the difficulty in selecting the required dose for a particular patient.
Serotonin itself, which is absolutely incorrectly called the “hormone of happiness” (hormones are produced in one organ of the body, but perform their function in another, serotonin in this context simply conducts nerve impulses in the parts of the brain responsible for good mood, and is produced there well), in fact, it performs much more functions. Yes, it affects mood, sleep, and appetite, so some cases of depression, bulimia nervosa, and OCD may be caused by insufficient production of this neurotransmitter and corrected with serotonin reuptake inhibitors. But in addition, platelets can actively capture it and affect blood clotting. Serotonin is also involved in the processes of memorization and learning. At the same time, not only vertebrate animals can produce it: according to a study by Chinese and American scientists, the pain from an insect bite is largely due to the presence of serotonin in the poison, and the dysentery amoeba, according to an article in Science, can cause diarrhea by releasing serotonin in our intestines.
The lists (not) included
But all these are only mechanisms, and besides, they have not been studied to the smallest detail. To understand how this works in real people and how often it helps, let's turn to clinical trials. However, anyone who enters the combination “fluoxetine depression double blind randomized controlled” into the PubMed scientific article database and filters clinical trial (clinical trial) will see more than 558 articles, up to work comparing the effectiveness of Prozac and homeopathy.
Double-blind, randomized, placebo-controlled method is a method of clinical drug research in which subjects are not privy to important details of the study being conducted. “Double-blind” means that neither the subjects nor the experimenters know who is being treated with what, “randomized” means that the distribution into groups is random, and placebo is used to show that the effect of the drug is not based on autosuggestion and that this medicine helps better than a tablet without active substance.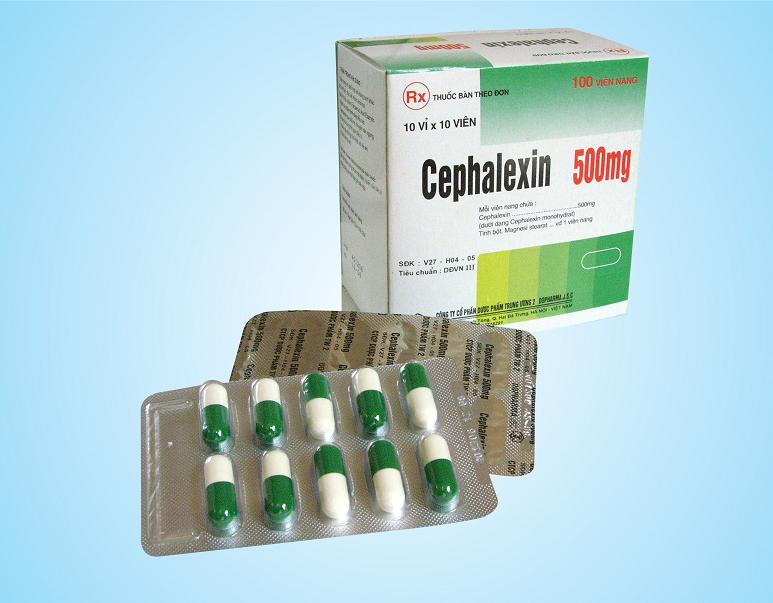 This method prevents subjective distortion of the results. Sometimes the control group is given another drug with already proven efficacy, rather than a placebo, to show that the drug not only treats better than nothing, but also outperforms analogues.
This method prevents subjective distortion of the results. Sometimes the control group is given another drug with already proven efficacy, rather than a placebo, to show that the drug not only treats better than nothing, but also outperforms analogues.
Indicator.Ru
Help
No living person can analyze them within an adequate period of time. And even Cochrane reviews can be found as many as 36 (that's really a lot), although not all of them consider the action of fluoxetine for its direct indications (depression, bulimia and obsessive-compulsive disorder).
The Cochrane Library is a database of the Cochrane Collaboration, an international non-profit organization involved in the development of World Health Organization guidelines. The name of the organization comes from the name of its founder, the 20th-century Scottish medical scientist Archibald Cochrane, who championed the need for evidence-based medicine and the conduct of competent clinical trials and wrote the book Efficiency and Efficiency: Random Reflections on Public Health. Medical scientists and pharmacists consider the Cochrane Database one of the most authoritative sources of such information: the publications included in it have been selected according to the standards of evidence-based medicine and report the results of randomized, double-blind, placebo-controlled clinical trials.
Medical scientists and pharmacists consider the Cochrane Database one of the most authoritative sources of such information: the publications included in it have been selected according to the standards of evidence-based medicine and report the results of randomized, double-blind, placebo-controlled clinical trials.
Indicator.Ru
Help
One of them is dedicated to antidepressants used against bulimia nervosa. Although in general the authors note that there is little data on this topic, fluoxetine (for which there were only five randomized double-blind controlled trials in 2003) is recognized as a leader in this direction. However, the authors refuse to recommend this medicine in the conclusion, arguing that not all clinical trial data have been published and are available for consideration.
A 2008 review reviewing the benefits of serotonin reuptake inhibitors (including fluoxetine) in obsessive-compulsive disorder, concluded that they worked better than placebo, and the side effects associated with them were much more significant, among which nausea was most common , insomnia and headache.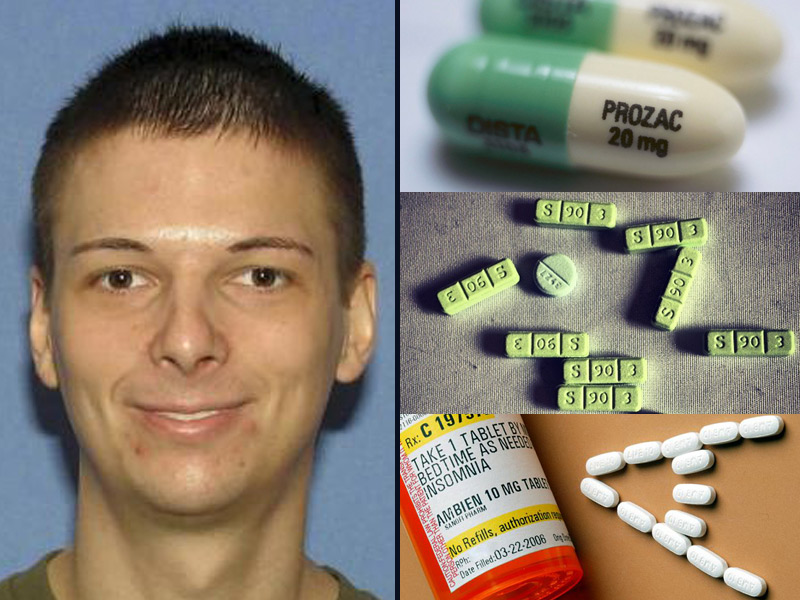 According to a 2013 review, the usefulness of this same group of drugs in autism and related OCD is unclear, and the data are insufficient to conclude.
According to a 2013 review, the usefulness of this same group of drugs in autism and related OCD is unclear, and the data are insufficient to conclude.
The most popular subject of fluoxetine reviews was fighting depression. But the authors of most of them note the lack of data (for example, in this 2013 review). In a broad inclusion criteria review of 1177 randomized controlled trials of fluoxetine for depression in adults, the authors conclude that it is about as effective as other antidepressants but less toxic. However, they warn against hasty decisions, since most of the studies were conducted on small groups of people (100 or less) and were funded by the manufacturer, which is more profitable to publish only positive results, hiding information about failures. Data on postpartum depression are also found to be insufficient and inconsistent. The same issues are highlighted by a review of articles on the effectiveness of antidepressants against dementia-related senile depression.
Indicator.Ru concludes: one of the best stimulant antidepressants is still not perfect
A large number of studies confirm the effectiveness of fluoxetine, a key component of Prozac. But part of the reviews of the Cochrane Collaboration note that not all trial data have been published by manufacturers. And this accusation is not an empty phrase: according to Eli Lilly's internal documents, manufacturers during trials often attributed suicide cases to worsening depression or overdosing on the drug.
As a result, following numerous reports of suicide by patients prescribed this drug, the US Food and Drug Administration (FDA) has issued a warning label to the drug's packaging.
This does not mean that the harm from the drug always outweighs its benefits, but such dishonest behavior of manufacturers does not allow us to assess the risks more accurately. Given the difficulty with the selection of an individual dose and the slow effect, adjusting the dosage is really not easy.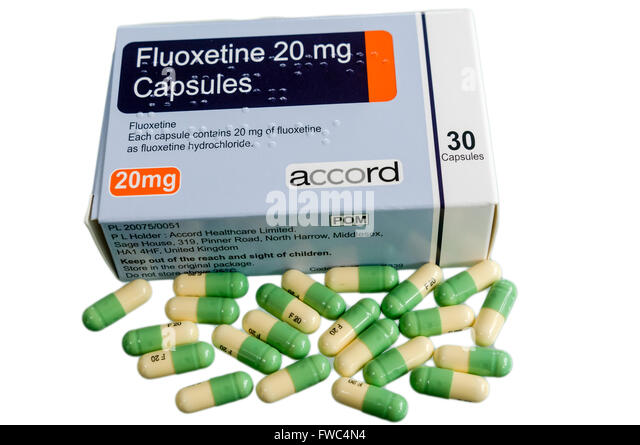
Prozac is also classified as a serotonin reuptake inhibitor, but if the cause of your condition is something else, you need to pay more attention to finding and eliminating them than fighting depression. As we wrote above, somatic diseases (for example, cirrhosis of the liver, cancer or diabetes), and even a lack of vitamins, can also cause depression. In addition, depression or another disorder may be the result of psychological trauma that will be difficult to deal with without psychotherapy.
All this suggests that the drug should be used under the supervision of a doctor (most likely, it will not be sold without a prescription), and that its action alone may not be enough for a complete recovery. And don't forget that serotonin is involved in many other processes in the body. Therefore, you should not use the drug in violation of the functions of the liver and kidneys, an increased risk of thrombosis, and not only during pregnancy and lactation. With manic states and suicidal moods, it is also better to abandon the drug.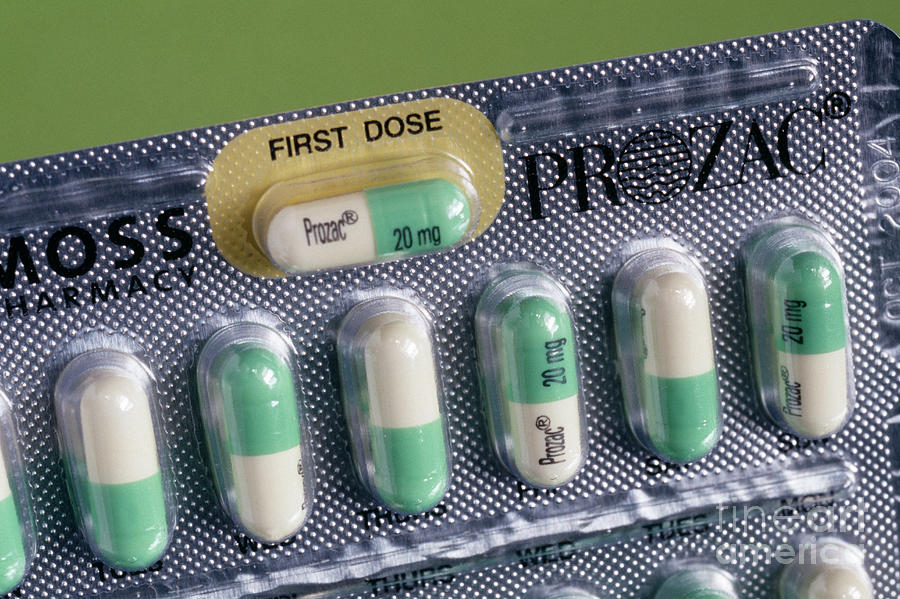
 decisions about the use of a particular drug.
decisions about the use of a particular drug.  20 mg: 14 or 28 pcs.
20 mg: 14 or 28 pcs. 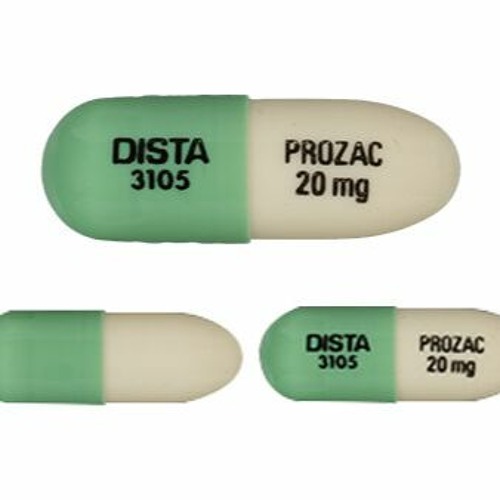
 Eating does not affect the degree of absorption, although it may slow down its rate. C max in plasma is achieved after 6-8 hours. C ss in plasma is achieved only after continuous administration for several weeks. Protein binding 94.5%. Easily penetrates through the BBB. It is metabolized in the liver by demethylation to form the main active metabolite of norfluoxetine.
Eating does not affect the degree of absorption, although it may slow down its rate. C max in plasma is achieved after 6-8 hours. C ss in plasma is achieved only after continuous administration for several weeks. Protein binding 94.5%. Easily penetrates through the BBB. It is metabolized in the liver by demethylation to form the main active metabolite of norfluoxetine.  2
2 
 Use with extreme caution in patients with moderate and mild renal impairment.
Use with extreme caution in patients with moderate and mild renal impairment. 

:strip_icc():format(webp)/kly-media-production/medias/2977951/original/030235400_1574750683-photo-of-a-man-kissing-a-woman-on-forehead-2532215.jpg)