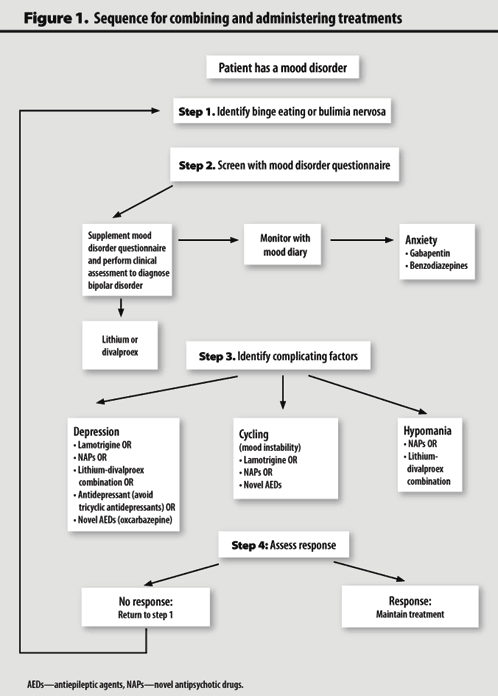
Diagnosing mood disorder
SAMHSA’s National Helpline | SAMHSA
Your browser is not supported
Switch to Chrome, Edge, Firefox or Safari
Main page content
-
SAMHSA’s National Helpline is a free, confidential, 24/7, 365-day-a-year treatment referral and information service (in English and Spanish) for individuals and families facing mental and/or substance use disorders.
Also visit the online treatment locator.
SAMHSA’s National Helpline, 1-800-662-HELP (4357) (also known as the Treatment Referral Routing Service), or TTY: 1-800-487-4889 is a confidential, free, 24-hour-a-day, 365-day-a-year, information service, in English and Spanish, for individuals and family members facing mental and/or substance use disorders.
This service provides referrals to local treatment facilities, support groups, and community-based organizations.
Also visit the online treatment locator, or send your zip code via text message: 435748 (HELP4U) to find help near you. Read more about the HELP4U text messaging service.
The service is open 24/7, 365 days a year.
English and Spanish are available if you select the option to speak with a national representative. Currently, the 435748 (HELP4U) text messaging service is only available in English.
In 2020, the Helpline received 833,598 calls. This is a 27 percent increase from 2019, when the Helpline received a total of 656,953 calls for the year.
The referral service is free of charge. If you have no insurance or are underinsured, we will refer you to your state office, which is responsible for state-funded treatment programs. In addition, we can often refer you to facilities that charge on a sliding fee scale or accept Medicare or Medicaid. If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
If you have health insurance, you are encouraged to contact your insurer for a list of participating health care providers and facilities.
The service is confidential. We will not ask you for any personal information. We may ask for your zip code or other pertinent geographic information in order to track calls being routed to other offices or to accurately identify the local resources appropriate to your needs.
No, we do not provide counseling. Trained information specialists answer calls, transfer callers to state services or other appropriate intake centers in their states, and connect them with local assistance and support.
-
Suggested Resources
What Is Substance Abuse Treatment? A Booklet for Families
Created for family members of people with alcohol abuse or drug abuse problems. Answers questions about substance abuse, its symptoms, different types of treatment, and recovery. Addresses concerns of children of parents with substance use/abuse problems.
Addresses concerns of children of parents with substance use/abuse problems.It's Not Your Fault (NACoA) (PDF | 12 KB)
Assures teens with parents who abuse alcohol or drugs that, "It's not your fault!" and that they are not alone. Encourages teens to seek emotional support from other adults, school counselors, and youth support groups such as Alateen, and provides a resource list.After an Attempt: A Guide for Taking Care of Your Family Member After Treatment in the Emergency Department
Aids family members in coping with the aftermath of a relative's suicide attempt. Describes the emergency department treatment process, lists questions to ask about follow-up treatment, and describes how to reduce risk and ensure safety at home.Family Therapy Can Help: For People in Recovery From Mental Illness or Addiction
Explores the role of family therapy in recovery from mental illness or substance abuse. Explains how family therapy sessions are run and who conducts them, describes a typical session, and provides information on its effectiveness in recovery.
For additional resources, please visit the SAMHSA Store.
Last Updated: 08/30/2022
SAMHSA Behavioral Health Treatment Services Locator
HomeWelcome to the Behavioral Health Treatment Services Locator, a confidential and anonymous source of information for persons seeking treatment facilities in the United States or U.S. Territories for substance use/addiction and/or mental health problems.
PLEASE NOTE: Your personal information and the search criteria you enter into the Locator is secure and anonymous. SAMHSA does not collect or maintain any information you provide.
Please enter a valid location.
please type your address
-
FindTreatment.
 gov
gov Millions of Americans have a substance use disorder. Find a treatment facility near you.
-
988 Suicide & Crisis Lifeline
Call or text 988
Free and confidential support for people in distress, 24/7.
-
National Helpline
1-800-662-HELP (4357)
Treatment referral and information, 24/7.

-
Disaster Distress Helpline
1-800-985-5990
Immediate crisis counseling related to disasters, 24/7.
- Overview
- Locator OverviewLocator Overview
- Locator OverviewLocator Overview
- Finding Treatment
- Find Facilities for VeteransFind Facilities for Veterans
- Find Facilities for VeteransFind Facilities for Veterans
- Facility Directors
- Register a New FacilityRegister a New Facility
- Register a New FacilityRegister a New Facility
- Other Locator Functionalities
- Download Search ResultsDownload Search Results
- Use Google MapsUse Google Maps
- Print Search ResultsPrint Search Results
- Use Google MapsUse Google Maps
- Icon from Find practitioners and treatment programs providing buprenorphine for opioid addiction (heroin or pain relievers).
 Find practitioners and treatment programs providing buprenorphine for opioid addiction (heroin or pain relievers).
Find practitioners and treatment programs providing buprenorphine for opioid addiction (heroin or pain relievers). - Icon from Find practitioners and treatment programs providing buprenorphine for opioid addiction (heroin or pain relievers). Find programs providing methadone for the treatment of opioid addiction (heroin or pain relievers).
The Locator is authorized by the 21st Century Cures Act (Public Law 114-255, Section 9006; 42 U.S.C. 290bb-36d). SAMHSA endeavors to keep the Locator current. All information in the Locator is updated annually from facility responses to SAMHSA’s National Substance Use and Mental Health Services Survey (N-SUMHSS). New facilities that have completed an abbreviated survey and met all the qualifications are added monthly. Updates to facility names, addresses, telephone numbers, and services are made weekly for facilities informing SAMHSA of changes. Facilities may request additions or changes to their information by sending an e-mail to [email protected], by calling the BHSIS Project Office at 1-833-888-1553 (Mon-Fri 8-6 ET), or by electronic form submission using the Locator online application form (intended for additions of new facilities).
Updates to facility names, addresses, telephone numbers, and services are made weekly for facilities informing SAMHSA of changes. Facilities may request additions or changes to their information by sending an e-mail to [email protected], by calling the BHSIS Project Office at 1-833-888-1553 (Mon-Fri 8-6 ET), or by electronic form submission using the Locator online application form (intended for additions of new facilities).
Affective disorders - symptoms, treatment, causes of the disease, first signs
Description
Affective mood disorders
These disorders are characterized by instability and instability of mood in children, adolescents and adults. Changes are observed predominantly in the direction of a major depressive disorder as depression or a manic mood swing. The intellectual and motor activity of the brain changes greatly.
Classification distinguishes the following types of affective disorders: seasonal, organic, bipolar, recurrent, chronic and endogenous affective personality disorder.
Among the majority of psychiatric disorders that exist today, not the last place is occupied by an affective disorder of various kinds. This disorder is quite common throughout the world. According to statistics, approximately every fourth inhabitant of the planet Earth suffers from one or another disorder associated with mood. And only twenty-five percent of these patients receive decent and competent treatment. In everyday life, this syndrome is commonly called depression. This condition is also quite common in schizophrenia. But the worst thing is that almost all people suffering from this disease simply do not realize that they are sick, and, therefore, do not seek the medical help they need so much.
All diseases of this direction according to microbial 10 can be divided into three main groups. These are depression, bipolar affective disorder or bar, and anxiety disorder. As part of the classification of these disorders among doctors and scientists there are constant disputes.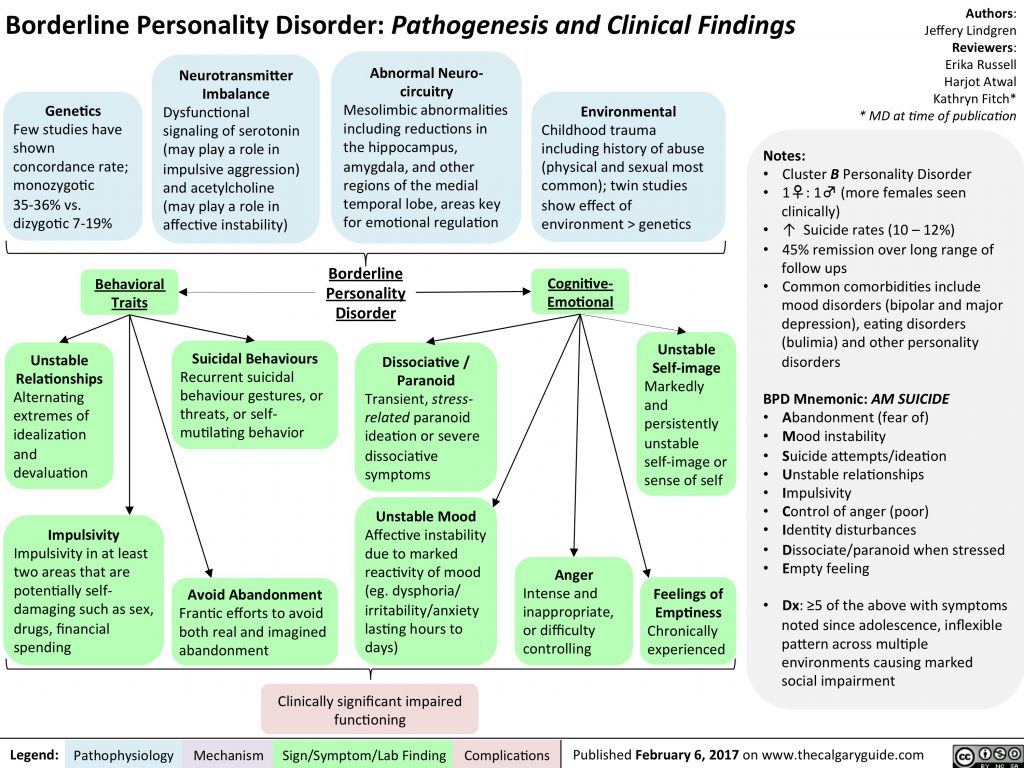
The whole difficulty lies in the fact that there is a huge number of different causes and symptoms that prevent a more complete and qualitative assessment. In addition, a big problem is the complete lack of high-quality and comprehensive methods of assessment and research based on various physiological and biochemical factors.
It is not comforting that mood disorders can easily overlap with the symptoms of many other diseases, which makes it difficult for the patient and doctors to obtain accurate information about which medical specialist is needed in a given case. If a patient has latent depression, then he can be under the supervision of many therapists and attending physicians for years and at the same time take medications that he does not need at all and are not able to provide effective treatment. And only in some cases the patient manages to get to a psychiatrist for further treatment.
All such disorders with untimely treatment have one prognosis. A person becomes exhausted and depressed, due to problems associated with the psyche, families can be destroyed, and the person is deprived of a future. However, as with any disease, there are specific ways and techniques to treat mood disorders, including the use of various medications and psychotherapy.
However, as with any disease, there are specific ways and techniques to treat mood disorders, including the use of various medications and psychotherapy.
Let's take a closer look at the types and patterns of affective spectrum disorders.
Depression
Everyone is familiar with this word. Stress and depression are the most common diseases on our planet. This disease is characterized primarily by despondency, apathy, a sense of hopelessness and a complete lack of interest in the surrounding life. And this should in no way be confused with the usual bad mood for several days. In the classic case of depression, it can be caused by abnormal metabolic processes in the brain. The duration of such depressive attacks can last from a few days to weeks or even months. Each subsequent day lived by the patient is perceived with longing, as a real punishment. The desire to live is lost, which often leads the patient to suicide attempts. Once joyful and full of emotions, a person becomes sad, sad and “gray”.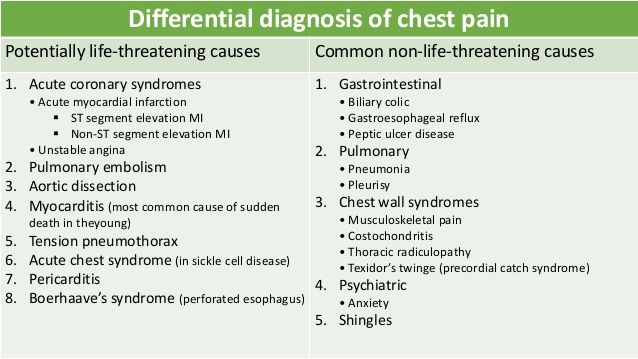 Not everyone is able to survive such a difficult period of life, since often such processes can be accompanied by loneliness and a total lack of communication, love, and relationships. In this case, only the timely intervention of doctors can help, which will preserve the mental and physical health of a person.
Not everyone is able to survive such a difficult period of life, since often such processes can be accompanied by loneliness and a total lack of communication, love, and relationships. In this case, only the timely intervention of doctors can help, which will preserve the mental and physical health of a person.
Dysthymia is a common medical disorder. By definition, this disorder is a milder form of depression. For a long time, perhaps for several decades, the patient experiences a constant sad mood. Such a state is characterized by a complete dullness of all feelings, which gradually begins to make life inferior and gray.
Depression can also be divided into expressed and latent. When it is pronounced, the so-called mask of grief can be seen on the patient's face, when the face is very elongated, the lips are dry along with the tongue, the look is menacing and frightening, tears are not noticed, the person rarely blinks. The eyes are most often slightly closed, the corners of the mouth are strongly lowered, and the lips are compressed.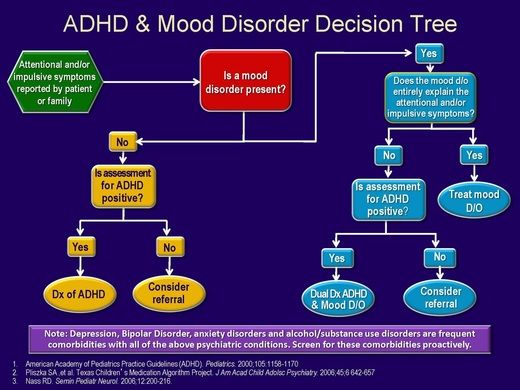 Speech is not expressed, more often such a person speaks in a whisper or silently moves his lips. The patient is constantly hunched over, and his head is lowered. A person can often mention his desperate and dreary state.
Speech is not expressed, more often such a person speaks in a whisper or silently moves his lips. The patient is constantly hunched over, and his head is lowered. A person can often mention his desperate and dreary state.
Latent or masked depression is a special case in medicine. In such patients, diseases of various organs and systems are most often observed, against which depression is masked. The disorder itself fades into the background, and the person begins to actively treat his body. However, this does not give a special effect, since the cause of all diseases lies in psychological depression and depression. Characteristically, patients themselves can completely deny and not accept their condition as depressive, concentrating with all their might on the treatment of sores caused by depression. Most often in these cases, the cardiovascular system and the gastrointestinal tract suffer. Pains of the migratory and localized type are noted. There is a breakdown, weakness, insomnia and vegetative-type disorders. All this happens with a parallel feeling of anxiety, anxiety, insecurity in one's actions and complete apathy towards one's life, work and favorite activities.
All this happens with a parallel feeling of anxiety, anxiety, insecurity in one's actions and complete apathy towards one's life, work and favorite activities.
Examinations done by doctors usually do not provide any specific explanations related to the patient's health complaints. Excluding all somatic diseases and taking into account a certain phase of the revealed disorders of the body, doctors single out an anxious and depressive state as a possible cause of all ailments, which can be confirmed by the observed effect after the start of psychotherapy and taking antidepressants.
Bipolar disorder
This mood disorder appears to be an alternating change in a person's state of being from depression to mania and back again. Mania is considered a period of time when a person has an excessively high mood, activity and good spirits. Often, such a state can be accompanied by strong aggression, irritation, delusional, obsessive ideas. Bipolar personality disorder, in turn, is also classified depending on how strongly it is expressed in the patient, as well as in what sequence the phases pass and how long they last separately. If these symptoms are mild, this condition of a person can be called cyclothymia. Let us consider the states of mania in more detail.
If these symptoms are mild, this condition of a person can be called cyclothymia. Let us consider the states of mania in more detail.
The state of mania
It is also called the manic state. The mood seems unnatural, the pace of thinking and movement is very fast. Optimism appears, facial expressions come to life. At these moments, a person seems to be able to do everything, he is tireless in his desires. There is a constant smile on his face, a person constantly jokes, makes jokes, and even considers serious negative events to be a mere trifle. During a conversation, he takes bright, expressive poses. The face is very red, the voice is quite loud. Orientation is usually not disturbed, and the person is completely unaware of the disease.
Anxiety disorder
This group of disorders is characterized by the presence of an anxious mood, constant anxiety and feelings of fear. Patients suffering from this disorder are constantly tense and expect something bad and negative. In especially difficult life situations, they begin the so-called motor anxiety, when a person rushes from side to side in search of a quiet place. Over time, anxiety grows and turns into unbridled panic, which dramatically reduces the quality of life of a person and those around him.
In especially difficult life situations, they begin the so-called motor anxiety, when a person rushes from side to side in search of a quiet place. Over time, anxiety grows and turns into unbridled panic, which dramatically reduces the quality of life of a person and those around him.
Symptoms
Photo: im9.kommersant.ru
Affective disorders, their general symptoms
Among the main markers are:
- sudden changes in mood for a long period;
- change in activity level, mental pace;
- changes in a person's perception of both various situations and himself.
- the patient is in a state of sadness, depression, helplessness, lack of interest in any activities;
- decreased appetite;
- lack of sleep;
- lack of interest in sexual activity.
For any symptoms suggestive of affective disorders, it is necessary to consider seeking the help of a psychiatrist for proper diagnosis and treatment.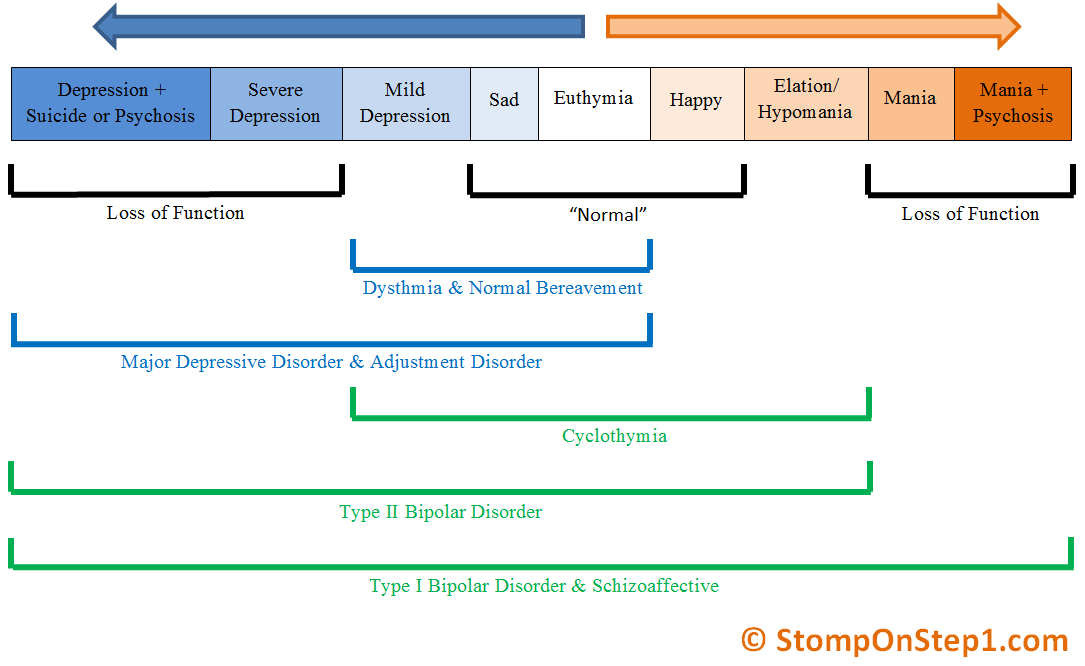
Causes leading to affective disorders
Disorders are the result of the patient's inability to control his emotions.
Depressive affective disorders, their symptoms and their types
Depressive affective disorders, formerly called clinical depression, are identified when a patient is diagnosed with several long periods of depression.
Several subtypes can be distinguished:
- Atypical depression. This type of depressive affective disorder is characterized by sharp mood swings towards positive, increased appetite (more often as a means of relieving stress), and, as a result, weight gain, a constant feeling of drowsiness, a feeling of heaviness in the legs and arms, a feeling of lack of communication.
- Melancholic depression (acute depression). The main symptoms are the loss of a sense of pleasure from many or all activities, a decrease in mood. Typically, these symptoms are aggravated in the morning. There is also a decrease in body weight, general lethargy, increased guilt.
- Psychotic depression - observed with prolonged prolonged depression, the patient has hallucinations, delusions may appear.
- Depression congealing (involutional). One of the rarest and most difficult types of affective disorders to treat. The patient, as a rule, is characterized by a state of stupor, or he is completely motionless, and the patient is also prone to making abnormal, meaningless movements. Such symptoms are also inherent in schizophrenia and may manifest as a consequence of neuroleptic malignant syndrome.
- Postpartum depression. It manifests itself in the postpartum period in women, the probability of diagnosing such a disease is 10-15%, the duration is no more than 3-5 months.
- Seasonal affective disorder. Symptoms appear seasonally: episodes are observed in the autumn and winter periods, disappearing in the spring months. The diagnosis is established when symptoms appear twice in winter and autumn periods without recurrence at other times of the year for two years.
- Dysthymia. It is a mild chronic deviation in mood, in which the patient complains of a constant decrease in mood over a long period. Patients with these problems have occasional manifestations of clinical depression.
Types of bipolar affective disorders and their symptoms.
Bipolar affective, defined as "manic-depressive syndrome", is a change from a manic state to a depressive one. In bipolar disorder, the following subtypes are distinguished:
- Bipolar disorder I. It is diagnosed in the presence of one or more cases of falling into a manic state, which can subsequently be accompanied by a state of clinical depression, or proceed without it.
- Bipolar disorder II. In this case, the patient's hypomanic state is always replaced by a depressive one.
- Cyclothymia. It is a less severe form of bipolar disorder. It proceeds in the form of infrequent hypomanic periods that appear from time to time against the background of the absence of more severe states of mania and depression.
Diagnosis
Photo: kremlinrus.ru.opt-images.1c-bitrix-cdn.ru
The disease, defined as an affective disorder, is by its nature close to the natural state of a person, duplicating emotional reactions that occur in moments of disaster or success . In connection with this fact, the diagnosis of bipolar disorders is significantly complicated. In the process of making a diagnosis, it is possible to conduct an examination of affective disorders using special techniques.
Mood disorders are often difficult to diagnose because the symptoms of the disease are similar to those of schizophrenia. Affective disorders include depressive and manic disorders. Depressive states, previously diagnosed as manic-depressive psychosis, are described by alternating periods of mania (lasting from 2 weeks to 4-5 months) and depressive periods (6 months).
Diagnosis of the main symptom that determines affective disorders consists in fixing changes in affect or mood without significant reasons for that. Affective state disorders include a complex of changes in habitual states of consciousness. However, the diagnosis of bipolar affective disorder only by the presence of the above signs is not entirely correct, since it concerns a separate type of disease.
Diagnosis of manic states consists in fixing the facts of sudden increases in mood to a state of admiration, a general increase in the patient's activity, obsessive thoughts with a visual overestimation of one's own personality. Periods of uplifting mood are replaced by short periods of depression, the ability to concentrate decreases, and there is a sharp increase in libido.
Manic disorders may be characterized by a lack of understanding on the part of the patient of his condition and the need for hospitalization in a specialized medical institution.
To diagnose mild or severe depressive mood disorders, the duration of the patient's condition must be at least a few weeks.
Diagnosis of bipolar affective disorder may be based on symptoms:
- deterioration in mood;
- lack of energy syndrome;
- lack of satisfaction;
- avoidance of social interactions;
- decrease in activity and decrease in motivation.
Diagnosis of bipolar affective disorder is carried out by a specialist in the presence of at least two manifestations of violations, of which one must be hypomanic or combined. In the presence of these symptoms, an examination of affective disorders is necessary. When analyzing research data and making a diagnosis, it is important to take into account that affective disorders can be caused by exposure to traumatic external factors. On the other hand, the diagnosis of hypomanic states can be hampered by the influence of chemical or non-chemical hyperstimulation on the outcome and diagnosis.
In any case, the diagnosis of bipolar affective disorder at an early stage is essential, since in the case of a single fact of violation of the patient's condition, treatment will be faster and easier than in the case of two or more episodes of the disease.
Methods for diagnosing affective disorders can be divided into:
- laboratory, which include tests to determine the content of folic acid in the body, the study of thyroid function, a general blood test, a general urine test;
- differential diagnosis of affective disorders, consisting in the presence of neurological diseases, the presence of disorders in the endocrine system, mental disorders with mood swings;
- special methods for diagnosing affective disorders, including magnetic resonance imaging, electrocardiogram;
- methods of a psychological nature: the Hamilton Depression Scale, the Rorschach test, the Tsung self-esteem scale.

Depending on the type of disease, a diagnosis of bipolar affective disorder is made. A positive test result for affective disorder requires treatment and, in extreme cases, hospitalization.
Sometimes, as a result of a diagnosis of bipolar affective disorder and additional investigations, a diagnosis of schizophrenia is made by specialists. This disease is characterized by specialists as an irreversible process, consisting in the destruction of the personality structure. Is it possible to remove the diagnosis of bipolar affective disorder? The likelihood of this happening is very low, as there is a complex procedure for removing the diagnosis of bipolar affective disorder, which is facilitated only if a misdiagnosis is identified. In fact, only if there is an error made by the doctor during the examination, you can remove the diagnosis of bipolar affective disorder. The second case in which the diagnosis of bipolar affective disorder can be removed is an error in the analysis of an affective disorder test, which is practically impossible.
Bipolar affective disorder is diagnosed by a specialist in a diagnostic center or hospital according to the ICD-10 system. Self-diagnosis often leads to errors that can aggravate a person's condition against the background of the possible presence of a disease, improper treatment due to the intricacies of the difference between diseases and the means used to cure them.
Treatment
Photo: topkin.ru
Treatment takes place under the supervision of a psychotherapist or psychiatrist. In the presence of provoking neurological, endocrine or mental disorders, therapeutic measures are carried out with the participation of doctors of the appropriate profile: neurologists, endocrinologists, psychiatrists. The following methods are used to eliminate affective disorders:
- Drug therapy. Drugs are used that eliminate the imbalance of neurotransmitters in the brain, normalize mood, have a calming, hypnotic or activating effect.
- Psychotherapy.
 Recommended a variety of psychotherapeutic techniques aimed at normalizing the emotional state. Psychological sessions in most cases are an obligatory part of the treatment, they are used in isolation or in combination with medications.
Recommended a variety of psychotherapeutic techniques aimed at normalizing the emotional state. Psychological sessions in most cases are an obligatory part of the treatment, they are used in isolation or in combination with medications.
The average course is 2-3 months, and sometimes lasts for several years. The duration depends on the reasons that caused this condition. In most cases, patients are observed on an outpatient basis. In the presence of severe disorders, which are accompanied by a manic state, suicide attempts, a decision is made to place the patient in a hospital. Electroconvulsive therapy (ECT) is sometimes recommended in the event of a negative response to drug therapy or the ineffectiveness of medications in severe cases.
Psychotherapy
Psychotherapy plays an integral role in the treatment of affective disorders. It is aimed at detecting psychological problems that affect the onset of symptoms of the disease, helping to achieve a complete recovery or sustainable remission. The most commonly used methods are:
The most commonly used methods are:
- Cognitive behavioral therapy. Recommended for identifying irrational thought patterns and their subsequent correction. After working with cognitive aspects, activities are carried out to change behavior.
- Training of cognitive functions. As part of the classes, exercises are carried out to improve memory, thinking, and concentration.
- Treatment management training. Useful in chronic pathologies. They help patients to determine the beginning of a possible exacerbation by characteristic signs, to control their condition.
Psychotherapy can be done in an individual, family or group format. At the initial stage, individual sessions are preferred. Along with cognitive-behavioral therapy, psychoanalytic techniques, gestalt therapy, art therapy can be used. If there are problems in the relationship that negatively affect the course of the disease, the patient's partner is involved in psychotherapy.
Group classes are switched to after the patient's condition improves. The method allows you to share your experiences in a friendly environment, conduct introspection and get the necessary support from people who suffer from the same problem. To increase the likelihood of a positive outcome, it is advisable to visit a psychologist not only for the patient, but also for his relatives. This is due to the fact that a comfortable living environment and an adequate perception of a person with psychological problems has a positive effect on his condition.
Treatment of bipolar disorder
Treatment for bipolar disorder aims to eliminate the underlying symptoms, achieve sustained remission, and prevent relapses. In general, medicines are used:
- in the presence of a depressive state, antidepressants are prescribed;
- with manic syndrome, which is accompanied by an unreasonable change in mood, increased activity, followed by a breakdown, anti-manic drugs are indicated: mood stabilizers, antipsychotics, antipsychotics.

Antidepressants should be taken long-term, 4 months or more. Even after the patient's condition improves, it is not recommended to interrupt the course of treatment on your own, as this can lead to a deterioration in the condition and the return of unpleasant symptoms. The effect of antidepressants becomes noticeable 2-4 weeks after the start of treatment. Sometimes the medicine has to be replaced due to insufficient effectiveness or severe side effects.
Rapid phase inversion indicates incorrect selection of drugs or therapeutic tactics. The use of various medications shows the best result during the debut period. If drugs are first prescribed after several affective episodes, it becomes more difficult to achieve a stable remission.
Treatment of seasonal depression
For seasonal affective disorder, methods such as:
- Light therapy. The patient is assigned several sessions, during which he is under special bright lamps for 30-60 minutes.
 This technique shows a good result, helps to improve the emotional state and normalize sleep.
This technique shows a good result, helps to improve the emotional state and normalize sleep. - Cognitive behavioral therapy. Aimed at eliminating the psychological problems that caused this disorder. Provides for a change in habitual behavior to improve adaptation to adverse conditions (cold, lack of lighting).
- Correction of circadian rhythms. When daylight hours decrease, melatonin levels decrease. This can affect a person's mood, impair sleep, and cause affective disorders. Melatonin preparations help eliminate the disorder. The method is especially indicated for shift work, night shifts.
- Medical therapy. Taking antidepressants, tranquilizers and sedatives is not indicated for all patients. Required for severe disorders, severe lethargy or emotional lability, sleep disturbances.
In order to prevent the development of the disease, it is recommended to monitor nutrition in the winter, play sports, lead an active lifestyle, and regularly go outside.
Prevention of affective disorders
Preventive measures are effective mainly in psychogenic disorders. With the endogenous nature of disorders are of lesser importance, they help to reduce the significance of aggravating factors. They include minimizing stress, normalizing the daily routine, good nutrition, regular physical activity, taking into account the state of health and level of training.
In the presence of childhood traumas, difficult life circumstances, frequent or prolonged stressful situations, psychotherapy is necessary. In addition, work with a psychologist is currently being considered as a way to improve the overall level of mental health and quality of life, and increase the amount of resources. A positive result appears when the patient receives the support of relatives, friends and doctors.
In severe cases, with a high risk of recurrence of the disease, supportive drug therapy is prescribed. Cancellation of any drugs can only be carried out by a specialist who is able to assess all the risks. An important aspect of the prevention of affective disorders is their recognition by society, respect for people with similar problems, and the absence of stigmatization.
An important aspect of the prevention of affective disorders is their recognition by society, respect for people with similar problems, and the absence of stigmatization.
Medications
Photo: medvoice.ru
Treatment of depression
Medications are selected taking into account the prevailing symptoms. Antidepressants with a calming or activating effect may be used. The first group of drugs is indicated for the predominance of anxiety and irritability, the second - for lethargy, apathy, lethargy.
The action of all antidepressants is due to their influence on the metabolism of neurotransmitters in the brain. The use of tricyclic antidepressants (TAD) is effective for disorders of any severity. MAO inhibitors show a higher effectiveness in mild forms of depression. Negative aspects of the treatment of TAD and MAO inhibitors are a significant period of time between the start of administration and changes in the psycho-emotional state, frequent side effects, most noticeable at the beginning of therapy.
To solve these problems, tranquilizers are often prescribed along with antidepressants. Unlike MAO and TAD inhibitors, which are used for six months or more, tranquilizers are always used for a short time (no more than 1 month), because with constant use they cause dependence. In patients with bipolar disorder, after the disappearance of depressive symptoms, the state may become hypomanic. In this case, neuroleptics are recommended in combination with various types of cognitive therapy.
Treatment of manic disorders
Antipsychotics are effective in severe mania. Treatment with lithium carbonate shows high efficiency at this stage of the disease, however, since the effect of its administration occurs after a week, this drug is usually not used in the acute phase of the disease. Normotimics help reduce the severity of mood swings. Includes the following groups of agents:
- lithium salts;
- anticonvulsants (also used to treat epilepsy).
Antiepileptic drugs are the preferred option due to the greater risk of lithium salts. During therapy with drugs of the latter group, it is important to strictly monitor the amount of table salt consumed, since it competes with lithium when excreted through the kidneys. An increased concentration of lithium can cause a feeling of weakness and incoordination.
During therapy with drugs of the latter group, it is important to strictly monitor the amount of table salt consumed, since it competes with lithium when excreted through the kidneys. An increased concentration of lithium can cause a feeling of weakness and incoordination.
Folk remedies
Photo: i-gency.ru
Folk methods of treatment play an auxiliary role in the treatment of affective disorders. They help to stabilize the emotional state, improve sleep and mood, reduce anxiety, relax the body. They are used only after the approval of the doctor. Most often, complex treatment programs include herbal medicine, aromatherapy, yoga, meditation and acupuncture.
Phytotherapy
Motherwort and valerian are widely known herbal remedies for normalizing the psycho-emotional state. In addition, herbal preparations are used, consisting of May lily of the valley, lemon balm leaves, mint and nettle, belladonna, chamomile flowers, flowers and herbs of St. John's wort, burdock root.
St. John's wort in any form is allowed only under the supervision of a physician, since herbal medicine can accelerate the transition from mania to depression. Licorice root and black cohosh contribute to the normalization of the menstrual cycle and may be useful for the treatment of mood disorders in women. Myrtle flowers give a good result, they are used for baths, added to tea, and infusions are made. Since ancient times, "black melancholy", as depression used to be called, has been successfully treated with saffron. To stabilize the mood, it is recommended to take baths with mint, lemon balm, oak bark.
Aromatherapy
Aromatherapy is indicated to relieve emotional stress, insomnia, to increase the effectiveness of drug therapy and psychotherapy. The result of the use of essential oils is due to the fact that the center of the brain responsible for the perception of smells is closely connected with emotions. Anxiety, irritability, fatigue and insomnia are treated with oils of citrus, juniper, mint, cypress, lavender, patchouli, marjoram. With obsessive fears, violet, rose, sandalwood, vanilla, and tea tree oils are useful.
With obsessive fears, violet, rose, sandalwood, vanilla, and tea tree oils are useful.
Acupuncture
Acupuncture or acupuncture is one of the healing methods of Chinese traditional medicine. Used in addition to drug therapy for the treatment of depression and bipolar disorder. Regular acupuncture sessions can reduce symptoms and prolong remission.
Yoga and meditation
Yoga and meditation reduce stress and promote relaxation. With the help of breathing exercises, you can learn to control emotions, relieve anxiety and get rid of mood swings. In addition, yoga helps to stay in good physical shape, which has a positive effect on the psychological state.
Precautions
Non-native medicine methods are a useful addition to the recommended course of therapy, but require certain precautions:
- A physician should be consulted before any methods are used. Self-medication can harm more disease.
- Natural doesn't mean harmless.
 You should learn about all possible side effects and interactions with other drugs before starting treatment.
You should learn about all possible side effects and interactions with other drugs before starting treatment. - Do not stop taking prescribed medications or psychotherapy sessions. Folk remedies cannot replace traditional treatment regimens; refusal to comply with medical recommendations can cause a deterioration in the condition.
The information is for reference only and is not a guide to action. Do not self-medicate. At the first symptoms of the disease, consult a doctor.
Sources
- Affective disorders. Teaching aid / Snedkov E.V., Lemeshev I.V. – 2017.
- Affective disorders / Krasnov V.N. – 2011.
- Fundamentals of General Psychopathology / Voropaeva S.V. – 2012.
- Clinical Guide to Mental Disorders / ed. Barlow D. - 2008.
Your comments about the symptoms and treatment
Cyclothymia - symptoms, causes, risk factors, diagnosis and treatment in medical centers "K + 31
Cyclothymia is a mood disorder that manifests itself as a cyclic change, fluctuations in good and bad mood. At its core, cyclothymia is very similar to manic-depressive psychosis (bipolar affective disorder, BAD), moreover, a number of psychiatric schools consider cyclothymia as a mild form of BAD. Also, cyclothymia has much in common with dysthymia and recurrent depression. There may be a period of mental health between episodes of high and low mood.
At its core, cyclothymia is very similar to manic-depressive psychosis (bipolar affective disorder, BAD), moreover, a number of psychiatric schools consider cyclothymia as a mild form of BAD. Also, cyclothymia has much in common with dysthymia and recurrent depression. There may be a period of mental health between episodes of high and low mood.
In the classic version, cyclothymia occurs at a young age and takes a chronic course. Initially, episodes of mood swings do not have a long course, leaving more time for a period of mental health (intermissions). Timely treatment prevents the progression of the disease, and in the absence of adequate medical care, the duration of intermissions is progressively reduced.
Causes of cyclothymia
The immediate cause of cyclothymia, as with most mental disorders, is unknown. Researchers in the field of psychiatry prefer the hereditary factor, since cyclothymia most often occurs in people whose relatives suffered from bipolar affective disorder. Other severe mental disorders in the form of major depressive, panic and anxiety disorders can also be considered a burdened heredity.
Other severe mental disorders in the form of major depressive, panic and anxiety disorders can also be considered a burdened heredity.
Persons with neurosis, anxiety, suspiciousness are prone to cyclothymia. The risk of cyclothymia is increased in people who use psychoactive substances or abuse alcohol (especially at a young age).
Clinical picture of cyclothymia
Symptoms of cyclothymia are divided into two opposite groups: symptoms of "good mood" and symptoms of "bad mood".
Symptoms of good mood (phase of hyperthymia) are manifested by energy, hyperactivity (personal, domestic, social), mood rise, increased efficiency. The patient is haunted by a sense of permanent well-being, which sometimes leads to an inadequate assessment of the environment. Reduced sleep time. Of the clearly negative aspects of hyperthymia - familiarity, rude behavior, irritability, decreased concentration, fussiness. Hypomania is a condition in which the above symptoms are more pronounced than with hyperthymia, but less than with manic episodes.
Symptoms of bad mood (phase of depression, dysthymia) are characterized by all the classic signs of ordinary depression, but they have a more erased course:
- Prolonged deterioration in mood;
- Decreased interest in all areas;
- Cognitive impairment;
- Decreased self-esteem, own capabilities;
- Hypodynamia, restlessness;
- Poor sleep at night and drowsiness during the day;
- Loss of appetite;
- Appearance of false pain and other symptoms from internal organs (according to the type of somatoform reactions).
Due to the peculiarities of the clinical picture, cyclothymia rarely comes to the attention of psychiatrists or psychotherapists. Very often, patients do not even suspect that they have this mental disorder, since it practically does not affect the quality of life, does not impair professional skills, and is not noticeable to others. Moreover, an episode of elevated mood (especially the phase of hyperthymia) is very often perceived by a person as a period of complete well-being, to which one should strive.
Despite the relative harmlessness or even the imaginary positiveness of cyclothymia, this condition is a mental disorder and requires adequate treatment. Otherwise, there is a high probability of progression of the disease up to the occurrence of bipolar affective disorder or other severe mental pathology.
Clinical treatment of cyclothymia k+31
Treatment of cyclothymia usually does not require hospitalization. All appointments of the attending doctor can be performed on an outpatient basis, but this requires regular supervision by a specialist. Inpatient conditions are indicated for patients who do not perform or violate the treatment regimen, as well as in case of need for active therapeutic actions. Otherwise, according to modern recommendations, cyclothymia is treated on an outpatient basis and for a long time (at least 6 months).
The main task of psychotherapy in cyclothymia is to fully inform the patient about the state of his health, about the need for treatment, despite apparent well-being, about adverse consequences in case of refusal or violation of the therapeutic regimen.



